 Ménière’s Disease: Causes, Symptoms & Support Strategies
Ménière’s Disease: Causes, Symptoms & Support Strategies
Ménière’s disease is a chronic disease of the inner ear characterized by vertigo, dizziness, tinnitus, the feeling of fullness in the ear, hearing loss, nausea, vomiting, and digestive issues. While there is no cure for the condition, there are several natural support strategies you can try if you have or are at risk of developing Ménière’s disease.
In this article, you will learn what Ménière’s disease is. You will understand its symptoms. I will explain the possible connection between Ménière’s disease and autoimmunity. You will understand the common causes of the disease and the conventional strategies used in treatment. Finally, I will share my top natural support strategies for Ménière’s disease.
What Is Ménière’s Disease
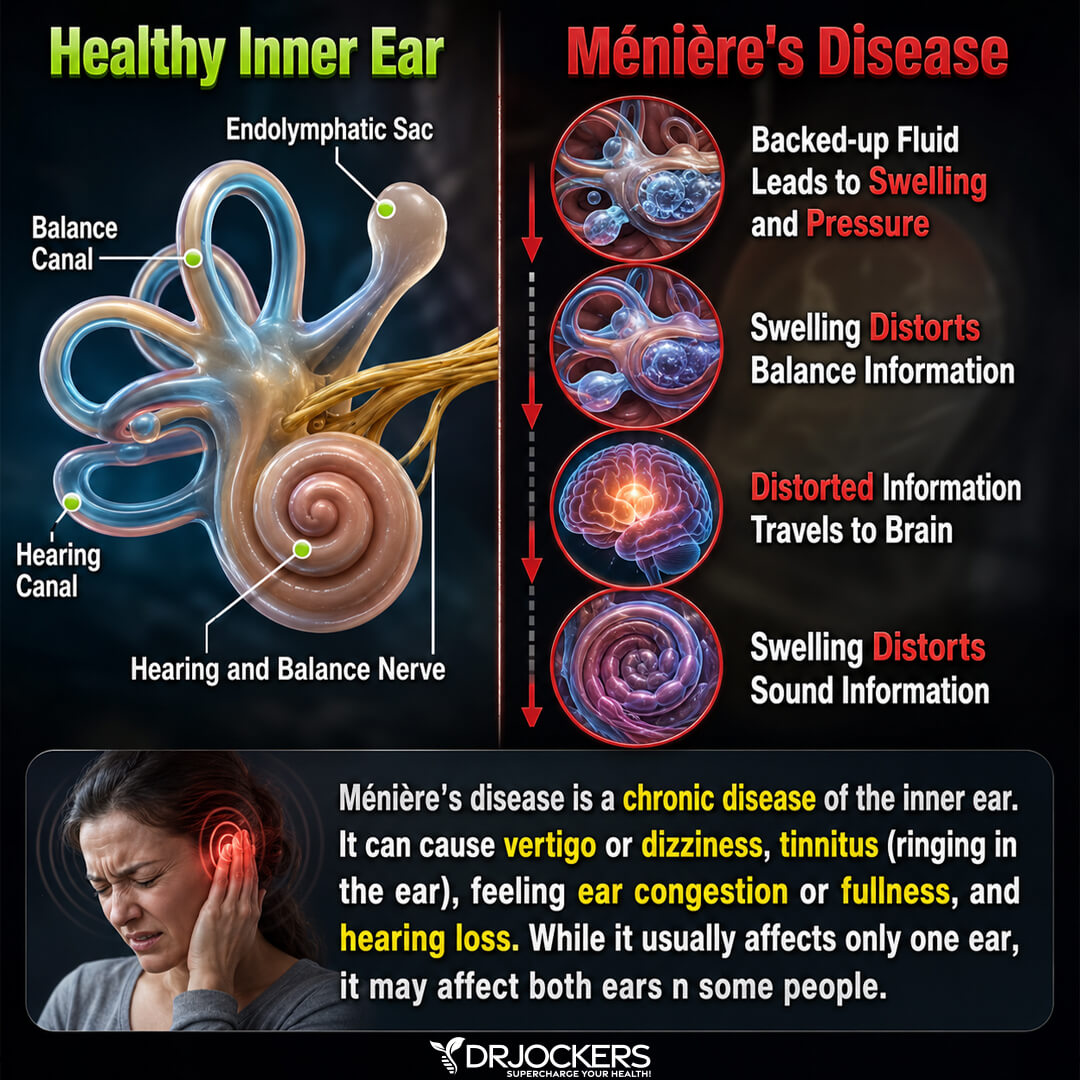
Ménière’s disease is a chronic disease of the inner ear. It can cause vertigo or dizziness, tinnitus (ringing in the ear), ear congestion or fullness, and hearing loss. While it usually affects only one ear, it may affect both ears in some people (1).
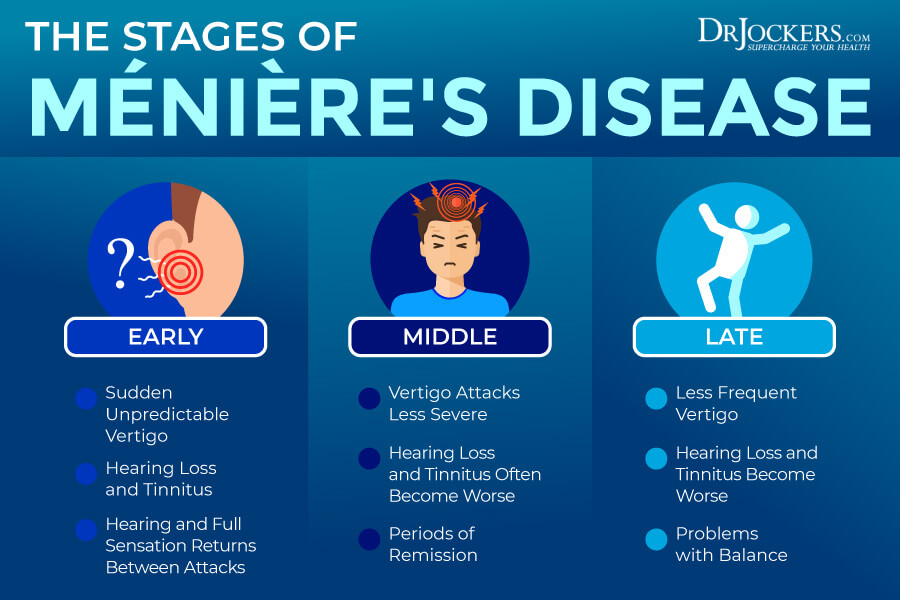
A person with Ménière’s disease may experience sudden dizziness, temporary tinnitus, or muffled hearing. While some people have one single attack of dizziness and none for a long time, others may have attacks closer together within a few days. In some individuals, vertigo can be serious, causing so-called ‘drop attacks’ where the person loses their balance and falls suddenly (1).
About 600,000 people are diagnosed with Ménière’s disease in the United States, along with about 45,000-60,000 new cases each year. While most people tend to develop Ménière’s disease between the ages of 25 and 50, it can develop at any age. Ménière’s disease is progressive and can be disabling (1).

Ménière’s Disease Symptoms
Ménière’s disease may be characterized by a buildup of fluid in the labyrinth of the ear, which is the compartments of the inner ear. This area of your ear contains the semicircular canals and otolithic organs necessary for balance and the cochlea needed for hearing. Symptoms of Ménière’s disease are the result of this buildup.
The labyrinth has two parts: the bony and the membranous labyrinth. If the membranous part gets filled with the fluid endolymph, it affects receptors when your body moves or changes position, which will send signals to the brain. This fluid build-up can lead to balance and movement issues. Fluid build-up in the cochlea can affect sound vibrations and sensory cells that send messages to your brain, hence affecting your hearing signals (1).
Common Symptoms of Ménière’s Disease May Include:
- Vertigo: This is an experience of compromised balance that can lead to a feeling of dizziness, spinning, moving, rocking, flip-flopping, or twisting. It may last for a few minutes to several hours. It may be severe and disabling and may lead to falling.
- Dizziness: Dizziness may happen upon standing up or walking up the stairs, or with other movements. It can be sudden and may worsen in a moving car or vehicle. It is less severe than vertigo.
- Hearing loss: Hearing loss of low frequencies can happen even at the early stages of the disease. It can progress over time and may lead to permanent hearing loss. It usually affects only one ear, but it may affect both. Some people only experience it during attacks and not in between, others do not experience remission, especially in later, more advanced stages of the disease.
- Nausea, vomiting, and other digestive issues: Vertigo and dizziness may cause nausea, vomiting, or even abdominal pain and diarrhea.
- Pressure in the ear: Ménière’s disease may cause general discomfort in pressure in one or both ears.
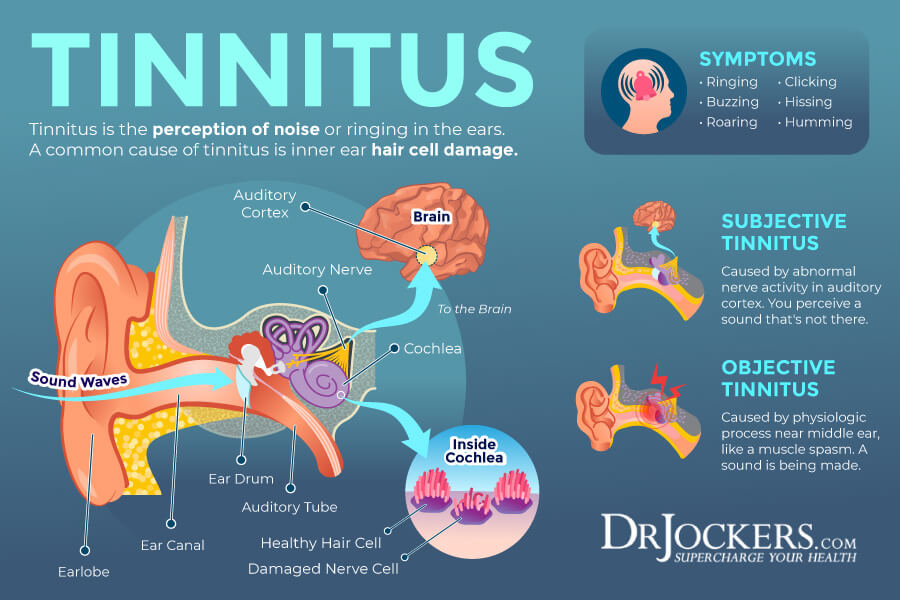
- Tinnitus: This experience is characterized by ringing, buzzing, chirping, whistling, hissing, or roaring in the ear. While it is not dangerous, it can be annoying and distracting, and may worsen over time.
- Uncontrollable eye movements: In some people, Ménière’s disease may cause nystagmus or ‘dancing eyes’ when the eyes uncontrollably move rapidly up and down, side to side, or in circles, usually connected to the sensation of movement and position.
Ménière’s Disease and Autoimmunity
Having an autoimmune disorder means that your own body’s immune system mistakes healthy cells for unhealthy cells and foreign invaders and mistakenly attacks itself. Some common autoimmune disorders include Crohn’s disease, Celiac disease, rheumatoid arthritis, lupus, and psoriasis, however, there are hundreds of less common and even more unidentified autoimmune disorders out there, and symptoms and diseases connected to autoimmunity. Having one autoimmune disorder increases your risk of developing other autoimmune conditions.
While it hasn’t been proven that Ménière’s disease is an autoimmune condition, some recent scientific evidence suggests it may be. A 2012 scientific review published in Autoimmune Review has discussed that Ménière’s disease may be connected to autoimmunity (2).
They’ve found that the immune response in Ménière’s disease is connected to antigens. Based on a positive response to steroids or clinical criteria, they’ve found that about one-third of cases may have an autoimmune origin, though the exact immunological mechanisms in the disease are not yet understood. Patients responded well to steroid treatment, which is often used in autoimmune disease.
Furthermore, a 2011 scientific study on 690 outpatient participants found a high prevalence of systemic autoimmune disease in those with Ménière’s disease (3). Researchers look at the prevalence of clinical criteria and immune system markers for rheumatoid arthritis, systemic lupus, and ankylosing spondylitis in those with Ménière’s disease. However, they didn’t look at patients with uni- or bilateral sensorineural hearing loss (SNHL), which can potentially be an important follow-up to the study.
While studies suggest that Ménière’s disease may be connected to autoimmunity, we don’t yet understand how it’s connected and whether or not Ménière’s disease is an autoimmune condition or triggered by autoimmunity. I suspect that we will learn much more about this in the upcoming years, and we can keep this information in mind when it comes to prevention and treatment.
Conventional Treatment Options for Ménière’s Disease
If you have symptoms of Ménière’s disease, it is important that you visit an otolaryngologist or ENT to go over your medical history and symptoms, get tested, and get the correct diagnosis. You doctor may order a variety of tests, including a hearing assessment, a balanced assessment, and various imaging tests, such as MRI and/or CT scans, to rule out a brain tumor, multiple sclerosis, and any other conditions with similar symptoms, and make sure that you, in fact, have Ménière’s disease (1).
Ménière’s disease is a chronic disease that has no known cure at this point. Doctors may use certain conventional treatment methods to alleviate symptoms or slow the disease. Later in this article, I will go over some natural strategies that may help you with Menier’s disease (1).
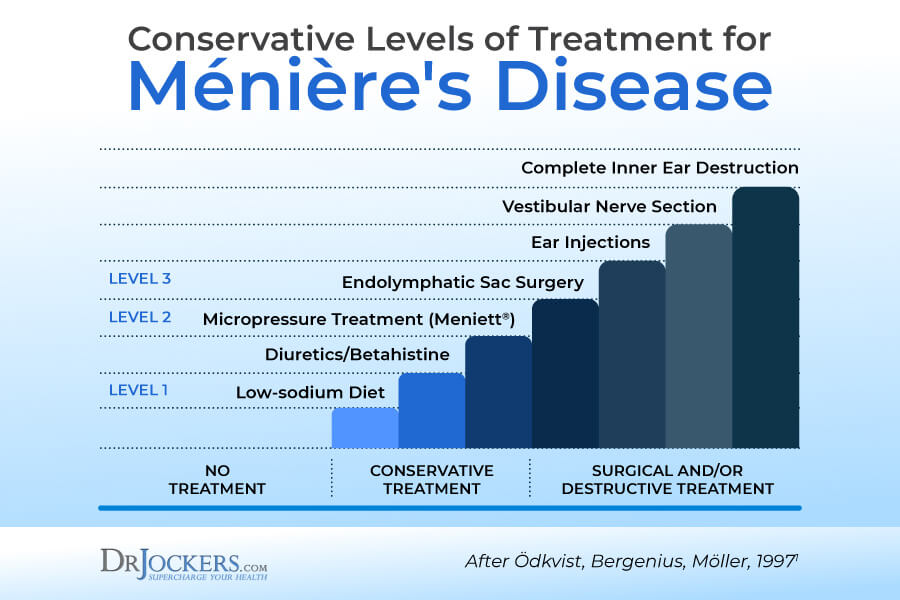
Ménière’s Disease: Conventional Treatment Options
Conventional treatment options for Ménière’s disease may include (1):
-
- Motion sickness medication and anti-nausea drugs: Motion sickness medication may be used to help with vertigo and nausea. Anti-nausea prescriptions may reduce extreme nausea or vomiting.
- Diuretics: Diuretics may help to control your dizziness by helping to lower fluid retention. Some of these medications may have certain side effects, including headaches, dizziness, thirst, muscle cramps, increased blood sugar, low sodium, and loss of potassium. Talk to your doctor if you experience any of these side effects while on these medications.
- Salt-restricted diet: Fluid retention may be associated with excess sodium. A salt-restricted low-sodium diet of fewer than 2,000 milligrams is often suggested by doctors.
- Other dietary and behavioral changes: Some patients may see improvement of symptoms when reducing or completely avoiding caffeine, chocolate, alcohol, and/or smoking.
- Cognitive therapy: Some people find cognitive therapy effective as it helps them to interpret and react to life experiences differently, reduces anxiety about the future and unexpected attacks, and helps them cope better.
- Hearing aid: Hearing aids may be suggested when one or both ears experience hearing loss. An audiologist can help to find the best available options for you if needed.
- Sign language: While sign language is not a treatment strategy, it may be a great idea if hearing loss is happening. It may not only help communication but also increase your confidence. Sign language is a ‘second language’ we can all benefit from learning, even with hearing loss or Ménière’s disease.
- Minett device: A Meniett device uses pulses of pressure to your ear canal to support inner fluid exchange to improve symptoms of vertigo and tinnitus. You can use this treatment at home.
- Rehabilitation: Vestibular rehabilitation may help to improve your balance, particularly between attacks, and may prevent falls and provide a sense of well-being and confidence.
- Injection: Antibiotic gentamicin injection into your ear may help to lower both the severity and the frequency of vertigo attacks. The problem with this method is that it may increase the risk of hearing loss. Using a steroid dexamethasone injection is an alternative option. It has less risk of hearing loss, however, it is also less effective than using antibiotics.
- Surgery: In some cases, when all treatment fails to reduce dizziness, surgery to decompress the endolymphatic nerve or, in some cases, to cut the vestibular nerve is performed. This is only a last resort strategy in serious cases.
- Alternative medicine: Some doctors are more open to alternative medicine and may suggest a more integrative approach involving acupuncture, acupressure, tai chi, or herbal medicine to complement conventional treatment. Later in this article, you will learn about all the natural support strategies I recommend that may support you with Ménière’s disease.

Causes of Ménière’s Disease
While we don’t have definitive answers to what causes Ménière’s disease, certain factors may increase your risk. Here are the most common causes of Ménière’s disease:
Family History & Genetics
Ménière’s disease seems to run in families. This may indicate that the disease may be the result of certain genetic variations or abnormalities that may affect the regulation or volume of the endolymph fluid in your ear (1). If you have a family member with Ménière’s disease, you may have an increased risk.
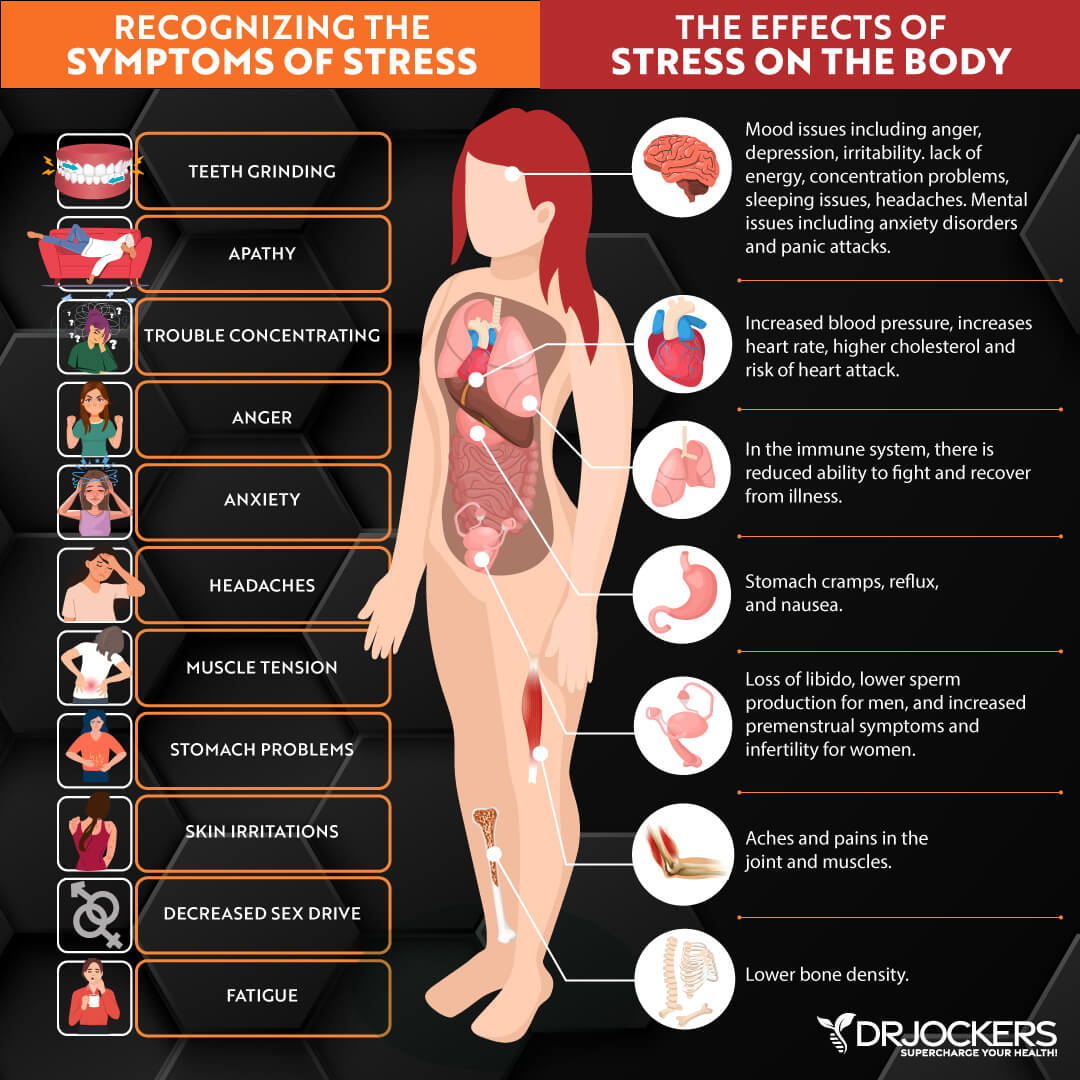
Chronic Stress & Poor Sleep
Chronic stress and poor sleep can increase inflammation in your body, which can increase your risk of any disease or increase in symptoms. According to a 2014 study published in the Annual Medicine and Health Science Research, psychological factors, such as increased anxiety and tension, can provoke and increase symptoms of Ménière’s disease (4).
Chronic stress and poor sleep can both trigger and increase anxiety and tension, hence may contribute to increased symptoms.
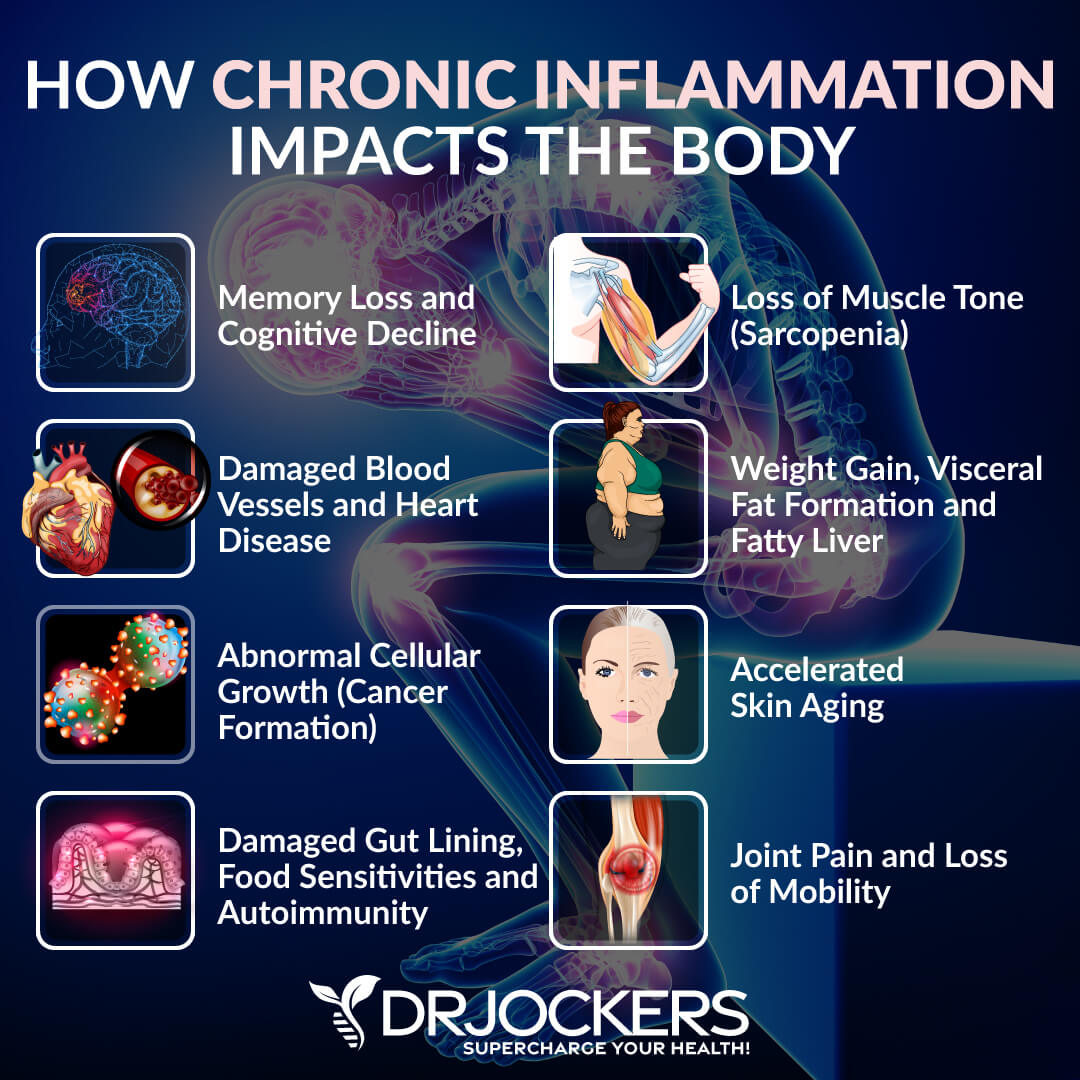
Inflammatory Diet
Eating an inflammatory diet high in refined sugar, processed foods, artificial ingredients, and junk food can increase your risk of inflammation and affect your symptoms of Ménière’s disease. Salt and sodium may increase fluid retention.
Many also find relief in symptoms when avoiding or limiting chocolate, sugar, caffeine, and alcohol, which indicates that these inflammatory foods may trigger symptoms of Ménière’s disease. An inflammatory diet may also increase your risk of autoimmunity, which has been linked to Ménière’s disease (1, 2, 3).

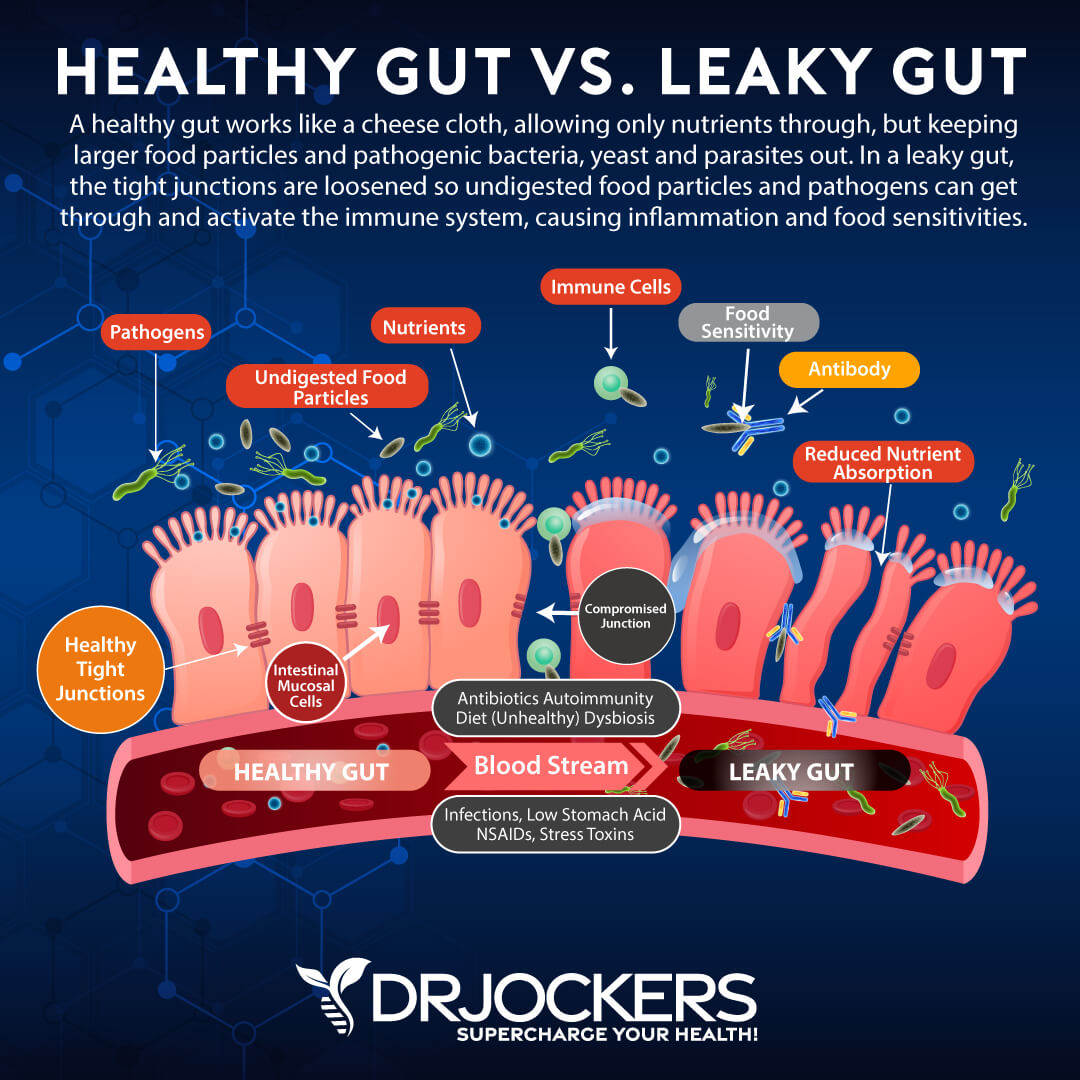
Chronic Infections and Leaky Gut
Your gut health is connected to everything in your body. Chronic gut infections and leaky gut syndrome can increase inflammation, autoimmune conditions, and chronic symptoms and health issues.
According to a 2018 study looking at urinary levels of mannitol and lactulose and fecal calprotectin ( all markers of altered intestinal permeability) in 26 patients with Ménière’s disease published in the American Journal of Otolaryngology, there may be a connection between intestinal permeability and Ménière’s disease (5).
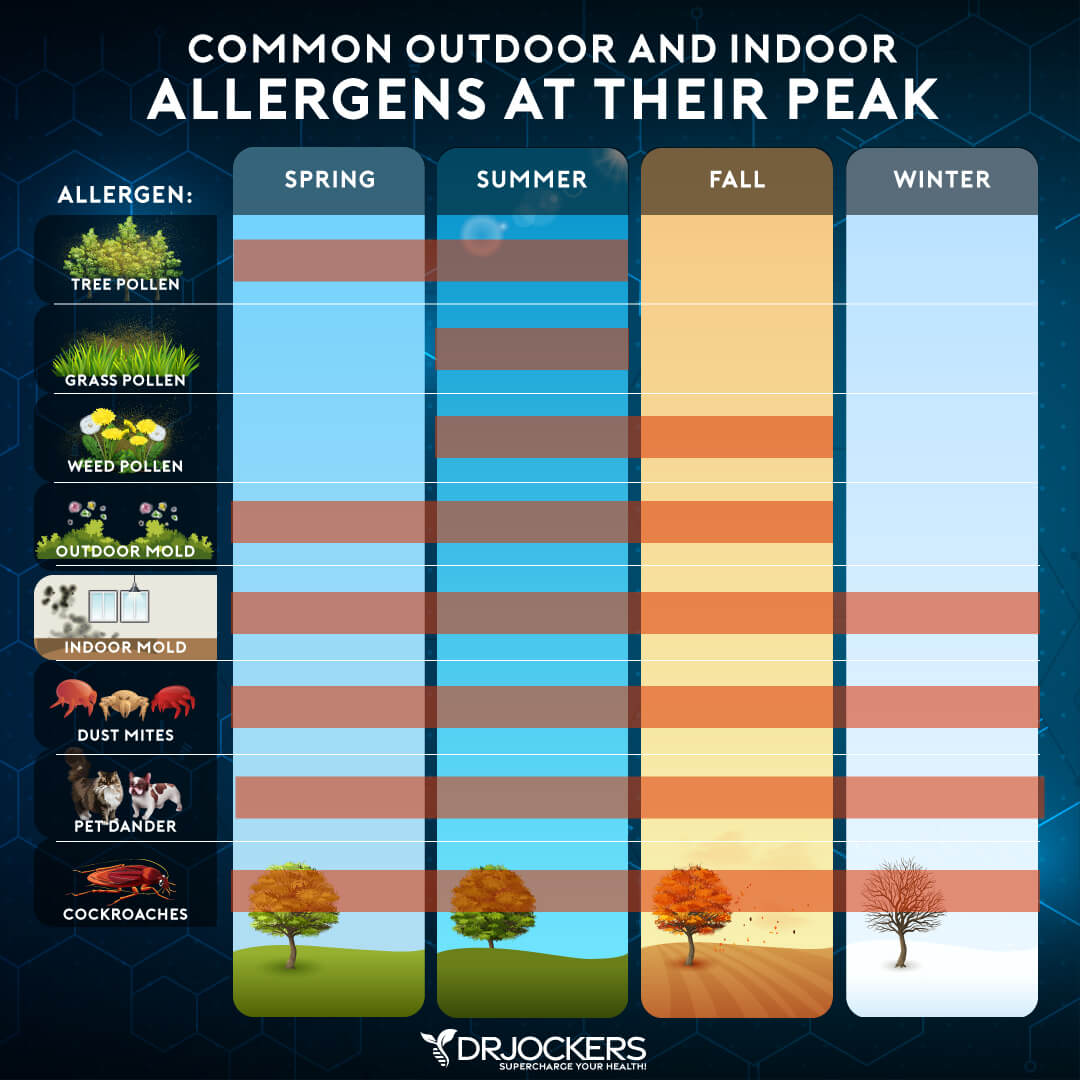
Food & Environmental Allergies & Sensitivities
Food and environmental allergies and sensitivities may increase inflammation and autoimmune conditions that have been linked to Ménière’s disease (1, 2, 3).
According to a 2014 study published in the Current Opinions in Otolaryngology & Head and Neck Surgery, allergic reactions in the inner ear may trigger Ménière’s disease, and there is a heightened allergic response can be observed in the disease (5).
Mold Exposure
Mold exposure can lead to inflammation and a series of symptoms and health issues. According to a 2018 study on mononuclear cells of patients with Ménière’s disease published in Scientific Reports, a pro-inflammatory cytokine release and a response to molds were observed, indicating the potential role of mold in symptoms of Ménière’s disease (7).
A 2013 study published in the Journal of Clinical Immunology has discovered an innate immune recognition of molds in those with autoimmune inner ear disease (AIED) and Ménière’s disease, and mold exposure is a potential trigger for autoimmunity in AIED (8).

Vitamin D Deficiency
Vitamin D is an important vitamin that may play a role in Ménière’s disease. A 2019 study published in Frontiers in Neurology found decreased vitamin D levels in those with vestibular neuritis, a condition characterized by vertigo, nausea, and vomiting that are similar to the symptoms of Ménière’s disease (9).
Another 2019 study published in Otology and Neurotology found that vitamin D may play a role in Ménière’s disease and inner ear conditions (10). If you struggle or have a family history of Ménière’s disease, I would recommend getting your vitamin D levels tested and making sure you get them over 50 ng/mL

Natural Support Strategies
If you are experiencing symptoms of Ménière’s disease or are at risk of the condition, there are some natural support strategies you can try. Here is what I recommend:
Anti-Inflammatory Nutrition Plan
Inflammation and eating an inflammatory diet can trigger symptoms of Ménière’s disease (1, 2, 3). I recommend following an anti-inflammatory nutrition plan to lower inflammation and reduce symptoms. Remove refined sugar, refined oils, artificial ingredients, processed foods, and junk food.
Since these may be triggering for Ménière’s disease, reduce or avoid caffeine and alcohol, and reduce your salt intake. Eat an anti-inflammatory diet rich in greens, vegetables, low-glycemic index fruits, herbs, spices, healthy fats, fermented foods, and clean animal protein.

Test for Food Sensitivities
Food sensitivities can trigger inflammation and increase or mimic certain symptoms of Ménière’s disease. I recommend that you get tested for food sensitivities. While there are some blood tests that are commonly used, they can produce false results and don’t cover all foods.
I recommend that you try some biofeedback testing strategies, such as pulse testing and muscle response testing. Additionally, following an elimination diet and watching your symptoms during the reintroduction phase is a great tool to uncover your personal food sensitivities.
Once you know that you are sensitive to food, remove it from your diet. Common food sensitivities include sugar, gluten, wheat, soy, corn, dairy, and legumes; however, many people have other, less common sensitivities. Certain food sensitivities may improve over time and new ones can also develop, so it’s a smart idea to test for food sensitivities yearly or if new symptoms arise.

Reduce Stress & Improve Sleep Quality
Support your anti-inflammatory nutrition plan with an anti-inflammatory, healthy lifestyle. Reduce your stress levels and improve sleep quality to lower anxiety, tension, and inflammation, and reduce symptoms (4). Try meditation, breathwork, yoga, Tai Chi, nature walks, grounding, gratitude practice, and prayer.
Spend time supporting people and learn to react to stress better with a positive and calm outlook. Develop a relaxing bedtime routine that helps you relax and unwind at night. Make sure to develop a regular sleep schedule supporting your natural circadian rhythms and getting 7 to 9 hours of sleep at night.

Avoid Molds & Allergens
Mold exposure and allergens can be a serious trigger for Ménière’s disease symptoms (7, 8). I recommend that you check your home for hidden mold and make sure that you get it professionally removed or move.
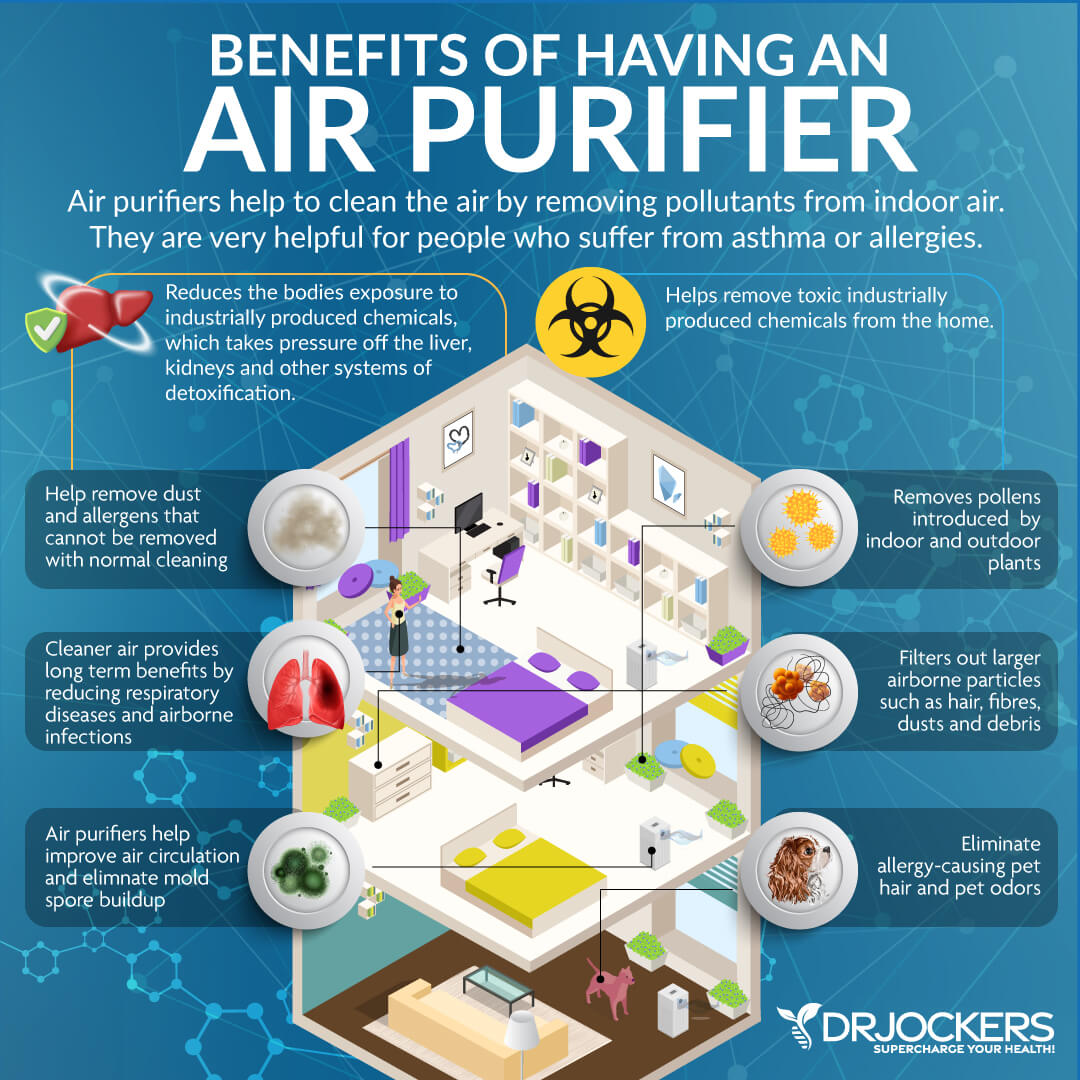
Use a high-quality indoor air filtration system to remove mold and allergens in the air. Support your immune system through nutrition, lifestyle, and supplementation to help your body be more resistant to allergens and mold.

Improve Indoor Air & Water Quality
Fresh air and clean water are essential for your health, and air or water toxicity can lead to an array of symptoms and health issues. I recommend getting a high-quality indoor air filtration system that can filter out bacteria, viruses, fungi, mold, and other toxins or pathogens.
I recommend a water filtration and purification system to make sure that you are drinking clean water instead of regular tap water. Avoid plastic bottles, and use glass jars, glass or aluminum bottles, or ceramic mugs instead.
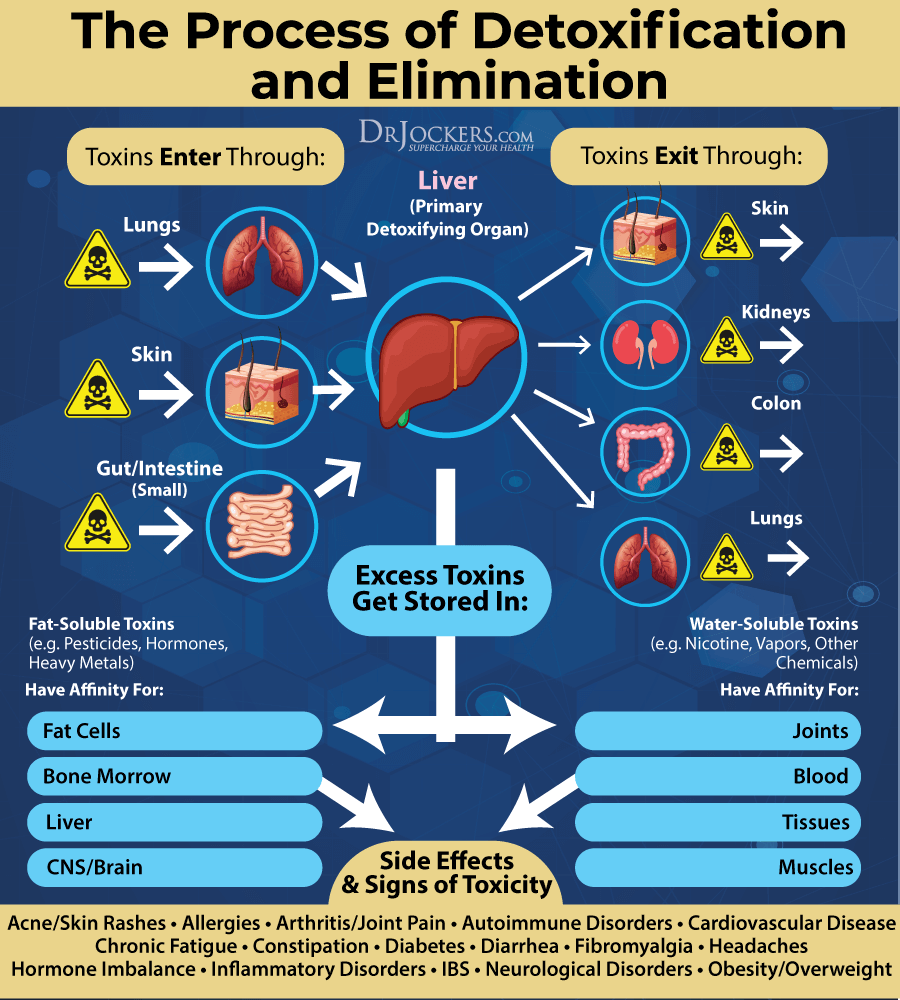
Improve Detoxification Pathways
While reducing toxic exposure is critical, it is impossible to avoid all toxins, and we all have toxic buildup in our bodies that we accumulated throughout our lives. Improving your detoxification pathways is non-negotiable.
Drink plenty of water and eat anti-inflammatory, nutrient-dense, detoxification-supporting foods to support your digestion, liver and kidney function, and elimination through urine and bowel movements.
Improve detoxification through the skin through sweating from exercise and infrared sauna use. Try dry brushing to support lymphatic health and remove dead skin cells.
Sound & Music Therapy
Sound and music therapy may help to reduce the risk of or slow the development of certain symptoms of Ménière’s disease related to hearing. According to a 2013 study on 23 patients with acute tinnitus published in the International Journal of Clinical and Experiential Medicine, 10 consecutive sessions of individualized music therapy have improved tinnitus in participants.
Since tinnitus is one of the main symptoms of Ménière’s disease, music therapy may be a great technique for the reduction of this symptom (11). I would recommend specific music therapy or classical music that can be calming for the brain.

Vitamin D Supplementation
As you’ve learned, there may be a correlation between vitamin D deficiency and Ménière’s disease, and vitamin D supplementation may help symptoms. According to a 2016 study published in Auris Nasus Larynx, vitamin D deficiency has been linked to vertigo, and supplementation may be beneficial (12).
According to a 2018 study published in Medical Hypotheses, vitamin D supplementation may help to improve symptoms of Ménière’s disease (13). While spending time out in the sun and eating foods rich in vitamin D, such as fish, liver, and egg yolks, are helpful, it is not enough to optimize your vitamin D levels.
I also recommend daily supplementation with vitamin D for optimal health. Look to get your levels tested once or twice each year and aim to get your levels in the 50-100 ng/ml range.

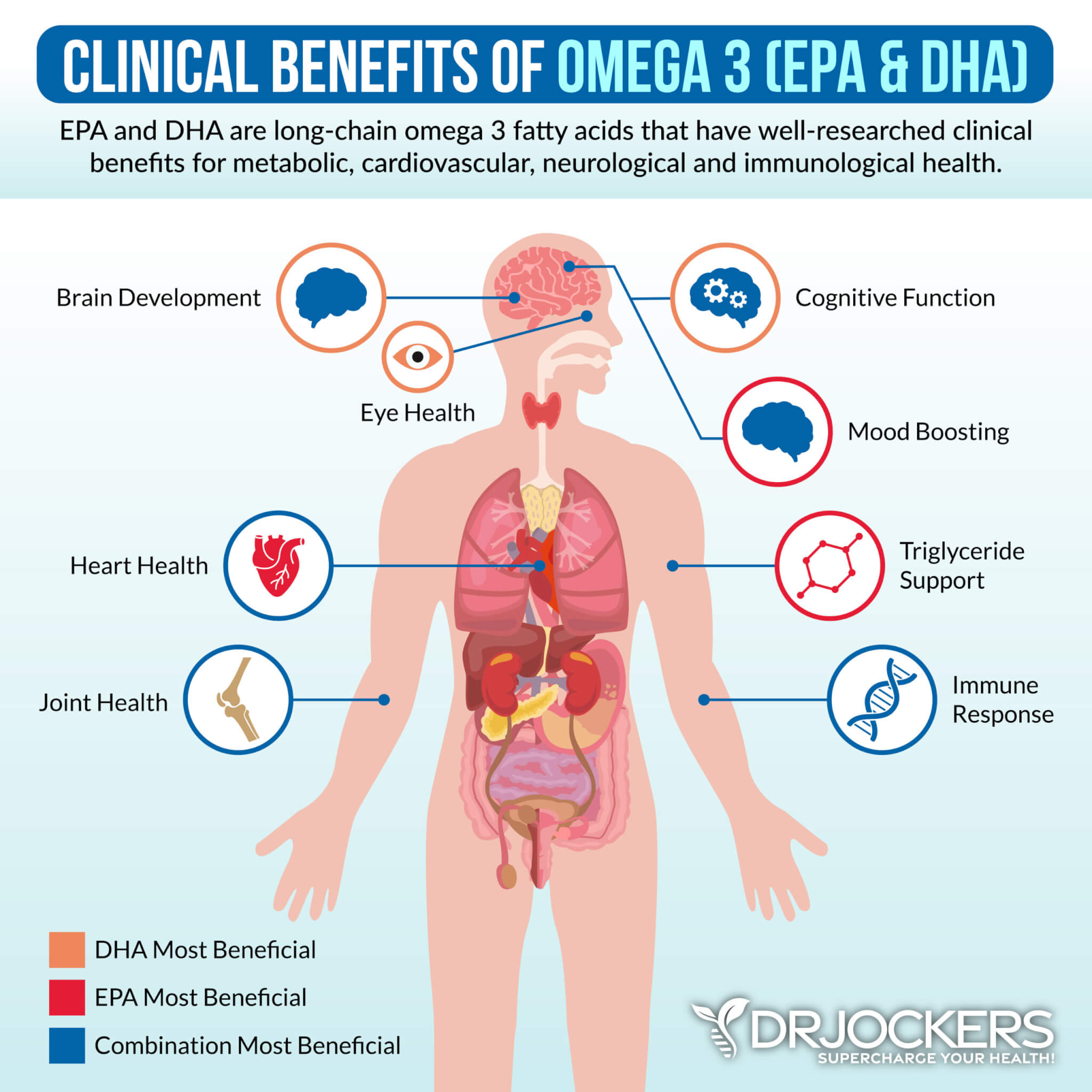
Increase Omega-3 Fatty Acids
Omega-3 fatty acids have powerful anti-inflammatory properties. A 2012 study published in Medical Hypothesis has found that supplementary omega-3 fatty acids may support homeostasis in the inner ear and benefit the treatment of Ménière’s disease and other inner ear disorders (14).
Fish, seafood, chia seeds, flax seeds, and hemp seeds are great sources of omega-3 fatty acids. Additionally, I also recommend daily supplementation with a high-quality omega-3 fish oil supplement.
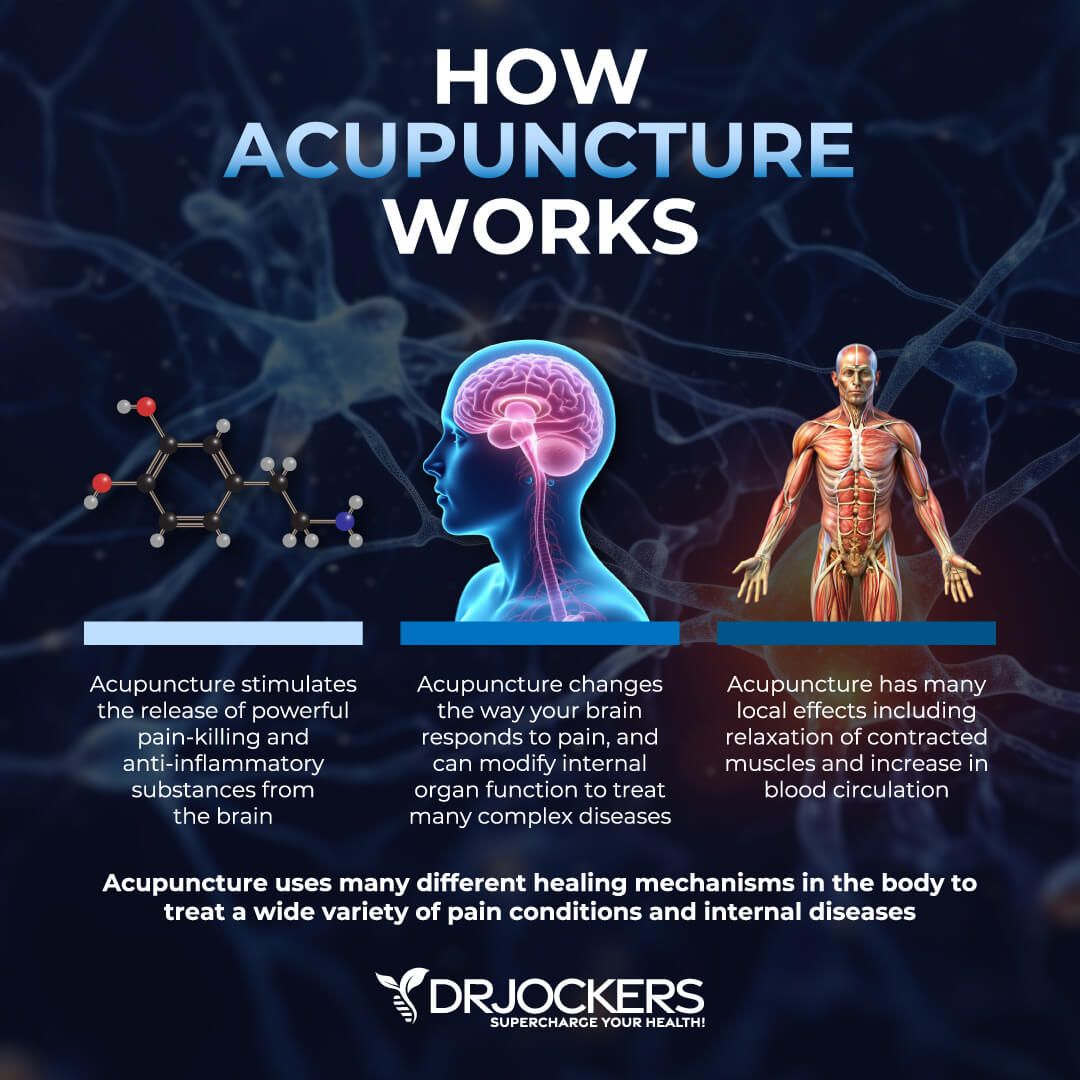
Acupuncture Treatment
Acupuncture is a form of alternative medicine and a part of traditional Chinese medicine (TCM). It uses thin needles in trigger or acupressure points that stimulate blood flow and specific organs and systems in your body to recreate balance and health.
Several studies, including a 2011 study published in Evidence Based Complimentary and Alternative Medicine, a 2016 study published in Evidence Based Complimentary and Alternative Medicine, and a 1983 study published in the American Journal of Chinese Medicine, all have found that acupuncture may benefit the treatment of Ménière’s disease (15, 16, 17). If you have Ménière’s disease, acupuncture treatment may be a safe way to improve your symptoms.
Chiropractic Care
Chiropractic care is another popular alternative medicine modality that involves spine manipulation and musculoskeletal bodywork to create balance and health in your body. A 2009 case study published in the Journal of Chiropractic Medicine found that chiropractic work was beneficial in the management of Ménière’s disease in a 40-year-old female patient (18).
A 2011 systematic review published in Chiropractic and Manual Therapies has found that chiropractic work and manual therapy may be effective for dizziness, which is one of the main symptoms of Ménière’s disease (19). If you have Ménière’s disease, chiropractic care may be a safe way to improve dizziness and possibly other symptoms.

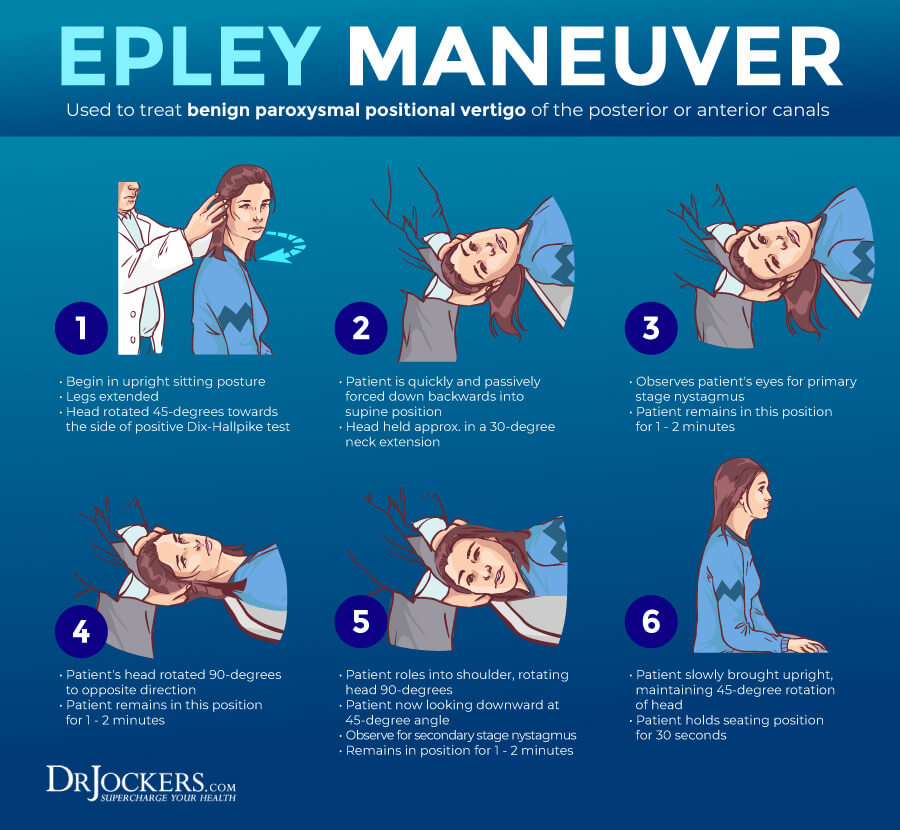
Vestibular Rehab & Epley Maneuver
Vestibular rehab is a method used by vestibular physical therapists to reduce symptoms of dizziness. The Epley maneuver is a method used by professionals to improve vertigo. Both dizziness and vertigo are associated with Ménière’s disease and may help the condition.
A 2017 pilot study on 70 patients published in Disability Rehabilitation has found that vestibular rehabilitation may help to improve imbalance related to Ménière’s disease (20). According to a 2007 study published in the Brazilian Journal of Otorhinolaryngology, the Epley’s maneuver may be beneficial for vertigo associated with Ménière’s disease (21).
Final Thoughts on Ménière’s Disease
Ménière’s disease is a chronic disease of the inner ear characterized by vertigo, dizziness, tinnitus, the feeling of fullness in the ear, hearing loss, nausea, vomiting, and digestive issues. If you have or are at risk of developing Ménière’s disease, follow my natural support strategies to benefit your health and well-being.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our team offers long-distance functional health coaching programs to help you achieve your health goals.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and thrive in life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!




GOD SAID THEIR IS A CURE FOR EVERY DISEASE EXCEPT DEATH IN ALL THREE MAIN HOLY BOOKS
Hi jockers.
I am a patient meniere’s disease
First attack 2010 diagnose in 2014
1 First question
Please give me dait food chart
2 next question my big problem
Biometric changes weather is too much problem I don’t have solution
Sorry to hear about this! I would encourage you to work with a functional health coach to customize a specific plan for you. Here is a helpful article: https://drjockers.com/functional-nutrition-tips-to-find-a-great-health-coach/