 How Your Genes Impact Weight Loss and Metabolism
How Your Genes Impact Weight Loss and Metabolism
Are you struggling to lose weight? Do you feel like you’ve tried everything yet the pounds are not coming off? We may have to look at your genes. Certain genes may impact your metabolism and your ability to lose weight.
The good news is, that once we understand what genes are impacting your health, you can turn off these genes with the help of some personalized dietary and lifestyle adjustments. Once you understand your genes better, they can actually help you lose weight.
In this article, you will learn about nutrigenomics. I will discuss how your genes impact your physiology and health. I will go over the key genes that impact your metabolism.
You will understand how certain genes impact your food intake, satiety, levels, fat metabolism, insulin sensitivity, fat breakdown, metabolic rate, inflammation, and susceptibility to stress. Finally, I will recommend a genetic test to get your personal genetic story. With the help of this test, we can create an individualized dietary and lifestyle plan to improve your health.
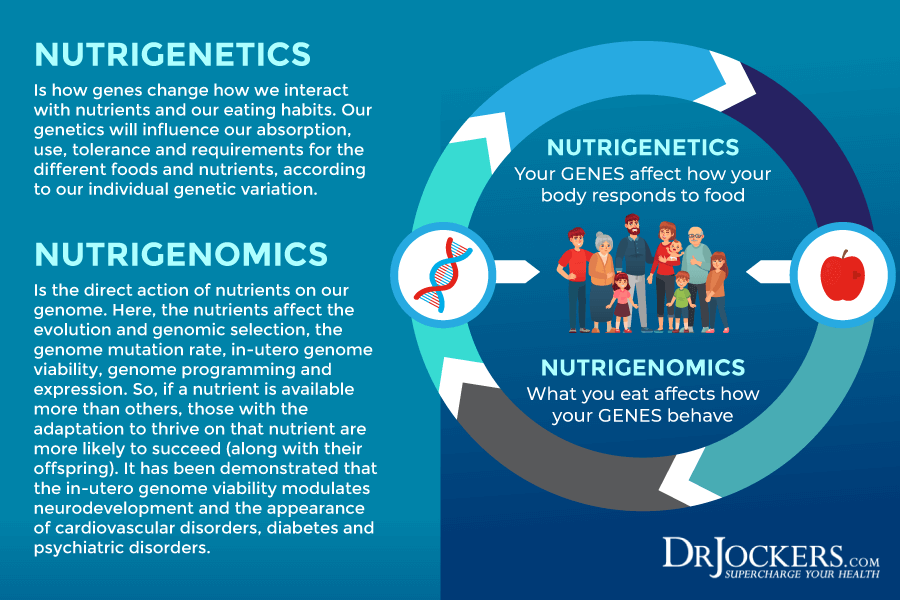
What Is Nutrigenomics
Nutrigenomics is a field of study looking at how our food affects our genes and how our genes affect the way our body responds to food. It basically looks at how nutrients affect your body’s expression of your genes. Nutrigenomics is not the same as nutrigenetics. Nutrigenetics looks at the effect of genetic variation on dietary response. The two fields of study can support each other.
According to a 2013 review published in the Journal of Food Sciences and Technology, nutrigenomics is an emerging and growing field due to our expanding awareness of how certain dietary modifications may potentially improve our health and decrease the risk of disease (1).
Though the field of nutrigenomics is still considered new, the idea that our diet, genes, and health are connected is not new. According to a 2016 article by Cambridge University Press, the earliest ideas in the field date back to Archibald Garrod, a British physician from the early 20th century who made a connection between nutrition, genetics, and phenotype (2).
In the 1990s, the Human Genome Project paved the next step to our current emerging field of nutrigenomics by looking at the influence of our genes on our body’s response to our nutrition intake and vice-versa. Using genetic testing is not uncommon to look at certain health information and now we can use this information to understand and improve our nutrition.

The field of nutrigenomics brings together a variety of scientific fields, including nutrition, genomics, molecular biology, molecular medicine, bioinformatics, and epidemiology. According to a 2007 review published in Environmental Health Perspectives, nutrigenomics initially only looked at the effects of diet on the expression of our genetic makeup, now it also looks at how nutrition can protect our genome from damage (3).
Nutrigenomics acknowledges that certain diets may increase the risk of diet-related disorders, however, and looks at the role of diet, supplementations, and gene alteration in our health. Understanding the field of nutrigenomics may help us to find new ways to improve our health, reduce the risk of disease, and support treatment.
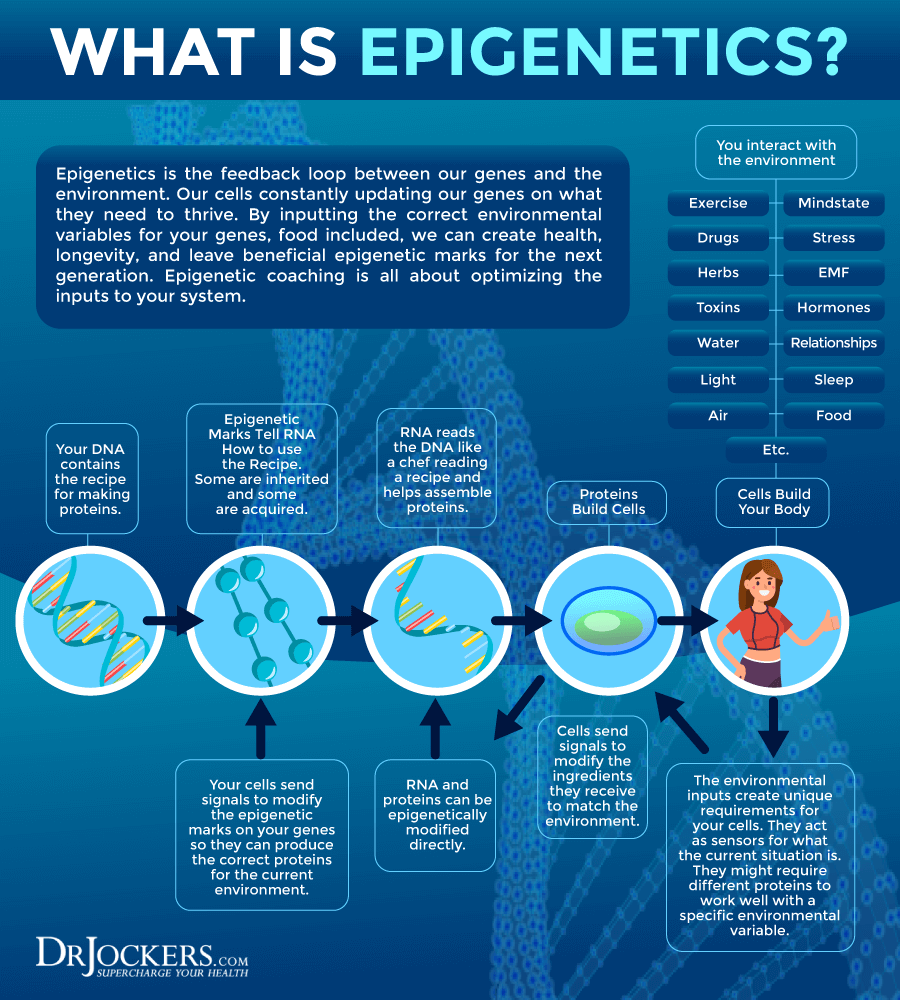
How Your Genes Impact Your Physiology
Your genes carry many instructions that will affect your life. Some of these instructions can make it more likely for you to develop a certain health condition. For example, if you have genes that are associated with obesity, your genes may tell your body to release or withhold chemicals that control your hunger and appetite, affect the size of your fat cells and how they use fat or even influence your behavior when it comes to food, exercise, and lifestyle choices.
However, genetics don’t determine everything. Many factors can influence how you behave or how your health turns out. For example, if you grow up in a household that has access to healthy, nutritious food, your parents teach you to limit your sugar and move your body, your life may turn out very differently than if you grew up in a low-income family in a food desert with access only cheap, overly processed, sugary food with parents who don’t teach you about the importance of nutrition — despite having the same genetics.
You may have genes linked to obesity, if you are following a healthy, nutrient-dense diet and lead a healthy lifestyle, these genes may never get activated. If you have the same genetic predisposition to obesity and follow a poor, high-sugar, low-nutrient diet and make poor lifestyle choices, there is a good chance that these ‘obesity genes’ get activated and increase your risk of weight problems.
Your genetics can increase your risk of weight gain, metabolic issues, and various health issues. However, with the help of a healthy diet and lifestyle, you may be able to turn off genetic triggers and reduce your health risks. This is where nutrigenomics comes in to play a role. Having a good understanding of your genetics and their relationship with food, you may be able to reduce your risk of weight gain, improve your metabolism, and decrease your risk of disease.
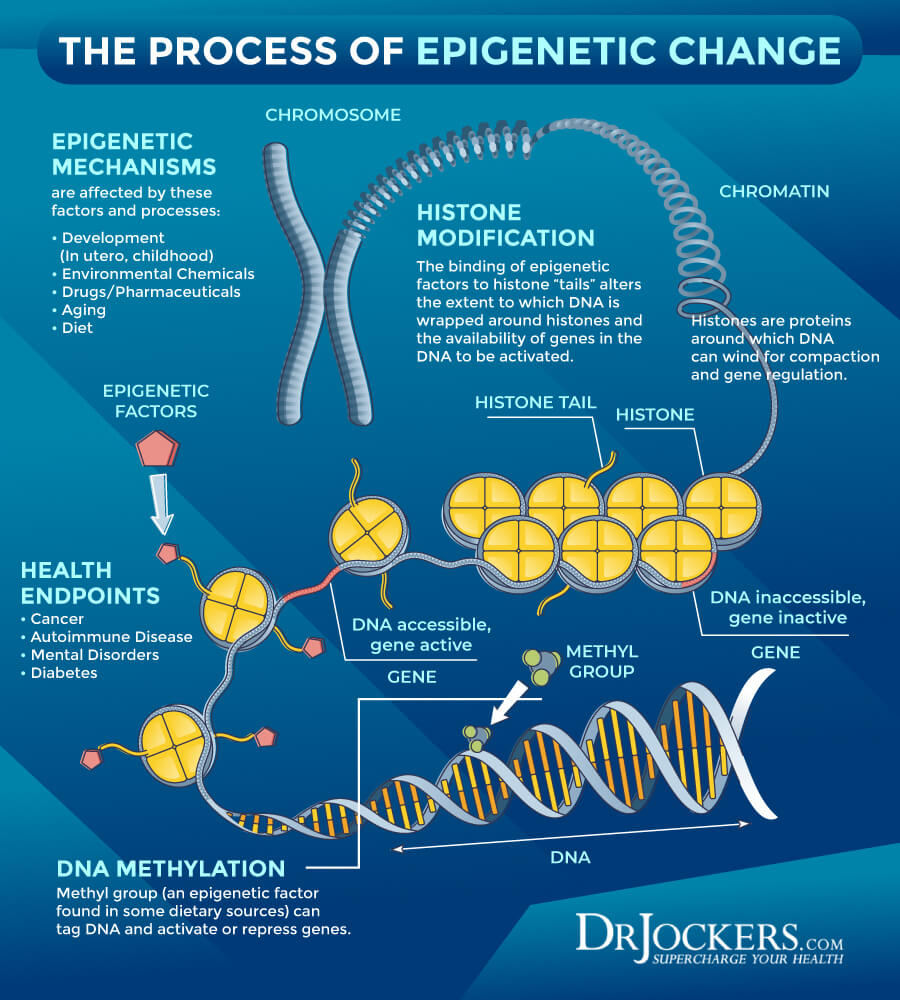
Though genetic testing being part of your regular healthcare visit or nutrition counseling may sound odd at first, you may benefit from a genetic workup to receive a personalized recommendation to improve your health. It may be particularly helpful for those who feel like they have ‘tried everything’ but still can’t lose weight or still can’t find relief from their symptoms.
Genetic testing allows us to understand your body better and offer personalized nutrition recommendations. Nutrigenomics may help us to offer a better-personalized plan with the right ratios and sources of macro- and micronutrients. For example, genetic testing may help us understand how well your body can convert vitamin D from sunshine, use omega-3 fatty acids from plant-based sources, or absorb certain nutrients.
Genetic testing can help to determine your risk for certain diseases, including obesity, diabetes, heart disease, cancer, and mental health issues. A 2014 study published in Translational Research has found that genetics and hereditary factors may play a role in obesity (4).
A 2014 review published in Current Genomics has found that genetics, nutrition, and nutrigenomics may play a role in diabetes and metabolic diseases (5). A 2016 review published in Cardiovascular Genetics has found that nutrigenomics may have the potential to play an important role in the prevention and treatment of cardiovascular and cardiometabolic diseases (6).
A 2009 review published in the Avicenna Journal of Biomedical Technology has found that understanding the relationship between our diet and genetics may help to lower your risk of cancer or reduce your symptoms (7). A 2012 paper published in Current Nutrition Reports has also found that nutrigenomics may play a role in cancer prevention (8).

Beyond our physical health, nutrigenomics may also help with our mental health as well. A 2019 review published in Psychiatric Genetics has found that genetics and nutrigenomics may play a role in schizophrenia, bipolar disorder, major depressive disorder, and other psychiatric issues (9).
Genetic testing can empower you with information and allow us to create an individualized preventative or treatment protocol to reduce your risks or improve your symptoms. A 2013 review published in The Proceedings of Nutrition Society has found that looking at individual differences, genetics, and nutrigenomics and creating personalized treatment recommendations may help with creating sustainable lifestyle recommendations, promoting health, and preventing disease (10).
If you are interested in your personal genetic story and to improve your health with the help of genetics and nutrigenomics, I recommend our 3×4 Genetics test. This simple genetic test tests over 134 genes that may affect your inflammation levels, metabolism, weight, fitness, hormones, cognition, detoxification, and your body’s response to food and supplements.
Key Genes That Impact Metabolism
Your genetics may play some role in weight gain, difficulty losing weight, food intake, and metabolism. However, being born with ‘bad genes’ doesn’t mean that you need to struggle with a slow metabolism, weight gain, and obesity. Your diet and lifestyle are more important than your genes. Dietary and lifestyle choices and other factors can turn on and off your genes and increase or lower the risk of weight gain and poor metabolism.
If you are struggling with a slow metabolism, weight gain, or weight loss resistance, looking into the specific genes that drive food intake, satiety levels, fat metabolism, insulin sensitivity, fat breakdown, metabolic rate, inflammation, and stress susceptibility can help us get some answers.
Once you understand your personal genetic predisposition, through the science of nutrigenomics, we can develop a personalized plan and you can start making appropriate dietary and lifestyle choices to turn off your ‘bad genes’, improve your metabolism, and aid weight loss, and support your health. Let’s look at the genes that affect these specific functions.

Food Intake: FTO and LEP Genes
The Fat Mass and Obesity Associated or FTO (“Fasto”) gene is one of the most well-known and most studied obesity genes. A 2020 review published in Frontier in Genetics has linked FTO to obesity and cancer (11). FTO may act as a nutrient sensor and as a result, it may affect your hunger levels and how much you eat. It may urge you to increase your food intake and lower your satiety after eating.
It seems that people with higher BMIs are more likely to have an FTO gene variation. What’s interesting when it comes to FTO is that the Amish population has a higher incidence of FTO. Yet, a 2007 study published in Medicine and Science in Sports and Exercise has found that obesity is very rare in the Amish (12). It seems that because of their regular physical activity and unprocessed, healthy diet, their FTO gene is turned off, reducing their risk of obesity.
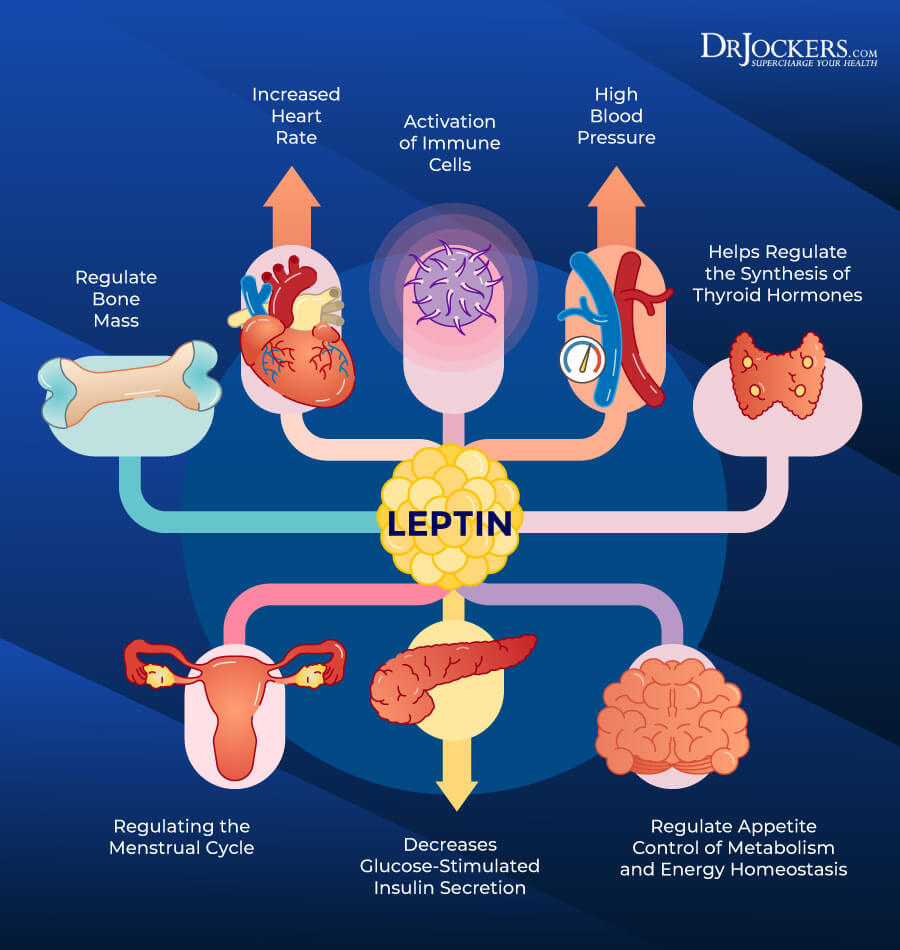
Besides FTO, the LEP gene may play a role in your food intake as well. The LEP gene triggers your body to create the hormone leptin (13). Leptin plays a role in your body weight. Your fat cells release leptin based on their size. If more fat builds up in your cells, they will produce and release more leptin.
Leptin binds to a receptor called the leptin receptor. By activating the leptin receptor, it sends a message to your hypothalamus, which controls hunger, thirst, sleep, and other functions. Increased leptin release will turn on your hunger signals and reduce satiety, which can prompt you to eat more, and may cause weight gain. According to a 2021 cross-sectional study, LEP expression and LEP methylation may play a role in obesity (14).
Satiety Levels: LEPR and MC4R Genes
The LEPR gene is responsible for triggering the creation of a protein called the leptin receptor. As you know, the leptin receptor plays a role in body weight regulation. Your hypothalamus controls your hunger and thirst. The leptin receptor can send messages to your hypothalamus to turn on hunger and turn off satiety.
Functional changes at the leptin receptor can lead to reduced satiety, increased food intake and weight gain. According to a 2018 study published in Nutrients, the LEPR gene plays a role in food consumption and weight gain in children (15).
Besides the LEPR gene, the MC4R gene may also play a role in your satiety levels. The melanocortin 4 receptor is encoded by the MC4R gene, which plays a role in feeding behavior, satiety, weight, regulation of metabolism, male erectile function, and sexual behavior. Those with an MC4R genetic mutation tend to gain weight starting from early childhood.
They often experience increased linear growth and again in lean mass as well and are often referred to as ‘big boned’. According to a 2016 case report published in Pediatrics Child Health, MC4R gene mutation may play a role in childhood obesity (16). According to a 2014 study published in Genes and Nutrition, MC4R may reduce satiation and increase the risk of obesity (17).

Fat Metabolism: PPAR-G and ADIPOQ Genes
PPAR-G is a protein that’s involved with fat metabolism and may increase the risk of weight gain. A 2010 review published in Cell Research has found that PPAR-G plays a role in energy metabolism and the development of metabolic diseases (18). PPAR-G helps your body to make fat cells. It also supports the uptake of dietary fats from your blood.
Increased PPAR-G activity may not only increase the risk of weight gain and obesity, but also diabetes, heart disease, and stroke. People who are obese tend to have higher levels of PPAR-G, while those with less fat in the gluteal areas or limbs tend to have little to no PPAR-G. Postmenopausal women with PPAR-G mutation tend to gain more weight than those without.
Beyond PPAR-G, the ADIPOQ gene also plays a role in fat metabolism. Adiponectin or ADIPOQ is a protein hormone and adipokine. It helps to regulate your glucose levels and it’s also involved with the breakdown of fatty acids.
ADIPOQ is mainly produced in your adipose tissue but can also be found in your muscles and brain. A 2020 study published in Lifestyle Genomics found that ADIPOQ levels were higher in metabolically unhealthy people (19). It seems that excessive adipose tissue and increased ADIPOQ may play a role in chronic metabolic disturbances and weight gain.

Insulin Sensitivity: INSR and TCF7L2 Genes
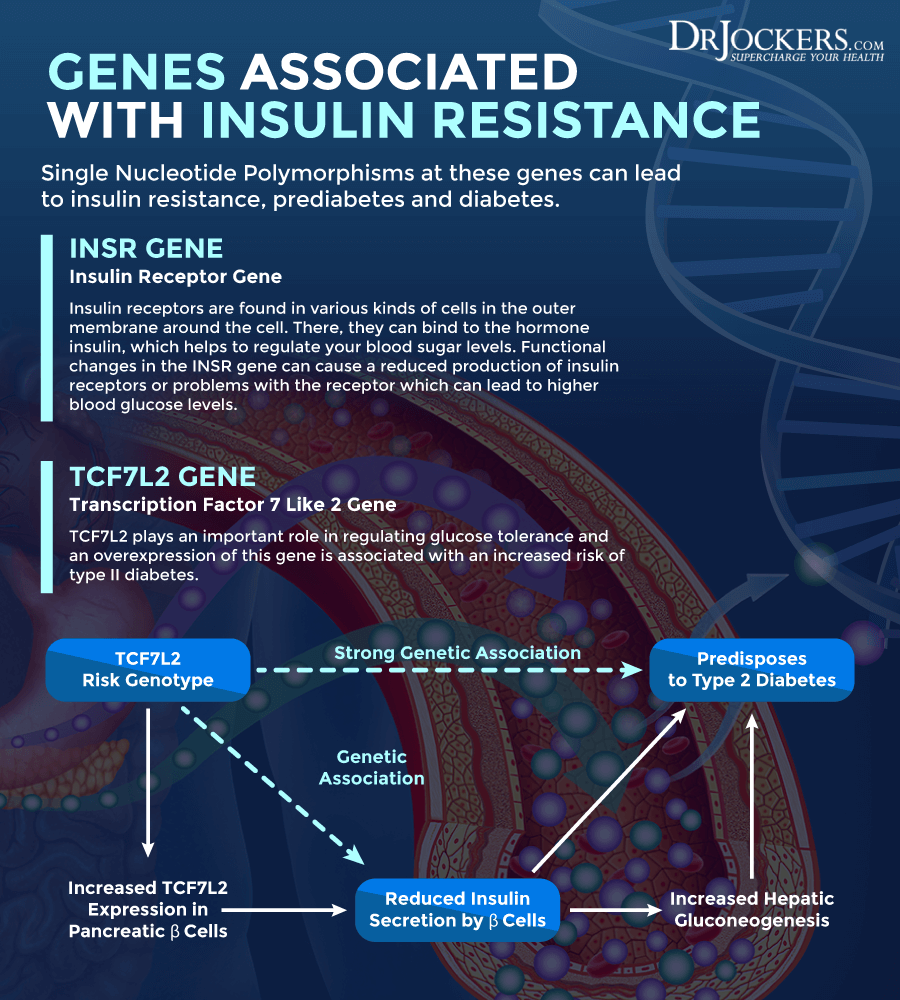
The INSR gene triggers the creation of the insulin receptor protein. Insulin receptors are found in various kinds of cells in the outer membrane around the cell. There, they can bind to the hormone insulin, which helps to regulate your blood sugar levels. According to a 2019 study published in the International Journal of Molecular Sciences, impaired INSR activity can increase insulin resistance and the risk of diabetes (20).
Besides INSR, the TCF7L2 gene also plays a role in insulin sensitivity. The TCF7L2 gene triggers the creation of TCF7L2. TCF7L2 is a protein that serves as a transcription factor. TCF7L2 polymorphism has been linked to an increased risk of type 2 diabetes and other diseases. According to a 2007 article published in The Journal of Clinical Investigation, the TCFL2 gene may play a role in diabetes (21). A 2006 study published in Diabetes has also found that TCF7L2 polymorphism may play a role in insulin resistance and type 2 diabetes (22).
Fat Breakdown: ADRB2 and ADRB3 and ADIPOQ Genes
The ADRB2 gene is a protein-coding gene that plays a role in breathing down fats. Epinephrine, a hormone, can attach to ADRB2, which leads to a boost in energy that helps the breakdown of fat molecules. Some ADRB2 gene variations may increase the risk of metabolic syndrome and diabetes, as well as cardiovascular disease. According to a 2002 study published in Metabolism, ADRB@ genetic polymorphism may be linked to obesity and type 2 diabetes (23).
ADRB3 gene is another coding gene mainly found in your adipose tissue. It plays a role in lipolysis and thermogenesis. It may play a role in weight gain and body mass index. According to a 2007 study published in the European Journal of Clinical Nutrition, ADRB3 gene polymorphism is common in obese individuals and may play a role in metabolic syndrome (24).
Beyond the ADRB2 and ADRB3 genes, the ADIPOQ gene also plays a role in fat breakdown. I’ve already discussed the role of ADIPOQ in fat metabolism, so it’s not surprising it can play a role in fat breakdown as well. A 2020 study published in Lifestyle Genomics found that excessive adipose tissue and increased ADIPOQ may play a role in chronic metabolic disturbances and weight gain and ADIPOQ issues are more common in obesity (19).
Metabolic Rate: UCP Genes
UPC1 is a protein-coding gene for UPC1. Thermogenin is also known as uncoupling protein or UPC1 is a mitochondrial protein. It is located in your brown adipose tissue. It plays a role in thermogenesis and metabolism.
A 2015 study published in Frontiers in Physiology has found that UCP genes may play a role in energy metabolism, metabolic rate, and obesity treatment (25).

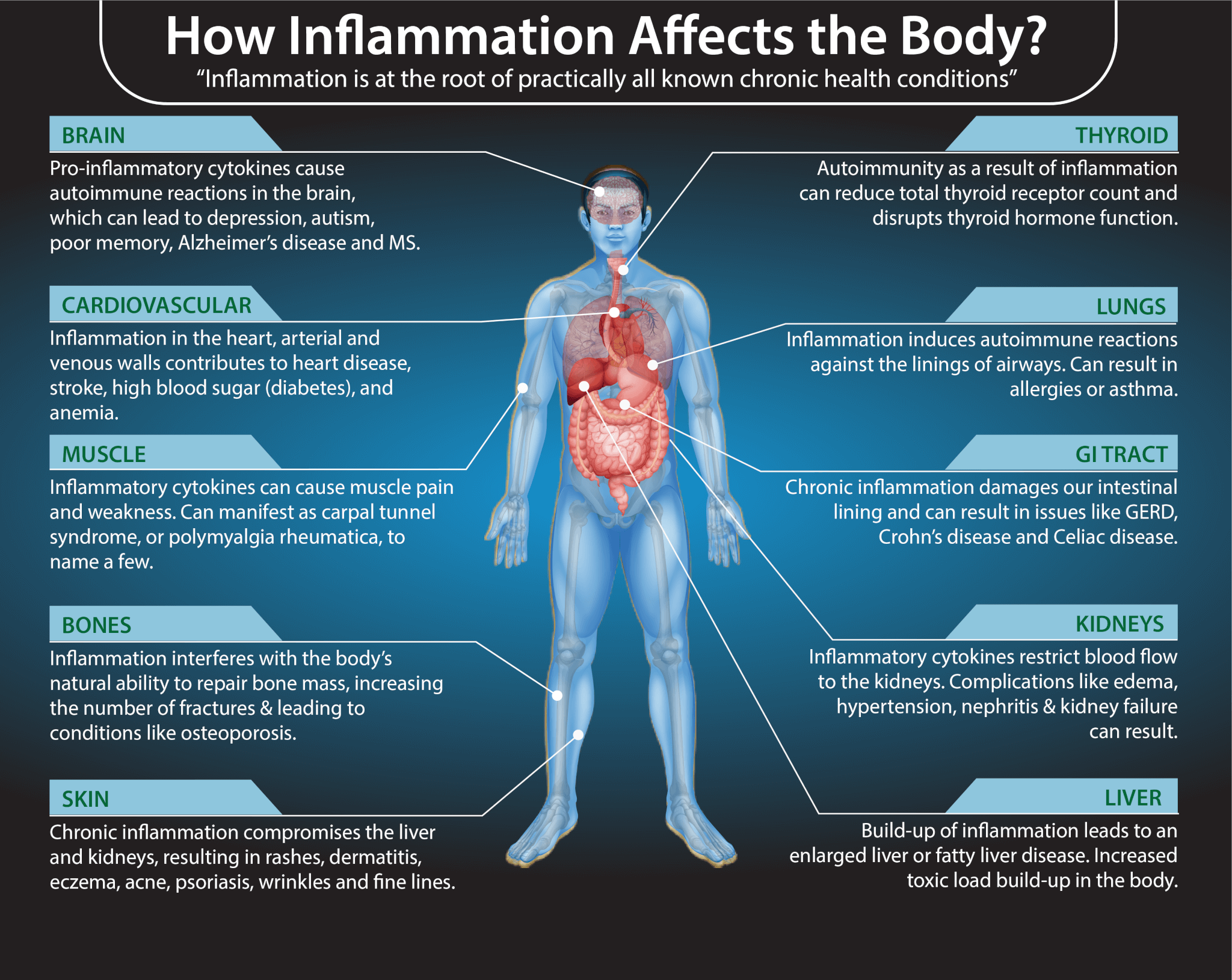
Inflammation: IL-6 and TNF-A Genes
Interleukin 6 is a type of interleukin. It plays a role as a pro-inflammatory cytokine and an anti-inflammatory myokine. Interleukin 6 is encoded by the IL6 gene which can play a role in turning inflammation up or down.
A 2006 research published in Arthritis Research and Therapy has found that IL-6 plays a role in chronic inflammation (26). According to a 2014 review published in the Cold Spring Harbor Perspectives in Biology, IL-6 plays a role in chronic inflammation, immune health, and autoimmune diseases (27).
Besides the IL-6 gene, the TNF-A gene also plays a role in inflammation. The TNF-A gene is responsible for the tumor necrosis factor (TNF). TNF is a cytokine and adipokine. It plays a role in the regulation of your immune cells.
TNF may be linked to inflammation, tumorigenesis, and viral replication. Certain cancers can be characterized by an overproduction of TNF. A 2017 study published in the Investigative Ophthalmology and Visual Science has found that TNF-A genetic predisposition may increase inflammation and pathogenesis (28).
Stress Susceptibility: FKBP5 and CLOCK Genes
The FKBP5 gene is one of the genes that may make you more susceptible to stress. It can trigger the hypothalamic-pituitary-adrenal (HPA) axis, your body’s stress response system. It can not only increase stress but also slow down your metabolism. It may also increase your risk of mental health issues.
A 2016 review published in Neuropsychopharmacology has found that the FKBP5 gene plays a role in stress regulation and addressing issues with this gene may play a role in treating stress-related disorders (29). A 2013 review published in CNS & Neurological Disorders and Drug Targets has found that the FKBP5 gene may play a role in mood disorders, such as depression, PTSD, and suicide (30).
The Circadian Locomotor Output Cycles Kaput or CLOCK gene is an encoding gene. It is responsible for encoding a basic helix-loop-helix-PAS transcription factor, which plays a role in your circadian rhythms. According to a 2021 review published in Biochemical Pharmacology, the CLOCK gene plays an important role in your stress levels, sleep, and memory (31). According to a 2021 study published in Frontiers in Physiology, CLOCK gene variations may increase depression as a result of stress exposure (32).

Get Your Personal Genetic Story
If you are interested in your personal genetic story and to improve your health with the help of genetics and nutrigenomics, I recommend our 3×4 Genetics test. This simple genetic test tests over 134 genes that may affect your inflammation levels, metabolism, weight, fitness, hormones, cognition, detoxification, and your body’s response to food and supplements. Understanding how your unique genetics impact these key processes can help you get smarter and make personalized decisions about your health.
The 3×4 Genetics test helps us to look at:
- Your unique nutritional needs: How do you respond to certain foods? How well do you tolerate fat and carbs? What’s your vitamin D need? Do you require extra antioxidants and Omega-3 fats compared to others based on your unique genotype? Should you limit gluten, salt, or caffeine?
- Your fitness strengths and exercise needs: What type of exercise will your body respond best to? How can you train smarter in alignment with your genes, for better performance, faster recovery, and fewer injuries? How can you enhance your athletic performance to get faster results and better outcomes?
- Your health risks and how to approach proactive prevention: Is your body more prone to high blood pressure, high blood sugar, or high cholesterol? How can you support your cardiovascular system and your immune system for more resilience as you age? We also look at processes like inflammation, detoxification, methylation, and more, to better understand what your body needs to cope better with the stressors of modern life.
- Your ideal weight: Why does your body resist weight loss and how can you manage your weight in a healthy and sustainable way that is personalized to your unique genotype?
- Your ideal strategies for stress: How does your life stress affect your brain health, your hormones, your sleep quality, and your overall wellness? More importantly, what can you do about it based on your genetic predispositions?
The 3×4 Genetics test has undergone rigorous examination for both scientific validity and clinical utility. Understanding your genetics is not enough, you need to be able to extract information from it to draw actionable insights and recommendations to improve your health.
As such, only the genes that have the greatest potential to influence health are examined because of genetics. Unlike some other genetic tests you find online, this test is practitioner-guided. Genetics is complex, you shouldn’t be left alone to understand your genes. Our highly trained health practitioners will work with you to translate your results and analyze how your genes work together in your body to impact your overall health. I highly recommend this simple test, you can sign up here.
Final Thoughts
Certain genes may impact your metabolism and your ability to lose weight. They can affect your metabolism. You will understand how certain genes impact your food intake, satiety, levels, fat metabolism, insulin sensitivity, fat breakdown, metabolic rate, inflammation, and susceptibility to stress.
Fortunately, once you understand your genetic make-up, you can develop a plan and make some changes to turn off these genes and turn around your health. I recommend that you get your personal genetic story. With the help of this test, we can create an individualized dietary and lifestyle plan to improve your health.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. On our website, we offer long-distance functional health coaching programs. For further support with your health goals, just reach out—our fantastic coaches are here to support your journey.
 Inflammation Crushing Ebundle
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!



