 Insulin Resistance: 10 Ways To Stabilize Blood Sugar
Insulin Resistance: 10 Ways To Stabilize Blood Sugar
Insulin resistance is an increasingly common problem people are facing today. Insulin helps your cells to absorb and use glucose for energy. Insulin resistance happens if your body is unable to respond to and use the insulin produced by your body. Insulin resistance can lead to prediabetes, diabetes, and an array of other health issues.
An increasing number of people are suffering from diabetes every day. It is estimated that the number of people with diabetes will double during the next 25 years. The numbers will go from about 190 million to 325 million unless we do something about it.
The good news is that it’s possible to prevent diabetes and stabilize your blood sugar naturally through dietary and lifestyle changes. The first step to prevent and reverse prediabetes and diabetes is to reverse insulin resistance, improve insulin sensitivity, and stabilize your blood sugar (1).
In this article, you will learn the role of insulin in your body, what insulin resistance is, what causes insulin resistance, what are its symptoms, and how it is diagnosed. You will learn what prediabetes is, which varying forms of diabetes commonly exist, and how they may affect your body. You will also learn 10 ways to stabilize your blood sugar naturally through simple dietary and lifestyle strategies, as well as via supplementation.

The Role of Insulin in the Body
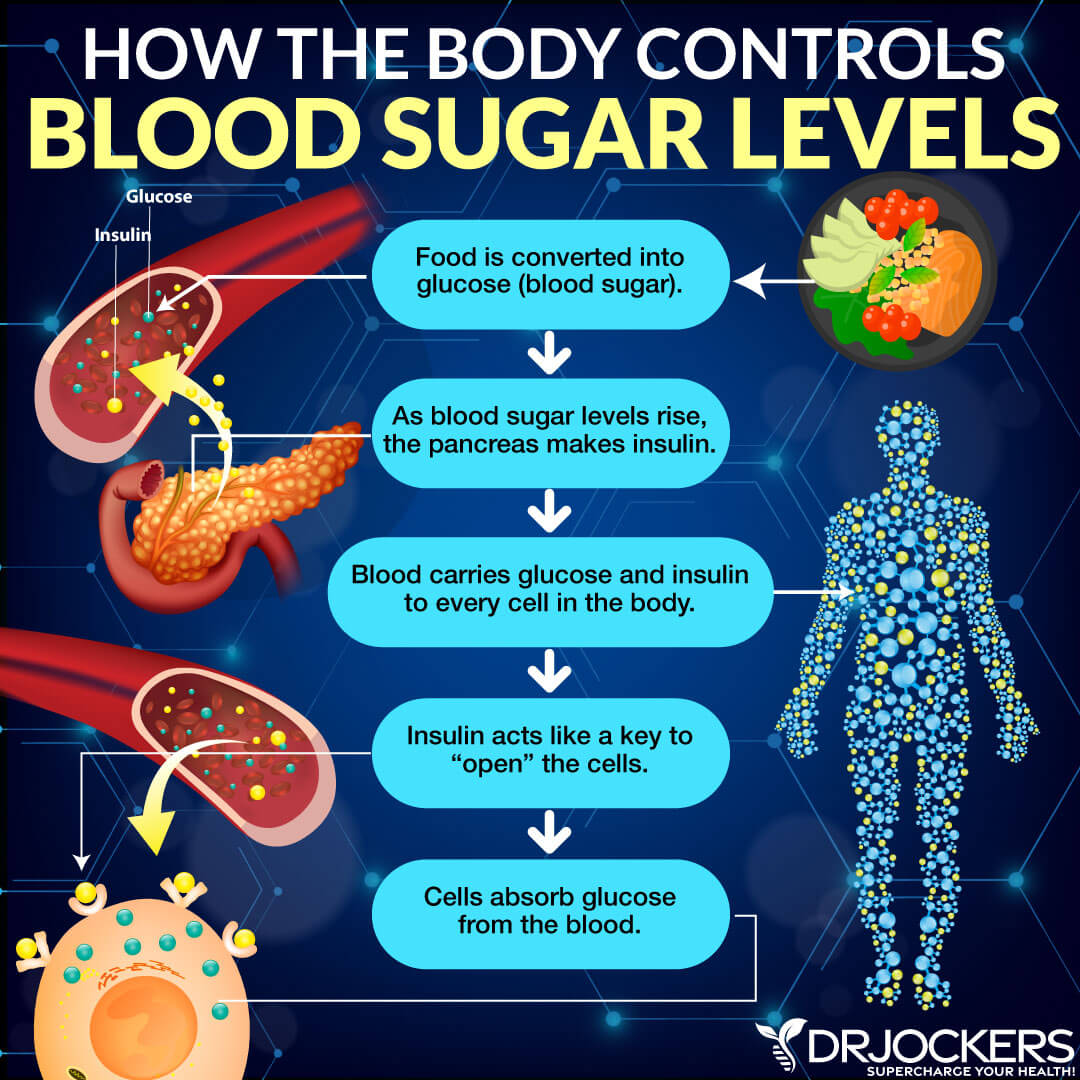
Insulin is a very important hormone in your body. It is made by your pancreas. Insulin allows cells to absorb and use glucose. It also assists the glucose in your blood to enter the cells in your muscles, fat, and liver and to be used for energy.
Your body gets glucose from the food that you eat. In times of need, such as fasting or famine, the liver can also make glucose.
As you eat, your blood glucose, also known as blood sugar, levels increase. Your pancreas releases insulin into your blood to help lower your blood glucose levels and to keep the levels at a balanced, normal range (2).
What is Insulin Resistance?
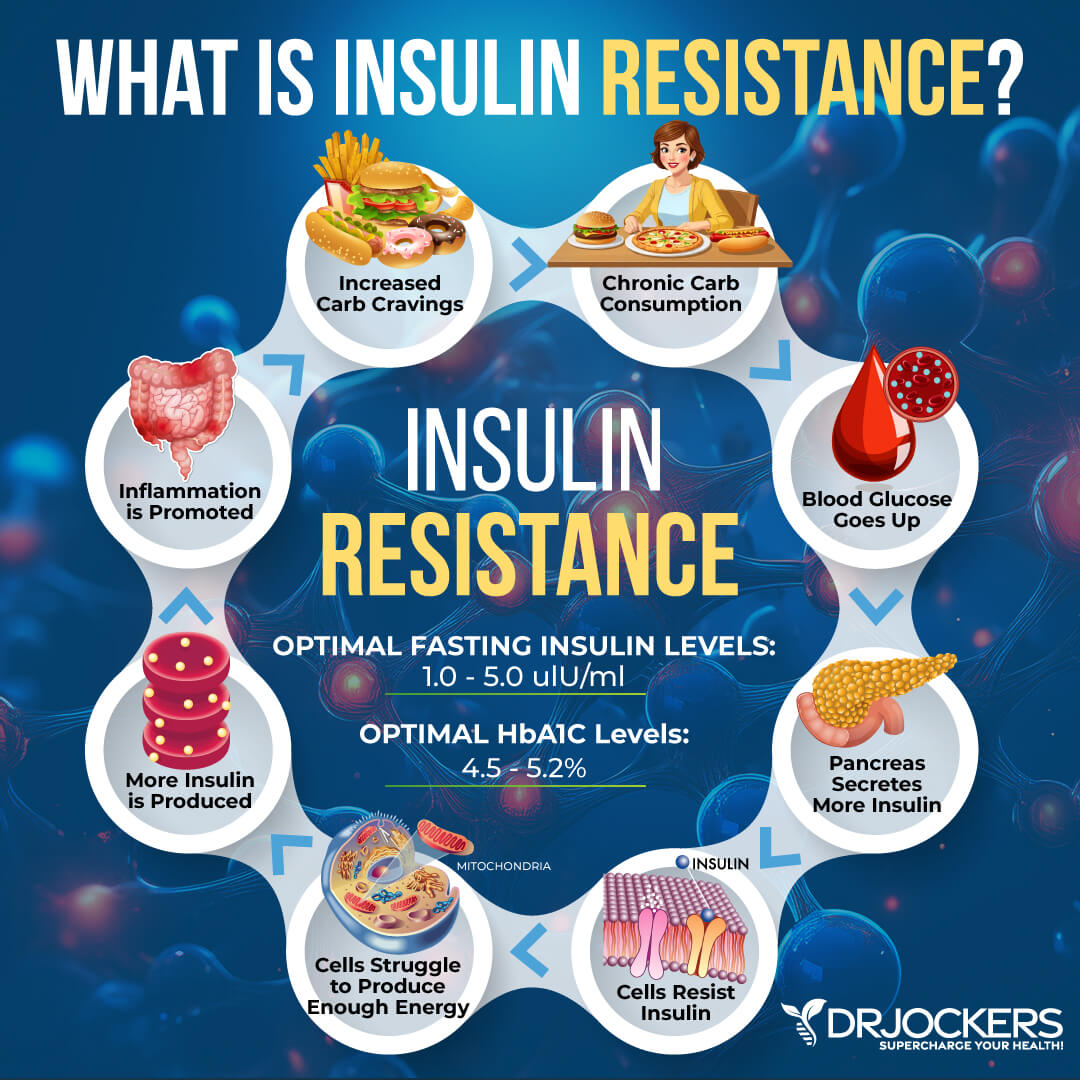
You have insulin resistance if your body is unable to respond to and use the insulin that your body produces. Your muscles, fat, and liver can’t respond appropriately to the insulin and are unable to easily absorb glucose from your blood. As a result, your pancreas ends up producing an increased amount of insulin to assist glucose to enter your cells. By trying to make enough insulin to overcome your body’s weak response to insulin, your body is aiming to keep your blood glucose levels at a healthy range (2).
However, the beta cells in your pancreas may not be able to keep up with the excessively high insulin demand. As a result, excess glucose builds up in your bloodstream. This may lead to more serious health issues including prediabetes and type 2 diabetes. Insulin resistance can exist without symptoms for years, and some symptoms may be confused with other health issues. Some people may go for years without knowing they have insulin resistance (2).
Maintaining balanced insulin levels at a normal range is important for your overall health and well-being. Problems are presented when insulin levels are too high or too low. If you have too much insulin, the excess gets deposited in your blood. If you have too low insulin levels, your liver continues to make glucose, thereby overtaxing your liver and other organs.
The Problem with Too Much Insulin
Low insulin levels are common for people with type I diabetes, whereas high insulin levels are a sign of insulin resistance, prediabetes, and type 2 diabetes. Insulin resistance increases your risk of prediabetes which is a precursor of type 2 diabetes (2).
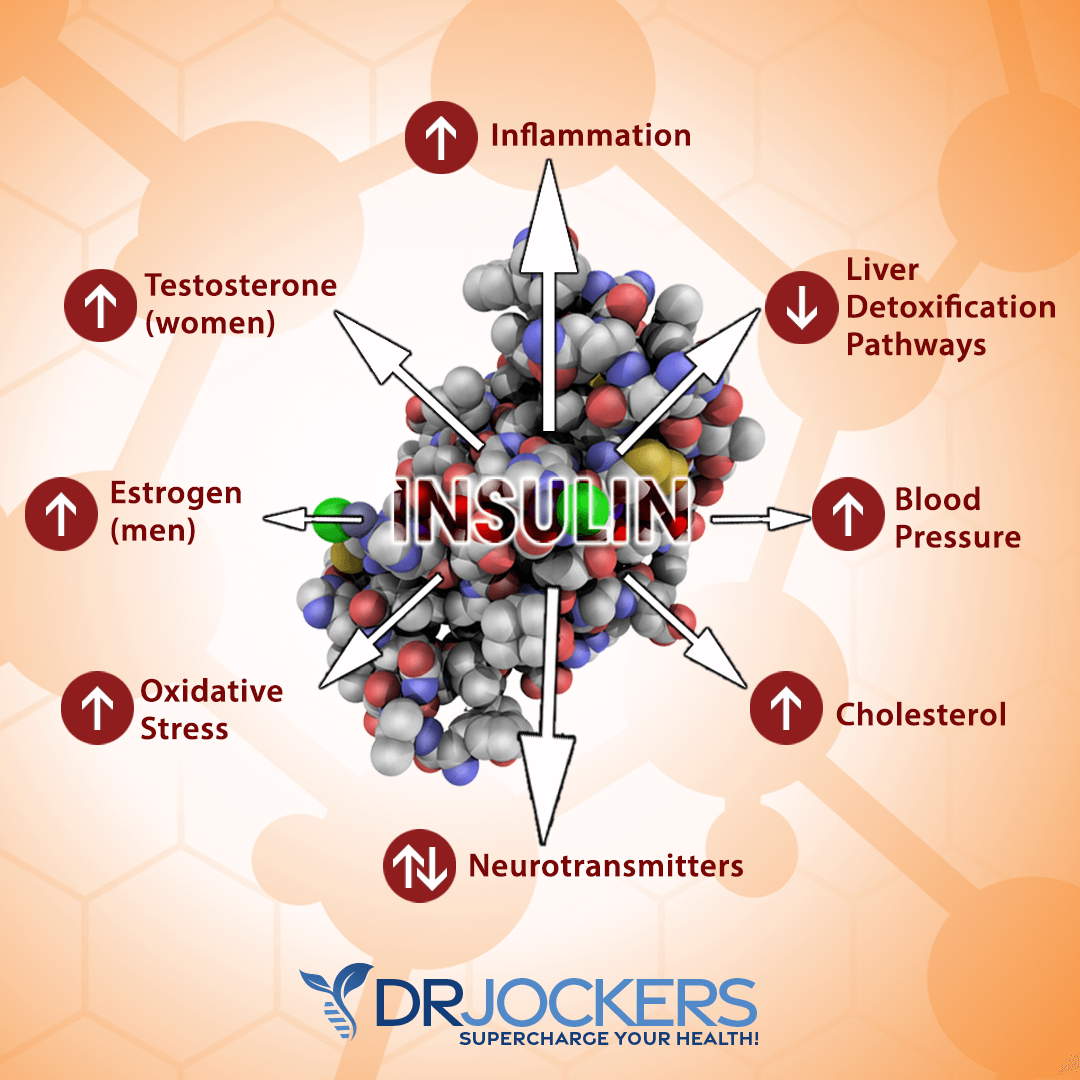
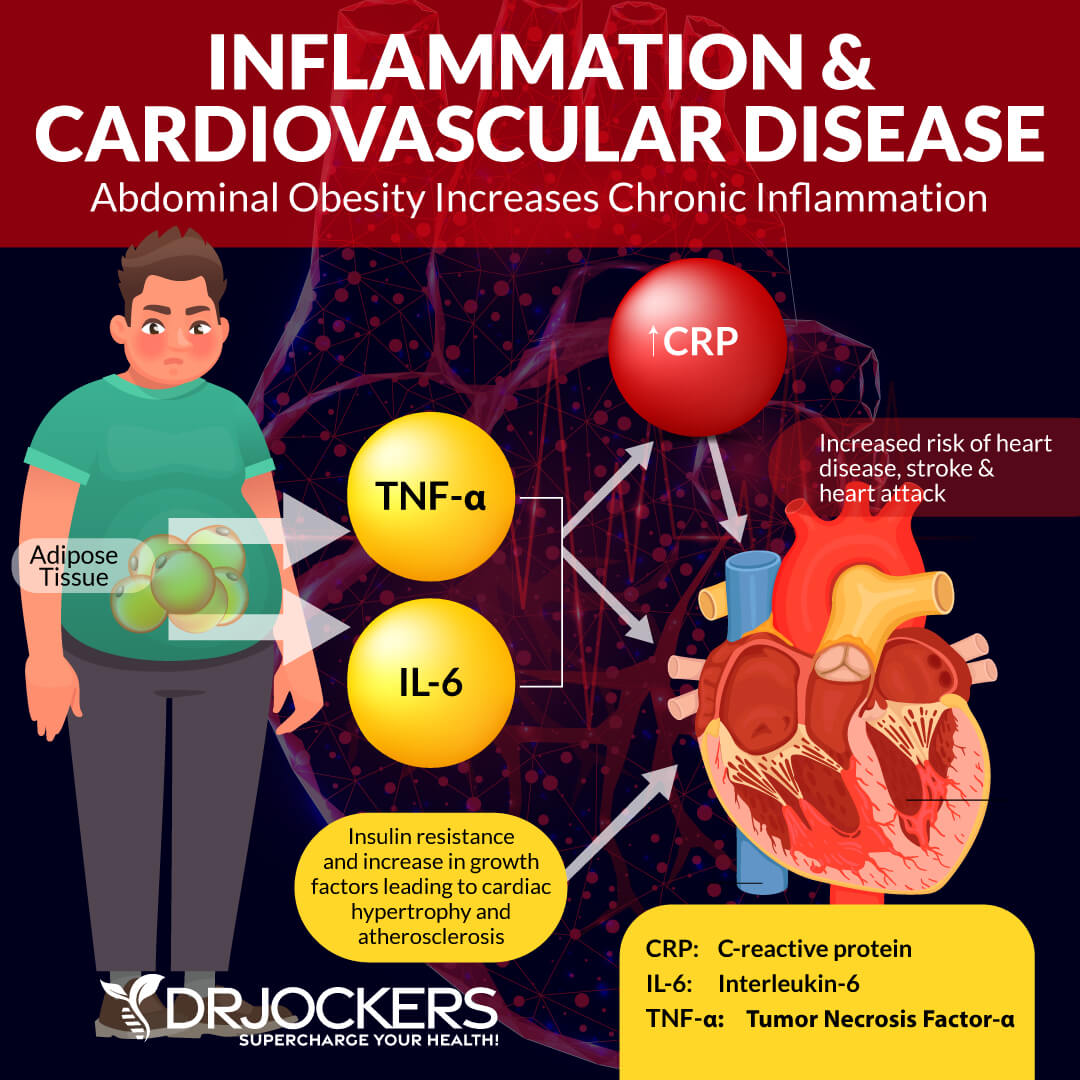
Too much insulin in your body promotes inflammation and weight gain. Chronic inflammation is the root cause of most diseases and chronic pain symptoms that people in our modern society are suffering from. Insulin resistance has been linked to obesity, high levels of fat in the blood, and hypertension.
It can increase the risk of heart disease and cognitive decline. If you have insulin resistance, your pancreas tries to produce more insulin to create balance. But eventually, it becomes too much for your pancreas and it wears out. When your pancreas cannot make enough insulin anymore to achieve healthy blood glucose levels, your body develops high blood glucose levels, prediabetes, and without appropriate dietary and lifestyle changes, eventually, type 2 diabetes (3, 4, 5).
Insulin Sensitivity
When we talk about insulin resistance, it is important to mention insulin sensitivity as well. Insulin sensitivity and insulin resistance are basically two sides of the same coin.
If you are insulin sensitive, your body requires less insulin to bring down your blood glucose levels when necessary. If you are insulin resistant, your body needs an increasing amount of insulin to create balance. If you have insulin sensitivity, you have low insulin resistance. On the other hand, if you have insulin resistance, you have low insulin sensitivity.
Being insulin resistant is dangerous to your health. However, being insulin sensitive is a good thing. Insulin sensitivity can lower inflammation, aid fat loss, lower sugar crashes, reduce the risk of disease, and lower the risk of cognitive decline.
Causes of Insulin Resistance
The exact causes of insulin resistance are not yet fully understood, however, there are some well-known factors that can lead to developing insulin resistance.
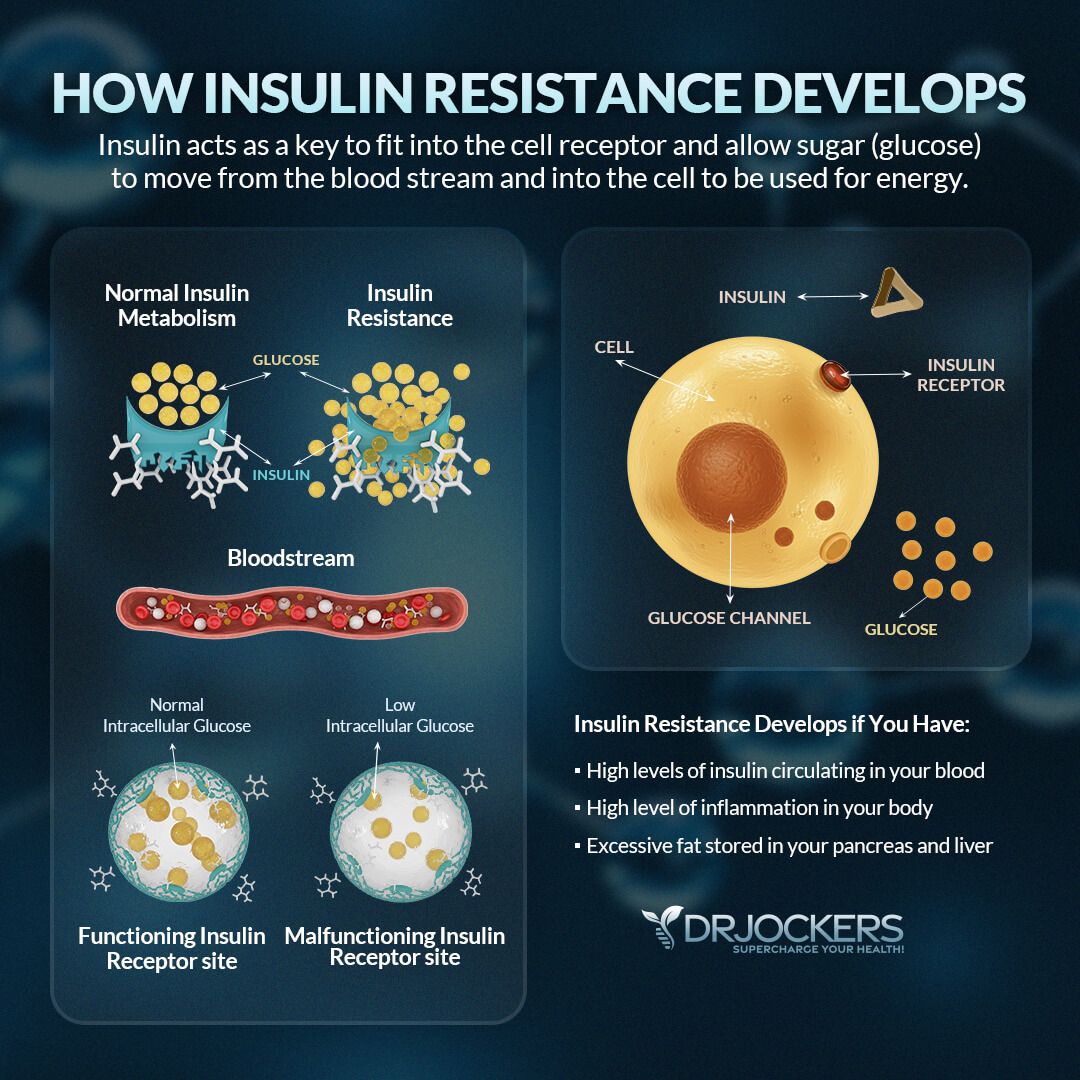
Insulin resistance develops if you have:
- High levels of insulin circulating in your blood
- High level of inflammation in your body
- Excessive fat stored in your pancreas and liver
Factors that may increase the risk of insulin resistance include (6):
- Being overweight or obese
- A high-sugar, high-carbohydrate, or high-calorie diet
- Sedentary lifestyle
- Chronic stress
- Smoking
- High blood pressure
- Sleep issues
- Using high doses of steroids for an extended period
- Polycystic ovary disease or Cushing’s disease

Symptoms Associated with Insulin Resistance
According to the Centers for Disease Control and Prevention (CDC), up to 90 percent of people with prediabetes don’t know they have insulin resistance. Therefore, it is particularly important to know the symptoms and signs associated with insulin resistance and visit your doctor if you notice any symptoms (6, 7).
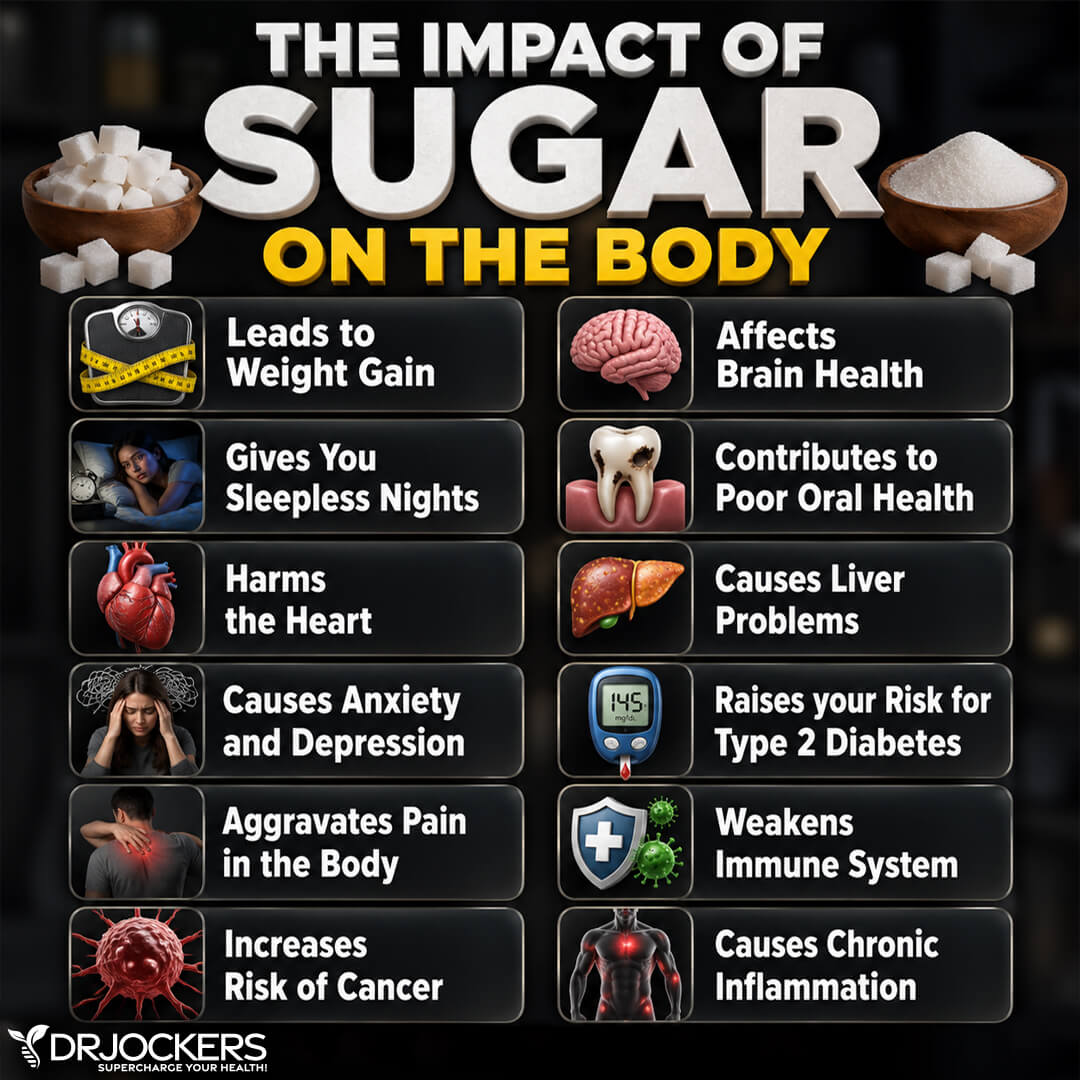
Symptoms associated with insulin resistance include (7, 8):
- Fatigue
- Lethargy
- Increased hunger
- Brain fog and difficulty concentrating
- Weight gain, especially around your mid-section
- High blood pressure
- High cholesterol levels
- Dark skin patches called acanthosis nigricans
Diagnosing Insulin Resistance
Doctors normally don’t test for insulin resistance, however, they use various blood tests to determine if someone has prediabetes or diabetes, including:
- HbA1C test
- Fasting plasma glucose (FPG)
- Oral glucose tolerance test (OGTT)
- Random glucose test
Most commonly, doctors order the FPG test or the A1C test to check for prediabetes. Though it is less common, some doctors may use the OGTT. The OGTT is more difficult to administer and it is also more expensive.
The FPG and the OGTT both reflect your blood glucose levels at the time of the test, whereas the A1C looks at average blood glucose levels over the 3 months before the test. The A1C test is less sensitive than the FPG and OGTT. Since it may miss prediabetes, it may be beneficial to get both the A1C test and the OGTT.

Hemoglobin A1C (HbA1C)
The HbA1C test measures the average plasma glucose concentration of a specific form of hemoglobin (Hb) or red blood cell over a period of 3 months. When Hb is exposed to plasma glucose, a glycation reaction happens. As your blood sugar increases, your glycated Hb increases as well (9, 10, 11).
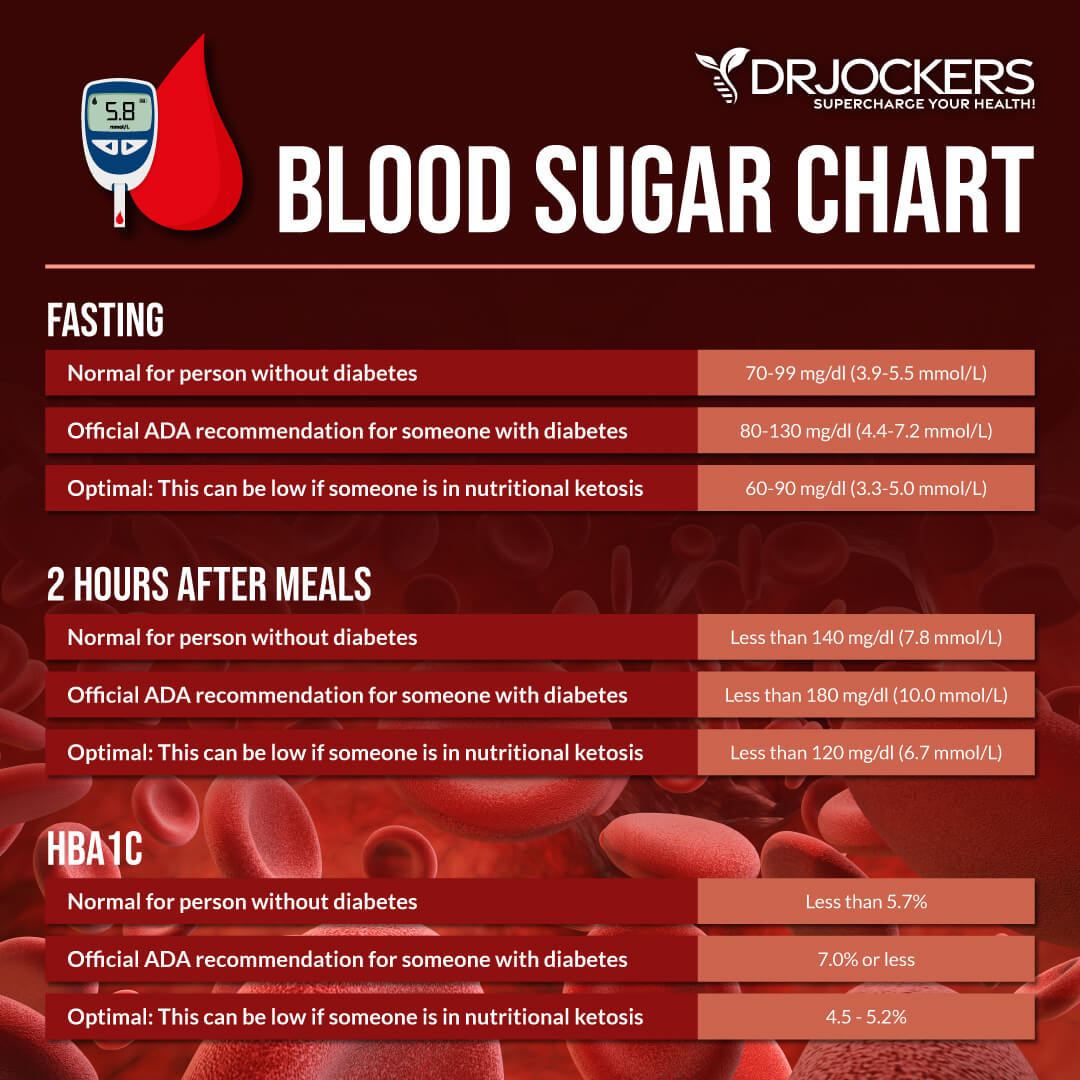
- Normal HbA1C: Healthy levels of HbA1C are under 5.6 percent. Most functional and holistic medicine doctors prefer to see them under 5.4 percent in order to stay on the safe and healthy side.
- Prediabetes: Between 5.7 and 6.5 percent is when prediabetes is diagnosed.
- Diabetes: Over 6.5 percent is when diabetes is diagnosed.
Fasting Plasma Glucose Test (FPG)
The FPG test measures your fasting morning blood sugar levels after at least 8 hours of avoiding any food or drink. Doctors advise skipping breakfast before the mid-morning blood test is performed. (9, 10, 11).
- Normal FPG: Under 100 mg/dl is considered normal, though functional and holistic medicine doctors prefer to see this number under 90 mg/dl.
- Prediabetes: Between 100 and 126 mg/dl, is considered prediabetic.
- Diabetes: Over 126 mg/dl, diabetes is diagnosed.
Oral Glucose Tolerance Test (OGTT)
The OGTT measures your response to a glucose load. This test uses blood samples taken up to four times at various points after eating sugar to measure blood glucose levels. Fasting is required similarly to the FPG test. After fasting, you are given a measured dose of glucose (75 grams for adults) to consume within 5 minutes. Your blood glucose is measured immediately after drinking the glucose mix, as well as, two hours afterward. Some doctors take one or two more measurements (9, 10, 11).
The OGTT can identify problems even before your fasting blood glucose levels become abnormal. The OGTT is also a fantastic tool to diagnose gestational diabetes, which can develop during pregnancy.
- Normal OGTT: Normal levels are considered to be under 140 mg/dl, though functional and holistic medicine doctors prefer to see numbers under 120 mg/dl.
- Prediabetes: A range from 140 to 200 mg/dl is considered prediabetic.
- Diabetes: Anything over 200 mg/dl is considered diabetes.
Random Glucose Test
This test measures your blood glucose levels at any point during the day. It is often used as a follow-up after diagnosis or when you have severe diabetes symptoms. Alarming results may also require further testing for appropriate diagnosis (9, 10, 11).
- Normal results: Normal results depend on when you ate last. However, most of the time they will be under 125 mg/dl.
- Diabetes: Regardless of what and when you ate last, a random blood sugar level over 200 mg/dl suggests diabetes.

Prediabetes
Insulin resistance can increase your risk of prediabetes. Prediabetes is a condition when your blood sugar level is higher than normal but not high enough to receive the diagnosis of type 2 diabetes. However, prediabetes increases your risk of type 2 diabetes. Moreover, prediabetes may already be contributing to some of the long-term damage caused by diabetes, including problems with your blood vessels, heart, and kidneys.
Just like insulin resistance, prediabetes often goes without symptoms. Fatigue, weight gain, brain fog, increased hunger, and darkened skin may suggest prediabetes. Once you experience classic signs, such as increased thirst, frequent urination, and blurred vision, you may already have diabetes. Therefore it is important to get your blood sugar regularly tested by your doctor and to make appropriate lifestyle choices to prevent prediabetes and diabetes.
The good news is that if you have prediabetes, it doesn’t mean that you are automatically going to develop type 2 diabetes. Type 2 diabetes is preventable. By eating the right foods, moving your body, maintaining a healthy weight, and following other simple lifestyle strategies which I will share with you soon, you can prevent diabetes, reverse prediabetes and insulin resistance, and stabilize your blood sugar (12).

Diabetes: Type I, Type II, and Type IIb Diabetes
Diabetes is a condition that happens when your blood glucose is too high. Blood glucose is normally the main source of energy, and insulin is the hormone that helps the glucose to make it into your cells. Depending on the type of diabetes, your body is either not making enough or any insulin or it is unable to use it well.
Having too much glucose in your blood, however, can lead to a variety of health problems, including heart disease, stroke, dental problems, kidney disease, foot problems, nerve damage, and eye problems (13). There are several forms of diabetes. Let’s look at them one by one.
Type I Diabetes
The majority of people around the world have type II diabetes, however, about 5 percent of people with type I diabetes is already a significant portion of the population. About 1.25 million people in the US have type I diabetes and there are 40,000 new cases diagnosed yearly.
Though type I diabetes used to be called juvenile diabetes, it is not a childhood disease and can occur at any age and in people of every race, gender, shape, and size.
Type I diabetes is an autoimmune condition. If you have type I diabetes, it means that your body doesn’t produce insulin. Without insulin, your body cannot help glucose to make it into your cells from the bloodstream. Insulin therapy and other treatments can help people to manage type I diabetes and to live a healthy life (14).
Type II Diabetes
Type II diabetes is believed to be a metabolic condition. It usually develops due to dietary and lifestyle habits. It is the most common form of diabetes.
If you have type II diabetes, it means that your body cannot use insulin properly. At first, your pancreas will try to make up for the extra insulin, but once your pancreas cannot keep up, it leads to high blood sugar. This first leads to insulin resistance, then pre-diabetes, and if not prevented through lifestyle choices, type II diabetes.
At first, a doctor may prescribe lifestyle changes to their patients, however, in most cases, eventually, people with type II diabetes end up taking medication, usually for life. However, with proper lifestyle strategies, you can reverse type II diabetes. In this article, you can find some simple tips to beat diabetes naturally (15).

Type IIb Diabetes
Research suggests that type II diabetes may not be as simple and straightforward as has been previously believed. It seems that besides the well-studied form of type II diabetes with poor insulin action, there is another, grossly understudied type of diabetes characterized by poor insulin secretion called Type IIb Diabetes (16).
Autoimmunity and Type II Diabetes
Type II diabetes has been considered a metabolic disorder instead of an autoimmune condition. However, recent research suggests that insulin resistance in type 2 diabetes is the result of B cells and other immune cells attacking your body’s tissues.
The study suggests that people with type II diabetes may have cells that mistakenly attack healthy tissue. While more research is needed, it seems that type II diabetes may also be an autoimmune condition or is linked to autoimmunity. These new discoveries are urging researchers to look for new preventive measures and treatment options looking at type 2 diabetes as an autoimmune condition (17, 18).
Gestational Diabetes
Gestational diabetes is a form of diabetes that may develop during pregnancy. In most cases, it goes away after the baby is born. However, those who have or have had gestational diabetes may have a greater chance of type II diabetes later on (19).
Other Forms of Diabetes
Two much more rare types of diabetes include cystic fibrosis-related diabetes and an inherited form of diabetes, called monogenic diabetes (19).
Alzheimer’s Disease: Type III Diabetes
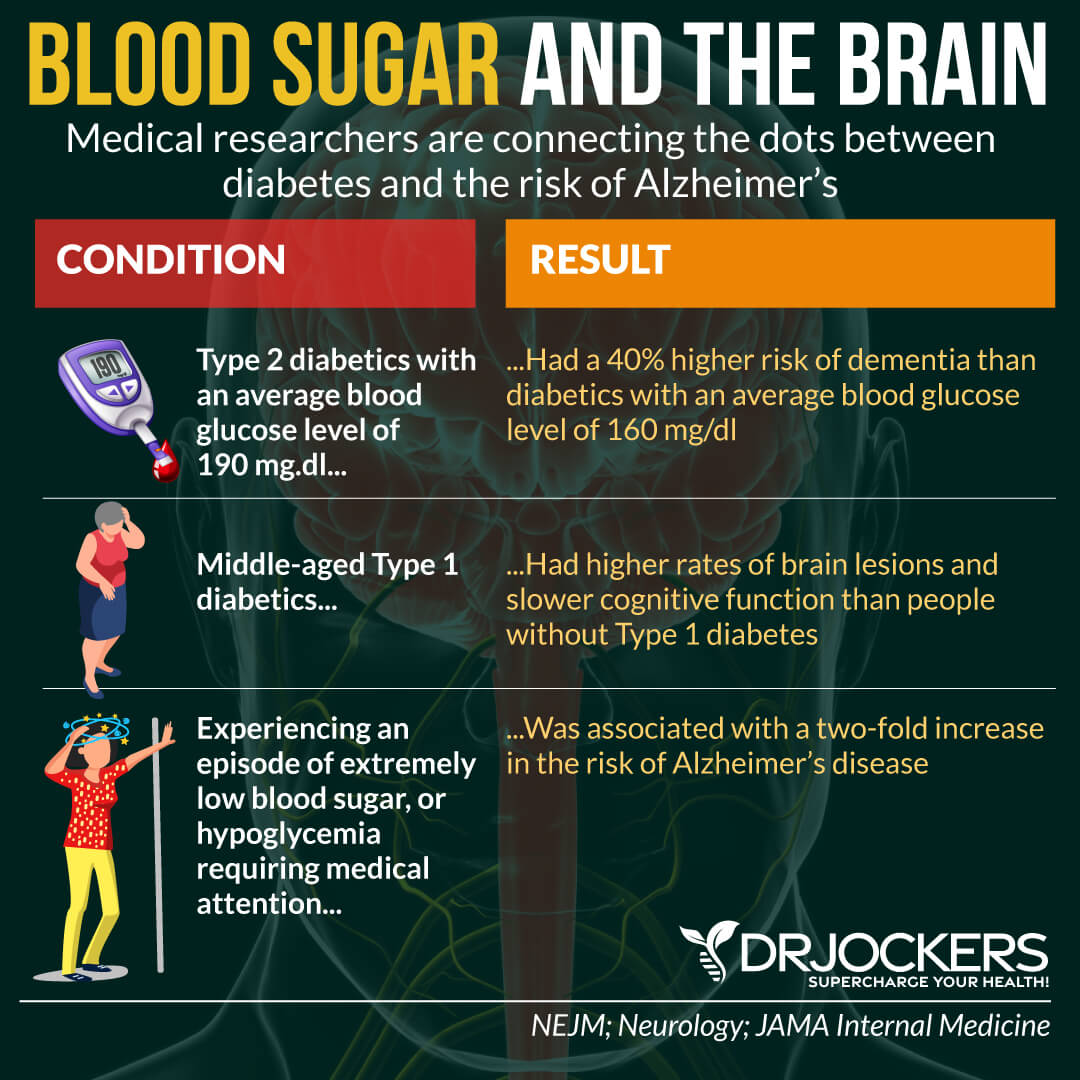
It’s been known in the medical and scientific community that type II diabetes can increase your risk of Alzheimer’s disease. However, there are recent developments regarding a new form of diabetes, type III diabetes which is directly linked to Alzheimer’s. An increasing number of researchers now call Alzheimer’s disease type III diabetes. Research has shown that insulin resistance is one of the main reasons behind memory loss and dementia which can lead to Alzheimer’s disease (4).
However, cognitive decline takes a long time to develop, and diabetes doesn’t happen overnight either. The good news is that through appropriate dietary and lifestyle choices, diabetes and cognitive decline can both be prevented (4, 20, 21, 22, 23).
10 Ways to Improve Insulin Sensitivity
Insulin resistance is not an issue that you should take lightly. It can lead to prediabetes, diabetes, and serious health consequences, including heart, kidney, and cognitive problems.
However, through simple dietary and lifestyle changes, you can reverse insulin resistance and improve insulin sensitivity naturally. Here are 10 powerful ways to stabilize your blood sugar and insulin. It is important to remember that these strategies have not been evaluated or approved by the FDA to prevent, mitigate, treat, or cure diabetes or any other major health condition.

1. Anti-Inflammatory Ketogenic Diet
Inflammation is your body’s way of protecting you from harm, such as injuries, illness, and infection. However, when inflammation turns chronic due to an unhealthy diet, stress, unhealthy lifestyle, and environmental toxins, it can be very harmful to your body.
Chronic inflammation is the underlying cause of most chronic health problems, including diabetes, heart disease, and cancer. Eating an anti-inflammatory ketogenic diet can be a powerful weapon by reducing chronic inflammation, stabilizing your blood sugar, and reducing insulin resistance (24, 25, 26).
Eating an anti-inflammatory diet provides your body with a healthy balance of fats, protein, and carbs, while also fueling you with necessary fiber, vitamins, minerals, and water. Nutrient-dense foods that are rich in antioxidants can effectively fight inflammation and free radicals.
Research has shown that low-carb diets, such as the ketogenic, or keto diet can effectively reduce inflammation, improve insulin sensitivity, help weight loss, and reduce the symptoms of metabolic problems (27, 28, 29, 30).

Best Foods to Improve Insulin Resistance
To lower inflammation in your body and stabilize your blood sugar, you need to remove toxic foods, such as sugar, artificial sweeteners, alcohol, caffeine, GMOs, trans and hydrogenated fats, artificial ingredients, high fructose corn syrup, and processed foods. Instead, you should fuel your body with nutrient-dense foods using the principles of an anti-inflammatory ketogenic diet.
The most important part of an anti-inflammatory keto diet is healthy fats, including avocados, coconut oil, olive oil, coconut butter, coconut milk, pasture raised eggs, and grass-fed butter. You can get plenty of antioxidants to protect your health from free radical damage through herbs, non-starchy vegetables, and low-glycemic fruits, such as berries, lemons, and limes.
Another important part of your diet on keto is high-quality protein, such as grass-fed beef, wild-caught fish, pasture-raised poultry, and wild game. Adding some nuts and seeds to your diet can add additional fiber and Omega-3s to reduce inflammation.
Fermented foods, such as sauerkraut, kimchi, and pickles can protect your gut health. Natural sweeteners, such as monk fruits and stevia can add sweetness to your life when needed in a recipe. If you want to learn more about the keto diet, you can read this article.

2. Reduce Stress and Practice Deep Breathing
Due to the increased release of a stress hormone, called cortisol, excessive and chronic stress can increase your blood sugar levels. Chronic stress can also increase emotional eating, overeating, and cravings for sugary junk foods and other unhealthy ‘comfort foods’, which can increase inflammation in your body and further increase your blood sugar. To stabilize your blood sugar and reverse insulin resistance, tackling chronic stress is crucial (31).
Meditation, relaxation exercises, yoga, journaling, coloring, using essential oils, creating some ‘me-time’, taking a relaxing bath, spending time in nature, and connecting with loved ones are natural stress relievers that can benefit your health if you are dealing with insulin resistance. These practices can help you lower overall stress levels and respond to stress more effectively without ruining your health (32).
Deep breathing is another practice that can reduce stress and stabilize your blood sugar. Diaphragmatic breathing is one form of a deep breathing technique you can try. Breathe deeply through your nose, hold it in for four counts, then exhale for two through your mouth.
Gradually increase the length of your breath until you can hold your breath for 20 counts and exhale for 10 counts. Repeat this two to three times a session for three times a day to reduce stress and improve insulin sensitivity. You can learn more about the benefits of breathing in this article (33).

3. Improve Sleep Quality
Being well-rested is absolutely essential in maintaining overall health, including stabilizing your blood sugar, improving insulin sensitivity, and reducing the risk of diabetes. According to the Centers for Disease Control and Prevention, about 35 percent of Americans obtain less than the recommended amount of 7 to 9 hours of sleep per night. And hence they increase their risk of a variety of health issues, including diabetes (34).
Sleep apnea, in fact, is a major factor in developing insulin resistance. A lack of sleep can increase your stress levels and appetite hormones and make you more likely to reach for sugary snacks and inflammatory foods. A lack of sleep, sugary foods, and excess caffeine can disturb your circadian rhythm triggering the rise of blood glucose and impaired insulin secretion.
To improve your sleep quality, reduce sugary foods and caffeine in your diet, especially in the evening. Following an anti-inflammatory ketogenic diet can help you get quality sleep. Develop a regular sleep schedule with an evening routine that works for you. Avoid blue light exposure and electronics in the evening. Choose relaxing activities such as meditation, reading, journaling, board games, a relaxing bath, and sipping on herbal tea.

4. Regular Exercise
Regular exercise is associated with countless health benefits, including weight loss, maintaining a healthy weight, heart health, and mental health. According to the National Diabetes Association, regular exercise can help you manage your blood sugar. Even short-term exercise can help your muscle cells take up more glucose to be used for energy and tissue repair.
This process can help you lower your blood sugar. Long-term exercise can also prompt your cells to increase insulin sensitivity and reduce and prevent insulin resistance. Research has shown that exercise increases the effect of exercise on insulin sensitivity through multiple adaptations in glucose transport and metabolism.
About 30 to 60 minutes of exercise on most days can help you lower inflammation, increase insulin sensitivity, manage stress levels, and improve your immunity, I recommend resistance training and high-intensity training (HIIT) 3 to 5 times a week, and low-intensity movement each day to my patients, friends, and family.
Resistance training can increase your strength and endurance, whereas HIIT workouts improve your cardiovascular health while also building strength at the same time. Exercise may include a walk in a park, playing outdoors with your kids, yoga, pilates, easy swimming, and stretching (35, 36).

5. Optimize Vitamin D Levels
Vitamin D is an essential vitamin you need for your overall health, including for stabilizing your blood sugar. While the sun is your best source of vitamin D, if you are living in a cooler area of the country with less sunlight or spending a lot of time indoors, unfortunately, you are not meeting your needs from the sun alone. While certain foods, such as fatty fish, beef liver, eggs, and mushrooms are rich in vitamin D, due to our depleted soils, they are also not enough to meet your daily requirements.
Supplementation with vitamin D is necessary and beneficial for most people, especially if you have insulin resistance. Pairing vitamin D3 with vitamin K2 helps improve calcium absorption and inflammation control. I recommend taking a vitamin D3 supplement with at least 3,000-5,000 IU’s of vitamin D3 and at least 90 mcg of vitamin K2.
Typically taking 1,000 IU per 25 lbs. of body weight will help you get your levels into a healthy range. You want to test your vitamin D levels at least 1-2 times each year and get your levels between 50-100 ng/ml. It has been hypothesized that a therapeutic level for diseases like pancreatic cancer is going to be between 70-100 ng/ml.
6. Practice Intermittent Fasting
Intermittent fasting is a powerful way to lower inflammation in your body. Intermittent fasting means that you are fasting only for a day or a part of a day regularly. One of the most popular intermittent fasting strategies includes the 5:2 approach, which means that you are reducing your calorie intake by 500 calories for 2 days a week. Another popular approach is the simple fast and crescendo fast where you are fasting for 12-14 hours straight. You may stop eating dinner at 7 PM and don’t eat until the next day at 9 AM. You can learn more about the best intermittent fasting strategies here.
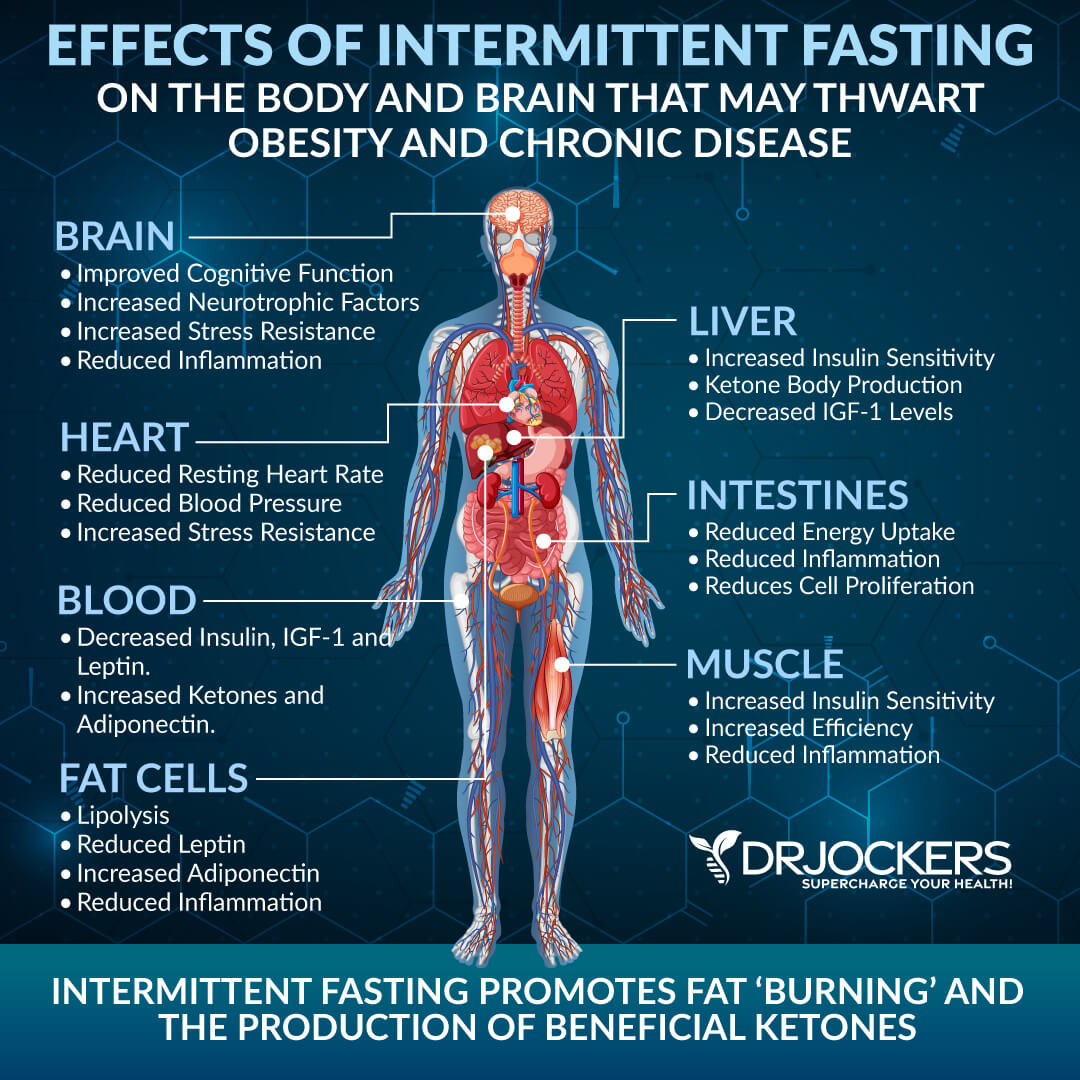
Intermittent fasting can help you burn fat, improve energy and digestion, better your relationship with food, increase your mental and spiritual health, and reduce the risk of chronic disease. Moreover, intermittent fasting can help you increase insulin sensitivity and stabilize your blood sugar.
Intermittent fasting has been shown to help balance your insulin levels and to help you lose fat when needed. Intermittent fasting can improve your relationship with food, reduce your cravings for sugary foods, and help you choose nutrient-dense, anti-inflammatory options. As a result, it can increase your insulin sensitivity. Intermittent fasting can also increase the human growth hormone (HGH), which helps you achieve a healthy weight and fat-muscle ratio, decreasing your risk of insulin resistance and diabetes (37).
You can learn more about intermittent fasting benefits in this article.
7. Improve Digestive Health and Use Probiotics
About 80 percent of your entire immune system is located in your gut. It is basically the foundation of your overall health. Having an imbalanced gut flora can result in a compromised immune system, inflammation, infections, insulin resistance, type 2 diabetes, and autoimmune disease. To stabilize your blood sugar and reverse insulin sensitivity, it is important to improve your digestive health (38).
First, get rid of anything that negatively affects your digestion, such as inflammatory foods and toxins. Eat a nutrient-dense anti-inflammatory ketogenic diet to support your gut health. Collagen, aloe vera, bone broth, and l-glutamine can help you repair your good lining. Digestive enzymes can help to improve your digestion and absorption.
More importantly, add beneficial bacteria via probiotics to help your gut health. Probiotics can balance your gut and fight harmful invaders, such as viruses, bacteria, fungi, and parasites. Fermented foods, such as kimchi, sauerkraut, kefir, yogurt, and kombucha can help to add more probiotics to your diet, however, if you are dealing with insulin resistance, inflammation, or other health issues, you can benefit from taking a daily dose of probiotic supplements.
8. Avoid Hidden Food Sensitivities
Hidden food sensitivities may be behind your insulin resistance and health issues. While food allergies come with obvious symptoms, such as rashes or anaphylactic shock, food sensitivities are not as obvious. Food sensitivities usually lead to more subtle health challenges. You may experience fatigue, headaches, digestive issues, brain fog, joint pain, and other unwanted symptoms for seemingly unknown reasons (39).
If you feel bad after eating, experience fatigue, feel like you need to take a nap, have to clear your throat regularly, have anxiety, and feel achy, you may have a hidden food sensitivity. Common foods include gluten, dairy, corn, soy, shellfish, fish, and tree nuts, however, you may be sensitive to something less common.
Food sensitivities can cause a big rise in blood sugar and insulin even if the food is low-carb, anti-inflammatory, and keto-friendly. Finding your food sensitivities and avoiding foods that you are sensitive to is crucial to stabilizing your blood sugar and reversing insulin sensitivity. Getting a food sensitivity test, trying an elimination diet, and doing a pulse test are effective ways to discover your hidden food sensitivities.
You can learn about how to identify food sensitivities in this article, and how to reduce them here.

9. Use Anti-Inflammatory Nutrients
As you’ve learned earlier, reducing inflammation is essential to stabilizing your blood sugar, improving insulin sensitivity, and preventing prediabetes and diabetes. There are some key anti-inflammatory nutrients that are important for supporting proper cellular health and insulin sensitivity.
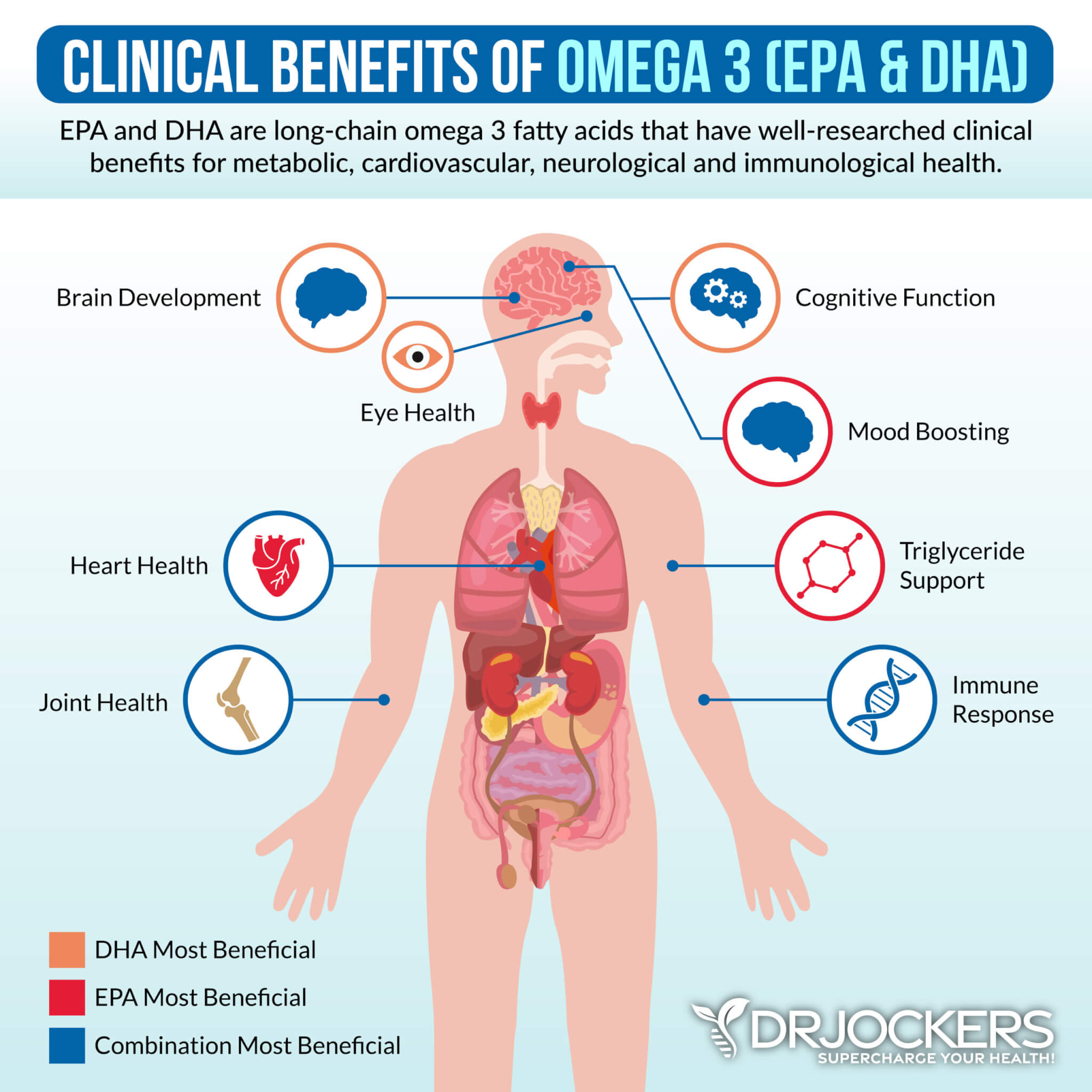
Omega-3 Fatty Acids
Omega-3 fatty acids are some of the most important nutrients your body needs. They play an important role in reducing inflammation and contribute to the health of your nervous system and brain. If you are not getting enough omega-3s in your diet, your risk of chronic illnesses, including diabetes, can increase greatly. Omega-3 can improve cellular health, depression, anxiety, stress, sleep, immunity, bone, joint, eye, heart, and brain health (40, 41, 42, 43, 44, 45, 46, 47).
There are main types of omega-3s: ALA, EPA, and DHA. EPA and DHA are derived from algae, fish, and mother’s milk. They are both extremely important for your health. While EPA and DHA can be synthesized in your body from ALA, this process puts extreme stress on your body and is very inefficient in meeting your needs.
ALA is derived from plant sources, such as nuts, seeds, and green plants. Foods high in ALA may also be high in omega-6 fatty acids. Omega-6s are important for your body, however, when you consume too much of them, they can lead to inflammation and health issues. Ideally, you want to achieve a 1:2 ratio of omega-3s and omega-6s, however, in reality, most people eat at a very inflammatory 1:20 ratio.
The best sources of EPA and DHA include algae and wild-caught fish, including wild salmon, cod, whitefish, Pacific sardines, anchovies, and herring. Flax, chia, and hemp seeds provide lots of ALA and DHA, however, they may not convert well to cover all your needs. Also, remember that your ratio of omega-3s and omega-6s is crucial for your health. Most people can benefit from additional supplementation to reduce inflammation and health problems. If you want to learn more about omega-3, read this article.
Curcumin
Turmeric is one of the most potent anti-inflammatory herbs that has been used for thousands of years as a staple in Indian cuisine, a natural remedy in Ayurvedic and Chinese medicine, and as a popular superfood in the United States in the past 30 years. Its anti-inflammatory properties lie in its active compound called curcumin.
Curcumin is a potent antioxidant with fantastic benefits to reduce inflammation and pain just as well as ibuprofen without harmful side effects. Curcumin can improve inflammation in those with diabetes, ulcerative colitis, and arthritis (48, 49, 50, 51, 52).

Glutathione
Glutathione is a specific peptide molecule that provides you with great antioxidant protection. It is often called the master antioxidant because of its ability to help maintain exogenous antioxidants, such as vitamins C and E in their active form. It protects your cells from outside attacks.
Glutathione can improve your immune function by strengthening your T cells and protecting you against viruses, bacteria, parasites, toxins, pollutants, and tissue damage. Glutathione can keep autoimmune responses in check and reduce free-radical damage (53, 54, 55, 56).

Berberine
Berberine is a powerful health compound that has been used for thousands of years by Chinese and Ayurvedic medicine. It has been highly regarded for its efficacy in supporting healthy blood sugar levels and insulin sensitivity. Research has shown that berberine may benefit the treatment of type 2 diabetes and have a positive impact on blood sugar levels, insulin, and triglycerides.
According to a 2019 meta-analysis, berberine is better than a placebo at lowering blood sugar levels and seems to be more effective when used in combination with blood sugar effective drugs when using medication alone.
A 2014 study has found that berberine may benefit those with diabetes who cannot take antidiabetic medication due to heart, kidney, or liver problems. According to a 2014 meta-analysis, combining berberine with lifestyle changes is more effective than lifestyle changes alone for improving blood sugar levels (57, 58, 59).

10. Take a High-Quality Multivitamin
One of the key aspects of health is meeting your micronutrient needs and meeting all of your mineral and vitamin needs. Unfortunately, most people are lacking micronutrients. If you are missing key micronutrients, it can contribute to inflammation, pain, insulin resistance, and health issues.
Unfortunately, even if you are eating a nutrient-dense diet, you may be lacking some nutrients due to depleted soils and poor packaging. Past unhealthy eating habits may further contribute to nutrient deficiencies, but taking a high-quality multivitamin can help you to correct these deficits.
When you are looking for a multivitamin supplement, it is important to find one with pre-activated (methylated) B vitamins, chelated minerals for absorption, and high doses of blood sugar support nutrients such as chromium and vanadium. Not all multivitamin supplements are created equal, and it is important to select high-quality and absorbable supplements.
About 30 percent of the population is unable to absorb unmethylated B vitamins. Methylated B vitamins are pre-activated, high-quality forms that are easily absorbable by everyone. Chelation is a process where minerals bind to other molecules to create an easily absorbable complex. Chelated minerals are easily absorbable and easy on your digestion. If you are dealing with insulin resistance, chromium and vanadium are two blood sugar supporting nutrients that you may benefit from within a multivitamin complex.

Final Thoughts on Insulin Resistance
An increasing number of people are dealing with insulin resistance every day. Insulin is important for your cells to absorb and use glucose for energy. Insulin resistance happens if your body is unable to respond to and use insulin. Insulin resistance can lead to prediabetes, diabetes, inflammation, and many serious health problems.
The good news is that through appropriate dietary and lifestyle changes, you can reverse insulin resistance and improve insulin sensitivity naturally. By following the 10 ways to stabilize your blood sugar, including following an anti-inflammatory ketogenic diet, reducing stress, improving sleep, exercising regularly, practicing intermittent fasting, eliminating food sensitivities, optimizing your vitamin D levels, improving your gut health, using anti-inflammatory nutrients, and taking probiotics, omega-3 fatty acids, and multivitamins, you can effectively stabilize your blood sugar.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. On our website, we offer long-distance functional health coaching programs. For further support with your health goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!





what about herbicides pesticides gmos wheat corn canola our food supply generally
Thanks Dr. Jockers
I’m going to recommend this article to my father.
He is type 2 diabetic.
I think it can help you improve your disease
Thanks again
You are welcome Pascual! I pray it will be insightful to him.
No gluten/dairy/soy/sugar/GMO/food with a label..taking vitamins/good oils/minerals…probiotic…LDN..detoxing may help. Oregon grape root (has berberine)/Mg/Cr/alpha lipoic acid/Ceylon cinnamon/Zn/fish oil/Orthobiotic probiotic before a meal/HCl and enzymes after a meal/evening primrose oil/lecithin (defats the liver)/coenzymated B vitamins/Nature’s plus- Source of Life multiple/coenzyme Q10 and more help my blood sugar and more. Gluten is wheat/barley/rye..oats/corn/rice. Rice is low in gluten. Grain free may help people/pets.
Thanks for sharing Shasha!
I can guarantee you that most people lack the discipline to eat the foods you recommended. Not only does one need endless discipline, one needs a lot of money and time to eat like that. It infuriates me that the average Joe can’t follow such strict rules…just sayin’.
Hey Robyn, the key is to do the very best with where you are at right now. There are many “average Joe’s” who can get themselves healthy if they really commit to the process.
Robyn my husband has been diabetic for almost 20 years and has Never taken a pill or a shot. He is very Disciplined. He had quadruple heart bypass in 2000 and that is when they found the diabetes. He made up his mind that day to change and he did. Unfortunately it takes something like this to see past our excuses. Respectfully .
.
Thanks for sharing this Kathy!! Great to hear that your husband is so disciplined! We all have it within us…it is just a matter of changing our mindset!
Hi, we have a dish allergy in the family so as much as we would love to take the Pro omega, we can’t, can you advise of an alternative with a different source of omega 3 than from fish. Interestingly the allergy doesn’t not extend to shellfish.
Susan
Hey Susan, if you don’t have an issue with shellfish, you can try a good krill oil or an algae oil. You can try this one https://amzn.to/2ygHFpV
Hi Dr. Jockers. I have been following intermittent fasting and generally eat within a 7-8 hour window every day. (A few months ago, I fasted for 5 days following your suggestions.) I also eat a low carb diet and am rarely hungry. My BMI is 24, which intermittent fasting has unfortunately not lowered. This week I fasted for 35 hours before getting routine wellness screening blood work done. I went to the appointment feeling well and without any symptoms of hypoglycemia – I figured my results would be better than ever! Instead they came back with my pancreas health in the danger zone; my glucose was at 60. I have never had an abnormal glucose reading in the past after fasting for blood work just the regular recommended 9 – 12 hours. Should I be concerned, or was the low glucose reading just because I shocked my body with a longer than usual fasting window? Thank you in advance for your perspective!
Hey Robyn, It is necessary to gently force the keto adaptation process with IF. This article has information on fasting strategies that will help balance your blood sugar levels. You may also want to work with a functional practitioner who can review your results including your fasting insulin and A1c levels and help you customize a strategy that works best for you!
P.S. I am not the same Robyn as the person who commented on this thread in July; interesting coincidence.
Another comprehensive article, Dr. Jockers. I wish this information had been available to me 30 years ago! I have tried sharing this information with my brother and my former sister-in-law (who has been diabetic for years) but they’re not interested. For many people, they really would rather just take the medication instead of making the changes. Then there are those M.D’s who say they would give their patients health information instead of drugs but the patients wouldn’t follow it anyway. I’ve actually heard them give this excuse as I used to be a medical transcriptionist. It’s too easy to spend 10 minutes with someone and give them a drug. I don’t think anyone just wakes up one morning and says to themself – Gee, wouldn’t I just LOVE to be fat and sick! Sign me up for that. Between the established mainstream medical profession and our government, it’s no wonder people can’t get well! I’m really hoping the keto lifestyle will help me get my life back. No M.D. ever told me that my lack of sleep, massively stressful sedentary job or even bread and margarine (which I don’t eat anymore) would make me overweight and sick – and I certainly sought them out for help – not drugs. Thanks for putting your knowledge and abilities out there for us, Dr. Jockers. You really are a God send. From now on I only listen to the real doctors – chiropractors and naturopaths!
Thanks for sharing! Praying for you and I know you will do great on this new lifestyle!
Thank you Dr Jockers for praying for your patients and honoring our loving Heavenly Father in your practice!!!
Hi Dr Jockers, thanks for your article. In fact, all your articles. They are super informative and the diagrams really help absorb the information.
I was just wondering how long it takes for blood sugars to stabilise, and insulin levels to come back to normal so everything is functioning as it should? (Which I appreciate might be a question like, how long is a piece of string?!)
I suspect I have/had insulin resistance due to too much sugar and too many calories overall.
I did a 5-day water fast just recently, and have been following most of your suggestions here over the last few weeks, including a 20:4 IM plan. Just not all keto though.
Does it take weeks or months or years to get back to normal?
Cheers
Nat
Thank you Nat! If you have done a 5 day water fast and have been doing a 20:4 then you should be well on your way to improving insulin resistance. Some individuals just have a greater genetic tendency for insulin resistance and need to be more diligent about getting regular activity and intermittent fasting than others do.
Great article except for the recommendation for nuts. Now I love nuts and I have to be very careful about them. ALL of them are much higher in omega 6 than omega 3. (Except macadamia). Here is a comparison of walnuts, the one so many recommend as high in omega 3; 2565 mg of omega 3 in an ounce (7 whole nuts) and 10,761 mg in the same ounce. That doesn’t give us much of an ideal ratio (1:1) does it? And my other question I always ask and so far have never gotten an answer, how does Almond rate as a flour substitute when it’s omega 6 are 3542/ounce (22 nuts) and 0 omega 3. I prefer to learn coconut flour uses.
Yes we prefer coconut flour as well but having some nuts should be fine if balanced with wild-caught seafood and grass-fed meats.
I purchased Sugar Support but need more information:
Why should I take it?
What exactly should it do for me while I’m taking it?
What results have others had and the length of time it takes to get those results?
Are there any side effects?
Hello Pam – you can find some helpful information here: https://store.drjockers.com/products/sugar-support
Please explain how your Sugar Support can help those who may be hooked in sweets and are overweight. Thank you!
You recommend sauerkraut to get probiotics into the gut, but at least with supplemental probiotics, we are told that they can’t survive stomach acidity unless specially encapsulated. How does that work with sauerkraut?
Thank,
Diane
Interestingly, the benefits of probiotics according to the research are not dependent upon them being “alive.” They seem to have a great impact on balancing the immune system even when they aren’t alive.
Hello! I’m a frequent podcast fan and just listened to one released back in April of 2024. Q&A which included Castor Oil and blood pressure/hypertension. I took notes and went to your site to purchase the recommended “Amino Charged” but can’t find anywhere. Is this sold somewhere else? Please advise and thank you! Love your podcasts!!!
Yes you are talking about Amino Strong: https://store.drjockers.com/products/amino-strong
Yes here it is: https://store.drjockers.com/products/immunocharge