 Breast Cancer: Causes, Symptoms, and Natural Support Strategies
Breast Cancer: Causes, Symptoms, and Natural Support Strategies
In Western countries, 12% or 1 out of 8 women develop breast cancer. In 2021, an estimated 261,840 new cases of invasive breast cancer were expected to be diagnosed in women in the U.S., along with 60,290 new cases of non-invasive (in situ) breast cancer.
Addressing key hormone levels and epigenetic immune system modifiers, such as vitamin D3 and glutathione, is critical for preventing or reversing breast cancer naturally. (23) Here are 12 natural support strategies to improve hormone and immune health.
Breast tissue is highly estrogenic, and estrogen is a major growth phase hormone in the body. Your risk of breast cancer comes down to your genetic profile, your levels of immune system modifiers such as glutathione and vitamin D3, and your hormone ratios.
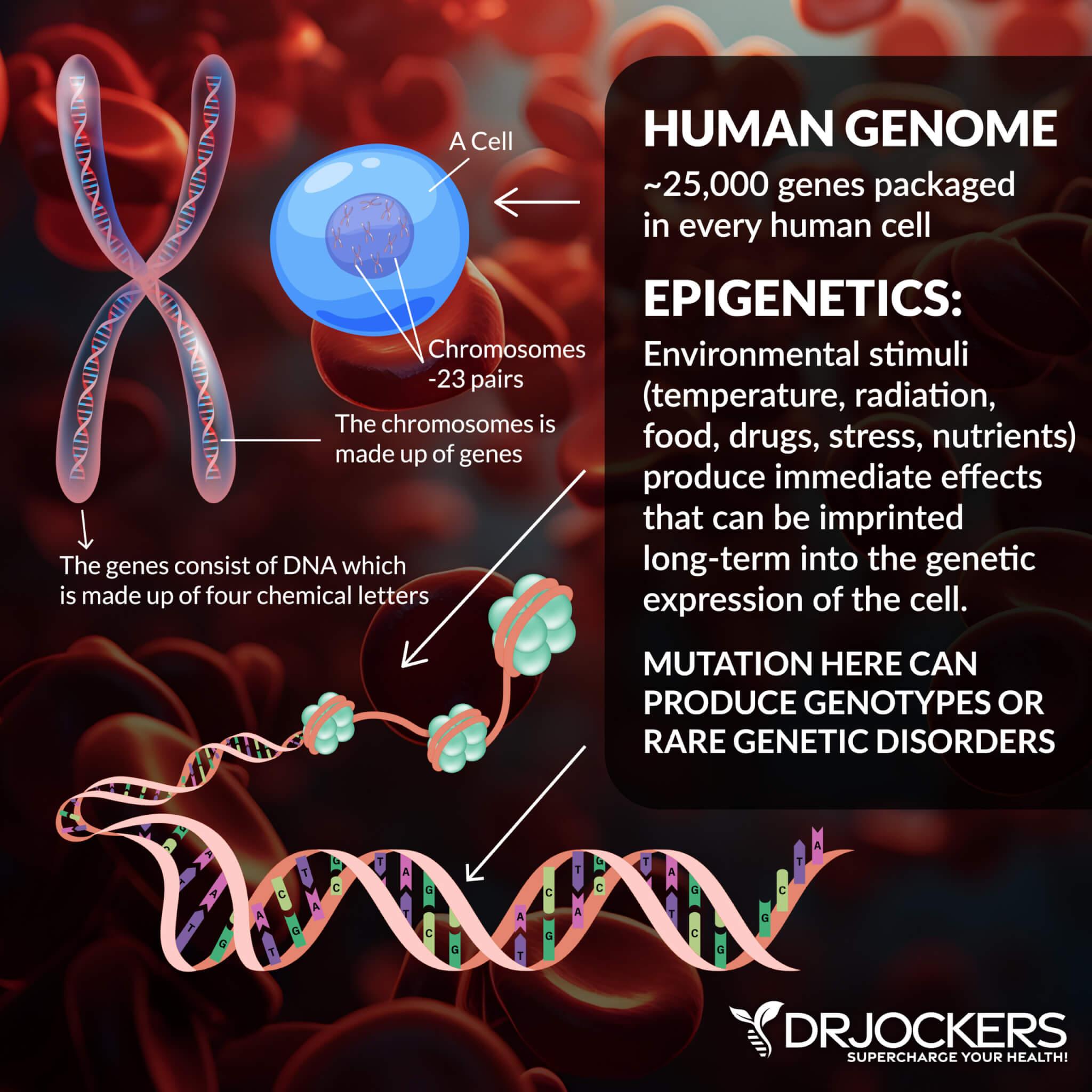
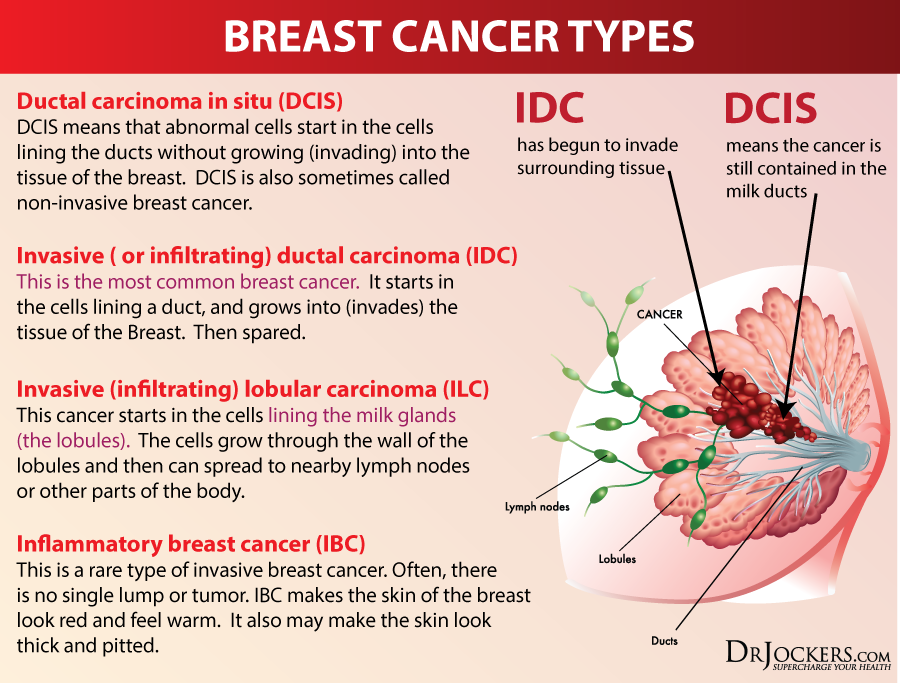
The 2 Classifications of Breast Cancer:
Contrary to popular belief, there are actually several different types of breast cancer. To properly diagnose the cancer type, there are two main categories that must first be assessed: (13)
- Noninvasive (in situ) breast cancer: Cancer is specific to the breast and has not spread to surrounding tissue, lobes (glands), or ducts (tubes).
- Invasive breast cancer: Cancer metastasizes to other parts of the body through the bloodstream and lymph nodes.
Breast Cancer Types
Breast cancer is further classified depending on the origin of the disease. Some of the most common types of breast cancer and some of their subtypes are: (13, 24)
- Invasive Breast Cancer: Also known as infiltrating breast cancer, this type of breast cancer spreads to tissue around the breast or other regions of the body. IDC (invasive ductal carcinoma) makes up 70% of all invasive breast cancer types and begins in the milk ducts.
- Ductal Carcinoma: This cancer is one of the most common cancer types and originates from the milk ducts, which carry breast milk to the nipple. Ductal carcinoma in situ (DCIS) is known to involve the cancer-promoting oncogene AC.
- Lobular Carcinoma: Lobes (glands that produce breast milk) are the original site of this cancer. This typically noninvasive form of breast cancer, lobular carcinoma in situ (LCIS), elevates the risk of developing invasive breast cancer in the future.
- Inflammatory Breast Cancer (IBC): IBC results in the blockage of lymph vessels in the skin of the breast from infected soft tissue. The description “inflammatory” is associated with the appearance of itchy, red, tender, warm, and firm breasts resulting from the accumulation of white blood cells and stimulated blood flow in the skin.
- Male Breast Cancer: This type of breast cancer develops from any cellular malignancy in breast tissue. Male breast cancer is most common in men between the ages of 60 and 70. A disorder known as gynecomastia in teenage boys can trigger concerns for cancer, but is rarely caused by a tumor.
- Metastatic Breast Cancer: This cancer is characterized by the spread of cancer cells to other areas of the body. Common locations for the metastatic breast cancer are the chest wall, the area where the breast used to be, lymph nodes, bones, lungs, tissue around the lungs, liver, and brain.
- Paget’s Disease of the Breast: A specific skin change on the nipple or areola may resemble eczema, but is actually evidence of this rare form of disease and breast cancer. This type of breast cancer results in 4.3% of breast cancers.
- Papillary Carcinoma: A rare breast cancer, papillary carcinoma is apparent by fern-like projections of cancer cells. This cancer is treated like invasive ductal carcinoma, although the prognosis is better than other invasive types.
- Triple Negative Breast Cancer (TNBC): Usually invasive, this type of breast cancer accounts for 10 to 20% of all breast cancers and originates from the breast ducts. These types of cancer cells do not contain receptors for estrogen, progesterone, or a protein called HER2, as do normal breast cells. On the other hand, 20 to 30% of breast cancer cases are characterized by the overexpression of HER2 receptors responsible for stimulating cell growth.

BRCA1 and BRCA2 Mutations
BRCA1 (BReast CAncer 1) and BRCA2 (BReast CAncer 2) are inherited gene mutations that are linked to an increased risk for the development of breast cancer. BRCA1 and 2 are both tumor suppressor genes, which means that they should function to prevent cell reproduction and proliferation. BRCA1 is on chromosome 17, while BRCA2 is located on chromosome 13. (14)
About 1 in every 400-800 people in our population carries an inherited mutation in BRCA1 or BRCA2, and roughly 5% of all breast and ovarian cancers are due to these mutations (25). Another 10% of breast cancer cases are in individuals with a family history of breast cancer but who do not carry the BRCA gene mutation.
The other 85% of breast cancer cases occur in women who did not have a previous family history of breast cancer. These are cases of epigenetic or environmental stressors, such as toxicity and emotional stress, that cause the breakdown and mutation in the genetic structure that leads to cancer cell proliferation.
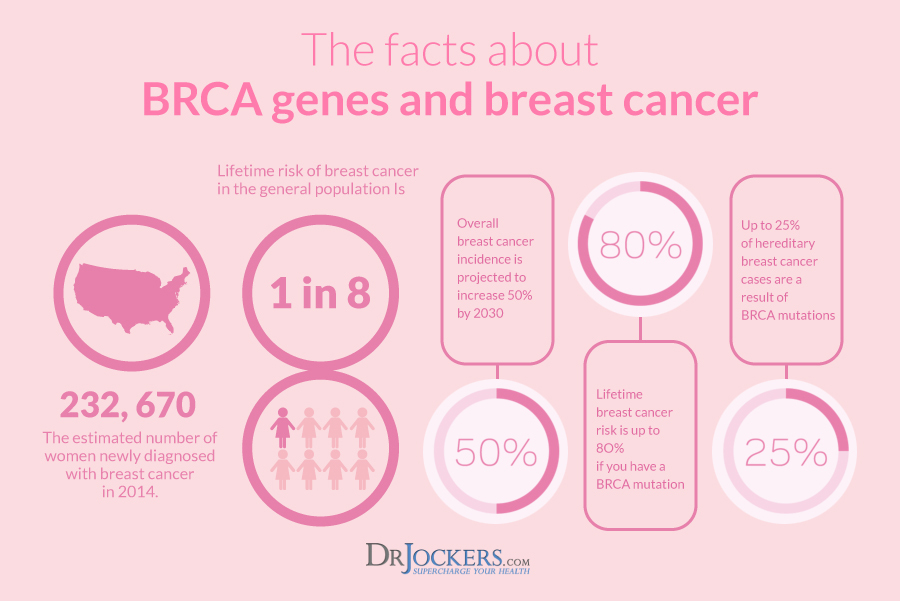
BRCA and Breast Cancer Risk
Mutations in these genes increase the risk of developing breast cancer by 60-87% and the risk of developing ovarian cancer by 20-54% (5). A mutated BRCA gene can be inherited from either of the parents. This is why it is called a hereditary mutation, because it is from the direct germline. An acquired or somatic mutation comes through environmental stressors.
The BRCA1 gene plays a very important role in stopping the development of cancer. Women who have inherited a damaged version of this gene will have a higher risk of developing breast cancer. BRCA1 may also get altered through environmental stressors that “switch it off” in as many as 30 percent of tumors in patients who had a normal version of the gene.
The BRCA1 mutation is most commonly associated with triple-negative breast cancer, which does not respond to hormonal treatments, chemotherapy, or radiation (15). These individuals will often have breast cancer appear about 2 decades earlier in the 25-45 age range.
BRCA2 is associated primarily with post-menopausal breast cancer, although the risk of pre-menopausal breast cancer is significant. It is typically highly responsive to hormonal treatments. (16)
Of course, a lot of women also get breast implants after a mastectomy due to breast cancer or breast cancer prevention with a breast cancer gene. It is also important for women to be aware of the signs of breast cancer to differentiate between post-surgery changes and potential warning symptoms.
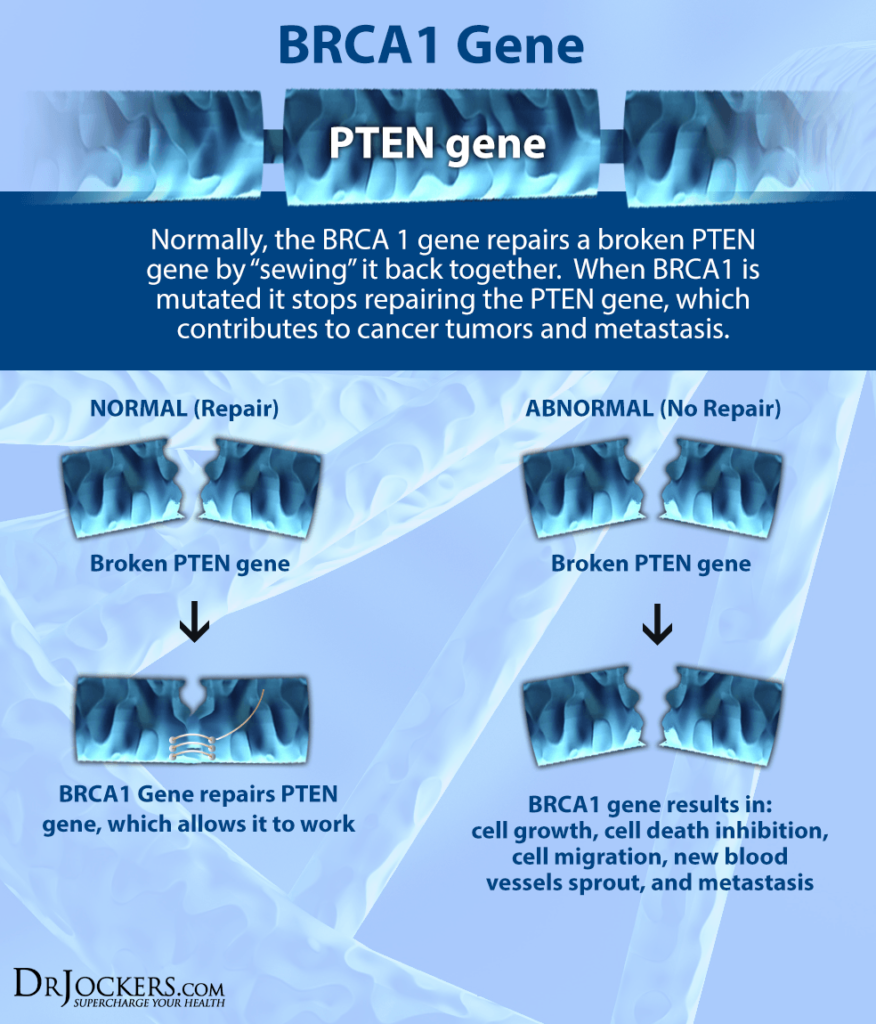
How BRCA Works
By nature, the BRCA gene works to suppress cell reproduction and proliferation. Cancer cells are highly proliferative, which means that they reproduce very quickly.
BRCA produces proteins that are used by the cell in specific enzymatic pathways to repair DNA molecules that have double-stranded breaks. BRCA1 also upregulates intracellular antioxidants such as glutathione, which helps protect the DNA from oxidative stress (8).
This process of precise DNA repair orchestrated by BRCA is extremely important to the integrity of our genome. If this process is not performed effectively, then it leads to abnormal cell development and proliferation. The whole goal of BRCA1 is to ensure that DNA information has been accurately replicated and translated into the daughter cells. It is a key safeguard of the genome.
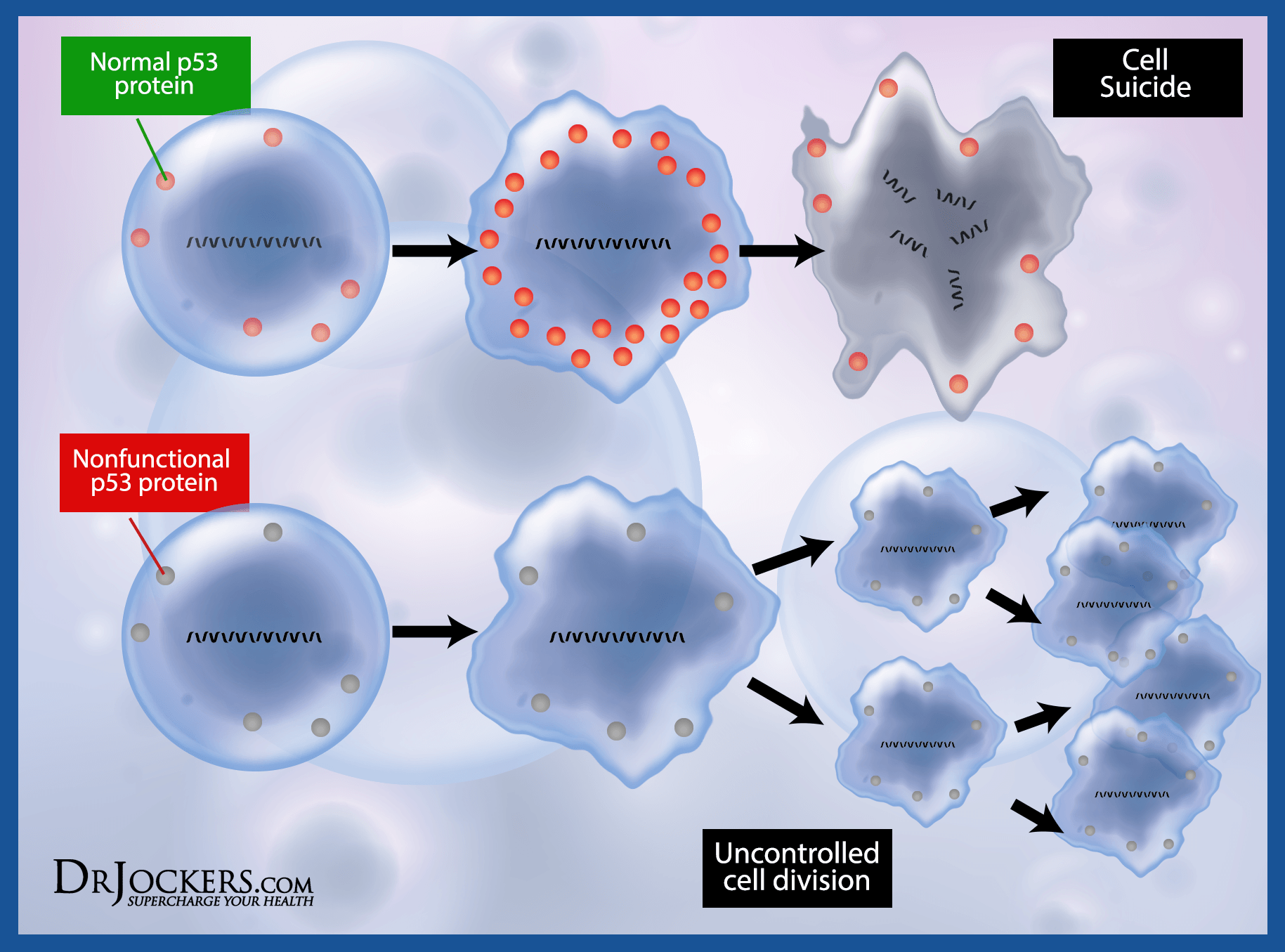
The body has the p53 gene (53BP1 in breast tissue) as a backup to the BRCA gene in order to regulate cell division and protect the genome. If the BRCA gene is unable to do its job effectively, 53BP1 would signal for the cell to go through a programmed death called apoptosis (26).
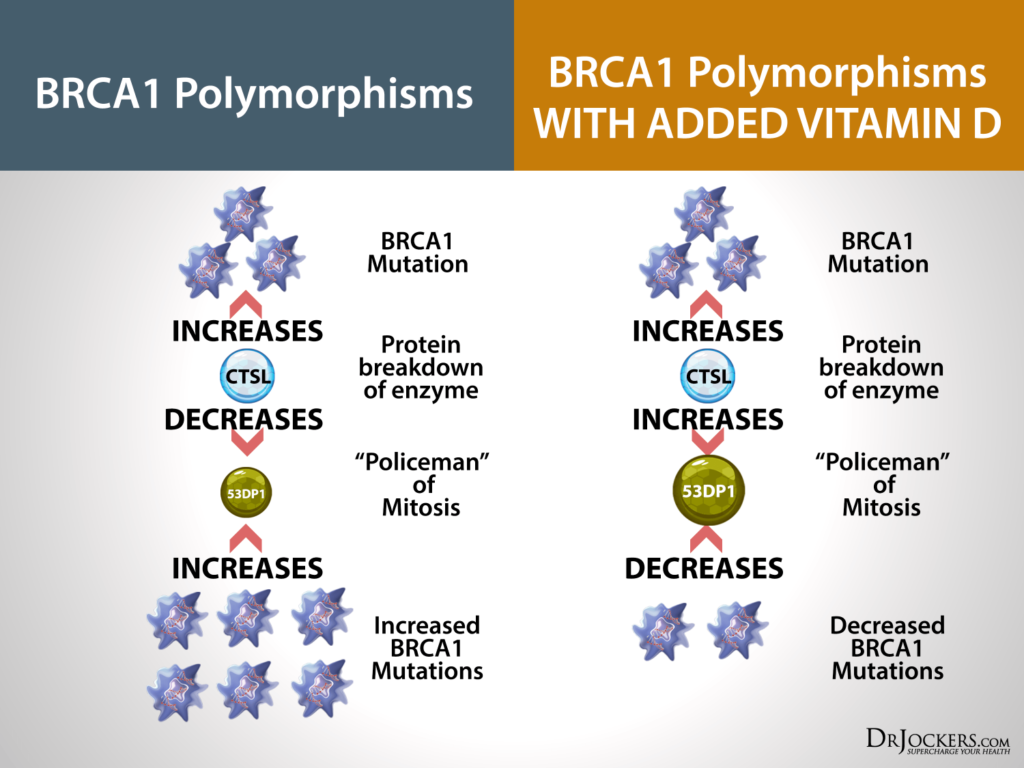
Certain types of mutations in the BRCA genes increase the activity of a protein-degrading enzyme called cathepsin L (CTSL), which breaks down 53BP1 (27). This allows for the proliferation and survival of the BRCA-mutated cell and the growth of an abnormal cell line.
Vitamin D and BRCA
Vitamin D has been known to regulate the epigenetic expression of thousands of genes. It helps to downregulate inflammation and oxidative stress at the tissue, cell, and genomic level, and it may be the secret key to reducing cancer risk in individuals with BRCA mutations.
Susana Gonzalo, Ph.D., and her research team published a powerful paper in the January 2013 edition of The Journal of Cell Biology (28). Her team showed that vitamin D inhibits CTSL-mediated breakdown of 53BP1 in non-tumor cells. During this study, they found that treating the BRCA1-deficient tumor cells with vitamin D restored high levels of 53BP1.
This increased the genomic stability and reduced the proliferation of abnormal cells. This study specifically found this issue in triple-negative breast cancers, which are the most challenging cases because they don’t respond to conventional treatments.

Optimizing Vitamin D Levels
Individuals with BRCA1, BRCA2, a family or personal history of breast cancer should optimize their vitamin D3 levels. One can do this by getting high-quality sun exposure that creates a light color change in their skin (pink, tan, or darker) without burning. If you do this over 40% of your body weight, you have gotten 10-20,000 IU of vitamin D.
Getting vitamin D3 levels checked every 90 days is highly recommended, and keeping the levels between 50-100 ng/ml is ideal. Individuals with chronic inflammatory diseases like cancer should aim to get their levels around 80-90 ng/ml.
Regular sun exposure and supplementing with 5-10,000 IU of vitamin D3 daily (take a supplement with a fat-based meal) will typically get the levels into this range. (21)

Glutathione and BRCA
BRCA1 and BRCA2 play a key role in controlling oxidative stress levels within the cell and in the DNA strands themselves. When these genes are mutated, they lose their ability to control oxidative stress within the genome. This leads to increased oxidative damage to the DNA and genomic instability.
Glutathione is the body’s master antioxidant and the most important antioxidant for protecting the DNA particles. Individuals with this gene mutation produce less glutathione endogenously (within the body) but can increase exogenous (acquired) glutathione levels through natural lifestyle strategies. (20)
The most important factors include a nutrient-rich diet full of vegetables, organic meat, herbs such as turmeric, onions, and garlic, along with fermented foods. Good sleep and stress management, as well as regular exercise, are especially key.
Additional supplementation with S-Acetyl Glutathione, Alpha Lipoic Acid, milk thistle, selenium, and N-Acetyl Cysteine is also extremely helpful and highly recommended for someone with BRCA gene mutations or a history of cancer.

Estrogen Quotient Testing
Estrogen is an essential hormone for the function and well-being of the female, and at a reduced level in the male body. Estrogen can be broken down into 3 major subtypes. The ratios of these subtypes give us a lot of critical health information that correlates to the risk of someone developing a hormone-sensitive cancer.
Estrogen is considered a growth and development hormone that is manufactured from cholesterol by a woman’s ovaries. It is also produced in lower concentrations in the fat cells and the adrenal glands in both males and females. The estrogen circulates in the blood and passes in and out of all the organs and tissues, and is eventually metabolized by enzymes in the liver. (22)
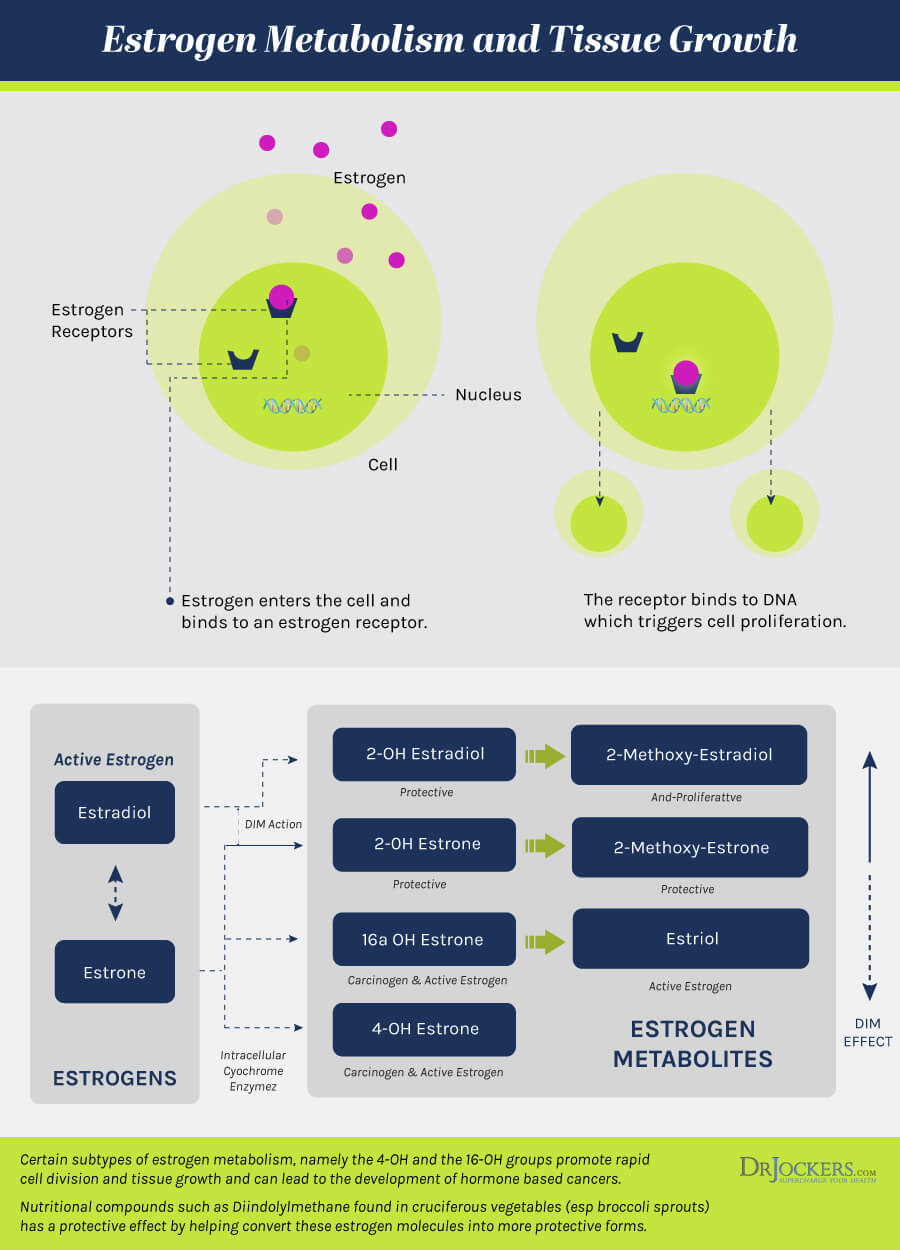
Three Major Estrogens
- E1 or Estrone: This is the main form of estrogen produced during menopause. This is produced mainly in your liver and fat cells. Since toxins such as xenoestrogens, heavy metals, and other pollutants that directly affect hormone levels are stored in your liver and fat cells, individuals with higher levels of toxicity have altered and contaminated forms of estrone.
- E2 or Estradiol: This is the predominant estrogen produced during reproductive years, and it is ten times more potent than E1 and about 80 times stronger than E3. Elevations in estradiol are linked to cancers of the breast, ovaries, and uterus.
- E3 or Estriol: This is the protective form of estrogen that reduces cellular growth factors and other estrogens. Estriol reduces the more aggressive estradiol and protects against radiation induced cancer of the breast. We should normally have a ratio of 90% Estriol, 7% Estradiol, and 3% Estrone in what is referred to as the Tri-Estrogen Formula. (17)

The Estrogen Quotient
The overall ratios of these hormones are titled your Estrogen Quotient or EQ. This formula was developed by estrogen researcher Dr Henry Lemon (29). He discovered that the greater the amount of cancer protective E3 is present in comparison to the growth promoting E1 and E2, the lower the risk of estrogen sensitive cancer development.
The EQ is found through the following formula:
Total E3
Total E1+Total E2
If the EQ is below 1.0, the risk of Breast Cancer is higher than that of the individual whose EQ is above 1.0. The optimal ratio that is considered most protective to breast tissue is an EQ that is greater than 1.5. This quotient can also be useful to determine other aspects of hormonal health and risk of autoimmunity.
Estrogen Receptors and Tissue Growth
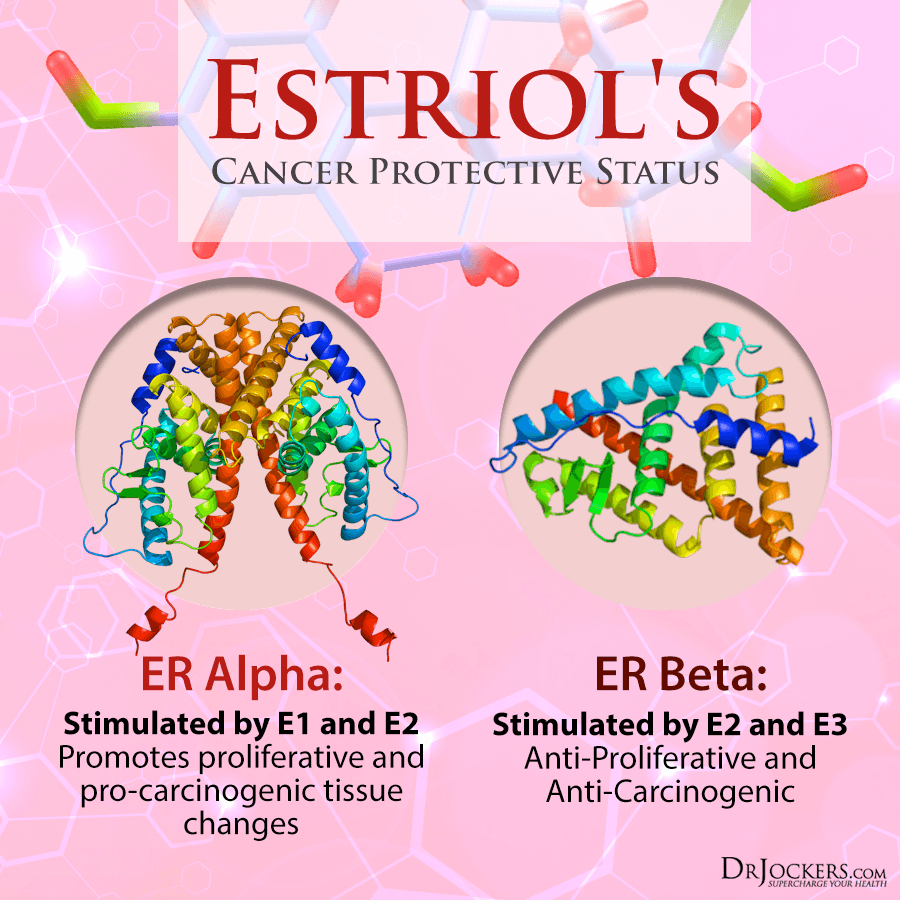
The estrogen receptor alpha (ER-alpha) is stimulated by both E1 and E2. ER-alpha receptor activation is considered to promote proliferative and pro-carcinogenic tissue changes. This receptor is found in the blood vessels, hypothalamus, ovaries, breast, liver, prostate, endometrium, lung, and testes. (18)
The estrogen receptor beta (ER-beta) is stimulated by E2 and E3. The ER-beta receptor activation is considered to be anti-proliferative and anti-carcinogenic. This receptor is found in the blood vessels, kidneys, prostate, breast, heart, skin, brain, intestines, endothelial cells, bone, and lungs. (19)
Estriol’s Cancer Protective Status
According to Dr Jonathon Wright, MD, “Most conventional physicians and pharmaceutical researchers have long dismissed Estriol as a weak and unimportant estrogen. They have considered it to be primarily a metabolite of Estradiol and Estrone, which are far more potent in producing estrogenic effects.” (29)
Estriol acts much like many plant estrogens in that it benignly binds to ER-beta receptors throughout the body and especially where they are dense in the uterus and breast. Estriol and plant estrogens have a much weaker estrogenic effect than E1 and E2 and thus shield the tissues from the more potent estrogens.
It is hypothesized that many xenoestrogens, artificial estrogens, act more like the stronger estrogen molecule E2, and thus, when they are not detoxified, they end up leading to symptoms of estrogen dominance. European studies have demonstrated that higher Estriol counts in menopausal women are correlated with lower menopausal symptoms such as incontinence, vaginal drying, thinning hair and hot flashes.
Early Detection
The American Cancer Society summed up their look into new studies involving the risks and benefits of breast cancer screening with updated guidelines in October of 2015. New recommendations follow for women with an average risk: (1)
- Most women should receive yearly mammograms starting at age 45.
- Women should speak with their medical provider if they choose to begin screening at age 40.
- Women should have mammograms every other year starting at age 55.
- So long as a woman is in good health, she should receive regular screenings.
- Both breast exams by a doctor nor self-exams are recommended.
These recommendations contradict the American College of Obstetricians and Gynecologists guidelines, which maintain that women should receive a clinical breast exam and regular screenings starting at age 40.
Experts analyzing the efficacy of early breast cancer detection learned that women between the ages of 40 to 69 who received regular mammograms reduced the number of breast cancer deaths (2). Dr. Richard Wender with the American Cancer Society stated that a “woman should make a personal decision as to whether she should start screening before age 45, but we clearly recommend that by age 45 all women should start regular screening every year (3).”
So, what is the right choice for you to make, and should mammograms be the recommended strategy for early detection screening?
Breast Examination
The absence of pain in a breast lump is not a sign of the absence of breast cancer as up to 98% of women in some countries may believe. Completing monthly breast self-examinations can help reduce mortality rates associated with breast cancer by increasing the likelihood that a woman will receive attention from a healthcare practitioner immediately. In fact, awareness that “early cancer lump is painless,” as it is coined, is an effective strategy for women in low and middle-income countries to decrease breast cancer mortality. (4)
Keeping cost-effective breast cancer screenings on the public health agenda in countries like the U.S. may seem worth its benefits to you. Conducting breast self-examinations continues to raise awareness of a disease that is the most common cancer in the world amongst women (6).

Risk of Mammography
The high cost and funding for mammograms may be partially to blame for the general public’s assumptions that mammography testing is essential to detecting breast cancer. Unfortunately, there are several risks and dangers involved in mammography use that you should be aware of.
- Radiation Exposure: Patients are exposed to ionizing radiation to produce an X-ray image of the breasts (9). For instance, cancer promoters such as oncogene AC prevalent in DCIS become stimulated from exposure to radiation during mammograms, increasing the risk of developing breast cancer.
- False Positives: Doctors in both the medical and natural health communities are skeptical of the high percentage of false positives detected during screening. False positives lead to further unnecessary, invasive, and dangerous testing that results in no presence of tumors in 70-80% of cases (12).
- Financial Burden & Stress: Patients undergo a considerable amount of pain and stress in receiving mammograms. Both the screening and treatment costs are enough to burden any individual and family, promoting greater emotional and physical stress.

Benefits of Thermography
Thermography testing is a new tool designed to detect physiological abnormalities present in the body. A digital map is produced using heat patterns that identify inflammatory pathways associated with infection and cancer. This type of screening can be used well before the presence of a large mass is detectable on a mammogram by providing detailed information on vascular function. Mammograms only detect anatomical changes. (7)
Thermography screening works by providing a relatively accurate image of blood flow and temperature of areas in the body. Areas that present a state of thermal asymmetry may indicate cancerous development. Cancer cells rely on a steady supply of blood flow and nutrients, resulting in the image of increased heat to the infected area.
Although thermography is not FDA-approved to diagnose breast cancer or any other medical condition, it can pick up on early levels of inflammation and abnormal cell growth, an estimated 10 years prior to the identification of a tumor by a mammogram.
Thermography screening was found in a large and longer-term study over 30 years and consisting of 250,000 women, to be 90% accurate. Unlike mammograms, thermograms are more cost-effective, painless, non-invasive, reliable, and safe (10, 11).

12 Ways to Support Hormone and Breast Health
Here are the best action steps to get started with on your journey to support hormone and breast health naturally. It is important to note that these strategies are not FDA-approved to prevent, mitigate, treat, or cure breast cancer and should not be confused as such.
You should always consult with your physician before stopping or changing medications or taking on new health strategies. Additionally, you should be working with a functional health practitioner to help guide you through these strategies. This is not an exhaustive list, and there are other natural therapeutic strategies that I and functional health practitioners will utilize to help individuals with breast cancer.
Anti-Inflammatory Diet:
Following a nutrition plan that is low in sugar and carbohydrates and rich in antioxidants, healthy fats, and clean, organic protein is extremely important. Be sure to avoid commercially raised meats, trans fats, and high sugar foods.
Load up on healthy fat sources like coconut products, avocados, grass-fed butter, and olives and olive oil. Get a lot of vegetables, herbs, and low sugar fruits like berries in your diet. Look for organic and grass-fed/pasture-raised animal products.

Optimize Your Vitamin D Levels:
Low vitamin D3 is associated with poor cellular growth control and increased risk of breast cancer. Scientists have found that vitamin D pathways used to treat breast cancer cells result in a 100% decline in cancer cell activity following a quick 7-day incubation period.
These in vitro studies suggest that D3 enables the ability of GcMAF to attack and eradicate human breast cancer cells. Researchers believe that an interaction between amino acids allows GcMAF receptors to effectively bind and stimulate the invasion of macrophages around cancer cells. Such macrophages are then able to “eat” and eliminate breast cancer cells. (30)
Be sure to increase your vitamin D through good amounts of regular sun exposure and/or taking a high-quality vitamin D3/K2 supplement. Ideal levels for chronic disease treatment are thought to be between 70-100 ng/mL. You can get tested a few times a year to see where you are at and supplement with roughly 1,000 IU per 25 lbs of body weight to improve and maintain ideal levels.

Good Sleep:
It is absolutely critical to sleep well in order to produce healthy sex hormones. Inadequate sleep will result in elevated stress hormone production and estrogen imbalance. It also causes blood sugar imbalances and abnormal breast growth.
The major sleep hormone, melatonin, has potent anti-cancer and immune supportive properties. When you have poor sleep habits or poor-quality sleep, you produce less melatonin, and this is detrimental to immune health. Follow the strategies in the image below to optimize your sleep quality.

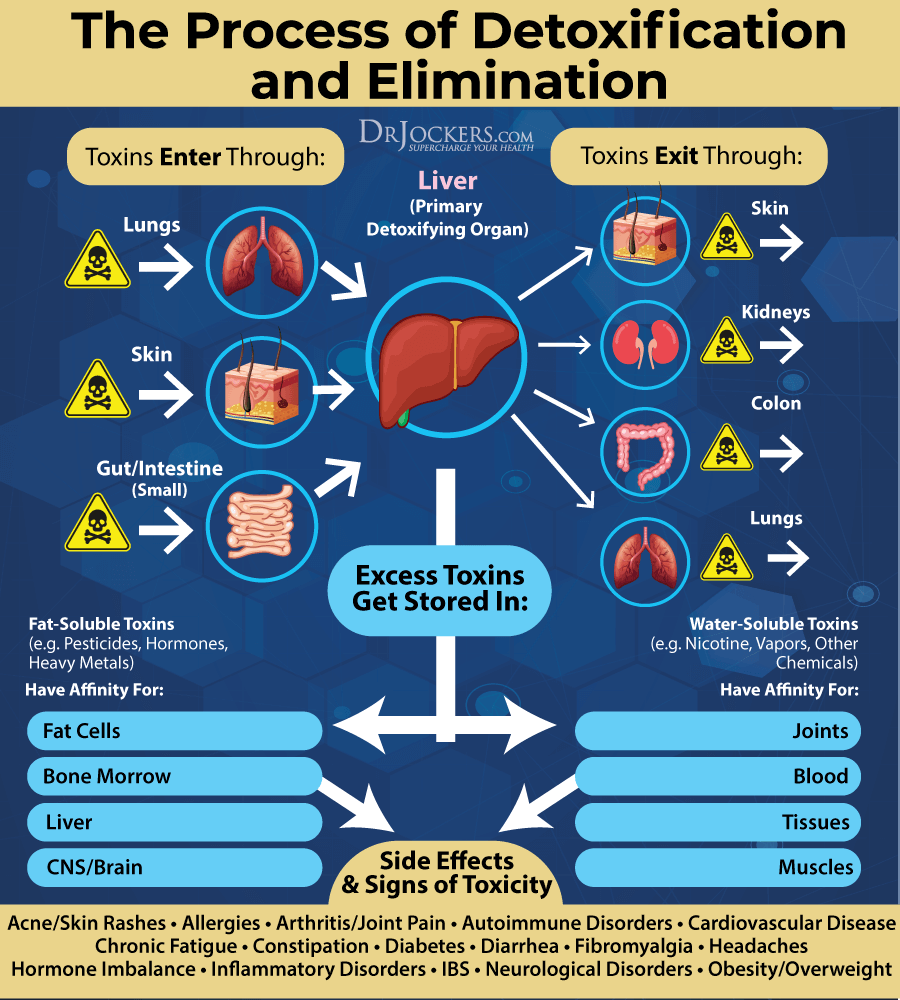
Improve Detoxification Pathways:
Detoxifying your body may help to prevent disease, facilitate your recovery from cancer, prevent recurrences of disease, and lead to a long and healthy life. There are many organs of detoxification, including the liver and gallbladder, skin, lymphatic system, lungs, and kidneys. It is important to support all of these detoxification organs to eliminate toxins and improve your health.
Juicing, coffee enemas, sauna, lymphatic cleansing, physical exercise, breathing exercises, heavy metal detoxification, and regular bowel movements are all pathways to eliminate toxins. It is also important to improve your dental health by removing amalgams and infected root canals and treating cavitations and periodontal disease. Bacteria in root canals and cavities produce toxins that put stress on the immune system.
Drink antioxidant-rich teas such as passionflower, chamomile, and decaf green tea for an extra dose of antioxidants and phytochemicals to assist the body in the detoxification cycles necessary for healthy estrogen levels.
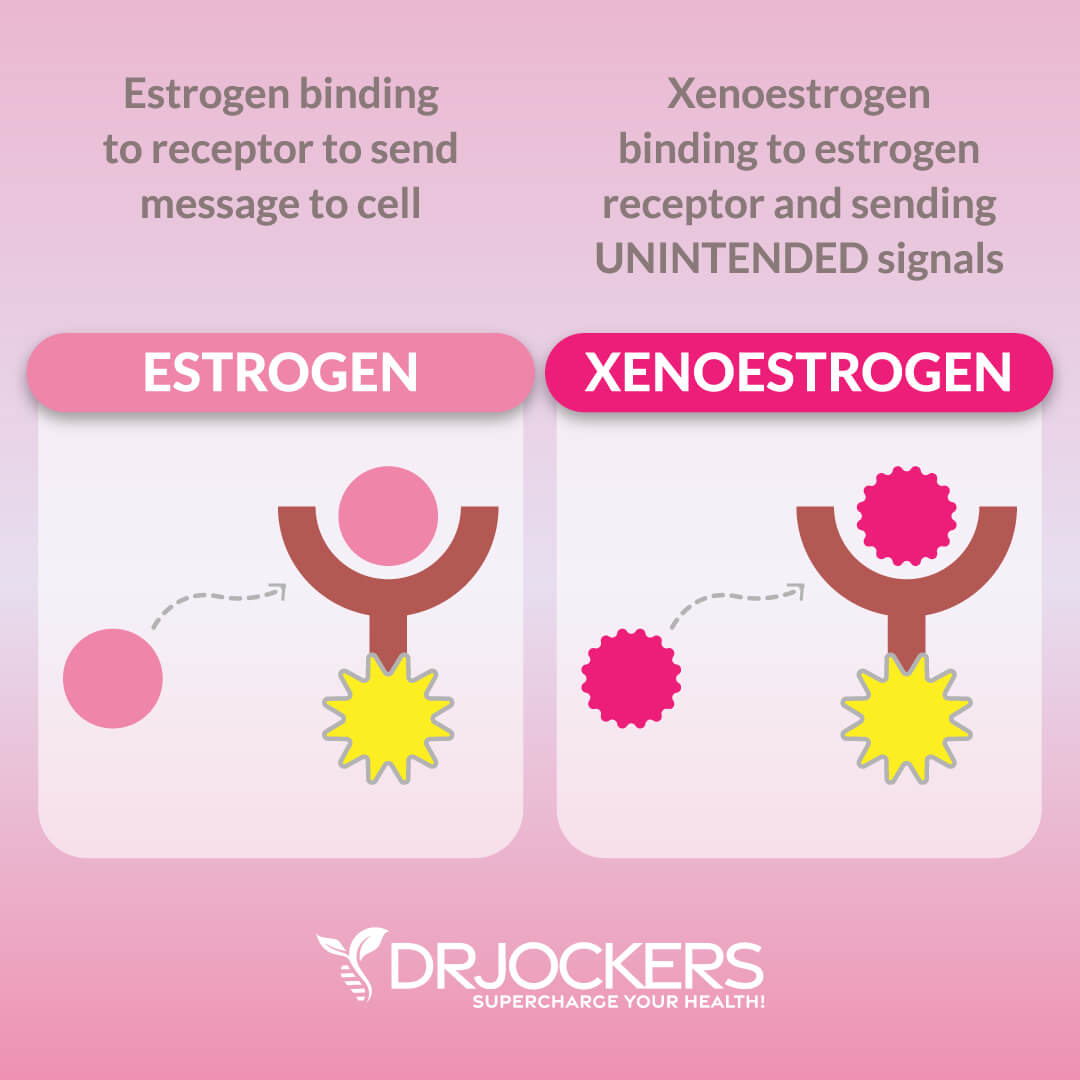
Avoid Xenoestrogens:
Be sure to avoid all plastics, deodorants, shampoos, household cleaning agents, and anything else with xenoestrogen substances. Endocrine disruptors are synthetic compounds that can interfere with the body’s endocrine system (31).
These hormonally active compounds mimic naturally occurring hormones in the body. Xenoestrogen exposure can lead to estrogen dominance and many serious health conditions, including cancer.
Unfortunately, xenoestrogens are found in many everyday products. Examples are plastic bottles, food cans, detergents, flame retardants, cosmetics, and pesticides may contain these endocrine-disrupting substances. Our exposure to xenoestrogens is mostly related to food ingestion.
You can look for natural products that do not contain phthalates, BPA, pesticides, and other xenoestrogenic molecules. There are more and more companies in various markets that are creating more natural and safer products.

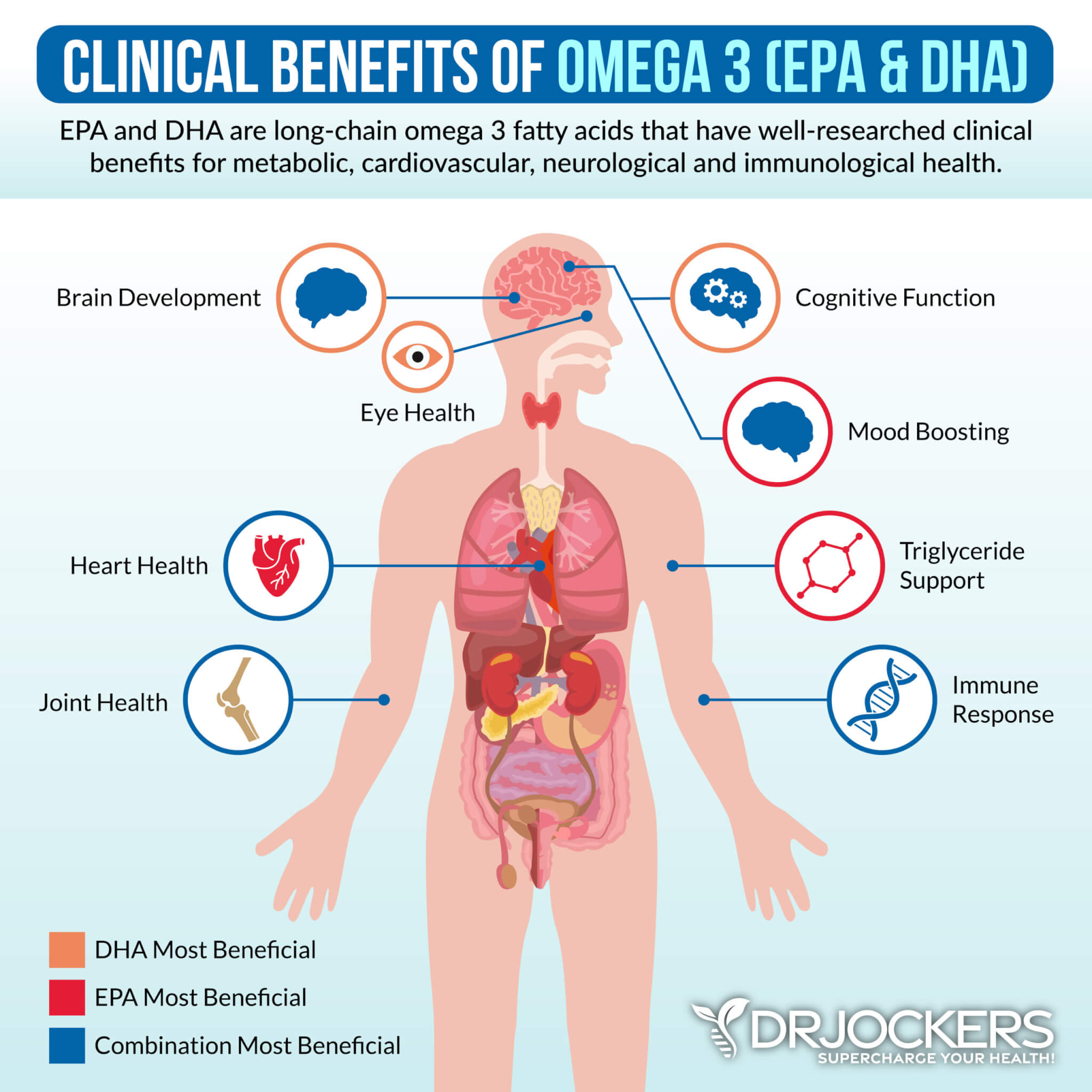
Use a High Quality Omega-3 Supplement:
I have all of my breast cancer clients using 2-5 grams of omega-3 fatty acids. This helps to reduce inflammation in the breast and estrogen dominance. Research has revealed that high-dose omega-3 fatty acids are very effective at balancing estrogen levels.
Omega-3 fatty acids are essential fats that are found in fatty fish such as wild-caught salmon and sardines, grass-fed meats, pasture-raised eggs, nuts (especially walnuts), and seeds (flax, hemp, and chia seeds). Flax, hemp, and chia seeds have the added benefit of improving estrogen levels in the body..
However, if your health is compromised, meeting your omega-3 needs may be difficult via diet alone, and you may benefit from supplementation.
Plant-based omega-3s such as flax oil only contain the small-chain omega-3 called ALA and do not have any DHA. It is very hard for our body to convert ALA into DHA, so it is best to get a high-quality fish or krill oil that is rich in EPA and DHA. You want to find a brand that is molecularly distilled to take out any heavy metals and other unwanted contaminants.
Zinc and Magnesium:
Lower zinc concentrations have been associated with a significant risk of breast cancer and recurrences in women (32). Deficiencies of zinc are also related to inflammation and lowered immunity. Zinc has antioxidant properties and protects our bodies against damaging free radicals.
Magnesium is involved in the production of estrogen, progesterone, and testosterone in the body. It is also critical to phase II liver detoxification and is a cofactor for the enzyme that removes toxic forms of estrogen from the body. Estrogen alters magnesium levels by enhancing magnesium utilization and uptake by soft tissues and bones.
Pumpkin seeds are one of the richest sources of both zinc and magnesium. Additionally, make green drinks or use super green powders, and consume healthy organic meat products.

Practice Deep Breathing:
Short shallow breathing tells the body we are in a state of “survival,” and we kick out a lot of stress hormones that help us to run, fight, or hide. Unfortunately, this fight-or-flight, sympathetic activation doesn’t allow for proper healing and detoxification.
Deep breathing can help calm an overactive sympathetic (fight-or-flight) nervous system and relax the body. This lowers stress hormones and reduces inflammation and abnormal growth in the body.
The body must be in a state of relaxation in order to heal and repair. Deep breathing is a signal to the nervous system that we are in a “safe place,” and we can focus our energy on healing and repairing the body. Check this article out for more info on deep breathing.

Low Intensity Movement:
A sedentary lifestyle is detrimental to estrogen balance and promotes overall estrogen dominance. Throughout the day, get a lot of low-intensity movement such as walking, light cycling, playing, etc.
Regular movement will help reduce inflammation in the body, support healthy circulation, and improve estrogen balance and breast health. Look for opportunities to keep your body moving throughout the day.

Intermittent Fasting:
Intermittent fasting is a form of fasting that cycles between not eating (fasting) and eating (feasting) over a period of time. The benefits of intermittent fasting include cellular repair, autophagy, immune regulation, inflammation levels, and insulin sensitivity.
Going 16 hours between dinner and breakfast is one of the best ways to cleanse the body and reduce whole-body inflammation and cancer growth. Consume your meals in an 8-hour window, such as 11 AM – 7 PM. Read this article for more info on fasting.

Use Cancer Stem Cell Killing Agents:
There are many natural agents that prevent the growth of cancer stem cells. Using things like green tea extract, curcumin, glycosinolates, DIM, lycopene, resveratrol, quercetin, and many others will help to induce cancer stem cell apoptosis and help to improve the body’s natural immune response.
You can find these compounds in natural foods like turmeric, onions, green tea, broccoli sprouts, ginger, etc. It is even more effective to take high-quality supplements with clinical dosages of these compounds.

Improve Your Lymphatic System:
The lymphatic system is like the drains in your home. When your toilet doesn’t flush, particles become stagnant in the drain, and the substances in the toilet begin to rot and decay.
Just like your pipes, the lymphatic system can become congested and lead to adverse health reactions, including soreness of the breast, fatigue, eczema, and chronic skin problems, cold limbs, bloating, headaches, body rigidity, and weakened immunity.

If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Through DrJockers.com, we offer long-distance functional health coaching programs. For further support with your health goals, just reach out and our fantastic coaches are here to support your journey.

Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!






Eek! I think there is an error on your detecting breast cancer picture. At 7 years.., a mammogram could possibly detect cancer. It states “thermogram” at the 7 year mark.
Thank you for an extremely informative article that could save many lives! ‘Wish everyone would read this! My younger sister died of triple negative breast cancer 5 years ago, and I wish she had known this invaluable information long before her cancer diagnosis.
So sorry to hear about that Dianne, that is why I do what I do! Thank you for reading and sharing!
Mammograms/gluten/GMO/sugar/soy/The Pill etc. may cause cancer. The pill may make a person estrogen dominant since progestin is not the same as progesterone which helps the immune system. At premenopause when progesterone goes down, then the immune system goes down and cancer may start. No gluten/dairy/soy/sugar/GMO/food with a label..taking vitamins/good oils/minerals…probiotic…LDN..detoxing may help. Zn/Mg/fish oil/Vit C/Vit E/Vit A/garlic/oil of oregano/Vit D3/sunlight may help the immune system. Essiac/mushrooms/juicing/ozone/grounding/exercise etc may help.
Thank you, Dr. Jockers, for this extremely comprehensive article. I have learned more from this one article than I have learned from searching many sites for similar info. There are several women in my life that I will be passing this article on to. Some who need it now, and some who will use it to help many other women. One more time, “Thank you so very much for your caring and hard work.”
Thank you for your support Barbara! Blessings to you!
I think it’s important to point out that things like curcumin can interfere with uptake of Tamoxofen and other AIs.
Thank you sssoooo much for such valuable information – I have received a diagnosis of the inflammatory kind – I don’t want to go the conventional route however it’s a minefield out there. Thank you for giving me hope as well as explaining clearly what to do, Thank you!
So glad this has been helpful for you! We are always here to help!!