 Raynaud’s Phenomenon: Causes, Symptoms and Solutions
Raynaud’s Phenomenon: Causes, Symptoms and Solutions
Raynaud’s phenomenon, also called Raynaud’s disease or syndrome, is a relatively common but often unrecognized condition. It is a vascular disorder that occurs when blood vessels temporarily overreact to low temperatures, emotional stress, or other exposures.
Raynaud’s phenomenon typically affects a person’s fingers, but can also affect the toes, nose, earlobes, or nipples. In people with Raynaud’s, the affected area is unusually sensitive to cold. It will change color to white, then blue, and will feel numb and tingly.
There are two types of Raynaud’s phenomenon, primary Raynaud’s and secondary Raynaud’s. Primary Raynaud’s happens without any other condition and the symptoms are often mild. Secondary Raynaud’s is associated with another disease or condition and can have complications.
There are natural support strategies to help people struggling with Raynaud’s. An anti-inflammatory diet along with numerous natural strategies and targeted supplementation may help to improve the health of those with Raynaud’s. For people with secondary Raynaud’s, it is also important to address the underlying or associated condition.

What is Raynaud’s Phenomenon?
Raynaud’s (ray-NOHZ) phenomenon causes areas of the body to feel numb and cold and change color in response to cold temperatures, emotional stress, or other exposures. This phenomenon was first described in 1862 by the French physician Maurice Raynaud, who at the time was a medical student (1). It was first called “Raynaud’s disease” but later referred to as “Raynaud’s phenomenon.”
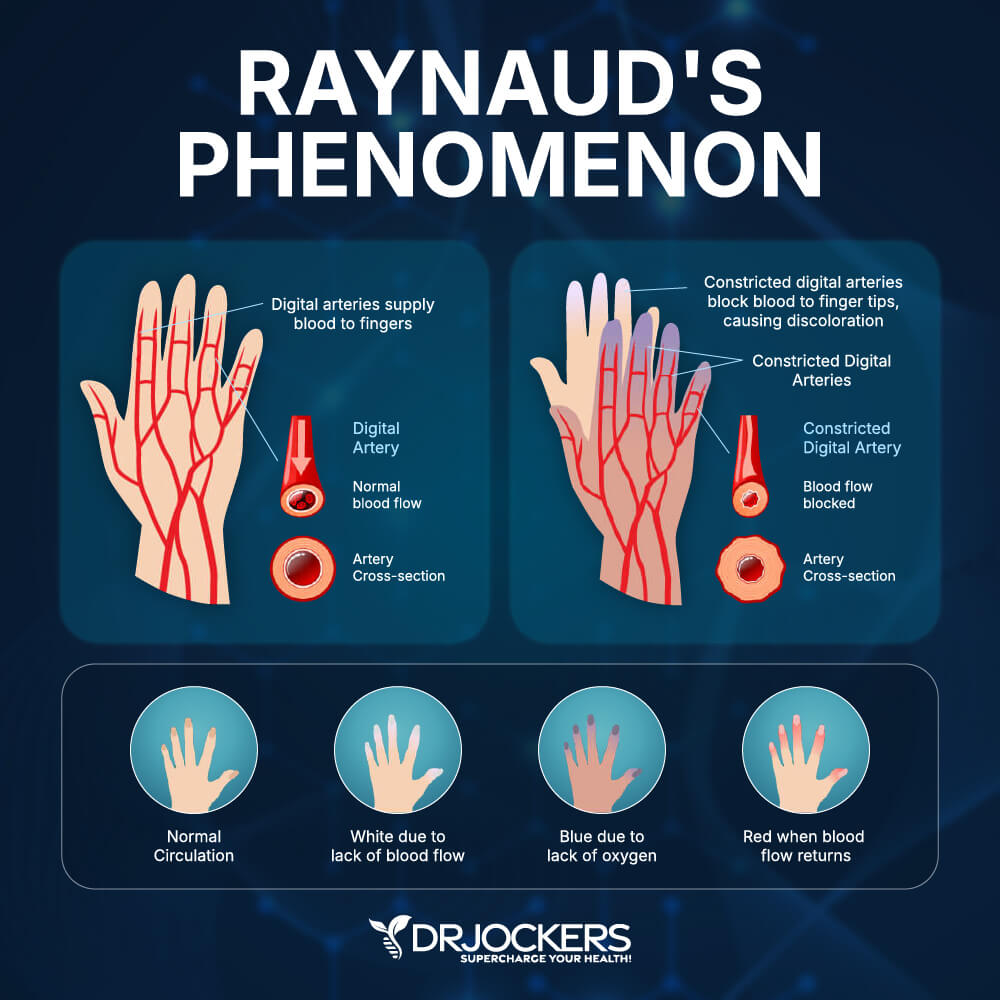
Raynaud’s most commonly affects the fingers and toes, but can also affect the nose, earlobes, or nipples. In people with Raynaud’s, the affected area is sensitive to cold. It will change color from white to blue to red. This is because the arteries to your fingers and toes go into vasospasm narrowing your blood vessels and temporarily limiting blood supply. Over time, these small arteries can thicken slightly, further limiting blood flow.
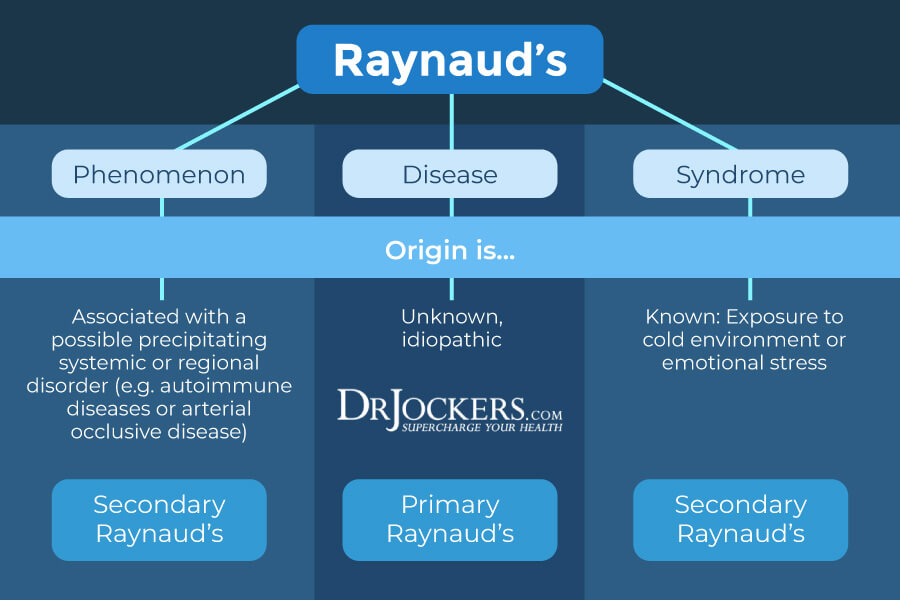
There are two types of Raynaud’s phenomenon: primary Raynaud’s (often referred to as Raynaud’s disease) and secondary Raynaud’s (often referred to as Raynaud’s syndrome). Most people have the primary form of Raynaud’s. Primary Raynaud’s is diagnosed when no underlying condition is found. It is usually a benign condition with mild symptoms.
Secondary Raynaud’s is associated with another condition or disease. The most common conditions associated with Raynaud’s are autoimmune connective tissue or rheumatic diseases such as lupus, rheumatoid arthritis, or scleroderma.
Raynaud’s is often the earliest indication of an underlying connective tissue disease. For example, 95% of people with scleroderma have Raynaud’s (2). Scleroderma is a condition in which the immune system causes your body to make too much collagen. Secondary Raynaud’s may be complicated by acral digital ulcers and gangrene, requiring medical treatment.
Symptoms of Raynaud’s
Symptoms of Raynaud’s vary in type and intensity. For most people, Raynaud’s is not disabling but affects their quality of life. These are the main symptoms of Raynaud’s phenomenon:
- The affected area is cold
- Color changes in the skin in response to cold, stress, or exposure
- Area is numb
- Prickly feeling or stinging pain upon warming or stress relief
During an attack of Raynaud’s, the affected areas of your skin usually first turn white, then they often turn blue. This area will feel cold and numb until you are warm and circulation improves as normal blood flow returns to the area. During this time, the affected areas may turn red, throb, tingle, or swell. A typical attack lasts less than an hour but can persist for hours.
Causes and Risk Factors
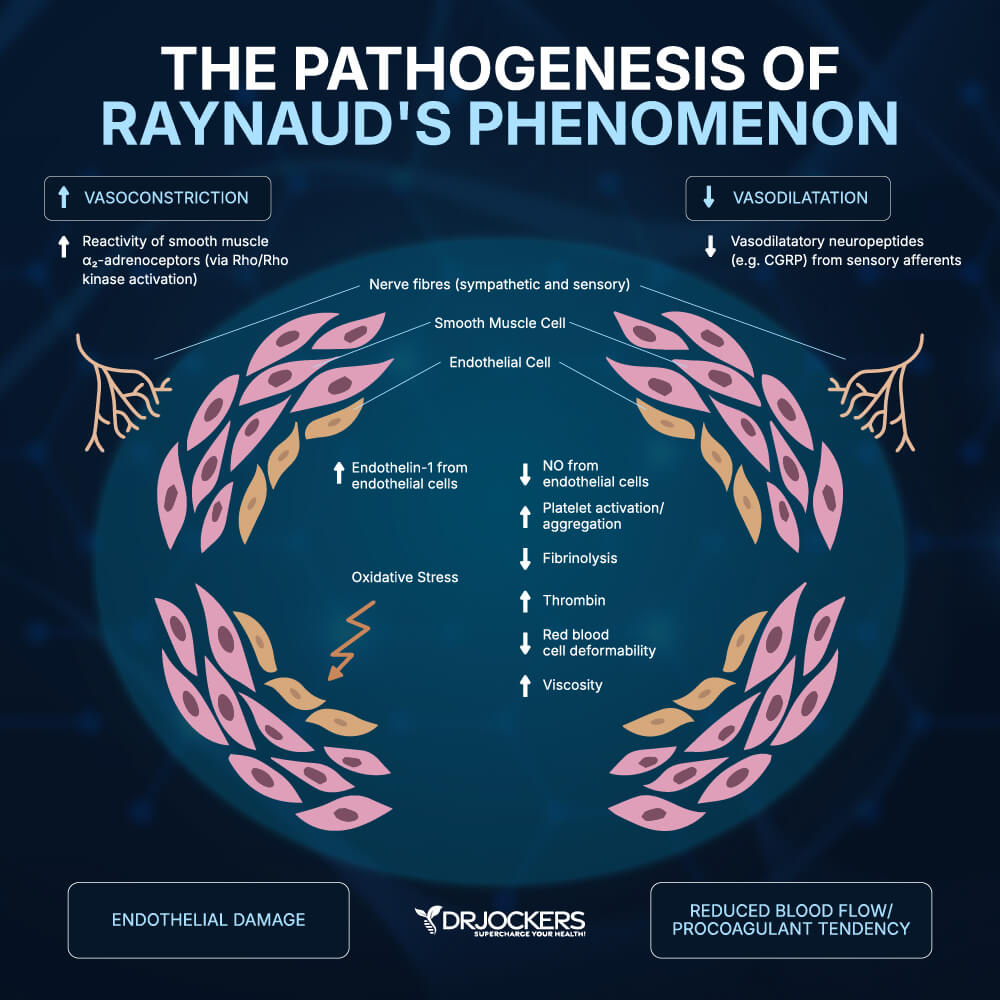
Despite more than 150 years of research, the exact pathology of Raynaud’s is not completely understood. There may be a genetic basis for Raynaud’s, but a strong causative link has not been affirmed.
Raynaud’s affects up to 10% of the general population (2). Women are more likely than men to get Raynaud’s. It is estimated that 5-20% of women and 4-14% of men have Raynaud’s (3). Primary Raynaud’s usually manifests between the ages of 15 to 25, while secondary Raynaud’s occurs more often in people over the age of 35.
The hormone estrogen plays a role in the development of Raynaud’s. There is a positive association between estrogen levels and Raynaud’s which is why women, especially premenopausal women, have a higher incidence of Raynaud’s (2).
Raynaud’s Risk Factors
Autonomic nervous system (ANS) dysfunction is another factor in Raynaud’s (4). Studies show there is sympathetic dysregulation and impairment of parasympathetic modulation of heart function in primary Raynaud’s patients (5). Overstimulation of the sympathetic (fight or flight) nervous system causes spasms of arteries, which results in reduced blood flow to the hands and feet.
Homocysteine and the MTHFR gene mutation may also play a role in Raynaud’s. Studies show that homocysteine levels are higher in people with Raynaud’s (6). Raynaud’s was more frequently observed in people with the MTHFR gene mutation.
Additional possible causes and risk factors for Raynaud’s include:
- Cold temperatures
- Emotional stressors
- Medications including those to treat cancer, migraines, depression, and high blood pressure
- Carpal tunnel syndrome
- Using vibrating tools (like jackhammers)
- Heavy metal exposure
- Chemical stressors (PVC)
- Smoking
- Taking stimulants
- Thromboangiitis obliterans

Diagnosing Raynaud’s Syndrome
Many people with Raynaud’s do not seek medical attention and dismiss their symptoms as poor circulation or just being sensitive to cold. When a person does seek medical attention, doctors often make a diagnosis based on the patient’s description of the color changes that occur suddenly after being exposed to cold temperatures.
Primary care doctors usually refer patients with Raynaud’s to a rheumatologist. Rheumatologists are doctors who have training in the diagnosis and treatment of musculoskeletal disease and systemic autoimmune conditions.
A helpful test for diagnosing secondary Raynaud’s is a nailfold capillaroscopy. This test is a simple microscopic examination of the small blood vessels (capillaries) at the base of the fingernail. It is used also to look for the presence of an underlying connective tissue disorder. This test can distinguish primary from secondary Raynaud’s.
Blood tests will typically include a complete blood count, comprehensive metabolic panel, erythrocyte sedimentation rate, muscle enzymes, rheumatoid factor, anti-cyclic citrullinated peptide, thyroid panel, and more. Many of these are included in the Comprehensive Blood Analysis.
It is important to test for antibodies associated with connective tissue diseases. The antinuclear antibodies test (ANA) tests for the presence of antibodies produced by a stimulated immune system which is common in people with connective tissue diseases or other autoimmune disorders.
There is no cure or gold-standard therapy for Raynaud’s. Conventional doctors commonly use medications called calcium channel blockers and vasodilators to relax blood vessels.

Natural Support Strategies for Raynaud’s
There are many natural support strategies that may be helpful for people struggling with Raynaud’s. If you have secondary Raynaud’s, addressing the underlying disease is also important. These strategies are not all FDA-approved for prevention, treatment or as a cure to Raynaud’s but they can be helpful for supporting the body and improving the condition.
1. Avoid the Cold
Avoiding the cold is the most effective therapy for any cause of Raynaud’s and is key to successfully managing the disorder (1). You should keep your whole body warm by wearing layered clothing, avoiding rapidly shifting temperatures, and avoiding cold and breezy conditions. For example, wear a hat, scarf, earmuffs, warm gloves, boots, and thick socks when you go outside in cold temperatures. It may also be helpful to wear gloves and socks to bed during winter.
Some other tips are to drink cold beverages out of insulated cups and protect your hands with gloves when you handle frozen food or other very cold items. If you experience a Raynaud’s attack, rub your hands under warm water to speed recovery. A typical attack lasts 15-20 minutes after rewarming (1).

2. Anti-Inflammatory Diet
Good nutrition is always important for any health condition. There are foods that can cause inflammation and intestinal permeability, both of which contribute to various health problems.
An anti-inflammatory, healing diet removes foods that cause inflammation and damage the gut lining. Instead, your diet should include organic, non-GMO vegetables, fruits, healthy fats, and clean protein. This will help to reduce inflammation, stabilize your blood sugar, reduce your toxic load, and support healthy blood pH levels.
Many people with Raynaud’s have nutrient deficiencies. An anti-inflammatory healing diet is nutrient-dense and will help to supply your body with the nutrients it needs.
Foods to Avoid With Raynaud’s
It is important to avoid highly inflammatory foods. Pro-inflammatory foods include:
- Refined sugars and grains (and any foods that are easily metabolized into sugar)
- Conventionally raised meat and dairy products
- Gluten-containing foods
- Farmed fish
- Processed foods
- Highly processed vegetable and seed oils, such as canola, grapeseed, and safflower
- Foods with additives and preservatives

Foods to Include
The foods you should be eating on an anti-inflammatory, healing diet are whole, unprocessed foods. Choose grass-fed and pasture-raised meats and wild-caught fish. Include a variety of low to moderate carbohydrate, lower glycemic, colorful vegetables, and fruits for their abundant antioxidants and phytonutrients. Plentiful amounts of herbs are a powerful addition to a healing diet.
Healthy fats are a very important part of a healing diet. Healthy fats are found in coconut, olives, avocados, and their oils and in grass-fed butter and ghee. Omega-3 fatty acids and conjugated linoleic acid (CLA) found in wild-caught salmon and grass-fed beef and dairy are fats with many health benefits. These healthy fats are an efficient source of fuel for the body to combat inflammation.

3. Add Warming Foods
According to traditional Chinese medicine (TCM), foods have thermal properties and are classified according to their energetic effects. Some foods are warming, blood building, and increasing energy. Certain other foods are cooling, detoxifying, and eliminating. Consuming warming foods that improve blood circulation may help to improve symptoms of Raynaud’s.
Foods with warming tendencies include garlic, leeks, onions, watercress, parsley, parsnips, ginger, dates (and most dried fruits), honey, leeks, and peppers. Warming herbs and spices are anise, basil, cumin, cinnamon, cloves, ginger, and rosemary.

4. Consider an Autoimmune Elimination Diet
For anyone with secondary Reynaud’s, an autoimmune elimination diet may be beneficial. An autoimmune elimination diet eliminates the most common allergenic/sensitive foods which may be contributing to or causing a negative reaction and inflammation. The goal in eliminating these foods is to identify foods that may be contributing to your autoimmune condition.
After the elimination period, you slowly reintroduce foods, one at a time, noting any reactions and symptoms you may experience. It is important to keep a journal during the entire process to document how you are feeling as you eliminate and reintroduce the foods. For more information on how to implement an elimination diet, check out this article.

5. Avoid and Detox Heavy Metals
Exposure to heavy metals is associated with the development and severity of Raynaud’s syndrome (7). Heavy metals such as nickel, lead, aluminum, and arsenic bind to proteins in the body causing oxidative stress, inflammation, and other health issues.
Arsenic exposure has been linked to Raynaud’s (2). Most arsenic gets into the body through ingestion of food or water. Common sources of exposure to arsenic are pesticides in commercially grown produce, rice, and apple juice. Arsenic in groundwater is a widespread problem.
6. Address High Homocysteine Levels
High homocysteine levels are associated with Raynaud’s. Homocysteine is an inflammatory amino acid that is produced as a byproduct of protein metabolism. Elevated homocysteine causes excessive blood clotting which diminishes blood flow to areas of the body.
Proper levels of methylated vitamins B2, B6, B12, folate, and magnesium help to prevent homocysteine from building up in the body. Vitamin B12 works with folate and its metabolites to change homocysteine into the non-toxic amino acid methionine. Providing proper methylation support can help to reduce homocysteine to a safe level.
It is important to test your homocysteine levels. The Comprehensive Blood Analysis measures your homocysteine levels. This thorough test also includes a CBC with differential, Complete Metabolic Panel, Fasting Glucose, Insulin, and Hemoglobin A1c, Lipid Panel, Iron Panel, Thyroid Panel, inflammatory markers, vitamins and minerals (zinc, copper, vitamins A, D, and B12, folate, magnesium), and more. It is a fantastic test to gauge overall health and identify potential health problems in their early stages.
7. Consider Acupuncture
Acupuncture may reduce the frequency and severity of Raynaud’s attacks (8). Acupuncture is a traditional Chinese medicine (TCM) practice. It has been used for more than 2,500 years to treat a variety of diseases, chronic pain, and stress-related symptoms.
With acupuncture, trained practitioners insert thin needles into the skin to stimulate specific points on the body. Acupuncture may be effective in improving pain severity and joint stiffness in Raynaud’s.
8. Manage Stress and Anxiety
Stress and anxiety cause blood vessels to constrict and reduce circulation. The sympathetic nervous system is activated, and your body has a fight or flight response during times of extreme stress or anxiety. This affects blood flow. It is important to reduce anxiety and manage stress if you have Raynaud’s.
To reduce stress and anxiety, it is important to consume a healing diet and balance your blood sugar levels. Grounding, deep breathing exercises, sunlight exposure, prayer and meditation, journaling, practicing gratitude, Epsom salt baths, prioritizing restorative sleep, exercising in nature, and dry brushing are fantastic stress-relieving strategies.
Supplementing with adaptogenic herbs such as ashwagandha, holy basil, rhodiola, and ginseng can be very helpful in balancing stress hormones. Most individuals with Raynaud’s need more magnesium and that plays an important role in reducing anxiety and improving sleep quality.

9. Reduce Chemical and Environmental Toxins
Exposure to chemicals and other environmental toxins may cause Raynaud’s. Chemicals such as polyvinyl chloride (PVC) have been linked to Raynaud’s (2). PVC is a colorless gas used in the manufacture of plastics.
To identify environmental toxins that may be in your body, you can do Environmental Toxicity Testing. The GPL-TOX measures levels of 172 chemicals, including PVC using advanced mass spectrometry.
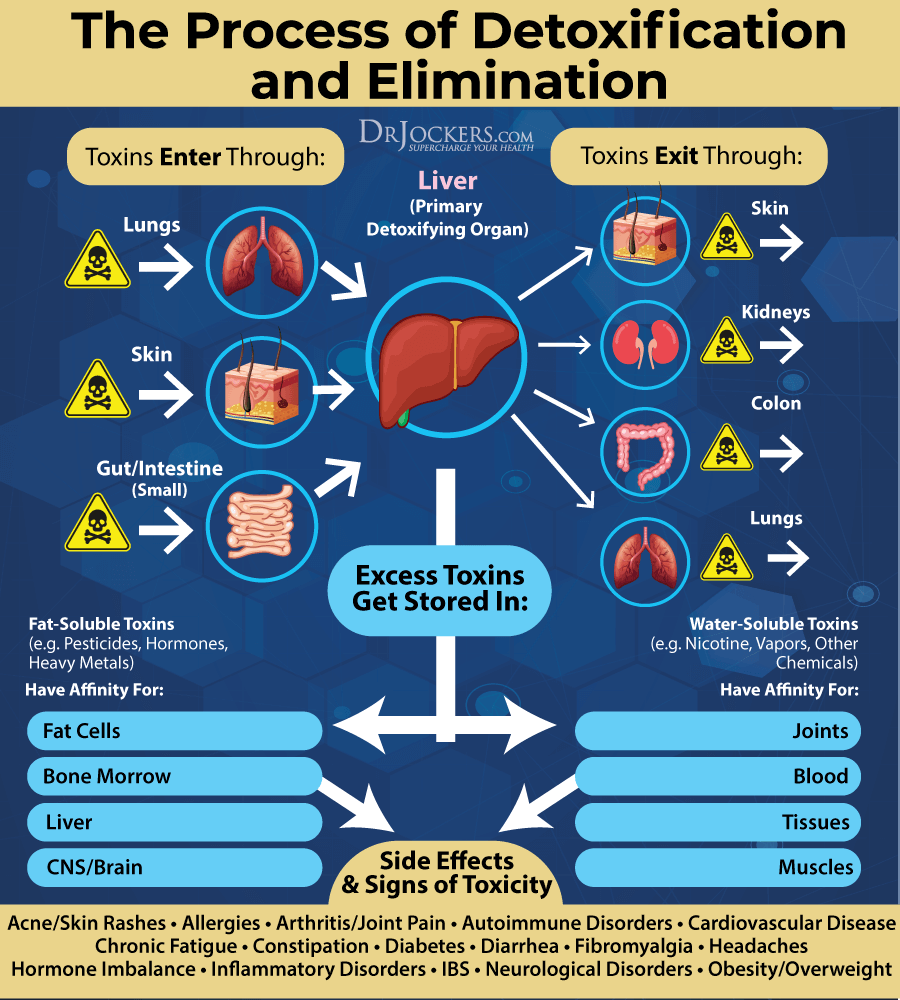
It is important to detoxify any environmental toxins from your body. There are many organs of detoxification, including the liver and gallbladder, skin, lymphatic system, lungs, and kidneys. It is important to support all of these detoxification organs to eliminate toxins and improve your health. Juicing, coffee enemas, sauna, lymphatic cleansing, physical exercise, breathing exercises, and regular bowel movements are all pathways to eliminate toxins.
To support the detoxification of chemicals from your body, we recommend adding bioactive carbons such as fulvic and humic acid to your protocol. Bioactive carbons work systemically throughout your body, bind to viruses, radiation, and chemicals, and works to remove environmental toxins from the body.
10. Avoid Vasoconstrictors
Nicotine is a stimulant that is found in cigarettes, as well as other tobacco and vaping products. It is an addictive substance that changes your brain chemistry. Nicotine can cause Raynaud’s because it constricts blood vessels. This restricts blood flow throughout the body and can damage blood vessels.
Cigarettes also contain other harmful substances, such as arsenic, which may contribute to Raynaud’s. It may also be helpful to avoid caffeine as well as vasoconstrictive medications. Be sure to discuss any changes to your medications with your primary care doctor.
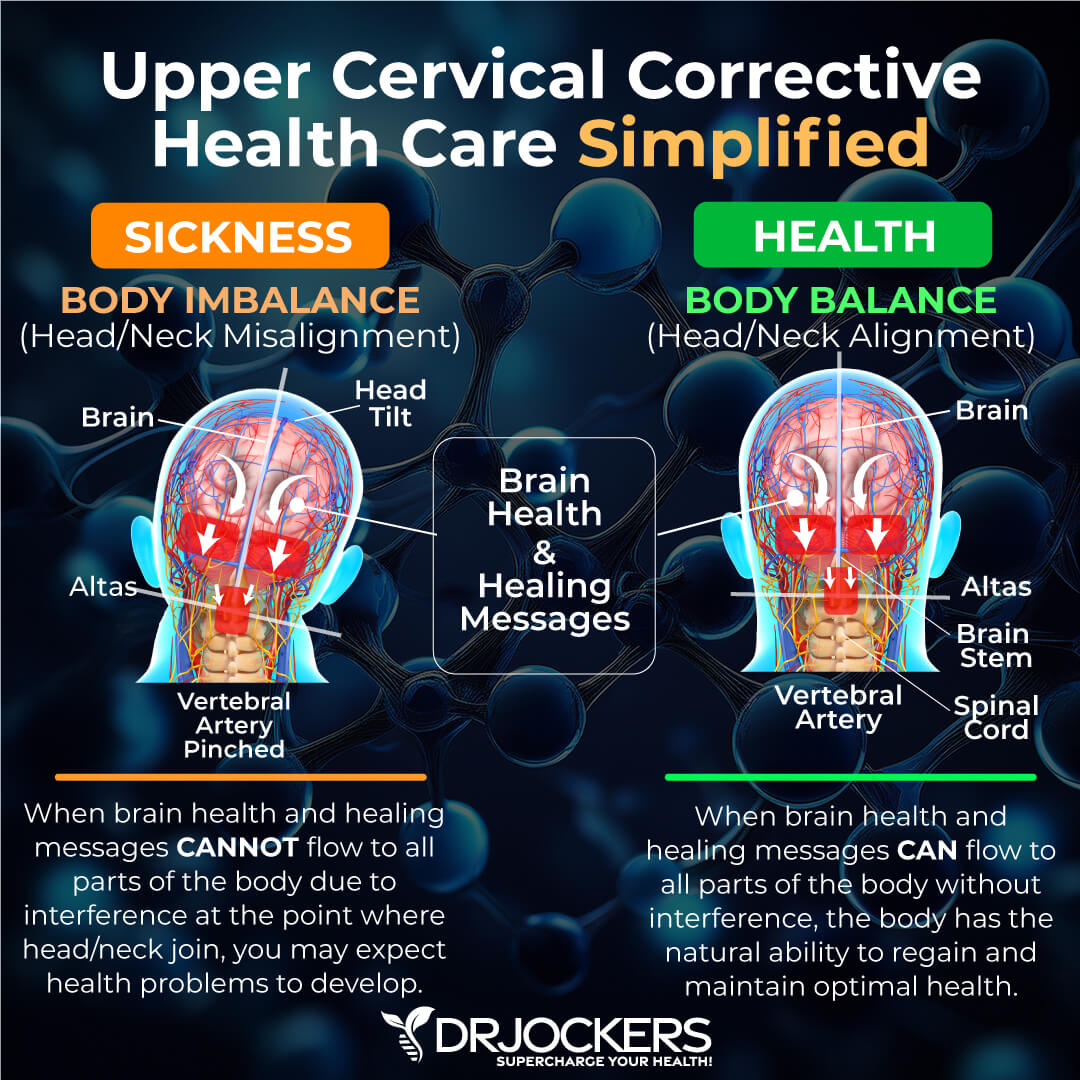
11. Chiropractic Care
The spine houses the nervous system, and the mobility of the spine affects the function of the nervous system. With Raynaud’s, the nervous system is stressed (overstimulated).
Increased stress on the body causes subluxation. Subluxation is the mechanical compression and irritation of spinal joints and nerves. Subluxation causes imbalances in the central nervous system between the sympathetic and parasympathetic systems.
Chiropractic care can remove upper cervical subluxations and restore proper structural and neurological function to the spine and nervous system. This helps to reduce stress on the body by improving the balance between the sympathetic and parasympathetic nervous systems. Chiropractic care may be very beneficial for anyone with Raynaud’s.
12. Essential Oils
Using essential oils, such as cypress, orange, thyme, and valerian, may be beneficial for Raynaud’s . Cypress strengthens the capillary walls and increases circulation. Orange and Valerian root have antispasmodic properties. Thyme may help with circulation.
There are many ways to use essential oils. You can apply essential oils topically, use them in a diffuser, or just breathe them in directly from the bottle. Essential oils are a safe and effective way to help symptoms of Raynaud’s.

13. Supplements to Improve Raynaud’s
There are several supplements that may help to improve the health of those with Raynaud’s. It is important to remember that these are not FDA-approved to prevent, mitigate, treat, or cure Raynaud’s but may improve the health of those who struggle with this condition.
Proteolytic Enzymes
Proteolytic or systemic enzymes promote healthy blood circulation. Enzymes clear unhealthy build-up in the circulatory system. They help to cleanse and detoxify the bloodstream. As a result, systemic enzymes enhance circulation and cellular oxygenation. Taking systemic enzymes may improve the circulatory issues in people with Raynaud’s.
Proteolytic or systemic enzymes are used to clean up fibrotic (scar) tissue in the body. These enzymes digest fibrolytic tissue and prevent fibrosis of our organs and tissues. Using proteolytic enzymes can help to break down antibodies associated with autoimmune conditions. It is important to note that these compounds are not FDA-approved to prevent, mitigate, treat, or cure Raynaud’s and should not be confused as such.

Omega-3 Fatty Acids
To improve blood flow, you should increase your intake of essential fatty acids. Essential fatty acids are essential fats that your body cannot produce. They include Omega 3 fatty acids which maintain cellular membrane health and have antioxidant, anti-inflammatory, and antifibrotic properties. Omega 3s may also help improve your tolerance to cold (11).
Omega-3 fatty acids are essential fats that are found in fatty fish such as wild-caught salmon and sardines, grass-fed meats, pasture-raised eggs, nuts (especially walnuts), and seeds (flax, hemp, and chia seeds). Flax, hemp and chia seeds have the added benefit of improving estrogen levels in the body which may play a role in Raynaud’s.
However, if your health is compromised, meeting your omega-3 needs may be difficult via diet alone, and you may benefit from supplementation.
Plant-based omega 3’s such as flax oil only contain the small chain omega 3 called ALA and do not have any DHA. It is very hard for our body to convert ALA into DHA so it is best to get a high-quality fish or krill oil that is rich in EPA and DHA. You want to find a brand that is molecularly distilled to take out any heavy metals and other unwanted contaminants.

Amino Acids
Nitric oxide plays a role in dilating blood vessels and mediating oxidative stress. In people with Raynaud’s, nitric oxide production in endothelial cells is decreased (9). Antioxidants help to fight free radicals brought on by oxidative stress, and nitric oxide is key in clearing them out.
L-arginine is an amino acid that helps to stimulate the production of nitric oxide and may reverse the tissue damage in those with Raynaud’s (10). L-arginine is naturally found in red meat, dairy products, poultry, and fish.
Bone broth is known for being a powerful immune tonic. Bone broth contains high levels of the amino acids L-glycine, proline, and hydroxyproline which act to improve liver health, support a healthy gut lining, and reduce inflammation throughout the body.

Magnesium
Magnesium is a crucial nutrient that supports over 300 physiological processes or functions in the body. It is called the “master mineral” and plays an important role in our overall health.
Magnesium maintains the relaxation of the smooth muscle of the small arteries, which helps to improve blood flow. People with Raynaud’s may have low levels of magnesium (12).
The top food sources of magnesium are leafy greens such as Swiss chard and spinach, sea vegetables, sprouts, and avocados. Grass-fed dairy and wild-caught fish are rich in magnesium. Pumpkin seeds, nuts, dark chocolate, and coffee are also good sources of magnesium.
I am a big fan of magnesium supplementation with an amino acid chelate form such as magnesium citrate, malate, lysinate, and glycinate. I also like magnesium L-threonate, the only form of magnesium proven to cross the blood-brain barrier.
Other great ways to get magnesium are Epsom salt baths and a topical cream or spray. Boosting your magnesium level is important for hormonal balance and overall health.

Curcumin
Turmeric is a powerful herb with abundant health benefits. It has been used for centuries to treat a variety of conditions. Turmeric has anti-inflammatory, antioxidant, anti-thrombotic, and antimicrobial properties. It is also a natural anticoagulant.
Curcumin is the active component of turmeric. The curcuminoids in turmeric help to boost the body’s natural antioxidant capacity to fight damaging free radicals. Due to its antioxidant, and anti-inflammatory effects, curcumin has an important role in the prevention and treatment of many conditions.
Turmeric powder should be added to foods after cooking to maintain its potency as an anti-inflammatory. Add a dash of black pepper and eat with healthy fats to allow for better absorption of the beneficial compounds.

B Complex Vitamins
B vitamins may be helpful for Raynaud’s. Vitamins B6 and B3 (niacin) may be particularly beneficial. Niacin causes blood vessels to dilate and stimulates circulation to the skin. B6 is necessary for the utilization of amino acids in the body. It also helps to regulate homocysteine and to maintain healthy blood vessels.
Foods that are rich in B vitamins include beans and peas, beef, wild-caught fish, pastured chicken and turkey, green leafy vegetables, dairy, and eggs. It can be difficult to obtain adequate amounts of all of the B vitamins from food. Supplementation with a high-quality B complex is a great way to ensure you have optimal amounts of these important vitamins.
A good B complex includes the pre-activated forms of vitamins B1, B2, B3, B5, B6, B7, B9 (folate), and B12 (as methyl-cobalamin). This combination of B vitamins supports mitochondrial, adrenal, and neurological function. Including a B complex multivitamin can be an effective strategy for improving the health of those with Raynaud’s.

Raynaud’s Conclusion
Raynaud’s phenomenon is a condition that causes the ends of the fingers and toes to feel cold, numb, and tingly. With Raynaud’s, blood vessels in the hands and feet overreact to cold temperatures or stress constricting blood flow to affected tissue. The skin can change colors, from white to blue to red.
There are two types of Raynaud’s, primary Raynaud’s and secondary Raynaud’s. Secondary Raynaud’s is associated with connective tissue and other autoimmune conditions. With secondary Raynaud’s, it is important to address the underlying condition to improve Raynaud’s symptoms.
Avoiding cold is the most important strategy for anyone with Raynaud’s phenomenon. Other natural strategies that may help to improve Raynaud’s are an anti-inflammatory diet with warming foods, acupuncture, using essential oils, managing stress, and chiropractic care. Avoiding and detoxing your body from chemicals and heavy metals is very important. It is important to test for and reduce high levels of homocysteine and to avoid nicotine and other vasoconstrictors. Targeted supplementation may also be beneficial.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. On our website, we offer long-distance functional health coaching programs. For further support with your health goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!





Under “ACUPUNCTURE” I don’t think “think needles” are inserted! I also don’t think anybody ever proof-reads these articles, but some typos are funnier than others! 😁
I am not sure where you are seeing that. It says “thin needles.”
Gluten may cause Raynaud’s. Gluten is wheat/barley/rye…oats/corn/rice. Rice is low in gluten. GMO/Roundup may also hurt. People who are gluten/GMO free may have 10 health issues disappear fast.
Yes a gluten-free, GMO free diet can help a lot!
I would like to see an article in depth on Transverse Myelitis.
Yes perhaps we will do that down the road!
Thank you so much for this article. It’s the most comprehensive I’ve seen, and has great resources and action items!
Great to hear that Wendy!
good article but not thorought enough. The infectious background is not listed. MYcoplasma, Chlamydia and borrelia infections all can cause sec.Raynaud. there are articels available. Also there are other supplements which are helpful in Raynaud which i snot listed here and also techniques.
Yes these are infections that can be triggers Anna! Blessings!
This article is baloney!! I have had Raynaud’s for 50 years!! It effects EVERYTHING in your body as it is a blood disorder which is essential in the human body! It is not brought on by stress or cold weather alone. Doctors have no clue as to why it happens and make up their own hypothesis and have no clue as to how to treat it. The answer is get warm clothes and sit next to a heater with a blanket. Do your homework and get tested for Lupus!!
Thank you for sharing your thoughts Anne!
Have you seen any help with castor oil packets or application to the hands? Thank you!