Is Your Gut Bacteria Making You Fat?
Did you know that your gut is interacting with bacteria every day to do more than help you digest food? The gut is so unique to every individual that scientists are only recently becoming more aware of the existence of a complex network of nerves that line our stomach and gut and is referred to as the second brain. Bacteria are so crucial to maintaining healthy gut functions that evidence exists of an animal’s altered biological state when exposed to bacteria-free environments (7).
A diverse number of bacteria colonize the gastrointestinal tract including the mouth, stomach, and intestines. Mostly contained in the intestines, bacteria provide an arsenal of tools for the gut to interact with. Depending on the type of bacteria available, some bacteria may serve as an ally in combating pathogens from entering into the human body while other species may be the perfect weapon of choice to make you fat.

The Host and Gut Microbiota Relationship
The environment contained in the intestines which inhabit bacteria is known as the gut microbiota. Ideally, when there is both abundance and diversity of healthy bacteria, these friends of our gut are able to outcompete pathogenic bacteria for space.
Working as a team effort, a healthy gut microbiota acts as a defense system for the host by destroying both toxins and carcinogens, supporting the synthesis of vitamins, improving the ability of the body to digest and absorb nutrients, and regulating a healthy immune system response from distant and neighboring organs. (4)
Is your Gut Hosting Friends or Foes?
Over 1000 species of bacteria are known to colonize the gut (4). Numerous factors contribute to whether or not your gut microbiota is currently hosting protective bacteria which will benefit your health or harmful bacteria and a state of dysbiosis, which may be the source of many of your health concerns.
Although some of these variables are not within your control, simple lifestyle changes can significantly impact the gut microbiota and improve your quality of life. The following factors can affect the gut microbiota and promote either health or disease:

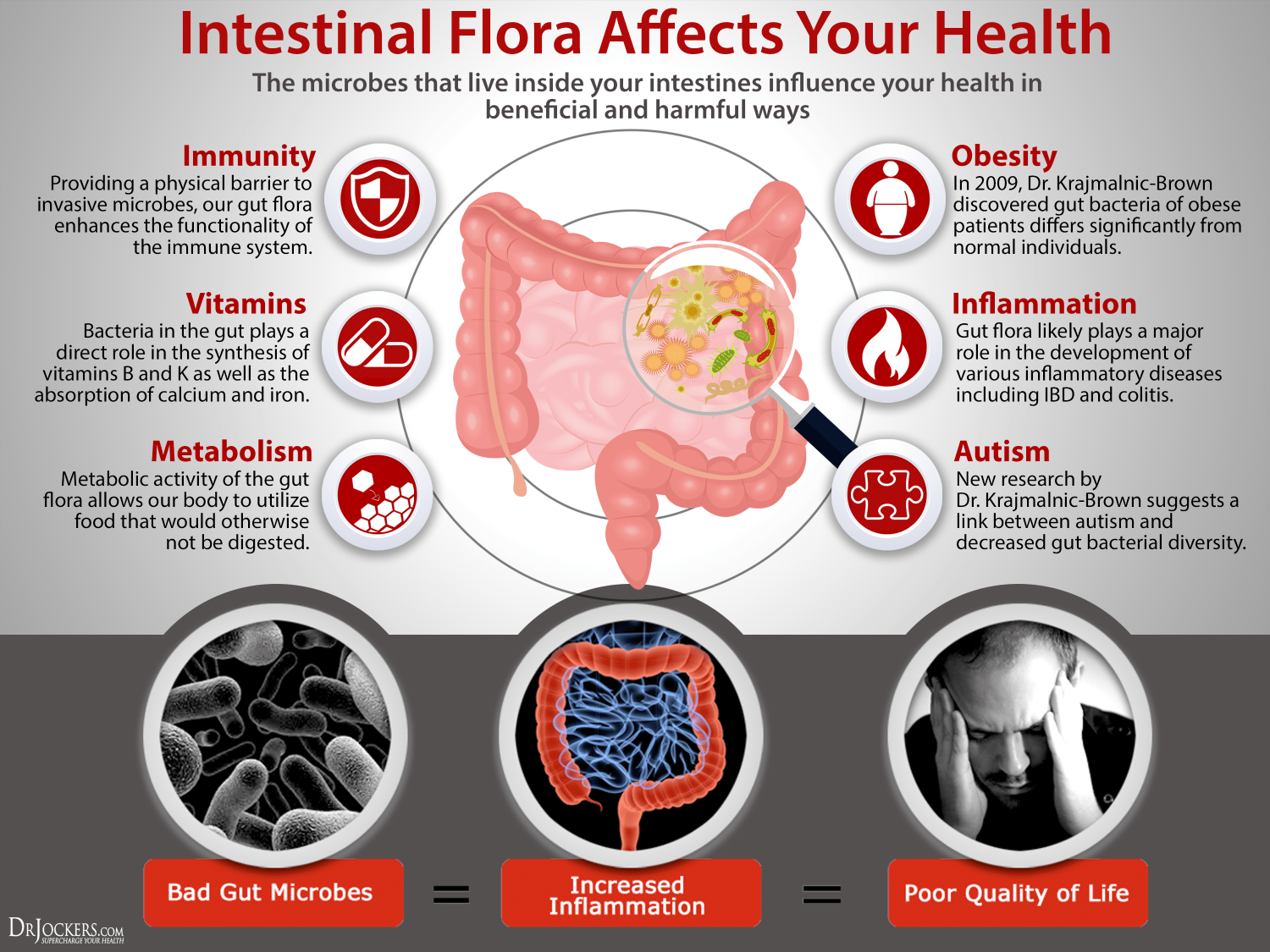
Obesity: A Symptom of Poor Gut Health
The obesity epidemic today has generated attention from various fields of research given its association with various diseases and cancer. As it turns out, if you are overweight you are likely harboring destructive bacteria species.
The World Health Organization predicts that almost 3 million people will die from obesity across the world by the end of a single year. (3)
An Imbalance of Healthy Gut Bacteria
There are over 100 trillion microbes that live on and in the human body. Most of these microbes take cover in the gastrointestinal tract. Accounting for 98% of the gut microbiota, Firmicutes and Bacteroidetes are two protective types of bacteria that are receiving the spotlight for their relationship with weight concerns.
Studies have found that the higher the ratio of Firmicutes to Bacteroidetes, the higher the risk of obesity (3, 6). (7)
Firmicutes
Firmicutes appear higher in concentration when an individual is consuming a high fat diet. Researchers propose that the bacteria species categorized as Firmicutes are very efficient at harvesting energy from food. For example, newborns who breastfeed have high concentration of Firmicutes in their developing microbiota. In the case of newborns, the population of firmicutes in the child’s microbiota is most necessary for the nourishment of organs, especially the brain which is primarily composed of fat. (6)
Evidence supports that an increase in the dietary intake of fat and reduction of beneficial fiber results in an array of health concerns as an individual ages and no longer has the high fat nutritional requirements. High fat, low fiber diets are known triggers of inflammation and can increase the permeability of the intestines (3). Chronic inflammation which results from an altered gut microbiota not only leads to obesity but may be responsible for the development of insulin resistance and inflammatory bowel diseases (6).

Bacteroidetes
Crohn’s disease is one type of inflammatory bowel disease characterized by a chronic state of inflammation of the gastrointestinal tract. Bacteroidetes have been studied in patients with Crohn’s disease to effectively reduce the state of inflammation and manage symptoms. Contrary to the effects of Firmicutes, Bacteroidetes actually prevent increased fat storage. (4)
Bacteroidetes Support A Healthy Immune Response: In fact, Bacteroidetes are so helpful to the maintenance of our gut health that these types of bacteria are the first to colonize the gut of a newborn (6). Eager to occupy space, these bacteria aid in the development of the baby’s gut and play a key role in developing the immune system.
Bacteroidetes help regulate the response of the body’s defensive T-cells which hunt down and destroy pathogens. (7)
Bacteroidetes Produce Organic Acids: Organic acids are required by the body for numerous benefits. Some of these benefits include absorbing water and regulating pH in order to prevent the colonization of destructive bacteria and pathogens (4). Bacteroidetes are key players in synthesizing one major type of organic acid known as butyrate.
Butyrate is responsible for the circulation of blood flow in the intestines and for its ability to increase the availability of electrolytes for absorption (8). Along with maintaining everyday health of bowel function, butyrate is also believed to protect against the growth and spread of tumors and may prevent colorectal cancer (7).
Improving Gut Microbial Balance:
Improving the balance of good bacteria in your gut is necessary to promote the normal function of your gut and your overall health. Although Firmicutes and Bacteroidetes are both considered friendly bacteria, your focus should be on welcoming Bacteroidetes in greater numbers than Firmicutes. How can this be accomplished?
Polyphenols
Polyphenols are micronutrients that are also associated with the prevention of disease and cancer for their antioxidant properties. Polyphenols have also been studied to promote the synthesis of organic acids by improving the balance of Firmicutes and Bacteroidetes in the gut microbiota (4). Consume more foods rich in polyphenols. Some examples include:
- Cocoa powder
- Berries such as elderberry, blueberries, raspberries and strawberries
- Dried herbs and spices including peppermint, cloves, oregano, rosemary, spearmint, thyme, and sweet basil
- Some nuts especially hazelnut, chestnut, and pecan nuts
- Vegetables like spinach, onion, broccoli, and asparagus
- Green and black tea
- Coconut Flour

Fiber
Along with polyphenols, fiber is a functional food that improves the activity of healthy bacteria in the gut. Undigested carbohydrates found in fruits, vegetables, and nuts serve as an excellent food source for friendly bacteria such as Bacteroidetes (4).
Gut health is so greatly influenced by bacteria that changes in our nutritional habits significantly impact the activity of healthy bacteria in the gut microbiota. This strong influence is observed in the contrasting gut microbiota of people who consume animal-based diets compared to those who primarily consume a plant-based diet.
Individuals with a high intake of meat, eggs, and cheeses and low fiber content have an abnormal gut microbiome with reduced levels of fermentation. Researchers also found that people consuming high amounts of animal fat also had an increased risk of pathogenic bacteria believed to be a direct correlation with increased iron consumption.
Those consuming higher plant-based prebiotic fiber in the form of fruits and vegetables were observed to have an abundance of healthy bacteria in their guts. (4)

Antibiotics Devastate Gut Health
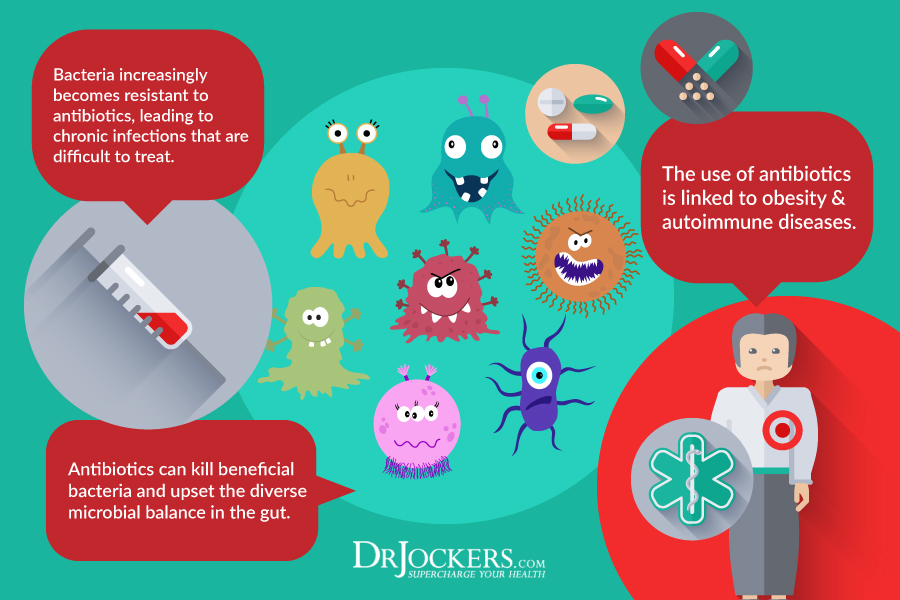
Unfortunately, consuming a healthy diet that feeds good bacteria is not the only strategy to deter the growth of harmful microbes. In a culture stricken with the belief that antibiotics are essential to a healthy lifestyle, developing research might prove that antibiotics may be doing more harm than good.
An abundance of evidence supports that the use of antibiotics, especially when taken orally, devastates our internal defense system. Healthy bacteria become depleted resulting in nutrient malabsorption which may actually promote weight gain. Bacteriophages are also prone to destruction from antibiotics and weaken the immune response to detect and remove pathogens from the body. (2, 6, 7)
One highly antibiotic sensitive bacterium species is known as Oxalobacter formigenes (2). This bacterium is responsible for breaking down oxalates in the body which can accumulate and form kidney stones. Researchers observed that some bacteria are not capable of repopulating the gut microbiota following only 4 weeks of antibiotic use (2). As a result, antibiotic use increases the likelihood of developing secondary infections.
Antibiotic Treatment and the Microbiota
When the gastrointestinal tract opens up vacancy for other microbes to colonize after the good bacteria are reduced in number, the gut microbiota is susceptible to increased pathogens. To simplify, bacteria bind to the intestinal tract and when protective bacteria are not occupying space, harmful bacteria are able to outcompete their opponents for a home.
Continued antibiotic consumption over time allows the harmful bacteria to thrive and increases the likelihood of hosting antibiotic-resistant bacteria and pathogens in the gut (2). Researchers have found that reduced diversity within the gut microbiota is associated with an increase in intestinal infections caused by E. coli and Salmonella. One study even found that one antibiotic treatment used to treat tuberculosis resulted in a 90% reduction in the bacteria population 12 hours after treatment. (2)
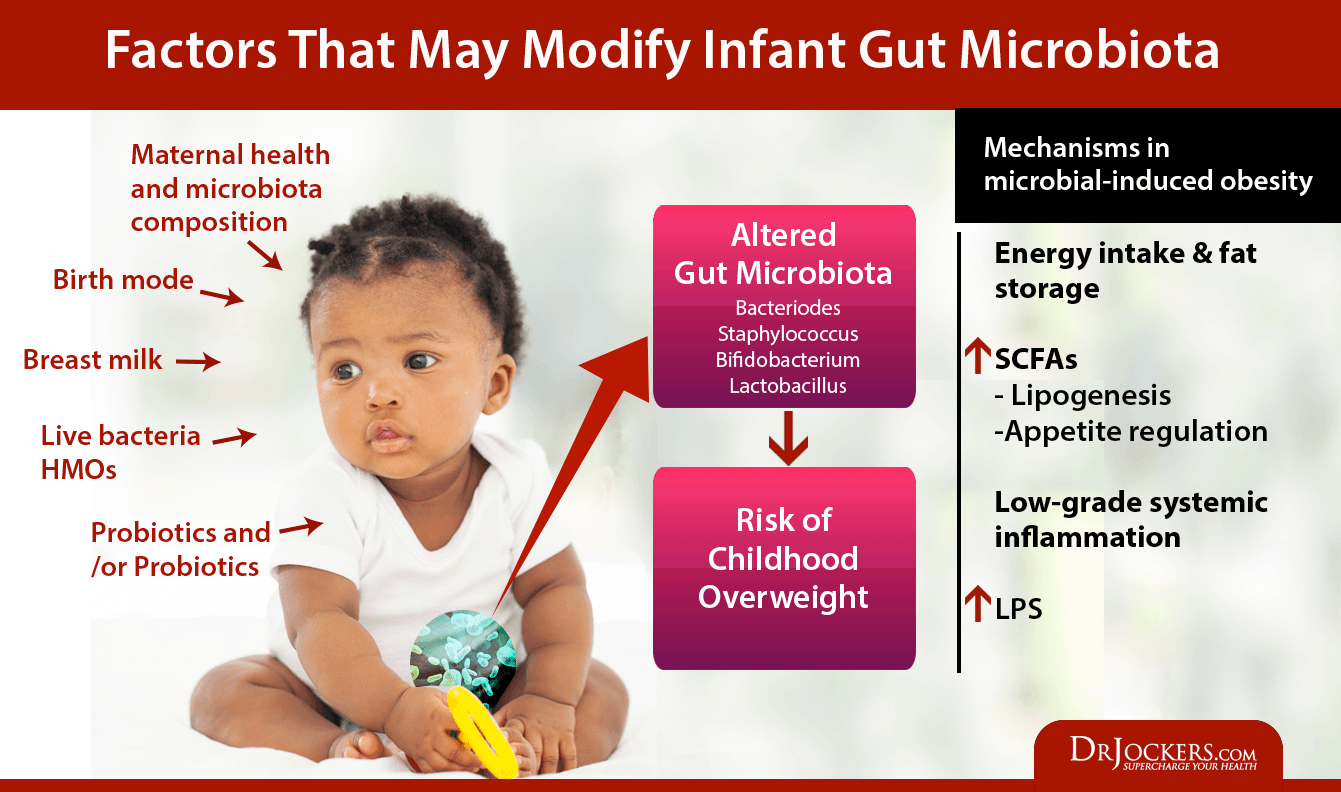
Maternal Health Affects Risk of Obesity
Several factors have been linked to increasing a child’s risk for obesity and they begin with mom’s health and lifestyle choices including birth mode, ability to breastfeed, exposure to antibiotics, and nutritional supplementation of probiotics and prebiotics.
All of these factors have been determined to affect the environment of a baby’s gut and can promote metabolic factors resulting from inflammation and lead to a higher risk of childhood obesity.
Birth Mode:
How a baby is born impacts his or her health. A vaginally delivered baby is able to pick up microbes that reside along the birth canal. The baby’s first gulp following birth is more likely to be full of healthy bacteria that are contained in the amniotic fluid.
These bacteria are known to aid in digestion. A baby delivered by cesarean section (C-section), does not come into contact with these helpful bacteria and instead is first covered in bacteria that live in contact with the skin. (4, 6)
Breast Milk versus Infant Formula:
Infants fed formula instead of breast milk may be at a higher risk of getting a bacterial infection and are at increased risk of developing childhood obesity. Breast milk contains healthy bacteria known to aid in the development of the baby’s digestive tract and immune system. Studies show that breastfeeding the first 6 months of a newborn’s life has been found to decrease obesity later in life. (6)
Breast milk has also been found to contain oligosaccharides, a source of fiber, and helps to maintain a healthy intestinal pH necessary to inhibit pathogens. The benefits of nursing mothers supplementing their diets with probiotics and prebiotics are further passed on to the newborn. In fact, this research also suggests that healthy bacteria that reside in a mother’s gastrointestinal tract are capable of passing the digestive barrier and can be found in her breast milk. (6)
Utilizing a mother’s natural capability to feed her infant provides the baby with a healthy supply of bacteria which will help him absorb nutrients, regulate appetite, control satiety, and contribute to the overall support of gut health.
The Promise of Bacteriotherapy
Bad bacteria can live and dominate the intestines which can result in symptoms ranging from fatigue, pain, chronic illness, and obesity. Scientists have learned that transplanting stool from lean, healthy donors can actually be used to treat sickness.
Called one of the top medical innovations in recent years, fecal microbiota transplantation is currently used with a 90% success rate in curing an antibiotic-resistant bacterial disease known as Clostridium difficile (C. diff) (2). C. diff is one of the most common hospital-acquired infections in the United States affecting over 500,000 Americans annually and killing 14,000 (1).
Promising research continues to show the benefits that occur when a lean donor’s stool is transplanted into a sick patient. Protective bacteria are introduced and allowed an opportunity to overwhelm the pathogenic bacteria and can therefore cure illnesses that originate from an unhealthy gut microbiome. The success of bacteriotherapy may one day serve as an effective means for treating obesity.
Prevent Your Bacteria from Making You Fat
Unfortunately, fecal microbiota transplantation is not yet a strategy in which you can opt to be a part of weight loss. In the meantime, what can you do to prevent your gut bacteria from making you fat?
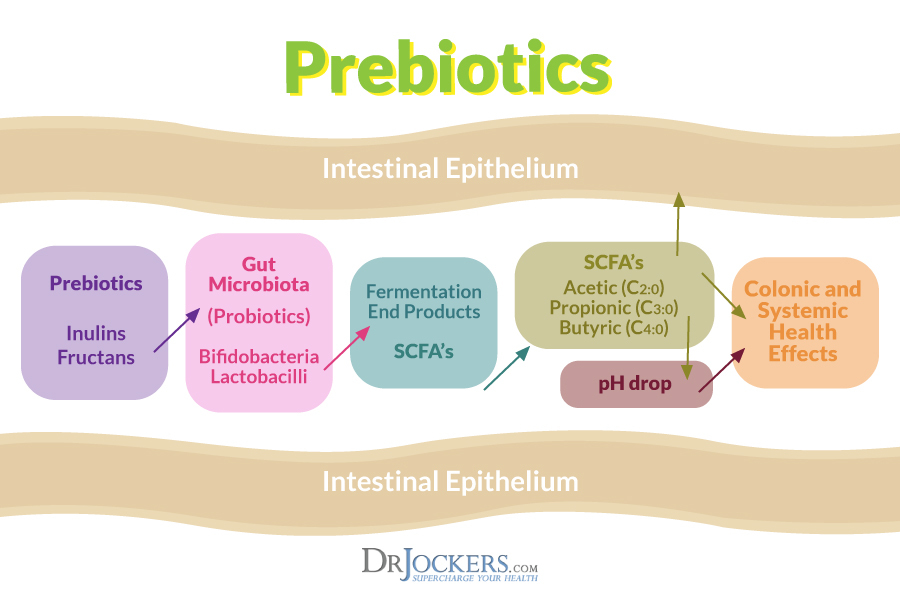
Probiotic & Prebiotic Use: A good probiotic will add small doses of healthy bacteria into the gut microbiota. With the support of prebiotics, the protective bacteria in your gut can proliferate and help you get rid of that stubborn belly fat. Just like probiotics, it is beneficial to be sure to supplement with a good prebiotic consisting of different food sources. Look for labels containing FOS, inulin, and galacto-oligosaccharides which will feed the good bacteria (6).
Kefir, kombucha, sauerkraut, and yogurt are great sources of probiotics. Yogurt alone has been shown to have a direct correlation with preventing weight gain with age (4).
Choose Alternative Healing: Heal without antibiotics by supplementing your dietary intake of vitamin C, zinc, beta-carotene, Echinacea, elderberry, cranberry, and garlic. Drink herbal teas such as ginger to support your immune system.
Detoxify with a massage, Epsom bath, steam shower, or sauna. First, use natural methods to eliminate skin infections by topically applying tee tree oil or vinegar. Flush out a sinus infection using warm salty water in a neti pot and as always, remain hydrated. (5)
Fiber: The advantages of a high fiber diet cannot be stressed enough. Fiber is necessary to maintain the normal functioning of the gut. Compared to a broom, fiber sweeps waste build up along the intestines and creates bulk in the stool so that you have a consistent and healthy bowel function.
Prebiotics are not only found in a powdered supplement but different fiber sources serve as food sources for gut bacteria. Excellent fiber and prebiotic foods include apples, cabbage, Jerusalem artichokes, and onions.








Hi Dr jocker,
Thank you for the article.
Elsa
I’m a bit confused. How are you defining “high fat”? Isn’t the Ketogenic diet a high fat diet that is beneficial? Is there a guideline I’m missing for doing a Ketogenic diet?
Thanks Joe, you beat me to it! I was reading that article thinking the same thing. I guess though if you pair the high fat with veggies, low-sugar fruit like berries and add in good prebiotic fiber it should be okay?
That is exactly right Elena! All the prebiotic foods are rich in high quality fiber that feeds the good gut microflora. The high fat foods help to stabilize blood sugar and reduce inflammation and the prebiotic foods help to nourish the healthy gut bacteria, which also reduces inflammation and stimulates peristalsis and gut motility to help detoxify the body. Hope that helps!
Hey Joe, this is referring to a diet that is both high in fat and high in sugar at the same time. Not a ketogenic diet.
Whew. Okey doke. Thanks, Doc.
About 15 yrs ago I had h-pylori bacteria. I had to take a double treatment of antibiotics. Since then I have had to take nexium during the day and Zantac at night to help manage the pain in my gut. I have had a few scopes into my stomach and I have been told by my Dr that my stomach lining is depleted. Other than the drugs I am taking (which she prescribed) she has given me to help or hope.
I don’t want to take theses drugs and it seems like there is no help for me.
Can you help??
Susan
So sorry to hear about your health struggles Susan! I would recommend reading this article on H Pylori https://drjockers.com/damaging-effects-h-pylori-infections/ and begin following what I suggest in that article.
Hi Susan
I’m taking Bone Broth powder for my leaky gut. I just started out and it has been working.
BB is supposed too help repair the gut n cells
Hi, thank you for you work!
My daughter is been diagnosed three years ago with a vitiligo. She is now 11 years! We currently tested her with the G.I. map stool analysis and her Bacteroidetes and firmicutes are high. Is this a bad thing ?
Also there is this bacteria prevotella copri that is high, how do we get rid of it?
Thank you for taking your time to answer this!
Dalia Ardeu
Hey Dalia, you should send this question to Danielle, one of my health coaches, at nutrition@drjockers.com. She is great and can help you with this!