 Is a Ketogenic Diet Safe for Diabetics?
Is a Ketogenic Diet Safe for Diabetics?
With the increase in interest towards the ketogenic diet and its benefits for improving health, I get asked a common question all the time – is it safe for diabetics? You may have heard that the best thing for you is to consume multiple small meals a day. If you are following this popular advice (along with other common practices) you may actually be doing yourself a disservice.
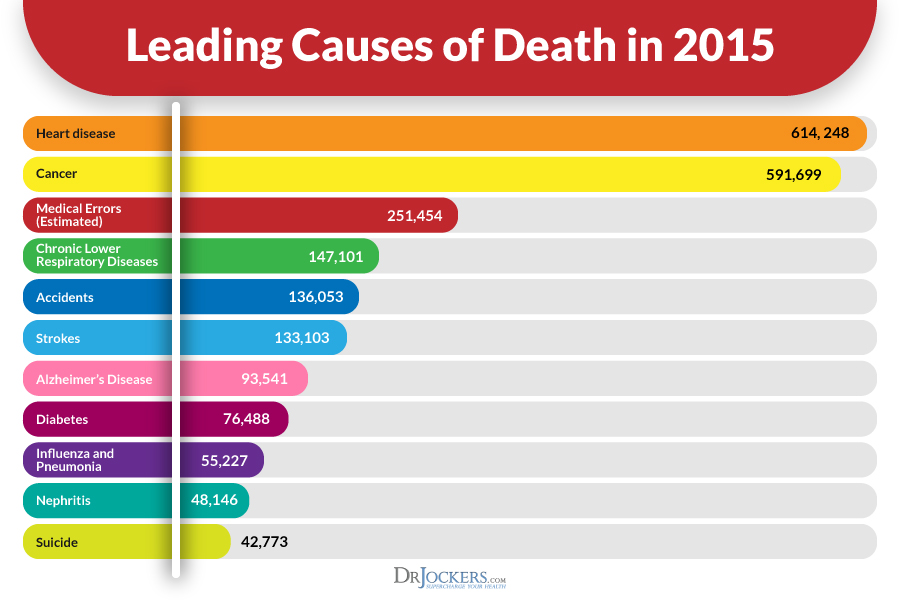
In this article, I am going to lay out the potential benefits and precautions of a ketogenic diet for those who are diabetic. I will also lay out practical steps for implementing one if you are new to the concept. In the process, you will also lower your risk of chronic diseases such as heart disease, cancer, and alzheimer’s.
Is Keto Safe?
Now first of all, I get asked if a ketogenic diet is safe a lot. The short answer is absolutely yes. Our obsession with sugar and processed foods is contributing to some of the most common chronic diseases of today.
The benefits of a ketogenic diet include:
Improved insulin sensitivity
Improved weight loss
Better cognitive function
Lower inflammation
Reduced risk of metabolic diseases
..and much more
Now there are certain things that must be accounted for in diabetics and I will discuss those things. Just understand that diabetes is most commonly a too much sugar issue that desensitizes our cells to insulin. What is the best way to restore insulin sensitivity? To stop hammering our bodies with sugar and carbs! Even if it is used as a temporary metabolic reset, the ketogenic diet can be extremely helpful for diabetics. By turning to fats as an alternative fuel source, you give your cells the break from sugar they need.

Nutritional Ketosis vs KetoAcidosis
In conventional medicine, the only time ketones and ketosis is brought up is in relation to the pathogenic state called ketoacidosis. This is a VERY RARE and highly unlikely state that anyone who attempts a ketogenic diet would ever encounter but diabetics should be familiar with it.
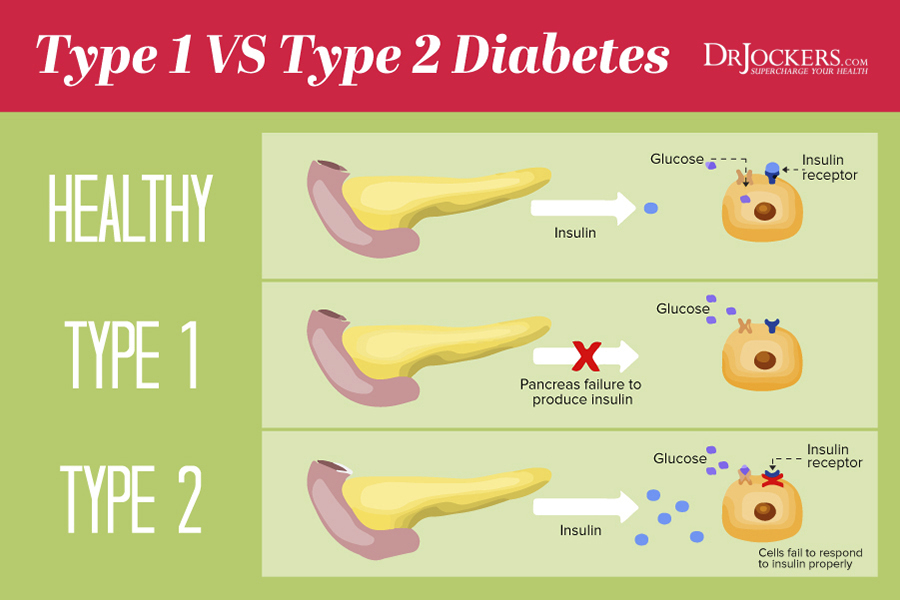
Type I diabetics cannot produce insulin. This means they must use self-administered exogenous insulin to stabilize blood sugar when they consume meals. This is because insulin is responsible for actually taking sugar from the blood and transporting it into the cells for energy. Without it, cells cannot make energy and they starve.
When insulin is not present for a period of time, the brain perceives the body to be in a starvation state and begins to produce ketones as an alternative energy source. Insulin also plays the role of regulating how many ketones are circulating in the blood at any one time. When insulin is not present, ketone bodies can reach levels upwards of 20 mmol/L in the blood. Ketoacidosis is characterized by very high blood sugar (250+) and high ketones. Whereas, nutritional ketosis is very low blood sugar and moderate levels of ketones.
To compare, a healthy person could fast for 20 days (a deep ketogenic stimulus) and only reach 5 or 6 mmol/L. Reaching this state of 20 mmol/L of ketones is dangerous as it makes the blood dangerously acidic and increases the viscosity of blood which can be potentially fatal.
Luckily, reaching this state through a ketogenic diet if you are a healthy person, a type II diabetic or a type I diabetic who is actually monitoring their blood sugar and insulin levels is virtually IMPOSSIBLE and should not be concern. It takes total neglect of one’s health for a diabetic to ever get into a state of ketoacidosis. If you are reading this article, you clearly care about your health and wouldn’t neglect yourself to get to this point.

Conventional Diabetes Nutrition Tips Harmful?
It is common belief that diabetics must consume regular meals with carbohydrates in order to keep blood sugar stable. At the same time monitoring blood sugar to adjust self-administered insulin accordingly.
In reality, what this may be doing is actually making the condition worse! The constant barrage of sugar on your cells is likely what led to the conditions you are facing in the first place. Continuing to consume carbs regularly while injecting insulin you are likely further numbing your cells’ response to those carbs.
In fact, one authority relied upon by those with diabetes is known to give recommendations such as the following:
-25-50 grams of carbs per meal
-6-11 servings of whole grains per day (including bread!)
-Insulin administered any time blood sugar leaves the “healthy” range
-A diet low in fats
-Processed foods marketed as “blood sugar friendly” alternatives
…etc.
Following a ketogenic diet may actually set you on the road to recovery from Type II diabetes. Type I diabetes is a different story however. Type I diabetics may not be able to do anything to reverse their condition. It is absolutely possible to manage more effectively, however. A ketogenic diet can reduce your insulin requirements and drastically reduce many of the negative side effects commonly faced.

High Blood Sugar Vs. High Insulin
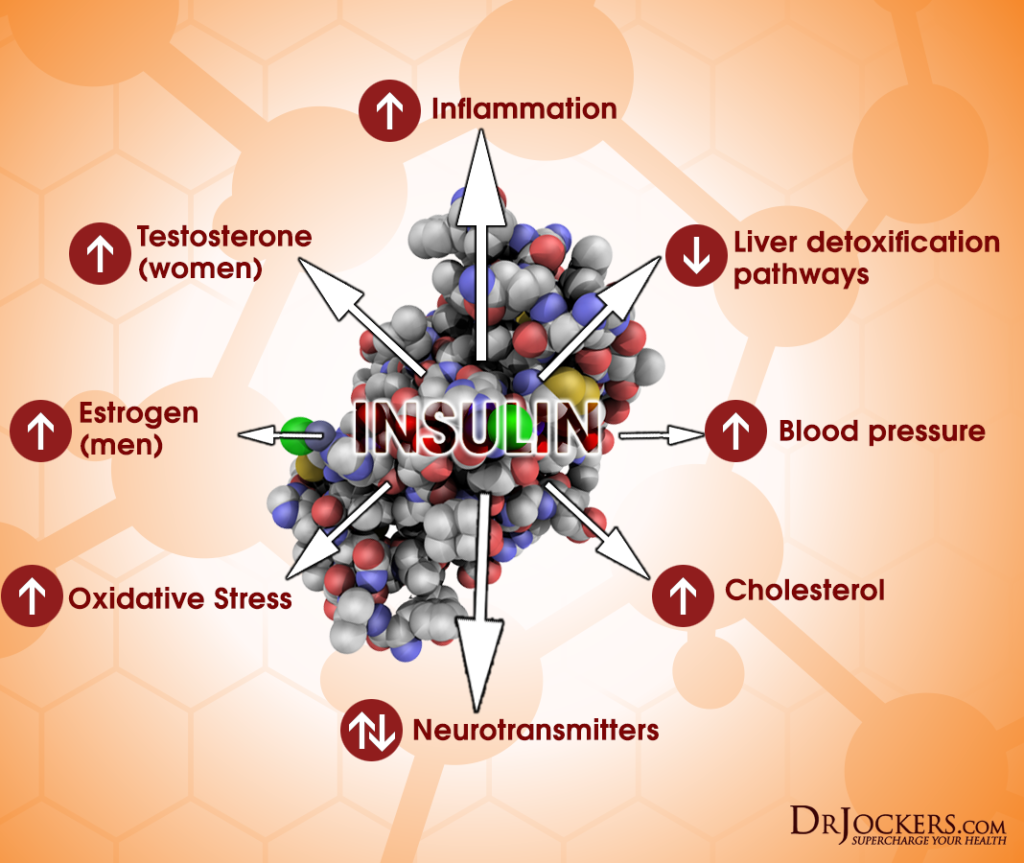
Having high blood sugar is certainly an issue for diabetics. Having chronically high insulin levels, however, may be even worse (and the real issue). High insulin levels lead to the further progression of Type II diabetes as cells are desensitized to its presence. Once cells become desensitized to insulin, blood sugar becomes higher, leading to an even higher need for insulin. This becomes a cycle that tends to get worse with time.
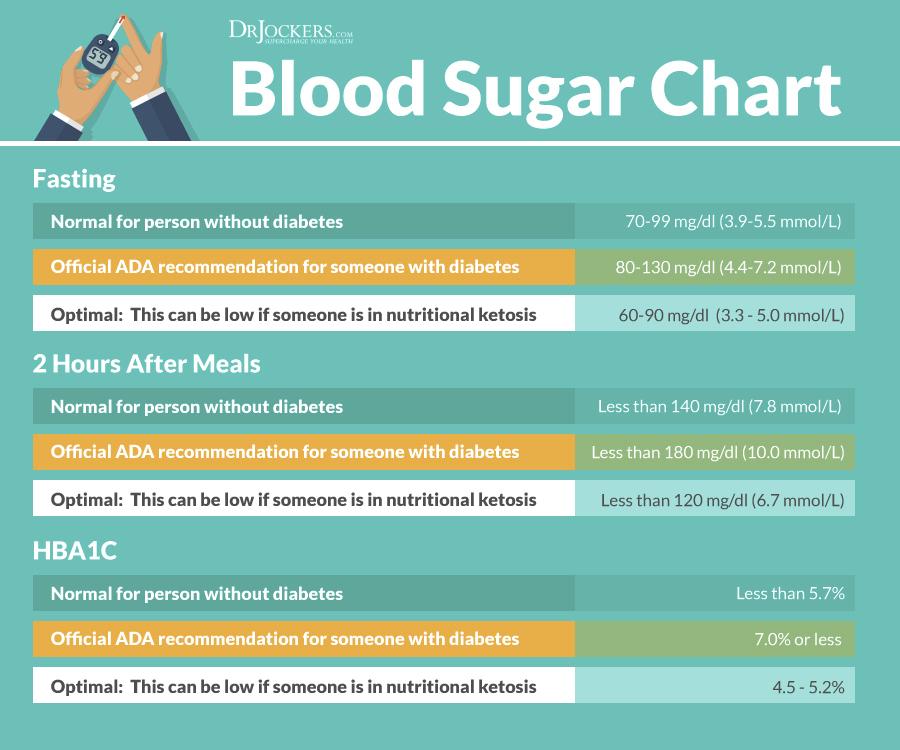
Additionally, while your blood sugar may be “in range” after a meal, your blood insulin may be a completely different story. In my article 9 Ways to Test Blood Sugar I explain the best ways to take a functional look at your blood sugar.
The Diabetic types are commonly characterized by the following criteria:
-High blood sugar with Low blood insulin (Type I)
-High blood sugar with High blood insulin (Type II)
-Slightly high blood sugar with or without elevated insulin (Pre-diabetes)
Now consider this, if your insulin was working properly, would you have elevated blood sugar? Elevated blood sugar is not a sugar issue, it is an insulin issue. So if we wish to improve the diabetic condition, we must improve the function of insulin.
Keto and Insulin Sensitivity
Research has been building in recent years supporting the idea that intermittent fasting and a ketogenic lifestyle are able to improve insulin sensitivity among other risk factors for metabolic diseases.
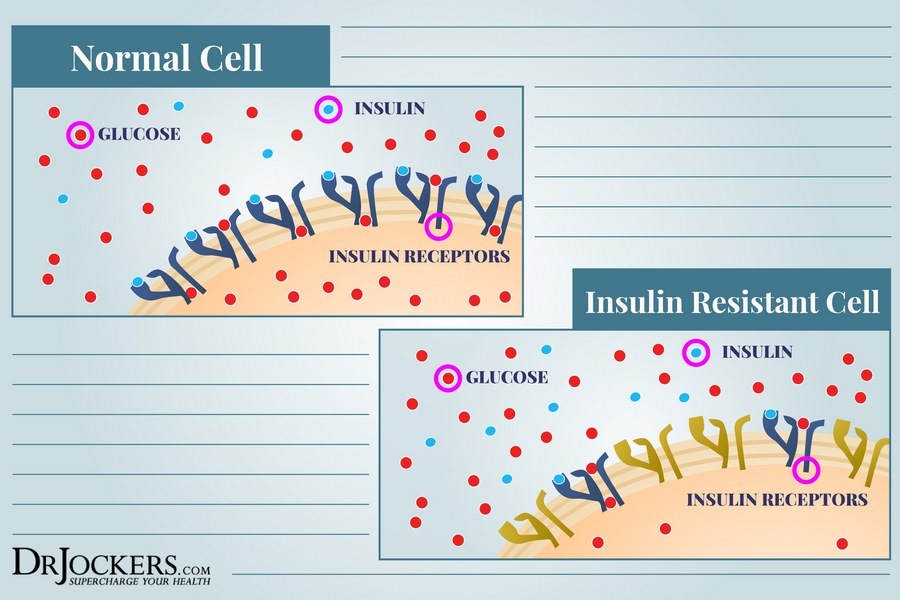
This is simply due to the fact that when you are burning ketones for energy instead of sugar, you are allowing your insulin receptors to rest from the usual constant bombardment they are accustomed to.
Recent literature reinforces the safety and effectiveness of a ketogenic diet in time ranges anywhere from 3 weeks up to a year (1). While it is typically a good idea to periodically cycle out of ketosis with a higher carb meal, the evidence supports heavily reducing carb intake to help with insulin sensitivity.
Type I Diabetics
For Type I diabetics, it is not as easy as simply adopting a ketogenic diet and calling it a day. These individuals will need to work closely with a doctor who has experience in this area to determine appropriate insulin dosages and monitor for any potential side effects.
What the ketogenic lifestyle can do for these individuals is drastically reduce the need for insulin and mitigate many common side effects such as peripheral neuropathy and eye problems caused by advanced glycation end products.
Another thing to consider is that Type I diabetes is usually caused by an autoimmune reaction towards the insulin-producing cells in the pancreas. What this means is that, in those who have not lost insulin function completely, reducing this autoimmune reaction could save some of the function of your pancreas long-term.
A ketogenic diet that avoids common food sensitivities can go a long way in reducing inflammation throughout the body and helping reduce autoimmune reactions.
Type II Diabetics
Type II diabetics are most commonly suffering from insulin resistance. It is these individuals who will see the most profound changes when adopting a ketogenic lifestyle. While Type I diabetics can make managing their condition much more bearable, those with Type II may potentially be able to reverse this metabolic disease in some cases.
It is typically not recommended to jump head first into a ketogenic diet however, especially if you already have metabolic issues. It is recommended to ease your way into it by implementing intermittent fasting and slowly reducing carb intake over several weeks. Utilizing readily available ketone sources such as MCT oils and exogenous ketones can be very helpful during this time.
To read more on the sequencing of implementing a ketogenic diet for the first time, this article is your guide: Keto Metabolic Makeover

Benefits of a Ketogenic Diet for Diabetics
So we’ve discussed how a ketogenic diet is safe for diabetics and potential ways in which it can improve the diabetic condition. Now, let’s look at some of the science behind why you may want to consider trying this style of eating out for yourself.

Lowers Metabolic Disease Risk
Blood sugar dysregulation is one of the the first change that occurs in the body on the path towards metabolic disease. Metabolic disease is a number of conditions characterized by obesity, diabetes, and an increased risk of heart disease.
When someone is diagnosed with diabetes, it should be stressed that measures should be taken to prevent further progression towards metabolic disease as it is also associated with things like cancer.
Luckily, a ketogenic-style nutrition plan has been shown to improve body weight composition, lower blood sugar, lower triglycerides, and lower Hemoglobin A1C (2,3). This was even further investigated and confirmed in a recent clinical trial (4).

Outperforms a Calorie-Restricted and Low-Glycemic Diet
Low-calorie and low-glycemic diets may have some benefits, but they do not provide the same level of benefit as a properly planned ketogenic diet. Research has shown repeatedly that the ketogenic diet outperforms these other nutrition plans in all areas of metabolic health including weight loss, cholesterol management, blood pressure, insulin sensitivity, and inflammation (5, 6).
Not only does a ketogenic diet provide more benefits, but it does so with less side effects. Low-calorie diets tend to place the body in a starvation state that actually contributes to additional weight gain. Low-glycemic diets are better than traditional diets but they still stimulate already over-stimulated insulin receptors.

May Lower Insulin Needs in Type I Diabetics
There are several case studies showcasing that a properly planned ketogenic diet can be beneficial for Type I Diabetics (7, 8). It is not realistic for Type I diabetics to come off of insulin on a ketogenic diet. It is however, very likely that being able to get into an adequate state of dietary ketosis will help manage blood sugar more effectively with lower doses of insulin.
At the same time, these individuals will likely enjoy the added benefits of improved body composition, improve cholesterol levels, improved blood pressure levels, more energy, and reduced risk of diabetic side effects such as glycation-related damage to the limbs, brain, and eyes.
If you have Type I diabetes, it is necessary to work with a doctor who has experience in this area to track blood sugar and adjust to the most ideal insulin dosage for you. The risk of going into ketoacidosis is increased when too little insulin is taken. Too much insulin would likely place the body in a dangerous state of hypoglycemia which is also very harmful to the body.
Another important consideration for these individuals is that there is often autoimmunity involved, making it imperative that immune modulating nutrients are optimized such as Vitamin D. Removing common inflammatory foods from the diet such as those outlined in the graphic below.

Prevention for Type II Diabetics
In addition to Type I and II diabetes being a very prominent issue in our society, prediabetes is also extremely common and often goes unrecognized. The insulin sensitizing benefits in addition to the range of other metabolic benefits may provide a solid strategy for preventing the progression towards Type II diabetes in the future (9).
In fact, low-carb diets consistently outperform other types of nutritional strategies for improving just about every risk factor for diabetes, obesity, heart disease, and other metabolic disease conditions (10, 11).
Again, this likely comes down to the fact that following a ketogenic lifestyle gives the insulin receptors a chance to re-sensitize while also drastically lowering inflammation. A more recent benefit that is being discovered is how a ketogenic diet can improve mitochondrial function which in of itself improves metabolic health from the cellular level.

Reduced Risk of Diabetes-Related Side Effects
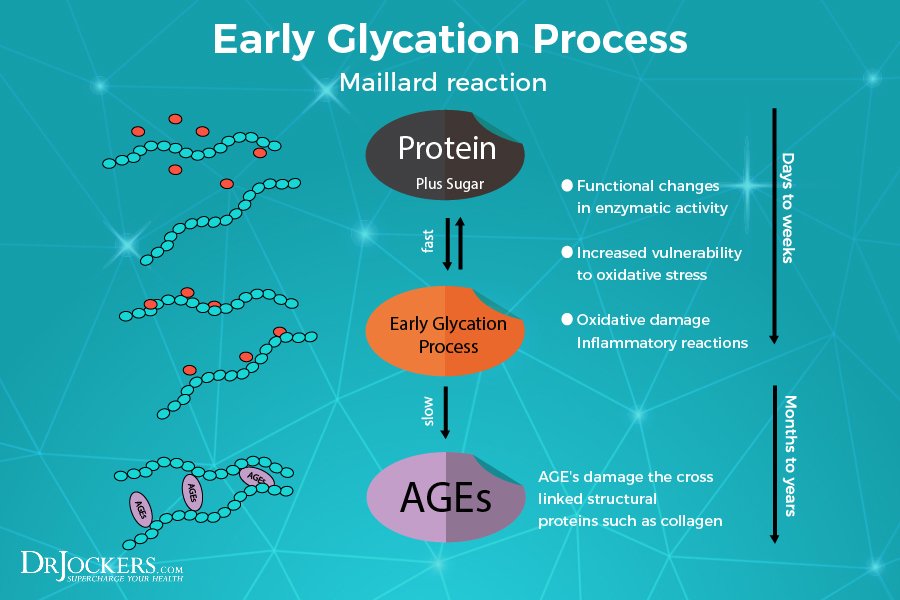
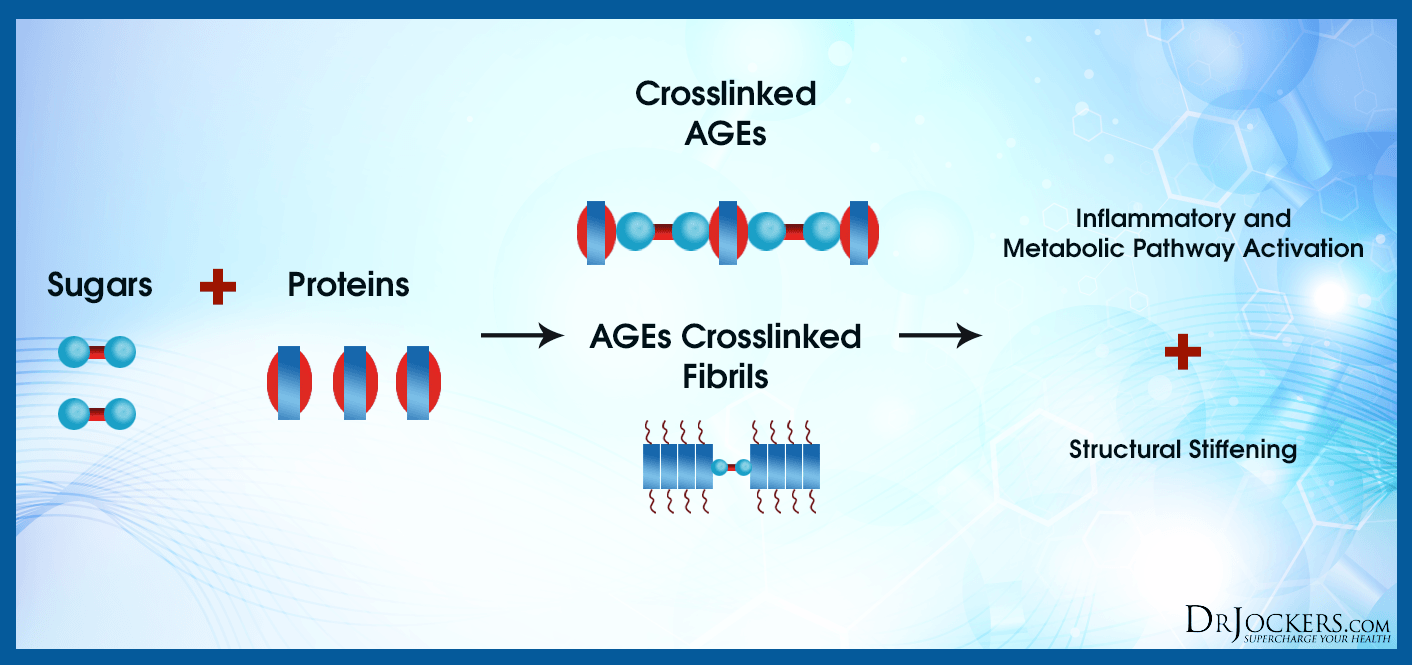
If diabetes goes unmanaged, many side effects can occur. The consequences of excess sugar and insulin in the blood can affect many tissues throughout the body via the formation of advanced glycation end products (AGEs). It is these molecules that lead to things like impaired brain function, peripheral neuropathy, and vision problems later in life.
In fact, literature highlights many consequences of unmanaged diabetic conditions including: heart disease, neuropathy (nerve damage), vision problems, pregnancy complications, kidney damage, and more.
Research shows that improving your blood sugar regulation can drastically reduce the risk of these complications.
Precautions For Diabetics
There are certain measures that must be taken to ensure your body is adapting well.
The first method is to closely monitor your blood sugar and ketone levels to ensure they are staying within optimal ranges. The other is to perform routine lab work to measure various markers of blood sugar, inflammation, and cholesterol. I will recommend my top methods for doing these things.

Ketoacidosis: Testing Ketones and Blood Sugar
To ensure blood sugar and ketones are remaining within desirable ranges, a dual blood sugar and ketone monitor is probably the best method. Many devices exist for doing both of things individually. The one that I have found most practical for doing both it the Keto Mojo monitor.
However, if you are diabetic you likely already have a blood sugar monitor.. If you would like to purchase a practical ketone monitoring device then there are two very solid options for doing so. The first is the Ketonix breath monitor which is the most popular option.
The next option is the LEVL device which is able to provide real-time breath ketone measures while also providing a simple digital user interface for tracking and graphing your fat burning potential over a longer period of time.
How to Assess your Progress
Taking periodic measurements of markers such as fasting blood glucose, oral glucose tolerance, fasting insulin, LDH, C Reactive Protein, and Hg A1C are imperative for long-term success.
The majority of these markers can be assessed in a comprehensive blood count as we feature on our Comprehensive Blood Analysis.
Similar tests run through your primary care physician often do not cover the full range of markers that are found in a functional thyroid and full blood panel. The added benefit of seeing the full range of thyroid markers (T4, T3, T3 Uptake, Free T4, Free T3, Reverse T3, TSH, TPO, TBG) is that these markers are strong indicators of metabolic health that regulate your blood sugar balance and fat burning potential.
The Comprehensive Blood Analysis also looks at Vitamin D levels which should be in the range of 60-100 for optimal blood sugar regulation and protection from Autoimmune-related side effects in Type I diabetics.
Conclusion
A properly planned ketogenic diet is a safe and effective strategy for diabetics. It is superior to many other dietary strategies for improving blood sugar balance, improving insulin sensitivity, and reducing the risk of diabetes-related side effects such as peripheral neuropathy, memory impairment, and vision problems.
That being said, it is important to take certain precautions such as monitoring glucose and ketone levels, periodically running comprehensive blood work to assess metabolic health, as well as working with an experienced physician to determine adaptive insulin and medication needs.




Great advice! Looking forward to using this to better my health.
All the best Max! Thanks for reading!
I am not diabetic but my 81 yo grandmother is Type 1. She manages it very well and doesn’t have any other serious health issues. I have recently started a keto lifestyle and have been telling her all the great things it can do. I had her over for dinner recently and after she ate all of my grain and sugar free stuff, her blood was pretty normal when she checked it about an hour later. The question is this, I told her about My Fitness Pal to track her macros, and when I was helping her set it up, she told me her doctor recommended 165g/carbs per day! I don’t know a whole lot about diabetes, but could that be correct? Wouldn’t that just increase her need for MORE insulin? I know you aren’t HER doc, but what would be a safe range of carbs to start on for someone like my Grandma?
Thanks for your time,
Kaya
Hey Kaya, Yes more carbs means more insulin for Type I. Many people gradually lower their carb intake and adjust insulin needs as necessary. I would say try lowering daily carbs by 20 grams every two weeks or so until she is under 50. Eventually down to 20-30 grams per day if she is tolerating it well! Using MCT while lowering carbs can be helpful as well to jumpstart the ketone formation process.
Thank you SO much for that advice! I really appreciate it! Have a great week!
So I am a type 1 diabetic who is a triathlete, marathoner, and cyclist who is also wheelchair bound, but my issue is that wouldn’t teaching your body to burn fat as fuel lower your anaerobic threshold due to the fat burning zones (zone 2), and anything getting your heartrate up past zone 3 require carbs to burn as a fuel source? I am attempting to utilize a keto diet but don’t want to lose FTP in the process. Maybe just consume my carbs before races and during interval training?
Not necessarily James. The body gets very efficient at conserving glycogen when it is fat adapted. This means you would be able to pull from those stores when needed. It appears using exogenous ketones preworkout can enhance this effect as well. From an anecdotal standpoint, I have heard people have mixed experiences with it so definitely something to test on yourself.