 Cholesterol: What is It and What are Healthy Levels?
Cholesterol: What is It and What are Healthy Levels?
One of the most confusing topics for many people is cholesterol. It is often portrayed as bad for your health, but cholesterol is actually essential for good health. Cholesterol is one of the most important molecules in your body and serves many necessary functions.
This article will explain the importance of cholesterol and how to determine if your levels are healthy. I will also discuss the top 10 factors that affect cholesterol and lipid ratios and ways to improve these numbers.
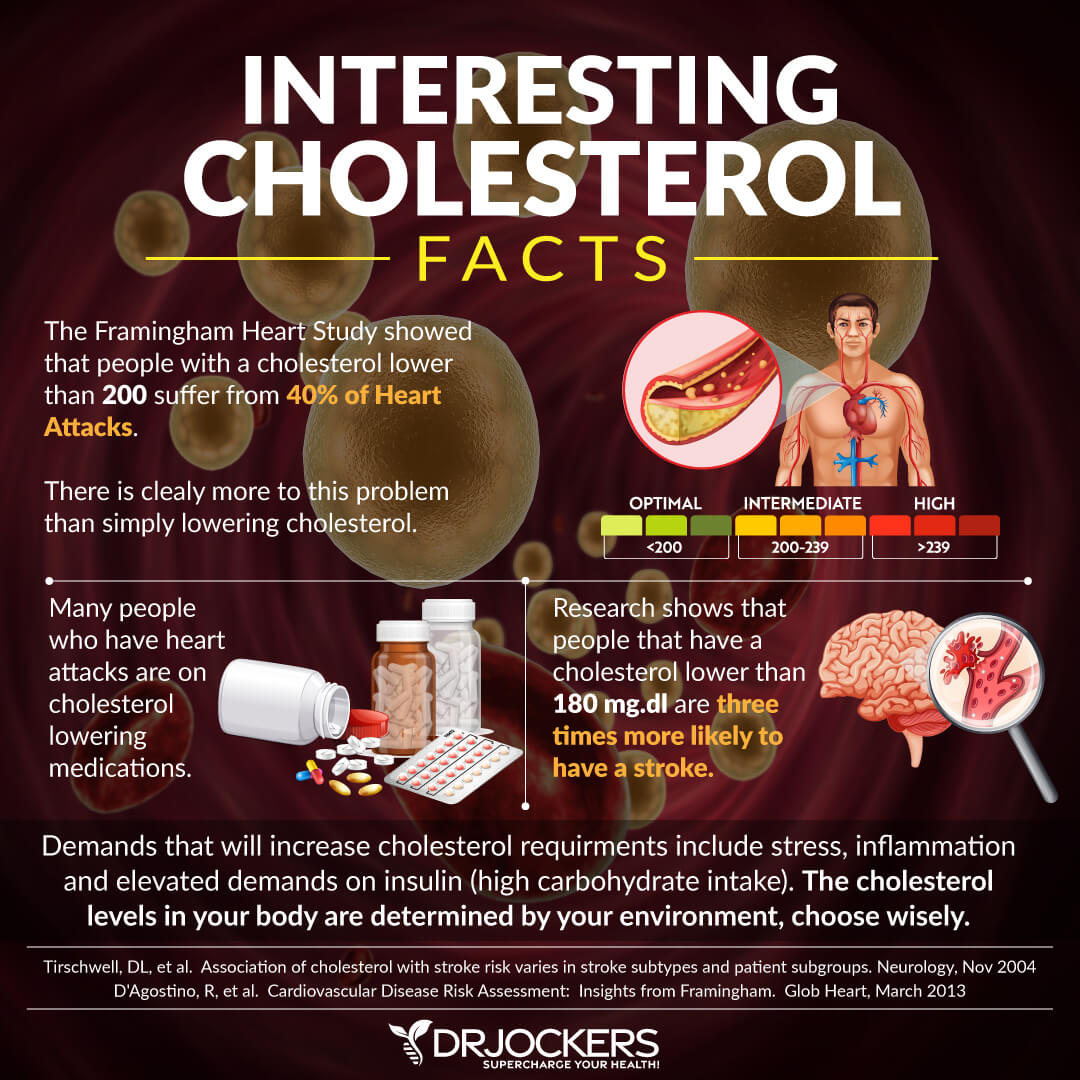
What is Cholesterol?
Cholesterol is a waxy substance found in your blood that is needed by the body to build healthy cells. It is produced in the liver or consumed in the diet from animal products.
Cholesterol is a lipid. Lipids are fats and fatty substances used by the body as a source of energy. Lipids include cholesterol, triglycerides, high-density lipoprotein (HDL), low-density lipoprotein (LDL), and very low-density lipoprotein (VLDL).
Dyslipidemia is when lipid levels are outside the normal range. It has a direct relationship with coronary artery disease (1). Dyslipidemia is characterized by:
- Hypercholesterolemia – increases in cholesterol only
- Hypertriglyceridemia – increases in triglycerides only
- Hyperlipidemia – increases in both cholesterol and triglycerides.
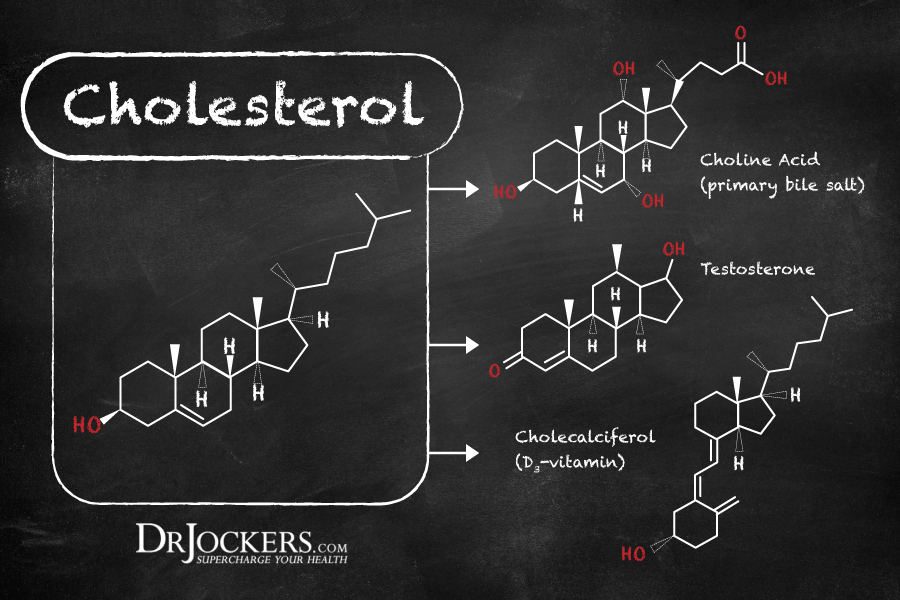
Importance of Cholesterol
Having good levels of cholesterol in the body is critical for good health. Cholesterol serves a number of important roles in the body.
- Cholesterol is a critical structural element in certain tissues, including the brain and nervous system. Around 25% of the cholesterol in our bodies is found in the brain. In fact, high cholesterol levels are linked to better cognitive function in the elderly (2).
- Cholesterol is a transport molecule to shuttles fat soluble nutrients into cells to be utilized appropriately.
- Cholesterol is an essential building block for hormones, including progesterone, estrogen, testosterone, cortisol, and vitamin D.
- Cholesterol is used by the body to make bile acids to help digest fats.
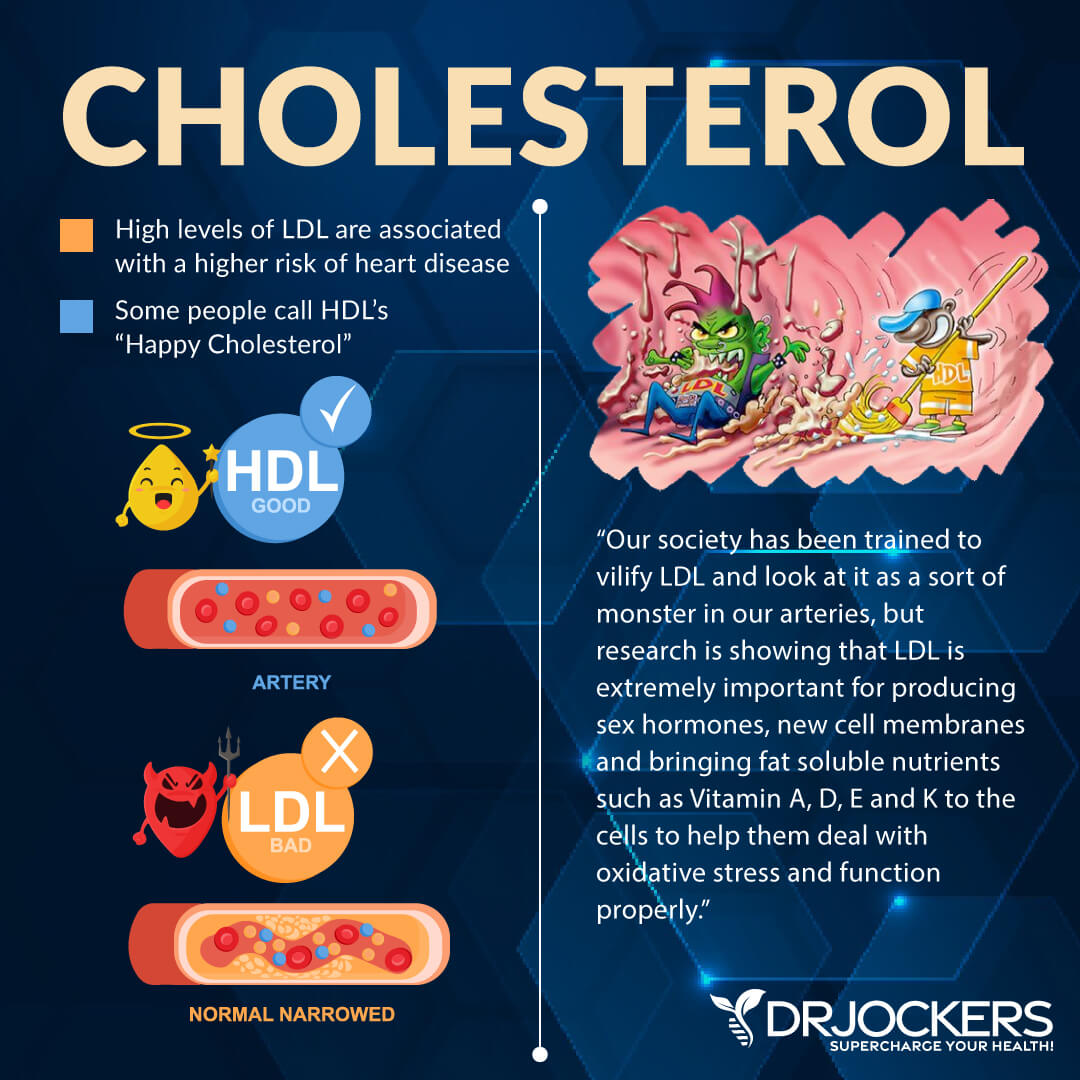
Subtypes of Cholesterol
Cholesterol is carried through the blood attached to proteins. This combination of proteins and cholesterol is called a lipoprotein. These lipoproteins are the transport mechanisms for cholesterol and fat. It has a phospholipid shell that acts as an emulsifier so the fat and blood will mix.
There are different types of cholesterol based on what the lipoprotein carries: LDL, VLDL, and HDL.
LDL Cholesterol
Low-density lipoprotein (LDL) transports mostly cholesterol. The primary role of LDL is to transport fat-soluble nutrients into cell membranes for use. LDL also helps to deliver saturated fat to the cell membrane.
While LDL is generally considered “bad” cholesterol, it is more complex. There are different types of LDL particles depending on their size. LDL particle size is important for determining whether LDL may contribute to heart disease or be protective of it.
LDL levels can be elevated in individuals with low thyroid activity because T3 helps sensitize the LDL receptor on the cell membrane. Lower active T3 will cause an inability of the LDL particles to dock on the cell membrane, dropping the cholesterol and fat soluble nutrients into the cell. So the body adapts and increases the amount of overall LDL cholesterol, similar to how insulin goes up in response to insulin resistance.
Ideal Range: 100-200
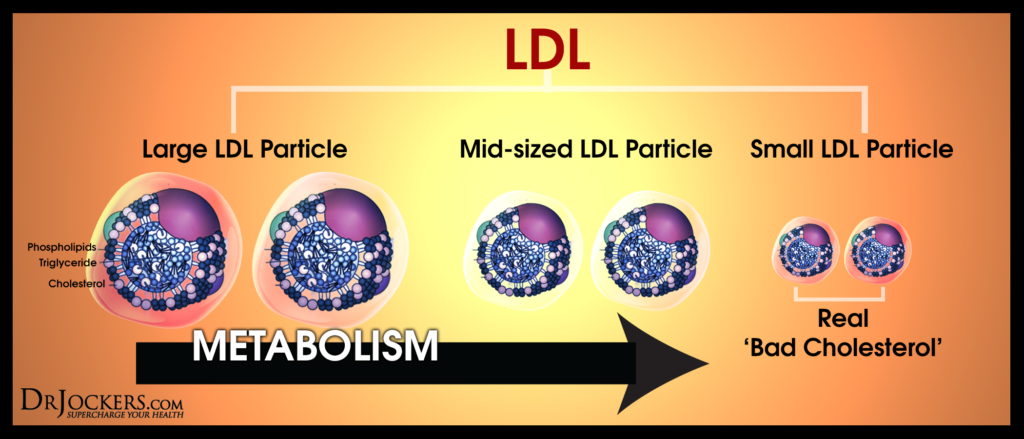
Pattern A
Pattern A LDL has a larger particle size. This pattern tends to carry more fat-soluble nutrients and antioxidants to protect the body from oxidative stress. Pattern A is more cardioprotective. Lower insulin and HbA1C levels are associated with these large, buoyant particles.
Pattern B
Pattern B LDL has a smaller particle size and is more prone to oxidation. It is small enough to enter the endothelial lining of the artery, where it can oxidize to form plaque. There is a high association between these small, dense particles and cardiovascular disease. Higher fasting insulin and HbA1C levels are associated with these small dense particles. These particle sizes can be looked at in closer detail in the NMR test.
 VLDL Cholesterol
VLDL Cholesterol
Very low-density lipoprotein (VLDL) carries mainly triglycerides to your tissues. VLDL is similar to LDL, but LDL carries mostly cholesterol instead of triglycerides. The triglycerides make VLDL denser than LDL. Once VLDL is released, enzymes in the bloodstream interact with triglycerides and change the lipoprotein from VLDL to LDL.
Ideal Range: 5-30 mg/dl
HDL Cholesterol
HDL or high-density lipoprotein has a high cholesterol to protein ratio (45-50% protein). It has the primary role of “SWEEPING UP” LDL particles and transporting them to the liver for recycling. It is important that LDL be cleared from the blood efficiently because of its high susceptibility to oxidation. LDL that remains in the bloodstream longer increases inflammation and your risk of heart disease.
Ideal Range: 55-80
Levels above 100 can indicate chronic inflammation or an active infection in the body.

Triglycerides
Triglycerides are a type of fat (lipid) found in your blood that helps to supply your body with energy. They are necessary for health, but can contribute to heart disease and stroke when elevated. The optimal range for triglycerides is 40-80.
Lipoproteins transport triglycerides to the cell membrane. There, they are broken down into fatty acids and metabolized to make adenosine triphosphate (ATP). Cells use ATP for energy. Triglycerides will be high in individuals with high insulin levels, insulin resistance, and in fatty liver disease.
Ideal Range: 40-80
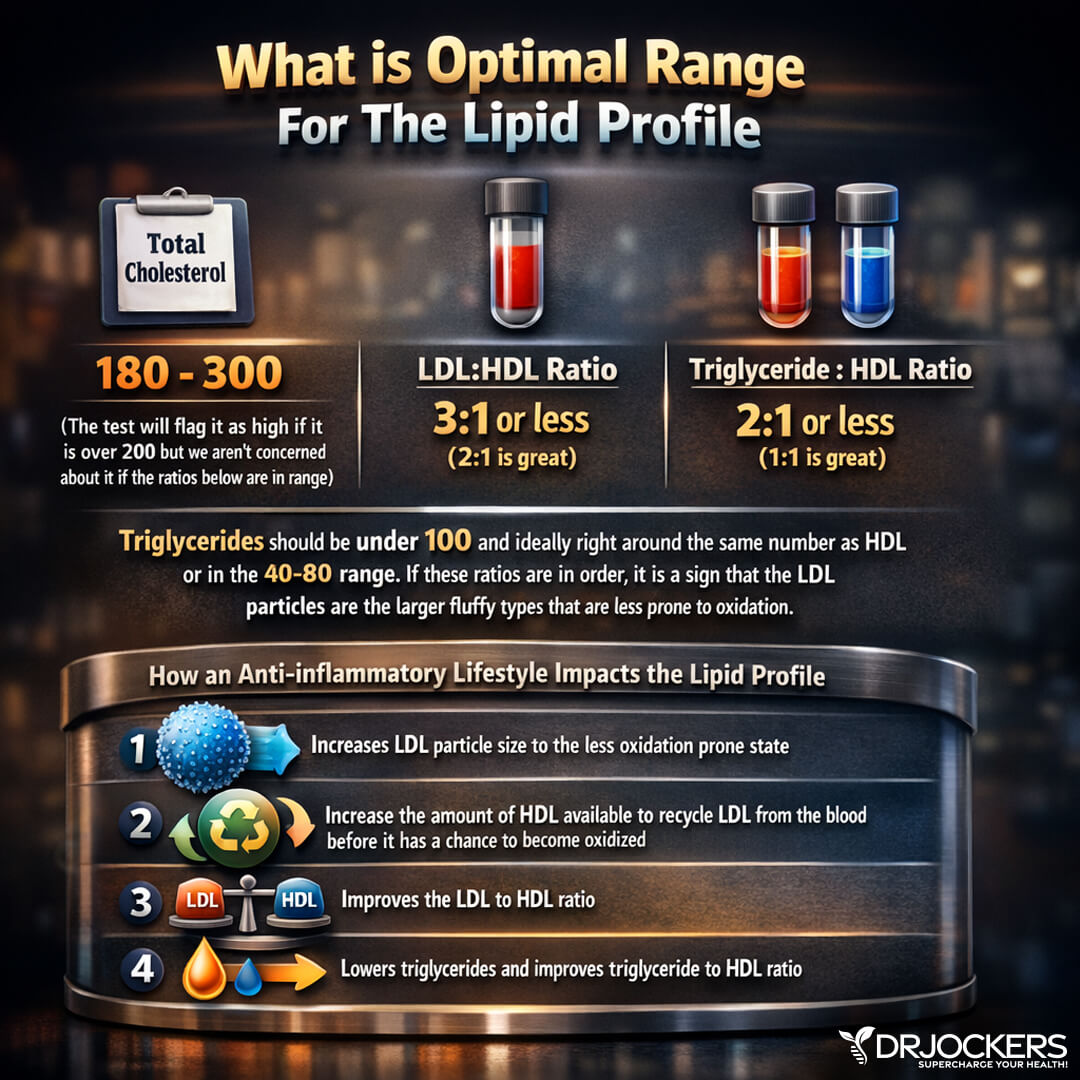

Healthy Ratios
There are important ratios to consider when analyzing cholesterol levels. Having a balanced ratio of LDL to HDL and triglycerides to HDL is essential for good health.
LDL: HDL Ratio: 3:1 or less (2:1 is optimal)
Triglyceride: HDL Ratio: 2:1 or less (1:1 is optimal). Higher triglyceride and lower HDL levels are typically an indication of insulin resistance and high fasting insulin levels
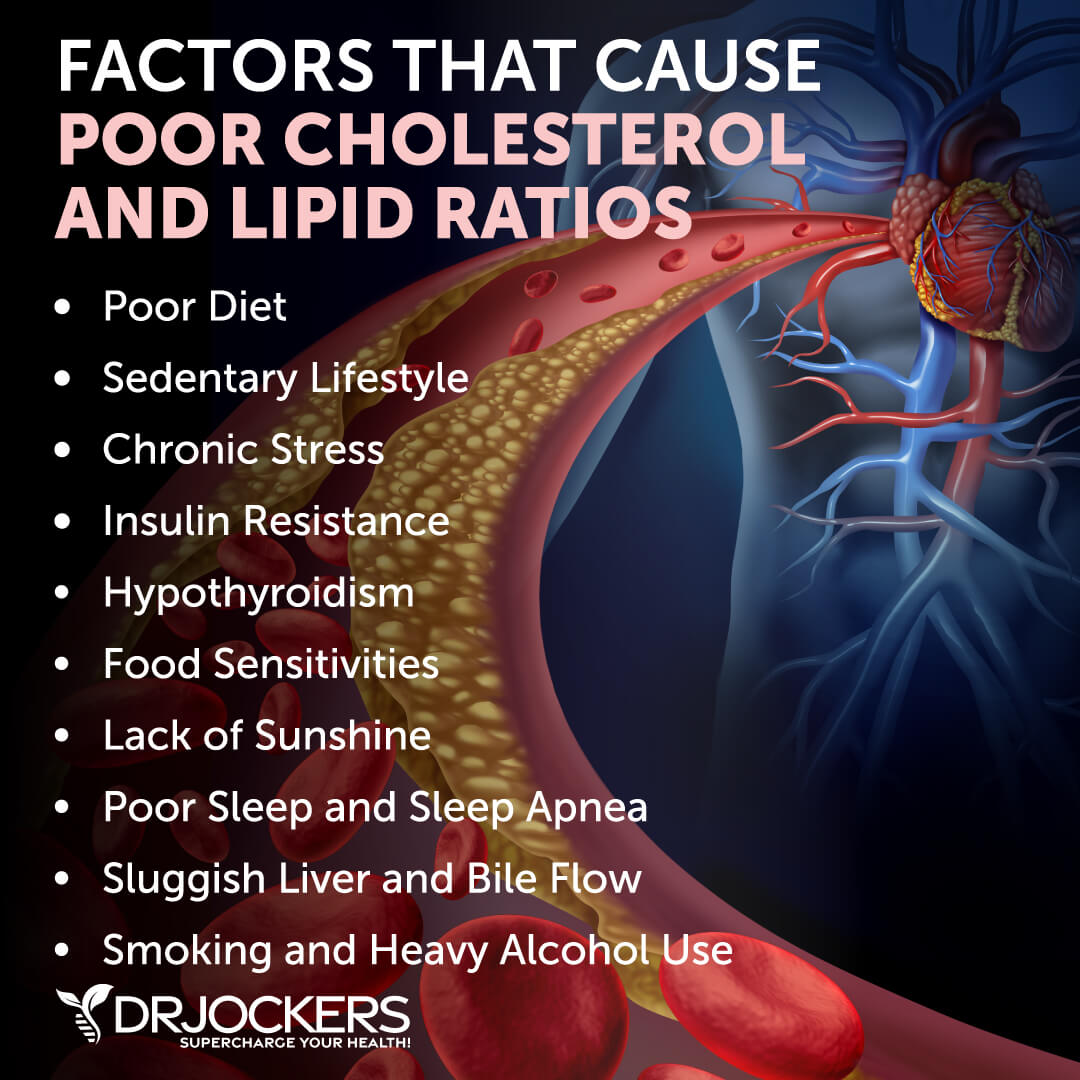
Factors that Cause Poor Cholesterol and Lipid Ratios
Poor cholesterol and lipid ratios are often the result of unhealthy lifestyle choices such as a poor diet and inactivity. For some people, the buildup of cholesterol and triglycerides in the blood may arise from medical conditions such as hypothyroidism.
1. Poor Diet
A poor diet is one of the leading causes of cardiovascular disease (3). It is estimated that between 25%-60% of caloric intake for people all over the world is ultra-processed foods. In studies, consuming processed foods has been associated with a higher risk of lipidemia, obesity, and overall cardiovascular disease and other health conditions.
A poor diet also increases inflammation in the body, which adversely affects cholesterol and lipid levels. Inflammation alters lipid metabolism. These changes include decreases in HDL cholesterol and increases in triglycerides and LDL levels (1). Inflammation also adversely affects lipoprotein function. LDL is more easily oxidized, and the ability of HDL to prevent oxidation is limited.

2. Sedentary Lifestyle
A sedentary lifestyle is associated with poorer lipid profiles (4). Spending too much time in sedentary behaviors, such as sitting, watching TV, or using a computer, has many negative health outcomes that affect cholesterol and lipid ratios. One of these is excess weight.
Over the long term, a lack of exercise can lead to obesity, which can significantly boost high LDL cholesterol and triglyceride levels (5). Obesity can also elevate the amount of small, dense LDL particles in the bloodstream.

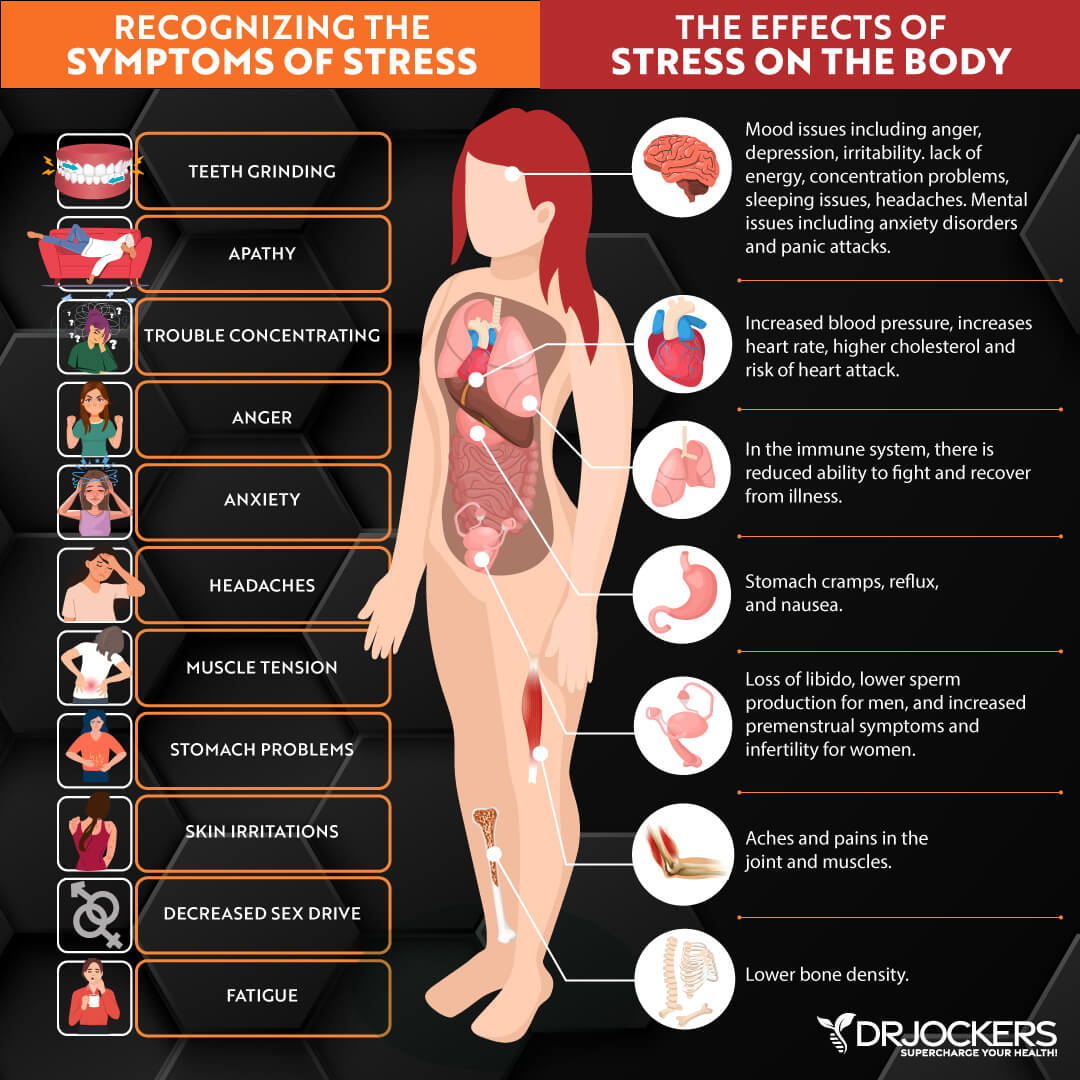
3. Chronic Stress
Your level of stress can have an impact on your cholesterol levels. In response to stress, your body releases hormones called cortisol and adrenaline. This is part of the “fight or flight” mechanism the body adopts to protect itself. These hormones, in turn, stimulate the release of triglycerides and free fatty acids, which can increase levels of LDL.
Stress may also lead to elevated cholesterol levels indirectly. Higher stress levels are linked to eating an unhealthy diet, exercising less, and a higher body weight. These factors can contribute to higher cholesterol.
4. Insulin Resistance
Insulin resistance and type 2 diabetes have been constantly associated with high triglycerides and low HDL cholesterol levels. Cholesterol synthesis is increased, and cholesterol absorption is decreased in people who are insulin resistant.
The classic pattern here is high fasting insulin, high LDL cholesterol, low HDL, and high triglycerides. The blood sugar and HbA1C can range and may be normal and healthy or not, depending upon what stage of insulin resistance they have.

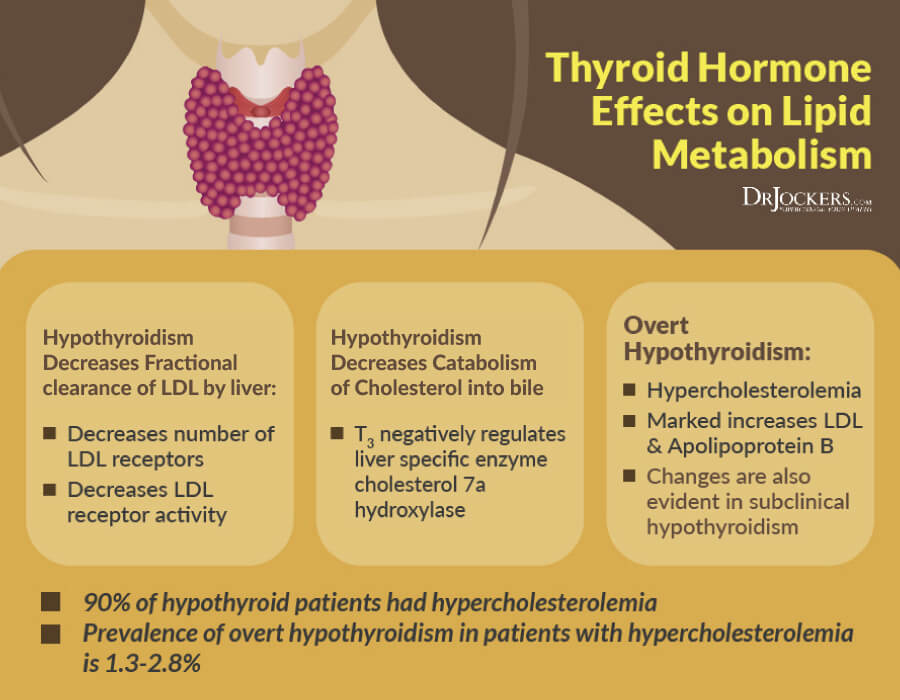
5. Hypothyroidism
Hypothyroidism, or low thyroid function, is linked to hyperlipidemia (6). Studies show that cholesterol levels increase as thyroid function declines. Having both hypothyroidism and dyslipidemia is closely linked to the development of coronary heart disease.
When thyroid hormone levels are low, the liver cannot process as much cholesterol as it should. The body does not break down and remove LDL cholesterol as efficiently, leading to high LDL levels. In addition, active T3 helps to sensitize the LDL receptor on the membranes of all the cells. Low free T3 levels will result in a form of LDL resistance (similar to insulin resistance) where more LDL will be produced in order to get the nutrients it carries to the cells of the body.
6. Food Sensitivities
A food sensitivity is an immune-mediated response to certain foods. When you have food sensitivities, your immune system reacts to certain foods as a threat, amplifying the immune response.
Repeated exposure to the foods causes inflammation and other health problems. Lipid metabolism is altered during acute and chronic inflammatory responses.

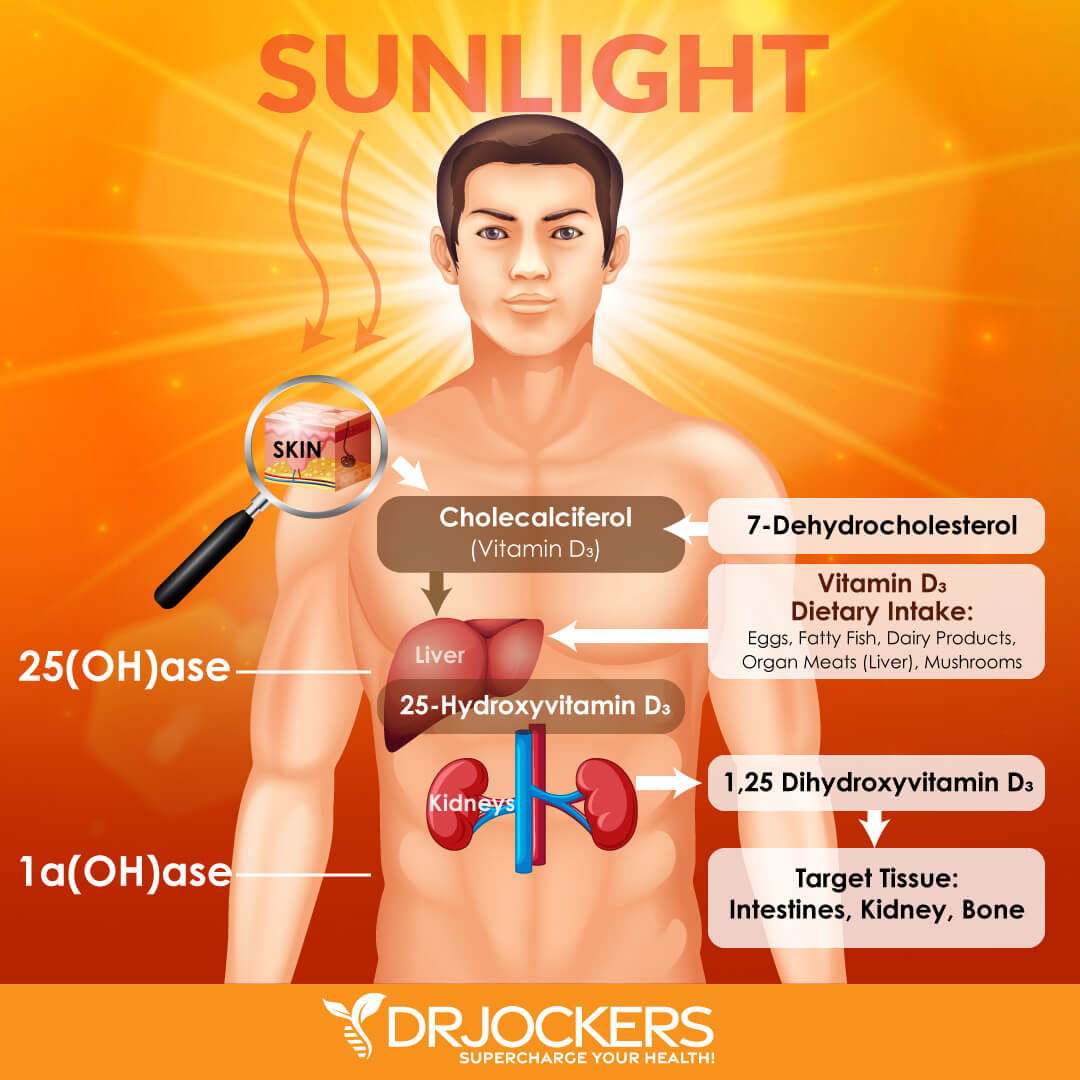
7. Sunshine Deficiency
Sunlight deficiency can increase blood cholesterol levels by allowing cholesterol synthesis rather than vitamin D synthesis (7).
Both vitamin D and cholesterol are derived from squalene. With sun exposure, squalene is converted into 7-dehydrocholesterol and vitamin D. In the absence of sunlight, squalene is diverted into the formation of LDL cholesterol.

8. Poor Sleep and Sleep Apnea
Studies have shown that poor sleep is associated with abnormal lipid profiles in women. For men, sleeping over 8 hours a night is associated with a lower risk of high LDL cholesterol levels (8).
Sleep apnea is linked to unhealthy lipid levels. Sleep apnea is a serious condition in which a person’s breathing stops and starts during sleep. Obstructive sleep apnea is the most common type of sleep apnea. With obstructive sleep apnea, breathing stops because the throat muscles relax, and the airway narrows as you sleep.
There is a strong association between higher total cholesterol, lower HDL, higher LDL, and elevated triglycerides and several measures of obstructive sleep apnea severity (9). The negative impact of sleep apnea on lipid levels may in part explain the association between sleep apnea and increased risk of cardiovascular disease.

9. Sluggish Liver and Bile Flow
The liver creates cholesterol for hormone production and tissue healing. When HDL carries cholesterol from other parts of the body to the liver, the liver is responsible for breaking down and eliminating cholesterol from the body.
The liver removes cholesterol from the body by converting it to bile salts and putting it into the bile so that it can be eliminated in the feces. A sluggish liver and poor bile flow will inhibit this process.
10. Smoking and High Cholesterol
Smoking is a leading cause of high cholesterol and triggers many problems that contribute to heart disease. Smoking decreases the level of HDL cholesterol and increases the level of triglycerides in the blood. It promotes plaque buildup on the walls of the arteries and leads to the formation of blood clots and inflammation.

Strategies to Improve Cholesterol and Lipid Ratios
1. Anti-Inflammatory Nutrition Plan
One of the best strategies for improving cholesterol and lipid ratios is to consume an anti-inflammatory diet. An anti-inflammatory diet removes pro-inflammatory foods and includes organic, non-GMO vegetables and fruits, healthy fats, and clean protein.
This diet reduces inflammation, stabilizes blood sugar, reduces toxic load, provides necessary nutrients, and supports healthy blood pH levels.
Foods to Exclude
Foods to eliminate on an anti-inflammatory nutrition plan are highly inflammatory foods. These include refined sugars and grains, food additives and preservatives, GMO foods, and foods with pesticides and toxic debris.
Additional foods to avoid are meat and dairy from conventionally raised animals, farmed fish, processed foods, hydrogenated fats, and highly processed vegetable oils, such as canola, grapeseed, and safflower. These foods upregulate inflammation, create extra acidity in the tissues, and cause poor cholesterol and lipid ratios.

Foods to Include
The foods to eat on an anti-inflammatory diet are whole, unprocessed foods. Always choose grass-fed meats, wild-caught fish, and pastured eggs. Include a variety of low-carbohydrate, low-glycemic, colorful fruits and vegetables.
Vegetables and fruits have abundant amounts of antioxidants and phytonutrients. Antioxidants can slow or inhibit the LDL oxidation process that leads to plaque development in your artery walls, damage to vessel linings, and heart disease. Excellent choices include vegetables like broccoli, cucumbers, asparagus, and leafy greens. Low glycemic fruits include berries, lemons and limes, grapefruit, and Granny Smith apples.
Quality fats are a very important part of an anti-inflammatory diet. Healthy fats are found in coconut, olives, avocados, and their oils, and in grass-fed butter and ghee. Omega-3 fatty acids and conjugated linoleic acid (CLA) are found in wild-caught salmon and grass-fed beef and dairy. These healthy fats are an efficient source of fuel to combat inflammation and maintain healthy cholesterol levels.
Studies have found that a higher fat diet is associated with a significant increase in LDL particle size and a significant decrease in the proportion of small LDL particles. This can occur in as little as three days of eating a high-fat, low-carbohydrate diet. HDL cholesterol can also significantly increase on a high-fat, low-carb diet (10). To learn more about the relationship between the amount of saturated fat and cholesterol in the diet and the risk of developing heart disease, read this article.

2. Intermittent Fasting
Intermittent fasting is a fantastic strategy for improving your cholesterol levels. In addition to supporting the digestive healing process, intermittent fasting boosts the immune system, stimulates cellular autophagy, improves genetic repair mechanisms, improves insulin sensitivity, and reduces the risk of chronic diseases (11).
Start with a simple fast of 12 hours for 1-2 weeks and see how your body responds. This short fast is basically from dinner until breakfast the next day. You can increase your fasting time as your body adapts to not eating at certain times of the day. For the best intermittent fasting strategies and information on how to fast, check out this article.

3. Regular Exercise
Regular exercise is beneficial for improving cholesterol levels (12). Performing moderate intensity aerobic exercise, resistance training and high intensity interval training (HIIT) can help boost HDL cholesterol while decreasing LDL and triglycerides.
Try to perform one of these forms of exercise most days of the week and build more activity into each day. In addition to improving cholesterol, exercise can help to increase your energy levels, burn fat, remove excess weight, and strengthen your muscles.

4. Watch for Food Sensitivities
Around 45-75% of individuals have food sensitivities. It is important to identify any food sensitivities and remove these foods from your diet for a period of time.
Food sensitivities can be hard to identify. This is because symptoms of food sensitivities are usually delayed up to 72 hours after consuming the offending food. For information about different methods of testing for food sensitivities, check out this article.

5. Support Thyroid Health
Optimal thyroid function is important for healthy cholesterol levels. There are many strategies you can incorporate to boost thyroid health.
Supporting your liver and digestive system, managing stress, and eliminating inflammatory foods can be helpful for improving thyroid function. It is also important to get specific nutrients for thyroid health. Selenium, iodine, zinc, vitamin C, bioflavonoids, vitamin D3, and vitamin K2 are all beneficial for thyroid health. In some cases, taking a specific thyroid hormone medication or supplement that has thyroid glandulars in it can be very helpful.

6. Reduce Stress
It is important to take steps daily to reduce the stress in our lives. Stress can be physical (such as infections) and emotional.
Following an anti-inflammatory, healing diet and balancing your blood sugar levels are two effective strategies for reducing stress on the body. Other powerful techniques are grounding, deep breathing exercises, sunlight exposure, Epsom salt baths, and dry brushing. Adaptogenic herbs such as those found in Cortisol Defense can help support the stress response.

7. Get Regular Sun Exposure
The sun activates cholesterol to form vitamin D. Regular sun exposure may help improve cholesterol levels.
In areas where there is sufficient UVB exposure, there are several factors to consider in determining how much sun exposure is appropriate. These factors include the portion of skin exposed to the sun, the color of your skin, and the strength of the UV rays.
If 60% of the body is exposed to the sun, it is ideal to seek 10,000 to 20,000 IU of vitamin D3 from sun exposure. Intentionally sunbathe no less than 3 times per week according to the following recommendations based on your skin color:
- Light skin = 15-20 minutes daily
- Medium Skin = 25-30 minutes daily
- Dark Skin = 40-45 minutes daily

8. Optimize Sleep Habits
Practicing good sleep habits and addressing sleep apnea are important strategies for improving cholesterol levels. For good sleep, diet is important. Consuming an anti-inflammatory diet can help to balance your blood sugar and correct nutrient deficiencies.
Other strategies for better sleep are sticking to a sleep schedule, getting sunlight during the day, avoiding artificial light, blacking out your room with blackout curtains, using a sleep mask, and reducing stress. Supplementing with magnesium, such as Brain Calm Magnesium, may also be helpful. For more information on the causes of poor sleep and how to reverse it, check out this article.
Strategies for improving sleep apnea include losing excess weight, getting regular exercise with resistance training and high intensity intervals, boosting omega-3 intake, optimizing vitamin D and magnesium levels, performing strengthening exercises for your mouth, throat, and breathing, practicing nose breathing, and changing your sleep position from your back to your side.

9. Support Liver Health and Bile Flow
The liver is central to the regulation of cholesterol in the body. It is important that the liver be functioning optimally for healthy cholesterol levels.
Consuming liver healthy foods such as the liver from organic, pastured animals, cruciferous vegetables, beets, and eggs is important for supporting the liver. Other strategies for liver health include improving gut health, optimal hydration, intermittent fasting, and castor oil packs.
Using herbs and nutrients to support the liver can also be helpful. Plant Based Kidney Health is a bioactive carbon product that focuses on drainage and immune support throughout the kidneys and liver. It contains milk thistle, along with NAC, parsley, gynostemma, collinsonia root, beet root, and marshmallow root. Milk thistle protects the liver from damage and enhances the detoxification process.
Improving Bile Flow
Good bile flow is also important for regulating cholesterol levels. Bile is a digestive fluid that emulsifies fats and creates fatty acids that can be absorbed and used by the body.
Supporting liver function, gallbladder health, bile flow formation, and bile duct motility is critical for good bile flow.
Bile Flow Support (here) is my go-to for boosting bile formation in the liver. It contains the necessary amino acids along with herbs like dandelion that not only provide the nutrients necessary for bile but also stimulate the proper flow from the gallbladder.
 Bonus Strategy
Bonus Strategy
A bonus strategy for improving cholesterol and lipid ratios is to use GI Detox or Activated Charcoal. Activated charcoal is one of the oldest detoxifying remedies. It will bind to and help remove excess bile and cholesterol from the body.
Activated Charcoal or GI Detox
I recommend Activated Charcoal or GI Detox to support your liver and gallbladder. Activated charcoal is one of the world’s oldest detoxifying remedies, with a history going back over 3000 years, and has been used in Chinese Medicine, Ayurvedic medicine, and Western medicine. It is a fantastic absorbent agent that binds and eliminates toxic bile, excess cholesterol, and other toxic substances.
GI Detox is a toxin binder that is formulated to provide broader activity than a single-ingredient product. Zeolite clay, activated charcoal, and silica are all binding agents with proven efficacy.
The other nutrients in G.I. Detox™+ support healthy digestion and elimination. The full-spectrum binding of G.I. Detox™+ provides a simple solution for environmental and internally produced detoxification. It supports healthy detoxification and full-body cleaning, reduces bloating and gas, helps the clearance of mold metabolites, supports mental clarity, and allows a more pleasant cleansing experience.
I recommend taking it one to two hours before or after meals to help bind to toxic bile and cholesterol in the gut and help to remove these through the bowels. One caveat with these binders is that they may reduce bowel motility. So be sure to hydrate well throughout the day and consider magnesium supplementation to help improve bowel function if necessary.
Additionally, don’t take charcoal with medications as it may bind to them and make them less effective.
Testing Cholesterol Levels
It is very important to test your cholesterol levels. The Comprehensive Blood Analysis is a detailed blood test that includes a complete lipid panel. It measures total cholesterol, LDL, VLDL, HDL, and triglycerides.
The Comprehensive Blood Analysis assesses your immune function, thyroid function, blood sugar regulation, liver function, nutritional deficiencies, and much more. In addition to the lipid panel, it includes a Complete Blood Count, Complete Metabolic Panel, Urinalysis, Iron Panel, and Thyroid Panel.
The Comprehensive Blood Analysis should be run regularly as a preventative measure and to monitor your cholesterol and triglyceride levels. Information about the Comprehensive Blood Analysis and how to order can be found here.

Final Thoughts on Cholesterol:
Optimal levels of cholesterol and triglycerides are important for overall health. It is helpful to look at lipid and cholesterol ratios to determine if your levels are healthy.
Many factors influence your cholesterol and lipid ratios. Most of these factors are influenced by your diet and lifestyle choices. However, there can also be an underlying medical reason for altered lipid profiles. Be sure to test your levels regularly and use the diet and lifestyle strategies discussed above to help keep your cholesterol levels within healthy ranges.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website offers long-distance functional health coaching programs with our world-class team of health coaches. For further support with your health and other goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!







Thank you for this excellent article, so clearly written and understandable.
Thank you Franklin! Your feedback is appreciated! Blessings!
Thank you for the well-explained article on cholesterol.
Absolutely! Thanks Vald! Blessings!
Brilliant explaining relationship between cholesterol, lipids, thyroid, liver(I’ve had tiny gallstones for 20+years which I control with diet, milk thistle & diluted Bragg’s), sunshine D3 makes sense, I avoid it after multiple dermatological procedures. Thank you so much, wish I had a Dr like you near me 06811, Danbury, CT. You are a blessing 🙏
Thank you for your kind words Shari! Blessings!
Nice article. Glad you discussed NMR Lipid Profile.
Two other tests that should be run before getting excited about cholesterol are Homocysteine (a major cause of oxidizing LDL) and oxidized LDL (the harmful form of cholesterol).
In medical practice we used these ratios.
TC divided by HDL ideally = <5/1
LDL divided by HDL ideally = <3/1
but the most important one is Triglycerides divided by HDL and
must be 2 or less.
Nice job.
Bill
Thank you for those ratios, very helpful.
I understand all of this information but never see issues discussed regarding complex heritable factors such as low HDL and LDL and mutations of mthfr. Should people like me do keto? I understand a diet low in carbs is essential, high in fiber, healthy environmental habits, but I can’t piece together what I never see. I use methylfolate, vitamin D 10,000iu, many nutrtional supplements, eat my greens, always moving, have antiphospholipid syndrome, and lupus SLE. Just bad genes! And bad luck. Giardia for 3 years which I mostly healed from except I require a huge amount of high quality probiotics. I developed mast cell activation syndrome resulting in high blood pressure after necrosis of my hip following a fall that also resulted in my lead levels rising. I added copper to my regimen and quercitin, did some chelation therapy and the mast cell is much better. I am continuing chelation . I haven’t addressed my liver’s polymorphisms.
I will never be able to achieve the goals for HDL and ratios for cholesterol nor get my triglycerides down to 80 without better understanding. And maybe not even then
My point is my body has been under stress for most of my life. I would like to do keto but get mixed messages. Currently following mostly Mediterranean Diet although I can’t eat fish at all except anchovy.
Hello Tyler – I would consider mold toxicity or heavy metals driving inflammation in your body!
As a fellow wounded warrior, life time nutritionist by passion and profession, I find the articles here on the Dr Jockers site to be superior in all areas. So much gratitude to you. Dr. Jockers and your staff. God Bless!!
Thanks for all your support Maggie! Blessings to you!
Excelente, muy, muy buenno el articulo
Everything is understandable and I also master science. I still underwent bypass surgery. I ate a low carb diet and did sports and fasting and still have hyperlipidemia. So what do you do to not take beta blockers or lower your cholesterol?
Yes be sure to follow the info in this article to get your ratios proper. The most important thing is your triglyceride:HDL ratio – if that is close to 1:1, than do not worry about total cholesterol or LDL cholesterol numbers.
This sounds all good, been there, done that. I was on meds for LDL but stopped due to painful bruises. I don’t eat junk food but I’m a low income senior and eating grass fed meats is beyond my budget (grass fed used to be all meats as I grew up until things changed). I’m not deficient in any vitamins as I take quality supplements daily. Exercise is a problem due to sciatica, insomnia has been a lifelong thing. I take cbd products for it.
Anyway, I’d be in the poor house if I bought all your stuff but it’s interesting reading sometimes..
Thank you for this article. It addresses many issues I had questions about. Great information!
Great article! I don’t see any recommended values for the different sizes and what it could mean if they are out of range:
LDL Peak Size
HDL, Large
LDL, Small
LDL, Medium
What should we be looking for there? Thanks!
Yes here is some helpful information: https://drjockers.com/nmr-heart-disease-risk/
My total cholesterol has always been above 200 but my old Drs never put me on a statin drug because my HDL cholesterol was always 60 or higher. My current doctor wants me to go on a statin drug because my recent lipid panel showed a total cholesterol of 207, LDL is 131, HDL is 60 and triglycerides are 70. In Jan the readings were 210, 120,69 and 119 respectively. I started taking psyllium fiber daily to bring the LDL down. Instead, it went up from 120 to 131 but the triglycerides came down greatly, from 119 to 70. What would cause that to happen? The ratios look good according to your article, but my current PCP says I am at risk for a stroke based on my age (76) and other factors she puts into some computer program she has.
No these are great ratios. Getting the triglycerides down means that your body is more insulin sensitive and has less inflammation. This is a positive response. Total LDL is not a good independent risk factor to follow.
Excellent explanation to help clearly understand the full story of ‘Cholesterol’ ! Exactly what I needed. Now I know what Specific steps I can personally implement to correct. I cannot thank you enough !
Barb Erck
Great to hear that!
This article was quite comprehensive however I’m very disappointed that there was no mention of the role of lipoprotein a. There was also no test for this in your panel. Do you not believe that this is an important risk factor? What are your recommendations regarding this?
Yes we discuss this in more detail here: https://drjockers.com/lipoprotein/
I got a better explanation on Cholesterol and the correlation between it and the other organs and the sunshine, sleep.
Thanks so much for this article. i will have to re-read
Wonderful thank you!
Hello,
My ratios are very off with regards to HDL and LDL and triglycerides. My HDL is 105 and LDL is 85. I thought it was good to have elevated HDL. How can I bring down my HDL or bring up my LDL? My triglycerides are 51. I am a 52 yr old female. Thank you!
It may be fine but it also may be due to high inflammation. I would focus on addressing any potential infections.