 Atrial Fibrillation: Causes, Symptoms & Natural Support Strategies
Atrial Fibrillation: Causes, Symptoms & Natural Support Strategies
More than 30 million people worldwide are affected by atrial fibrillation (AFib). AFib is a type of cardiac arrhythmia, or irregular heartbeat. This common and serious condition can lead to blood clots, stroke, dementia, heart failure, and even death.
Most people with atrial fibrillation experience abnormal heart rhythms, including racing, fluttering, or pounding heartbeats. Other common symptoms include fatigue, dizziness, weakness, and shortness of breath. However, some people with AFib experience no symptoms and are unaware they have this condition. AFib can lead to serious health consequences, even for people who are asymptomatic.
There are a number of underlying causes and risk factors associated with AFib. It is important to identify and address these issues. Fortunately, there are natural support strategies to help improve heart health and cardiovascular tone. In this article, I will review some of the best strategies to improve your overall heart health.
What is Atrial Fibrillation?
Atrial fibrillation, also called AFib or AF, is the most common type of heart arrhythmia. A person with AFib has abnormal firing of electrical impulses in the two upper chambers of the heart (the right atrium and left atrium, or collectively the atria). This causes the atria to beat chaotically and irregularly out of coordination with the two lower chambers (the ventricles).
Within the right atrium, there is a group of cells called the sinus mode. This is your body’s natural pacemaker and produces the signal that normally starts each heartbeat. A normal heart rate is 60-100 beats per minute.
With AFib, the signals in the atria are chaotic. As a result, the atria will quiver (or fibrillate) and often a person’s heart rate will increase. The heart rate in atrial fibrillation may range from 100 to 175 beats per minute (1). The impulses do not get through to the two lower chambers of the heart, the ventricles, so they do not beat as rapidly.

Prevalence of Atrial Fibrillation
AFib affects 2.7-6.1 million people in the United States and 9% of people over age 65 (2). This number is expected to reach 12 to 15 million by the year 2050.
Worldwide, the prevalence of AFib is increasing in both developed and developing countries. AFib is the leading cause of cardiovascular disease worldwide and affects over 33.5 million people (3).
Types of Atrial Fibrillation
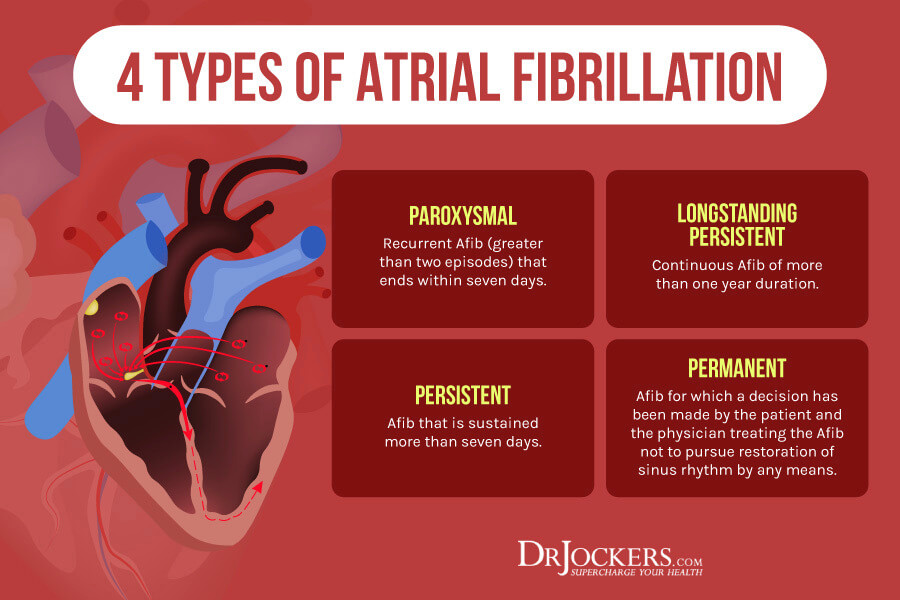
There are different types of AFib:
- Paroxysmal fibrillation: Occasional AFib with symptoms that come and go, usually lasting a few minutes to several hours and sometimes days.
- Persistent: Irregular rhythm that lasts longer than 7 days; heart rhythm does not go back to normal on its own; electrical shock or medications are needed to restore heart rhythm.
- Long-standing persistent: AFib episodes that are continuous and last longer than 12 months.
- Permanent: Abnormal heart rhythm cannot be restored; medications are required to control heart rate and prevent blood clots (1).
Symptoms of Atrial Fibrillation
AFib can be silent or symptomatic. People with silent AFib do not experience any symptoms and may be unaware of their condition.
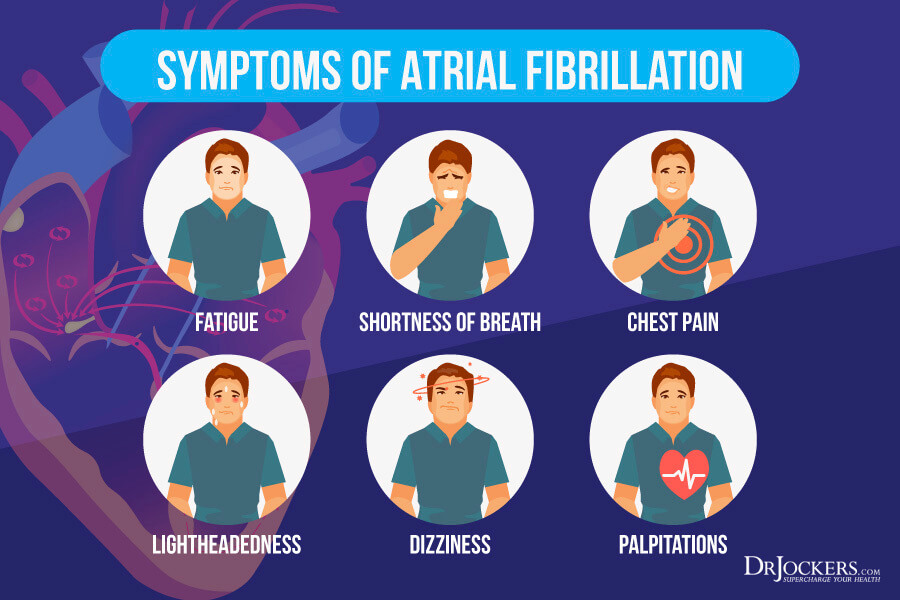
For people who do experience symptoms, the most common signs and symptoms of AFib are:
- Palpitations – sensations of a racing, uncomfortable, irregular heartbeat or a flip-flopping in your chest
- Fatigue
- Shortness of breath
- Chest pain
- Lightheadedness
- Dizziness
- Weakness
- Reduced ability to exercise
Atrial Fibrillation Causes and Risk Factors
There are many factors that may increase your risk for developing or lead to atrial fibrillation. When AFib is caused by a factor other than heart problems, it is often referred to as lone atrial fibrillation. With lone atrial fibrillation, the cause if often unclear and serious complications are rare.
1. Advanced Age
A prominent risk factor for AFib is advancing age (4). The overall lifetime risk of atrial fibrillation is around 25% for people over the age of 40 and 37% for people over 55. This risk may increase or decrease depending on the presence of other risk factors. In older adults, the estimated death rate of people with AFib is 20% one year after initial diagnosis and 50% five years after diagnosis.
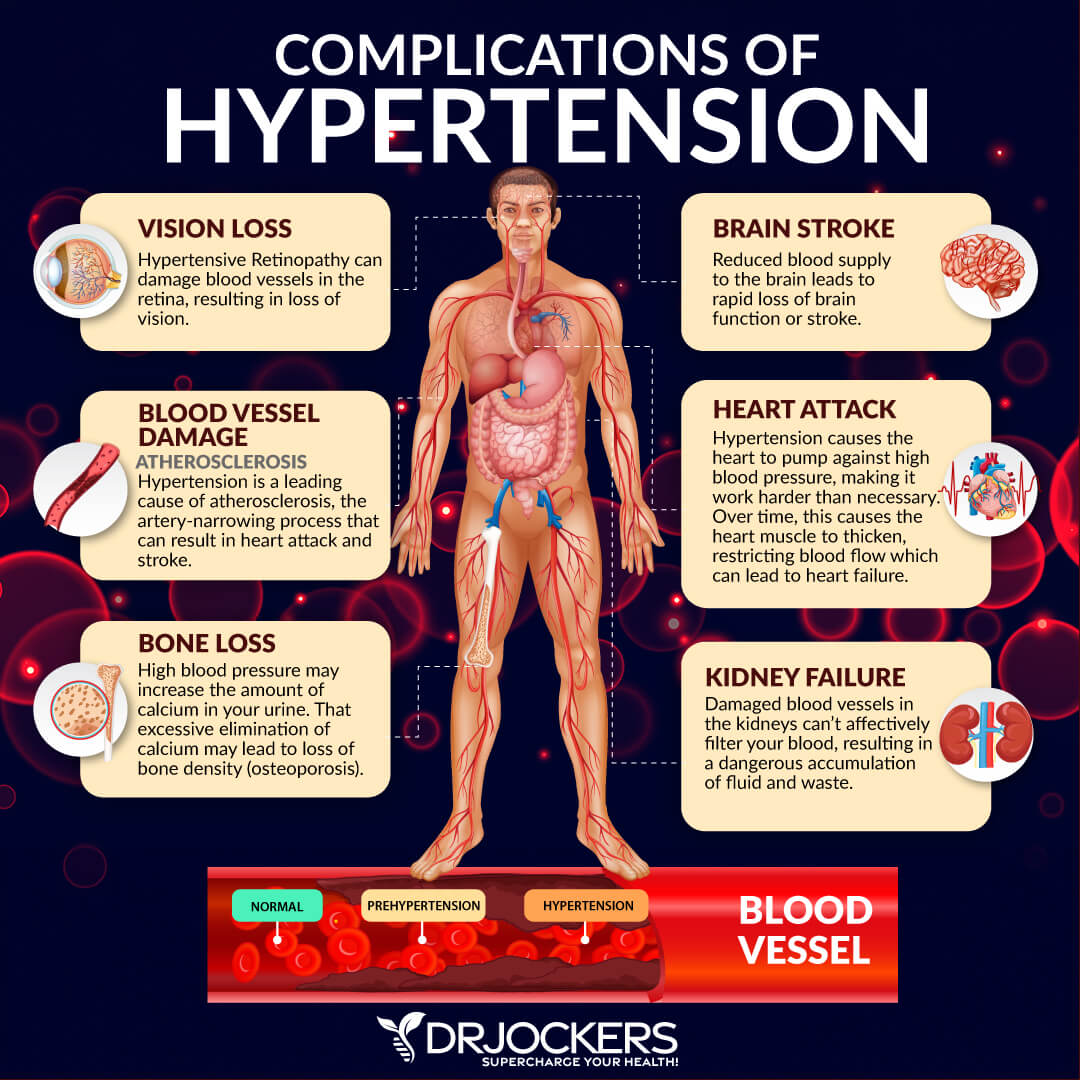
2. High Blood Pressure
High blood pressure accounts for 14 to 22% of AFib cases (2). Blood pressure is the force of blood against the walls of the arteries. Over time, high blood pressure can damage the heart’s electrical system, resulting in AFib. Both high blood pressure and AFib increase a person’s risk for stroke and heart failure.
3. Obesity
Obesity is a significant risk factor influencing a person’s lifetime risk of AFib (4). It is one of the most important modifiable risk factors for atrial fibrillation, doubling the risk of new onset AFib.
4. Heart Issues
A history of heart disease or another myocardial infarction increases a person’s risk for AFib. Heart abnormalities or damage to the heart’s structure are the most common causes of AFib. These include:
- Heart Attack
- Coronary Artery Disease
- Abnormal Heart Valves
- Congenital Heart Defects
- Previous Heart Surgery
5. Genetics
Over the last 10 years, the discovery of AFib related genetic variants has been accelerated (5). Current studies are focusing on mapping the polygenic structure of AFib.
6. Certain Medications
Medicines including adenosine, digitalis, and theophylline can increase your chance of having AFib (6). Bisphosphonates, a class of medications used to treat osteoporosis, have also been shown to increase a person’s risk of developing atrial fibrillation (7).
7. Hyperthyroidism
Hyperthyroidism is when your thyroid makes too much of the thyroid hormone thyroxine. When there is a high amount of thyroxine in the blood, the heart becomes overstimulated. This can cause a fast or uneven heartbeat or heart palpations.
8. Sleep Apnea
When a person has sleep apnea, there are sudden drops in blood oxygen levels while they are sleeping. This strains the cardiovascular system and may increase your risk of AFib.

9. Stress and Distress
Stress, anxiety, and depression are linked to AFib (8). People with psychological distress may have more severe AFib symptoms and adverse outcomes (9).
10. Sick Sinus Syndrome
Sick sinus syndrome occurs when there is improper functioning of the sinus mode, the heart’s natural pacemaker. This can lead to AFib.
11. Using Stimulants –Caffeine, Alcohol, Tobacco, and Medications
Smoking and alcohol consumption increase your risk of AFib. Men who consume more than 14 alcoholic drinks per week, and women who consume more than 7 drinks per week have an elevated risk (4). Drinking excessive caffeine and using stimulant medications may also raise your risk of AFib.
12. Gastrointestinal and Liver Issues
It is estimated that at least 40% of people with AFib also have gastrointestinal issues (10). These include dyspepsia, gastroesophageal reflux disease (GERD), peptic ulcer disease, and GI bleeding.
Gastrointestinal and liver diseases are common in people with AFib (11). Researches have shown a bidirectional relationship between AFib and these diseases. Gastrointestinal conditions may directly relate to AFib and the drugs used to treat AFib may cause gastrointestinal diseases.
13. Lung Disease
People with long-term lung disease, such as chronic obstructive pulmonary disease (COPD), have a greater chance of having AFib.
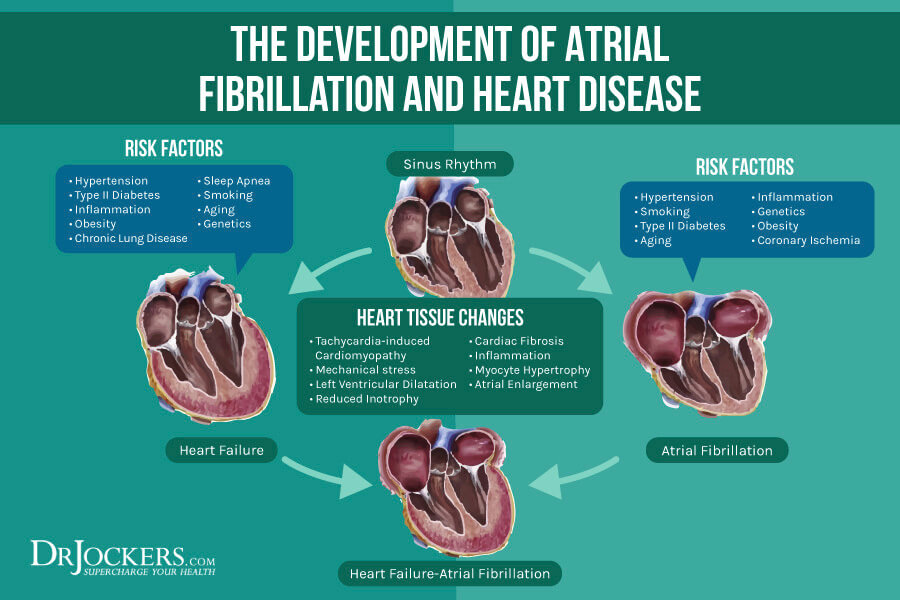
Complications of Atrial Fibrillation
1. Blood Clots
With AFib, blood does not flow through the heart properly. This can lead to the pooling of blood in the heart and the development of blood clots within the upper chambers of the heart. These blood clots may circulate to other organs and lead to ischemia, blocked blood flow.
2. Stroke
A stroke occurs when a blood clot gets stuck in a person’s brain. AFib increases a person’s risk of stroke by 4 to 6 times on average, and this risk increases with age (12). AFib-related strokes are nearly twice as fatal and disabling as non-AFib related strokes.
People with AFib can have multiple strokes, including silent strokes. Silent strokes do not have physical symptoms but show up on a brain scan. Over time, silent strokes can cause dementia. There is twice the relative risk of stroke in women with AFib than men.
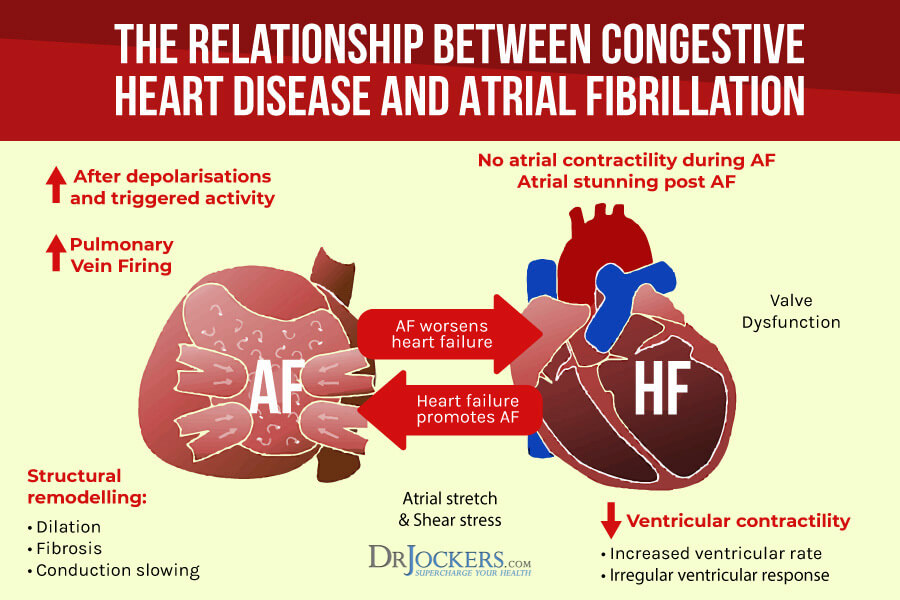
3. Cardiovascular Disease
Atrial fibrillation is a leading cause of cardiovascular disease worldwide (3). AFib is associated with a wide range of cardiovascular events, heart failure, ischemic heart disease, and sudden cardiac death.
Gender Differences with Atrial Fibrillation
Women experience AFib differently than men and have an increased risk of complications from atrial fibrillation (3). Studies show the following gender differences in men and women with AFib:
- Women may be more likely to have symptoms during an attack of atrial fibrillation;
- Women may have higher heart rates; and,
- AFib is associated with a stronger relative risk of all cause mortality, cardiovascular mortality, stroke ischemic heart disease, and heart failure in women than in men.
How is Atrial Fibrillation Diagnosed?
Atrial fibrillation is difficult to diagnose because it shares the same symptoms with other heart disorders. To diagnose AFib, your doctor may review your symptoms, medical history, and conduct an examination.
There are a variety of tests doctors may order to diagnose AFib. These include an electrocardiogram (ECG), portable ECGs, echocardiogram, blood tests, stress test, and a chest x-ray of the lungs and heart.

Strategies to Support a Healthy Heart Rhythm
There are many natural lifestyle strategies you can follow to improve cardiovascular health and heart rhythm. These are not FDA approved to prevent, mitigate, treat or cure A Fib, however, many people who have practiced these have seen positive results.
How we take care of our body matters and it can make a big difference in your life! Follow these strategies for improving your heart rhythm and overall health.
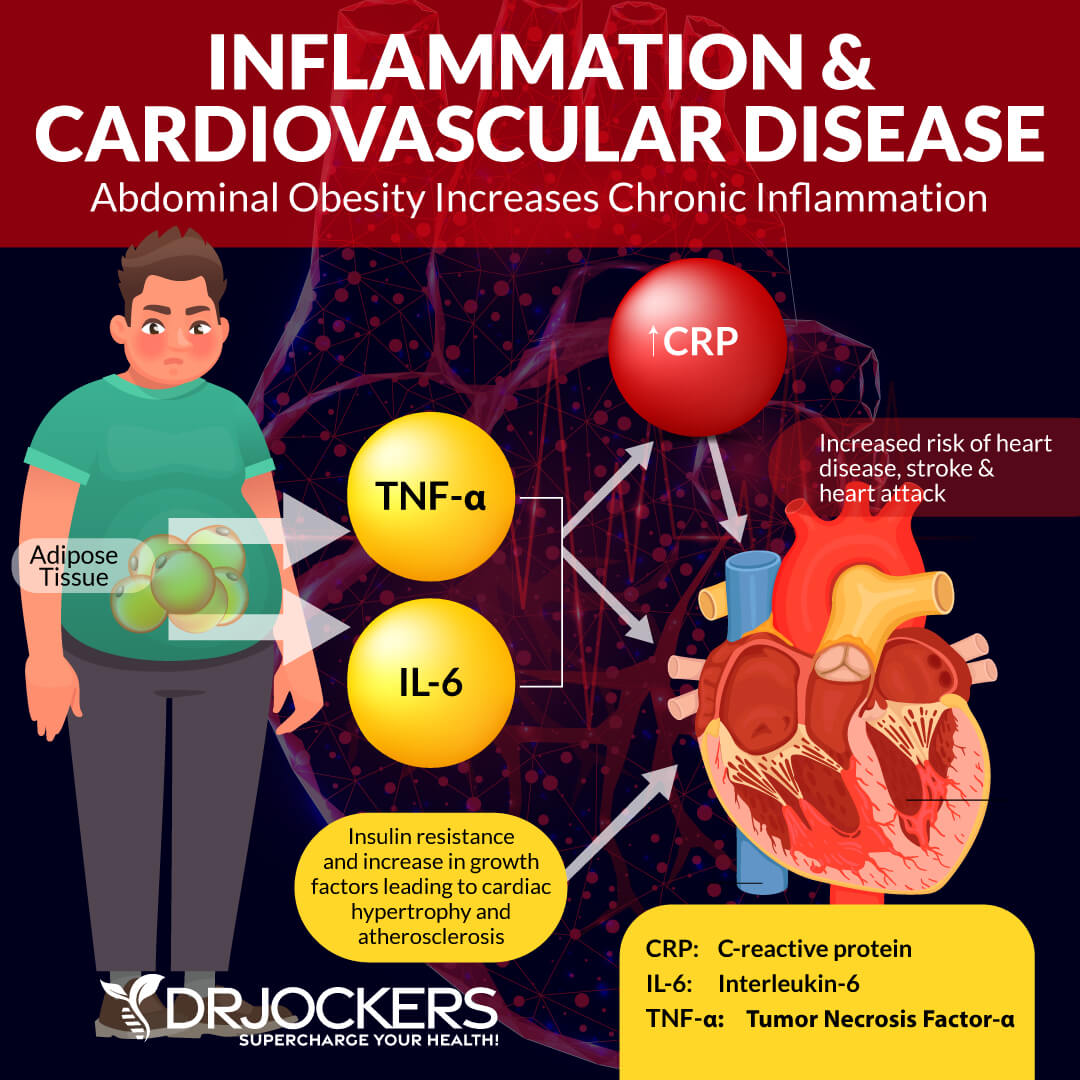
Anti-Inflammatory Diet
Reducing inflammation is key for improving heart rhythm. One of the main causes of inflammation is the highly processed, Western (or standard American) diet. It is critical to remove proinflammatory, disease causing foods and consume an anti-inflammatory diet of high quality, whole, unprocessed foods.
An anti-inflammatory diet is rich in antioxidants, phytonutrients and essential fatty acids. This nutrition plan helps to reduce inflammation, stabilize blood sugar, lower your toxic load, and support healthy blood pH levels, lower oxidative stress, and help fight free radical damage in your body. These factors contribute to AFib and other chronic conditions (13).

Foods to Eliminate
It is important to remove these foods which are very harmful to heart health (14):
- Refined carbohydrates
- Added sugars
- Hydrogenated and partially hydrogenated oils (trans fats)
- Factory farmed meat and dairy products.
- Pre-packaged and fast foods

Healing Foods to Include
You should consume a variety of low to moderate carbohydrate, lower glycemic fruits and vegetables, healthy fats, grass-fed, organic, pastured meat and dairy, and wild-caught, omega-3 rich fish. These foods contain powerful compounds and nutrients to reduce inflammation and heal our bodies.
Some of the top foods for heart health are leafy greens and berries. These foods contain abundant antioxidants which help lower the risk of cardiovascular disease by inhibiting LDL cholesterol oxidation, promoting plaque stability, improving vascular endothelial function, and decreasing the tendency for thrombosis (blood clotting) (15, 16). Antioxidants protect cells from free radical damage and oxidative stress.
Healing fats are also great for heart health. Studies have shown that both polyunsaturated and monounsaturated fats are inversely associated with the risk of heart disease (17). These fats may help improve your cholesterol levels and lower your risk of cardiovascular disease. For more information on the best foods for heart health, check out this article.

Regular Exercise
Regular light to moderate exercise is good for the heart and improves risk factors associated with AFib. Some of the many benefits of exercise include maintaining a healthy weight, improving muscle tone, lowering blood pressure, and relieving anxiety and stress.
It is important to monitor your AFib symptoms while exercising. People with AFib can tire more easily when exercising. They may also notice their heart racing if the exercise is too strenuous.
Lifting light weights, riding an exercise bike, or using an elliptical machine are good exercises for people with AFib. Be sure to warm up before exercising with stretches and low impact walking. It is also important to stay well hydrated.

Lose Excess Weight
Losing excess weight is very important for anyone with AFib. There are many weight loss strategies which may be helpful. Implementing the anti-inflammatory diet discussed above helps with weight loss and reduces inflammation which contributes to excess weight. It is also important to support digestive health by healing leaky gut and balancing the microbiome.
A very effective strategy for losing excess weight is intermittent fasting. Intermittent fasting is eating during a smaller window during the day such as only eating from 8 AM to 6 PM. This can help you burn fat by optimizing insulin sensitivity, down-regulating inflammation, and increasing growth hormone in the body (18). For detailed information on how to practice intermittent fasting, read this article.
Many people are unable to maintain a healthy weight despite exercise and dieting. This may be due to insulin resistance and hormonal imbalances. Weight gain, particularly abdominal fat, is a classic sign of insulin resistance and chronic inflammation. Low thyroid function and low levels of vitamin D3 are also associated with weight loss resistance. These issues must be addressed to lose excess weight.
Manage Stress and Prioritize Sleep
Managing stress and getting restorative sleep are important for people with AFib. High stress and sleep deficiencies cause blood sugar imbalances, promote inflammation, and increase cortisol secretion. Sleep deficiencies and stress are also linked to high blood pressure, diabetes, and obesity, all of which are associated with AFib.
Fortunately, strategies to reduce stress may also benefit sleep. Balancing your blood sugar levels with a healing diet is critical. Other powerful strategies include prayer or meditation, grounding, deep breathing exercises, sunlight exposure during the day, Epsom salt baths, and dry brushing. For better sleep, avoid artificial light, black out your room with blackout curtains, use a sleep mask and/or ear plugs, and implement healthy sleep habits.

Balance Electrolytes
Balancing your electrolytes may be helpful for AFib. Our bodies have mineral salts in the form of sodium, potassium, sulfate, magnesium, calcium, and phosphate that help to control the electrical charge and water flow around cells. Electrolyte levels that are too high or too low can affect your heart’s electrical impulses and contribute to arrhythmia development.
To help maintain proper electrolyte balance in the body, you can add natural salt (pink Himalayan or grey Celtic) to water or to drink mineral rich organic vegetable or meat broths. You can learn more about symptoms of electrolyte imbalances and how to correct them in this article.

Supplements to Improve Heart Health
1. Glutathione
Glutathione, commonly referred to as “the master antioxidant,” is important for heart health. It is a powerful anti-inflammatory and has the essential role of maintaining exogenous antioxidants such as vitamins C and E in their active form. Glutathione protects cells from free radicals and repairs free radical damage that does occur.
Many people are deficient in glutathione and may benefit from supplementation. Normal glutathione gets metabolized in the digestive system and dosn’t make it to the cells. However, you can find N-Acetyl Cysteine (NAC) which is a natural precurser to glutathione production and has been shown to increase intracellular glutathione levels.
NAC is widely available and fairly low cost. The most absorbable forms of glutathione are S-acetylated glutathione and liposomal forms of glutathione. These forms cross through the gut and go directly into the cells. They cost more than NAC but are also more effectively bioavailable for the body.

2. Curcumin
Curcumin is the active compound in turmeric. This powerful compound is good for the heart due to its anti-inflammatory, antioxidant, anti-thrombotic, and antimicrobial properties. It effectively balances serum cholesterol levels by eliminating excess LDL (“bad”) cholesterol from the arteries and blood vessels.
The antioxidant effects of curcumin have been shown to reduce cardiotoxicity and prevent cardiac complications (19). Turmeric also boosts the body’s natural antioxidant capacity to fight damaging free radicals.

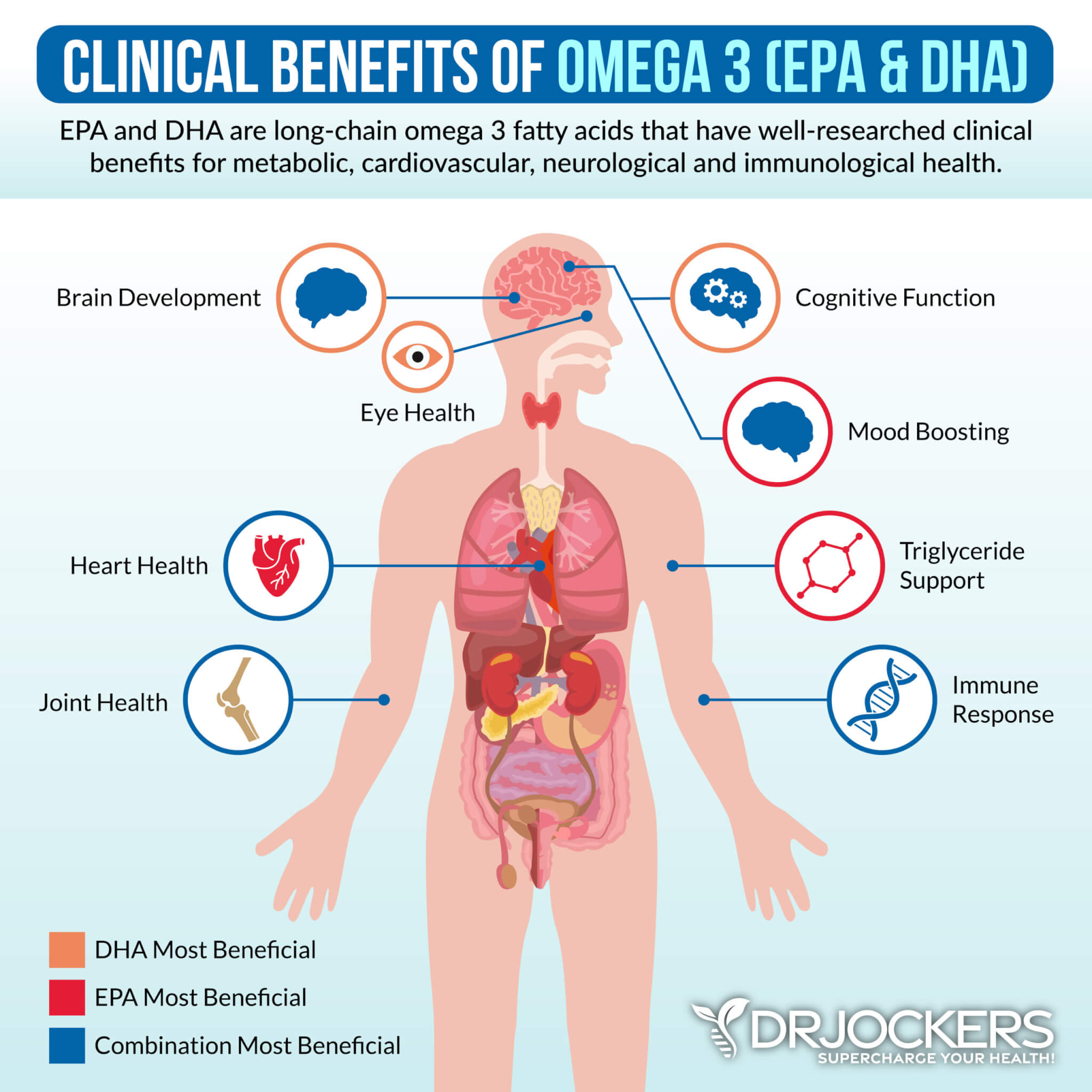
3. Omega-3 Fatty Acids
Omega-3 fatty acids are essential fats that your body cannot produce. You must get Omega-3s from dietary and supplement sources. There are three main kinds of omega-3s, DHA, EPA, and ALA. Omega-3s have direct and indirect anti-arrhythmic effects. They have antioxidant, anti-inflammatory, and antifibrotic properties (20).
Plant based omega 3’s such as flax oil only contain the small chain omega 3 called ALA and do not have any DHA. It is very hard for our body to convert ALA into DHA so it is best to get a high quality fish or krill oil that is rich in EPA and DHA. You want to find a brand that is molecularly distilled to take out any heavy metals and other unwanted contaminants.
Be sure to discuss with your physician before using as fish oils have a blood thinning affect and can be contraindicated if you are on blood thinning medications.
4. Mitochondrial Support
Your mitochondria are the powerhouses of your cells. They generate cellular energy in the form of adenosine triphosphate (ATP) and are involved in major metabolic functions of the body.
The heart contains 5,000 mitochondria per cell and mitochondrial dysfunction results in cardiac issues. To improve cardiovascular health and heart rhythm it is important to focus on enhancing your mitochondrial function.
Support your mitochondria with clinical doses of CoQ10, L-carnitine, N-acetyl cysteine, creatine monohydrate, B vitamins, magnesium, alpha lipoic acid and D-ribose. You can find mitochondrial support supplements that have most if not all of these key nutrients.

5. Magnesium
Magnesium is an essential macro-mineral that the body needs in large amounts. It is the “master mineral” and supports over 300 physiological processes or functions in the body. Magnesium plays an essential role in the cardiovascular system and other systems in the body. Deficiencies in magnesium may lead to irregular heartbeats and other health issues.
Around 68% of Americans are deficient in magnesium. Magnesium is critical for keeping the calcium: magnesium ratio in balance within the cardiac cells. When there is too much calcium within the cell, it fires more frequently, and this causes A-fib. I recommend supplementing with a good quality magnesium malate or glycinate for best results.

Final Thoughts on Atrial Fibrillation:
AFib is a common but serious type of heart arrhythmia. It occurs when the heart’s upper and lower chambers beat out of coordination. This increases a person’s risk of blood clots, stroke, heart failure, and can lead to death.
Some people with AFib do not experience symptoms. For those who do, symptoms can include heart palpitations, fatigue, lightheadedness, dizziness, shortness of breath, and chest pain.
AFib is most often linked to underlying heart issues such as high blood pressure, coronary artery disease, or a heart abnormality or defect. Other factors can increase your risk. To improve AFib, it is important to identify and address these underlying issues. An anti-inflammatory diet, along with lifestyle changes and targeted supplementation may improve your heart rhythm and overall health.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. On our website, we offer long-distance functional health coaching programs. For further support with your heart health and other goals, just reach out and our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!




Chloride is not an element, it is a compound. #17 is chlorine.
Thanks for sharing!
Isn’t Taurine a good supplement to take to prevent A-fib?
It can be helpful!