 Immune Nutrients to Calm Cytokine Storm
Immune Nutrients to Calm Cytokine Storm
Immune nutrients could not be more important to consider than they are right now. We have recently experienced a respiratory virus that led to a global pandemic that shut down most of the world. One of the major issues that respiratory viruses can trigger in our body is the phenomena of a “cytokine storm,” where the immune system damages our respiratory tissue. As we get a better understanding of how respiratory viruses work, we realize that certain immune nutrients can support our immune system and calm down this cytokine storm.
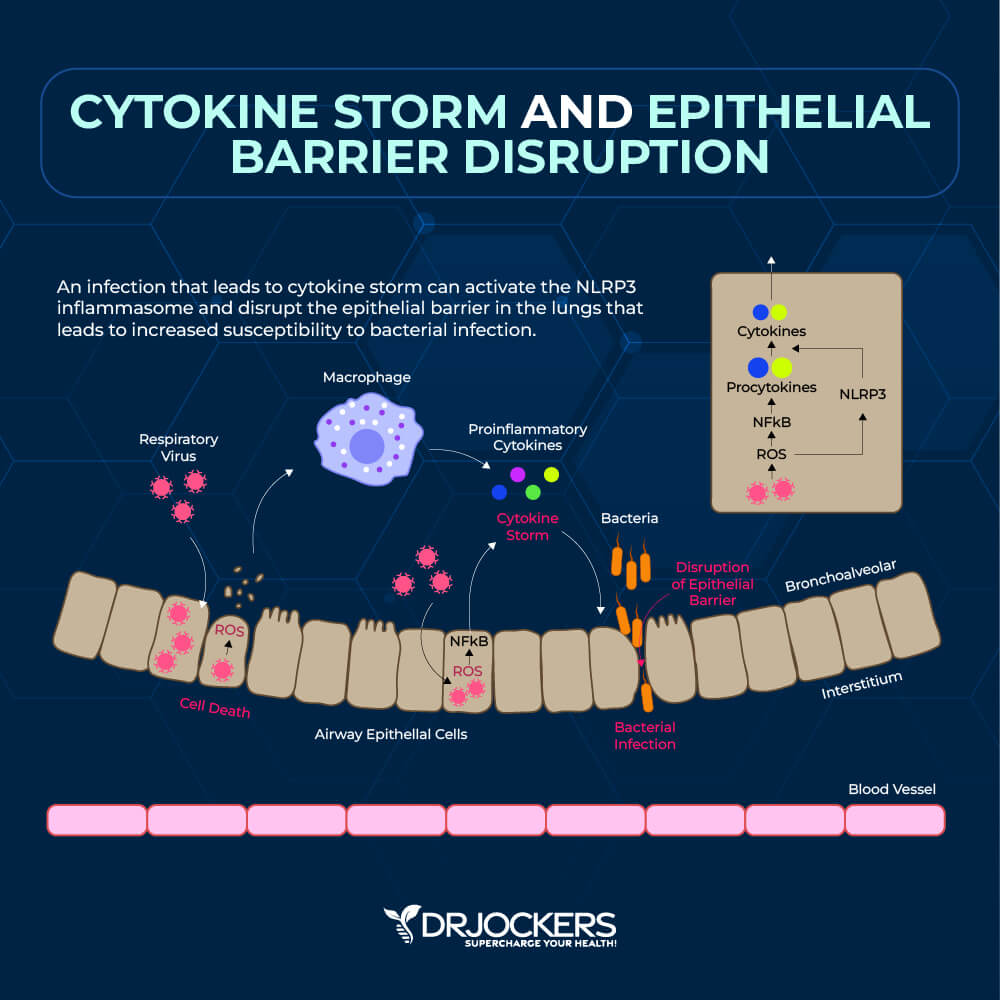
Cytokines are an important part of your immune response. Your body releases them as a response to an infection to trigger inflammation for your protection. A cytokine storm, however, is not good news. A cytokine storm happens when the body releases excessive or uncontrolled levels of cytokines, which results in hyperinflammation and may lead to serious complications or even death. It has contributed to complications and death in more serious cases of COVID-19.
Along with discussions popping up about the cytokine storm and COVID-19, I also noticed a lot of misinformation about elderberry causing cytokine storm. These speculations have no known scientific evidence, so I want to create clarity about the potential health benefits of elderberry as an immunomodulator and its potential benefits as an immune nutrient for optimizing your immune system.
In this article, I will discuss how COVID-19 works and how it enters your body. You will understand what a cytokine storm is and why it is a problem. I will share the top immune nutrients that may help to calm a cytokine storm. Finally, I will discuss and create clarity on whether or not elderberry can cause a cytokine storm.
How COVID-19 Works
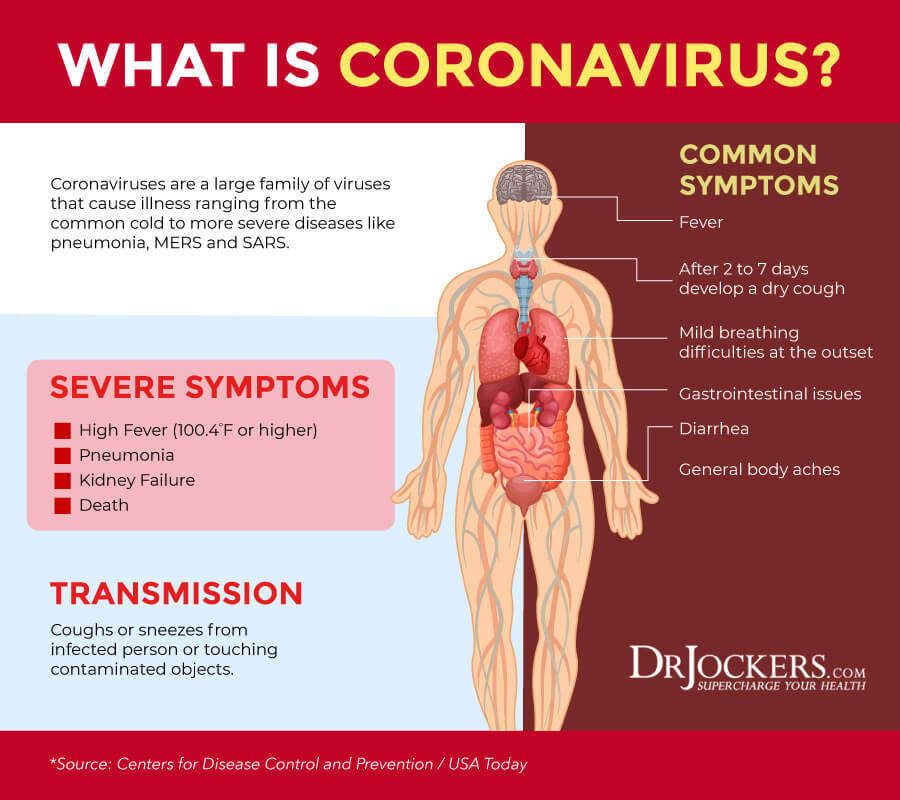
COVID-19 (or SARS-CoV-2) is a novel coronavirus. Coronaviruses (CoV) are a large group of enveloped, positive-sense, single-stranded RNA viruses. They have different strains that may cause different illnesses ranging from the common cold to more severe illnesses. In the past two decades, we’ve seen two coronavirus outbreaks, the Severe Acute Respiratory Syndrome (SARS-CoV or SARS) in 2002 and the Middle East Respiratory Syndrome (MERS-CoV, or MERS) in 2012 that led to serious illness and in many cases, death.
Coronaviruses are zoonotic viruses, which means that they can be transmitted between humans and animals. SARS was transmitted from civet cats to humans, and MERS originated from camels. While scientists are not clear where COVID-19 originated, recent evidence has indicated that the virus was made or altered to have increased virulence in the Wuhan, China viral research lab and somehow this was leaked out to the public in China.
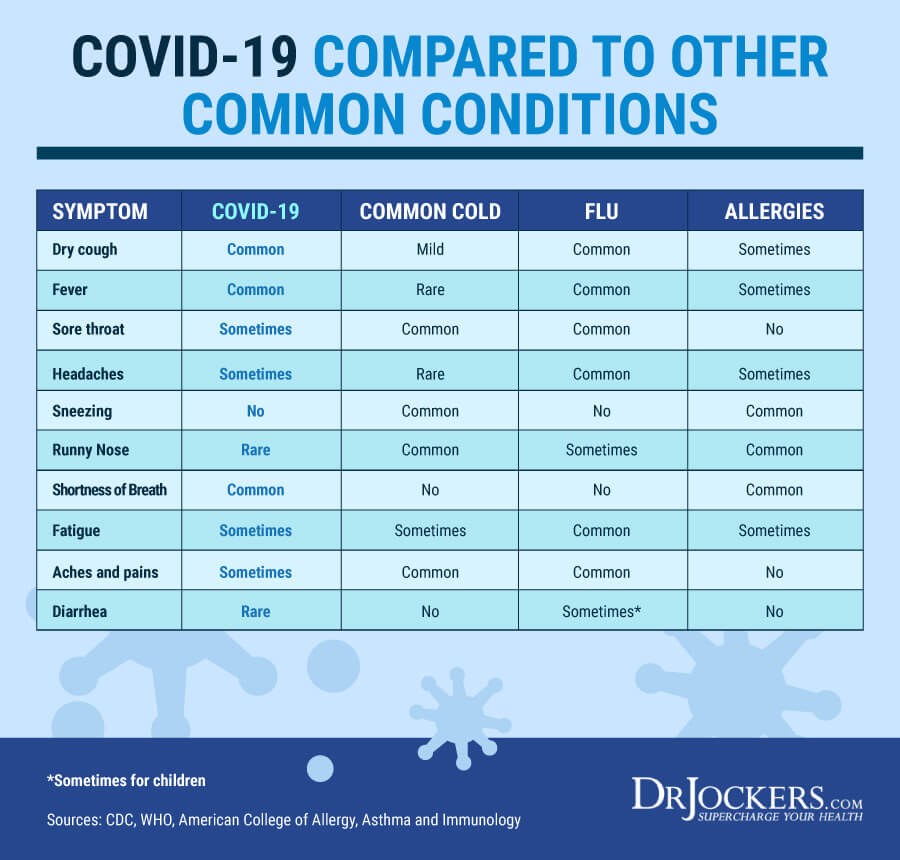
The main symptoms of the virus include cough, fever, and shortness of breath while some people experience other respiratory and even gastrointestinal issues. Up to 80 percent of the population may only develop mild to moderate symptoms that they can recover from at home and about 20 percent may develop more serious issues, including bronchitis and pneumonia which will require hospitalization.
COVID-19 And The ACE2 Receptor
Those over the age of 60 and people with a compromised immune system are at higher risk, however, we have also seen cases of younger and otherwise healthy people needing care at the hospital. While at a less than 1 percent mortality rate, COVID-19 is not the most deadly (SARS had a mortality rate of ~15 percent, MERS had a mortality rate of ~35 percent), but it is certainly the most serious coronavirus we have seen that has lead to a global pandemic and national emergency (1, 2, 3, 4, 5).
In the midst of the ongoing COVID-19 pandemic, scientists are currently studying the virus to understand how it is similar to and different from the severe acute respiratory syndrome (SARS-CoV or SARS) that led to the outbreak in 2002.
While there are definitely some differences between the two viruses as well as the extent of the outbreaks we are dealing with, the way the two viruses work in your body show some similarities. Both SARS and COVID-19 seem to exploit the angiotensin-converting enzyme 2 (ACE2) receptor in your body to gain access inside your cells.
How COVID-19 Gets Into Our Cells
Understanding how a virus gains entry to human cells is important for the development of potential vaccines and treatment methods, and may also help us to better understand preventative measures and immune nutrients that may help us. This is especially important since COVID-19 is a virus, not a bacteria, which means that our current method of treatment is simply supporting your immune system and body and in more serious cases, organ support.
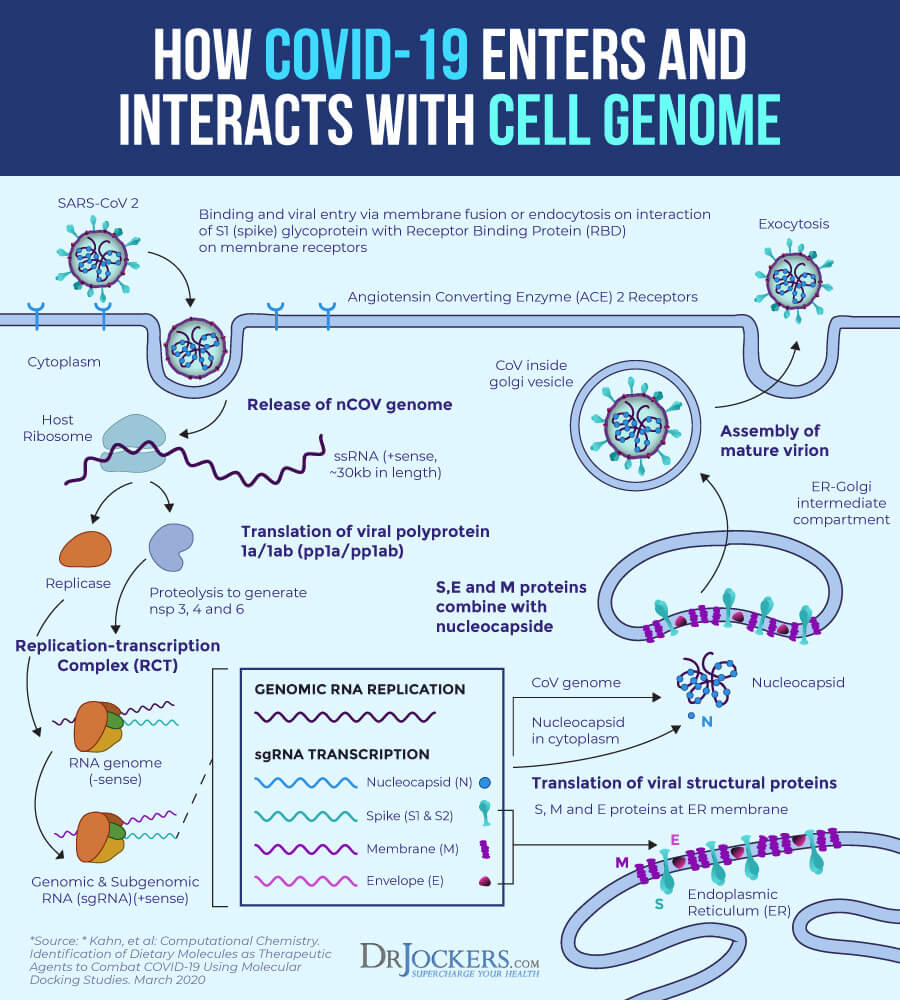
Coronaviruses, and therefore the COVID-19 genome encodes four major structural proteins: the spike (S), nucleocapsid (N), membrane (M), and envelope (E) proteins. The S protein is the one that helps the entry of the virus to the target cell in the body. Research has shown that about only about 75 percent of the COVID-19 S protein genome is the same as the SARS S protein genome, however, most of the amino acid residues needed for receptor binding are the same between the two viruses. This also suggests that the entry receptor, ACE-2, used by SARS is the same for COVID-19 as well.
ACE-2 is a type I transmembrane metallocarboxypeptidase with a similar structure to ACE, which is an enzyme that is an essential part of the Renin-Angiotensin system (RAS) and an important target for hypertension treatment. ACE and ACE-2 are both expressed in vascular endothelial cells, the renal tubular epithelium, and in the testes Leydig cells. ACE-2 is also expressed in your lungs, gastrointestinal tract, and kidneys, and plays a protective role in your cardiovascular system and other organs in your body.
SARS and COVID-19 show sequence similarities, and it seems that both viruses use the ACE-2 as a cellular entryway to your body. Researchers believe that COVID-19 can use ACE-2 from humans, civet cats, pigs, and Chinese horseshoe bats to access the body. Research has shown that the affected ACE-2 in neurological tissue may lead to neurological tissue damage which may also contribute to the morbidity and mortality of the disease (6, 7, 8, 9, 10, 11, 12, 13)
What Is Cytokine Storm
When reading about the symptoms and complications of COVID-19, chances are, you will run into the word cytokine storm. But what is a cytokine storm and why is it a problem? Let’s take a look at this phenomenon.
Cytokines got their name from the Greek words cyto (cell) and kinos (movement). They are small proteins that your body’s cells may release in different areas. For example, the cells of your immune system may release them as a response to an infection and to trigger inflammation for your protection.
The problem occurs when your body’s reaction to an infection goes into overdrive. For example, researchers have observed that when the COVID-19 virus enters the lungs, it triggers an immune response that prompts immune cells to fight the virus and to create localized inflammation. In a small number of patients, however, the body releases excessive or uncontrolled levels of cytokines, which results in hyperinflammation and may lead to serious complications or even death. This hyperinflammation and consequent damage are called the cytokine storm.
Cytokine storms are not a new phenomenon in the medical field. It is not only a complication that is observed in some COVID-19 patients, but also in patients of seasonal influenza (flu) virus. It has been observed that other coronaviruses, such as SARS and MERS, as well as the bird flu (H5N1 influenza virus) lead to many cases of death. Cytokine storms may also happen in non-infectious diseases, such as pancreatitis and multiple sclerosis.

COVID-19 and Cytokine Storm
We know that while a large percentage of the population only experiences mild to moderate symptoms of COVID-19 and won’t require hospitalization, others experience severe symptoms and complications, require hospitalization, or may even die. The cytokine storm may be one possible way to explain the severe reaction of those in our hospitals.
This may also explain why younger people and those with a healthy immune system and without preexisting health conditions tend to have an easier time. Their bodies may release lower levels of cytokines creating just enough inflammation for healing.
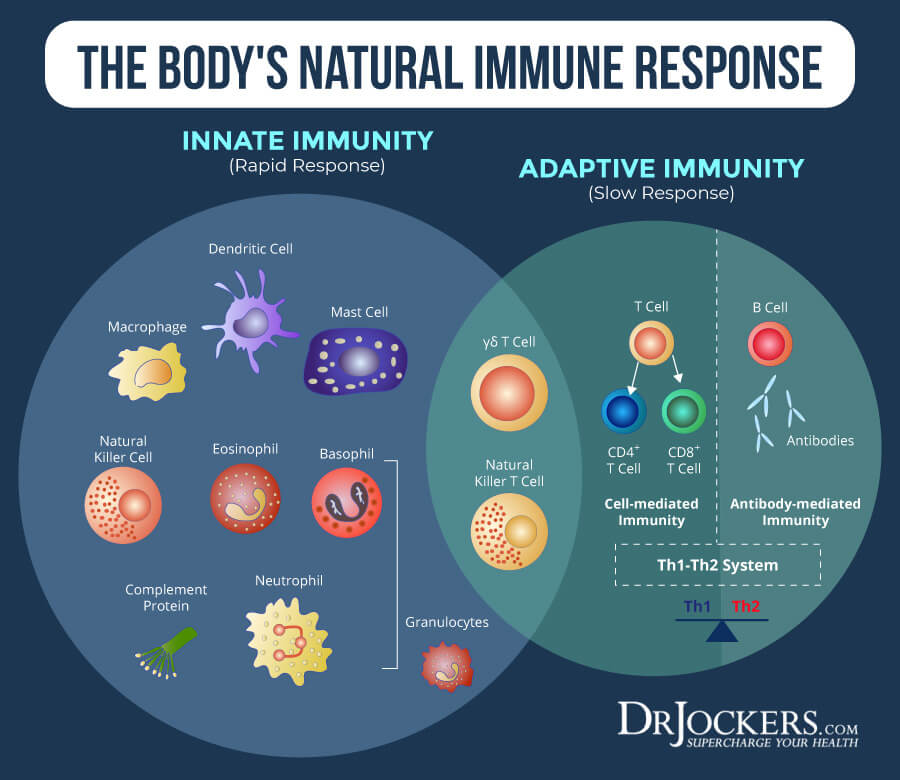
Research has found that COVID-19 increases (IL)-1β and IL-6, IL-17 pro-inflammatory cytokines, which act as a mediator of lung inflammation, fever, and fibrosis. On the other hand, the suppression of pro-inflammatory cytokines may be beneficial in treatment. Other cytokines, such as Interferon (IFN-alpha and beta), along with IL-37 and IL-38, show the ability to suppress innate and acquired immune responses. While more research is needed, these findings may lead to a new strategy.
Nutrients to Block COVID-19 Molecular Docking
As you know, COVID-19 is a new virus. Treatment includes supportive care and supporting organ functions when necessary. While research is ongoing looking at the potential benefits of certain existing drugs, including remdisivir and chloroquine, and the search for new medications and a vaccine is ongoing, looking at alternative options is critical. In recent decades, research has shown that certain edible herbs and vegetables have various health benefits with little to no side effects.
The hope of this research is that dietary molecules in these plants may also be developed as herbal medicines or therapeutic agents to be used in the treatment or prevention of COVID-19. Past research has shown the potential benefits of curcumin, savanin, and betulinic acid for SARS.
To understand the benefits of certain herbs and plants further, one recent molecular docking study looked into 18 dietary molecules, including epigallocatechin gallate (EGCG), curcumin, beta-glucan, piperine, apigenin, gingerol-[6], resveratrol, myricetin, quercetin, genistein, daidzein, alliin, allicin, sulforaphane, phycocyanobilin, ferulic acid, and alpha-lipoic acid, to explore their potential benefits for COVID-19. (43).

Top 3 Immune Nutrients to Block COVID-19 Cell Entry
Researchers used a molecular docking analysis using a computer cluster system to understand the molecular interactions of these dietary molecules with the binding pockets of different types of proteins of COVID–19. Researchers wanted to understand which proteins are responsible for the high virulence and replication of COVID-19, and what may prevent the infection or destroy the virus.
Based on past research, main protein targets included “main protease COVID–19 (6lu7), the structure of the 2019-nCoV HR2 Domain (6lvn), the structure of the post-fusion core of 2019-nCoV S2 subunit (6lxt), prefusion 2019-nCoV spike glycoprotein (6vsb), the structure of 2019-nCoV chimeric receptor-binding domain complexed with its receptor human ACE2 (6vw1), the crystal structure of NSP15 endoribonuclease from SARS CoV–2 (6vww) and crystal structure of the free enzyme of the SARS-CoV–2 (2019-nCoV) main protease (6y2e)”.
To get some answers for their second question regarding prevention and treatment they selected the 18 dietary molecules I just mentioned based on their anti-viral or anti-SARS potential indicated by earlier studies. Their findings indicate that curcumin, EGCG, and beta-glucan are some of the strongest options and people may benefit from using them as a dietary supplement for immune nutrient support (43).

Immune Nutrients to Calm Cytokine Storm
If you want to optimize your immune health and reduce your risk of a cytokine storm, there are various immune nutrients that may help you. It is important to note that since COVID-19 is a new virus, there is no research suggesting that these immune nutrients would specifically benefit COVID-19 prevention or recovery.
However, there are scientific studies that show their immune benefits for other viral infections, including the flu, other coronavirus infections, and other respiratory infections. As with other infections, I recommend protecting your body and optimizing your immune health with the best immune nutrients.
While at this point, research is ongoing and scientists are working hard to understand COVID-19 and find treatment options, these are some promising developments. The good news is that you don’t have to wait to take steps to protect your health. There are a number of things that you can do to improve your immune system, including using immune nutrients that may help to calm a cytokine storm (14, 15, 16, 17, 18, 19, 20).

Vitamin D
Vitamin D is an essential immune nutrient. It supports your immune system, brain, nervous system, lung function, cardiovascular health, bones, and teeth. The best way to meet your vitamin D needs is through the sun. Unfortunately, during the winter months and times of gloomy weather, it is impossible to meet all your needs.
Research suggests that low vitamin D levels may contribute to viral epidemics in the winter, while optimal vitamin D levels may help to reduce the risk of viral epidemics and pandemics. Observational and supplement trials suggest that higher 25(OH)D concentrations of vitamin D immune nutrient supplementation may reduce the risk of various viral infections, including influenza, dengue, hepatitis B and C, pneumonia, and respiratory viral infections.
Research suggests that vitamin D supplementation may reduce the production of proinflammatory cytokines by the innate immune system and as a result may also lower the risk of a cytokine storm and pneumonia (21, 22, 23).

Resveratrol
Resveratrol is a powerful plant compound found in grapes, berries, and red wine. This immune nutrient acts as an antioxidant and helps to optimize your immune system. Resveratrol may also help to calm a cytokine storm. In one animal experiment mice were given superantigen staphylococcal enterotoxin B (SEB), to induce lung inflammation. SEB can lead to respiratory failure and treatment options are limited to supportive care.
The study has found that the administration of resveratrol had anti-inflammatory benefits on pulmonary inflammation. The study has shown that resveratrol may be effective in suppressing the potent immune responses induced by a superantigen and may help to reduce the risk of acute lung inflammation. These findings are incredibly exciting when it comes to the prevention and treatment of respiratory infections (24, 25).

Quercetin
Quercetin is a pigment that is found in plants, vegetables, and fruits and serves as an immune nutrient offering many health benefits. Elderberry, red onions, white onions, and cranberries are the richest sources of quercetin. It is a flavonoid and antioxidant that may help to reduce inflammation, infections, and allergies. Research has found that quercetin may be particularly beneficial for viral respiratory infections.
One study has found that quercetin may have the ability to inhibit influenza infection. It may be beneficial for various strains of the influenza virus, including H1N1, H3N2, and H5N1. It also shows promise for blocking the COVID-19 from entering into the cells. Results suggest that quercetin may be a safe natural method for preventing and aiding recovery from viral infections (26, 27).

Curcumin
Curcumin is the active compound of one of the most rigorously studied herbs. It has been used in Asia for its medicinal properties and countless studies have shown its anti-inflammatory, anti-viral, anti-biotic, and anti-fungal benefits. It has been used for joint pain, digestive issues, and many other chronic health conditions. Curcumin is a powerful immune nutrient with countless benefits, and current research on COVID-19 treatment options has shown its potential benefits (42).
The molecular docking study found that curcumin, EGCG, and beta-glucan, as well as quercetin, myricetin, genistein, myricetin, and daidzein, may show benefits as a potential treatment for COVID-19. Curcumin ranked number two in most categories. It ranked number two against 6lu7, 6lvn, 6vw1, 6vww, 6yte number four against 6vsb, number five against 6vsb and 6lxt of COVID-19. The study recommends 500 mg of curcumin.
Taken in the form of turmeric, they suggest 15.625 gm per day. Take it 3 times a day every 6.5 hours. If you are using turmeric, mix it with lukewarm milk or plant milk. You can also look for a good quality curcumin supplement (43).

EGCG
EGCG is a powerful plant compound and immune nutrient primarily found in green tea. It is known for its many health benefits. This immune nutrient is rich in polyphenols and antioxidants. It may help to lower oxidative stress, decrease inflammation, improve heart health, support brain health, and aid weight loss. Research on COVID-19 treatment and prevention found it to be potentially beneficial (44).
The study we’ve discussed under the curcumin section found that EGCG among other herbs may show benefits as a potential treatment for COVID-19. The study also indicated that EGCG may also act as a COVID-19 inhibitor, and recommends it for further treatment and drug treatment research.
EGCG ranked number one against all proteins, including 6lu7, 6lvn, 6vw1, 6vsb, 6vww, 6lxt, and 6yte of COVID-19. The study suggests taking 800 mg of EGCG or 16.67 gm of green tea a day. Brew it for 3 minutes in boiling water. Let it cool a bit then drink it 3 to 4 times a day every 4.5 hours.

Beta-Glucan
Beta-glucans are beta-D-glucose polysaccharides that are naturally found in the cell walls of cereals, bacteria, and fungi. They have been used for a number of issues, including the flu, swine flu, digestive issues, ear infections, allergies, Lyme disease, chronic fatigue syndrome, and more. It is not surprising that research on COVID-19 prevention looked into beta-glucans for its potential benefits (45).
The study we’ve discussed under the curcumin section found that beta-glucan among other herbs may show benefits as a potential treatment for COVID-19. Beta-glucan ranked number three against 6lu7, number four against 6vww, and number five against 6y2e. You can get beta-glucans in medicinal mushrooms such as Cordyceps, Reishi, Maitake, and Shiitake or as stand-alone supplements (43).

Melatonin
You may know about melatonin as a supplement that can support your healthy sleep cycle. Assisting sleep and rest is already an immune system-supporting benefit, but melatonin has more to offer. It is a powerful antioxidant that supports your immune health, brain, eyes, digestion, and more. It may even be helpful when it comes to COVID-19.
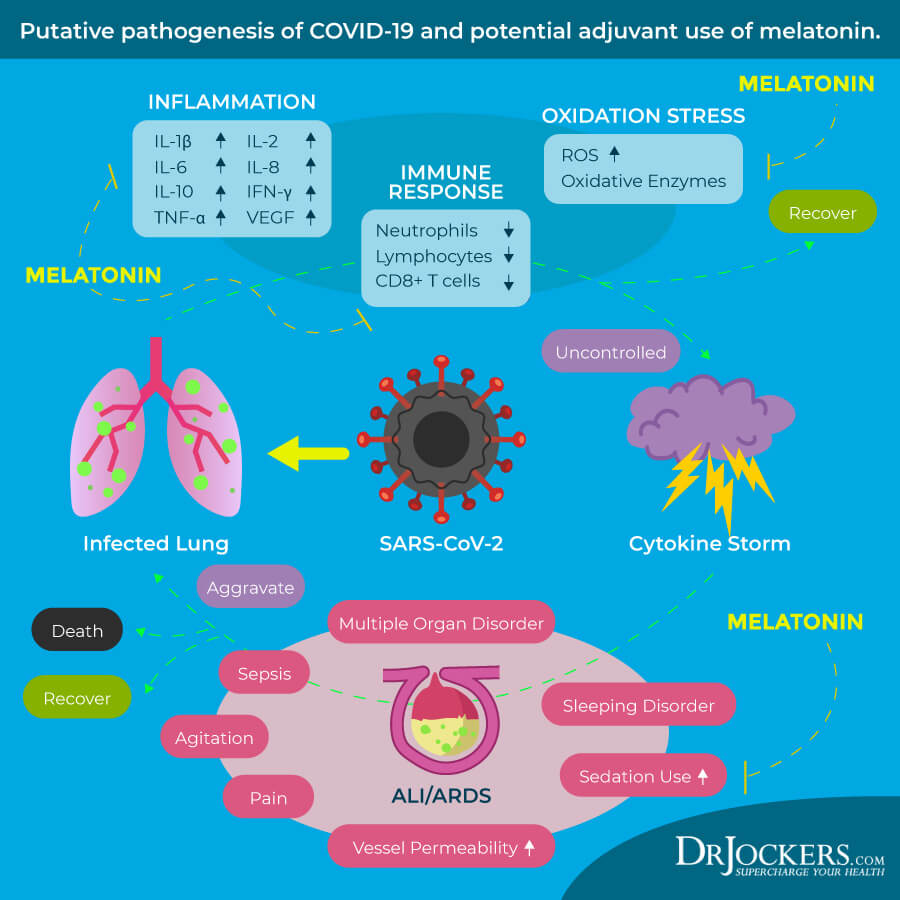
One recent paper discussed that melatonin is a powerful anti-inflammatory and anti-oxidative molecule that may be protective against acute lung injury (ALI) and acute respiratory distress syndrome (ARDS). This is important because most serious complications of COVID-19 happen because of a cytokine storm that can lead to ALI, ARDS, and even death.
The paper notes that melatonin is a safe supplement that has already shown benefits for other viral infections and may be helpful for cases of COVID-19 by calming the cytokine storm (28, 29).
Probiotics
Probiotics are incredibly important for your digestion and gut health. Since your gut is connected to all areas of your body, healthy gut flora is important for your immune system as well. It’s not surprising that probiotics may help as immune nutrients.
Researchers have found that probiotics may have immunomodulatory effects. According to a scientific review some probiotics, including certain species of Lactobacillus and Bifidobacterium can play an important role in innate immunity. They may help your body by increasing the cytotoxicity of natural killer cells and supporting adaptive immunity.
Probiotics may help to stimulate anti-inflammatory cytokines and improve your body’s defense system against invasion by bacterial, fungal, viral, and other infections (30, 31).

Vitamin C
Vitamin C may be one of the most well-known immune nutrients that protect against immune deficiencies and which support the prevention and recovery from the common cold and upper-respiratory issues and also protects your cardiovascular system, eyes, skin, and other parts of your body. Research has found that vitamin C may help to optimize the innate and adaptive immune system.
On the other hand, vitamin C deficiency may lead to impaired immunity and higher susceptibility to infections. Vitamin C may help to improve your body’s immune response and to prevent and treat respiratory and systemic infections, including respiratory issues (32, 33).

Zinc
Zinc is another powerful immune nutrient known for its benefits for providing immune health support and inflammation reduction as well as for improving cold and respiratory symptoms, wound healing, acne reduction, and lowering the risk of age-related diseases. Research on atherosclerosis and diabetes mellitus suggests that zinc deficiency may contribute to low-grade systemic inflammation.
Zinc deficiency may also lead to increased inflammatory cytokines. However, zinc supplementation may have anti-inflammatory benefits, increase the expression of anti-inflammatory cytokines, lower oxidative stress, and help to achieve homeostasis. Findings suggest that zinc may help to prevent or calm a cytokine storm (34, 35).

Does Elderberry Cause a Cytokine Storm
Elderberry syrup and tea has been one of the favorite natural remedies on the market for immune support. Over the past few months, however, I’ve noticed an emerging new concern that people are discussing. Even though there is no research indicating this, people are worried that elderberry can cause a cytokine storm and that it is not a safe immune nutrient choice when it comes to COVID-19. Is this true? Does elderberry cause a cytokine storm? Let’s find out.
As I said earlier, there is currently no research that indicates that elderberry can cause a cytokine storm and that it is unsafe for COVID-19. It is unclear how this misconception came about. Recent studies circulating on the internet about cytokine storm and COVID-10 do not mention elderberry at all.
To be clear, COVID-19 is a new virus, and there is also no research linking elderberry to COVID-19 in any way. However, elderberry is a long-known immune nutrient remedy that may boost your body’s ability to prevent and recover from upper respiratory infections and illnesses.
One double-blind, placebo-controlled, randomized study on Sambucol (Sambucus nigra L.) standardized black elderberry extract against various strains of the influenza virus has found that elderberry has anti-viral properties and that it reduced the duration of flu symptoms by 3 to 4 days. While the study did find that elderberry may support the healthy immune system by increasing inflammatory cytokine production, there is no indication that it would lead to a cytokine storm.
Remember, a cytokine storm happens when your body creates excessive or uncontrolled levels of cytokines leading to hyperinflammation. Normal levels of cytokines, on the other hand, are essential for recovery. (36).

Elderberry is an Immune System Modulator
Elderberry is nature’s richest source of quercetin and this compound helps it act as an immunomodulator to help balance the immune system. One study examining the structures and the immunomodulating properties of the pectic polymers from elderberries has found that Sambucus elderberries contained immunomodulating polysaccharides and may benefit respiratory illness. Another study examined the immune-modulating effects of astragalus root and elderberry fruit extracts in bone marrow-derived murine dendritic cells by measuring IFN-β and other cytokines with ELISA and RT-PCR tests.
Results suggest that both elderberry and astragalus increased L. acidophilus-induced IFN-β production while decreasing pro-inflammatory reaction to E. coli. These findings suggest that both elderberry and astragalus offer antiviral and immune-enhancing benefits.
Furthermore, a meta-analysis of randomized controlled trials of 180 participants on the effectiveness of black elderberry for respiratory issues has found that elderberry supplementation may substantially reduce upper respiratory symptoms and may be beneficial for cold and flu recovery (37, 38, 39).
Again, cytokines are an essential immune response to fight off any kind of infection. None of the research indicates that elderberry would lead to excessive or uncontrolled levels of cytokines and hyperinflammation from a cytokine storm, instead, they show that elderberry may help to balance the immune system and offer the right amount of benefits.

Cytokines and AutoImmune Conditions
It is also important to note, however, that there have been some experimental models of human autoimmune diseases and observations in patients that showed that pro-inflammatory cytokines may increase autoimmune inflammation, and anti-inflammatory cytokines may help to reduce autoimmune inflammation and aid recovery from an acute phase of an autoimmune disease.
While the evidence regarding the relationship between cytokines and autoimmunity is still lacking, it may be possible that taking elderberry may not be the right choice in some cases of serious autoimmune diseases. Elderberry may also negatively interact with certain medications that decrease the immune system, including azathioprine, basiliximab, cyclosporine, daclizumab, muromonab-CD3, mycophenolate, tacrolimus, sirolimus, prednisone, corticosteroids, and others (40, 41).
Everything considered, there is no research evidence that suggests that elderberry would cause a cytokine storm in COVID-19, and current studies suggest that elderberry may be beneficial for your immune system.
However, as with every supplement, it is important that you talk to your healthcare practitioner before taking elderberry supplements, especially if you have an autoimmune condition, take any medication, or have COVID-19. Always watch your body’s reactions when taking any supplements, and back off if you experience serious side effects.
Final Thoughts on Immune Nutrients
Cytokines are an important part of your immune response. However, when your body releases excessive or uncontrolled levels of cytokines it results in hyperinflammation called a cytokine storm. A cytokine storm may lead to serious complications and even death in serious COVID-19 cases and other infections.
Optimizing your immune system is critical to improve your health and decrease your risk of a cytokine storm. I recommend that you take my recommended immune nutrients along with a nutrient-dense diet and a healthy lifestyle to optimize your immune system and overall health.

Functional Health Coaching
If you are struggling with your health or are just looking for lab testing to monitor key health metrics and strategies to optimize your health, then I recommend working with a functional health coach. A well-trained functional health coach will look at your health history, do a detailed analysis of current risk factors, signs & symptoms, and an in-depth interview process to find the root cause factors behind your health challenges.
Based on this data, your functional health coach will set up a lifestyle plan to help you improve your nutritional status and reduce major stressors and toxicities that are causing problems and use labs to help monitor outcomes. If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach.
Our website offers long-distance functional health coaching programs with our world-class team of health coaches. For further support with your health and other goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!





Wonderful,informative article Doc Jocker’s & staff!…
I love how you present health info and look forward to your book(s).
I’m sure that many folks will take notice with this one.
Thank you for going the ”extra mile”…
Rob Two Hawks
Thanks so much Rob!
I read an article recently that stated individuals taking ACE inhibitors for hypertension are at greater risk for Covid-19 complications. Dr. Jockers, can you comment on this? Thank you, I trust your research and advice and appreciate your website.
Yes that appears to be the case which is why the majority of the severe cases are people with comorbidities such as hypertension.
Hi, After reading the comment re: ACE inhibitors, I was considering stopping my Losartan, thinking it made me more susceptible to covid complications. So I googled (so glad algore invented the internet!) and came across this:
(from medicalexpress.com) By inhibiting ACE1, ACE inhibitors reduce the levels of ANG II and its ability to increase blood pressure and tissue injury. ACE inhibitors are commonly prescribed for patients with hypertension, heart failure and kidney disease.
Another commonly prescribed class of drugs, angiotensin receptor blockers (ARBs, e.g., losartan, valsartan, etc.) have similar effects to ACE inhibitors and may also be useful in treating COVID-19.
So, now I infer that the losartan may actually be beneficial? Which is good because none of my doctors will prescribe HCQ for me, even though I am 70 and diabetic, and WANT to take HCQ prophylactically.
I would be sure to discuss this with your physician. Unfortunately, I was notified today by the FDA/FTC that I have to pull this article down because they are saying it claims treatment, diagnosis, mitigation, or cure of COVID-19.
Dr. Jockers, my question, is it because one is taking an Ace Inhibitor/ARB that lets the virus in OR is it simply because you have hypertension? I’ve read the same articles stating this information early on, but have since heard and read that Ace Inhibitors protect the virus from coming in. This is all so confusing. You commented on this back in April, can you please give an update now that it’s been 4 months later? Any further information on this that you could possible share?
I would be sure to discuss this with your physician. Unfortunately, I was notified today by the FDA/FTC that I have to pull this article down because they are saying it claims treatment, diagnosis, mitigation, or cure of COVID-19.
CBD helps with inflammation. I am taking it for CIRS from mycotoxin poisoning. Has anyone tried it for Covid 19? I also use high dose melatonin and most of suggested nutrients.
Thank you for good article.
I have heard from others it can be effective for COVID-19 as well!
In your cytokine storm article you have a typo referring to COCID -10 when i think you meant COVID -19:
“Coronaviruses, and therefore the COVID-10 genome encode four major structural proteins: the spike (S), nucleocapsid (N), membrane (M), and envelope (E) proteins. The S protein is the one that helps the entry of the virus to the target cell in the body. Research has shown that about only about 75 percent of the COVID-19 S protein genome is the same as the SARS S protein genome, however, most of the amino acid residues needed for receptor binding are the same between the two viruses. This also suggests that the entry receptor, ACE-2, used by SARS is the same for COVID-19 as well.”
I mean you had “COVID-10” instead of COVID19.
Yes thank you for letting us know. We have now changed this!
informative article .. this helped me gain confidence about my vitamin c and d supplements
Great to hear that!
Great article. I posted it on fb, so I am now preparing for the expected pushback ! 🙂 Yesterday a friend said she doesn’t even believe CoVid is a virus and doesn’t believe in wearing masks. Friends at the other extreme are scared to leave their homes. Truth is elusive, but I’m grateful that you are doing your best to remedy that, even if part of the truth today is “we don’t know yet”. I’m excited to see your tests thru LabCorp, too!
Yes so true Janet. Unfortunately, I was notified today by the FDA/FTC that I have to pull this article down because they are saying it claims treatment, diagnosis, mitigation, or cure of COVID-19.
Dr. Jockers
I read all your informative booklets and use all the information! I forward this information to all my contacts! You definitely go more than the extra mile!!!
Thanks for all your support! Blessings to you and your family!
Hey Dr, thanks for the article, some good information. For elderberry, wouldn’t it’s modulatory effects depend on one’s preexisting condition i.e. viral vs bacterial infection, acute vs chronic? e. g. wouldn’t someone with a chronic bacterial infection have high th1 and, since elderberry increases th1, taking it would worsen this person’s condition? Otherwise, if you say infections are associated with underractive immunity than elderberry might help?
This is a good question. Elderberry has an immunomodulatory impact and isn’t necessarily a specific driver of Th1. It hasn’t been shown to drive up Th1 in individuals with elevated Th1 activity.
Thank you! And great that it is again online, now I saved it :), I have been looking shortly ago for the article from the last year wiht the information about Lavendel & Coconut oil using them for the breast & feet, but I couldnt find it. Is there any link for that info/articel? thank you in advance
Not sure exactly what you are looking for here.
Wow! What an informative, well-compiled article, with helpful pictures. Thank you so much.
Great to hear this! Thank you for the feedback!
What would you recommend to mitigate the effect of vaccine? Asking for a friend who either has to take a jab or quit work (school in Chicago).
Hello Margaret,
Here is our protocol for those who want to reduce vaccine side effects. First off, if possible, take these starting at least 1 week before taking the vaccine and then for 60 days after taking the vaccine.
Proteo Enzymes: Take 5 caps – 3x daily away from meals (this will break down the spike protein and the inflammatory proteins)
Glutathione Boost: Take 2 pumps – 2x daily before meals (powerful antioxidant – protect you from oxidative stress)
Bioactive Carbon MetChem: Take 2 caps – 3x daily with or without food (powerful binder that will pull out mRNA, glyphosate, heavy metals, etc. from within the cells)
You can find these on our online store and use the coupon code Jockers10 at checkout to save 10% on your order.
Team Jockers, thanks for continuing to question your own beliefs regarding more complex topics like the potential harm of certain neutraceuticals for specific conditions like those hyperactive immunity. My health coach warns against those like me, with a long-standing bacterial infection (th1 dominance), in taking things like beta glucans, echinacea, and elderberry. Can you explain in more detail of the research and clinical evidence you’ve seen about the pros and cons of these for th1 dominance? It’s been very difficult for me to find a consensus amongst online articles written by clinicians and researchers. Thanks for all you do, you’re amazing! p. s. I don’t think I’ve been able to get a notification for past replies despite seeing at least one after later reading the q+a. Please feel free to email me the notification andor response.
Hello KP, yes we have tried to research this as well and haven’t found any good info. It is a theory that has circulated in the natural health world for the last 10 years but dosn’t have a true scientific basis. I haven’t seen it be a factor clinically as these herbs and compounds act to modulate and balance the immune system unless the individual has a unique sensitivity or allergy to the herbs or compounds, in which case, it would drive up inflammation.
Thank you, Dr. Jockers, for this report. Cytokine storm is of interest to me: I see it as the same as immune system dysfunction that I live with. It also seems to be the same as acute intermittent porphyria, and disorder of
olfaction (of the smell system) that presents as an extraordinary hypersensitivity to smells, odors, fumes and to certain substances. Many of the helpful items you cite here as helpful in dealing with cytokine storm also are helpful in quieting episodes of these named illnesses. You leave out grapefruit that is a crucial helper. Have you ever done any writing on these three illnesses I name? Thank you again for this report.
Yes for sure. Thanks for sharing!
Thanks, Dr. Jockers, for your reply. Can you give me links or titles to any related writings you’ve done on immune system dysfunction and acute intermittent porphyria?
Thank you.