16 Ways to Achieve Healthy Poop!
Have you looked before you flushed lately? If not maybe you should. Nobody wants to discuss the basic human function of pooping unless you have an appreciation for potty humor, but opening up the discussion may save your life.
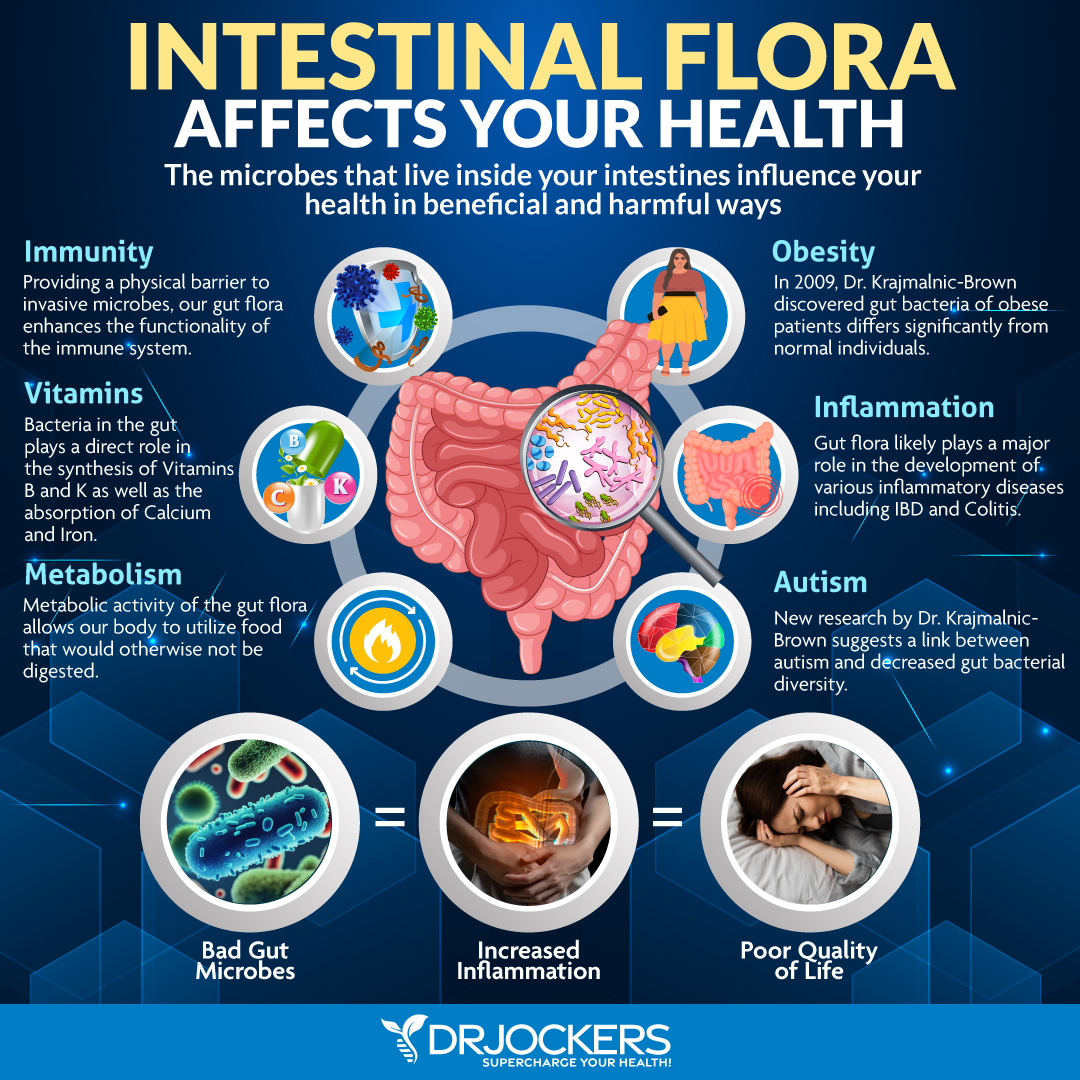
Microbes ferment the food we eat and create good and bad chemicals. Good chemicals we call nutrients and bad chemicals are toxins. Good microbes eat toxins and poop out B vitamins and other beneficial compounds. Bad microbes eat nutrients from the food and poop out toxins. When we have a bowel movement, we release much of these endotoxins and reduce our microbial load. This takes a huge stress off of our gut, brain-adrenal axis and our immune system.
Before you flush next time, ask yourself: Is my poop normal or not? Do I have healthy poop? In order to answer these questions, you first have to understand what normal stool is.
 The Bristol Stool Scale:
The Bristol Stool Scale:
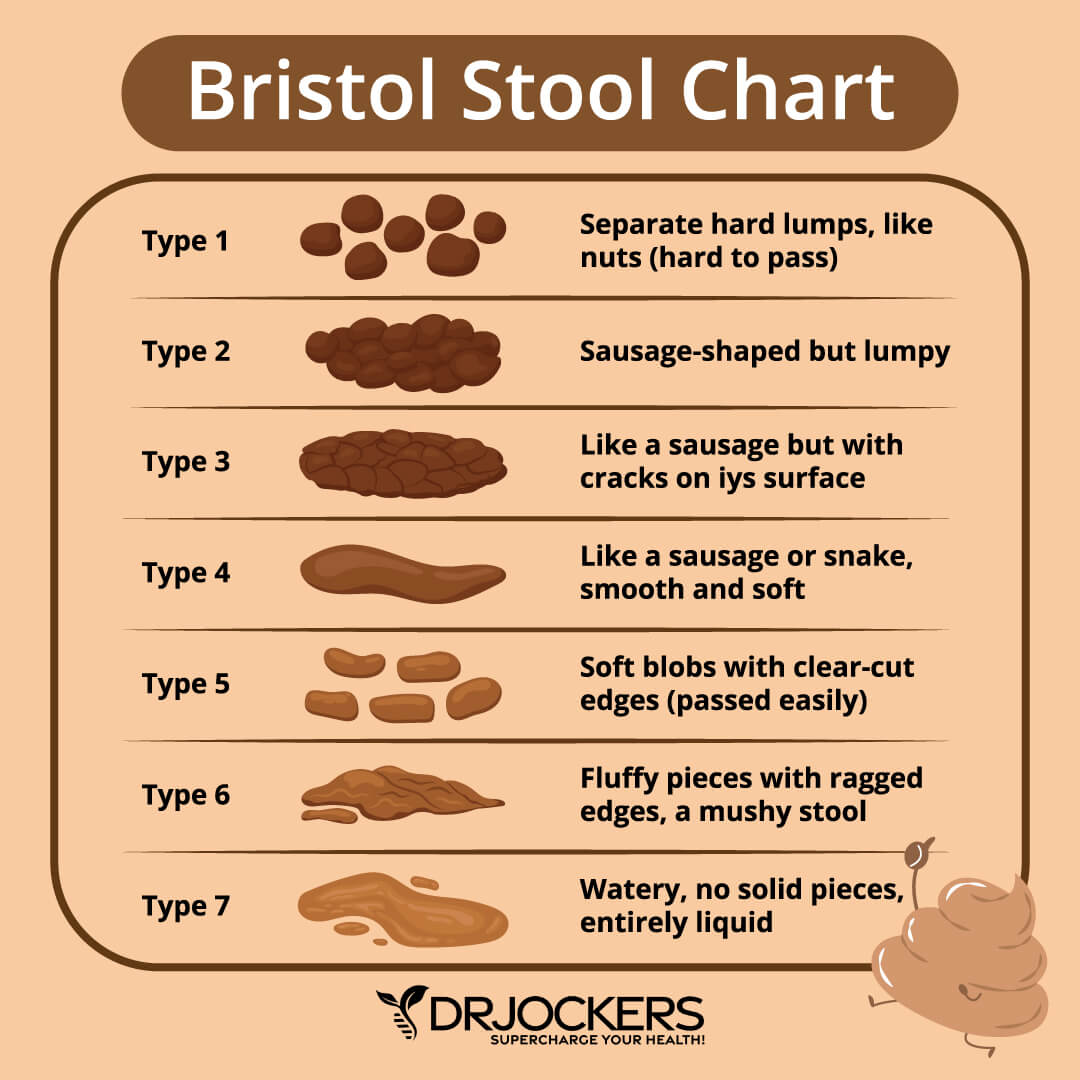
The Bristol Stool Scale is a chart that categorizes human feces into 7 different types based on appearance. A hospital in England created the chart to assess intestinal function in patients. The following is a brief description of each type of poop according to the Bristol Stool scale: (1, 2)
Type 1-2: Associated with Constipation
Type 1: Stool is characterized by hard, separate lumps often difficult to excrete. If you have a pet rabbit perhaps you will understand this comparison.
Type 2: Very lumpy but otherwise formed stool.
Type 3-4: Normal
Type 3: Comparable to a sausage with slight cracks on the surface.
Type 4: The ideal poop; Described as soft, smooth and snake-like in appearance.
Type 5-7: Associated with Diarrhea
Type 5: Soft, separate and easily passed stool.
Type 6: Described as mushy stool with ragged edges attributed by excess liquid.
Type 7: Stool not containing any solids but instead is entirely liquid.
Normal Stool
Normal stool is the result of a healthy digestive system ridding the body of waste. It should be brown in color as a result of bile that has been excreted from the liver to aid in digestion. Normal stool should also not have any visible food products that look the same coming out as they did going in.
If so, you may want to work on slowing down at the dinner table and chewing your food. Try having a conversation while you eat and avoid eating on the run or at times of high stress.
Perhaps you have heard, drink your solids and chew your liquids. The gastrointestinal tract begins at the mouth where enzymes are excreted into the food and prepares the nutrients for absorption and digestion as it continues on track.
Breaking down solids allows your body to receive the optimal nutrition from food. Guzzling down liquids, especially anything other than water prevents any nutrients in the liquid from first mixing with saliva and enzymes in the mouth so that the nutrients are digested appropriately later on.
Abnormal Stool
Abnormal stool can be the first hint from your body that something is not right. Simple factors such as color and consistency can serve as major red flags for doctors to test for medical conditions.
Doctors look for these characteristics to determine if your poop is normal or not and you should do the same.
Red Flag #1: Color
The color of your bowel movements can indicate a variety of different medical ailments. Red, dark or pale green and even black stool should trigger your immediate attention. The following colors of stool can indicate the following issues with your health:
Red: Red indicates blood and may be representative of bleeding along your lower gastrointestinal tract such as the large intestine or rectum and may indicate diverticulitis.
Green: Green is an indication that nutrients were not properly absorbed from the food matter and could be a sign of Crohn’s disease, or gallbladder disease.
Black: Black is a sign of upper gastrointestinal tract bleeding possibly from the stomach or even esophagus. Ulcers, cancer or chronic inflammation from disease may to blame. Sometimes hard to detect the presence of blood in black stool, at home kits are available for initial testing. Otherwise, seeing a doctor for a test and eventually a colonoscopy needs to be a priority. (7)

Red Flag #2: Shape
The two major conditions attributed to the shape of your last poop can indicate if you are experiencing constipation or diarrhea. These conditions may be alarming features that require further investigation if symptoms persist longer than 3 days.
According to the Bristol Stool Scale, constipation is evident by poop that is not continuous because of straining, lack of liquid and excess gas (1). If you have gone to the bathroom fewer than 3 times this week, you are considered constipated by medical standards (2). Diarrhea of course is the opposite and contains excess liquid making it easy to go and hard to hold.
Hazards Associated with Constipation
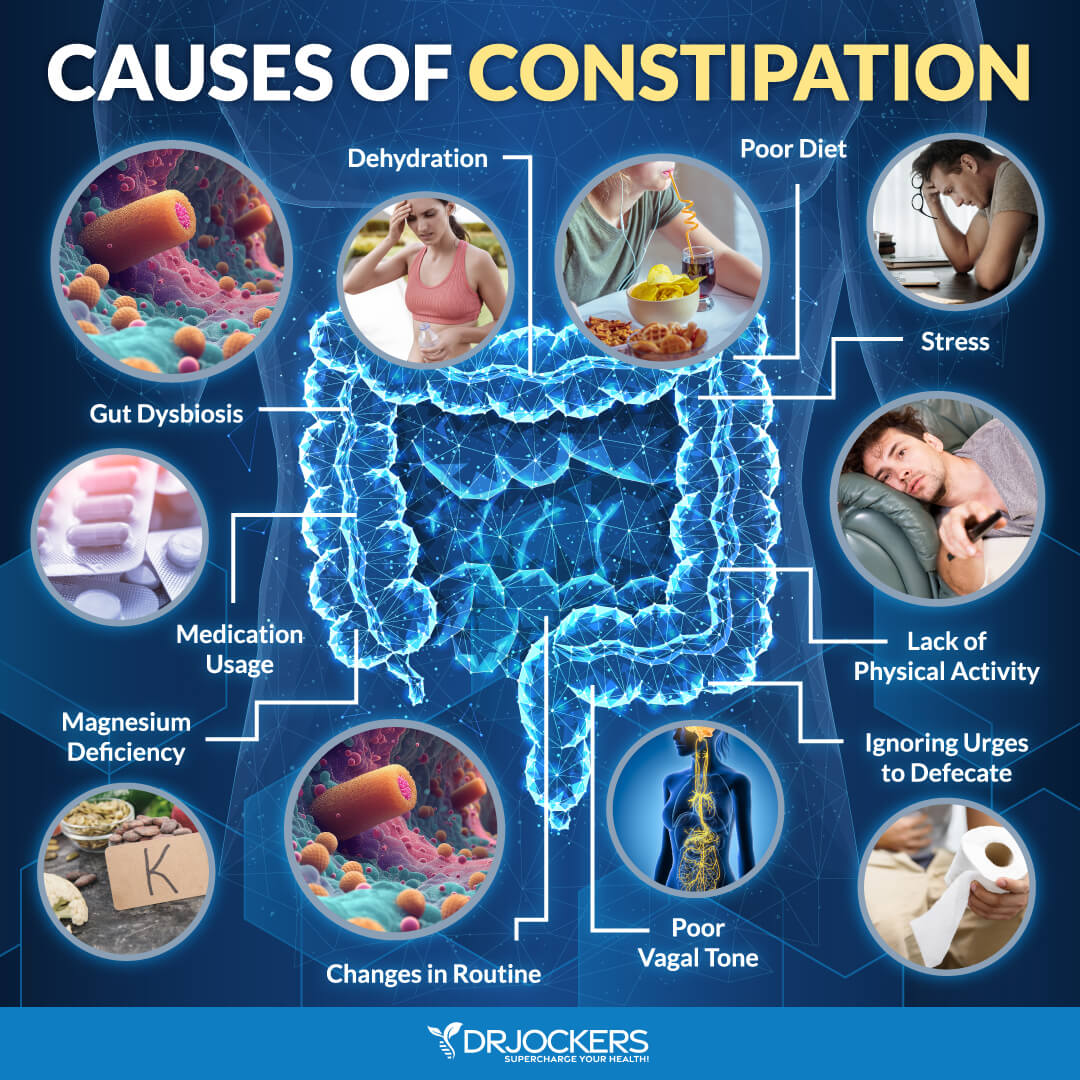
Unfortunately, constipation is a very common problem among the population today. People are consuming less nutritious foods, are over stimulated and stressed, are not maintaining healthy exercise habits and are damaging their entire bodies with highly processed, chemical ridden food from man rather than nature.
Understanding if you have chronic constipation and addressing the concern with your doctor can save you from suffering from a condition or allowing a disease to progress. Individuals over 50 years of age are at increased risk of Crohn’s disease, bowel polyps and ulcerative colitis and are recommended for medical screening (7).

Stress Can Increase Constipation
One of the main triggers of constipation in today’s fast paced world is stress. The gut has been titled as the “second brain” because of its interaction with the brain. The gut influences the same neurotransmitters affected by emotions such as anger and anxiety and has more neurons lining the gut than are contained in the spinal cord (9, 10).
Next time you can’t control your emotions, ask yourself if the stress is worth an ulcer or not.
Stress Creates That “Gut Feeling”
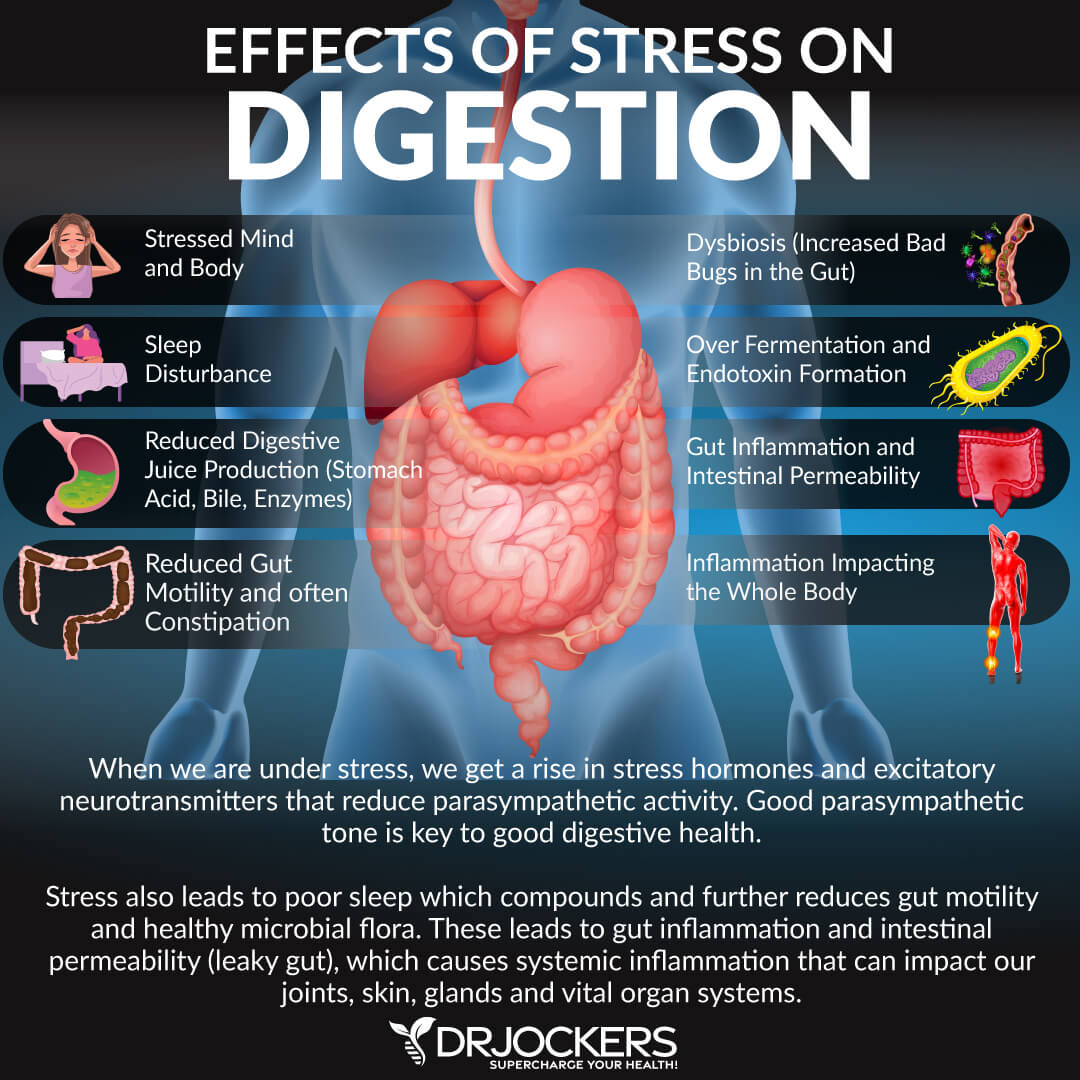
Have you ever been cautious about a certain scenario and you communicated to someone that you “had a gut feeling”? The vagus nerve extends from the brain to your gut and is affected by stress. As a result, histamine, cortisol and other chemicals are secreted by the body stimulating inflammation and weakening the immune system. (9, 10)
Think of a time that you may have been frightened; perhaps at night while sleeping alone somewhere new and you hear a suspicious sound outside your door. Was the first thought that came to mind, I need to poop? Of course not, your body responded with an increased heart rate, dilated pupils and a heightened sense of hearing preparing your body for a fight or flight.
Chronic stress, whether an immediate concern or one only perceived as a potential problem that you just can’t take your mind off of, can result in constipation.
Medications Cause Constipation
If chemicals naturally secreted by the body to defend against stress affect the frequency in which you are able to poop, it should be obvious that medications should have the same consequences. Medicines that are known to cause constipation include antihistamine drugs, antidepressants, chemotherapy drugs and analgesic drugs such as opioids.
These drugs have been found to be the cause of constipation in 90% of cancer patients and up to 40% of non-cancer patients (2).

Conditions Associated with Constipation
Problematic symptoms associated with the formation and movement of stool throughout your body may manifest in a variety of symptoms. Irrelevant of color, the symptom of constipation alone is linked to a variety of conditions and diseases.
1. Colorectal Cancer: Although constipation may simply result from dehydration, if you have a history of colon cancer or inflammatory bowel disease in your family you should get tested.
2. Ulcerative Colitis: Ulcerative colitis is a disease that is strongly associated with the increase in white blood cells in the colon (2, 4). These cells produce inflammation in order to defend the body from infection and trigger a domino effect of health consequences.
Inflammation increases the permeability of the intestine and allows bad bacteria to sneak through holes and cause infection in neighboring organs.
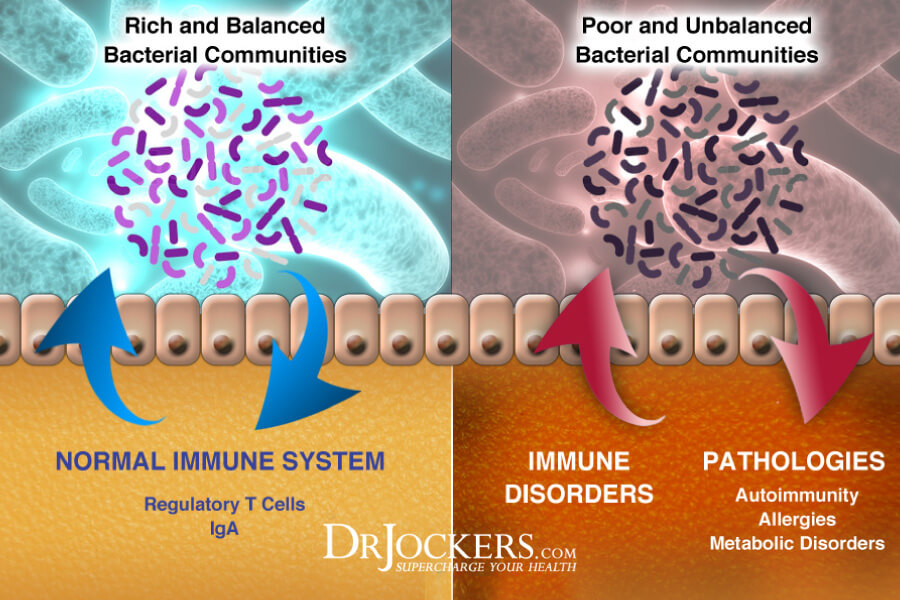
3. Constipation Dominant IBS:
Irritable bowel syndrome is the most frequently diagnosed gastrointestinal disorder affecting an estimated 90 million people worldwide (6). IBS results from a change in the movement of gas through the intestines leading to abdominal pain, constipation or diarrhea. Researchers are learning that these patients have a problem with their guts, possibly a result of the mind-gut connection. (4)
Scientists have noticed a significant difference in how the brain responds to anxiety and fear in individuals with IBS. The link between the brain and the gut is therefore partially responsible for the secretion, absorption and motility of poop through the intestines.
Another cause of IBS may be a result of decreased healthy bacteria such as lactobacilli and bifidobacteria. These two kinds of bacteria compete with pathogens to take up space and do not stimulate gas production. Studies have found that IBS patients have decreased activity of these bacteria in the colon. (4)
IBS is also related to SIBO or small intestinal bacterial overgrowth. This is where there is an overgrowth of bacteria in the small intestine. SIBO damages the intestinal lining and creates a state of mild-severe leaky gut syndrome and resulting food allergies, sensitivities and chronic inflammatory processes (2). The malnutrition and inflammation this causes can lead to bouts of diarrhea and constipation.
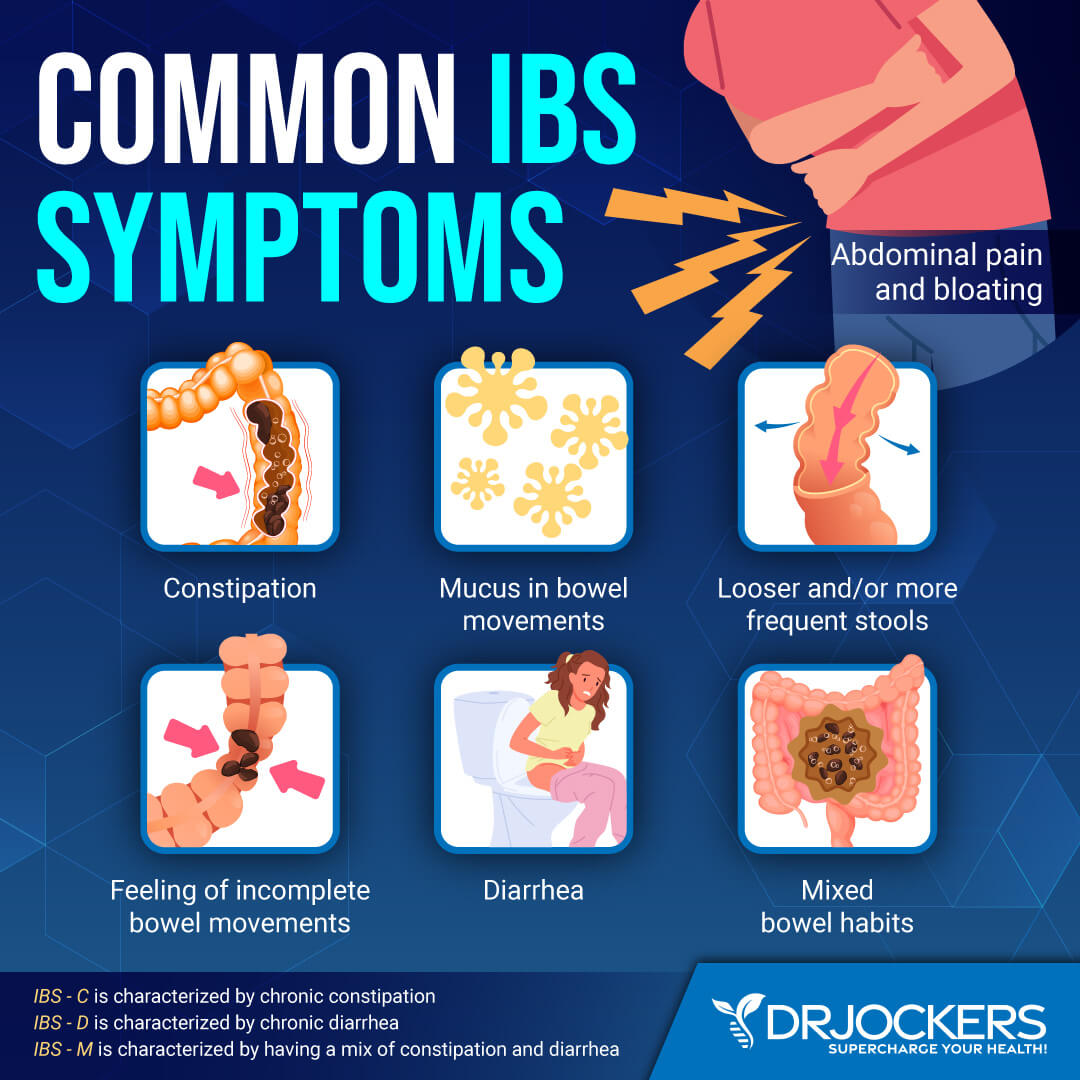
4. Psychological Stressors: Constipation is frequently problematic in people suffering from depression, anxiety, and eating disorders. Again, the mind is so intrinsically designed and effective at prioritizing life’s demands that at times it might seem like it can work against us.
5. Neurological Problems: Especially in people over 50 years of age, constipation can be a cause for concern because of the effects that nerves play in connection to the gut. A long term change in your bowel habits may be an indication of dementia, muscular dystrophy, stroke or Parkinson’s disease (2).
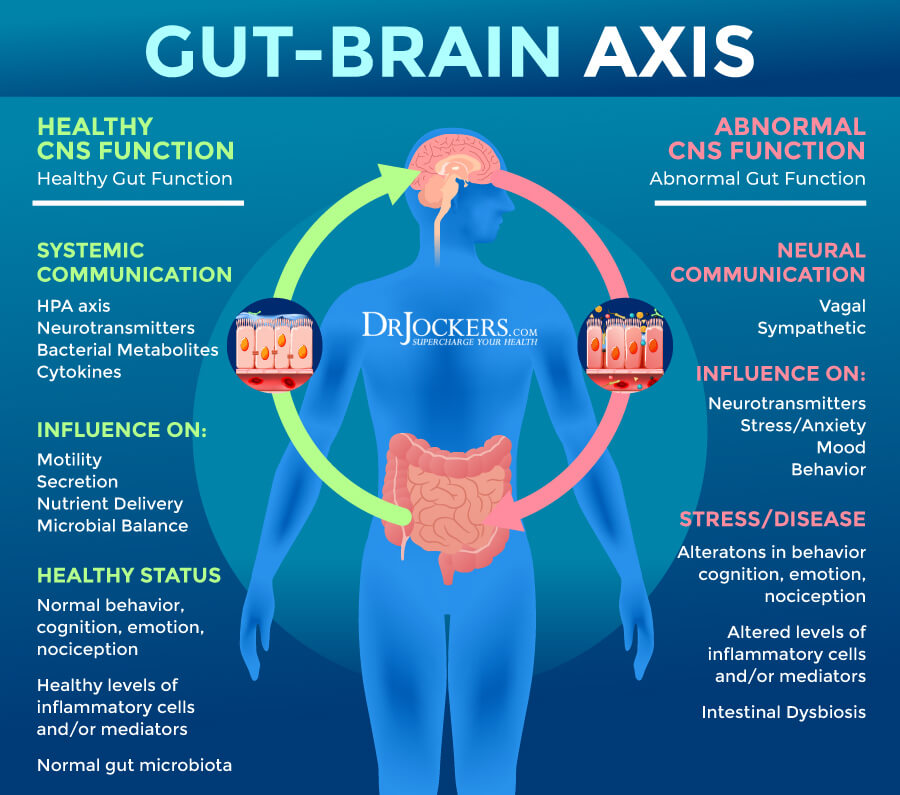
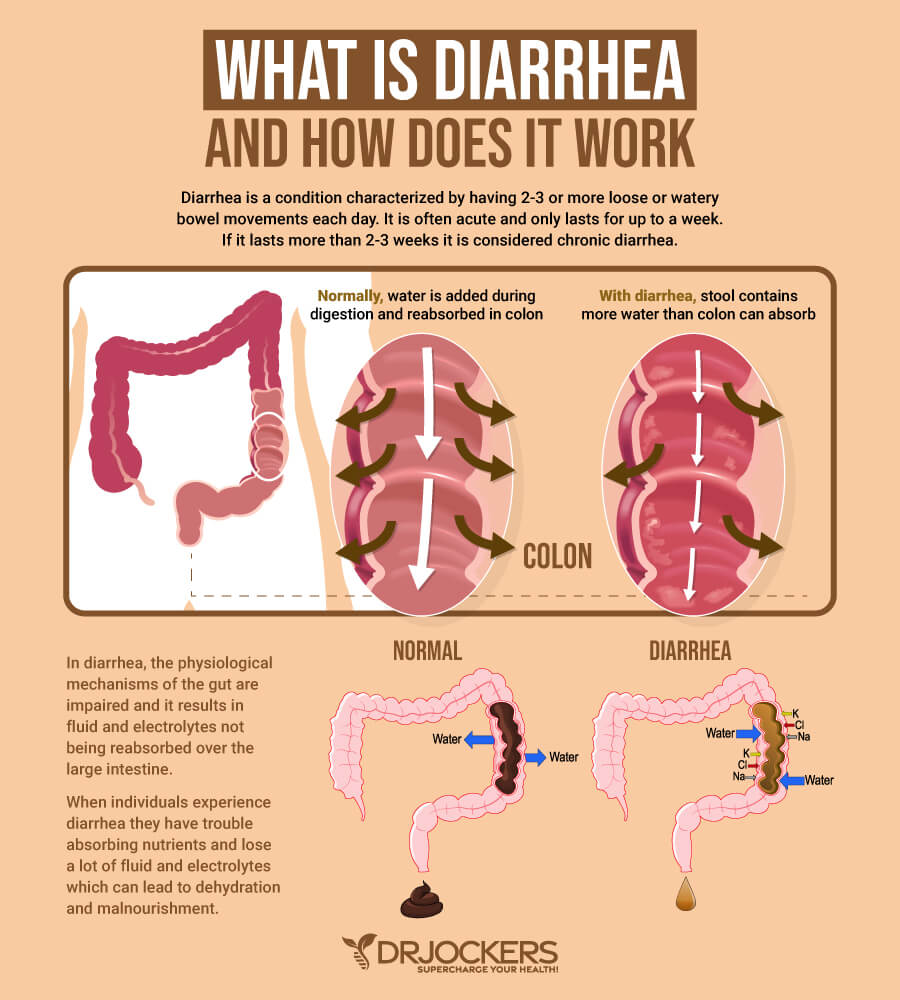
Conditions Associated with Diarrhea
Although constipation may seem like a more dominant problem, diarrhea can also be a sign of declining health. Despite the frequency of bowel movements, diarrhea is associated with 3 of the 7 types of poop according to the Bristol Stool Scale. Individuals suffering from diarrhea typically have an infection due to bacteria overgrowth (1).
1. Infection: The microbiota, or gut environment, needs to be a priority for maintaining a healthy bowel regimen. The colon can contain upwards of 500 to 1,000 different bacterial species influenced by diet, environment, age and antibiotics. An overgrowth of bad bacteria and viruses can lead to a gut infection and resulting diarrhea.
Healthy bacteria in the gut can relieve symptoms associated with diarrhea and prevent the body from infectious agents such as harmful bacteria (6, 11).
2. Bile Acid Malabsorption: Researchers recognize that diarrhea may be an underappreciated symptom of bile acid malabsorption. Bile acid is produced by the liver to help absorb lipids in the small intestine. Diarrhea can therefore be a signal from your body that a greater problem exists.
Disorders may include Crohn’s disease, Celiac disease (gluten intolerance), liver cancer or pancreatitis. (5, 6)
3. Diarrhea Dominant IBS: Diarrhea is also associated with IBS symptoms. If diarrhea is a persistent problem, IBS may be to blame (3). Weight loss might be another side effect that results in individuals who have diarrhea dominant IBS.
16 Ways to Achieve a Healthy Poop
You may snicker at the concept that there is actually a way to maintain regularity and achieve a healthy poop, but it is essential not only to promoting a healthy gastrointestinal tract but also to achieving optimal health and vitality. If increased energy and happiness is what you desire, set all awkwardness aside and prioritize your goal to achieve a healthier poop.
In time you may learn how to develop a healthy stress management response by removing stressors in your life or by calming your mind through the practice of meditation. In the meantime, the following tips can help you achieve success by making a few changes in your lifestyle now.

1. Cop a Squat: Don’t just cop a squat as you might do in a public restroom but squat to poop. You’re right; there is a right way and a wrong way to sit on the toilet. After all, our ancient ancestors likely found themselves digging holes and squatting to poop and you should be doing the same.
Placing your feet on a stool or trash can and leaning forward relieves the tension from your intestines and allows you to eliminate waste with greater ease. (8)

2. Hydrate: Are you nourishing your body with a healthy intake of water daily? Or perhaps you are excessively consuming caffeinated or sugary beverages. Increase your daily consumption of water and decrease drinks that may be adversely affecting your health. Be sure you are drinking at least half your body weight in ounces.
In the summertime, I recommend three quarters of your body weight in ounces. Drink 8-24oz of clean water first thing in the morning (and give yourself 30 minutes to an hour before eating) to help induce gut motility and healthy bowel activity. The morning is the most active time for your colon and the best time to eliminate waste.

3. Salt Water: The salt-water flush has been used for centuries to improve bowel motility. Simple take a 1 tsp of salt in 2-4 oz of water and swallow it down. Follow this up with 8-16oz of water. The salt helps to flush the colon so be sure you have some time over the next 1-2 hours to spend in the bathroom.
4. Avoid Processed Foods and Alcohol: Having to wipe too many times may be a consequence of too much mucus in your colon. Eliminate or reduce manufactured and highly processed foods and alcohol from your diet. I would also advise to stay away from gluten, pasteurized dairy, soy, corn and peanuts. Follow an anti-inflammatory nutrition plan here
5. Medication Intervention: Medications affect gut health and produce common side effects such as constipation and diarrhea. Open up the conversation with your prescribing physician and discuss if pharmaceutical drugs are causing you more harm than good.
6. Increase Healthy Gut Bacteria: The microbiome and activity of bacteria in the gut changes daily (5). Introduce healthy bacteria into your diet by taking a daily probiotic and consuming fermented foods such as saurkraut, kimchii, coconut yogurt and coconut water kefir.
Probiotics increase intestinal health and protect against inflammation, increased permeability apparent in those with leaky gut syndrome and hypersensitivity concerns in patients with IBS and psychological disturbances (4).
7. Avoid Food Allergens and Sensitivities: You may already be aware if specific foods such as cabbage, wheat, dairy or smoked meat products increase abdominal discomfort and change the frequency or urge to poop (4). Test for and avoid food sensitivities using a biofeedback test or specific blood test.

8. Play Around with Fiber Content: Fiber can be found in a supplement source typically containing psyllium, but it is best to receive the benefits from fiber from nature. Increase the amount and variety of fruits and vegetables into your diet. Individuals consuming plant based diets have been studied to have fewer carcinogens in their microbiome than those who primarily consume meat (5). (2)
Some individuals do well with more fiber, while others need less. Experiment to find out which camp you are in when it comes to fiber.
9. Decrease Reliance on Laxatives: Although traditional laxatives may be the first offensive move to treat constipation, laxatives have not significantly proven beneficial at relieving pain and may aggravate the problem. Instead of relying on a laxative in pill form, try a more natural approach by drinking apple, pear or prune juice (2). (4)
One supplement I use that works amazingly well and is non-addictive forming is Oxy Powder. People notice that this is very gentle on their system, and it really works!!! I would be sure to have some of this on hand and use it as needed.
10. Don’t Hold It In: You may be taken back by the necessity to poop in a public bathroom, but at times this is a must. Holding it in allows water and nutrients to be reabsorbed back into the body. Poop is waste and if the urge presents itself, do not hesitate to go.
11. Supplement Magnesium Into your Diet: Magnesium can stimulate the movement of stool through the bowels by serving as a muscle relaxant (8). Magnesium is easily depleted under chronic stress but can be replenished in our food supply. Excellent food sources of magnesium include green leafy vegetables, nuts, seeds and some fruits such a bananas and apples.

12. Exercise: Increasing physical activity has provided significant health benefits both physically and emotionally. Inducing a cardiorespiratory fitness response increases oxygen consumption in the body.
Exercise has been studied to decrease the frequency of pain, regulate bowel movements, combat fatigue, decrease cortisol and alleviate symptoms of depression and anxiety (3).
13. Proper Testing for SIBO or Candida: Unhealthy stools are a red flag sign of microbial dysbiosis. This is often due to small intestinal bacterial overgrowth or Candida. Read up on these health problems and get the proper testing, diagnosis and treatment to heal your gut. For more info on gut dysbiosis read this article.
14. Carminitive Herbs: Carminatives are herbs that stimulate the digestive system to work better. These herbs contain a high content of volatile oils that are effective at expelling gas, reducing bloating and easing griping pains from the stomach and intestines.
They also tone the mucous surfaces & increase peristaltic action within the esophagus, stomach. This peristaltic action propels food and wastes through the system. The major carminative herbs include coriander, cinnamon, ginger, juniper, anise, fennel, cloves, caraway, dill, peppermint, thyme and licorice.
These carminatives are often combined with aloe. Aloe is a cathartic herb that increases intestinal transit time and is used to alleviate constipation. These herbs help to tone down the powerful gripping effect that aloe often promotes in the gut. This combination helps stimulate effective and comfortable stools for those with chronic constipation.

15. Smooth Move Tea: Used for thousands of years to get your “movement” moving again, senna works by gently stimulating your intestines and aiding your body’s natural elimination process. This tea combines senna the carminitive herbs fennel, coriander and ginger to reduce the potential for unpleasant feelings like cramping. Smooth Move tea is best taken at bedtime to help improve bowel movements the following morning.
16. Gut Repair Supplement: This supplement combines aloe vera along with the carminative support of deglycyrrhizinated licorice extract. It also contains L-glutamine which helps to form good healthy stools and a powerful prebiotic fiber in arbinogalactan.
Arbinoglactan minimizes ammonia synthesis and absorption, enhances production of short chain fatty acids and increases the gut microflora population. It is one of the best fiber sources for healthy bowel movements. I use this supplement for clients with leaky gut syndrome, irritable bowel syndrome and for diarrhea and constipation issues.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!








The presentation was very helpful. It provided valuable information about a serious digestive problem, but was done in a comical way. It cracked me up!!! As I kept reading, I couldn’t stop laughing, but I absorbed all the material, pictures included. Now I have a mental image of elimination which doesn’t cause me stress when I think about it. First problem solved. Manage stress better for good elimination. Thank you for the information.
Thanks for reading Allen! Glad this information was able to “stimulate a movement” in your stress patterns!
Great info thank you!
My daughter is 6 and has never pooped brown. It is always green/yellow/colour of the food she ate and it is alway soft and stinky.
She had her liver tested and results came back fine.
Another dr recently did celiac test and receptionist said it looked fine 1 or negative or something.
She is 20lb over bmi.
She poops at least once a day. She gets cramps everyday.
She has a adult tooth that came in that has no enamel and you can see the yellow Dentin in it. And she is also missing 4 adult molars.
Im trying to look out for her future to prevent any further damage, especially as colon cancer does run on one side of our family.
Which direction should I be headed with this?
Any advice would be so greatly appreciated!
please delete my comment if it was not appropriate and does not warrant a response
Hey Kelly, I would recommend finding a functional medicine doctor near you and having some comprehensive testing done!
Smooth Move is not safe, and not sure why you recommend it. It has Senna which ruins the gut and causes a dependency.
hi, my stools in the beginning are hard lumps somewhat slippery but I struggle, then the last of it is like toothpaste, not watery but no shape at all, and I always have some leftover of that inside and when im walking that leftover slips out, it’s terrible because I cant go outside. what can be causing this problem ? im not on medications. thanks.
Sorry to hear this! I typically see food sensitivities, inadequate enzymes and gut infections as the primary causes here. This is a good article: https://drjockers.com/7-ways-reduce-food-sensitivities/
Your information awake me. Now I know our nature has given everything to survive and cure ourselves but we the so called educated people are eating pizza burgger, hot dog, KFC chicken and making our digestive system hell. It’s Very important to know the value of natural foods and ingredients Which God made for us.
Thanks a lot. And Love from India.
Yes for sure Bablu! Blessings!
Sir, I’m suffering from constipation from a very long time and then from piles also it’s Always comes for a few days and my poop is somewhat in sticky with hard pebbles and it’s like very stinky and dark brown in color I am using white husk for fibre but still it comes back please help me and suggest me what should I do am very tensed about it m just 21
Hi Priya, I don’t recommend the use of psyllium husk. Instead, Oxy Powder can help move bowels: https://store.drjockers.com/products/oxy-powder
Your site is truly excellent. The best. Wish I had had access to all this info when I was young.
Thank you for all your articles.
Thank you for the encouraging feedback Joy! Blessings to you!
Dr…
Why wen I get excited or scared do I smell like straight poop, sewer.. Trash.. Ect! N I have had poop that floats.. Smells insanely awful…
Sorry to hear this! Sounds like you have a sympathetic stress release and you have poor fat digestion if you poops smell that bad and float. Here is a helpful article to improve your bile flow. https://drjockers.com/bile-liver-gallbladder/
Where is the instructions for the 7 day liver cleanse?
Here you go Lori https://drjockers.com/liver-cleanse/
Hi, I am doing a health, nutrition, and safety board for my early childhood development class. I am doing it on gut health. Can I use some information from this page for my project? I will cite you as my resource of course. Thank you.
Yes you can Jamie!
Dr. Jockers, I finished chemo 2/2021. immunotherapy 11/2022. Radiation=7/2023.
My poop is still black, has not changed. When is this going to change?
I eat protein, veggies, salads. NO beef NO carbs.
I may go daily or every other day!
Magnesium citrate may help or not at times.
At times I still feel the chemo chemicals are def still inside my body. I have to rinse with water after using the bathroom or I get severely itchy then my skin burns.
Sorry to hear about this! I would advise working with a functional nutrition practitioner to help you get this figured out. Our team works with people all over the world and customizes plans for them: https://drjockers.lpages.co/long-distance-coaching-dr-jockers/