
Measuring Your Risk of Developing Heart Disease:
Heart disease is the leading cause of preventable death in the United States. Scientists are now saying that 95% of these heart disease related deaths are caused by cellular inflammation. Today’s technology allows us to analyze our level of cardiovascular inflammation and our risk of developing heart disease.
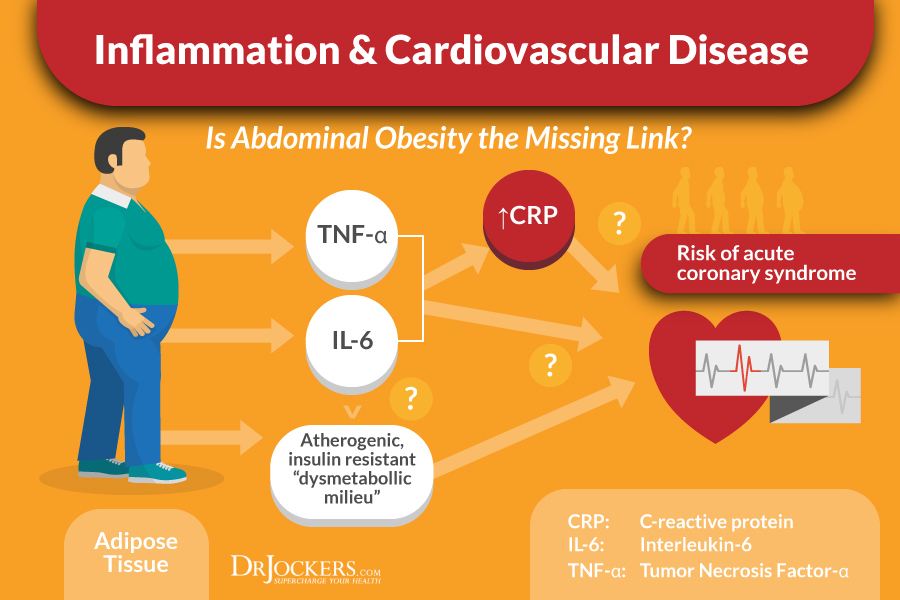
Inflammation is driven by several different routes in our body. Oxidative stress from excessive free radical formation and/or a deficiency in antioxidants is a common mechanism. Increased sympathetic stress response within the body causing catecholamine overload and burnout plays a role in most inflammatory cycles (1, 2, 3).
Finally, improper cell signaling due to excessive pro-inflammatory prostaglandin formation and immunological cytokine reactions is a staple ingredient in the inflammatory soup.
Tests to Analyze Inflammatory Levels:
When it comes to cardiovascular health, lipid panels are archaic and scientists have demonstrated that these tests have many limitations and only identify 40% of those at risk for coronary heart disease. People drop dead everyday with “normal” cholesterol levels, “normal” blood pressure and “normal” EKG findings.
Scientists have found much more advanced blood tests that can far more accurately assess your risk of heart disease. Three great tests that analyze the risk of inflammation in the coronary arteries include C Reactive Protein, Homocysteine, and Lipoprotein (a).
We include all of these key tests and more in our CardioPower Testing here I recommend this test to all my clients with a family or past history of heart disease.
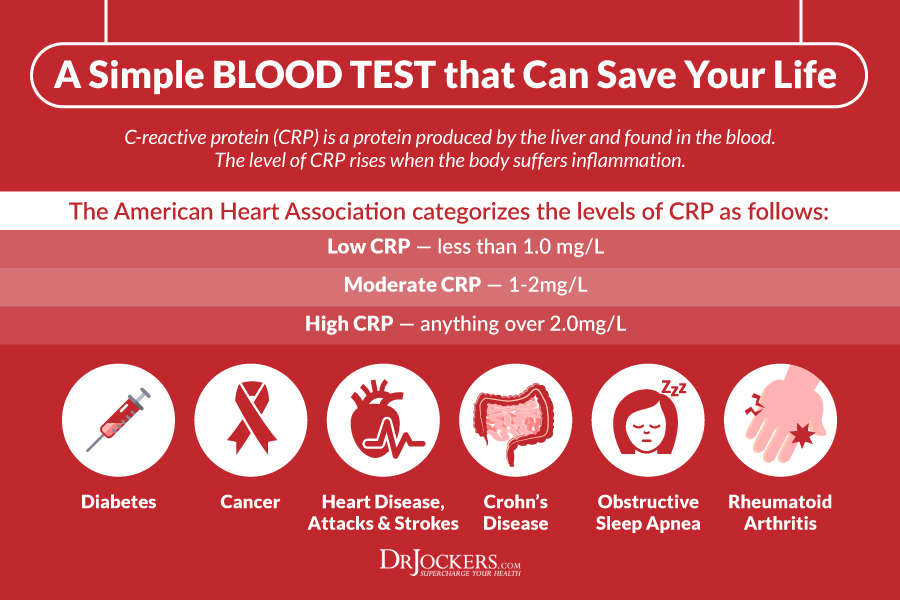
C Reactive Protein (CRP):
This is a protein found in the blood that rises in response to inflammation. During times of acute infections and resulting inflammatory responses CRP can elevate up to 50 times higher than normal. When the artery walls are inflamed and damaged CRP remains elevated (4, 5).
Even though many causative factors can increase CRP, research has shown that laboratory test level above 2.4 mg/l are at much higher risk of a heart attack compared to levels below 1 mg/l (6).
An anti-inflammatory diet and lifestyle are the critical keys to reducing CRP levels. This begins with a diet rich in phytonutrient dense vegetables, healthy fat and clean protein sources. Healthy fat sources include coconut products, avocados, olive oil, nuts, seeds, & purified omega-3 fish oil supplements.
Healthy protein includes wild-caught fish, grass-fed red meat and free range chicken, turkey and eggs. Anti-inflammatory herbs such as turmeric, cinnamon, ginger, rosemary, oregano & garlic are also powerful aids.
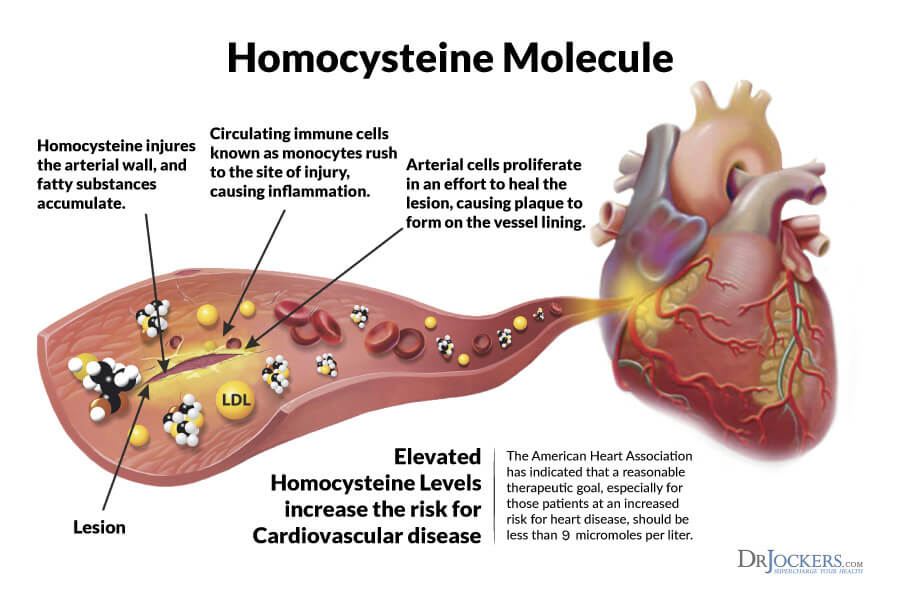
Homocysteine and Developing Heart Disease:
Homocysteine is an inflammatory amino acid that is produced as a byproduct of protein metabolism. Homocysteine-induced injury to the arterial wall is one of the factors that can initiate the process of atherosclerosis, leading to endothelial dysfunction and eventually to heart attacks and stroke (7, 8).
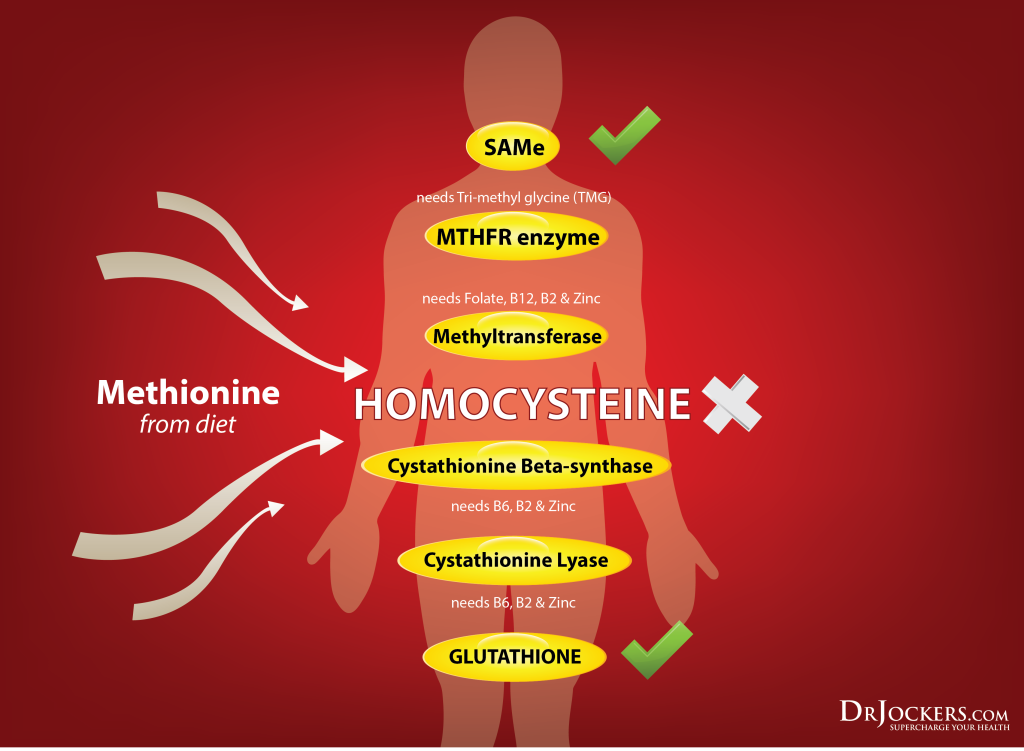
The amino acid methionine is digested and metabolized into homocysteine. When the body is sufficient in Vitamin B12, B6 & folate, excess homocysteine is remethylated into methionine or transsulfurated through vitamin B6 (9).
B Vitamins and Homocysteine:
When the body is deficient in any of these key B vitamins, it is unable to remethylate or transsulfurate the homocysteine. This leads to elevated levels of this inflammatory agent in the blood (10). Blood tests that show homocysteine levels above 6.3 umol/L are an indication of methylation deficiencies and elevated risk of heart disease (11).
Many individuals that have the MTHFR gene polymorphyism and other single nucleotide polymorphisms (SNP’s) have trouble with the methylation process and often have elevated homocysteine levels. To address this, one could try to juice green veggies and beets on a regular basis to get large amounts of these B vitamins and methylation elements.
Supplementing with premethylated forms of B2, B6, B12, and trimethylglycine have been shown to significantly lower homocysteine levels. Adequate amounts of magnesium, zinc and cellular anti-oxidants are also critical players in homocysteine metabolism (12). Clinically, I use Methyl Power as a main supplement to help reduce homocysteine levels.
Lipoprotein (a) Levels and Developing Heart Disease:
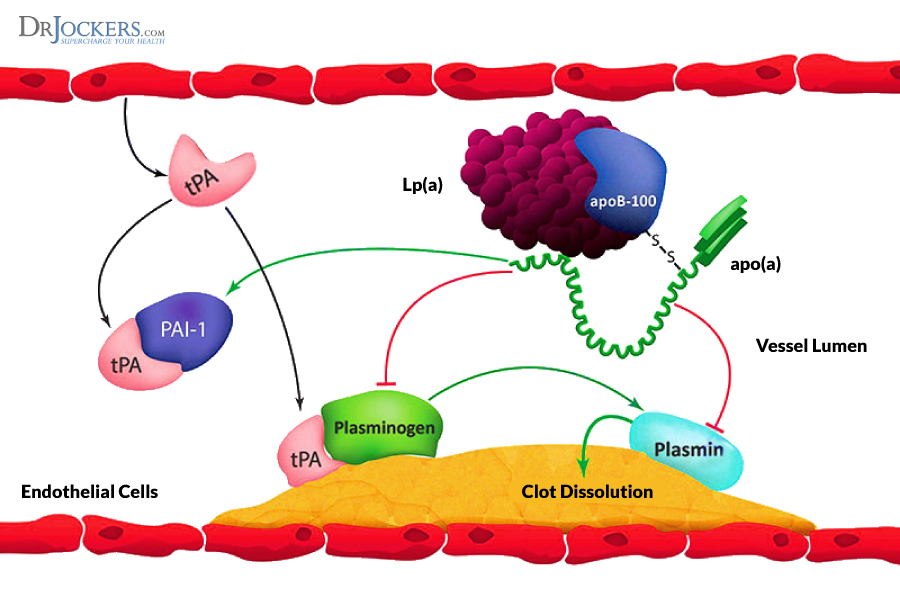
Lipoprotein (a) is a particular subclass of LDL cholesterol. Lp (a) is very similar in structure to a critical enzyme called plasminogen (13). Plasminogen helps the body dissolve blood clots. At any one time, our bodies are constantly making and dissolving microscopic blood clots. This dance is very delicate and dependent on a healthy balance of two blood clotting systems and this balance is key to know for your risk of developing heart disease.
If Lp(a) competes for binding spots for this blood clot dissolver, the blood system balance may form blood clots. The majority of heart attacks are caused by a blood clot in a heart artery at a site of atherosclerosis. Lp(a) has been shown to stimulate our immune cells to deposit cholesterol into heart artery walls thereby promoting the development of atherosclerosis (14).
A Lp(a) levels should be under 20 mg/dl and ideally under 14 mg/dl. This is an important test to consider when it comes to developing heart disease.
Lower Lipoprotein Levels:
Several nutritional supplements have been shown to lower Lp(a) naturally. High doses of vitamin B3 or Niacin is the most effective way to bring down Lp(a) levels (16, 17). The challenge with high doses of niacin is that it causes annoying hot flushes where the face and neck get red and the individual feels very warm.
This is quite scary for the individual if they are not educated on the flush beforehand and most doctors do not understand that this is a normal phenomenon.
Other key supplements include CoQ10, N Acetyl Cysteine, Acetyl-L-carnitine and alpha lipoic acid to boost mitochondrial health (18, 19, 20, 21). I put my clients with elevated Lp (a) on Mito Support which contains clinical verified dosages of these mitochondrial enhancing nutrients.






Thanks for that article. I read another article recently:
https://www.naturalnews.com/043882_homocysteine_heart_disease_circulatory_system.html
where it says:
“How one develops high levels of homocysteine
Homocysteine is a metabolic byproduct of protein metabolism and in particular the metabolism of methionine. Methionine is found in meats, seafood, dairy products, eggs, sesame seeds and Brazil nuts.”
Does it mean that if one has elevated homocysteine levels one should avoid these foods?
Marek – I wrote that article on homocysteine in NaturalNews. No, individuals with high homocysteine do not necessarily need to avoid methionine containing foods…they need to increase their methylated B6, B2, methylfolate and methylcobalamin and anti-oxidants.
I have an opportunity at a nearby hospital to have a test they call Cardiac Scoring? Would this test be helpful in evaluating my heart health. thank you for all you do.
Utley – I had a calcium scoring test, it evaluates levels of calcified plaque (not good) in your arteries. Non-invasive test, very low radiation.