
What are Your Homocysteine Levels?
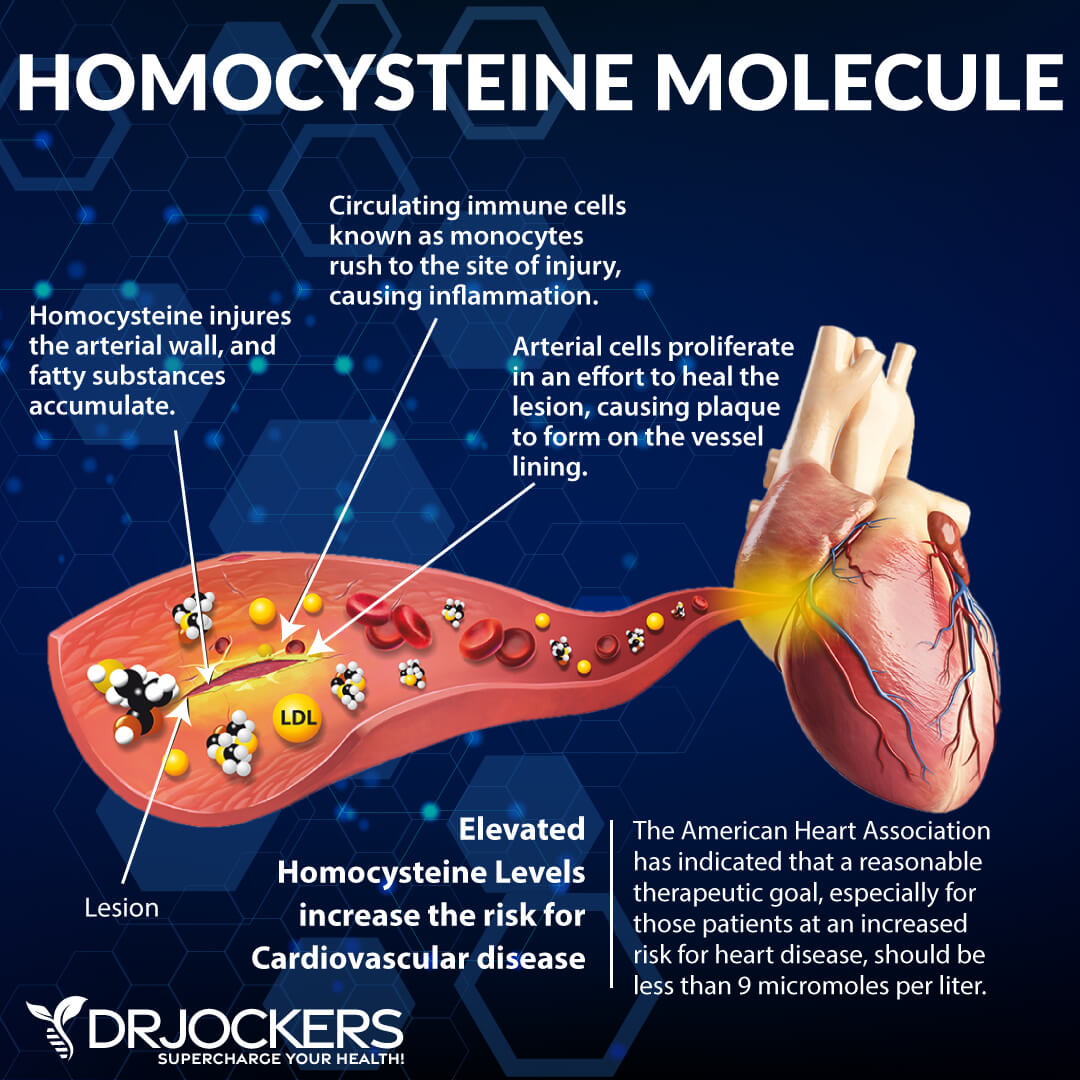
Homocysteine is an inflammatory amino acid that is produced as a byproduct of protein metabolism. Homocysteine-induced injury to the arterial wall is one of the factors that can initiate the process of atherosclerosis, leading to endothelial dysfunction and eventually to heart attacks and strokes (1).
Dr. Kilmer S. McCully originally reported in 1969 that elevated homocysteine was associated with advanced atherosclerosis and premature death (2). He found that children born with a genetic disorder called homocystinuria, which causes the homocysteine levels to be very high, often died at a very young age with advanced atherosclerosis in their arteries. However, it was not until the 1990s that the importance of homocysteine in heart disease and stroke was appreciated.
Problem With Elevated Homocysteine Levels:
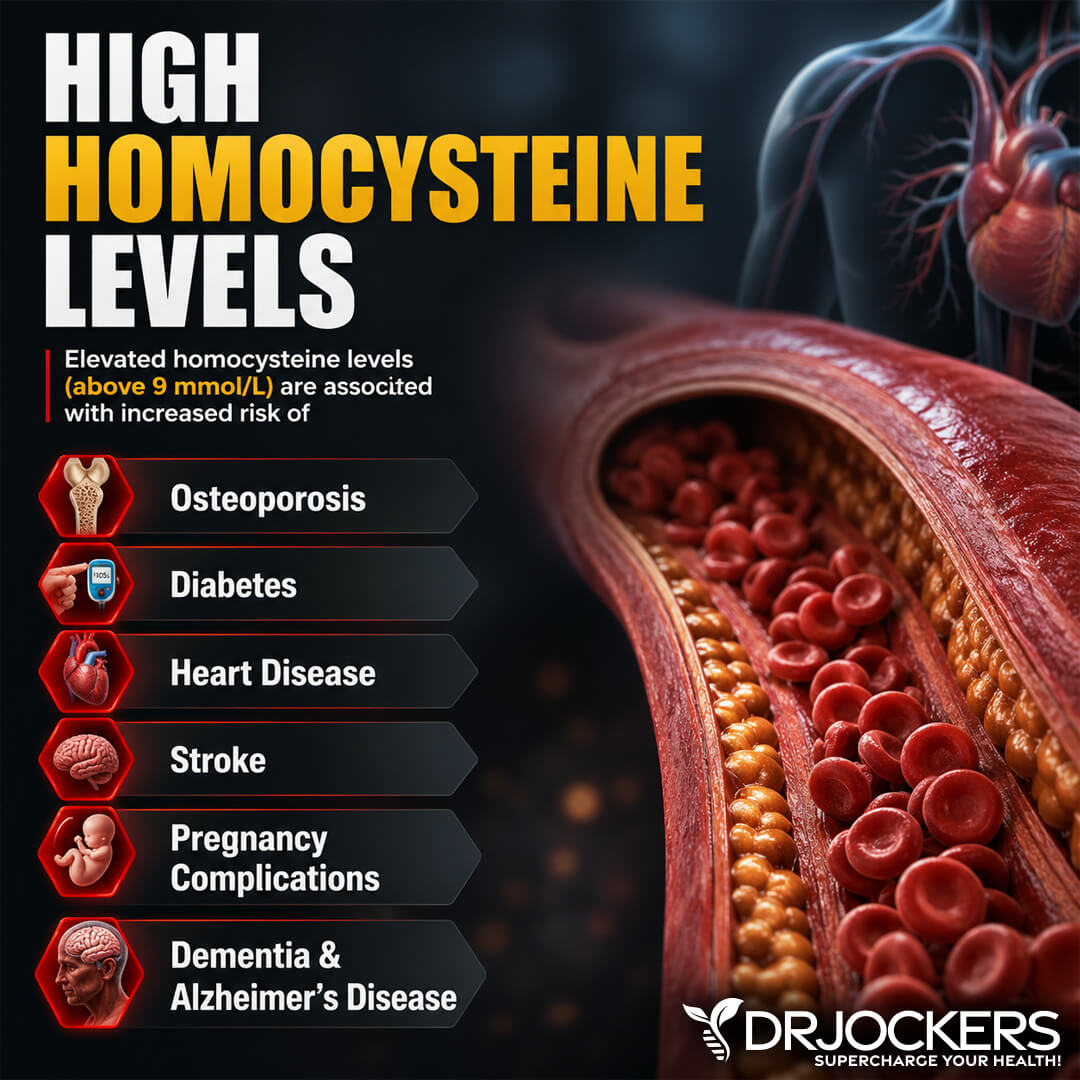
Elevated homocysteine causes excessive clotting, which diminishes blood flow to major regions of the body. The lack of blood supply to the heart may cause heart attacks, and the lack of blood supply to the brain accelerates the development of dementia and may lead to strokes (3, 4).
High homocysteine is also associated with blood clots in other major regions of the body. This includes the veins in such conditions as deep vein thrombosis and pulmonary embolism. In some studies, even moderate levels of homocysteine showed higher rates of incidence of blood clot formation (5, 6).
Who Should Get Tested:
Anyone who has a family history of heart disease, stroke, diabetes, or cognitive degeneration. Additionally, anyone who has already been diagnosed with any of these conditions should be monitoring their homocysteine levels. Individuals who have a family history or personal history of alcoholism or kidney disease will also be at risk.
The best way to test homocysteine levels is through a combination lab that looks at other factors involved in cardiovascular health, such as C-Reactive Protein, Lp(a), lipids, liver enzymes, B12 levels, and so much more. Getting a Comprehensive Blood Analysis is a great blood test that allows us to look at all these factors of your health.

Elevated Homocysteine Levels:
Homocysteine is a metabolic byproduct of protein metabolism and, in particular, the metabolism of methionine. Methionine is found in meats, seafood, dairy products, eggs, sesame seeds, and Brazil nuts.
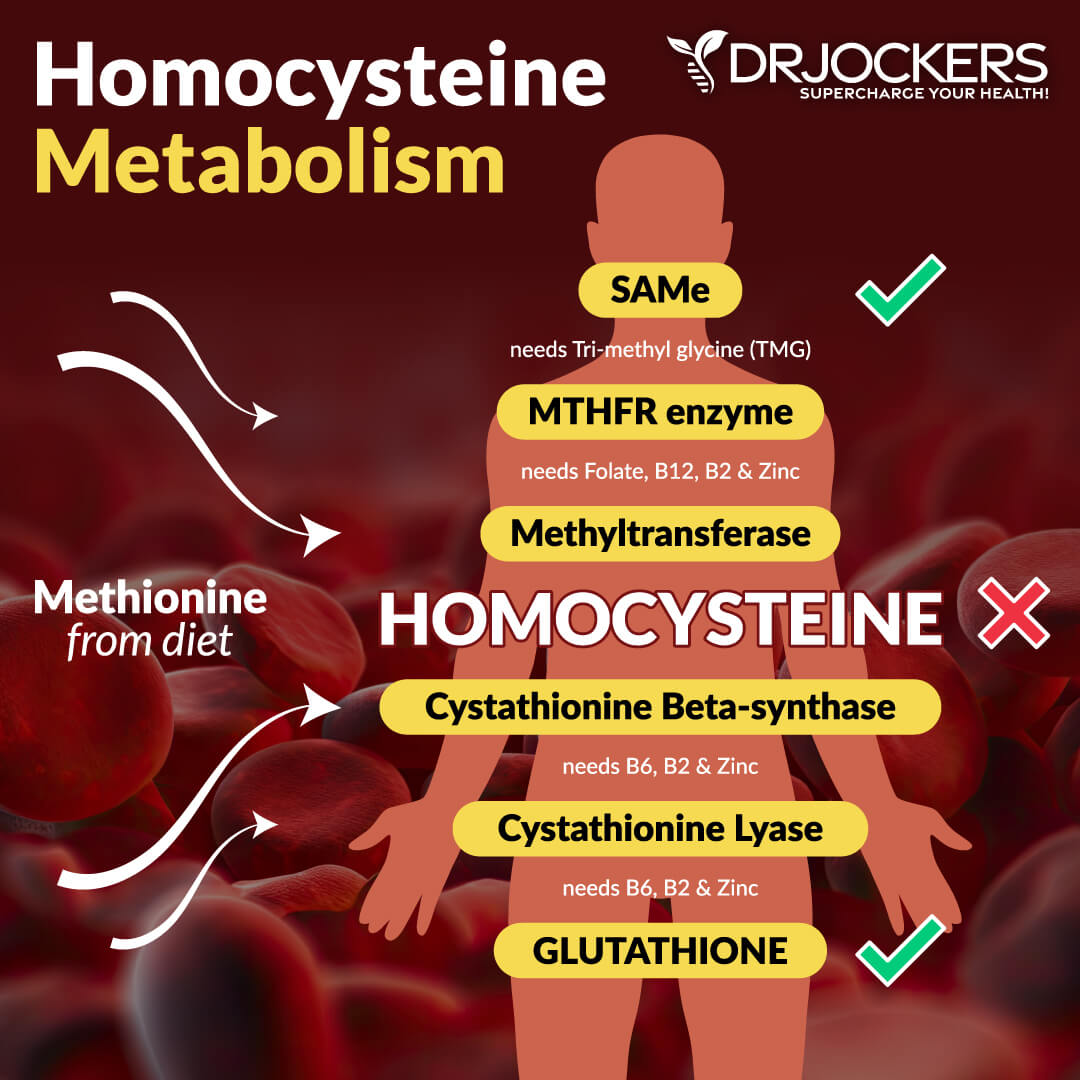
Homocysteine is metabolized through two pathways: remethylation and transsulfuration. Remethylation requires folate and B12 coenzymes, while transsulfuration requires pyridoxal-5-phosphate, the B6 coenzyme.
The Methylation Cycle and Homocysteine:
Typically, about 50% of homocysteine is remethylated, and the remaining homocysteine is transsulfurated to cysteine. The cysteine that is formed is then used to produce glutathione. Glutathione is a powerful antioxidant that protects cellular components against oxidative stress.
Vitamin B2 and magnesium are involved in homocysteine metabolism. Without proper levels of methylated B6, B12, folate, B2, and magnesium, dangerous levels of homocysteine may build up in the body (7).

Poor Diet and High Homocysteine:
A poor diet that is high in sugar and carbohydrates can deplete these key B vitamins and magnesium. If an individual has gut dysbiosis, they can have poor absorption of these key nutrients, which can result in high homocysteine as well (8, 9, 10).
Finally, genetic defects such as the MTHFR gene mutation can often cause problems with folate and B6 absorption and utilization are often found in individuals with elevated homocysteine (11).
Proper Supplementation:
Blood tests that show homocysteine levels above 8 umol/L are an indication of methylation deficiencies and elevated risk of cardiovascular disease. These individuals should supplement with pre-methylated forms of B vitamins such as methyl-folate, methyl-B12, Pyridoxal 5′ Phosphate, riboflavin, trimethylglycine, magnesium, and choline.
Clinically, I use a product called Methyl Power, which has clinical doses of each of these nutrients and will lower homocysteine levels when the issue has to do with B vitamin deficiencies.
N-Acetyl Cysteine and lipoic acid are also great supplements to help boost glutathione and lower homocysteine levels (12, 13). High-quality omega-3 fatty acids and medium-chain saturated fats from coconut oil are critical players in lowering homocysteine as well (14).
We have many of these powerful glutathione boosting compounds and mitochondrial enhancing nutrients, such as CoQ1,0 in our Mito Support product here.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!







I have a cbs mutation but cannot tolerate B6. Gives me severe anxiety like a heart, attack.P5P gives me some anxiety. I believe the cbs mutation is active. What is causing the B vitamin issue? Thanks. 🙂
If I purchase the b12 methyl and brain vitamins would I just follow the recommended dose
Yes, I would recommend starting with that and you can test your B vitamin levels, neurotransmitters and mitochondria with this test: https://drjockers.com/comprehensive-organic-acid-test/
It is such a disaster trying to figure out our problems when the medical system won’t do some of the highly critical lab tests such as vitamin D and also homocysteine, which is in my family; most likely because there is not a drug to help these problems. Last time I checked mine, I paid for the tests for Vit D and homocysteine (in Canada regular blood work is paid for). I took a methylated form of B Vitamins which doesn’t have all the B’s included. It did bring level down to normal. I have a problem with really high, 1.5 to 2 times, level of B12. I quit taking my B complex supplement because of this, but now, seems to me some of my problems could be a result of lack of some Bs. (mostly sticking to keto type foods) I have checked this out and we (doc)are checking every 3 months to also monitor the immature white blood cells test is up a bit so pretty scary, I guess. Also have urate level up in most blood work. I know you can’t go into my medical issues but thought sometimes there is a possible issue that the Docs don’t look at. Have multiple food allergies and sensitivities, which is one thing mentioned that causes Immature Granulocytes and I know it could possibly be something really worse than that. Most of blood work is actually good, all levels seem to be in the middle of scale amounts shown. Thank you for all your great work and help!
Yes I would recommend working with a functional health practitioner to help you figure this all out!