
Depression: Root Causes and Natural Support Strategies
Depression is rampant in Western countries which have more money and privilege than anywhere else in the world. About 1 in 4 adults in the U.S., more than 26% of the population, suffers from a diagnosable mental disorder. Anxiety afflicts more than 40 million Americans. Nearly 10% of the U.S. adult population has a mood disorder for which powerful drugs are prescribed. (That’s about 30 million people on psychiatric drugs!) (1)
Depression, which affects one in ten of us (including a quarter of women in their forties and fifties), is now the leading cause of disability worldwide. People with chronic depression oftentimes have significant biochemical imbalances in their neurological tissue. In this article, you will discover the root cause factors involved in depression and the best natural support strategies.
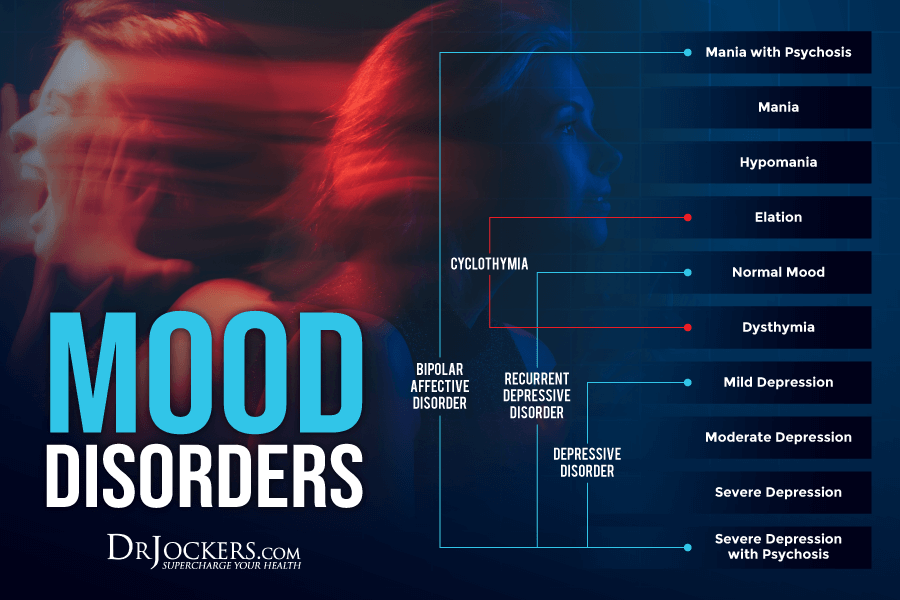
Depression and Brain Inflammation:
New research has indicated that this imbalance is not a genetic flaw as was once thought but instead is due to a heavy onslaught of toxicity or severe nutritional and lifestyle based deficiency that cause massive brain inflammation that disrupts normal neurological processing (2, 3, 4).
Fortunately, when these causative factors are addressed, one can overcome the chemical imbalances and beat depression naturally. My hope is that this article gives you realistic strategies to use yourself and with family members and friends to ease the burden of depression in our society.
The Pharmaceutical Solution:
Depression and neuro-emotional diseases such as bipolar, schizophrenia, etc. are at an all-time high. The pharmaceutical industry has brought out dozens of blockbuster drugs to treat all of these conditions with billions of dollars of revenue every year.
Many individuals have gotten some benefits from these medications to treat depression. Most report short-term benefits with waning long-term results (5).
Unfortunately, none of these drugs treat the cause of the chemical imbalance but merely treat the symptoms and come with a whole host of frightening side effects. In fact, years back the FDA mandated labeling requiring anti-depressant manufacturers to include a warning that these drugs increase suicide risk (which is one of the things they are supposed to prevent) (6).
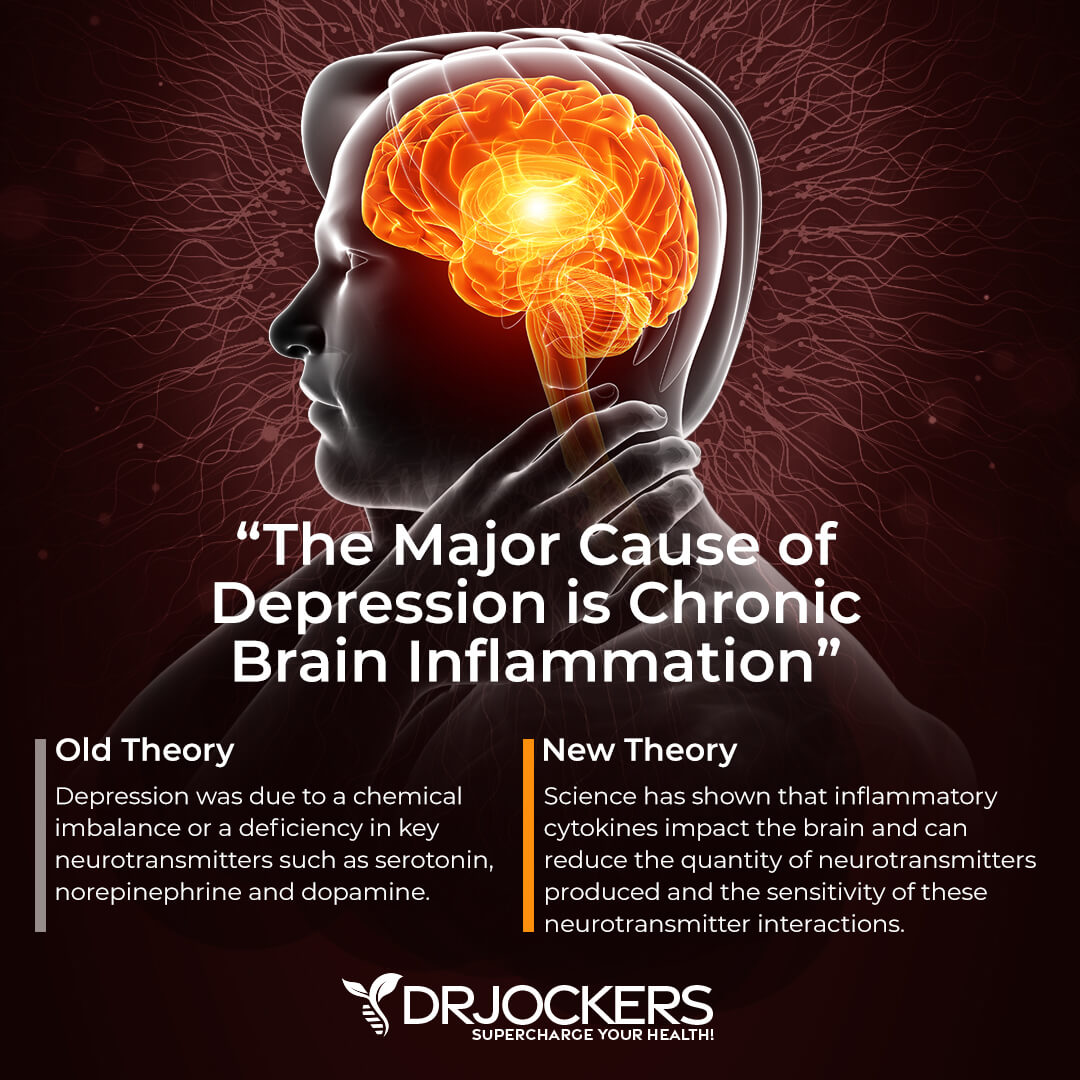
Inflammation and Depression:
The body creates inflammation to prevent infections. Since systemic infections have killed more people in the history of mankind than anything else, it makes sense that the body has adapted to hardwire a sophisticated inflammatory mediating system.
One major inflammatory mediator is called a cytokine. Cytokines are cell signaling molecules that aid cell-to-cell communication in immune responses and stimulate the movement of cells towards sites of inflammation, infection, and trauma. Examples of cytokines include interleukins and interferons which are found in abundance in sites of inflammation.
Individuals with depression have been shown to have higher levels of inflammatory cytokines in their neurological tissue (7, 8). One study showed that individuals suffering have significantly higher plasma inflammatory cytokines compared to a control group and after 12 weeks of treatment they saw these markers reduce (9).
Growing evidence suggests that specific cytokines signal the brain to generate neurochemical, neuroimmune, neuroendocrine, and behavioral changes. An imbalance of cytokines within the central nervous system (CNS), or even systemically, may play a role in the pathophysiology of mood disorders (10, 11).
 Brain Inflammation and Anti-Depressants:
Brain Inflammation and Anti-Depressants:
Modulation of these cytokines by chronic antidepressant treatment may result in restored balance. Many scientists believe that the benefits some individuals receive from anti-depressants are actually due to the mild anti-inflammatory effect these drugs have and not on the chemical neurotransmitter regulation that the medications are marketed and sold for (12).
A New England Journal of Medicine review on Major Depression stated:
” … numerous studies of norepinephrine and serotonin metabolites in plasma, urine, and cerebrospinal fluid as well as postmortem studies of the brains of patients with depression, have yet to identify the purported deficiency reliably.”
This also explains why natural anti-inflammatories outperform anti-depressants in clinical trials. These natural anti-inflammatories include exercise, sun exposure, omega-3 fatty acids, curcumin, resveratrol, and adaptogenic herbs like ashwagandha for example (13, 14, 15, 16, 17).

The Microbiome and Depression:
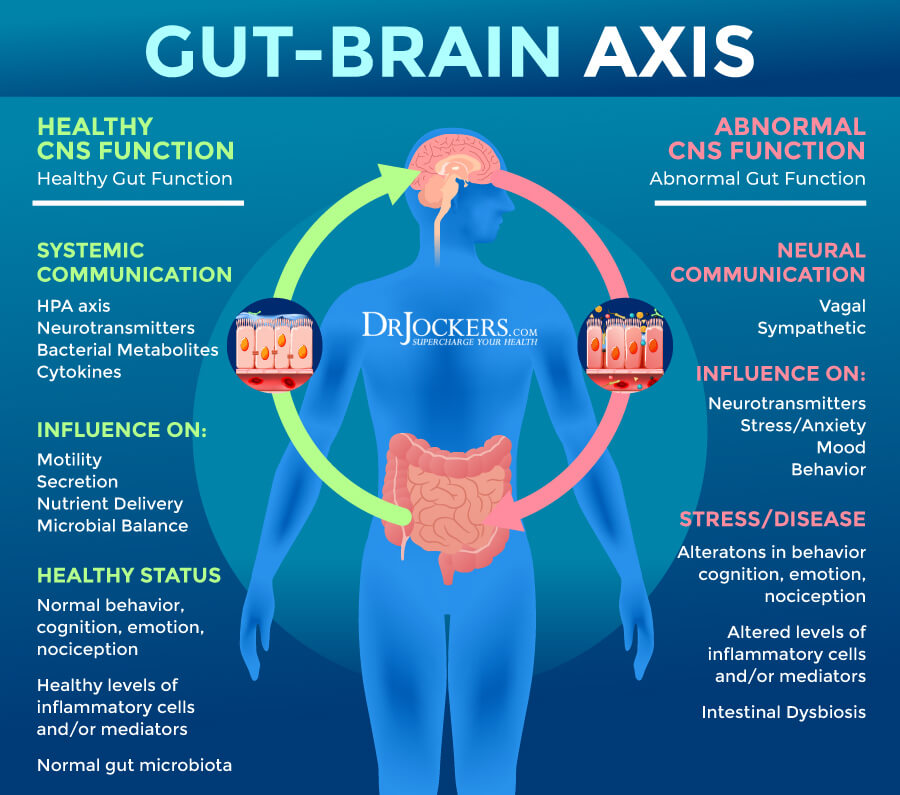
There has been a tremendous amount of research linking the gut microbiome and neurological health. Gut bacteria produce hundreds of neurochemicals that the brain uses to regulate basic physiological processes as well as mental processes such as learning, memory, and mood. For example, gut bacteria manufacture about 95 percent of the body’s supply of serotonin, which influences both mood and GI activity.
Research has indicated that low levels of healthy lactobacillus and Bifidobacterium are linked with increased brain excitability and neurological inflammation (18, 19, 20). These microbes help to break down the excitatory neurotransmitter glutamate into the inhibitory neurotransmitter GABA. Low levels of GABA production are associated with anxiety, seizures, depression, dementia, and Alzheimer’s.
Additionally, pathogenic microbes can secrete toxic metabolites that cause increased excitatory responses in the brain and increase inflammatory cytokine activity. In particular, a substance from gram-negative bacteria (E coli, Salmonella, Shigella, etc.) has a waste product called lipopolysaccharide (LPS) that inflames the brain and creates depressive like behavior (21, 22).
Blood Sugar and Depression
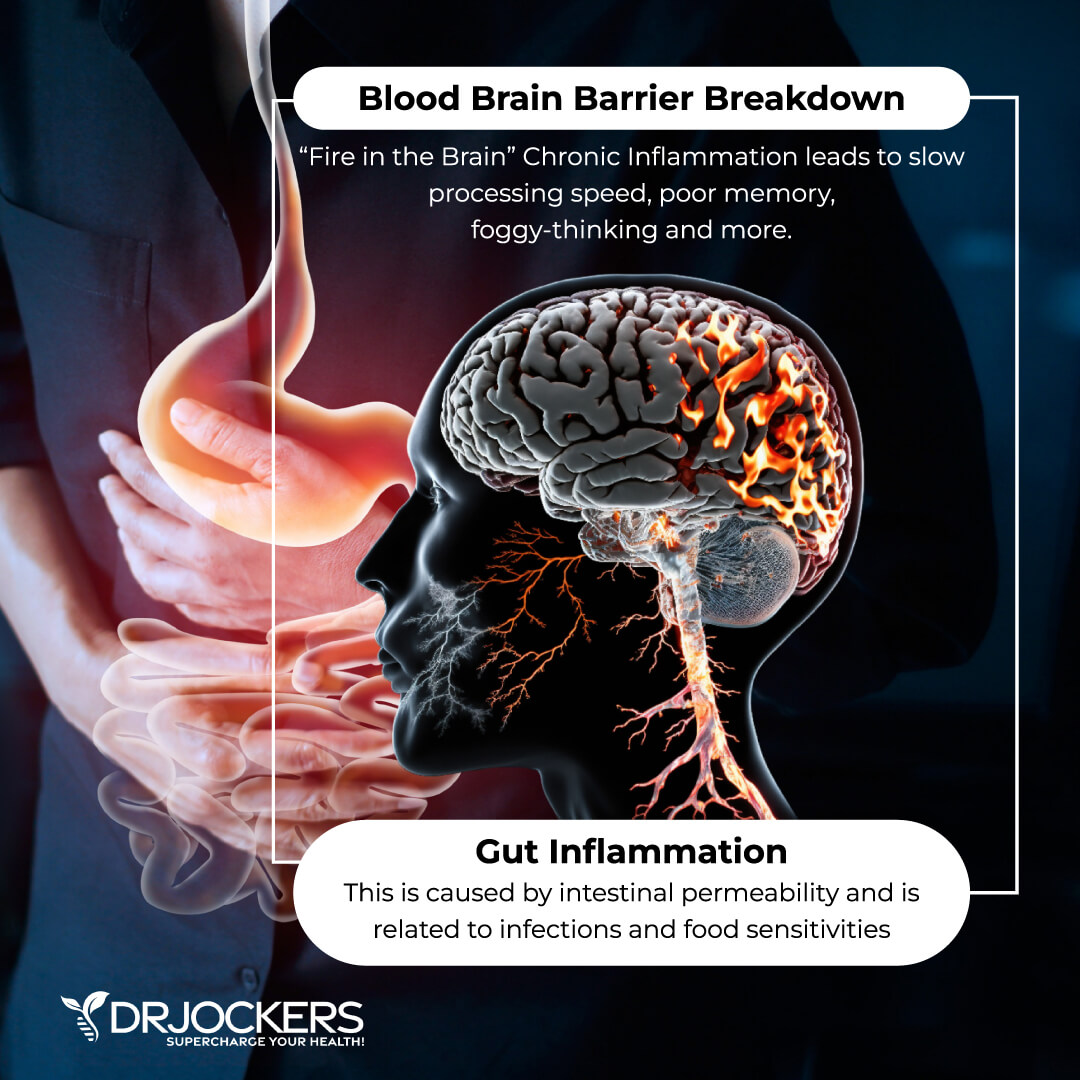
The blood-brain barrier (BBB) is a tight network of blood vessels that is designed to only allow small nutrients to pass into the brain. The BBB is a mechanism the body uses to protect the brain from oxidative stress, infectious microbes, infectious microbes, and chronic inflammation.
When blood sugar is thrown off balance it leads to openings in the BBB that allow for toxins to cross into the brain and increased inflammatory activity in the brain. This inflammation reduces neurotransmitter levels and leads to increased states of anxiety and depression (23, 24).
Blood sugar imbalances also lead to nutrient deficiencies in key B vitamins, trace minerals, and magnesium that further weaken the BBB and increase oxidative stress and inflammation in the brain.

Poor Sleep & Circadian Rhythm Disruption
Your body needs proper sleep for your physical, mental, and emotional health. Sleep is the time when your cells can finally rest, relax, and repair. Without proper sleep, they cannot do that, which may lead to inflammation, low mood, low energy, morning fatigue, and other health issues.
According to research, about 90 percent of people with depression suffer from sleep quality complaints. About two-thirds of patients undergoing a major depressive episode will experience insomnia, with about 40% of patients complaining of problems initiating sleep (sleep onset difficulties), maintaining sleep (frequent awakenings), and/or early-morning awakenings (delayed or terminal insomnia), and many patients reporting all three (25).

Hypersomnia occurs in about 15% of patients. Hypersomnia is a condition that is characterized by excessive sleepiness and long stretches of sleep even during the day.
Insomnia is the opposite, characterized by trouble falling and staying asleep. Sleeping too long or too little disrupts your circadian rhythms. Your body will be confused and won’t be able to tell when it’s time to sleep or stay awake. This will feed the cycle of sleep troubles, depression, and low energy.

Gluten and Brain Inflammation:
Gluten is the common protein molecule found in wheat, barley, rye, kamut, and spelt. Gluten is a sticky storage protein that binds to the small intestinal wall where it often causes digestive and immune system disorders.
There is extensive research on gluten sensitivity and disorders in every part of the neurological system. Gluten is a significant trigger in psychiatric disorders such as anxiety, bipolar disorder, depression, and schizophrenia (26, 27). If you have one of these issues it is critical to go 100% gluten-free.

Mitochondrial Dysfunction:
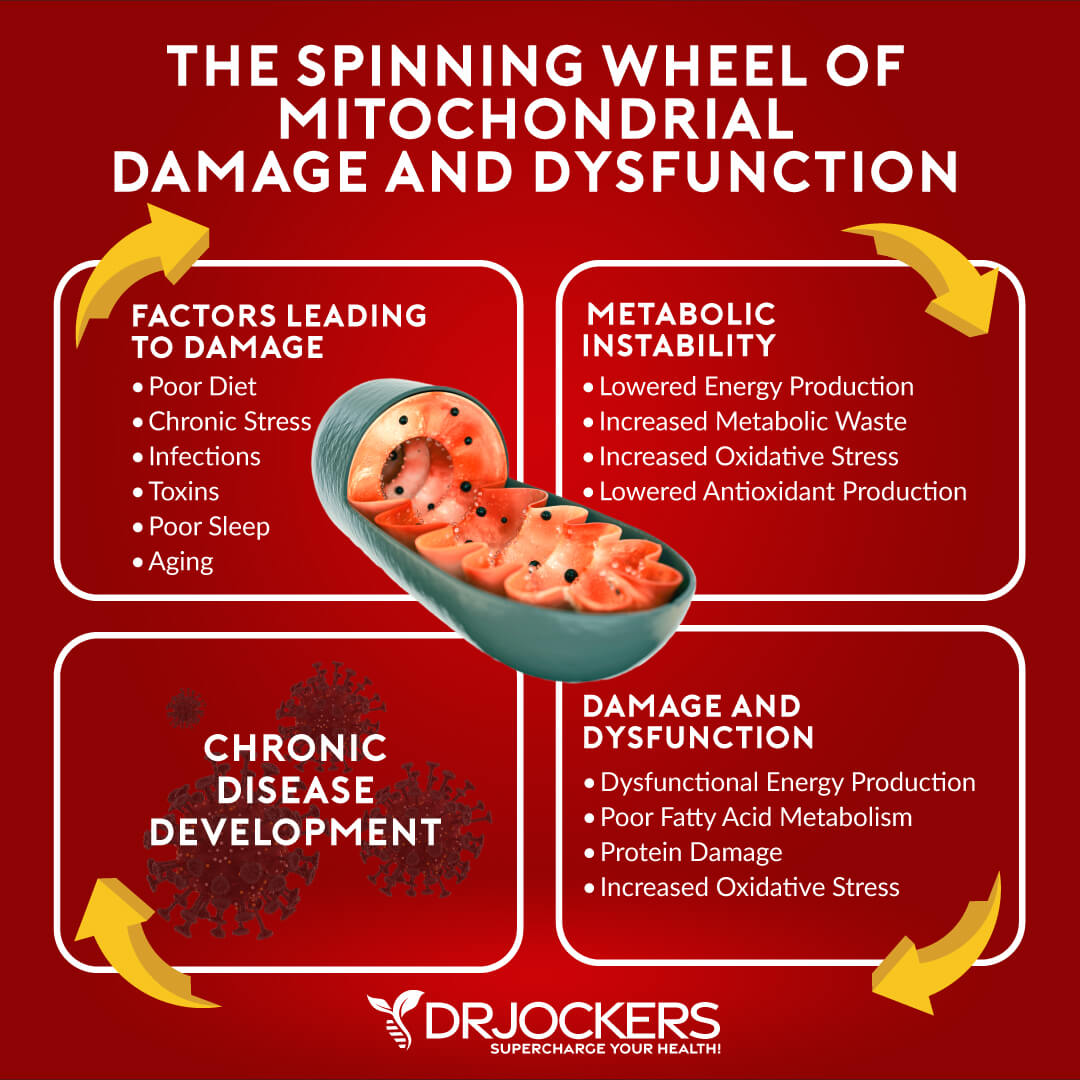
Every cell of the body has mitochondria within it that produce energy for the cell. The mitochondria are the battery packs of the cell, and they are extremely important. High levels of oxidative stress wear down the mitochondria and cause a dysfunctional state.
Studies have found that individuals with major depressive disorder have an advanced state of mitochondrial dysfunction (28, 29). Abnormal mitochondrial morphology, size, and density have all been reported in the brains of individuals with major depressive disorder and schizophrenia. Research has shown that this is initiated by a profound glutathione (GSH) decrease and a mitochondrial dysfunction (30, 31).
Glutathione Depletion and Nrf2:
In depressive states, the cells are under so much stress that their main protective shield (GSH) gets worn down and oxidative stress damages the mitochondria and the DNA leading to cell death. Poor blood sugar control and high environmental toxin exposure are known to deplete glutathione levels and impair mitochondrial function (32).
A key pathway that maintains cellular glutathione levels and the ability of the cell to adapt to stress is called Keap1-Nrf2. When this pathway breaks down it causes increased levels of oxidative stress within the cell that leads to glutathione depletion and mitochondrial dysfunction (33). This pathway is important to address to prevent or reverse depressive symptoms (34).

Methylation and Depression:
Methylation is a controlled transfer of a methyl group (one carbon and three hydrogen atoms) onto proteins, amino acids, enzymes, and DNA in every cell and tissue of the body to regulate healing, cell energy, genetic expression of DNA, liver detoxification, immunity, and neurology.
Adapting to stress and the challenges of life is an aspect that methylation provides the body. Without adequate methylation processes the individual cannot adapt to stress effectively. Research shows that individuals with depression have altered methylation processes due to genetic polymorphisms (MTHFR, MTRR, and COMT among others) and nutrient deficiencies (35, 36).
Key methylation elements include methylated B vitamins (riboflavin, B6, folate, and B12 in particular), magnesium, selenium, zinc, and various trace minerals. Individuals with depression are often deficient in these key nutrients and need nutritional and supplemental strategies to address these key methylating agents.

Anti-Inflammatory Nutrition:
An anti-inflammatory nutrition plan that is low in carbohydrates and rich in healthy fats and antioxidants is critical to preventing and treating major depressive disorder. The brain is primarily water, fat, and cholesterol. These are all key building blocks for promoting healthy brain function and rebuilding a damaged brain.
The proper diet to beat depression is rich in phytonutrient dense vegetables, healthy fat, and clean protein sources. Healthy fat sources such as coconut, avocados, olive oil & sprouted nuts, and seeds must take a central role in the diet to promote healthy brain function.

Stimulating Neurogenesis:
One of the biggest breakthroughs in neuroscience over the last 20 years has been the discovery of neurogenesis. This refers to the ability of the brain to generate new healthier and stronger cells and synaptic junctions. The brain can literally rewire itself.
In the case of depression, the brain is undergoing extreme damage from inflammation. This is happening much faster than the body can heal which is why it is called a neuroinflammatory disorder (37). Long-term examples of neuroinflammation include dementia, Alzheimer’s, and Parkinson’s disease.
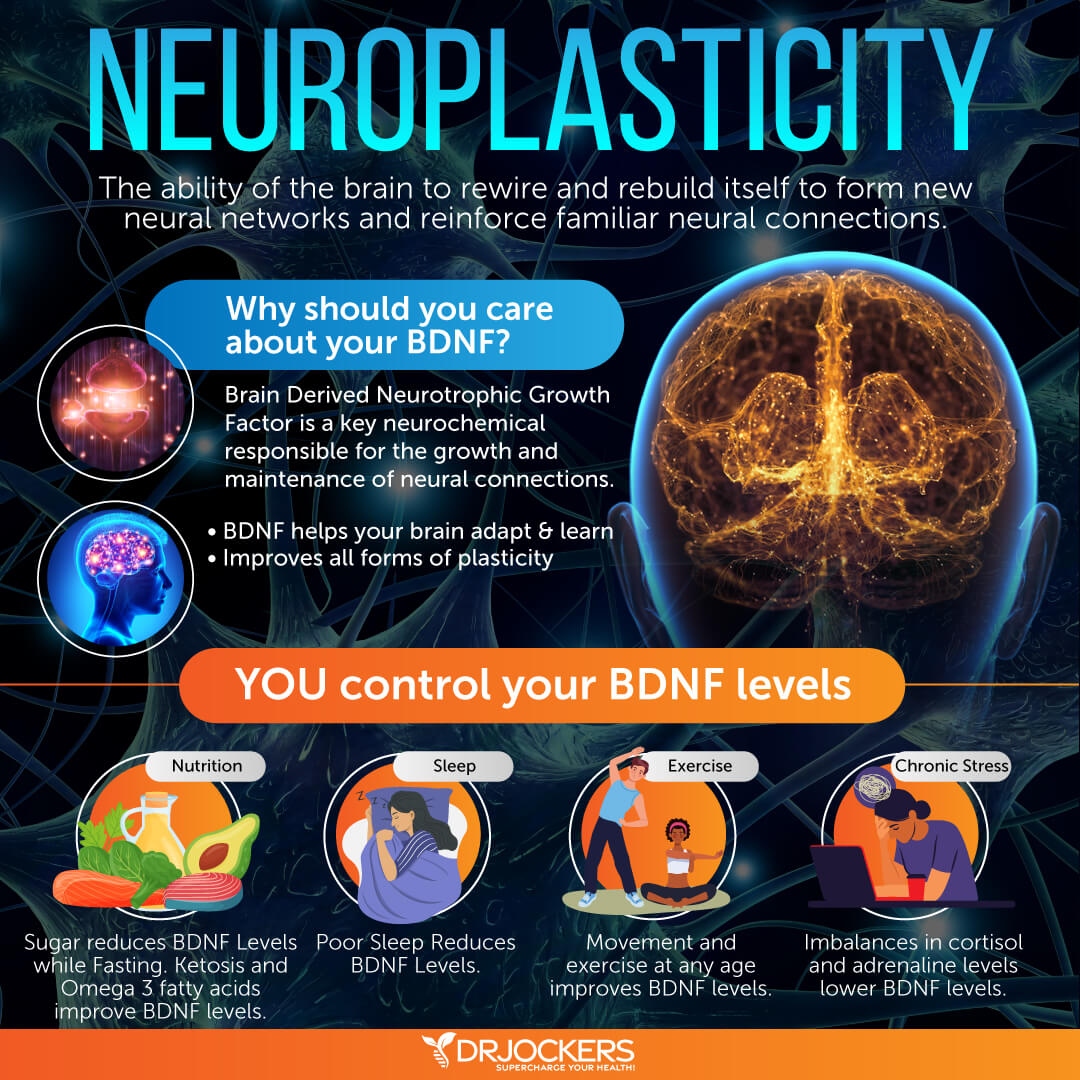
In order to grow stronger and healthier neuronal cells the neurons secrete a compound called Brain derived neurotrophic growth factor (BDNF). BDNF encourages the growth and differentiation of new neurons and synapses. In the brain, it is most active in the hippocampus and cortex and is vital to learning, memory, and higher thinking (38, 39). It also plays an important role in mood and happiness.
Key ways to simulate BDNF include regular exercise, novel movement patterns such as using your non-dominant hand for activities, doing cross-crawl style movements, aromatherapy, learning new concepts, listening to classical music, social interaction, and laughing.
Natural Support Strategies For Mental Health
Here are the best action steps to get started with on your journey to improve your mental health. These strategies are not FDA-approved to prevent, mitigate, treat, or cure depression and should not be confused as such. You should always consult with your physician before stopping or changing medications or taking on new health strategies.
Additionally, you should be working with a functional health practitioner to help guide you through these strategies. This is not an exhaustive list and there are other natural therapeutic strategies that I and functional health practitioners will utilize to help individuals with mood issues.

Anti-Inflammatory Diet & Ketosis
Eating an anti-inflammatory diet rich in nutrient-dense foods is the first best thing you can do to support a positive mood and improve your brain health. First, eliminate all inflammatory foods, including refined sugar, gluten, refined oils, deep-fried and processed foods, conventional dairy, grain-fed meat and eggs, soda and sugary drinks, and foods that you are sensitive to.
Instead, I recommend eating an anti-inflammatory diet and loading up on greens, vegetables, low glycemic index fruits, herbs, spices, healthy fats, grass-fed meat, and wild-caught fish. I also recommend a ketogenic approach for individuals with mental health conditions if they are willing to follow it.
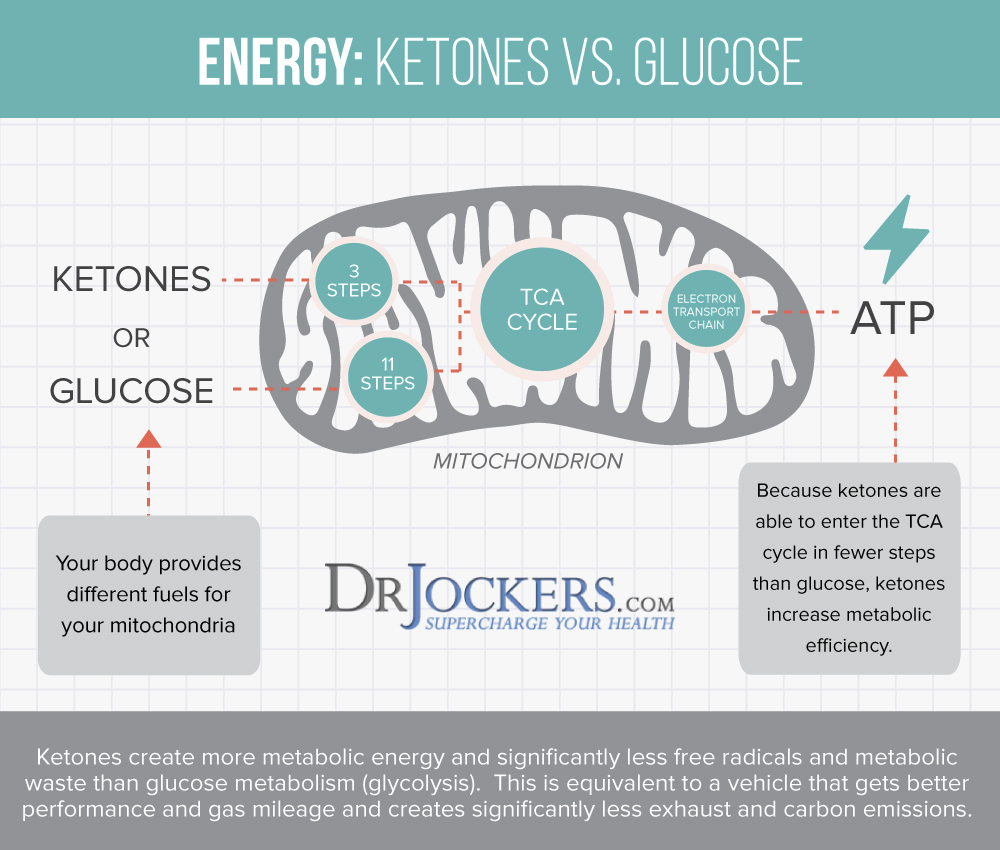
Getting into ketosis will enhance mitochondrial function in the brain. Many people report a huge boost in their mood when following a ketogenic diet. Although a ketogenic diet cannot change emotional trauma, it can help calm and clear your mind to help give you a better chance to do so (40).
Beta-Hydroxybutyrate (BHB), a ketone body that is produced when following a ketogenic diet has demonstrated anti-inflammatory properties in brain tissues. A 2017 study observed in rats that BHB helped to mitigate stress-induced inflammation in the brain and exhibited anti-depressant activity (41). Learn more about following a ketogenic nutrition plan here and avoid exposure to herbicides and pesticides by choosing organic food as much as possible.
Intermittent Fasting:
Intermittent fasting is a form of fasting cycle between not eating (fasting) and eating (feasting) over a period of time. The benefits of intermittent fasting benefits include cellular repair, autophagy, immune regulation, inflammation levels, and insulin sensitivity.
It also helps to improve mental health and brain function. Going 16–18 hours between dinner and breakfast is one of the best ways to improve mitochondrial production. Your body improves energy efficiency by increasing and strengthening the mitochondria during periods of fasting. Consume your meals in a 6-8 hour window such as 11 AM–7 PM or 12–6 PM.
When you do this you enhance cellular healing and brain cell regeneration. Fasting increases the production and utilization of ketones as an energy source which reduces inflammation in the brain. Additionally, fasting increases BDNF which enhances the growth and development of brain cells (42). To learn more about the benefits of intermittent fasting and best intermittent fasting practices, I recommend this article.

Reduce Stress and Focus on Gratitude and Prayer
Reducing stress is critical for reducing inflammation and improving brain health. I recommend that you reduce stressors in your life as much as possible. Turn off the news, and only look at it once a day or a few times a week for a specific period. Reduce your social media use and time on the internet.
Avoid people and situations that bring you down. Surround yourself with loving and uplifting people. Engage in uplifting and relaxation-promoting activities. Read, try some arts and crafts, play cards or board games, sing, and dance.
Depression and emotional exhaustion cannot exist at the moment when your mind is focused on gratitude. Managing your emotional state, mindset, and attitude can help to improve your depression, elevate mental fatigue, and increase your physical energy. Gratitude and prayer may help you with this.
Having regular gratitude, prayer, or spiritual practices are some of the best ways to improve your mood. Begin your morning by counting the blessings in your life and by saying a short prayer. Stop throughout the day to appreciate new and small things. Take time to laugh about something each day!
Keep a gratitude journal and write down at least three things you are grateful for before the end of the day. Try to come up with three new things each day to challenge yourself and to keep your mind in a positive state. Say a prayer before meals or bedtime or whenever you seek connection to a higher power.

Prioritize Good Sleep Habits
While poor sleep is one of the contributing factors of depression, it is also one of the main symptoms. If you are depressed, you may find yourself rolling around in bed at night, experiencing interrupted sleep, and having nightmares or night terrors. You may have trouble going to bed on time or falling asleep, yet, you may wake up feeling exhausted and want to stay in bed all day.
Prioritizing good sleeping habits and supporting your natural circadian rhythms is critical for mental health. Make sure that you have a comfortable bed, bedding, and pillows. Create a safe sanctuary in your bedroom. Develop a regular relaxing nighttime routine that works for you.
Turn off electronics and avoid sugar or caffeine close to bedtime. Engage in relaxing activities. Sip on herbal tea and light a candle. Try prayer, meditation, journalism, reading, board games, crossword puzzles, and coloring at night. Do a quick stretch, check in with your body and emotions, say your intentions, be grateful, and take time for a short prayer.

Move Your Body
I know, if you are dealing with the symptoms of depression, getting out of bed can be difficult as can going to the gym. But trust me. Moving your body regularly is one of the regularly recommended and scientifically proven ways to improve your mood and any form of depression.
Moving your body helps to release happy chemicals, including endorphins that may help to ease sadness or brain fog. Research suggests that even 10 minutes on the treadmill or 30 minutes of walking may result in significant and lasting benefits (43).
Don’t worry, it’s okay to start out slow. Research suggests that consistency and frequency are much more important than duration or intensity when it comes to the benefits of exercise to combat depression. Start out with light walks, practice yoga, dance to your favorite song, or join a group fitness class to start out.
As you get into it, you can start developing a regular routine combining cardiovascular, resistance, and strength training. No matter what, stay consistent and move your body 20 to 30 minutes each day. Start and finish your day with a short, few-minute stretch or yoga routine.

Get Daily Sun Exposure
Higher levels of sun exposure are associated with improved mood and lower rates of depression. This is due to the fact that sun exposure stimulates vitamin D, improves mitochondrial health, and stimulates feel good neurotransmitters like serotonin and endorphins as well as the brain enhancing compound BDNF (44, 45).
Depending on where you live, this may be tricky during some months. However, I recommend that if possible, obtain some exposure to the sun. Remember, the sun may be peeking through the clouds even if it’s hard to notice.
I recommend that you keep your curtains and blinds open during the day and at night, so you get a bit of sunshine peeking through whenever possible. If there is a ray of sunlight outside, get outside for a short time even if it’s cold outside. Bundle up and embrace the season. You may combine this with a morning stroll or outdoor exercise routine.
However, since sun exposure is not possible every day when you live in colder parts of the world, I recommend regular red-light therapy to receive similar benefits while indoors.

Ground Your Body:
In our society, we are surrounded by toxic electromagnetic frequencies (EMF’s). These EMF’s increase stress within our body and alter neurotransmitter function (46).
By going outside daily and walking barefoot on grass, dirt, or sand you absorb natural EMFs from the ground that balance your electrical rhythms. Follow the steps in this article here.

Include Magnesium & B Vitamin Rich Foods:
Magnesium helps to improve blood sugar signaling patterns and protects the blood-brain barrier. The best magnesium and B vitamin rich foods include dark green leafy veggies, avocados, grass-fed animal products, raw cacao, and pumpkin seeds.
You can also do Epsom salt baths to support your magnesium levels. It would also be wise to supplement with a good magnesium and B complex supplement. Look for magnesium L-threonate which is the best form of magnesium for crossing the blood-brain barrier.
When it comes to B vitamins, it is best to look for one with pre-activated forms such as methyl-folate, methyl-cobalamin (B12), Pyridoxal-5-Phosphate form of B6, and Riboflavin-5-phosphate form of vitamin B2. The methyl groups are in the active form and will be better utilized by the body.

Reduce Toxin Exposure
Reducing your toxic exposure is critical for protecting your health from leaky brain. Buy organic food as much as possible. Stop using conventional beauty, body, and household products, and replace them with organic, natural, or homemade alternatives.
Use glass, stainless steel, wood, and bamboo products instead of plastic. Spend time in nature and breathe in the fresh air. Use a good indoor air filtration system. Make sure that you drink clean, toxin-free water by using a high-quality reverse osmosis system. Add a slice of lime for some extra flavor.

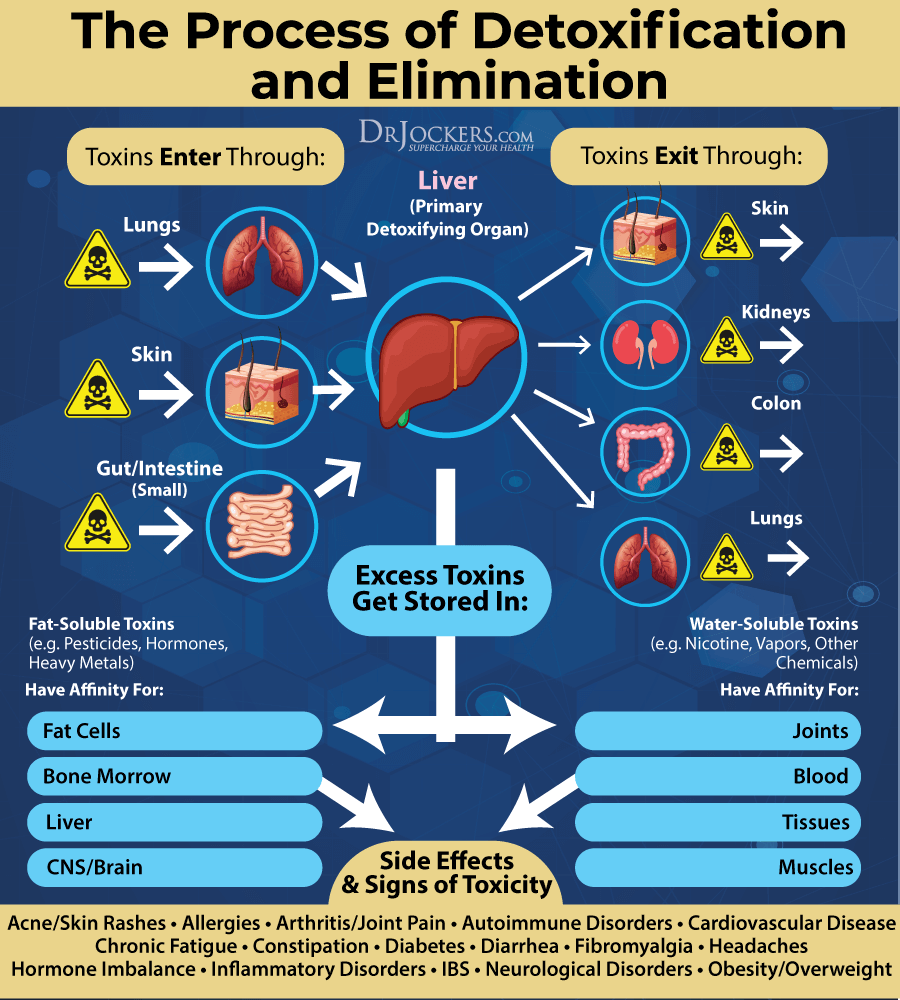
Support Detoxification Pathways
It is not enough to put good things into your body, you have to make sure that the bad things come out as well. Drink plenty of water to support detoxification through sweating and urine. Support your detoxification pathways to protect your body from brain inflammation.
I recommend using infrared saunas to promote detoxification through sweating. Try rebounding and dry skin brushing to support your lymphatic pathways. Support two major detoxifying organs, your kidneys and liver with herbs like milk thistle, parsley, dandelion, and bioactive carbons which can penetrate and remove toxins from deep within the tissues and cells.
Supplement with Vitamin D
One of the main benefits of getting out into the sun is a natural boost of vitamin D. No wonder that vitamin D is also called the sunshine vitamin. Vitamin D is an important vitamin that is critical for many areas of your health, including your immune function, bones, muscles, and mental health.
Vitamin D has been linked to depression and mood disorders. People with depression often have low levels of vitamin D and supplementation may help. Research has found that vitamin D may be an important treatment method for mental health disorders (47).
Since obtaining enough sunshine while spending a lot of time indoors during the colder months is difficult, supplementing with vitamin D is critical. In fact, vitamin D is one of those vitamins that everyone may benefit from. I recommend taking a daily vitamin D3 supplement with vitamin K2. Vitamin K2 optimizes the absorption of D3 and further enhances your health.

Find Ways to Laugh Daily
Did you know that children laugh 300 to 400 times a day, while adults only laugh 17.5 times on average? I notice this in my children when they burst out laughing all the time and get excited about the small things. Everything is funny and exciting in their world. It is a joy to watch.
Adults tend to be more serious and full of worries. Yet, laughing has incredible health benefits. It may improve your immune system, hormones, mood, and pain levels, work your muscles, and make you happier. It increases endorphins in your body and may reduce depressive symptoms.
Make sure to laugh more during the day. Be a kid again for a moment. Get silly and laugh with your kids or pets. Watch a funny movie. Read a comic book. Look up some jokes. Attend a comedy show.
Laugh at yourself in a positive way and laugh with others. Laugh for no reason. Try laughter yoga to create more laughter in your life without more reason. Read about the benefits of laughter here and start your own laughter-positivity challenge.

Consider Using Omega-3 Fatty Acids
Inflammation is one of the common culprits behind mood disorders. Omega-3 fatty acids are healthy fats with anti-inflammatory benefits. Research has found an association between omega-3 fatty acids (alpha-linolenic, eicosapentaenoic, docosahexaenoic) and depression and found that supplementation may improve symptoms. Increasing your intake of omega-3 fatty acids may reduce your risk and improve your mood (48).
Foods that are rich in omega-3 fatty acids include salmon, cod liver oil, herring, sardines, anchovies, mackerel, other fish and seafood, algae, pasture-raised eggs, grass-fed butter, hemp seeds, chia seeds, and flax seeds. However, if your health is compromised, meeting your omega-3 needs may be difficult via diet alone, and you may benefit from supplementation.
Plant-based omega 3’s such as flax oil only contain the small chain omega 3 called ALA and do not have any DHA. It is very hard for our body to convert ALA into DHA so it is best to get a high-quality fish or krill oil that is rich in EPA and DHA. You want to find a brand that is molecularly distilled to take out any heavy metals and other unwanted contaminants.

Improve Your Mitochondria:
The mitochondria are the energy powerhouses of every cell. The brain is the densest area of mitochondria with over 10,000 mitochondria per neuron as opposed to 1,000 mitochondria in each muscle cell. When someone has a chronic mood or mental health disorder, some experts believe it is a clinical sign that they have dysfunctional activity going on in the mitochondria.
Support your mitochondria with clinical doses of CoQ10, L-carnitine, N-acetyl cysteine, creatine monohydrate, B vitamins, magnesium, alpha lipoic acid, and D-ribose. You can find mitochondrial support supplements that have most if not all of these key nutrients.

Support Gut Health
Your brain and gut are closely connected and supporting your gut is important for preventing and reducing brain inflammation. Make sure gut-friendly, anti-inflammatory, and nutrient-dense diet abundant in veggies, healthy fats, clean protein, and probiotic-rich foods, such as sauerkraut, kimchi, and kefir.
Additionally, I recommend taking a daily probiotic supplement. Probiotics help to optimize your gut health and improve your nutrient absorption while reducing gut related inflammation. When gut inflammation goes down it also reduces inflammatory mediators in the brain and improves depressive symptoms (49).

Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!
Final Thoughts on Depression
Depression is a common and growing mental health condition that is characterized by sadness, low energy, fatigue, and trouble sleeping. The strategies I discussed in this article are not FDA-approved to prevent, treat, mitigate, or cure depression but they have been helpful for many individuals looking to improve their mental health.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website health coaching team offers long-distance functional health coaching programs. For further support with your brain health and other health goals, just reach out and our fantastic coaches are here to support your journey.




Thank you for this very informative and revealing article, Dr. Jockers. I’m wondering how adopting these suggestions would affect someone who is already taking anti-deps and has been doing so for many many years? Still gain to benefit? Or what other suggestions might you have for someone who is currently taking them (Wellbutrin and Zoloft)? And finally, does your clinic work with people with such conditions who want to heal from it and gradually wean off the pharmaceuticals?
Hey Oscar, yes you can still see benefits! We do not make medication suggestions so you will need to work with a doctor to reduce dosages and monitor side effects!
Thank you! When you say doctor, are you referring to a psychiatrist? (This is not for me, but I would be relaying the information to her)
Whoever was in charge of prescribing those medications in the first place Oscar!
This is a great article with all the scientific facts to support it. Thanks for sharing this.
Thank you Nina! Blessings to you and your family!