 Post Birth Control Syndrome: Symptoms & Natural Treatment
Post Birth Control Syndrome: Symptoms & Natural Treatment
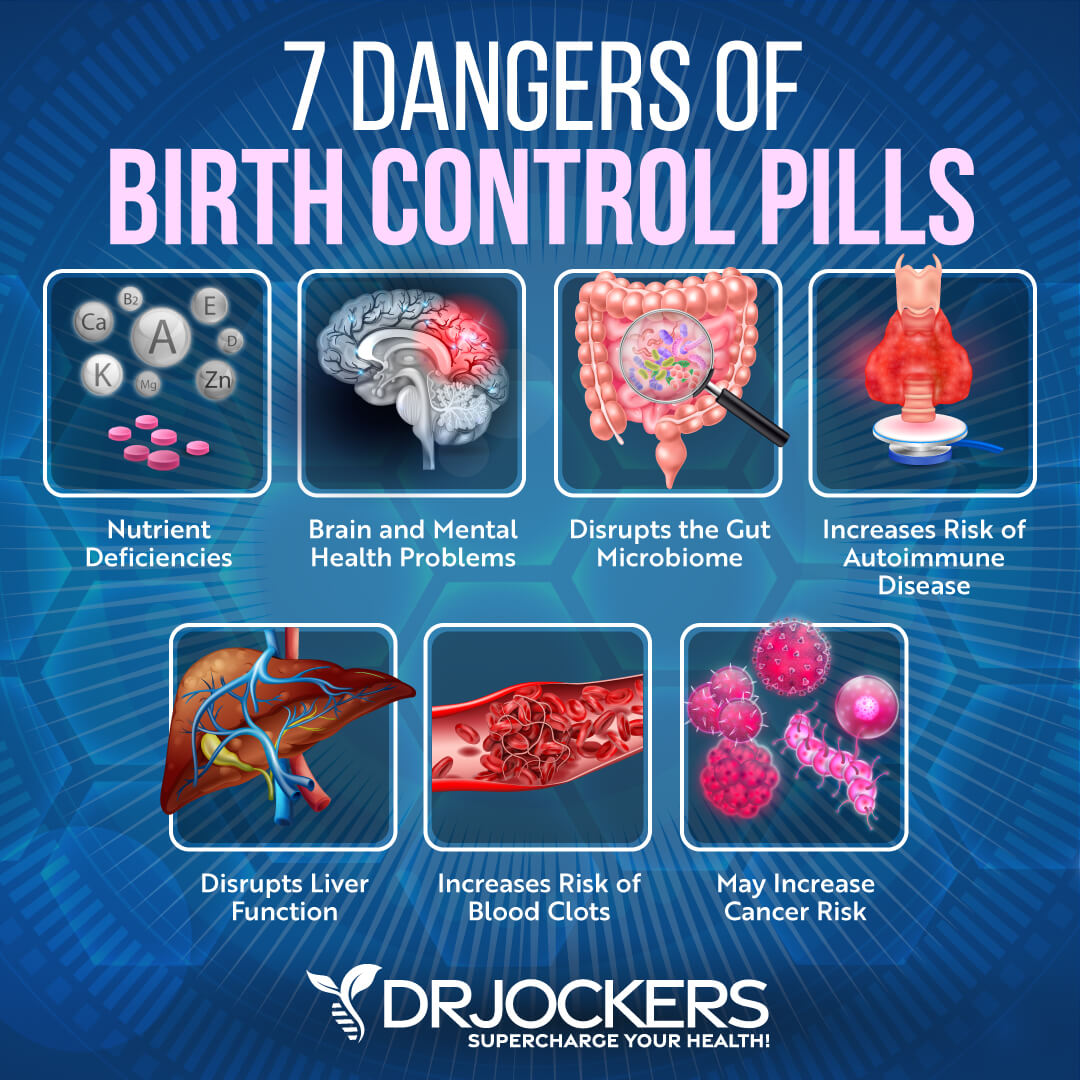
The pill, or oral contraceptives used for birth control, are a way of artificially altering female hormones to prevent pregnancy. Many women choose to utilize this type of therapy in order to reduce their risk of pregnancy during times when it would not be desirable for them.
Other uses include reducing the risk of osteoporosis, certain cancers, and anemia. There are certainly pros and cons to oral contraceptive use. One commonly overlooked downside is post birth control syndrome.
Post Birth Control Syndrome is characterized by a set of symptoms that arise 4-6 months following the discontinuation of oral contraceptives. In this article, we will follow a common narrative of someone dealing with post birth control syndrome.

Common Symptoms of Post Birth Control Syndrome
Oral contraceptives largely exhibit their effect in the body by altering hormone levels. Consequently, many of the symptoms of post birth control syndrome seem to be related to hormonal imbalance issues.
The symptoms of post birth control syndrome often include:
- Irregular Periods
- Interrupted or Halted Menstruation
- Unwanted Weight Gain
- Mood Imbalance
- Skin Issues
- Hair Thinning
- Digestive Issues
- Blood Sugar Imbalances
Not every woman experiences these symptoms when stopping their birth control. For those who do, they can be very disruptive to daily life. Luckily, there are ways to mitigate the imbalances.
Real Life Testimony of PBCS
“I feel like I’m doing everything right and my jeans still don’t fit,” my 32-year-old patient Carla said during our first office visit. “I feel bloated, gassy and pretty much unsexy all the time. I’m depressed for absolutely no reason – and it gets much worse just before my period”. It never used to be this way, but ever since I stopped the pill I’ve been feeling worse.
Carla consulted me because she struggled with post birth control syndrome (PBCS). These symptoms were occurring ever since she made the decision to go off the pill more than eight months prior. Reviewing her health history, I noticed Carla’s doctor had recently prescribed several rounds of antibiotics for a urinary-tract infection (UTI).
Also, Crohn’s disease ran in her mom’s side of the family and her father’s side had a history of severe depression. As a doctor who helps women treat autoimmune disease and balance their hormones, I drew the parallel between Carla’s symptoms and her gut health.
Carla was gaining weight and feeling inflamed almost daily. Her story revealed that her weight gain began within months of beginning birth control and despite stopping it, she wasn’t able to make her weight budge. She had once been physically active, but now, she felt that her knees and other joints complained a little too much for her to continue her normal exercise regimen.
Birth Control and Gut Health
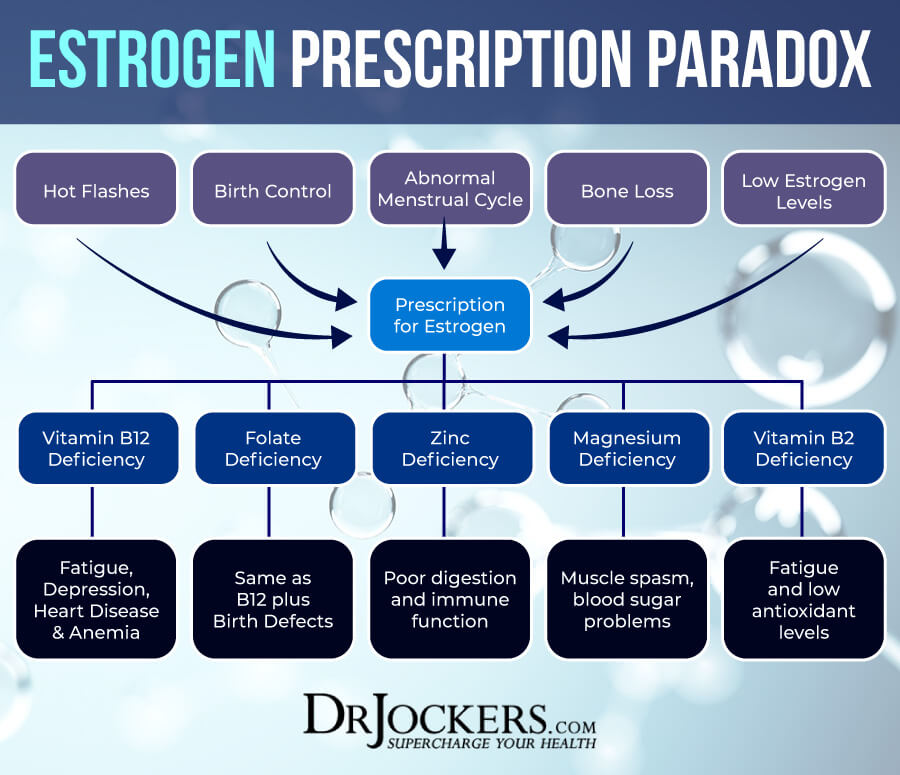
Studies show that even a short round of antibiotics can lead to an imbalance in gut health for up to two years (1). Just like antibiotics, birth-control pills can contribute to leaky gut, dysbiosis (an imbalance in gut bugs and reduced microbial diversity), and can even trigger autoimmunity.
Among those problems, studies show that the pill can disrupt estrogen metabolism and contribute to weight-loss resistance (2). The pill also increases your risk for inflammatory bowel diseases like Crohn’s disease and ulcerative colitis. In fact, two large prospective cohort studies of American women linked oral contraceptive use with Crohn’s (3). (For the record: These women also had a history of smoking.)
We’re unsure exactly why oral contraceptives trigger inflammatory conditions like Crohn’s, but researchers speculate that impaired immune function leading to inflammation, an out-of-balance microbiome, and increased intestinal permeability (leaky gut) are potential causes (4).
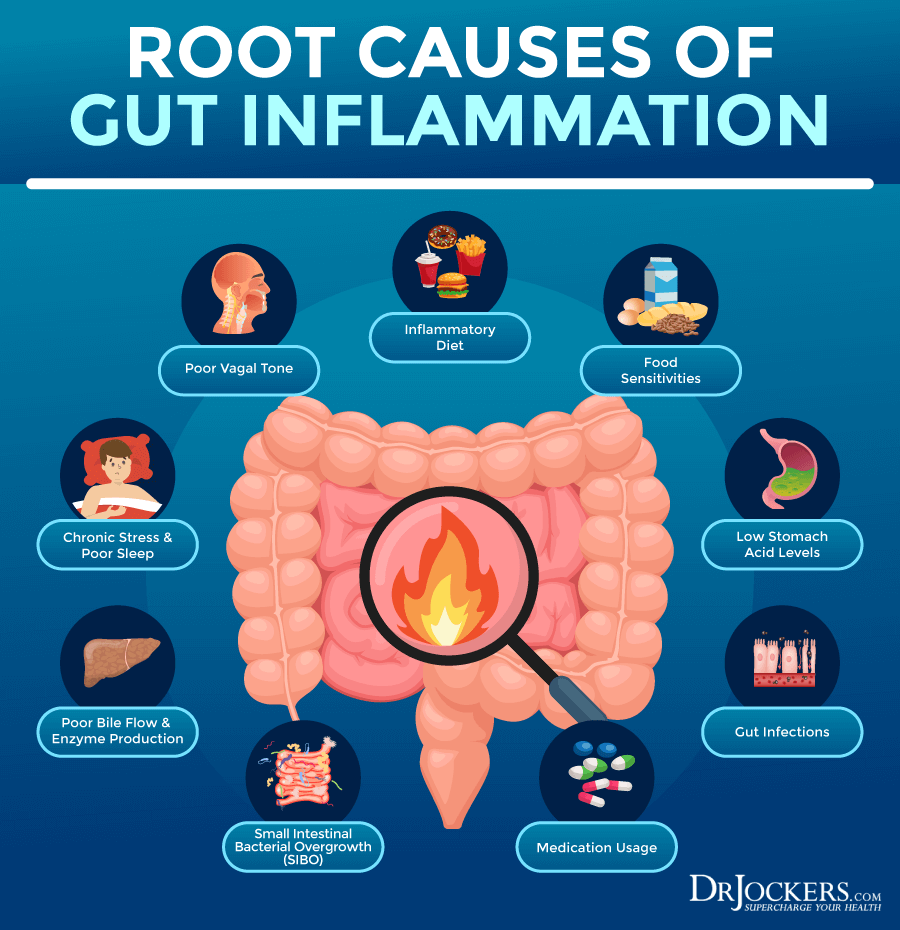
Birth Control and Inflammation
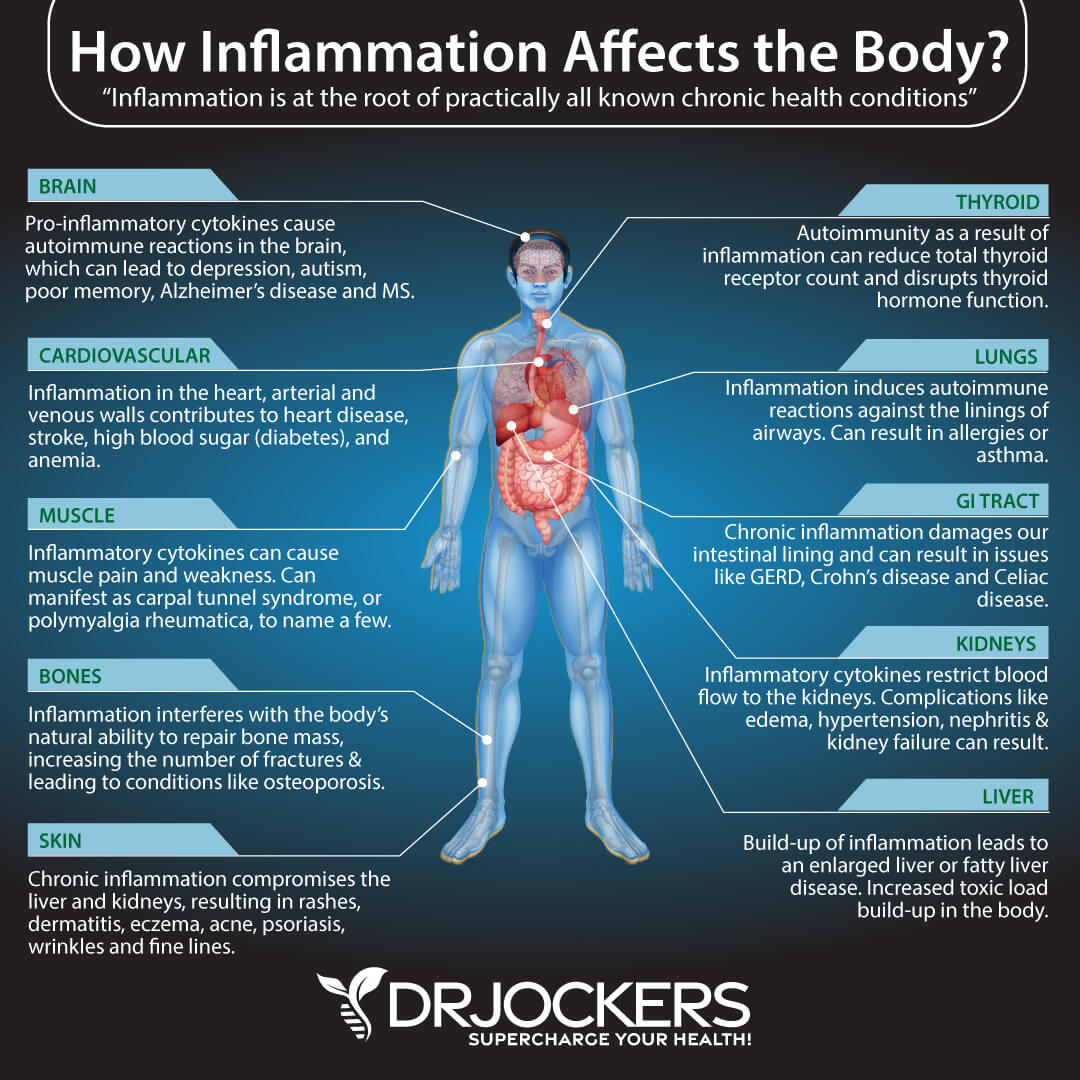
Carla’s problems were obvious once we put it all together. She had weight-loss resistance, depression, and leaky gut. All of which are heavily tied to inflammation. After all, chronic inflammation plays a part in nearly every disease on the planet, including autoimmunity, depression, thyroid disease, insulin resistance, and obesity (5).
Carla was struggling to lose weight. Clinically, I find that women will not be able to lose weight until they’ve resolved their inflammation by focusing on the root cause. The majority of women who struggle with birth control related weight gain begin to lose weight once inflammation is lowered. This makes sense given that studies show chronic inflammation contributes to obesity and other symptoms of metabolic syndrome. These include elevated cholesterol and high blood pressure (6).
We now understand that hormonal birth control can be inflammatory and contribute to insulin resistance. The good news is that once you begin to address the inflammation you can begin to lose weight. As you lose weight, you will also lower inflammation, which improves gut, mood, hormones and overall health (7).
Post Birth Control Depression
Carla had blamed her depression on genetics, but as we know, many women struggle with mood imbalances. These mood disorders can be a result of post birth control syndrome. They can also be present while still on birth control. About 95 percent of serotonin is manufactured in your gut. This makes gut health an important component of emotional stability (8).
The pill can disrupt this process by destroying healthy gut flora, increasing intestinal permeability, and causing inflammation. All of this meant Carla wasn’t making enough of this “happy” neurotransmitter that also plays a role in gut mobility, explaining why she felt so bloated.
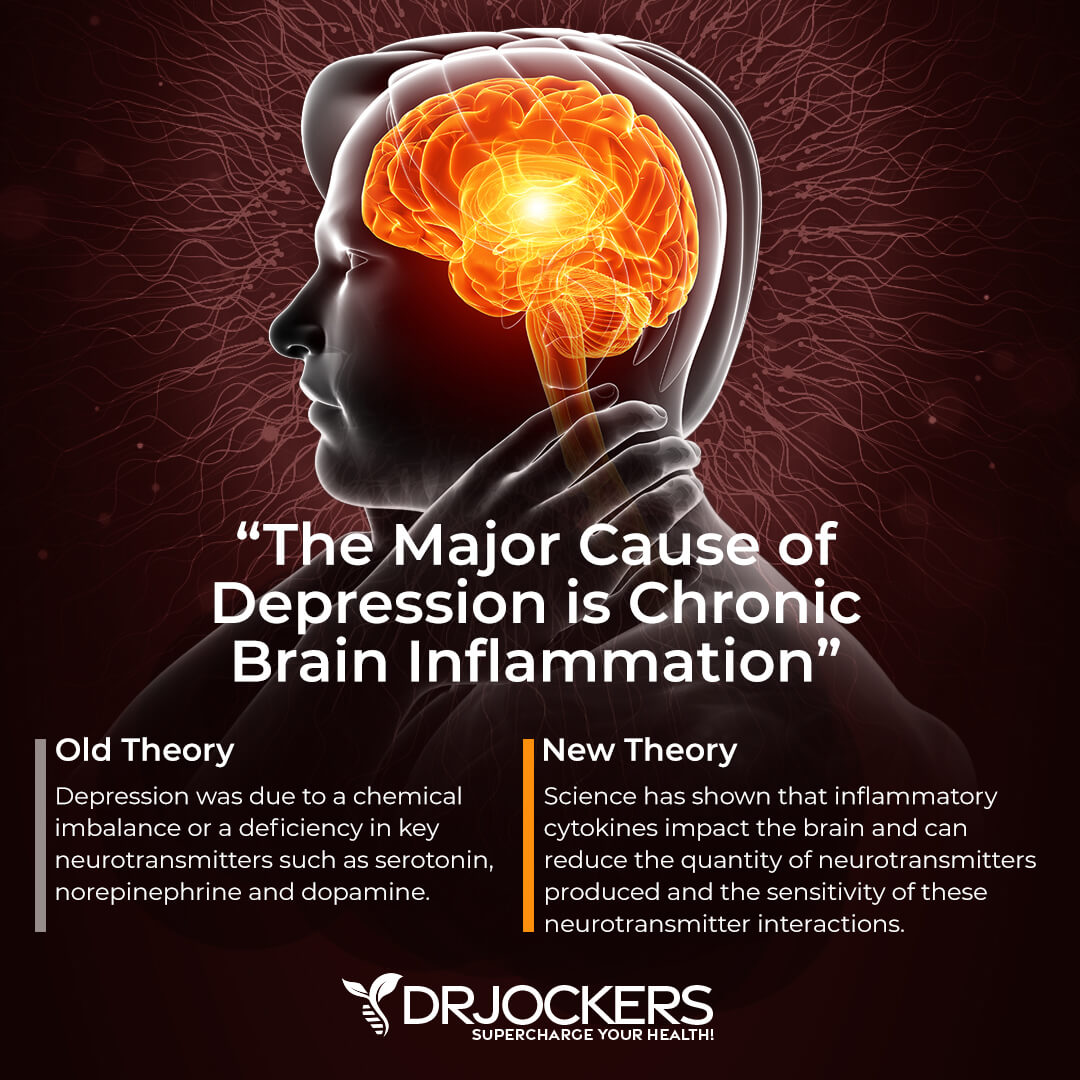
Newer studies have also begun to explain the connection between depression and inflammation, suggesting that depression might occur due to chronic inflammation itself (9). If your gut, cardiovascular system or other parts of your body are feeling inflamed, then you’re more likely to struggle with your mood.
Birth Control and Leaky Gut
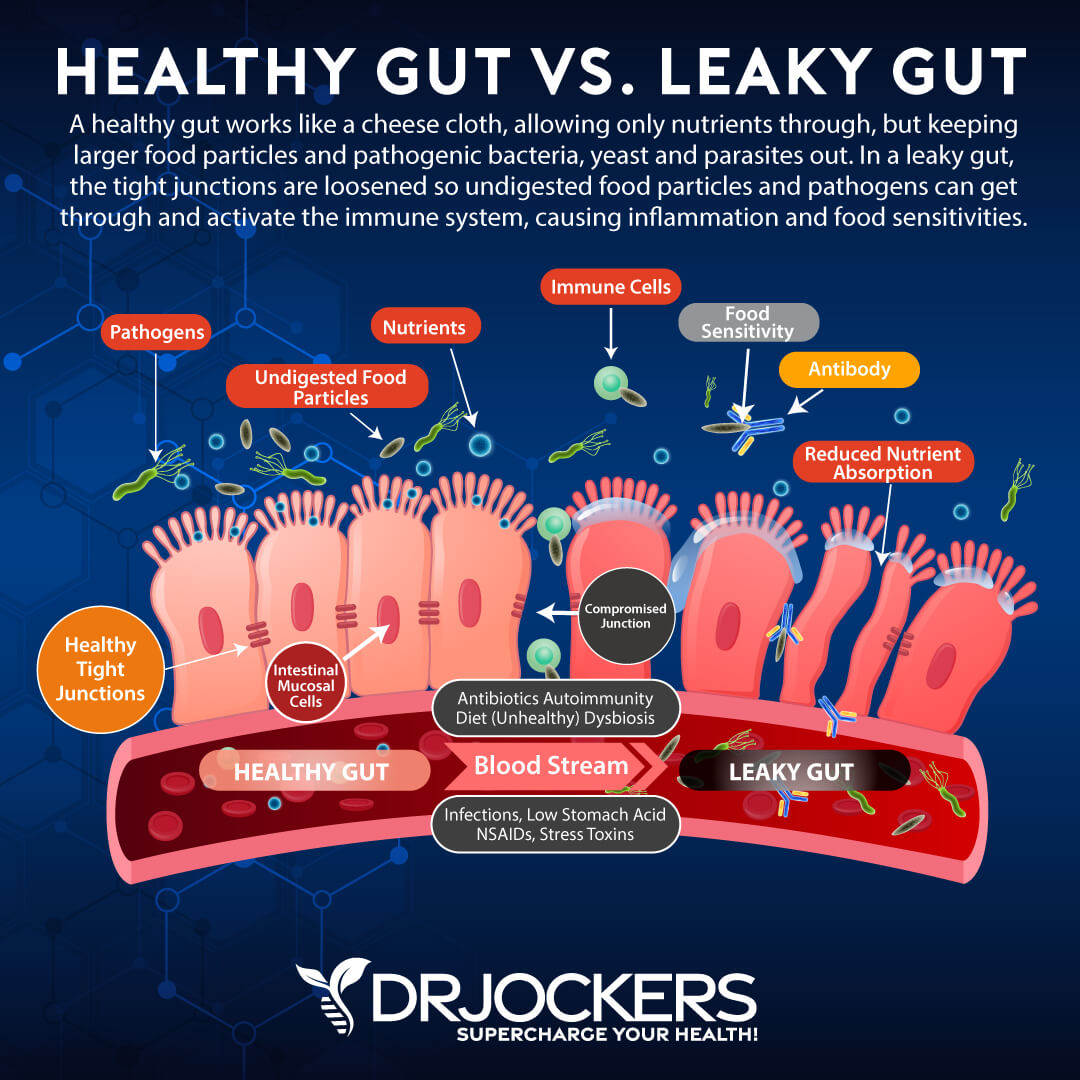
Leaky gut conditions weren’t doing Carla any favors. With leaky gut, undigested food proteins and microorganisms like bacteria or yeast make their way through your gut wall. This typically leads to an over-active immune response (10). This is part of how autoimmune disease, food sensitivities, and chronic inflammatory diseases develop.
For Carla, the number of foods she developed a sensitivity to continued to climb. “I remember it wasn’t long after I started the pill that I noticed more and more foods would make me feel bad. My other doctor told me to just stop eating them,” she explained.
Sadly, I see this all too often in my medical practice that women will be told to eat less and less foods without anyone ever making the connection that the root of the issue is the pill. And without intervention, the gut will not heal, and most women will remain sensitive to the foods they’ve become intolerant even as they discontinue birth control.
Disruption of Ovulatory Cycle
Carla was not ovulating regularly. Hormonal birth control, like the combination pill, works by shutting down brain-ovarian communication. That means for as long as you are on it, your ovaries and brain do not talk.
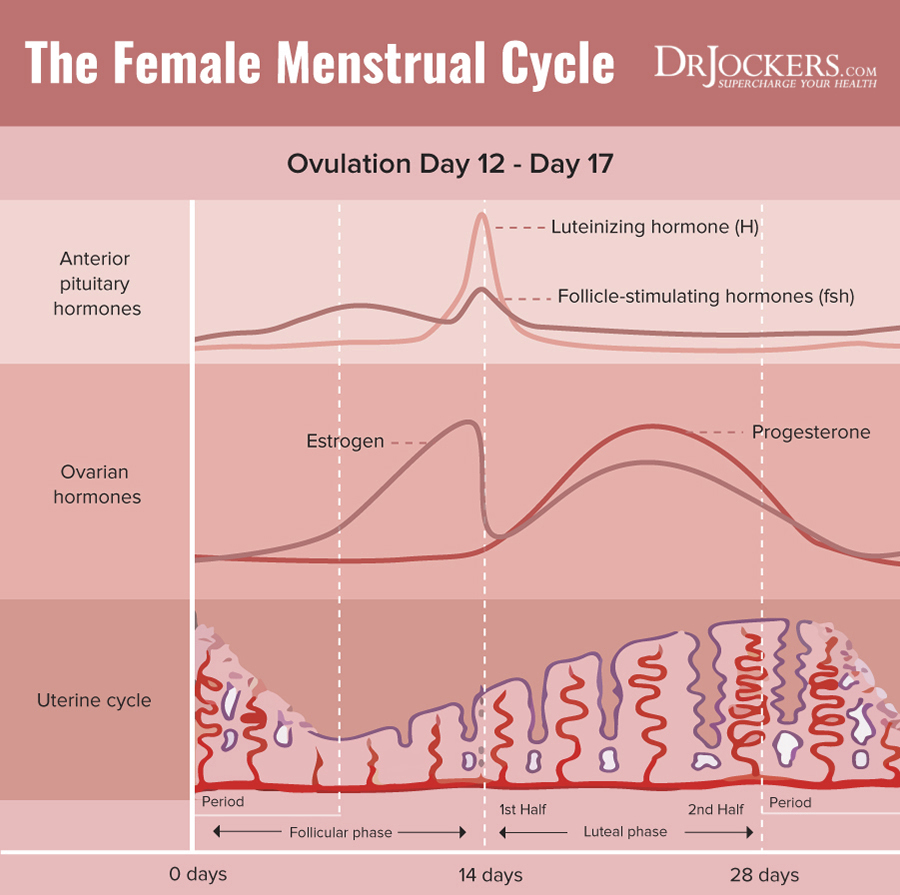
In a typical cycle, the brain secretes Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH) in order to support egg maturation, ovulation and the production of hormones—namely estrogen and progesterone. But like many women with post birth control syndrome, Carla’s body was struggling to re-establish communication again.
She had enjoyed regular 30-day cycles before beginning the pill, but now off, her cycles were more irregular and signs of ovulation were “hit or miss” in her words. Without ovulation, we do not make progesterone.
Following ovulation, a structure known as the corpus luteum is formed and secretes progesterone. For Carla, the lack of ovulation meant she didn’t have sufficient progesterone, which led to a state of frank estrogen dominance. This was part of the puzzle piece for the mood, bloating, and weight gain.
 Other Menstrual Issues
Other Menstrual Issues
In post birth control syndrome, we see several forms of ovarian dysfunction. Some women fail to ovulate at all, leading to symptoms of estrogen dominance and PMS. Others don’t produce enough estrogen at all in their cycle, leading to hot flashes, night sweats, vaginal dryness, and increased aging of the skin.
For others, their issue may be excess testosterone in what I’ve termed an androgen rebound. This is where working with a health practitioner that can order labs and interpret your symptoms can make all the difference in your healing.

Healing Post Birth Control Syndrome
Carla clearly was struggling with PBCS. Her mood, digestion, weight, and hormones were all in need of attention. Luckily, the body has a good memory of what homeostasis is.
By supporting the body with good nutrition, supplementation, and certain lifestyle strategies, many women can sort out their post birth control syndrome symptoms.

Eliminate Sugar
Numerous studies have shown that a diet high in added sugars can lead to increased inflammation and weight gain (11). No surprise there. But it was more than just cutting out the sugar she added to her daily cup of coffee.
Carla’s diet needed to shift away from processed foods and other places where sugar loves to hide. Any diet that leads to increased inflammation can cause your body to pack on pounds, make you feel sad, drive PMS up, and cause hormone imbalances. For Carla, label reading was a must, and she was surprised to discover her favorite yogurt had over 30 grams of sugar in every serving!

Anti-Inflammatory Nutrition
In addition to eliminating sugar, we also had Carla increase whole foods that are known to bring down inflammation. Studies have shown omega-3 fatty acids, like the kind you find in cold water fish, to be beneficial in inflammatory gut disease, including inflammatory bowel disease (IBD) (12). Fish is also rich in selenium and iodine, which support thyroid and overall hormonal health. Wild-caught salmon is one of the best options for this.
Carla also began including a cup of cruciferous vegetables daily, which are great for supporting optimal estrogen metabolism. Getting lots of herbs and spices like rosemary and turmeric are great to support liver detox, support a healthy microbiome and lower inflammation.
For more information on taking the first steps to implement an anti-inflammatory diet, check out this article here: How to Follow a Healing Diet

Control Stress
Research has connected psychological stress with gut dysfunction, including inflammatory gut disease and irritable bowel syndrome (IBS) (13). In my experience, everyone has their own unique way to de-stress.
For Carla, she needed 10-minute walking breaks at work and to schedule more social time with friends. For you, it might be an Epsom salt bath, massage, deep breathing, meditation, or a cup of calming tea.
Other important strategies for reducing stress include using herbal adaptogens, supplementing with extra magnesium, sauna use, cold plunges, regular exercise, and following the other strategies listed in this article.

Optimize Sleep
Poor sleep goes hand in hand with low progesterone and for Carla, the week before her period was the worse. She had trouble getting to sleep and so would spend hours scrolling through social media. Our first step was to break the screen time habit and instead, we got Carla doing deep breathing and gentle stretching to unwind before bed.
Poor sleep has been shown to cause immune dysfunction and can lead to increased inflammation (14). We added in magnesium, which Carla was deficient in, and wearing amber glasses to support healthy serotonin and melatonin production in the evening.

Eliminate Highly Reactive Foods
Carla had numerous foods sensitivities that contributed to her inflammation, hormone imbalance and you guessed it—digestive issues. While we worked on healing her gut, she needed to let go of two big offenders—dairy and gluten.
Both of these foods on their own can lead to leaky gut, set the immune system into a rage, drive weight loss resistance, and a variety of other problems. Cutting gluten has been shown to lower inflammation and improve insulin sensitivity, both of which are made worse by the pill (15). While we eliminated these foods, we also used nutrients like L-glutamine and quercetin to heal Carla’s gut. After a month, Carla began to reintroduce foods that previously made her feel ill and found that she was much less reactive than before.
Depending on the severity of your digestive issues, here are 3 great strategies for eliminating reactive foods:
Elimination Diet: This is a nutrition plan in which a set of food groups are avoided for a period of time (such as 30-90 days). After this period, foods are added in one at a time and monitored for reactions in the body. Read more about this here: 5 Steps to Following an Elimination Diet
Food Sensitivities Testing: The most efficient method of identifying reactive foods is to use food sensitivities lab testing. There are many options available for this that can be read up on here: What is the Best Food Sensitivity Testing Method
Fasting & Liquid Nutrition: While it is a more restrictive option, partaking in a water fast, followed by a period of liquid nutrition (elemental diet) can be a powerful reset for the gut. For greater benefits, this period can be followed by a carefully planned elimination diet. Read more about Fasting and Liquid Nutrition here: Healing Leaky Gut with Fasting and Liquid Nutrition

Post Birth Control Awareness Summit
Post-birth control syndrome can be a real challenge for most women, especially when they stop birth control only to find their symptoms remain. Women are often told that this is just a normal part of being female and getting back on birth control is the solution.
There is so much more you can do to heal and I’d love to show you how! That is why I have created the first ever Post Birth Control Syndrome Awareness summit aimed at connecting you with the experts to get you comprehensive support wherever you are in your birth control journey. In this online conference, we have a wide range of expert classes addressing PBCS, birth control side effects, acne, infertility and more.
There are six speaker tracks designed to get you the answers you need on or off of birth control:
Track 1: Post-Birth Control Syndrome
Off birth control and now your hormones are worse than when you started? Sign up for this track if you want to reverse symptoms or minimize damage when you get off hormonal birth control.
Track 2: Resolving Skin Problems and Preventing Breakouts
If acne or chronic yeast infections are your core problem, we’ll cover what you can do about both here.
Track 3: Reversing Period Problems
Heavy periods? Painful periods? Missing periods? Unpredictable periods? This track will help you get your period back to normal.
Track 4: Prevent Birth Control Side Effects
This track will help you understand why birth control causes the side effects it does and what you can do about it — whether you plan to stay on birth control or come off.
Track 5: Recover Libido and Fertility
If your libido or fertility has been off since your experience with birth control, this track reveals why, what you can do about it, and how you can finally get “in the mood” again.
Track 6: Cancer, Mood and Metabolism
You may have heard about the studies that link birth control to cancer, mood disorders, and a breakdown in women’s metabolism. This track will address what you can do about these things with the most up-to-date research.
Check out the entire program for yourself by going here. Consider owning this powerful information and sharing it with other women in your life. Together we can change women’s medicine for the better, raise awareness about PBCS, and help you feel your best!
About the Author
 Dr. Jolene Brighten is a Functional Medicine Naturopathic Medical Doctor and a nutritional biochemist. She is the founder of Rubus Health, a women’s medicine clinic that specializes in women’s hormones. She is recognized as a leading expert in Post Birth Control Syndrome and the long-term side effects associated with hormonal contraceptives. Dr. Brighten is the author of the upcoming book, Beyond the Pill, which is the first book to detail how to maintain your health on birth control and reverse symptoms of post-birth control syndrome. She is a speaker, urban farmer, and the medical advisor for one of the first data-driven apps to offer women personalized birth control recommendations.
Dr. Jolene Brighten is a Functional Medicine Naturopathic Medical Doctor and a nutritional biochemist. She is the founder of Rubus Health, a women’s medicine clinic that specializes in women’s hormones. She is recognized as a leading expert in Post Birth Control Syndrome and the long-term side effects associated with hormonal contraceptives. Dr. Brighten is the author of the upcoming book, Beyond the Pill, which is the first book to detail how to maintain your health on birth control and reverse symptoms of post-birth control syndrome. She is a speaker, urban farmer, and the medical advisor for one of the first data-driven apps to offer women personalized birth control recommendations.





we have been on 3 different types of medications so far, but none seems to help me. Either I can’t tolerate it or one didn’t give any results.there is a herbal approach that has worked across Africa and China for centuries, this herbal approach has recorded a tremendous success stopping the disease progression and gradually alleviate all symptoms for MS.in other to purchase from them kindly visit their online website totalcureherbsfoundation c om
Good luck to each and every one of that’s trying this herbal formula.