 When Heartburn Medications Can Be Dangerous
When Heartburn Medications Can Be Dangerous
If you are one of the millions of Americans who are dealing with heartburn on a regular basis, you know the discomfort of burning in your chest or throat and indigestion. If you’ve been to a doctor with your issue, there is a good chance that you’ve been suggested or prescribed heartburn medications.
The problem is that taking heartburn medications long-term doesn’t solve heartburn and may lead to serious health issues. Instead, I recommend natural strategies to improve your stomach acid levels for heartburn.
In this article, you will learn about the role of stomach acid in your body. You will understand what heartburn is. I will explain what proton-pump inhibitor heartburn medications (PPIs) are, when they may be appropriate, and why they may be dangerous long-term. I will also share my best tips to improve your stomach acid levels naturally.
The Role of Stomach Acid
Digestion is a complex and complicated process that involves several key players, including digestive juices and enzymes. Stomach acid, or gastric acid, is one of the most important substances that help digestion. Stomach acid is a digestive fluid created in your gut to help the digestion of food. Its main component is hydrochloric acid (HCL) along with potassium chloride and sodium chloride.
With the help of HCI, your stomach is able to transform a large solid meal into a semi-liquid soupy substance called chyme that can move through the rest of the digestion process without a problem. However, if there isn’t sufficient HCI production or your body is unable to provide a healthy gut environment, your body cannot break food down properly (1, 2).
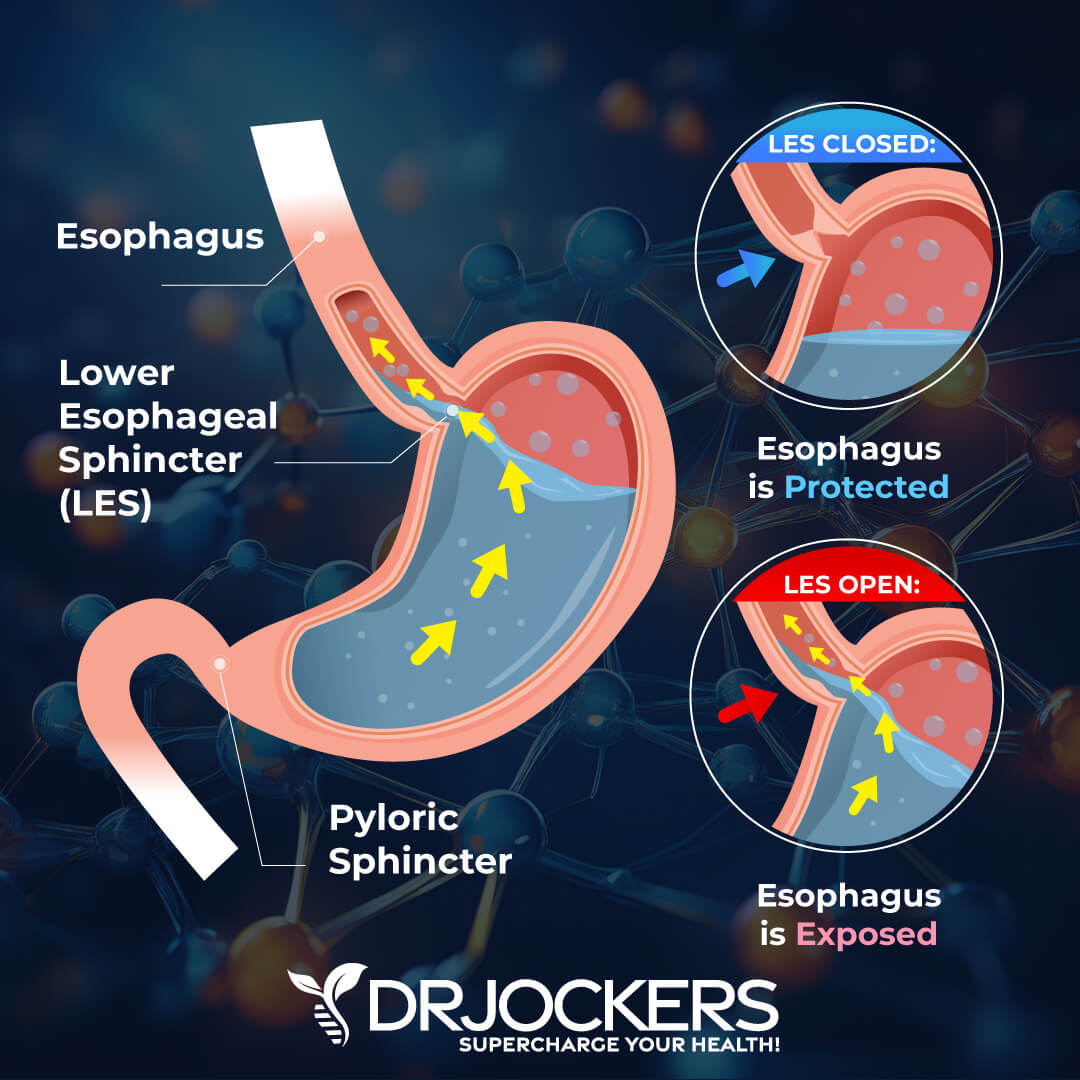
How Stomach Acid Works:
Hydrochloric acid production during mealtimes is important to:
- Acidify your stomach and help the creation of chime
- Break down proteins to make them more digestible for your body
- Active the protein-digesting enzyme pepsin to aid the digestion of proteins
- Allow bile and pancreatic enzyme flow to help the breakdown of proteins and carbohydrates and aid the absorption of fats and fat-soluble vitamins
- Help your body to absorb minerals and trace elements, such as magnesium, zinc, iron, and calcium
- Aid nutrient absorption, including vitamin B12, folate, and beta-carotene
- Kill unwanted micro-organisms from contaminated food, including bacteria, viruses, yeasts, parasites, and molds
- Protect your body from infections and pathogen overgrowth
- Support your immune system and reduce inflammation
- Send signals to trigger other important players of your digestive system, including your pancreas
 What Is Heartburn
What Is Heartburn
Heartburn is a common problem 15 million Americans experience every day after meals. This doesn’t include those who experience heartburn regularly but not daily or have it only occasionally.
If you have heartburn, it means the content of your stomach is forced back into your esophagus resulting in a burning sensation and pain in your lower chest area. Heartburn is a symptom of gastroesophageal reflux disease (GERD), which is persistent acid reflux that occurs twice a week or more (3, 4, 5).
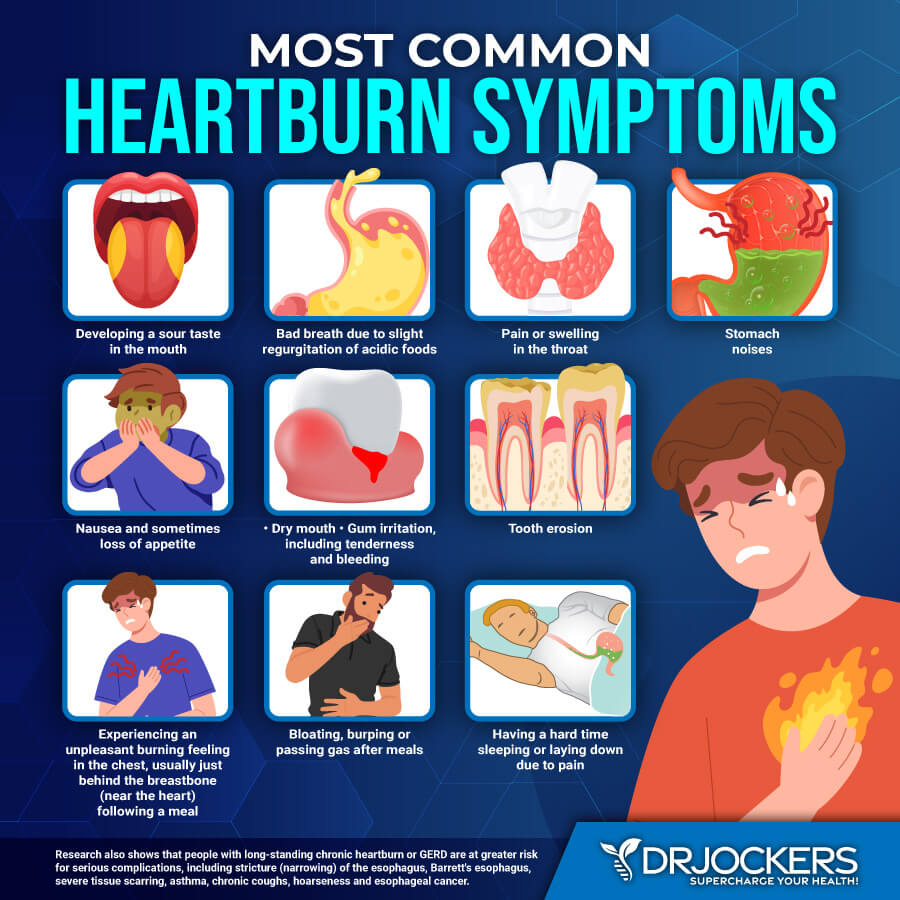
Symptoms of Heartburn
Symptoms of heartburn include:
- Warmth, heat, or burning in your chest or throat
- Burning pain after eating or at the end of the day
- Burning sensation in the middle of your chest
- Indigestion-like pain
- Acrid or foul taste in your mouth
- Rising pain that may reach your jaw
- Pain that worsens when lying down
What Are PPI Heartburn Medications
In the mid-1970 cimetidine (Tagamet) was introduced as the first medication targeting stomach acid production to relieve heartburn. Next, H2 blockers, including famotidine (Pepcid) and ranitidine (Zantac), were developed. They were followed by proton-pump inhibitor drugs (PPIs).
PPIs are claimed to be superior to H2 blockers and are the most commonly prescribed drugs to decrease stomach acid, relieve heartburn, acid reflux, and GERD, and treat ulcers in the stomach and duodenum. Common PPIs include lansoprazole (Prevacid), omeprazole (Prilosec), esomeprazole (Nexium), dexlansoprazole (Dexilant), rabeprazole (Aciphex), pantoprazole (Protoxin), and omeprazole (Zegerid).
In the United States alone billions of dollars are spent on PPIs. Even generic varieties may cost about 200 US dollars while paying the full price for non-generic brands can be ten times or more. Besides the price, the main concerns regarding PPIs include overuse, drug interactions, and side effects. While PPIs are not necessary in mild cases of heartburn, many believe that taking medication is the best in all cases, which results in overprescription and overuse of these heartburn medications.
PPIs may also interact with clopidogrel (Ceruvin, Clopilet, and Plavix) which discourages artery-clogging blood clot formation. PPIs may also increase the risk of fractures, B12 deficiency, pneumonia, and Clostridium difficile infections. Overuse, drug interactions, and side effects are not the only problems with PPIs. Later in this article, I will discuss other problems with long-term use of heartburn medications (6, 7, 8). Check out the infographic below made by the TheProductLawyers.com

Heartburn is a Symptom of Low Stomach Acid
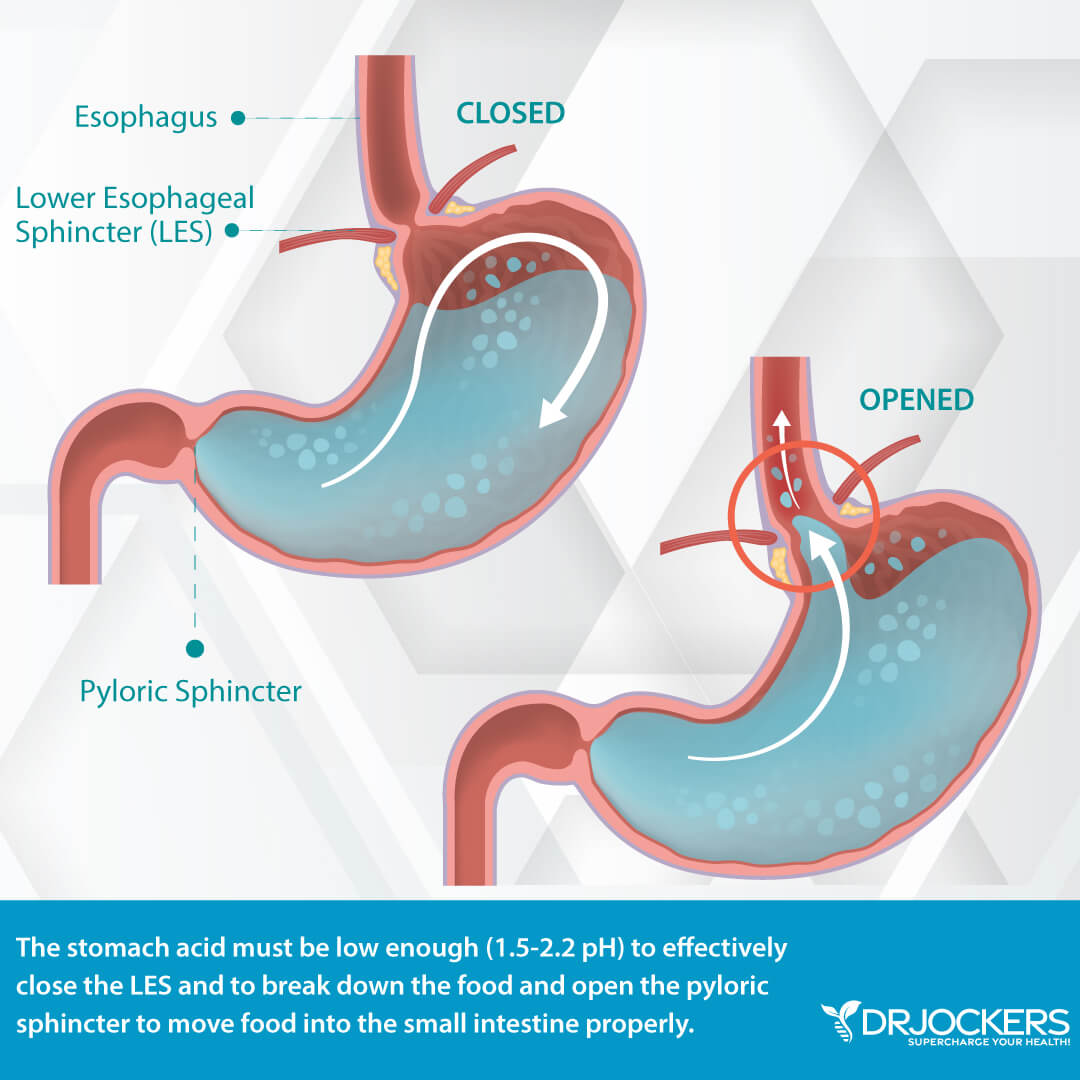
What most people don’t realize is that heartburn is a symptom of poor stomach acid production and not too much stomach acid production. At rest, our stomach acid environment is at a 3-3.5 pH level. For contrast, a neutral pH is 7.0.
In order to effectively digest a protein rich meal, we need to get our stomach acid environment down to 1.5-2.2. This is very energy demanding and due to a variety of factors, many people struggle to produce enough acid.
When we don’t produce enough acid, food sits in our stomach longer and begins to ferment and create gas and pressure that opens up the lower esophageal sphincter. The acid that is in the stomach now regurgitates up into the esophagus where the tissue is not protected from the acid and it creates a burning sensation and over time creates significant damage to the esophagus.
So it is important to know, that suppressing stomach acid further with heartburn medications may relieve the symptoms but it only further worsens your digestive health and ability to protect your body from pathogens and absorb essential nutrients.
When Are Heartburn Medications Beneficial
In most cases, heartburn medications are not necessary and as you will learn, they may be downright dangerous. However, for individuals struggling with gastric ulcers, heartburn medications may be beneficial. To learn more about gastric ulcers and some natural solutions, I recommend that you read this article.
For short-term use to reduce acid reflux and heartburn, heartburn medications may be helpful, however, I do not recommend taking them long-term for the reasons I will explain in the next section. I recommend that you speak with your doctor before taking heartburn medications.
It is best if you consult with a functional medicine or another holistic health doctor, who can help you with natural solutions and treating the root cause of your heartburn and digestion-related issues. Here is an infographic that I got from Core IM podcast.

Why Are Heartburn Medications Dangerous
As you’ve just learned, heartburn medications can lead to overuse, drug interactions, and negative side effects. However, long-term use of heartburn medication may also result in many health problems including increased overall mortality.
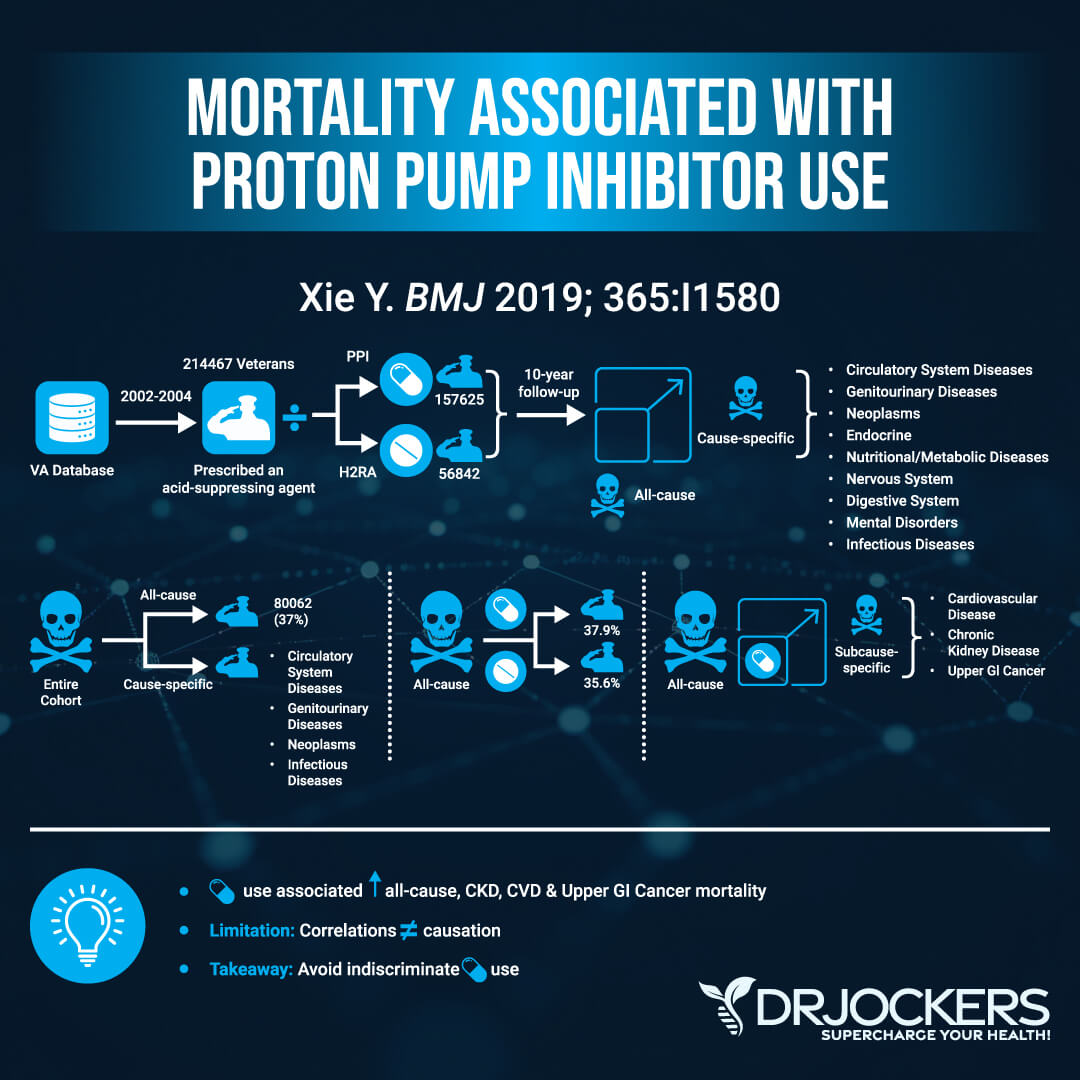
A longitudinal observational cohort study on US veterans looking at mortality rates, associated mortality, and PPI and H2 blocker medications found 45.20 excess deaths per 1000 patients in those taking PPIs, including infections, parasitic diseases, neoplasms, and genitourinary disease associated with PPI use. They found excess mortality due to cardiovascular disease, kidney disease, and gastrointestinal cancer associated with PPIs (9).
Increased mortality, however, is not the only problem with heartburn medication. Let’s look at other issues that long-term heartburn medication use may lead to.

Increased Microbial Overgrowth
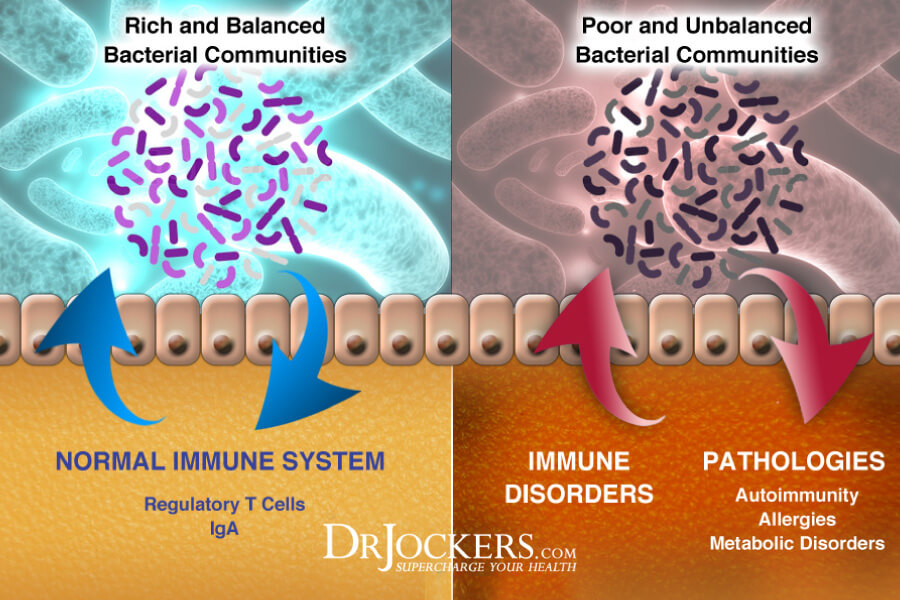
Stomach acid serves an important role in your digestion. For example, stomach acid plays a role in keeping bacteria overpopulating your small intestines and causing small intestinal overgrowth (SIBO). The problem is that PPIs and other heartburn medications decrease stomach acid levels, hence interfering with healthy digestion and may lead to increased microbial overgrowth.
Research has found that the long-term reduction of stomach acid through PPI use can interfere with your microbiome balance and lead to dysbiosis. It may increase the risk of food poisoning, diarrhea, SIBO, parasite overgrowth, yeast overgrowth, and microbiome imbalance (10, 11).
Heartburn Meds and Poor Protein Digestion
One of the main roles of stomach acid is to help proper protein digestion. When proteins are broken down into small enough particles, your immune system cannot mistake them for invaders or pathogens, and they can go through the digestion process and healing. However, when heartburn medication reduces stomach acid levels in your body, they can interfere with normal protein digestion.
If proteins or other food particles are not broken down properly, your body may mistake them for pathogens leading to digestion and immune system havoc, as well as inflammation. Poor protein digestion can result in altered metabolism, lowered immune health, and poor tissue healing and recovery (12, 13).

Poor Mineral Absorption
Stomach acid plays an important role in mineral absorption. PPIs lower stomach acid levels and interfere with digestion and nutrient absorption. Research has found that the overuse and long-term use of PPI heartburn medications can reduce nutrient absorption. They may reduce your body’s ability to properly absorb important minerals, such as zinc, iron, calcium, and magnesium.
These minerals are critical for immune function, brain health, relaxation, sleep, digestion, bone health, energy, mental health, and more. These mineral deficiencies may have a particularly serious impact on elderly and malnourished people. If you are already eating an unhealthy diet low in nutrients, taking PPIs long-term can lead to serious issues related to poor mineral absorption (14).
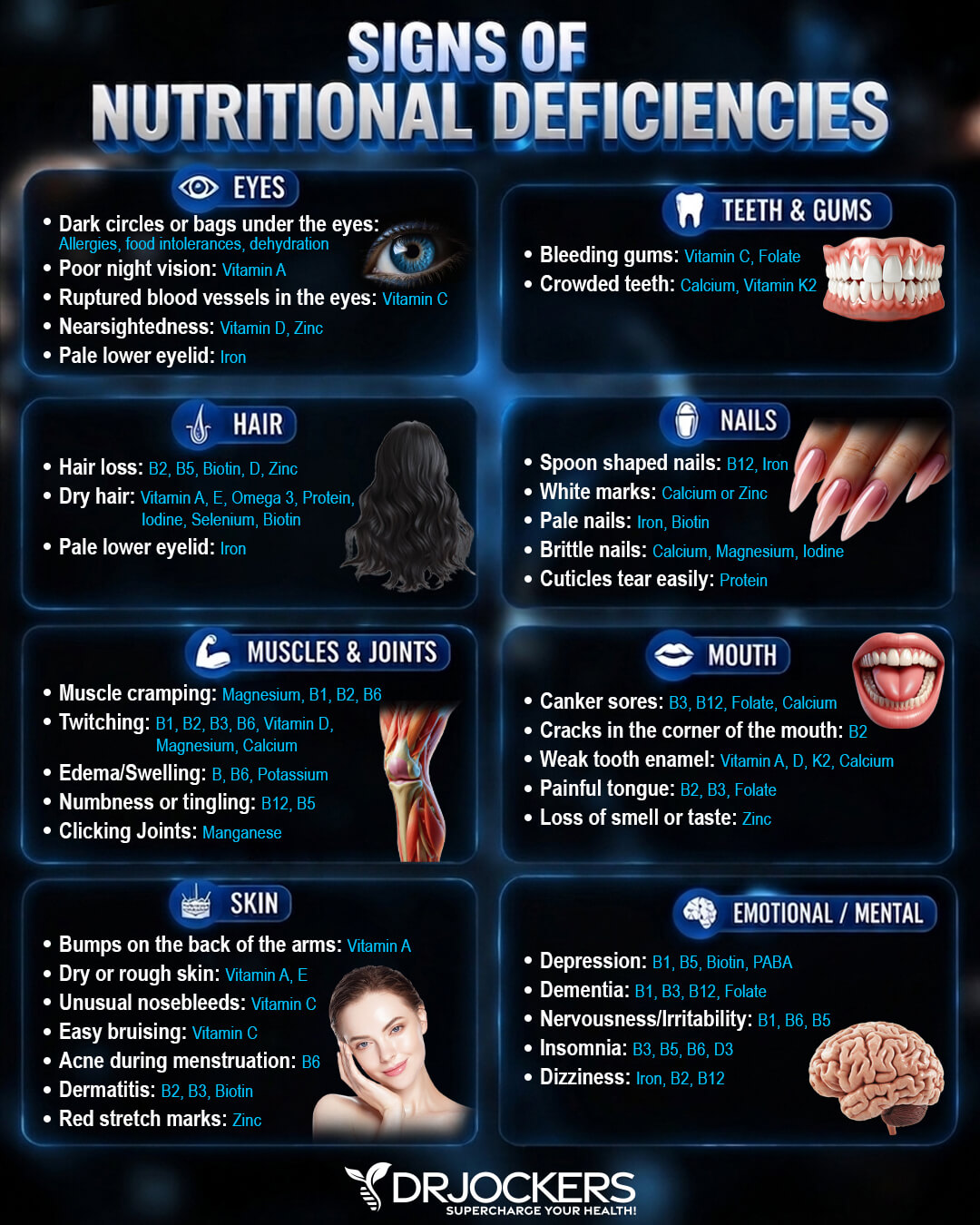
Poor B12 Absorption
PPIs not only interfere with the absorption of minerals but also some vitamins. Long-term use of PPIs can lead to poor B12 absorption. Again, this may be even more problematic for the elderly, those who are malnourished or eat an unhealthy diet, and vegans who don’t supplement and may not be meeting their B12 needs in the first place.
When it comes to B12, we must mention homocysteine. Homocysteine is an inflammatory amino acid that is produced as a byproduct of protein metabolism.
Elevated homocysteine leads to excessive clotting which diminishes blood flow to major regions of the body and leads to heart attacks and brain problems. B12 is necessary for one of the ways homocysteine metabolizes, remethylation.
Methylation deficiencies can also lead to low levels of B12, so it is important that you take pre-methylated forms of B12 to support homocysteine function. It is important that you pay attention to your B12 intake and support optimal absorption. Poor B12 absorption may result in fatigue, trouble concentrating, mood disorders, and cardiovascular and neurodegenerative conditions (14, 15, 16, 17).

Increased Cardiovascular Mortality
As you’ve already learned today, using PPI heartburn medications may increase the risk of mortality, including cardiovascular mortality. A systematic review of 37 studies investigated the connection between PPIs and morbidity and mortality.
They found that PPIs can increase the risk of all-cause mortality. They also found that long-term use of PPIs can also increase the risk of cardiovascular morbidity, cardiovascular events, and cardiovascular mortality (18). Here is an image from several studies I found that was listed and created by Medscape and can be referenced here.
Improve Stomach Acid Levels Naturally
Now that you understand that PPIs and other heartburn medications may harm your body and may not benefit your heartburn, you are probably wondering how you can relieve and prevent heartburn without them.
The good news is that you can improve your stomach acid levels naturally which may help to reduce the risk of heartburn and improve your overall digestive health. These strategies are not FDA approved to prevent, treat or cure heartburn but many clinicians have seen positive changes in individuals who have applied them.
Anti-Inflammatory Diet
Eating an anti-inflammatory diet is critical for improving your stomach acid levels and reducing heartburn. Remove all inflammatory foods, including refined sugar, refined all, artificial ingredients, deep-fried food, conventional dairy, conventional animal products, junk food, and processed food.
Eat plenty of anti-inflammatory organic greens, such as kale, spinach, and collard greens, vegetables, such as broccoli, cucumber, and celery, low glycemic index fruits, such as berries, lemon, and lime, herbs, and spices, such as ginger, turmeric, mint, rosemary, and basil, healthy fats, such as avocadoes, coconut oil, and organic butter, clean protein, such as organic pasture-raised beef, free-range poultry and eggs, and wild-caught fish, and fermented foods, such as kimchi, sauerkraut, and kefir. To learn more about the anti-inflammatory ketogenic diet I recommend, reading this article.

Reduce Stress & Improve Sleep
Chronic stress and poor sleep can lead to inflammation in your body and interfere with your digestion to increase your risk of heartburn. To improve your stomach acid levels naturally, it is important that you reduce stress and improve your sleep.
Spend your time with positive people that you love, reduce stressful activities, spend more time in nature, do some grounding walking barefoot on grass, journal, meditate, practice gratitude, pray or engage in spiritual practices, and smile more.
Develop a nighttime routine that works for you. Stay away from electronics, stressful activities, and food for several hours before bed. Sip on herbal tea and wind down with relaxing activities. Make sure that you sleep in a dark room on a comfortable bed, bedding, and pillow. Make sure you get 7 to 9 hours of sleep each night.

Heal Gut Infections
Gut infections can lead to gut dysbiosis causing imbalanced stomach acid and heartburn. To improve your stomach acid levels, it is critical that you address gut infections. H Pylori is a bacterium that is one of the most common culprits behind gut infections. H Pylori infections can lead to stomach ulcers, gallbladder issues, heartburn, anemia, osteoporosis, and autoimmunity.
To find out if you have an H pylori infection, I recommend this simple and affordable test. Along with anti-inflammatory, anti-microbial diet, I recommend plenty of garlic, onions, and herbs such as oregano, basil, thyme, ginger, and turmeric, and supplementing with GI Clear to support healthy microbial activity in your gut. To learn more about H Pylori infections, I recommend this article (19, 20, 21).

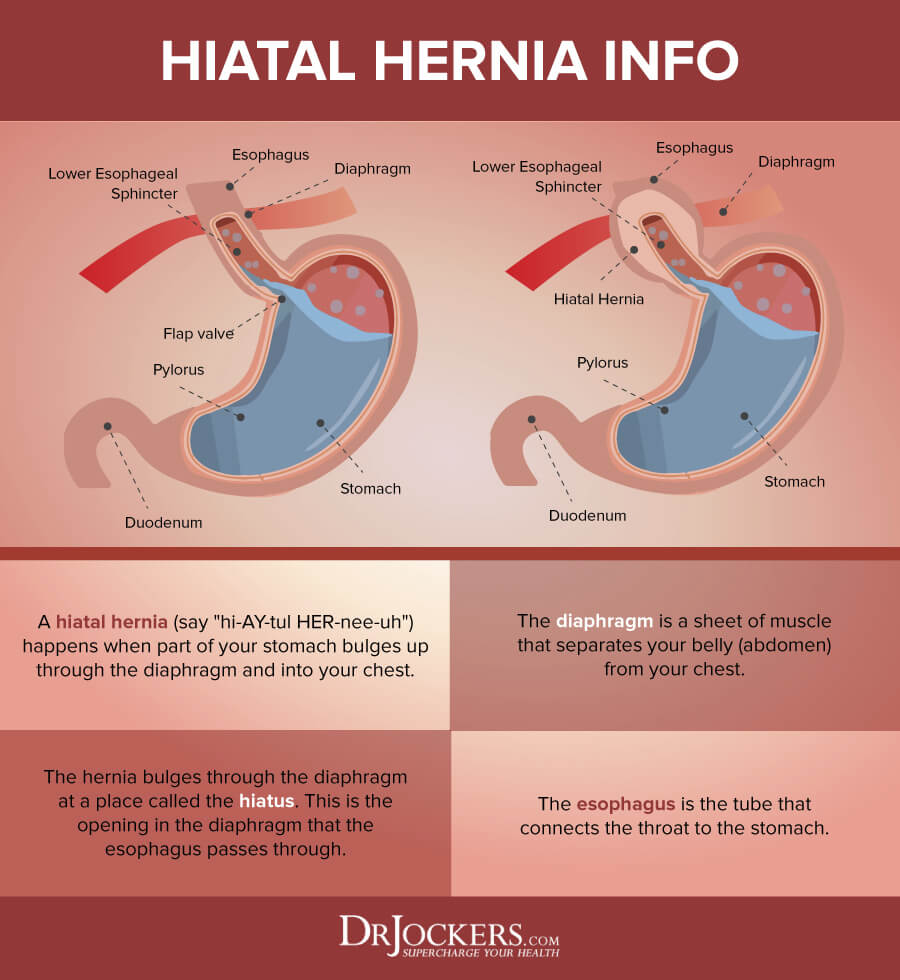
Reduce Hiatal Hernia if It is Present
A hiatal hernia forms inside the diaphragm, the muscular area between the chest and the lower abdomen. It can result in bulging inside the stomach and interfere with stomach acid and digestion. One of the main symptoms of a hiatal hernia, so if you have a hiatal hernia, it is important to reduce it to improve your stomach acid levels and heartburn.
Natural options for hiatal hernia include a warm water fix, self-massage, yoga, apple cider vinegar, cinnamon, chamomile, baking soda, aloe vera, slippery elm, an anti-inflammatory diet, fermented foods, and digestive enzymes, such as Super D-Zyme. To learn more about hiatal hernia, I recommend reading this article (22).
Proper Digestive Hygiene
To improve your stomach acid levels and reduce heartburn, it is important that you practice proper digestive hygiene. My 10 tips for proper digestive hygiene and improving your stomach acid levels include:
- Consider liquid nutrition throughout the day.
- Drink 2 to 3 cups of ginger tea a day and use ginger in your meals.
- Hydrate throughout the day outside of mealtimes to improve gastric motility.
- Don’t drink during your meals but wait with hydration for at least 30 minutes after mealtimes.
- Add apple cider vinegar and/or lemon to your water to support digestion and absorption.
- Eat protein foods at the beginning of your meal.
- Support your gut microbiome digestion with fermented foods.
- Eat fermented drinks, such as apple cider vinegar (ACV), coconut water, or kefir to support your gut flora.
- Eat your largest meal when you are the most relaxed to help proper stomach acid production.
To learn more about proper digestive hygiene to improve your stomach acid levels, I recommend this article.

Use Probiotics
To improve your gut microbiome, support your digestion and absorption, improve stomach acid levels, and reduce heartburn, I recommend that you take probiotics every day. Probiotics help to create gut flora balance and support your digestion.
I recommend SBO Probiotics – Ultimate, a shelf-stable probiotic supplement with 50 billion CFU, prebiotic superfoods, and an organic fermented botanical blend for optimal results.

Consider Using Betaine HCL with Meals
To support optimal digestion, consider using Betaine HCL with your meals. This can dramatically help improve your ability to digest protein, absorb minerals and B12 and optimize your digestive terrain.
I recommend Super Digest HCL. This supplement is made with betaine hydrochloride (HCl), an excellent source of hydrochloric acid, dipeptidyl peptidase IV (DPPIV), lactase, an enzyme that aids the breakdown of lactose, “milk sugar”, and ox bile extract and lipase to emulsify and digest fats and fat-soluble vitamins. Take it regularly with a meal for optimal results.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!
Final Thoughts on Heartburn
About 15 million Americans who are dealing with heartburn daily experiencing the discomfort of burning in your chest or throat and indigestion. Conventional doctors regularly prescribe PPI heartburn medications for heartburn, however, taking heartburn medications long-term doesn’t solve heartburn and may lead to serious health issues.
Instead of relying on heartburn medications as a long-term remedy, follow my natural support strategies to improve your stomach acid levels and optimize your digestive health.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. At DrJockers.com, we offer long-distance functional health coaching programs. For further support with your digestive health and other health goals, just reach out and our fantastic coaches are here to support your journey.





Specific Guidance on how to get off of these drugs is needed. Everything you say is true; but these drugs cannot be stopped easily. A specific protocol – even a generalized approach to tapering off and stopping these drugs is needed.
Hello Nicola, yes unfortunately we are unable to give specific advice on this through our web articles based on FTC laws. I would suggest hiring a functional health coach to help guide you with this. Blessings!
Would fasting be ok to do if you have the bacterium causing these symptoms
Yes it can be helpful!
24 hour water fasting fixed my repeated heartburn, (this is thinking inside the square) give that part of the body a break from processing food all the time and time to heal.
No more heartburn when I went back to eating, as normal. Think, no doctor visit, no medication. faster more healthy natural repair.
THANK YOU Dr. David Jockers for talking me into Water fasting and going to a fat burner.
Wonderful to hear that Eric!!