
Suffering From Histamine Intolerance?
As a clinician, it is imperative that I understand all the different types of unique health problems and metabolic challenges. On a biochemical level, what may be a superfood for one individual may be poison to another. Histamine intolerance is an area where this is the case.
People who are unable to effectively metabolize histamines must restrict their consumption of many foods that I typically recommend on a regular basis. If you have a histamine intolerance, consuming histamine-rich foods can lead to chronic health issues such as allergies, asthma, sinus problems, eczema, chronic pain, menstrual problems, and much more (1).
The Unique Nature of a Histamine Intolerance
I always wondered about what was happening with individuals who told me they were “allergic to the sun.” Interesting research indicates this is a histamine response, as UV light can trigger histamine release (2).
Other research indicates that those susceptible may have problems with high-intensity exercise, especially done in a warm environment (3). Individuals with periods of high estrogen may have higher than normal histamine responses, and high stress increases histamine levels and decreases the body’s ability to metabolize the histamine (4, 5).

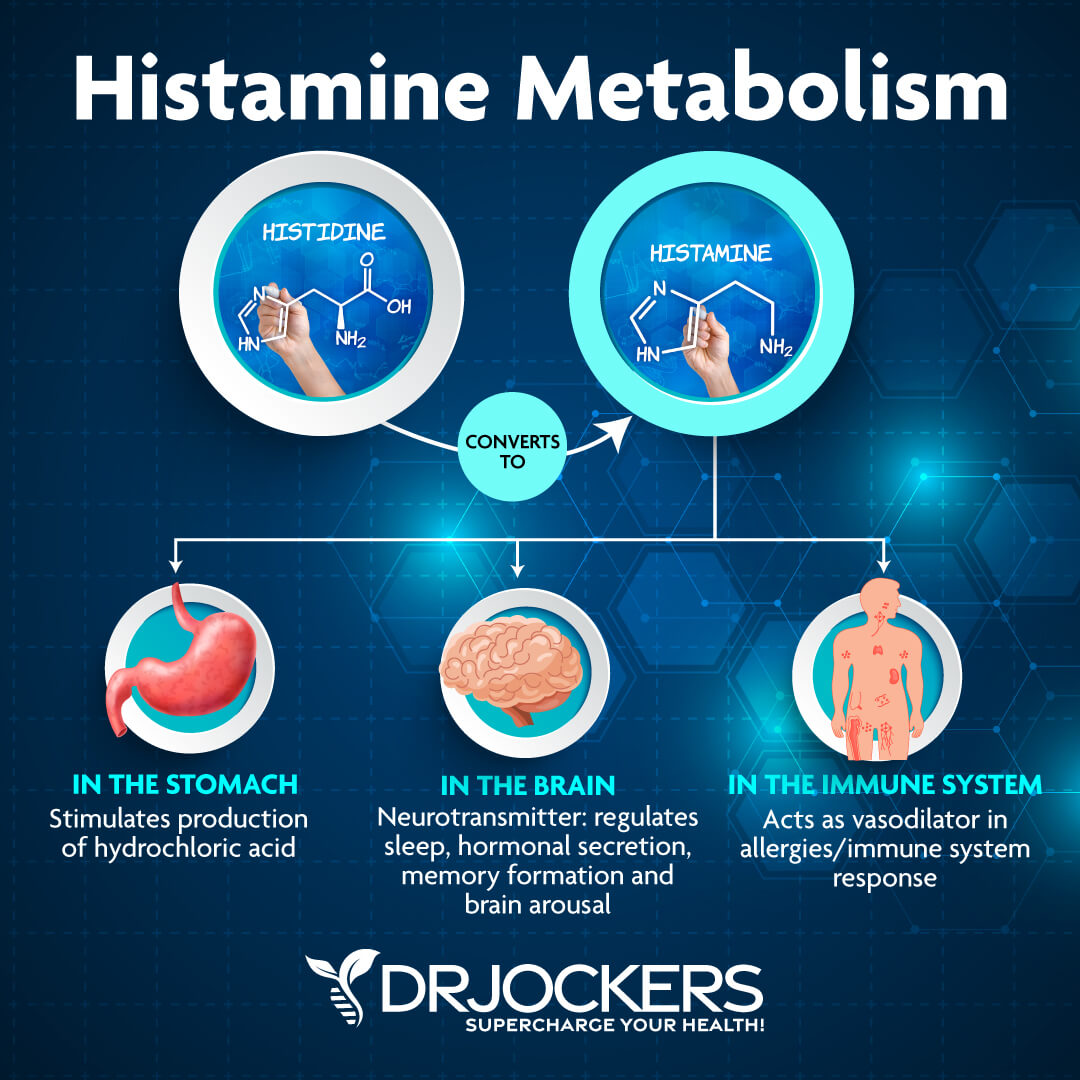
What is Histamine?
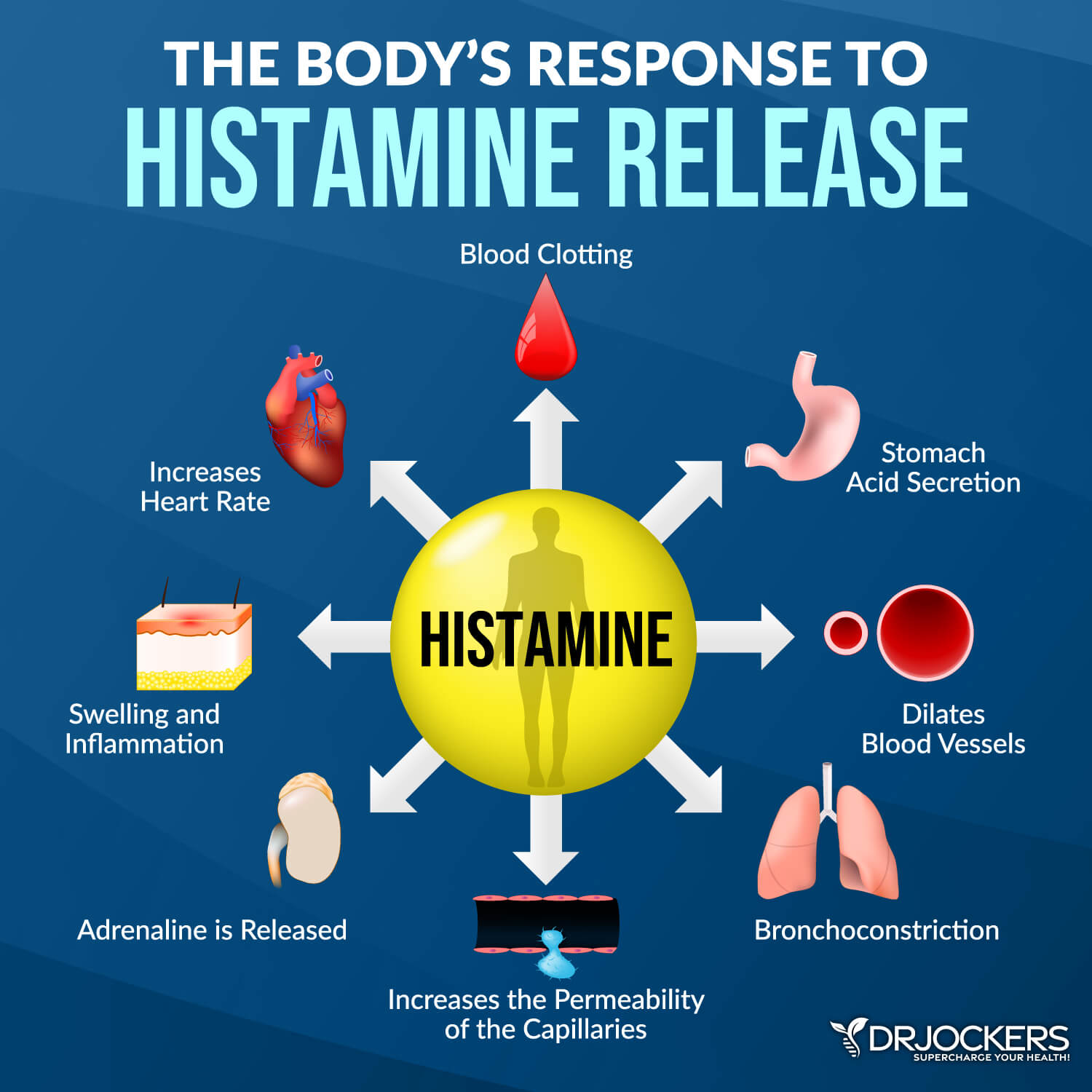
Histamine is an important neurotransmitter and immune messenger molecule. It is involved in processes involving hydrochloric acid secretion for digestion, triaging water reserves to key areas of the body, and the inflammatory response. Histamine receptors are located all over the body and have many important functions, including:
- Histamine H1 receptors: Smooth muscle and endothelial cells affecting skin; blood vessels (Benadryl and Claritin block activity of these receptors)
- Histamine H2 receptors: Cells in the intestines control acid secretion, abdominal pain, and nausea; heart rate
- Histamine H3 receptors: Central nervous system controls nerves, sleep, appetite, and behavior.
- Histamine H4 receptors: Thymus, small intestine, spleen, colon, bone marrow, and white blood cells; inflammatory response
One of the major effects of histamine is causing the blood vessels to swell and dilate. When the body senses that it is threatened, it will secrete higher amounts of histamine. This allows the white blood cells to quickly move through the bloodstream and find the potential threat or infection. This is an important component of a healthy immune response.
When Does Histamine Become a Problem?
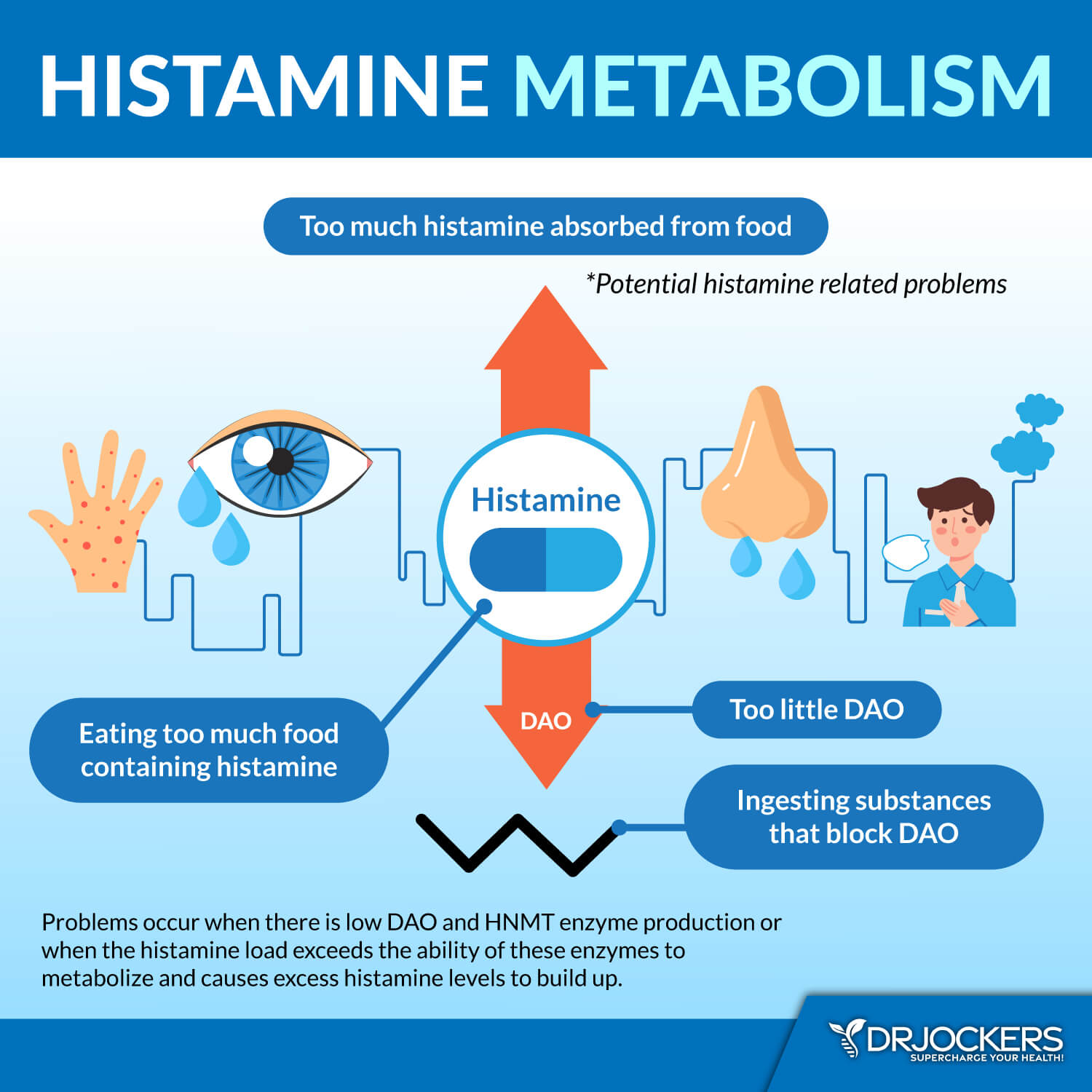
Histamine only becomes a problem when we have metabolic disturbances that do not allow us to effectively metabolize histamine properly. When histamine is formed, it is broken down by specific enzymes. In the central nervous system, it is metabolized by histamine N-methyltransferase (HMT), while in the digestive tract, it is broken down by diamine oxidase (DAO).
The experts state that DAO is the major enzyme involved in histamine metabolism (6). The enzyme converts the histamine into imidazole acetaldehyde, which does not trigger any sort of reaction in the body. DAO is responsible for ensuring a steady histamine level required for the balance of numerous chemical reactions taking place in the body.

Altered DAO Enzyme Production:
Some individuals have altered DAO production due to a number of different factors, including (7):
Small Intestinal Bacterial Overgrowth (SIBO) – some gut microbes produce high amounts of histamines as a byproduct of their metabolism.
Copper, Vit C & B6 Deficiency: Copper and Vit C are crucial components of the DAO enzyme, and B6 is a key cofactor that enables DAO to degrade histamine.
Leaky Gut Syndrome: Intestinal permeability creates major inflammatory stress in the body, which can contribute to poor DAO function.
Genetic Polymorphisms in DAO enzyme – this can be seen on the 23andme SNP’s. A homozygous DAO would make someone more susceptible to developing a histamine intolerance.
Use of Certain Medications:
- Non-steroidal anti-inflammatory drugs (ibuprofen, aspirin)
- Antidepressants (Cymbalta, Effexor, Prozac, Zoloft)
- Immune modulators (Humira, Enbrel, Plaquenil)
- Antiarrhythmics (propranolol, metoprolol, Cardizem, Norvasc)
- Antihistamines (Allegra, Zyrtec, Benadryl)
- Histamine (H2) blockers (Tagamet, Pepcid, Zantac)
According to expert Dr. Amy Myers, MD, “histamine blockers, a class of acid-reducing drugs, seem like they would help prevent histamine intolerance; these medications can actually deplete DAO levels in your body” (8).
According to Chris Kresser L.AC, “Histamine is different than typical food sensitivities or allergens in that it is a cumulative problem” (9). So, we begin to have symptoms when we either take in too many histamine molecules or we reduce the DAO enzyme to the point where the histamines overload the system. These symptoms will last until the body metabolizes the histamines and removes them from the system.
Who Has Histamine Intolerance:
According to available research, histamine intolerance manifests in approximately 3% of the population (9). In up to 20% of these cases, the symptoms occur mostly when histamine containing foods are used in combination with DAO inhibitors such as alcohol. Approximately 80% of individuals with histamine intolerance are women, and most of them are over 40 (10).
The three biggest factors involved with histamine intolerance include leaky gut syndrome or related disorders such as Crohn’s disease, Irritable bowel, celiac, gluten sensitivity, etc. (11). The second factor is a genetic polymorphism with the DAO enzyme. Heavy alcohol and/or medication usage is another strong risk factor.

Diagnosing Histamine Intolerance:
This is a challenging condition to diagnose for a number of reasons. The first is that there are so many popular foods, many of which are considered healthy foods that are high in histamines. Also, some individuals have a unique gut flora that is producing high histamine levels.
Most doctors are not familiar with histamine intolerance and never consider this as a contributing factor in the individual’s health challenges. In fact, many physicians, including myself, typically recommend a diet high in histamine-containing foods. This includes fermented foods, which have incredible health benefits for those with adequate histamine metabolism.
Research has shown that people react quite differently to elevated histamine, making it that much harder to pinpoint (12). As a clinician, I have learned that when individuals react very poorly to fermented foods, it is a sign of histamine intolerance.
Most people respond very well to small amounts and gradually increasing levels of fermented foods. Individuals with histamine intolerance often break out with hives, eczema, rashes, puffy eyes, headaches, etc.
Symptoms and response to high histamine foods can be adequate for diagnosis, but the gold standard is the Histamine Testing blood work that I describe below. Be sure to check that out.

Common Symptoms of Histamine Intolerance
- Headaches/Migraines
- Difficulty falling asleep, easily arousal.
- Hypertension
- Vertigo or Dizziness
- Arrhythmia, or accelerated heart rate
- Difficulty regulating body temperature.
- Anxiety
- Nausea, Vomiting
- Abdominal cramps
- Flushing
- Nasal Congestion, Sneezing, Difficulty Breathing
- Abnormal Menstrual Cycle
- Hives
- Fatigue
- Tissue swelling
Histamines travel throughout the bloodstream and therefore can affect the gut, lungs, skin, brain, and entire cardiovascular system. This is why there is such a wide array of health problems associated with it, and it is quite challenging to pinpoint and diagnose if you are not aware of the condition (13, 14).

Testing For Histamine Intolerance:
The 23andme genetic test will look at genes associated with DAO enzyme production. When an individual has a homozygous mutation, they will most likely struggle with histamine metabolism. This may not occur until after a stressful season of their life when their gut barrier breaks down, and their adrenal glands are unable to keep up with the demands placed upon them. This creates a vicious cycle of chronic inflammation and inflammatory stress that depletes the body of vital reserves and exposes the genetic weaknesses of the individual.
There are lab tests that can be done that analyze the ratio of histamine/DAO enzymes. A high histamine/DAO ratio indicates that one is ingesting too much histamine and is not producing enough DAO to effectively metabolize it. Here is the lab test my team uses on a regular basis and if you want to have one of my functional health coaches analyze your test, then simply order it from our site.
The Histamine Challenge Test
Without getting the blood test, you could do a histamine challenge by consuming a number of different fermented foods and high histamine foods, and see if this aggravates your symptoms. If so, try a low-histamine diet for a week, and if you notice significant improvements, you most likely have histamine intolerance.
To improve your tolerance to histamine, it is critical to heal the gut and address the dysbiosis issues that are at the root of the problem. I would recommend working with a qualified health practitioner to assess and create a specific plan to address the bacterial imbalance.
Foods High in Histamines (15):
Some foods naturally have more histamine content, while others accumulate histamines as they age. Fermented and dried foods typically have the highest levels of histamines. A low histamine diet must be focused around getting foods at their peak level of freshness. Here is a list of high-histamine foods:
- Fermented alcoholic beverages, especially wine, champagne, and beer.
- Fermented foods: sauerkraut, vinegar, soy sauce, kefir, yogurt, kombucha, etc.
- Vinegar-containing foods: pickles, mayonnaise, olives
- Cured meats: bacon, salami, pepperoni, luncheon meats, and hot dogs.
- Soured foods: sour cream, sour milk, buttermilk, soured bread, etc.
- Dried fruit: apricots, prunes, dates, figs, raisins
- Most citrus fruits
- Aged cheese, including goat cheese.
- Nuts: walnuts, cashews, and peanuts
- Vegetables: avocados, eggplant, spinach, and tomatoes
- Smoked fish and certain species of fish: mackerel, mahi-mahi, tuna, anchovies, sardines
- Processed foods of all types – Preservatives are high in histamines.

Histamine-Releasing Foods (16):
These foods do not necessarily contain histamine, but they block the action of DOA, and therefore, they potentiate the effects of elevated histamines.
- Alcohol
- Bananas
- Chocolate
- Cow’s Milk
- Nuts
- Papaya
- Pineapple
- Shellfish
- Strawberries
- Tomatoes
- Wheat Germ
- Many artificial preservatives and dyes

DAO-Blocking Foods (17):
- Alcohol
- Energy drinks
- Black tea
- Mate tea
- Green tea
Low Histamine Foods (18):
- Freshly Cooked Meat & Poultry (frozen or fresh)
- Freshly Caught Fish
- EV Olive Oil
- Pasture-Raised Eggs
- Gluten-Free Grains: brown rice & quinoa
- Fresh Fruits: Other than citrus, avocado, tomato, pineapple, bananas, and strawberries
- Fresh Vegetables (except spinach and eggplant)
- Coconut milk, Rice milk, Hemp milk, Almond milk
- Coconut oil & Grass-fed Butter/Ghee
- Organic coffee
- Almond butter
- Leafy herbs
- Herbal teas

Unique Variables with Histamine:
People with histamine intolerance react in a multitude of different ways. (19) Some people cannot handle any high histamine foods, while others can handle certain types but not others.
As an example, an individual may tolerate avocados, berries, and lemons quite well but have significant reactions to any sort of fermented foods or wine. You will have to find the unique ways that you react and understand what triggers reactions and what doesn’t.
Over time, as histamine content is reduced and the individual improves their gut health, reduces inflammation, improves liver function, and stabilizes their adrenals, they will be able to handle more of the histamines. For some, this will mean they will be able to incorporate small amounts of all the higher histamine foods. For others, they will only be able to handle certain foods, while others will continue to trigger reactions.

What This Means to You:
If you struggle with the major symptoms listed above when you have various high histamine foods, you may have this problem. In particular, if you struggle with fermented foods and probiotic supplements, that is a classic sign of histamine intolerance.
Chances are, you do not have this problem, but you may come across a friend or a client (for those of you who are health coaches and doctors) who will have these signs and symptoms. If so, have them try a low-histamine diet for a week and see if it makes a difference. If so, then continue on the diet and work with a functional medicine practitioner to support the gut and detoxification systems.
If you are suffering from an acute histamine reaction, taking 2 caps of Allergy Defense every hour and taking DAO enzymes (I created a custom DAO enzyme product called Hista Protect) can help to reduce the effects of this.
A diet rich in the flavonoid luteolin has been shown to reduce mast cell activation. This is found in carrots, bell peppers, thyme, rosemary, peppermint, oregano, romaine lettuce, artichoke, pomegranate, rooibus tea, buckwheat sprouts, and cucumbers, among other things.
Consider Using Immunoglobulins
Finally, I recommend using some immunoglobulins. Immunoglobulins, commonly known as antibodies, are specialized proteins produced by the immune system. They are designed to identify and neutralize foreign invaders like bacteria, viruses, and toxins.
They are a critical part of the adaptive immune response. They allow the body to recognize and remember pathogens. Immunoglobulins are produced by B cells and plasma cells in response to the presence of antigens.
A 2024 article published in Nutrients found that serum-derived bovine immunoglobulin may help to reduce inflammation and improve gut barrier integrity (20). Using immunoglobulins may help to improve butyric acid levels by allowing the gut to neutralize pathogens and decrease gut inflammation more effectively.
IgA is an immunoglobulin that may be great for improving mucosal immunity, creating a balanced gut microbiome, reducing gut inflammation, and supporting gut health. Taking immunoglobulins will help reduce the histamine response and improve immune balance.

Consider Using Supplemental Butyrate
You may also want to consider using supplemental butyrate. Oral butyrate supplements can be absorbed by your small intestine and also enter your bloodstream.
They may offer anti-inflammatory benefits. However, since your small intestine doesn’t use butyrate well, the benefits may be more apparent in the large intestine versus the small one. By being absorbed in the bloodstream, it can offer anti-inflammatory benefits to various organs.
Still, the best way to benefit from butyric acid is from your microbiome, which makes it in your large intestine. Supplementation is an extra step that doesn’t replace the recommendation I just shared earlier to help your body make more butyric acid.

Introducing Tributyrn-X
I recommend using Tributryn-X. If you need support for a dysfunctional immune system, leaky gut, chronic inflammation in the digestive tract, food sensitivities, bloating, or digestive discomfort, then your body deserves to try this supplement. It’s the most advanced formula on the market. It’s great for gut health.
Many clinicians we know use around 1,500 mg a day. And in certain cases, higher amounts than that. However, EVERYONE should start slowly with one capsule a day, 500mg, as each person’s gut integrity, motility, and microbiome are different.
Each person’s effective dose can also be influenced by alcohol consumption, tobacco consumption, fat mass levels, speed of digestion (too fast might need more, too slow might need less), and other variables. This means you start with 1 soft gel a day and may take 1-3 gel capsules per day of Tributyrin-X or more as directed by your health provider.
Introducing Mega IgG
I also recommend using Mega IgG. Immunoglobulin G (IgG) is the most abundant antibody in the system and can be found in blood and extracellular fluid, allowing it to control infections in the body. IgG antibodies can bind a variety of pathogens, including bacteria, viruses, and fungi, as well as their toxic by-products.
Binding these toxins will neutralize them and allow the immune system to safely remove them from the body. This supplement may help to maintain the gut barrier function and can also support your H. pylori protocol. It helps support the H. Pylori protocol and helps maintain the gut barrier function.
Unlike other milk-derived immunoglobulins on the market, Mega IgG2000 is derived from bovine serum, making it lactose-free, casein-free, and β-lactoglobulin-free. Take 1 scoop daily with or without food or as directed by your healthcare practitioner. Mix powder into 16 oz. of cold water or liquid of your choice. Stir for 20 seconds. For children under the age of 2, please consult your healthcare practitioner. Drink plenty of fluids
Consider Using Immunocharge:
ImmunoCharge is specifically designed to provide you with optimal dosages of these key immune-modulating nutrients and compounds. The synergy of these key nutrients and compounds strengthens immune function and improves the process of histamine metabolism and balancing inflammation levels.
Each ImmunoCharge capsule contains the same amount of powerful immune-modulating compounds. These include quercetin, resveratrol, vitamin D, vitamin A, selenium, zinc, vitamin C, N-Acetyl Cysteine, vitamin K2, and magnesium.
These ingredients support the body’s natural immune mechanism to help maintain good health. Rather than taking multiple different supplements to get these key nutrients, you can get the clinical dosages within 2 capsules daily of ImmunoCharge. I recommend taking 2 capsules with food, 2 times each day for best results.
Histamine Support Pack
There are several supplements that help the body to reduce histamine levels naturally. We have put these into the histamine support bundle, which offers a significant discount on these products compared to purchasing them individually. These supplements should be done in conjunction with a low-histamine diet and healthy lifestyle activities.
Tributyrin-X: This postbiotic supplement may help with histamine issues by stabilizing mast cells. It’s a form of butyrate that may help regulate the immune system and inflammatory response.
Normal Dosage: 1 cap – 2x daily (morning and night) with or without food. Advanced Dosage: 1-2 caps – 2-3x daily
Mega IgG2000: The immunoglobulin blend in Mega IgG2000 strengthens gut structure and physiology, detects and removes pathogenic agents and their toxic by-products, as well as assists in maintaining the gut immune system and your overall wellness.
Normal Dosage: 2 caps – 2x daily (morning and night) with or without meals. Advanced Dosage: 3-4 caps – 2x daily
ImmunoCharge: This product is specifically designed to provide you with optimal dosages of these key immune modulating nutrients and compounds. The synergy of these key nutrients and compounds strengthens immune function and improves the process of inflammation.
Normal Dosage: Take 2 capsules, 2 times daily with meals for optimal absorption, or as directed by your healthcare practitioner.
Advanced Dosage: Take 3-4 capsules, 2 times daily with meals for optimal absorption, or as directed by your healthcare practitioner.
Conclusion:
Histamine intolerance is a serious issue that many people are suffering from. Use the strategies in this article to help support your healing journey!
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. On our website, we offer long-distance functional health coaching programs. For further support with your health goals, just reach out and our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!










Thank you for this article! Like an answer literally dilivered to my inbox !
I’ve been dealing with chronic uticaria for 11 years now and this really shed some new light on my issue. I have new things to try now thank you dr. j!
Hi Dr Jockers,
This article has given me more light into what I have been through ,13 years back.
But no doctors were able to give me this kind of truth.any way God has healed my gut problems and I changed my eating habits and it helps me to stay in good health now.
May God bless you
Elsa
Dear Dr Jockers,
This is one of the best articles i came across in the last years regarding nutrition and natural healing,
your work is truly fantastic, balanced and to the point,please keep on the excellent articles u put out
endless gratitude,
Vishva
Once again Dr. Jockers an excellent article. I learned alot. Keep up the good work.
All the best
Kevin
Great article, I love the diagrams – makes it all so much easier to understand!
I have issues with histamine and when I’ve tried to eat sauerkraut that’s when my issues got really bad – my histamine buckets overfilled!
I stick to a simpler diet now to reduce inflammation – fresh meats, coconut oil, and certain vegetables. I feel better for it!
Which vegetables are best to eat
Check out the article above. It says which to avoid and which to eat.
Very good article. Several people I know would benefit from this knowledge.
Thank you so very much for this article! It is extremely helpful!! Please keep sending these great articles….you are helping so many people with problems that the “medical” doctors cannot help with!! God bless!!
Be very aware of seaweeds/algaes. Even though highly nutritious they are also very high in histamine. They are used extensively in many foods as a binder or thickening agent. Most prevalent is carrageenan which is in many organic milks. Almost all commercial ice cream contains it as well. It is used in cottage cheese, cream cheese, some deli meats, toothpaste, etc. The list is rather extensive.
Thank you for this insight Mike! Here is my article about Carrageenan and what to look out for: https://drjockers.com/?s=carrageenan&submit.x=0&submit.y=0
ALSO BE AWARE OF GUAR AND XANTHUM GUMS WHICH MANY WHO HAVE GUT ISSUES ARE INTOLERANT TO OR AT LEAST DOES NOT HELP THE GUT. THESE ARE IN MANY ORGANIC LIQUID PRODUCTS AND IN THE COCONUT MILKS ESPECIALLY.
My pleasure Doc J. Keep the good info coming. Much appreciated.
I’m in my early thirties and allergic to latex fruits like avocado, banana, and kiwi. Is this the same as histamine intolerance? I don’t have any of the symptoms on the above list, but I’ve heard people relate my allergy to histamines! If I can heal the allergy, I’ll try anything!!
Hey Heather,
That is probably not a histamine intolerance, but an IgE food allergy. One of the biggest things people with histamine intolerance notice is that they have increased symptoms with fermented foods.
Hey Dr, J,
Will our digestive Health program work for someone with HIT? Thx.
Correction:
Dr. J,
Will your…
Hey Mike,
Yes, the Digestive Health Restoration program is designed to help people with SIBO, Candida and parasitic overgrowth. With a few tweaks, we handle histamine intolerances as well. If you have a histamine intolerance, I would highly recommend doing the program!
How do you enroll in this program
You can get the Histamine support pack here: https://store.drjockers.com/products/histamine-support-pack
My issues all started with SIBO and lots of stress prior to that. I have been struggling now for almost two years and still trying to heal my gut! Dr Jockers do you see patients across state lines? So need to get this fixed!
Hey Teri, so sorry to hear this! Here are some helpful tips to find a good functional health practitioner: https://drjockers.com/functional-nutrition-tips-to-find-a-great-health-coach/
Best thing that helped to heal my stomach (in addition to diet changes, probiotics, GI Encap/aloe vera, etc.) was using L-glutamine once or twice a day in water on an empty stomach. There’s a great resource that is basically what I did called Good-bye Leaking Gut, by Norm Robillard.
TY.
I was wondering why avacado is included in the low histamine shopping list?
Also i was wondering about olive oil. A lot some people say its actually benificial to eat with a histamine intolerance while others like whole 30 have olive oil as something to avoid and say olives release histamine
Very good questions Thomas. I have found that many with histamine intolerance can handle small amounts of avocado (we will make that distinction now on the shopping list). Olives and olive oil are great unless they are packed in vinegar. Packed in water should be very good for someone with histamine intolerance.
Great article Dr. Jockers. In your video you say to avoid eggs but in this article they’re listed as ok to eat. What about duck eggs, could they be more tolerable than chickens eggs?
Eggs are not high histamine so they are fine, however, for some individuals, they may have a food sensitivity to them. Duck eggs may be more tolerable.
Hey Doc J,
Here is another ingredient, TBHQ, which like carrageenan, has caused me serious health issues. This synthetic ingredient is made up of phenols and butane. Eliminating this and carrageenan have given me my life back. I thought you would like to do a followup on this poison for the benefit of your readers. I have to wonder how many people with histamine intolerance are just allergic to a certain ingredient or ingredients. This appears to be my situation. Thanks for all you do
Thanks for letting us know about this Mike and I will have my research team look into writing an article about that!
What is TBHQ and what is it in? I’ve never heard of it.
The allergy defense has derivatives from pineapple! There are a few great studies out there showing the histamine inhibiting effects of watercress and pea sprouts. I have an egg, dairy/casein, almond, gluten allergies plus nightshade sensitivies, plus sulfide sensititivy (NAC, B6) and histamine sensitivy! My food list is super restrictive. It’s nice to see a list layout. I personally react to olives in water and sea salt but not olive oil. I have been AIP for a year and my antibodies have been dropping, I also found a correlation between my histamine high when my antibodies went up slightly. What about seeds and histamine? Chia, sesame, sunflower etc? The first reintroductions with seeds I have tried haven’t been successful and I am wondering if there is a correlation with seeds and histamine.
Many thanks!
Hey Bre,
Thanks for your input. Sorry to hear about your struggles. Bromelein is an enzyme that works well at metabolizing histamines and I have used it (Allergy Defense) clinically with people with histamine intolerance with very good results. Seeds can increase histamine so your inability to tolerate them is most likely due to that. Olives in water are higher histamine than olive oil. Hope that helps!
Our functional doctor just diagnosed our 9 yo daughter with histamine intolerance. I’m trying to wrap my mind around what we should feed her and what we shouldn’t, as many of the healthy foods we eat are off limits for her now. I was thinking we need to give her a probiotic now since she can’t have kefir/fermented foods/etc. But then I saw this quote at the bottom of the article: “In particular, if you struggle with fermented foods and probiotic supplements that is a classic sign of histamine intolerance.” Is there a safe probiotic for her to have to help boost her gut/immune system?
Hi Nicole ..
I was wondering the same thing; that you are after reading the issue of probiotics being a risky consideration. ( Hoping the doctor can leave a response on this thread ). I’m now 100% convinced that a gut healing diet will help these issues; but then where do we stand on a safe probiotic ..? I’ve been debating all week; on what type to buy or not to buy ..? ~ Feeling perplexed .. as I type this. After years of doing my own research into good common sense health solutions; I still refer back to: “How to Eat for your blood type”. By Dr. James A’dammo. It really is a good tool for anyone dealing with food sensitivites + issues.
Yes we just added a new section on this and here is what I recommend: https://store.drjockers.com/products/prescript-assist-broad-spectrum-probiotic?variant=1068435529
I tried this link and it is no longer valid. Are you now recommending a different SBO probiotic? Thanks.
Hey Nicole,
So sorry to hear about your daughter’s issues. The probiotic I see people with histamine intolerance respond well too is Prescript Assist here: https://store.drjockers.com/products/prescript-assist-broad-spectrum-probiotic
Begin with 1 capsule and see how she does. You can slowly work up to 2 caps – 2x daily.
Can’t thank you enough for your simplistic, yet detailed explanation with pictorial of this little known and/or accepted health condition in the mainstream medical community. For the past 2 months, I have been following a low-histamine diet after *stumbling* across the term “Histamine Intolerance” on the web. I’ve experienced more relief in those 2 months than I have in 20 years of attempting to get a diagnosis. I will be emailing all my friends and family a link to this article in hopes that they might gain an insight and recognize I am not the hypochondriac they have deduced I was for all these years. You have truly written the most concise and easily understandable explanation of HIT on the internet… thanks for sharing!
Thank you so much for the great comment! So glad you are getting results with this!!!
Subject: Probiotics .. / Avoid ? or … Take them … ? .. I could use some expert medical advice on this.
I’ve been following: “How To Eat For Your Blood Type” diet for over 10 years now. I’ve noticed a big improvement in how I feel; when I stick to this plan of beneficial foods and “avoid” my avoids. But; I unfortunately fell off the wagon too many times; knowing I shouldn’t have. For more information: google .. Dr. James A’damo / How to eat for your blood type. A list of books will pop up, etc. Recently; I noticed they now sell probiotics; on their web site. ” A probiotic for each specific blood type”. I’m definitely curious about this product + would like to find out more about this. I’m now starting a GAPS diet; knowing it’s time to heal my gut once and for all. Glad I found this web page / thread tonight. I had no idea; that probiotics could be a “histamine” issue. WOW .. good to know. I would love to know if their is a safe probiotic for those of us who have histamine issues. I really want to heal my gut issues and bring back the good bacteria. I just started the GAPS diet this week.
Susan,
This is a great suggestion. I just added a section discussing the right probiotics for histamine intolerance. I recommend Prescript Assist here: https://store.drjockers.com/products/prescript-assist-broad-spectrum-probiotic?variant=1068435529
Please do your homework. The GAPS diet is NOT a good idea for those with histamine issues. Dr. Jockers, please address this!
Dr Jockers,
I have a 16 year old that I believe may be suffering from histamine intolerance. Is it possible that hormones/stress can initiate this intolerance and that it may disappear as hormones/stress factors change? Your article was very clear and informative. We will test fermented foods to try and pinpoint that this is the problem. Thank you!
Cindy
Thank you Cindy. Yes, it is very possible that hormones/stress will aggravate the condition. When we are overly stressed, it will drive up inflammation and make us much more prone to conditions like histamine intolerance. We can keep that in remission with healthy lifestyle, keeping stress down, good sleep, advanced supplementation, etc.
Do you know of any SC based physicians that practice this type of health?
I’d look for a naturopath or functional medicine doctor, in my experience. Each is a bit different in their specialties/interests, but it’s the place to start and ask the questions of them in particular.
Doctor, I have been researching gut issues for my son and for my furbaby struggle;ing with mast cell tumors, Im ordering several of your products today for my son but was wondering if your products specifically the Allergy Defense and Prescript Assist Broad Spectrum can be used on dogs? thanks for so much valuable information!!
Hey Maria,
Sorry to hear about your son! Yes, you can simply open a capsule and put it in the dog’s food. The recommended dosages are for a 150 lb individual, so based on that, lower the dosage of allergy defense for your son and start low and gradually work up (same with your dog). The Prescript assist you can begin with 2 caps.
Hello Dr. Jockers,
I see that cow’s milk is not advised on this diet, but what about goat’s milk? Also, will following this diet help me to tolerate even the low Histamine foods at some point? For example, I cannot eat coconut, fruit other than banana, or leafy greens due to intestinal reactions.
Thank you for this helpful article!
Unfortunately dairy is a higher histamine food. If you have a histamine intolerance than reducing histamine load can help your body heal, which should help you reduce other food sensitivities.
Vitamin A. At least 10k units per day. And another 5 from cod liver oil if you tolerate it.
Good afternoon Dr. jockers
You recommend some type of diet especially, to avoid allergies of any kind, such as allergy to histamine
Vegetarian
Vegan
Macrobiotic
Diet according to blood group
Just a low-histamine diet as explained in the article Pilar.
Hello from Quebec Canada
Thank you so very much for your your article, following an anaphylasic shock I went to the ER, all test were negative, I am waiting for an appointment with an allergist. I now know I’m histamine intolerant, have put myself on a low histamine diet and probiotics for a week now and I feel a lot better.
I had all the symptoms and burning skin sensation. I thought I was allergic to the sun. I’ m so grateful to have found your site.
Wow Mona I’m happy to hear that!You’re headed in the right direction! I wish continued healing for you as you move forward.
Blessings!
Hi!! Is there correlation between abnormally low ‘T’ + acute bloating (bloating virtually after any food, no experience of trying low-h. diet so far – just low fodmap,dairy free,grain free,nut free,refined sugar free,gluten free,nightshades free,high GI carbs free – NONE of those have helped) in general, acne around chin sides/around lips (+nose) and histamine intolerance?
In other words – ibs+low ‘T’+histamine intolerance+severe acne around chin sides and lips – COULD THEY GO HAND IN HAND? Might we add histamine here as a potential trigger/offender of all other issues? But where in turn then histamine int. takes its origin? From wrecked immune system?
Hey V,
Histamine intolerance could be due to several factors (overexposure, autoimmunity, chronic inflammation, etc.) If you are having GI issues as well leaky gut could also be a culprit. I wouldn’t say there is one primary cause.
Hello Dr. Jockers,
I just found out about this histamine intolerance.Previously I thought I was allergy to seafood. But when I ate fresh seafood, there was no allergy reaction.
Furthermore, I was diagnosed with endometriosis stage 3-4. Does this has relation with histamine intolerance. I am a little bit confused with the choice of foods. Not only I have to avoid foods with histamines but also foods that is bad for endometriosis.
Your advice is very much appreciated. Thank you.
Hey Mary, they could have a similar underlying cause. It would require some investigation. You could look into hormone balance: https://drjockers.com/12-tips-to-balance-estrogen-levels-naturally/
and Chronic Inflammation: https://drjockers.com/chronic-inflammatory-conditions/
Hi Dr. Jockers
I have seen food lists that say no to peanuts but peanut butter is ok. What is your opinion? I also see no cashews–what about cashew milk and cashew butter? I am so happy I found your website. You have helped me tremendously after some unsuccessful derm visits with misdiagnosis. One last question if I may– every summer I get awful rashes on arms when working in my gardens. That is what I think finally triggered this awful HIT to hit me and spread from arms to rest of body. I am finally clearing after four months by following your advice. Most of my body has cleared with the exception of my arms. Is it possible my arms are super sensitive or super triggered due to repeated exposure and rash on arms every summer??? Can histamines be stored in there??? Thank you!!!
Hello, Dr. Jockers
I think I fall into the medication induced histamine intolerance category. I took Zyrtec brand antihistamine, daily, for approximately 10 years. My doctor recommended Zyrtec after an isolated incident of itching/hives. So began my horrific journey of trying to end my Zyrtec dependency. Each time I attempted to stop taking Zyrtec, withdrawal itching, phantom pinpricks, flushing, etc., were only alleviated by taking more Zyrtec. I was convinced I was allergic to something and still needed Zyrtec. It was an endless cycle. After a hiking fall, my doctor discovered my liver was inflamed. I do not use drugs, tested negative for all hepatitis strains, and am not a big drinker. The only meds I was taking was Zyrtec and a multivitamin. My doctor assured me Zyrtec was safe to continue using. I went online and started educating myself. It turns out, hundreds of thousands of consumers have experienced adverse effects of long-term Zyrtec use. There is a whole online community, although many doctors still argue the Zyrtec withdrawal phenomenon is not real. While on Zyrtec, I experienced almost every symptom on the drug’s list of negative side effects, even those termed as “rarely occurring”, which included rapid/irregular heartbeat, night sweats, anxiety, digestive issues, breathing problems, the list goes on and on. I stopped Zyrtec cold turkey almost 5 months ago. I went through weeks of horrific withdrawal, and a flood-gate of histamine in my body. Reading this article was a light-bulb moment for me! I have experienced a firestorm of itching, hives, flushing, etc., after unknowingly consuming many foods on the high histamine list. I also feel a sense of “fullness” in my abdomen, as if my internal organs are inflamed. My body and tissues feel as if I am retaining fluid. My skin has become super sensitive and reacts to even the slightest pressure, resulting in an episode similar to those suffering from chronic idiopathic urticaria. I was never diagnosed with this condition, and did not experience this type of allergic reaction, prior to using Zyrtec. My questions are: 1. Is my body now irreparably histamine intolerant? 2. Will my body ever be “normal” again? 3. How do I reduce the internal inflammation, water retention, etc.? I am not currently on any medication. I stopped the multivitamin, as it seemed to make me itch more (vitamin C?). I started taking Align probiotic, hoping to alleviate my IBS type symptoms. Please help!
Hey Cherie, thank you for sharing this information and so sorry to hear what you are going through. You may consider using something like this: https://store.drjockers.com/products/hista-response
There are probably a number of factors that need to be addressed in a periodical manner to fully tackle whatever is going on in your body. Reach out to michael@drjockers.com if you are interested!
In my experience Zyrtec is absolutely addictive and has withdrawal symptoms. It works on my asthma, but I noticed that if I start taking a half-Zyrtec every other day the asthma goes away. But after a week I need to take a half-Zyrtec every night. Then the asthma starts getting worse and I need to take a full Zyrtec every night to control it. It’s obviously inducing tolerance.
I wouldn’t advise anyone to take Zyrtec for long-term use. I’d use it for a few days and that’s it. It has strong mental side effects, I joke that it’s like legal LSD and it often feels like you’ve taken some. I have found greater success with inhaled steroids for short periods to reduce my asthma without withdrawal. Usually a week or two of Flovent will wipe out the asthma.
Thanks for sharing that Robert!
I recently started showing signs of cholinergic urticaria without the welts. It’s really amped up with the high pollen here in NC. So many of my other issues now make sense too now that I realize I likely have histamine intolerance. Thank you so very much for this article. I’ve been miserable the last few days and depressed at the idea of yet another chronic illness but now I feel hope that there are things I can do to help it and maybe it’s the root of other issues too. I’ll be adjusting my diet immediately and looking into supplements.
You’ve got this Melody!
Hello from Australia…
Can a person’s primary symptoms of HIT be used to determine what types of factors are the major contributors to their HIT? I.e. food, GIT issue, external environment.
My HIT has dramatically worsened after several possible triggers that occurred around the same time in my life. Moved from city to hills area, had first child, stressful pregnancy and very challenging first couple of years.
My primary symptom is skin crawling and hives/sores. Other symptoms include foggy brain, low energy and mood, poor internal stress management, eye complaints.
I have pyroluria and have been on standard supplement regime for this for 12 months. Also following gut health and low histamine diet for last month. Diet prior was good and had no sensitivities, therefore i suspect food will not be an issue for me once i get Histamine build up under control.
So, my question is – is there any way to determine what type of histamine source i should work on restricting most? And, is there a treatment approach that is best at targeting the skin?
I hope this makes sense, i am still getting my head around understanding how histamine works in our bodies so i can try figure out what it is doing in my body. I have not been able to identify any consistent triggers for my HIT issues, despite great effort.
Any thoughts you may have would be hugely, hugely appreciated.
Hey Holli, this would likely come down to reducing histamine sources while improving histamine metabolism in the body while identifying different stressors in your environment whether it be food, mold, underlying sensitivities. etc. We do have a protocol for improving degradation and addressing all of these factors together may make a big difference in improving inflammation and helping to resolve your skin issues. You can email michael@drjockers.com if you’d be interested in this protocol or doing a coaching plan to figure this out!
Can you ever recover from this ? I’m struggling with what foods to eat as everyone has a different option some say no to coffee but organic is ok ? Is coconut yogurt ok ? I was starting to think I had lupus or Lyme but this is me to a t I can’t eat tomato red wine chocolate cocoa salami banana nuts eggs also big sure why I can’t eat eggs happened after a flu vaccination
Yes you can definitely recover. I would recommend avoiding coffee and coconut yogurt during your histamine avoidance phase. Still plenty of good foods to enjoy though!
These lists are so confusing. It says nuts are high-histamine foods and should be avoided. However, almond butter is in the low-histamine list. Wouldn’t almond butter, as they are made from nuts, be high-histamine? It’s so confusing, to say the least. There are so many conflicting lists it’s hard to know which to follow. You just have to listen to your own body and lower your overall histamine load I suppose. Thanks for the information
I would avoid almonds and almond butter to reduce your overall histamine load but yes, symptoms can vary and some do better on certain foods than others.
Dear Dr. Jockers
I was wondering if almond flour was ok on a low histamine diet. If not, what kind of flour would you recommend?
No almonds are higher histamine but you can use coconut flour!
Thank you so much for the informative article! It pretty much sums up my issues that came out of the blue following a cortisone injection I received for a running injury. I’ve been told I have leaky gut, adrenal fatigue and histamine intolerance. I’ve been to so many doctors (conventional and naturopath) and no one has been able to help! I’m tying my hardest to heal my gut and remove high histamine foods from my diet, but what foods can help heal the gut? Fermented foods are out, but what foods are recommended? My diet is so restricted due to my sensitivities, but I’m willing to try anything to heal my gut. Thank you!
So sorry to hear this Jessica!! We are praying for you!!
Snap! I have exactly the same symptoms. I was told I had adrenal fatigue, histamine intolerance & leaky gut caused by candida overgrowth (though that was fairly low). I’ve finally found the root cause – its Mitochondria Dysfunction. Google it. There is lots of information on it. I have opted for Mitochondrial Replacement Therapy (devised by NASA scientists) that a relatively (2 hours away) local nutritionist offers. She tested me and yes that is absolutely whats wrong. Damage to those cells causes fatigue, high inflammation, and causes the gut walls to weaken so you get leaky gut which can lead to histamine intolerance. Once your gut is healed the histamine problem should correct my nutritionist tells me. If you can’t afford to go for therapy or there is no one near you it seems that the Ketogenic diet which is high in good fats so it feeds your mitochondria will help heal you. You possibly need Vitamin C, Magnesium and some other supplement but there’s information on it. Also books on the subject “Its Mitochondira not Hypochondria” is one. You also need to lower your stress levels (difficult I know when you can’t eat and you are frantically looking for a cure) meditation, EFT are both very helpful for lowering stress, plus the STOP technique for interrupting repetitive negative thinking. Our bodies are genetically designed to heal so long as we are not in stress, with help from the right diet, supplements and a little exercise. Good luck!
Thank you for sharing Fiona! Praying for your healing.
I hope you are doing better by now. I was helped greatly by a naturopath, but not until I read about and added L-glutamine to my regimen did I fully recover. Take a look at Good-Bye Leaking Gut by Norm Robillard.
*Good-bye Leaky Gut*
I want to reduce my histamine levels. Why are they elevated? I had random itching on my arms and upper back below the neck with no apparent cause. It went away at the end of summer so I assumed it was an allergic reaction to a plant in my gardens…also I m a professional gardener for a living. I had a heart attack in October 2018 (related to the high histamine level?) I ll do whatever it takes not to have another. I had no need for surgery, I weigh 125 pounds, and have since been getting my cardio exercise at least 3 times a week because apparently my job is not enough physical activity to strengthen the heart. Point me in the right direction please! My head is spinning with information overload!
So sorry to hear this! I would highly advise following the diet and supplement protocol I go over in this article! Praying for fast healing!!
This a great article! Thanks for adding the infographics which made it easier to understand. I just get myself tested.
Thanks Bianca!
This article is so helpful thank you! I believe I have this condition. I had random days of nausea and vomiting with a slight headache and I couldn’t figure out the reason. I even googled why do I have a hangover with when I didn’t drink any alcohol! I finally put it together that I was feeling terrible the following day after having afternoon coffee drinks at Starbucks. I cut out coffee but then I was feeling bad the day after eating a bar of chocolate. I don’t know if I should see a functional doctor or an allergist? I have read that the food sensitivity tests are useless.
Hi Christine, There are different methods to test for food sensitivities but a functional health practitioner can certainly help you identify areas of concern. I recommend reading this article: https://drjockers.com/food-sensitivity-testing/
I experience elevated histamine when I was younger and slowly it decreases in time, I don’t know why. I usually have hives and red skin every time my histamine shoots up. And worst, I also experienced difficulty in breathing when I had allergies before that hospitalized me for days. This article should be read by all so that people would become aware of what histamine is so that they would know how to handle it.
I am sorry that you deal with this Jhoei. This article may help you further understand what triggers your intolerance to histamine: https://drjockers.com/histamine-testing/
I have been searching for this article. Thank God i have found it.
Hives Hives Hives. I got to a point in my life where I thought, its incurable. Am on daily antihistamines which am dependent on. I have also noticed that every house i have lived in has had one mold issue or the other. Am really desperate for help/support.
It feels like ‘where do i start from?’
Amanda
Hi Amanda, I am glad you found this article! I don’t recommend the use of antihistamine drugs that can adversely impact DAO production. I would recommend that you work with a functional health practitioner that will help to customize a plan to navigate your health journey! These articles can help: https://drjockers.com/health-benefits-msm/, https://drjockers.com/functional-nutrition-tips-to-find-a-great-health-coach/
This article just about pinpoints my problem. I bought the histamine pack and would like to understand the dosage better. I have had reoccurring whelps on my arms and legs for 2 months now. I am almost sure it is related too much allergy meds, digestion meds, NSAIDs. Doctor currently has me on prednisone to try to control whelps with no further plan of action.
The dosage in this article seems to say….Take 2 Allergy defense every hour? Does that mean 48 capsules in a 24 hour period? Take Hista protect every time I take the Allergy Defense? Hista Response twice a day on empty stomach? Please help me know the best dosage. Thanks.
Hey Sheryl, Take 2 caps of Allergy Defense twice daily (morning and night) at least 1 hour away from meals. Hista Protect is meant to be taken with a meal and you can follow the advanced dosage protocol and take 2 caps daily with a meal. Hista Response can be taken with or without food either 2 or 3 caps twice daily depending on the normal or advanced protocol.
I have Sibo and histamine intolerance. I have not been able to treat Sibo due to side effects of antibiotics and the herbal supplements are too hard on my stomach I know I need probiotics but can’t tolerate them. I have eczema around eyes and on scalp and am sensitive to everything I try to help it with I have a cat that I’m allergic too Can the cat be aggravating my histamine intolerance?
Hey Shirley, I am sorry to hear about this. Unfortunately if you have an allergy to the cat your immune system is being stimulated. Following the steps in the article above can help along with consuming an anti-inflammatory nutrition plan. This article offers some valuable anti-inflammatory foods you can include regularly: https://drjockers.com/anti-inflammatory-foods/
Thank you so much for this article, as I do believe I suffer from a histamine intolerance issue. I have had allergies my whole life. Environmental (lived in Colorado most of my life), pet and some foods. All of this started coming to a head for me about 3 years ago, I was pregnant with baby #5 at 42 years of age, and at around the 8-month mark, I started having reactions to different foods I would eat. Not many, but mainly fast foods, like McDonald’s. My blood pressure would drop, then I would get light-headed, blood pressure would rise (very high), I would start to see black dots and feel like I was about to pass out and would get a flushed feeling, and anxiety. I was at work when I had this first attack, the ambulance was called because I was 8 months pregnant and the doctor had told me that it seemed as though my blood pressure dropped, not sure why, and then elevated, because I was freaked out, but they gave me meds and I was better. No mention of anything else. Followed up with OBGYN, and they had me on some sort of anxiety meds to help with the heart palpitations also told me that Benadryl can help slow the heart rate. So I would take the Benedryl when it happened but would take the anxiety pill only when the Benadryl didn’t seem to be enough. I have since moved to Amarillo, TX area and my environmental allergies seem to be better here, but my histamine intolerance seemed to kick it up a notch when I started making and eating and drinking my own fermented products like Kefir, Kombucha, saurkraut, and Kimchi. Would get massive yeast infections and all started reacting as above to almost everything I ate. Fast forward to now, I have done a ton of research, have taken a food sensitivity test and have also partaken in a 4-week Histamine Reset protocol. Which really seemed to help me get traction underneath my feet. Until I got a UTI infection, then everything went haywire! Again, I couldn’t eat anything because the infection and the pain from the infection had tipped my histamine bucket again. My question for you is if I can’t tolerate probiotics, supplements, turmeric, ginger, Apple Cider Vinegar, how can I begin to build good bacteria in my body? Also, the infection always comes back every couple of weeks or so. I’m having a hard time gaining any real progress when these infections keep popping up and taking me back to step one. Any suggestions you might have would be very much appreciated! I did take a round of antibiotics the first UTI I had about a month ago because it was so bad. But that was a huge mistake, because, it through my body into a frenzy! HELP!
Hi Christina, I’m sorry to hear! It sounds like you have a lot going on. If you find that you do not react well to certain foods it is probably best to avoid them and an elimination diet can help. I would also recommend that you speak with a functional health practitioner who will get to the root cause of your problems and customize a specific plan! These articles can help: https://drjockers.com/10-ways-improve-gut-microbiome/ & https://drjockers.com/functional-nutrition-tips-to-find-a-great-health-coach/
Also, since I seem to be intolerant to ANY and ALL supplements, I am leary of purchasing yours, what if I can’t take them, that’s too much money for me to just waste, do you have a money-back guarantee? I have spent so much money on supplements only to find out I can’t use them.
Thank you in advance for any advice, help, or tips you can offer!
Hey Christina, I would recommend that you speak with a functional health practitioner to help you decide what supplements work best for your health goals. Please don’t hesitate to contact our customer support if you have any specific order questions!
Sorry, thought of one other question, I read in your article that allergy medicine actually contributes negatively to this histamine issue rather than helps it, am I understanding that correctly? Currently, I take an Allegra in the morning, one spray of Flonase in the morning and 1 Benadryl at night before bed. If my histamine is low, I only take the Allegra in the morning and try to forgo the Flonase and the Benadryl. Should I be trying to wean myself off of all allergy medicines?
Hey Christina, That is correct. Certain anti-histamine medications deplete the enzyme DAO that assists in breaking down histamine. Common allergy medications also affect neurotransmitter health. I don’t recommend them and working with a functional health practitioner will help you.
Thank you for responding! I appreciate you and your efforts! Have a blessed day!
Hello Dr. Jockers,
Thank you for this great information! I’m following a low histamine diet at the moment as I’m having a flare up.
I find once I’ve gained some stability in my diet, I can eat some medium histamine foods; but I’ve overdone it, & now paying for it!!…Do you know if chickpeas & yellow split peas (gram flour) are high? Some lists say avoid, yet this has been a staple in my diet & mostly have no problems with it, but as my bucket is high right now, I’m not sure if I’m safe with it. Also buckwheat? This also is listed as high on some sites. I’m going to try cassava flour, as I need snacks! So maybe make cookies with this? Or pancakes… Just wondered what your thoughts were.
Thank you so much!! 🙂
Sorry to hear that Anni! Legumes such as chickpeas and yellow split peas are moderate, so you may be able to handle some of them. Cassava is good as well.
I would recommend taking some of the anti-histamine supplements which will really help…especially the Quer-C Powder https://store.drjockers.com/products/querc-c-powder
Ahh, thank you so much! I seem to be able to eat moderate but then go up to high as I think I’m ok for quite a few months, then obviously overload; which then takes a while for me to get down again. I will definitely try your suggestions, again, many thanks!
Have a wonderful day!🙂
Yes you have to monitor and adjust your load! But as long as you keep working on your health it should continually get better over time! Blessings!
Yes! Thank you so much! Getting there, have stopped dairy, which really wasn’t helping! Have a lovely day 😇
Please help I have been investigating your website and listening to your talks and I can’t seem to find where I would be able to get the histamine test and if it’s even possible I live in Canada I’ve asked my doctors they have no idea what I’m talking about and I definitely believe that I have histamine intolerance I’ve been doing all the right things with the diet changing it and noticing things that are really affecting me histamine wise I would really like some insight if there is a test to be done I would like to take that thank you
Yes Stephanie – here is the test https://drjockers.com/histamine-testing/
I’m so happy to see you are following comments in this post. It was a total eye opener. Two people you cited in the post are on my heroes list: Amy Myers and Chris Kresser. I was a patient of his several years ago. I went back and read his article you cited with fresh eyes. But. This is what really hit me like a ton of bricks. First, I just got a positive h.pylori test. Second I’ve been eating tons of smoked salmon lately on my keto diet. Third I’ve been taking Benadryl every night to sleep. And finally I happen to have gotten back in my 23andMe results that I have three of the undesirable alleles! They are AOC1 codes DAO insufficiently, IL8 (A35T) making me susceptible to h.pylori, and worst of all HNMT (C314T) which is possibly related to Parkinson’s (my mom and her dad both died from dementia related causes secondary to Parkinson’s Lewy Body type) and I also have the bad alleles in the three methylation conversion pathway. Fortunately I know what to do. Stop eating high histamine foods and stop Benadryl immediately. Then I’ll up my vitamin C, switch my B6 to P5P and start taking samE.
Thanks for a great blog post. My diet right now is practically bordering on a semi elemental diet — low FODMAP keto with no histamine foods. And to knock down the GERD I’m eating solids once meal a day. I drink home made bone broth (crowd cow beef shanks or pastured chicken from butcher box) three times a day plus added collagen. I switch brands daily from Dr. Myers to Perfect Keto to Primal Kitchen and Dr. Axe’s. Since both almond milk and coconut milk are off the table I’m mixing these in water. Occasionally I toss in a handful of raw spinach or kale. I’m so happy to have found your site because it’s going to enable me to craft a meal plan to make me (low carb paleo) and my doc (standard FODMAP) happy. I’ll never use a low FODMAP standard American diet ever ever. No grains or legumes ever again. So this is a happy medium.
Glad you are figuring this out Claire! Praying for healing for you! Blessings!
Hi!
I was wondering if nuts are in the high histamine category because they are not frozen after picking, and they tend to be sold months after the dates that they were picked. Is there any research on this?
I have been freezing nuts and they stay much fresher than in a cabinet.
Yes nuts do tend to be higher in histamines. Almonds are a lower histamine nut.
In your photo diagram of The Body’s Response to Histamine Release at the top of the picture is blood clots. Is it possible for the blood clots to cause a stroke? I have suffered from high histamine response for about 15 years since receiving a tetanus shot. I recently had a stroke and we are trying to figure out what caused it. When I saw your article here I had a “Thank you God moment for showing me this page”. Now I am wonderering if DAO might heal my body. I am very sensitive to all excitotoxins, & lots of foods due to leaky gut. I have lost so much sleep due to extreme headaches that start during the night. Thankfully I do get some sleep now & then, but don’t want to go onto statins for my stroke! Thank You!
Yes blood clots are exactly what causes a stroke. It is possible that this could be histamine related. Here is a helpful article on Cerebrovascular disease as well: https://drjockers.com/cerebrovascular-disease/
What about Nutritional Yeast? Is that a high histamine or low? I can’t seem to find that on any histamine intolerance food list. Trying to empty the bucket and miss having nutritional yeast. Thank you for this awesome article Dr. Jockers!
Unfortunately it tends to be high histamine. Of course, histamine reactions are individual and some folks react to certain things much worse than others.
Thank you so much Dr. Jockers for replying and for helping shine some deeper light on this wild long list of seemingly healthy foods that am be such a detriment! Was hoping to hear you say nutritional yeast is different than yeast used in baking breads as daras histamine levels but so appreciate finally knowing for sure! We appreciate it greatly! And all the content you share with the world!
Your huge fan, trying to stay super healthy living in our van,
Amanda
Thanks so much Amanda! Blessings to you and your family!
Well thank God I found this video.
I don’t know where to begin.I have been suffering for almost 10 years. So all of the foods and beverages you mentioned I can not eat or drink..I will get a huge rush of histamine and its so scary.Whenthis happens I take benadryl to bring it down..I want to/ need to get help..The crazy part is when I get a reaction from high histamine I get this inflammation that seems to target my should and area that is very tender due to and injury..So what should I take.Im lactose intolerant and it seems im getting worse as far as foods..Please help
Yes I would recommend following the recommendations in this article.
Hello Dr. Jockers,
Such an excellent overview of histamine intolerance.
Citrus is on the avoid food list for histamine.
1. Should one avoid both fresh citrus and citrus juices?
2. Are supplements containing citrus seed extracts ok to take or do they too pose a histamine problem?
Thank you! Beth
Hey Beth, each person is different and there are some with histamine intolerance that do fine with citrus. However, others do very poorly with it. It is a good idea to avoid it for 10-14 days and then try adding it back in small amounts and see how you respond. Usually this is ok in supplements but not a bad idea to take it out for 10-14 days and then try it back and see what you notice.
Dear Dr. Jockers,
Thanks so much for answering my above question on citrus…most helpful.
Another question comes to mind regarding ALCOHOL and HISTAMINE INTOLERANCE. Many homeopathic solutions contain alcohol often at 20%. Is it possible that the alcohol in homeopathic remedies could possibly aggravate one’s histamine intolerance?
Thank you once again!! Beth
It should be fine since you are taking such low doses of these.
Dear Dr. Jockers,
Love your article! Makes so much sense.
I looked up the ingredients of your supplement. Would you please have a vegan version of it? Yours has an egg in it…I do not tolerate eggs well.
Thank you. M
Very informative article. I’ve been having side pain and back aches, took some Benadryl (which I now know not to), but it helped my symptoms. So that’s one reason it seems to be histamine related.
I was okay until I took an antibiotic earlier this year and was also on Prozac. Have stopped taking it because I was worried it was hurting me, apparently that was the right call.
How long does it take to get better from a histamine intolerance? Also, will this affect a future pregnancy?
Sorry to hear about that! You can get better within 4-6 weeks in many cases and most likely can still have healthy future pregnancies.
Hi Dr Jockers. Thank you for this article. I have recently become aware of histamine intolerance due to my daughter having experienced it in tandem with her period EVERY MONTH. She finally realized that she wasn’t getting a “cold” with her menstrual cycle but an “allergic reaction” aka high histamine symptoms.
So….doesn’t seem to be food or a particular thing she is eating that triggers it but that her menstrual cycle is triggering this response.
Have you heard of this before? Is there any information you could point us in the direction of in order to calm or totally get rid of this strange response?
Yes that is potentially possible. You should have her work with a functional health practitioner to figure out the root cause factors.
Cannot thank you enough for this detailed and such an informative article Dr. Jockers. It’s only in the past 7 or 8 months that I’ve developed a red rash on my face and neck. It was not too bad and I applied organic cold pressed avocado oil because on those spots the skin was dry. But 4 weeks ago I came down with what looked like flu symptoms . Runny nose, itchy throat and a cough. No fever but very fatigued. The red patches just flared up, especially the one on the neck.
I eat an avacado almost everyday and see that it is on the list of foods to avoid fir a histamine condition. What about freshly squeezed lemon juice and a tablespoon of apple cider vinegar which I have every morning? And bone broth?
Thank you .
Blessings,
Joyce
Sorry to hear about this. Many people with histamine issues struggle with lemon juice, ACV and bone broth. You can do water with a bit of sea salt and ginger tea is great as well.