Dopamine For Motivation and Focus
Dopamine (dopa) has been called the “motivation molecule,” as it helps provide the drive and focus needed to get stuff done. Dopamine is also involved with the “pleasure system” of the brain and functions to create a feeling of enjoyment and a sense of reward to motivate performance.
People who suffer from low dopamine often experience hopelessness, worthlessness, and struggle to handle stress. These individuals will often isolate themselves from others and have self-destructive thoughts and behaviors (1).
Being easily distracted and having trouble focusing and finishing tasks can be signs of early deficiencies (2). Long-term, poor dopa signaling can result in hand tremors, slowness of movement, and pre-Parkinson’s symptoms.

Dopamine’s Activity in the Brain
Dopamine is a neurotransmitter that plays a key role in the reward-motivation behavior mechanisms. Any sort of reward, such as getting food, sex, making money, earning praise, etc., increases dopamine and the feeling of pleasure. Most addictive drugs increase dopamine activity in the brain.
Dopamine is also involved heavily in the following:
- Reward and pleasure centers.
- Attention and Learning
- Sleep and Overall Mood
- Behavior and Cognition
- Movement and emotional responses.
- Enabling us not only to see rewards but to take action to move toward them.
- Voluntary movement, motivation, and reward.
- Inhibition of prolactin production (involved in lactation).
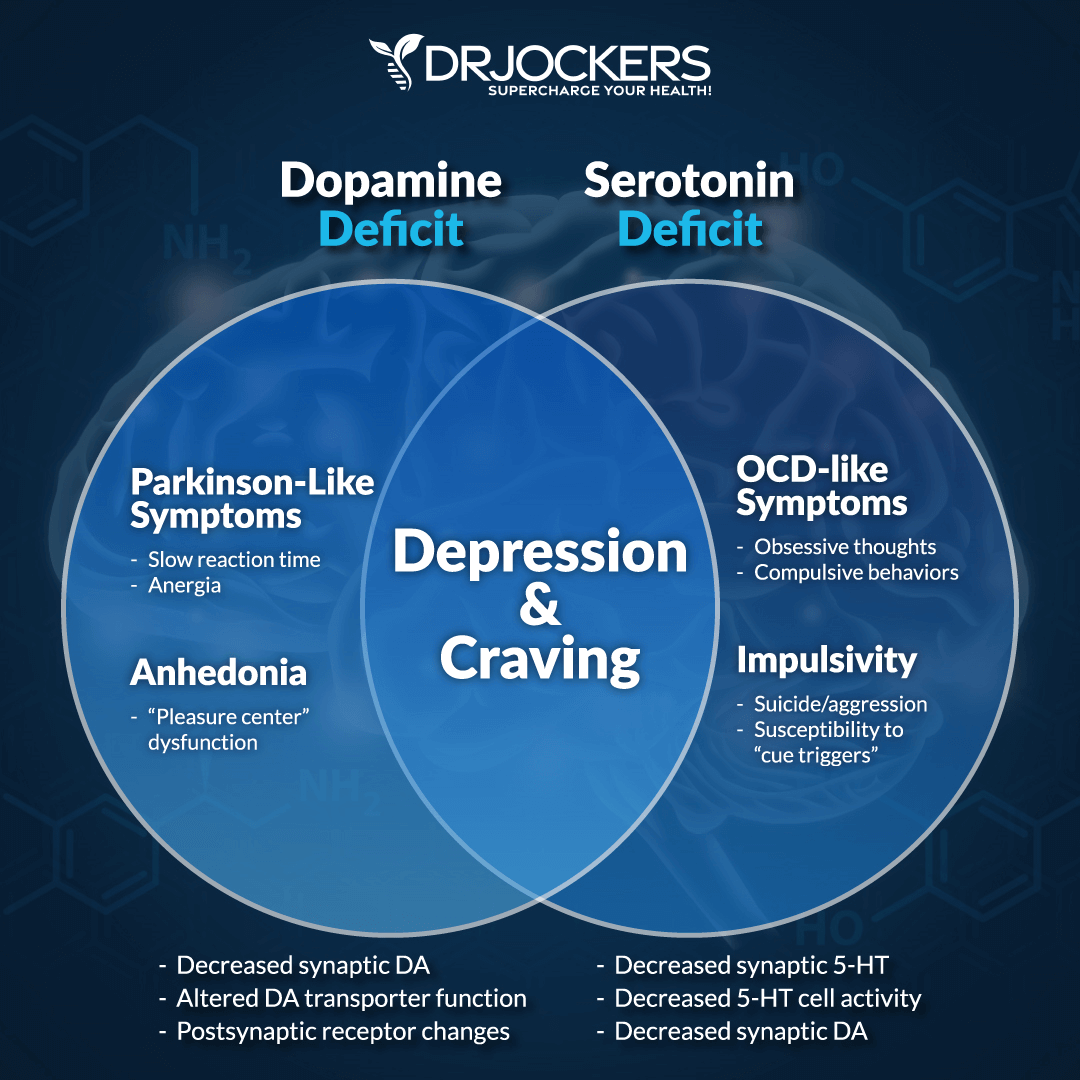
Symptoms of Low Dopamine
Dopamine depletion is classically represented in Parkinson’s disease. Other issues involving low dopamine include schizophrenia, autism, attention deficit hyperactivity disorder (ADHD), and drug abuse. Low dopamine levels that occur when trying to get off of heroin, cocaine, cigarettes, sex, and sugar addictions are why it can be so difficult (3, 4).
Individuals with these addictions display downregulation (reduced production) of dopamine receptors in the region of the brain called the nucleus accumbens. This process has a genetic component, but is produced by the continual usage of the drug or stimulus. The more severe the addiction is, the more blunting of dopamine receptors is present (5).
Dopamine also plays an important part in morning wakefulness as it inhibits the pineal gland’s melatonin-producing effects and shuts off melatonin production in the morning when the brain needs to awaken (6).
Individuals with low dopamine also display increased levels of impulsiveness. A 2012 study using 23 adults was given a hypothetical choice between receiving a smaller amount of money immediately or a significantly larger amount at a later time.
The individuals who made the impulsive choice for immediate money in the initial part of the study later demonstrated less impulsivity and chose to wait for the larger sum after taking a drug that blocks a dopamine-degrading enzyme (so they had more dopamine in their brain) (7).

Dopamine Metabolism:
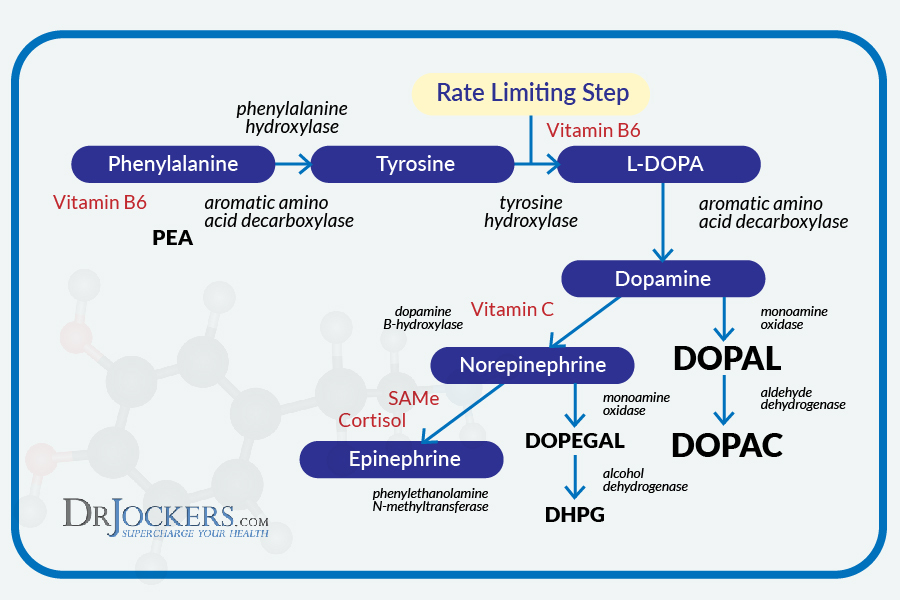
The precursor amino acids to dopamine are L-phenylalanine and L-tyrosine. These are converted to L-DOPA and eventually dopamine with tetrahydrobiopterin, oxygen, iron, and the active form of B6 (pyridoxal-5-phosphate) as the cofactors (8).
Dopamine is also used as a precursor to make the neurotransmitters norepinephrine (Nr) and epinephrine (Epi). Dopamine is converted to norepinephrine by the enzyme dopamine-B hydroxylase with vitamin C as the cofactor.
Nr is converted into Epi by the enzyme phenylethanolamine N-methyltransferase with SaMe as the cofactor. If any of these amino acids or cofactors are low, it will limit the synthesis of these key neurotransmitters.
This conversion of dop to Nr and Epi is very important for a healthy response to stress. Without it, one is more likely to develop addictive behaviors as they have too much dopamine interacting in their system, which can lead to burnout of the receptors.
Problems with Dopamine Metabolism
One could have issues with the 4 major aspects of dopamine metabolism as discussed below.
1) Too Little Production:
It is possible to have too little or too much dopamine production. This is often due to the level of stress the individual is under. In phase I, alarm response to stress, we produce more dopamine and other catecholamines.
In phase II adrenal fatigue, stress hormones begin to plummet. In phase III, when we have adrenal exhaustion, we produce too little because the cells are burned out. Our dopamine-secreting cells can be overwhelmed with stimuli to produce dopamine and begin to shut down, effectively reducing our ability to produce stress hormones on demand.
In addition, when too few precursors such as phenylalanine and tyrosine are available due to low protein diets or, more commonly, low stomach acid and/or leaky gut, then we can have an inability to produce enough dopamine. In addition, low conversion factors, such as a B6 deficiency, can create an inability to produce enough dopamine (8). Also, poor sleep, hypothyroidism, and hypoglycemia will lead to poor dopamine repletion and symptoms of low dopamine.
Additionally, single-nucleotide polymorphisms (SNPs) in some of the critical enzymes involved in dopamine synthesis can result in too little dopamine production. In particular, the ones involved include Tyrosine hydroxylase (TH) and DOPA decarboxylase (DDC) (9).

2) Increased Dopamine Breakdown:
There are some conditions that increase the breakdown of dopamine. Blood sugar instability and insulin resistance have been shown to increase dopamine turnover mechanisms (10).
Additionally, there are certain genetic single-nucleotide polymorphisms (SNPs) that increase dopamine, Nr and Epi turnover. The most common one of these is Catechol-O-methyltransferase (COMT) and Monoamine oxidase (MAO-A and MAO-B), which all speed up the activity of dopamine-regulating enzymes (11, 12)

3) Dopamine Transporter Problems:
The major issue here is with dopamine B-hydroxylase, which converts dopamine to Nr. This can be blocked by toxic metabolites produced by C Diff bacterial overgrowth. Many individuals with addiction problems, ADHD, and autism, etc., have C Diff overgrowth that is compromising their ability to form a healthy Dopamine-Nr conversion (13, 14).
Another issue would be vitamin C and/or copper deficiencies since these compounds are necessary cofactors that work with Dopamine B-hydroxylase to convert dopamine to Nr.
4) Down Regulated Dopamine Receptors:
When dopamine is elevated for long periods, it can cause a downregulation of dopamine receptors. This can be due to addictions, which overstimulate dopamine production and overwhelm the dopamine receptor sites.
Think of the example of loud music. If you aren’t used to hearing loud music, then you are very sensitive to the sound. However, if you are used to the loud music, then you habituate to it and no longer hear it in the same way. This happens with the cells of our body.
Cells have a sensitive threshold to stress hormones. Too much stress hormone activity will overexcite the cells to death. So when we continually flood the cell receptors with these stress hormones, they reduce their production of receptor sites so as to not overexcite the cell.
Addictions lead to down-regulated dopamine receptors, and this is why it can be very challenging to get over addictions. The worse the severity of the addiction, the more down-regulated the dopamine receptors are (15).
Finally, SNPs to dopamine receptors, such as DRD2 gene mutations, can also cause poor dopamine signaling in the brain (16). Magnesium can help improve dopamine receptor activity (17).
Testing For Low Dopamine Levels:
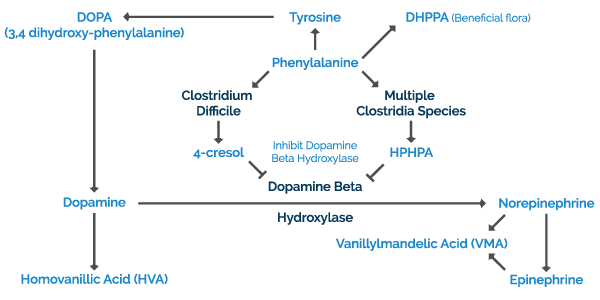
The metabolite homovanillic acid (HVA) is a breakdown product of dopamine metabolism by MAO and COMT. When this is found in high amounts in the urine, it is a sign of elevated dopamine turnover, which is typically due to adrenal fatigue and/or high firing MAO and COMT pathways. Additionally, this can take place with C Difficile overgrowth, where the C Diff binds to dopamine beta hydroxylase and impairs conversion from dopamine to norepinephrine as explained above.
In dopamine-secreting neurons, dopa is metabolized into HVA, which can be measured in the urine organic acid test. In neurons in the peripheral and regions of the central nervous system, and in the adrenal gland, dopamine is converted to norepinephrine by dopamine-beta-hydroxylase. Dopamine-beta-hydroxylase requires vitamin C (ascorbic acid) and copper as cofactors. In the adrenal gland, norepinephrine is further converted to epinephrine. Both epinephrine and norepinephrine may then be metabolized into vanillylmandelic acid (VMA).
When HVA levels are very low, it is an underproduction of dopa, typically due to adrenal fatigue and/or a deficiency in L-phenylalanine, L-tyrosine, and/or vitamin B6. When HVA is high and VMA is low, it is a sign of poor conversion from dopamine to norepinephrine and epinephrine. This could be due to low vitamin C or copper, or due to C Diff overgrowth.

Best Foods For Boosting Dopamine Levels
- Organic coffee
- Raw cacao or minimally processed dark chocolate
- Organic green tea
- Avocado
- Green Leafy Vegetables
- Beets
- Nuts & Seeds
Be careful not to overdo the coffee or dark chocolate, as they can be addictive and can lead to adrenal fatigue and neurotransmitter receptor downregulation if used too much. I would limit consumption to 1 tsp of cacao powder or 2-4 oz of a dark chocolate bar and no more than 8oz of organic coffee daily.
In addition, be sure to consume vitamin C-rich foods such as citrus fruits and green veggies throughout the day or take extra vitamin C supplementation to make sure we are converting dopa to Nr.
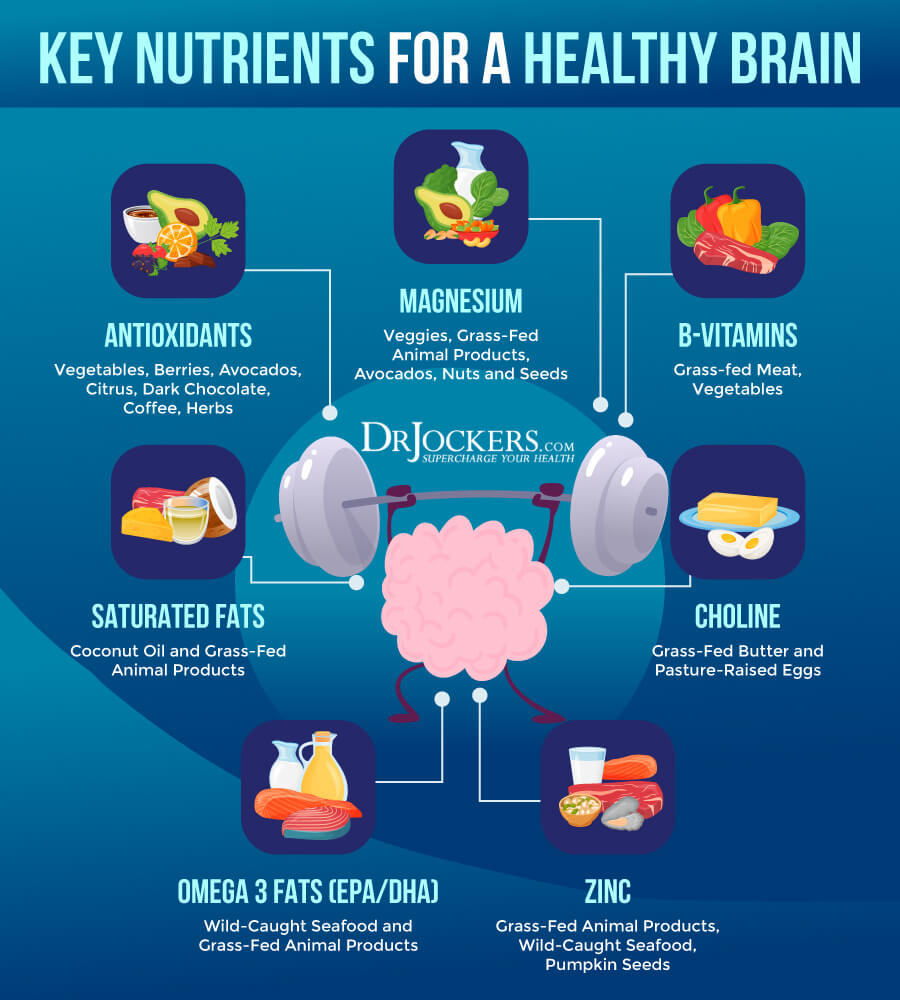
7 Strategies to Raise Dopamine:
For the body to manufacture dopa, we need good stomach acid and digestive function to break down proteins into amino acids so we can absorb L-tyrosine and L-phenylalanine. In addition, we need proper amounts of iron, copper, zinc, vitamin B6, and magnesium. If we are deficient in these nutrients, we will not be able to produce adequate amounts of neurotransmitters.
- Adapt to Stress Better: Chronic stress will deplete your dopamine levels. Find things to be grateful for, practice deep breathing, listen to enjoyable music, get regular sun exposure, find ways to laugh, and find other stress management strategies to help reduce stress and become more resilient.
- Anti-Inflammatory Diet: Be sure to follow the anti-inflammatory nutrition plan using real and organic foods in order to provide the right nutrients to support healthy neurotransmitter function. In particular, consuming foods rich in good fats such as coconut, avocados, grass-fed butter, and olives can be helpful. Getting a lot of phytonutrients from fruits, vegetables, and herbs is important as well.
- Sleep Better: It is key for you to prioritize sleep if you are going to improve your dopamine levels. Sleep improves neurotransmitter production and receptor activity. When we sleep, our brain flushes out the neurotransmitters, repairs receptor sites, and regenerates neurotransmitters to be used the next day. Follow the strategies in this article to help you sleep better.
- Improve the Microbiome: Consume fermented foods, anti-microbial and carminative herbs such as garlic, onions, oregano, basil, thyme, peppermint, ginger, etc., to help improve the overall constitution of the gut microbes. Remember, C Difficile overgrowth is a major player in poor dopamine metabolism, so the better you take care of your gut microbiome, the more you will reduce C Diff and improve neurotransmitter metabolism.
- Set Goals: Making healthy goals in relation to your career, relationships, spiritual, emotional growth, and physical health can all improve dopamine levels. I recommend making goals that challenge you but are achievable. The act of challenging yourself and accomplishing the goal will do wonders for your neurotransmitter metabolism. If you are a creative individual, try creating something that interests you. This could be a painting, writing a poem or an article, building something with your hands, making a meal, etc.
- Small Tasks: One of the best ways to boost dopamine if you are deficient is by giving yourself very small, but important tasks to do. This may as simple as taking the trash out or making your bed. Accomplishing small, but important tasks will help to stimulate better neurotransmitter release and give you some momentum for larger tasks.
- Regular Exercise: Regular movement is good for all neurotransmitters. Individuals with adrenal fatigue and low dopamine should be doing low-intensity movement, such as walking or yoga, and doing lots of deep breathing. If you are in good condition, but are looking to boost your dopamine levels for high performance, then I recommend high-intensity resistance training and interval sprints, which will give a significant boost to dopa production and utilization.
Some of the other things that will help include listening to enjoyable music, getting out in the sunshine, and laughing. Practice these things daily!
Best Dopamine Boosting Supplements:
L-Tyrosine: This amino acid is a precursor to dopamine. For boosting tyrosine, take dosages between 500-2500 mg on an empty stomach.
DL-Phenylalanine: This dosage can be between 1 – 2 grams on an empty stomach.
Vitamin B6: Best dosage is between 50-100 mg taken 2 times daily with or without meals.
Rhodiola: Best to be taken 1-2 times in a dosage of 100-200 mg each time.
Cordyceps: Best to be taken 1-2 times in a dosage of 400-800 mg each time.
Both rhodiola and cordyceps are called adaptogenic herbs. Adaptogenic herbs help to buffer the negative effects of stress and allow our body to accurately adapt to stress. They are able to help increase catecholamines (Dopamine, Nr, Epi) when they are low, but also lower them if they are shooting up too high.
This is very important because we don’t want to overshoot our catecholamine production, or we risk burning out the adrenals and causing dopa receptor dysfunction. Rhodiola and cordyceps have the strongest effect on modulating dopa levels. Some other great adaptogens include ashwagandha, ginseng, holy basil, and reishi mushroom, among others.
These should be used in addition to amino acids (L-tyrosine and DL-phenylalanine) when working with dopamine levels.

Dr. Jockers Strategy
For individuals with low dopamine, I focus on blood sugar stability, stress reduction, and adaptation strategies, and look to improve thyroid if it is a problem. If I see elevated C Difficile on lab testing, we will use anti-microbials and probiotics to reduce the levels.
We do a low-carb diet, but will use dark chocolate, organic coffee, nuts, and seeds, so long as they aren’t dealing with an autoimmune disease. I use both of the following supplements to help individuals with low dopamine. I will also typically include Brain Calm magnesium, which crosses the blood-brain barrier and improves overall receptor function, and plays a huge role in modulating stress hormone production and allowing it to be used most effectively.
Adapt-Strong: This formula provides clinical dosages of vitamin B6, rhodiola and cordyceps. This formula provides useful support for both hyper- and hypofunction of the adrenals. Hyperfunction is when the adrenals are overproducing hormones, such as cortisol, and hypofunction is the opposite, when the adrenals are underproducing.
Normal Dosage: Take 1 cap – 2x daily
Advanced Dosage: Take 2 caps – 2x daily
Dopamine Plus: This formula contains clinical dosages of L-tyrosine, DL Phenylalanine, vitamin C, and B6, and it contains 5-HTP, which helps keep the dopamine-serotonin balance in order. This product helps improve focus, concentration, and reduces cravings for sugar or other addictive behaviors.
Normal Dosage: Take 2 caps – 2x daily away from meals
Advanced Dosage: Take 4 caps – 2x daily away from meals
Common Question:
Can I Take the Adapt Strong with the Dopamine Plus?
A: Yes, the only overlapping nutrient is B6, and based on my experience and research, this water-soluble nutrient is very low in most people with lower dopa symptoms and if you were to get too much, your body would urinate it out.
What is the best dosage to begin with of these supplements?
A: Begin with the normal dosage, and if you don’t notice anything or begin feeling good, you can experiment and go up to the advanced dosage. If you feel poorly on the normal dosage, take 3 days off and then take ½ of the normal dosage and see how you do.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. On our website, we offer long-distance functional health coaching programs. For further support with your health goals, just reach out and our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!










Thank you for this very insightful write-up. With all the distractions and demands of our daily lives, it is easy to experience a dip in dopamine levels. I quoted you from my “Get Sleep” segment. Thank you again!
Great! Thank you Kat!
My friend was given dopamine for restless legs, but maybe instead she needs a higher dose of Amour thyroid and Mg and other minerals/no gluten. Dopamine is made in the gut lining. No gluten may help minerals absorb and help make Dopamine in the gut lining.
Yes definitely avoid gluten and increase magnesium intake. Also spend more time in the sunlight if possible, especially in the morning when it comes up.
Thank you for your great information. I’m 55 and based on the symptoms beginning to realize that I have probably had low dopamine levels for much of my life. I also have an uncle, my mother, and a few other more distant relatives on that side of the family who have been diagnosed with Parkinson’s Disease. I have been a big fan of coconut oil over the last few years but am seeing some conflicting info regarding it’s use and dopamine. Some say it is quite good for increasing dopamine while others say that saturated fats dull dopamine reception. Please help clarify. Thank you.
Hey jeffrey, good question. Many of these studies did not control for carbohydrate intake. So high saturated fats and high carbs would have a negative effect. However, lots of saturated fats, especially from coconut oil, along with a ketogenic or low-carb diet would be beneficial.
Thank you so much for this insightful and informative article. I’m a mental health therapist and treat many persons suffering from addictions. Personally, however, my father died after a 10 year battle with PD and I have been diagnosed with RLS since 19! This article streamlined an enormous amount of info, often conflicting, into a work of art! I will reference all the info in therapy sessions, as well as my own life and health! I cannot thank you enough!
Wow! Thanks for reading Dana!
Is it common knowledge among MH and addiction therapy that serotonergic drugs can cause cravings and addiction to alcohol, gambling, etc? SSRIs downregulate and/or interfere with dopamine signalling. They also cause suicidal depression in some people (as stated in the Prescribing Information), also thought to be due to interference with dopamine, causing akathisia. Pharma paid the FDA to keep the term “akathisia” out of the PIs. (ref: Jay Cohen MD).
I worked in psychopharmacology for several years and those dangers were kept very hidden, but are a bit better known now.
Thanks so much for sharing this!
In the case of c-diff interfering with the dopamine beta hydrolydroxylase enzyme, what would be the best approach to assist the conversion of dopamine to norepinephrine and epinephrine while working to get rid of the C diff at the same time?
Hey Sally, using Vitamin C and SAMe could potentially help but there is not much evidence on this specifically. Following the strategies in this article may be helpful as well: https://drjockers.com/25-lifestyle-strategies-to-heal-adrenal-fatigue-naturally/
That’s a lot of b-6 to take! Those with the MFTHR gene should be extremely careful taking high amounts as their body does not excrete it out. I was taking B-6 for 2 years (50mg) and started having MS symptoms. I had numbing and tingling in limbs, slurred speech, vision problems, internal body vibrations, and limb weakness. I had a MRI and it showed no MS. Later on I read a book on PMS and hormones and it happened to talk briefly about b-6 given to patients for PMS. Some experienced MS symptoms. I immediately knew this was my answer and I came off of the b-6. I had my levels checked after 6 months free and it was still extremely high at 56. I no long have MS symptoms thankfully and it took 3 weeks of no b-6 for things to get better. Please be careful with it! It can cause permanent damage. There are many others who have experienced this as well and many Facebook groups to discuss healing.
Thanks for sharing Lisa!
I believe I have a capilary inflamation problem, associated with autoimmune disease. It usually affects my scalp, neck and facial areas. Fluids build under the surface of these loose skin areas. So, you say to refrain from nuts, but I know that a diet with them is very good. And dopamine should increase with them. Would you suggest the supllements from this website instead, of a variety of nuts?
I would start here Ronald: https://drjockers.com/reduce-autoimmunity/
Many people do not tolerate nuts well!
What type/form of magnesium will help the dopamine receptors help and repair?
Hey Shawn, the best for the dopamine receptors is the Brain Calm magnesium here: https://store.drjockers.com/collections/top-sellers/products/brain-calm-magnesium
Hi and thanks so much for this article ,, i have been battling with porn and masturbation for so many years now , i have tried in quting so many times but i end up relapsing even after i start seeing benefits ,, i dont know what to do anymore , i have got pretty much every dopamine, serotin deficiency symptoms i have ever read about ,,, what supplements do you suggest i start taking since i am on another streak of qutting PMO .. thanks and i look forward to your reply
Hi Pace, I am sorry to hear that you have been battling these addictions. I would recommend that you find a functional health practitioner that can recommend specific testing and help you understand neurotransmitters that may be imbalanced to help you navigate your health journey. These articles can help: https://drjockers.com/functional-nutrition-tips-to-find-a-great-health-coach/ & https://drjockers.com/low-serotonin-levels/
i can relate to you..i tried what you tried more than a decade ago and it didn’t work, so finally, i asked God, i can’t do it , help! and since then my erg was gone and all i have to do is not gaze at walking butts.. hahaha
Pace, as a natural health care professional, I would remind you we are body mind and spirit. These are not separate departments of our being; they are inextricably intertwined in ones make up. So grateful for dr Jockers ministry addressing the physiological aspect of your challenge. It is an absolute piece of the puzzle. My husband spent decades helping men overcome the addictions you struggle with and more. One tool he utilized….. in combination with what Dr Jockers addresses, is a ministry called Pure Desire. Believe you can find them online…. Maybe in your own community.
Excellent article Doc…
Can I use the following supplements (1) Brain Calm magnesium, (2) Adapt-Strong and (3) Dopamine Plus, if my low dopamine levels/receptors are due to porn induced erectile dysfunction (pied) due to excessive porn consumption over 20 years?!
I watched so much porn over the years that I can’t even maintain an erection watching porn let alone with real women.
Will these supplements in your article above help me fix my dopamine receptors and cure my psychological erectile dysfunction and low motivation?!
Kind regards,
Zak from the UK
For more information on PIED please visit the following reputable website…
https://www.yourbrainonporn.com/
Hey Zac,
Yes this protocol will help your brain and body heal from the over stimulation. Praying for you!
Is screen/internet addiction a contributor to low dopamine?
Yes absolutely!
Excellent article! The best I have read about dopamine. So thorough! Thank you so much! xo
Thank you!
Unfortunately, my lifetime of crisis/stress/ADHD (more like ADD at age 66 … lol) & being the ‘family’ ROCK finally caught up with me. After a BAD fall in 2016 that physically & mentally impacted my life I’ve been in depression. I can’t take ANY antidepressants, I’ve tried them ALL & they make me crazy! Consequently I have NO options available to help me which is even MORE depressing. I’m tired of living like this & was ready to give up until I saw YOUR info on Pinterest‼️Can your products successfully level the brain chemicals or hormones that cause depression? I’ve had two bad concussions, one at age 14 ice skating (front brain) & the 2nd one was a serious fall (the back of my head hit a tile floor & I lost consciousness) & I’ve had to research brain info to help overcome issues associated with PCS (Post Concussion Syndrome). I was also wheelchair bound for 5 mths & gained a lot of weight that I can’t seem to lose. Please Advise …
So sorry to hear about this! Here is a helpful article on Concussions https://drjockers.com/concussion-protocol-symptoms-and-healing-strategies/
I am not a physician, but have worked in psychopharmacology for many years.
Most antidepressants target serotonin and deplete or dysregulate dopamine. After decades of serotonin drugs (given for mild fatigue only initially), I developed movement disorders with severe muscle pain (dystonias), rhabdomyolysis, drug-induced lupus, adrenal exhaustion, brain injury (per MRIs), and became permanently disabled in my 30s.
After all of that, my doc tried an ADD drug and it was the first I felt somewhat normal in decades. I’m not fond of pharmaceuticals, but supplements just haven’t gotten me to a level of being able to function after all of the damage by pharma.
I just found Dr. Jockers and hope he may have more input about rx drug induced brain injuries/dementing processes.
When using free-form amino acids, it you have gut dysbiosis, you may find the oral route doesn’t respond well to the intake. I have found that many of these are pleasant-tasting and can be taken sublingually for better absorption and faster response time.
Always begin with low dosages and work up from there. In fact, I would recommend using this as an initial test to see if that amino acid helps – you know within a few minutes if it begins to help you feel better. Use aminos at different times than protein and vitamin C for best results. If you ‘test’ an amino and you feel worse, take a dose of vitamin C to help reduce the discomfort.
A great doctor, and a great man.
Thank you David!
I appreciate you breaking everything down and the detailed explanations. Exactly what I was looking for. Truly educational. Excellent work Doc!
Thank you!
Hi Dr. Jockers,
A deep heartfelt thanks for all that you do to educate people on living their best life possible! My question is about Tyrosine and a mechanism by which it apparently inhibits insulin secretion in the stomach. I have 2 wild type COMT SNP’s . Supplementing with Tyrosine has been a god-send, but I have issues regulating blood sugar levels. Can you offer any advice to counteract the affect on insulin down regulation?
Would these supplement mentioned in article be ok to take as I am on a 5mg dose of lexa pro?
Yes these supplements should be just fine but it is always best to discuss medications with your physician.
Can doing coffee enemas help improving dopamine as drinking it? Thank you?
Yes they can help by improving gut health and detoxification.
Are you familiar with any supplements to take for support while tapering off Wellbutrin ?
I would like to know what the dosage levels would be for a child. Many of the strategies are aimed at adults. As a teacher I’m always looking for better ways for children with ADHD and information to share with parents on this journey.
Hello Connie, for children, we like to use probiotics and the NDF Calm here https://store.drjockers.com/products/ndf-calm
“The individuals who made the impulsive choice for immediate money demonstrated less impulsivity and chose to wait for the larger sum after taking a drug that blocks a dopamine degrading enzyme.”
What? Does anyone proofread?
I am being followed for possible PD and will likely have a DAT brain scan for this soon. What do you know about, and what is you opinion about that test? Also, are there any blood or other types of lab tests one can do to determine dopamine levels? And if a traditional physician would not offer to do these, who would and how do I arrange how to get them done? Thanks!
I was surprised not to see beef on your list of foods. It is the #1 source of Tyrosene, which you say is the precursor of dopamine. With my Sz adult daughter, it’s so important to use foods as medicine! I wonder if you have an anti-meat bias? I should also add, I source most of my meat from a Guernsey, 100% grassfed local farm. This farming is regenerative, adds to the ecosystem, nurtures wildlife and improves the soil including CO2 capture.
That is fantastic! So glad you are getting regeneratively farmed grass-fed beef!
Thank you for this article. My husband has just been diagnosed with Parkinson’s and is finding it very hard to deal with it. The medical profession doesn’t know enough about it and I feel much better trying natural medicine first. Considering dopamine is the main problem here could your supplements help?
Hello Evi, very sorry to hear about this! Yes, here is a detailed article on Parkinson’s for you to review: https://drjockers.com/parkinsons-disease/
I have the mthfr genetic mutation and I was taking b6 separately from my multivitamin and I have peripheral neuropathy. I don’t have diabetes. The 3rd neurologist Checked my b6 level and it was four times what it should be. It was rechecked after stopping the b6 but I still have the neuropathy. It is a water soluble vitamin but it can be harmful if overdosed. I found out the hard way. I don’t want others to suffer like I do. Usually the doctors check b12 levels but it took the 3rd neurologist to discover this. Be careful when taking high doses of anything.
What are your thoughts on using directly the L-Dopa molecule (L-DOPA 98% (from Velvet Bean Extract), let’s say 1-2x a week along with the other precursors that you recommend?
Yes that can be helpful!
Very interesting, easy to read, and fine helpfull drawings. Today especially helpfull by the writing about Dopamine, as my wife probably suffer from Parkinson’s. Told so by neurolog 3 month ago, not by measure, but by her walking, and a bit with hand, and sleeping problem. I own 11 books about Parkingson’s disease, among around 600 health and doctor books.
But the problem is that nearly all of the doctors knows nothing about vitamins and minerals, which I want to connect to either L-dopamine, or Mucuna pruriens, instead of the bad drug the neurolog has put her on.
As a remark. Some also use the B1, 200 – 5,000 IU, which an Italian doctor found out to use.
Very informative article, thank you! Can Adapt-Strong and Dopamine Plus be used to wean off Adderall? Any other supplements recommended or articles written on this topic?
They can be helpful, but it is always advisable to work with your physician or functional health coach when coming off any meds. Here is another helpful article: https://drjockers.com/adhd/
What about taking Sam-e? Would this help with seratonin or dopamine or both?
There was once an NIH article on using sam-E for adolescents and now I can’t access it.
Would you recommend your dopamine supplement for an adolescent?
It may help, but it would be wise to work with a functional practitioner when using SAMe. For a dopamine supplement, check out our Dopamine Plus: https://store.drjockers.com/products/dopamine-plus
Hello, could you please share what the relationship is between cortisol and adrenaline, as shown in the diagram above?
Doctor Jokers,
do you think it is possible that with low cortisol in the evening blood sugar drops, this raises adrenaline as a compensatory mechanism and in fact the seemingly low cortisol actually leads to insomnia and falling asleep in the wee hours?
Yes it is possible, although typically it is high cortisol in the evening.
thank you so much Dr.Jockers
I’m a Phenylketonuria (PKU) carrier with a snp that causes a mis-folded protein which has low affinity to bind to BH4 – so top end of normal phenylalanine and bottom end tyrosine on my organic acids test. Recent research suggests carrier status can also lead to a higher level of phenylalanine, not just PKU, which I’d suspected given my and my Dad’s symptoms. Is there anything I can do to improve my dopamine level given this genetic bottleneck? Thanks.