The Dangers of Root Canals
Root canal treatment of infected teeth has been around for hundreds of years. Dentists removed only the obvious decayed matter while sometimes leaving the canal completely exposed (14).
As soon as the early 1900’s doctors believed that root canal treatment was a flawed procedure and increased the risk of future health complications. The theory that root canals could trigger chronic diseases and sepsis caused most dentists to perform tooth extraction for almost 40 years. Following advancements in medicine including the use of X-rays as a tool for better diagnosis, doctors eventually followed the lead of a small group of dentists deeming root canal treatment safe. (13)
Skepticism Today
Despite better diagnostic tools and improved patient experience thanks to anesthesia, there is still much criticism regarding root canal as the safest and most effective option for treating an infected tooth.
Scientific evidence validates old theories that oral health is a foundation for systemic, or whole body, health. A growing body of doctors stand behind Dr. Weston Price and his medical concerns that originally outraged his peers. Dr. Price posed the theory that root canals can endanger the body, both near and far, by promoting disease.
In years following his research the World Health Organization (WHO) would also begin to question the relationship between oral health and whole body function (15).
Understanding Root Canals:
Before you consent to a root canal treatment, understand the risks and benefits to the procedure and then make a decision that works best for you.
The Reason: Dentists recommend root canals to patients who are experiencing pain from a tooth. The procedure is designed to alleviate pain without removing the tooth.
The Cause: The nerve beneath a tooth can become infected or damaged as a result of plaque buildup, tooth erosion, gum disease and other inflammatory consequences of poor oral hygiene.
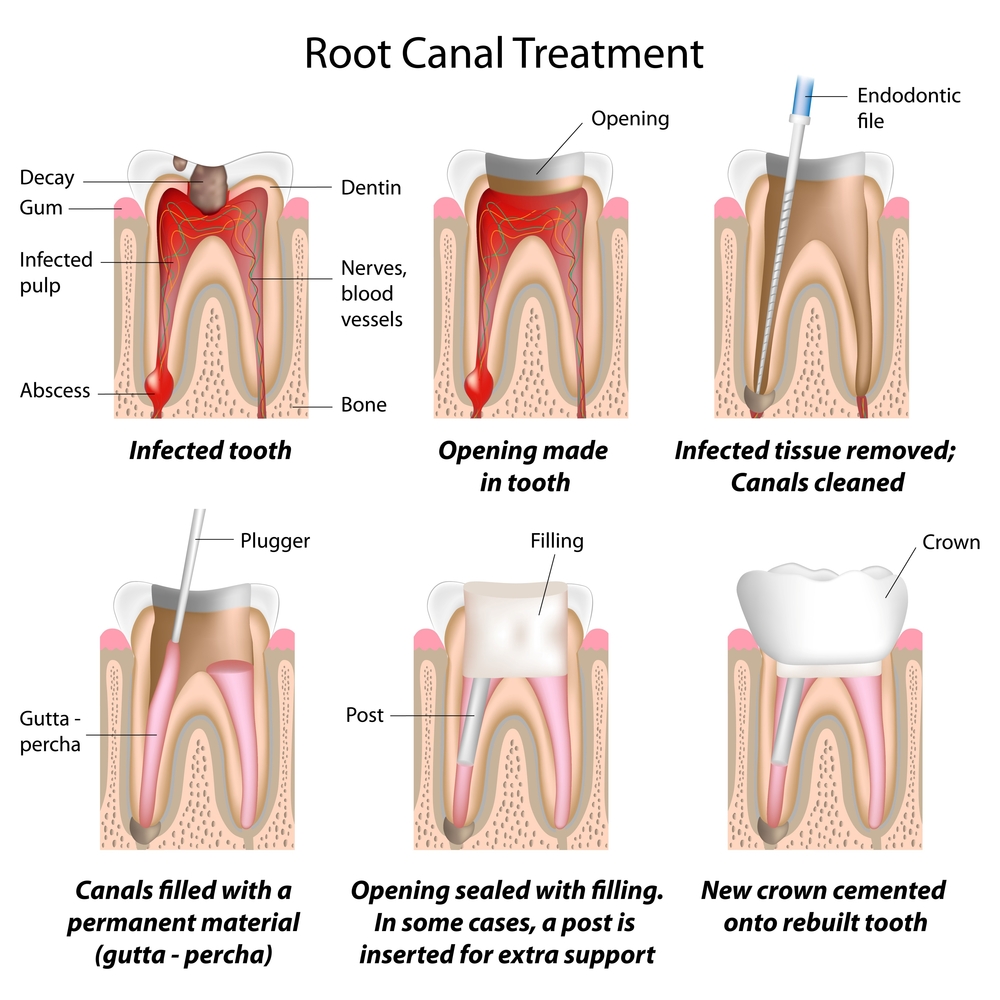
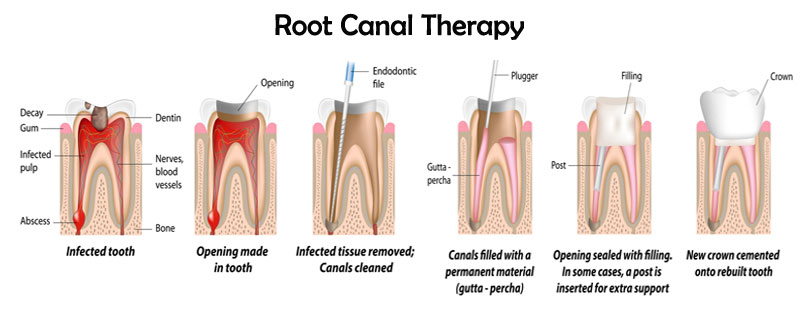
The Procedure: A root canal procedure involves drilling into the tooth so that the nerve and dental decay can be removed.
The blood supply from the body to the tooth is severed, lymph vessels are removed and the inside contents are cleansed with a chemical solution. A filling seals the empty space and the tooth remains intact.
In theory, the sterilization process is designed to completely remove any bacteria causing inflammation and therefore the source of infection. (6)
The Problem: There is a relationship between oral health and the pathology of chronic diseases including diabetes, osteoporosis and kidney disease (16). This information is not new and it is a well-known fact.

Know the Risks:
The American Dental Association (ADA) claims that there is lacking scientific evidence that root canals definitively cause major health complications (6). They are correct that no study can undoubtedly blame root canals for an individual’s health issues.
However, an understanding of oral health, pathology and microbiology provides evidence that the dangers of root canals cannot be unnoticed. For this reason some dentists today will provide a referral to an endodontist (root canal specialist) if a patient requests the procedure.
Human Error
Any medical operation must account for the likelihood of human error to occur. Performing dental procedures is no different. The best dentist or endodontist may perform an “operative error” that results in root canal treatment failure.
Examples of human error may include a missed root canal, negligent planning, injury or abrasion to the gums, over-irrigation, the introduction of secondary infection, incomplete removal of pulp, overfilling, improper diagnosis, and poor quality tooth restoration. (6, 17, 25)
Technological Limitations:
Many factors contribute to the success, or failure, of root canal treatment.
Toxic Fillings: The material used to fill or seal a tooth is often made of a toxic substance including the popular amalgam. Amalgam contains a mixture of metals including mercury. Chronic exposure to this toxic substance can cause severe allergic reactions and contribute to mercury toxicity. (23)
Instrumentation Breakage: Although rare, tools used during the procedure can also fail putting your health in jeopardy. Shaping instruments can break or produce undesired lesions in the gums that can go undetected.
Imperfect Seal: Filling a tooth isn’t an exact science. If a doctor uses more filling than required, there is an increased likelihood for bacteria to penetrate the seal and develop into another tooth infection. Consequently this can result in a second root canal. (25)
Limited Detection: Despite medical advancements, X-ray imaging is also limited in its capabilities to detect infection, tooth damage or disease (7). Typically an X-ray is only useful at identifying obvious infection.
Although CT scans can be better at detecting infection, they are expensive and expose the patient to higher amounts of radiation.
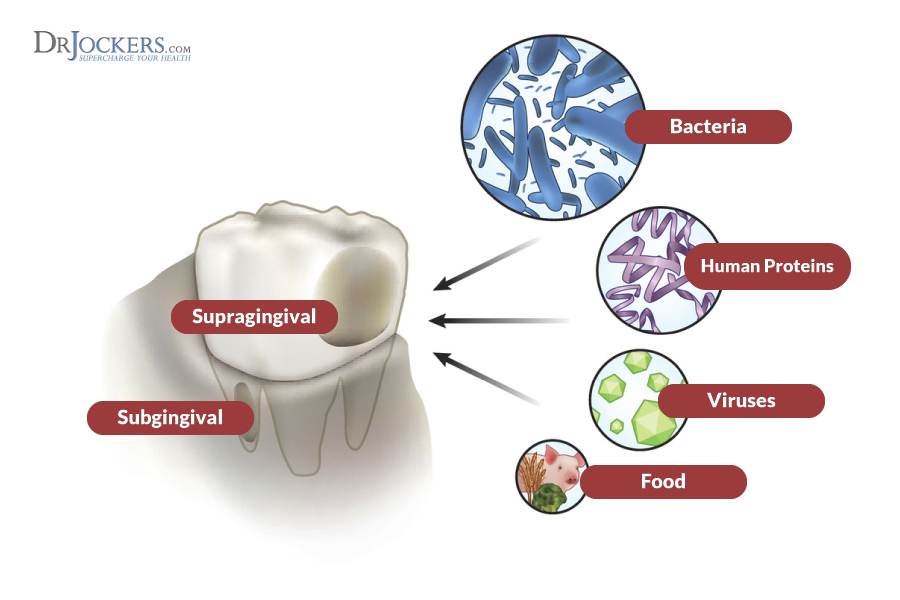
Sanitation is Impossible
There is one major false assumption made regarding root canal treated teeth and that is that sanitation of the oral cavity kills 100% of all infectious agents.
Microbes, fungi and viruses can remain out of reach and unsterilized in the miles of microscopic tubules beneath a tooth much like the root system of a well aged tree (3). Radiographic images of well treated root canals show that bacteria can reside and persists from long periods while the patient remains asymptomatic (23).
A commonly used disinfectant, sodium hypochlorite, was tested to determine how much bacterial residue remained in the treated area. Scientists found that up to 50% of the bacteria population was left behind following the sterilization process.
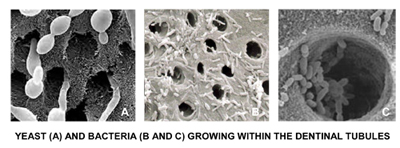
Photographic Evidence
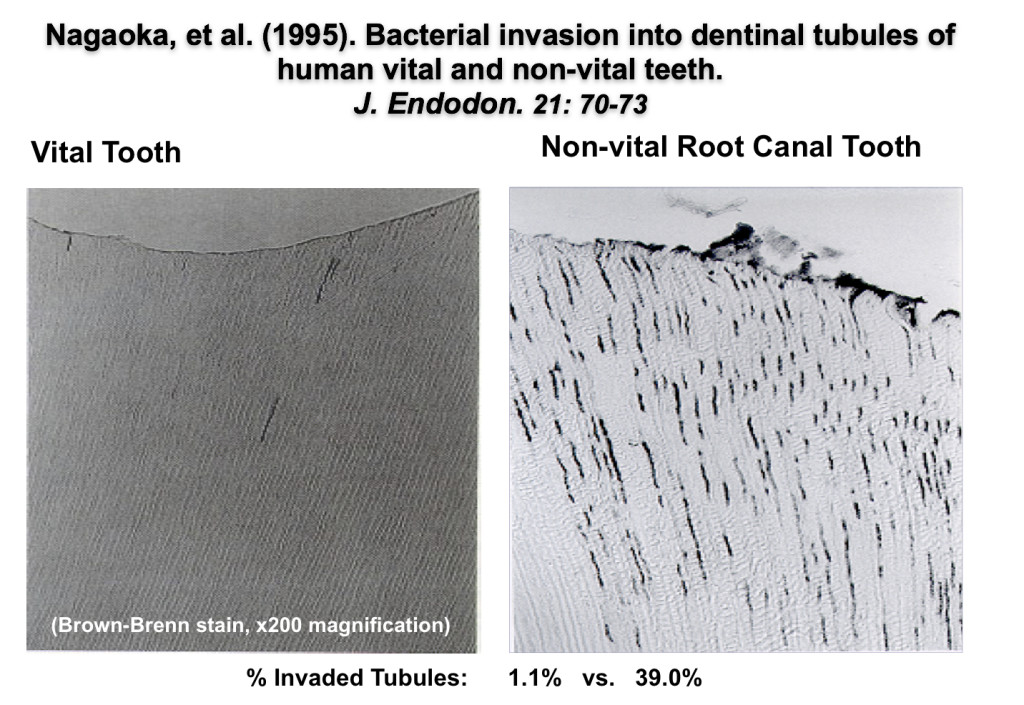
In the image below you will see a study published in the root canal specialists (Endodontists) journal. The authors of the study took individuals who were preparing to have their wisdom teeth extracted.
They did a root canal on one side and then removed both wisdom teeth in three months. The study showed that the tooth without the root canal had only 1% of its tubules infected. However, the tooth that had a root canal three months earlier had 39% of the tubules infected (12).
How Root Canals Promote Secondary Infections:
Denying the association between disease and pathogenic bacteria in the oral cavity is like ignoring a smoking gun for evidence. Root canals are successful at alleviating pain but they create a chronic burden on the immune system.
Harbor Pathogens
The function of the entire body is susceptible to compromise as long as pathogens exist in the oral cavity.
The Perfect Conditions: When a root canal is sealed and the blood supply is removed from the tooth, an oxygen free environment is created. Anaerobic bacteria left behind during the treatment not only survive but may have evolved to thrive!
Toxins Travel: These flourishing bacteria are termed “inflammophilic” because of their liking to inflammation. Endotoxins leach into surrounding tissue and migrate into any areas of the body. Coupled with havoc wreaking bacteria found in root canals that secrete macrophages, endotoxins degrade collagen and increase vascular permeability that leads to disease. (20, 24, 26)
Evidence: The presence of anaerobic microbes was discovered in the blood and root canals analyzed from 26 patients with no pain symptoms. The anaerobic bacteria found cause pneumonia, acne, and necrotic tissue infections among other ailments. These pathogens also serve as major inflammatory mediators inducing disease in the body. (18, 19)
A 3 year post root canal follow up study found that the health of 87 patients significantly declined. Health authorities will say correlation does not equal causation. The true misunderstanding and illogic here is that this statement is always true. (3, 7)
Sometimes correlations do show us cause and effect relationships. I believe it is up to every individual to learn the risks of root canal therapies and decide on a treatment that is best for himself.
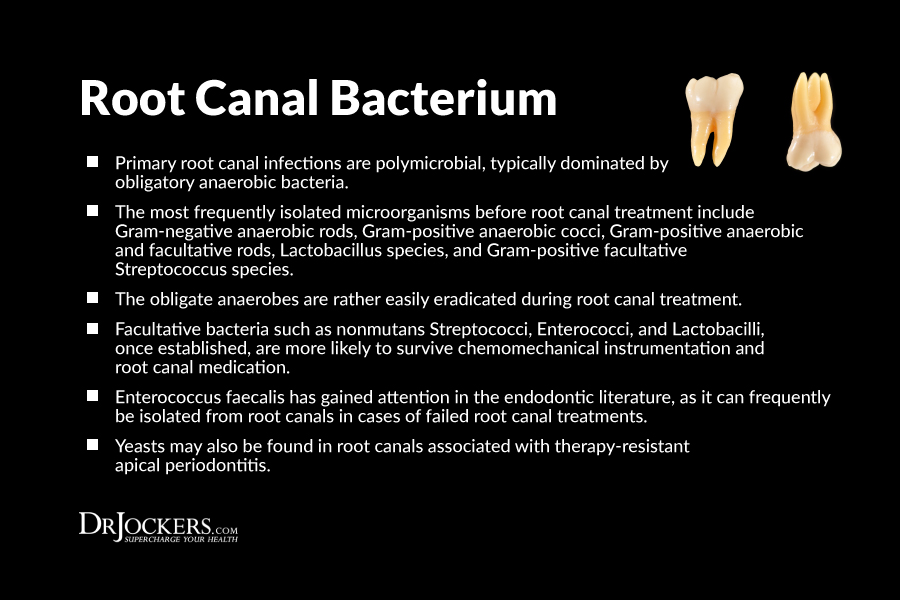
Antibiotics Promote Drug Resistance:
Antibiotics are no different from the disinfectants that cannot reach bacteria or the oxygen that is depriving the root canal environment. Without circulation and blood flow, antibiotics intended to kill the pathogens in your mouth are instead depleting the healthy bacteria in your body designed to protect the immune system. (3, 7)
Another unnecessary prescription and the overuse of antibiotics is a growing alarm for the prevalence of antibiotic resistant pathogens. Some of the most common types of antibiotic resistant bacteria associated with infections from root canals are: (6, 19, 31)
Enterococcus feacalis: Presence of these bacteria are often the cause of urinary tract infections, meningitis and is also one of the most antibiotic resistant bacteria known. These bacteria are thought to stimulate the production of toxins and further infections in the entire body.
Enterococcus faecalis are one of the most prevalent and virulent bacteria strains present in an infected root canal. They are also most commonly discovered post endodontic treatment. (28)
Pseudomonas: Some strains of these bacteria are antibiotic resistant and can ultimately cause death. Symptoms associated are a weakened immune system, pneumonia and blood infections.
Staphylococci: Commonly referred to as staph, these bacteria cause skin infections, pneumonia, blood poisoning and toxic shock syndrome.
Streptococci: Some strains of these bacteria can be referred to as flesh eating bacteria. This bacterium is linked to symptoms related to strep throat and serious health complications involving pain, fever, swelling, dizziness, rash, confusion, abnormal blood pressure and toxic shock syndrome.
Pro-Root Canal Specialist Recognizes Health Threat
One of the original founding members of the Root Canal Association, Dr. Meinig, commented on a study performed by Dr. Weston Price in the early 1900s. Dr. Meinig notes that the cause of secondary infections is not solely dependent on the presence of pathogenic bacteria but also the production of toxins produced from these bacteria. (7, 11)
Dr. Price’s research team found that implanting an infected tooth from a human to another animal would cause the same systemic complications to the animal in which the human was suffering (7). In fact, Dr. Price ran well controlled experiments contrary to popular medical rumors and discovered that animals infected with the toxins alone had a significantly higher rate of becoming sick and dying.
If one of the major proponents for root canal treatment can re-assess his understanding of oral health and its relationship with chronic disease, it is logical that more dentists should understand the health risks and focus on educating and providing informed consent to their patients.
Weakened Immunity
One of the easiest assumptions for an individual to make is that if there are no symptoms of infection post root canal treatment, the root canal is not contributing to deteriorating health. Unfortunately, this assumption has one limiting factor: time.
Dr. Meinig comments in an interview that some individual’s immune systems may be better equipped to manage the bacteria and the released toxins (7). Over time, the body’s natural defense systems weaken and eventually become destroyed.
It is inevitable that infectious agents will maneuver their way to other organs in the body. Symptoms can manifest as chronic diseases which can be fatal if left untreated.
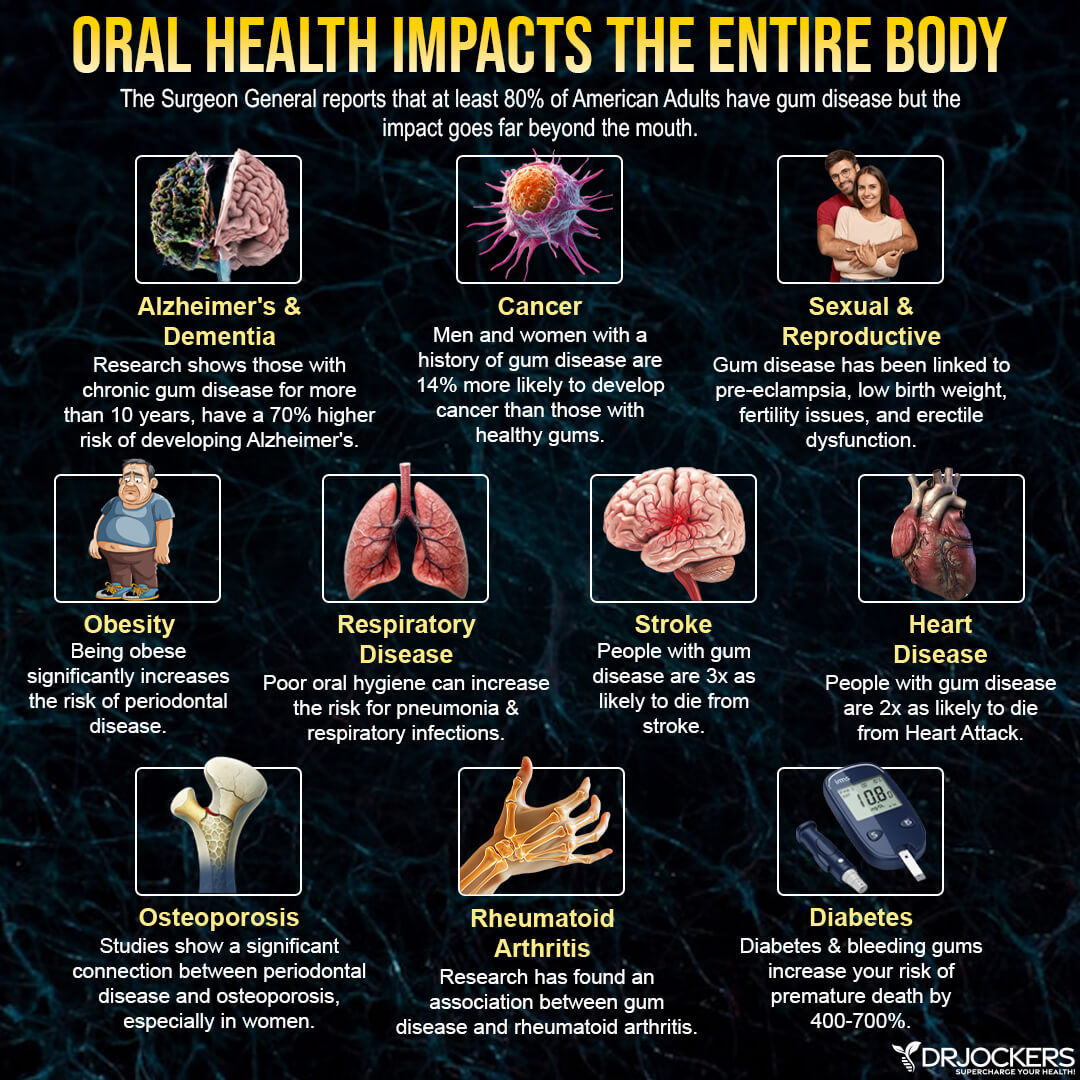
A Pathway to Degenerative Disease:
According to the work performed by Dr. Price and his team, there are specific chronic and degenerative diseases that stood out in greater prevalence than others. In order of the highest risks found associated with root canals are: (7)
- Heart and circulatory disease
- Inflammation in the body found in arthritis and rheumatoid arthritis
- Brain and nervous system diseases
Cardiovascular Disease
Virulent bacteria harbored in a root canal emit toxins that cross into the circulatory system and congregate to induce cardiovascular dysfunction. The accumulation of bacteria appears as lesions in or surrounding an infected tooth. Including people with that have received endodontic treatment, the presence of these lesions is shown to increase the risk for coronary artery disease (30).
Individuals with missing teeth were up to 76% more likely of developing a heart attack compared to those with most or all of their teeth (10).
Cancer
In fact, periodontal infections induces chronic inflammation that is linked to autoimmune diseases including cancer metastasis. One 24 year study of more than 1,000 individuals found a high rate of cancer growth and diagnosis in the people whom had developed dental infection. (22, 26)
Diabetes
Mounting evidence supports the likelihood that a root canal procedure can increase an individual’s risk of developing type-2 diabetes.
Metabolic complications associated with type-2 diabetes is intimately linked to the body’s immune system. Periodontal disease and tooth loss induces inflammation that can trigger physiological factors evident in type-2 diabetics. (11)
Periarticular lesions, similar to those linked to heart disease, are commonly present in people with diabetes. These lesions were produced in rats by exposing the inside of a tooth to the oral cavity or by introducing bacteria pathogens. (27)
Only 3-5% of all teeth examined in dental patients had periarticular lesions. In patients with previously treated root canals, these same lesions comprised up to 61% of individuals.

Care Tips for Oral Health:
Don’t be alarmed that you are destined for total health failure if you have already had a root canal treatment. Preventing dental decay is of primary importance but there are strategies you can take to better your teeth and gums while also reducing your risks of chronic diseases.
Consider the following care tips to improve oral health: (9, 11, 21)
- Brush your teeth a minimum of twice a day and flossing daily
- Visit the dentist as recommended by your doctor
- Replace your toothbrush once the bristles become frayed or at least every 3 or 4 months
- Use a tongue scraper to remove dead cells and bacteria which cause bad breath
- Brush using a nontoxic toothpaste free of fluoride and chemical additives
- Limit acidic foods and beverages in your diet by removing soda altogether and replacing it with purified water
- Consume a healthy diet rich in whole food sources and nutrients. Fat soluble vitamins A, D, E and K and essential minerals like calcium and magnesium are an integral part of maintaining oral health.
Ayurveda Heals
Some preventative methods at maintaining the health of your teeth and gums may be new to you but stem from a traditional style of medicine that dates back to over 3,000 years ago in India (8).
Ayurveda medicine is a holistic health system suggested to prevent and heal an estimated 30 systemic diseases that result from deteriorating dental hygiene (8).
Some members of the medical community compare its benefits similar to that of reflexology in which the tongue has a specific location that can stimulate either harm or healing abilities to a distant organ in the body.

Oil Pulling
The practice of oil pulling may sound unappealing but is a very simple practice that is claimed to cure headache, asthma and is a remedy for bleeding gums, dull senses including taste and vision, sore throat, and tooth decay. Although sesame oil is known as the Queen of Seed Cropsfor its health benefits, sunflower oil has also been traditionally as well as coconut oil. (8, 9)
Compared to standard mouthwash, oil pulling practices using sesame oil actually was found to significantly prevent against plaque-induced gingivitis by decreasing plaque and bacteria. Two methods are referred to often in oil pulling practices and can be used on a daily basis: (8).
Graha Gandusha: In this style of oil pulling, the mouth is completely filled with oil and held for up to 5 minutes without gargling.
Kavala Graha: If expanding your cheeks for up to 5 minutes while holding liquid is uncomfortable or cannot be done, Kavala Graha involves filling the mouth with only enough oil to be swished throughout your teeth and gums for 3 minutes.

Essential Oils
Have you ever thought to dip your floss in essential oils for added antibacterial and antifungal properties? Using a 100% pure and therapeutic grade of essential oil from a trusted supplier, rub a drop of tea tree oil or peppermint oil along a strand of floss to receive its many health benefits.
Experiencing pain and swelling in teeth or gums? Clove oil acts as a topical anesthetic. Ditch the chemically derived products containing benzocaine and switch to a natural pain remedy proven to be just as effective as its conventional and toxic alternative. (2, 4)
The natural oils found in herbs are another great source at preventing microbial diseases in the oral cavity. Herbal tooth gels have been shown to provide the same effectiveness as fluoride in eliminating carcinogenic bacteria and contain no adverse health consequences following use.
Aside from clove, peppermint and tea tree oil, other herbs such as neem, licorice root, cinnamon, turmeric root and parsley have antiseptic, antifungal and antiviral properties. (5, 8)
Herbs and Spices
Do you have a favorite toothpaste flavor? Varieties may include peppermint, fennel, cinnamon or clove.
These spices are not only trendy flavors but their presence in toothpaste acts as anti-inflammatory agents killing bacteria and oral pathogens. Add these spices and other herbs like pepper, ginger, turmeric, garlic, oregano and basil to your go-to culinary staples for their protective benefits.
Probiotics
Do your eating habits resemble this scenario? You start the day with a cup of coffee. Maybe later you snack on an orange or get the fresh squeezed lemonade for a beverage at lunch. Dinner consist of a plate of pasta and meatballs drenched in red sauce only to be followed up with a taste of sugar laden sweet treat for dessert or a glass of red wine.
Since you last brushed your teeth after waking up your mouth has been saturated in acidic foods and beverages. This acidic environment encourages the growth of bad bacteria, plaque buildup and dental decay.
Supplementing your diet with probiotic rich foods and beverages such as sauerkraut and kombucha can help inhibit the growth of bad bacteria (5, 9). Healthy bacteria support dental hygiene by improving the pH balance and providing your mouth with the weaponry it needs to prevent decay.

Green Tea
Unlike any other herbal tea, green tea has a natural compound known as catechins. Catechins are a type of polyphenol which is not only a micronutrient found in our diet but a powerful antioxidant. Green tea has anti-inflammatory properties that are far reaching in both oral and overall health.
Tobacco users who either smoke or used smokeless products and drank green tea regularly had a lower risk of developing cancer than the tobacco users who did not consume the tea. (9)
It is speculated that the anti-inflammatory components of green tea disrupts inflammatory agents and its triggers that breakdown collagen in tissue (29). Daily consumption can inhibit bacteria in the oral cavity and support healthy teeth and gums.
People who consume 2 cups of green tea per day have been shown to have lower levels of the bad LDL (low-density lipoprotein) and total cholesterol. Green tea may reduce one’s risk of cardiovascular disease by up to 33% as well as prevent obesity and slow the progression of Alzheimer’s disease (9).

Find A Holistic Dentist Near You
If you are not already seeing a holistic dentist, find one near you trusted to ensure your optimal health. Already have a root canal? A holistic dentist can provide recommendations to protect you from the dangers associated with root canal treatment.
Visit the IAOMT page to search for accredited members of the IAOMT whom are trained in holistic dentistry (1).
You can also visit the Holistic Dental Association to view the dentists’ profiles and learn about the services they provide (2). These dentists are trained in natural strategies to help you remove root canals and improve your oral health.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and thrive in life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!








What if you already have a root canal, what now?
It’s causing problems so is it better to remove the tooth completely? What does one do if you already have one in place and are struggling with health issues that are most likely connected to having that infection in your mouth all the time?
Hey Elaine,
I would advise you to look for a holistic dentist in your area to help you with your oral health. I am not a dentist, so they would know the best route for you much better than I. However, I would also recommend following much of the health advise you can find on our site.
Yes, I agree with Elaine. I have to do something about getting rid of two root canals in my upper mouth, however I don’t know what to do. I’m not sure if I can stand dentures although I already have a partial which goes across the roof of my mouth and is VERY annoying. I was considering implants but would imagine you’d be facing the same problems with them. What is your take on implants vs. dentures, Dr. Jocker? I know you are not a dentist but your article shows you know a lot about oral health and it’s effects on overall health. BTW, holistic dentists are nowhere to be found where I live. Thanks. Andrea K
I was wondering if you have a list of biological dentists in the southeastern US. I live in southeast Alabama and would like to find one within driving distance. Thanks
Hey John,
Here are a list of biological dentists https://iaomt.org/
I went to the dentist for a routine teeth cleaning and check. About 4 days later started with many odd symptoms that escalated into a few weeks later with several trips to the ER. There I was diagnosed with Guillian Barre Syndrom. I feel in my gut it was caused by the teeth cleaning. I feel I’m not being taken seariously and now i’m fighting to get my life back.
This is very serious Linda! Have you worked with a functional medicine doctor? I do work with people long-distance if you are pursuing a plan to detox and get well.
I’m not Linda but would like to know where your practice? I have multiple issues including malabsorption ru a DC, ND, DC, md?
Dr Jockers,
I have had MANY root canals over the years, and I have several crowns and a bridge. I can’t afford to have any major dental work done, or see a functional doctor, as I have NO health insurance.
I eat and supplement very similar to your lifestyle plans on this site, but is it enough? I’ve been eating well and supplementing wisely for years now, but I still can’t lose that last 30 pounds, and I still don’t feel 100% well yet. Thank you.
So sorry to hear this Susan! These root canals are most likely one of the reasons for your health struggles. I would continue to do everything in your own power to improve your health and do oil pulling multiple times daily. https://drjockers.com/health-benefits-oil-pulling/
Thanks, I love oil pulling.
Hello, I have one root with four canals. Need to have drilling thru four tooth pulps.
had a root canal and they struggled with the infection, I’ve since been diagnosed with Parkinson’s Disease. I’m sure they’re linked, has this happened to anyone else?
My uncle was diagnosed with Parkinson’s disease several years ago. Anytime I talk to my grandmother (his mom) about it she always says, “You know, Uncle had that really bad tooth infection right before all this happened. I think that had something to do with it.”
I’m sorry for your troubles but it’s interesting to read that someone else has a similar experience.
I think that if you are going to put out an alarming article like this you should have some solutions or reccomendations for those millions of people that don’t have the finanacil means to see a holistic dentist. In addition for those that already have a root canal you are instilling fear that can be just as detrimental to their well being as a root canal. I am a health coach but I think you have to be careful about scaring people.
I agree here Lisa. I’ve been an ND in clinical practice and know many people who HAVE had successful root canal therapy performed by very skilled clinicians. There are many people with root canals in great health, I’ve personally seen this in clinical practice. But, there are probably more people out there who have had bad dental work performed on them resulting in very poor root canal work, and then you could expect issues down the road ranging from mild to the very extreme. Same goes for any medical procedure or treatment. Fear mongering is rife online with many websites now unfortunately. I’d rather see a patient get a root canal done expertly and keep the tooth rather than have it pulled. Eating/chewing properly is critical for great GI and overall health. I’ve also seen very poor advice given to people by chiropractors and naturopaths, resulting in very poor clinical outcomes regardless of their dental status. We need to be careful not to fear monger people.
Dr. Jockers,
I had 1 root canal some 20 years ago. Never seemingly had a problem. About 12 years ago , I was experiencing pain and burning in my feet. My doctor said I had Neuropathy. Could that root canal 20 yrs ago have anything to do with my problem. I have since had another root canal, 3 yrs. ago and it has remained tender even after several x-rays, a new crown and routine cleaning. I am very concerned after reading your comments and would be most interested in knowing what you think. What should I have done to this tooth in your opinion?
Thanks so much for your advice,
Mary Brewton
Hi Mary,
You need to get a second opinion and a good set of X-rays on this suspect tooth, it sounds like a residual infection at the tip of the root. The root canal needs to be re-done, and properly this time! Either that or a dental implant depending on your finances. Tenderness means infection, and infection is not good long-term. It is highly unlikely the 20 year old root canal had much to do with your neuropathy, especially if the neuropathy came eight years after that root canal.
Ms. Bakker,
I was wondering if you watched “The Root Cause” documentary, and if so, do you really still remain non-convinced that there simply isn’t such thing in this universe as a “successfully done root canal”? It is merely irresponsible on your end to advise someone to “re-do” their old root canal. If we, General Public, can’t count on NDs to help spearhead the stoppage of the root-canal epidemics while all of the clear clinical data out there shows undeniable linkage of root canals (“successful” or not) to cancers, heart disease, neuro and autoimmune conditions, then we are really in trouble.
With the estimated 25000000 new root canals every year in the USA no wonder we are falling further and further down among developing countries in terms of our general health and life expectancy.
Hello.
I was told I needed a root canal on my wisdom tooth. Now, I have lost most of my molars so it’s hard to eat and that is why the dentist is trying to safe it. I already have health issues,: scoliosis, bulging and degenerate on L4,5,6, and other problems not solved yet. Is it wise to go ahead and do a root canal?
Hey Liz, I would recommend using this link to find a holistic oral health specialist that you can reach out to: https://iaomt.org/
Do these risks apply to all root canal procedures or only those done improperly? I have a tooth that requires a root canal and I am so conflicted- should I just have it extracted or can a root canal be performed by an IAOMT dentist without adverse effects? Will extraction prevent future issues or are there risks associated with that also? Thanks!
The risk is always there as the microtubules in the tooth bed are extremely hard to reach and sanitize. An IAOMT may have a better approach for this but oil pulling, colloidal silver, and proper oral hygeine can all be great!
Interesting article, There isn’t a mention on removing the root canal tooth and if this will solve the problem though. Are there any studies or information on people having root canal teeth removed and seemingly unrelated health problems disappearing? Or is it too late once the bacteria are in there?
Hey Stephen, there are many dentists who can safely remove and clean the tooth. Keeping up with good oral hygiene as discussed above (especially oil pulling) will help keep bacteria controlled!
Hi, I am a 21 year old girl and had a root canal done when I was about 15. I have had endless problems with energy, digestion, skin and general immune system problems for the past 4 years. I do not have any pain or anything around the root canal tooth but am considering getting it extracted in 3 weeks time and getting a small partial denture. I am very very nervous to be making a mistake. Do you think the root canal be the cause of my health problems even though I have no pain or swelling? I follow a nutrient dense healthy diet and have tried everything I could try and haven’t got better. Pretty desperate but don’t want to make a mistake and have a denture for the rest of my life.
By the way, thank you for the article!
Also if anyone has successful testimonies of healing after removing a root canal please post, it will be so much appreciated!
It could potentially be causing you issues Lucy. You may also consider something like this:
https://drjockers.com/bio-health-gi-pathogen/
https://drjockers.com/complete-thyroid-report/%20
So would you recommmend I look into these areas before removing the tooth?
Potentially all of them Lucy, it depends on what is contributing to the majority of your symptoms.
what i can do to replace my teeth .. what’s the most safe option?
Not sure, but reach out to a great holistic dentist and they can consult with you on that. http://www.iaomt.org
I have left jaw pain a dear pain had a root canal in upper left side could that mean I have an infection in my root canal?
Yes it absolutely can be. I would be sure to get that looked at by a holistic dentist as quickly as you can!
Thank you for your article to raise awareness about root canals. I have now had 2 infected root canals. And, many many health issues that I believe can be traced back to the chronic infections from infected root canals. I left 1 of infections go on for years, not realizing what it was. The pain would come only when I was stressed and/or tired. I used to joke that when my jaw started to hurt, I had to quit doing so much, working late, etc.
Well, in
2012 I had a health crash. I paid to see a functional medicine physician, he did a scan of my mouth and told me to have my 5 root canal teeth extracted and replaced with implants. I was quoted $25,000 from the holistic dentist he referred me to. He also told me I had an infected root canal that should be extracted. He had done an (ultrasound?) scan of my jaw.
He sent a letter to my regular dentist, and my dentist said he was a quack and ignored the recommendation.
At around the same time my physician found my CRP (the lab test for inflammation) was elevated. He couldn’t understand why.
Then in 2013, I had a minor heart attack. The cardiologist couldn’t understand why as I had no usual markers of heart health risk, except for the inflammation marker.
Well, later that year, I went in for dental surgery because I had a necrotized jaw from the infected root canal. The dental surgeon was shocked I had let the tooth go so long. Well, I made the mistake of trusting my dentist. When the tooth was extracted, I started to feel better. My health started to improve.
But, I’ve been developing several auto-immune conditions.
Recently I have been feeling particularly low energy. And I’ve been experiencing an area in my upper jaw that has pain that comes and goes. So, I made a dental appointment. Just today, I saw a root canal specialist and he said I have an infection in the tooth that has a root canal. He is pulling the tooth.
And so, here I am, on the internet trying to find out about failed root canals and overall health. I found your excellent article.
I’ve decided I’m getting all my root canals extracted.
I’ll just have to cash in some retirement savings. My long term health is worth it.
So sorry to hear this Elaine! We are praying for you and believe that good things will come from this!
I just had a root canal yesterday and today I am experiencing chest pains and random pain all over my body… could they be related? I am only 23 and I don’t want to lose a main molar, but I also don’t want to hurt my health (I already have an autoimmune disease).
So sorry to hear that! I would find a holistic dentist to work with!
I had 2 root canals 2 years ago and every since then ive had vertigo. Diagnosed with bppv then needed prism glasses now they think it’s my neck. Could my root canal be causing all of this or is this just a coincidence?
So sorry to hear that! Yes, absolutely a silent infection from a root canal can definitely contribute to this!
If I pull them how long does it typically take before people tend to feel better?
It is really very variable for everyone but the most important thing is to get the process started!
Im an scared to get a root canal, im 24, i have an infected tooth #19, i have an appointment for a root canal in 2 days and i dont know if i should cancel it . I read that a bridge is a better option , please help me! 🙁
I live in california , oxnard area, ventura county, i talked with my dentists assistant and she said that im too young to get the bringe and that my teeth are gonna fall out faster , if i get the infected tooth pulled out
I would get it pulled out. Please see a holistic dentist. http://www.iaomt.org
Yes I would recommend getting a bridge instead!
Excuse me , i saw videos of the bridge getting done and i noticed that it applies some pressure to teeth and then u get gum ressesion, would my teeth start to fall out too? Im more concerned about my future health😭
And with the bridge they have to cut your teeth to make it fir inbetween? Would u recomment a partial or an implant?
Implant is great!
Hi what and how does oil pulling work
Here is a helpful article Melina https://drjockers.com/benefits-oil-pulling/
Excuse me if i get the infected tooth pulled out does that mean they clean my gum too or is my gum prone to infection too? And when they pull out the tooth do they kill the nerve too?
Thank you for this article. It was very informative. I’m facing the possibility of a root canal because of a couple fillings poorly and unnecessarily done (There were no cavities) by a dentist I’ve long since left. He said he wanted to do “preventative work” and I was naive. It’s been a year a half since he drilled into my teeth and the two molars have still been sensitive. My childhood dentist, who I’ve been going back to, has been encouraging me to look into a root canal but I think i might insist on a crown, especially since there seems to be nothing wrong with those molars – no decay or cracks she can tell. It seems like she just wants to end the pain instead of getting to the root problem – but after reading this, I don’t want to kill the tooth for no reason. She just re-did the fillings with IRM, so hopefully that will calm the nerve so I don’t have to think about this. This is so frustrating because I’ve always taken good care of my teeth and just had poor dental work done!
Hi Ritasharma, I am so sorry to hear about this! Praying for your healing and pain relief.
I had some old mercury fillings replaced with white fillings and one tooth is still sensitive like yours were. Did having the filling replaced work at calming the nerve like you were hoping? Because I too don’t want to kill the tooth.
I have space between my teeth, i am looking for a dental visit. Is is possible that unevenly sized teeth could have problems of root canal?
Hey Jai, There are many factors associated with oral health and complications of root canals. I would recommend consulting with a holistic dentist to help you understand your unique risks.
Thanks for the info.
is the gentle wave root canal therapy a safe alternative or is it still dangerous.
your help is greatly appreciated.
Kind regards
I haven’t heard of that Chris but would recommend asking a holistic dentist about it.
Do be I need a crown after root canal, too expensive
Would an extended fast help eradicate any bacteria that may be forming or thriving in a root canal? This was a disturbing yet informative article, thanks Dr Jockers. Off to oil pull now!
It can be helpful, as can oil pulling. However, I would recommend a consult with a holistic dentist!
Thanks much Dr Jockers. I actually got the root canal from a holistic doctor and also received many ozone injections to ‘help the cells rejuvenate’. As soon as she said those words, I thought FASTING AND STEM CELL ACTIVATION! :). It certainly can’t hurt to try it, only help heal me on many levels. Ok, I’m fasting! Thank you for bringing this all full circle in a way for me!