 Edema: Symptoms, Causes, and Natural Support Strategies
Edema: Symptoms, Causes, and Natural Support Strategies
Most of your body is made up of water. Water moves throughout your body. But due to various issues, water can build up in your tissues in certain areas of your body, causing swelling. This swelling is called edema, which is mainly common in the skin, especially around your ankles, feet, hands, arms, and legs, but also in various organs. Fortunately, you can use natural support strategies to reduce your risk factors and improve edema.
In this article, you will learn what edema is. I will go over the signs and symptoms of edema. You will understand the causes of edema. I will discuss conventional treatment options for edema. I will share my best natural support strategies for edema, including my favorite supplements, to reduce your risk for edema, improve edema, and regain your health and well-being.
What Is Edema
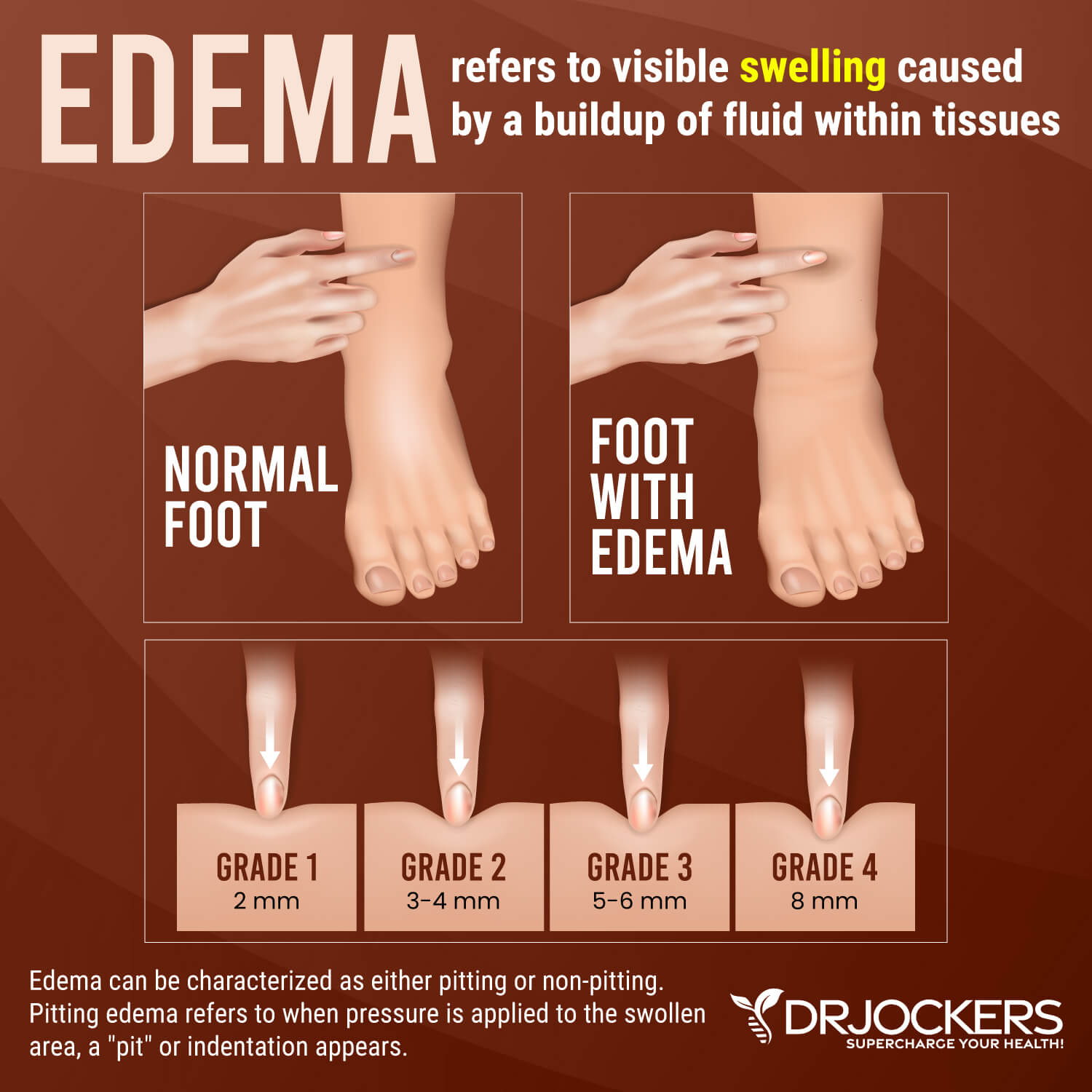
Edema is characterized by fluid buildup in bodily tissues causing swelling and puffiness. Edema is common in the skin, especially in the feet, ankles, legs, hands, and arms. However, you may develop edema in the muscles, lungs, brain, eyes, bowels, and other organs. In some cases, edema has a sudden onset.
In other cases, it begins more slowly. Edema is common in pregnant people and older individuals. While it is a common condition that is often not dangerous, in some cases, it may be a sign of a serious condition (1, 2).

Signs & Symptoms of Edema
The word edema means swelling, so it’s not surprising that one of the main signs of edema is swelling. Edema develops when fluids gather in tissues causing swelling in a certain part of the body (3).
Signs and symptoms of edema may include:
- Swollen, stretched, and shiny skin
- Puffiness of the ankles, wrists, face, or eyes
- Skin that retains a dent after applying only a few seconds of pressure
- Stiff joints
- Aching in the affected body parts
- Decreased urine production
- Fuller hand and neck veins
- Other visual anomalies
- Weight gain or weight loss
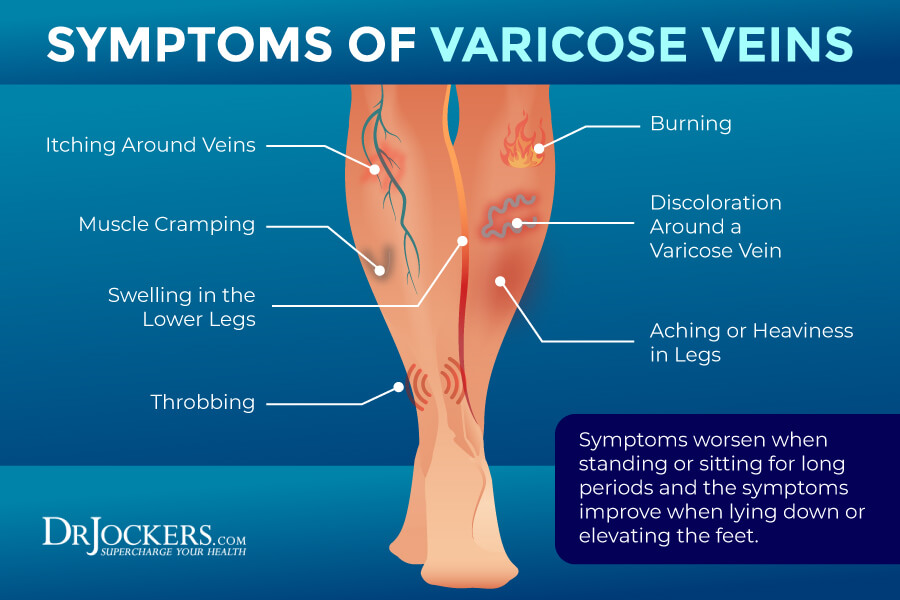
Peripheral edema, affecting the arms or legs, is the most common type of edema. Common signs and symptoms of peripheral edema may include (3):
- Visibly swollen arms or legs
- A heavy or full feeling of the arms or legs
- Retaining a dent when pressing on the swelling
- Jewelry or clothing feeling tight or uncomfortable
- Warm skin around the edema
- Tight-feeling skin around the edema
- Difficulty moving any joints in the affected area
- Pain or discomfort in the area

Root Causes of Edema
To reduce your symptoms, risks, and re-occurrence of edema, we have to look at and address the root causes of the issue. The most common root causes of edema include chronic inflammation, insulin resistance, kidney problems, lymphedema, varicose veins, certain medications, pregnancy, and sitting too long.
Let’s look at these potential root causes of edema one by one:
Chronic Inflammation
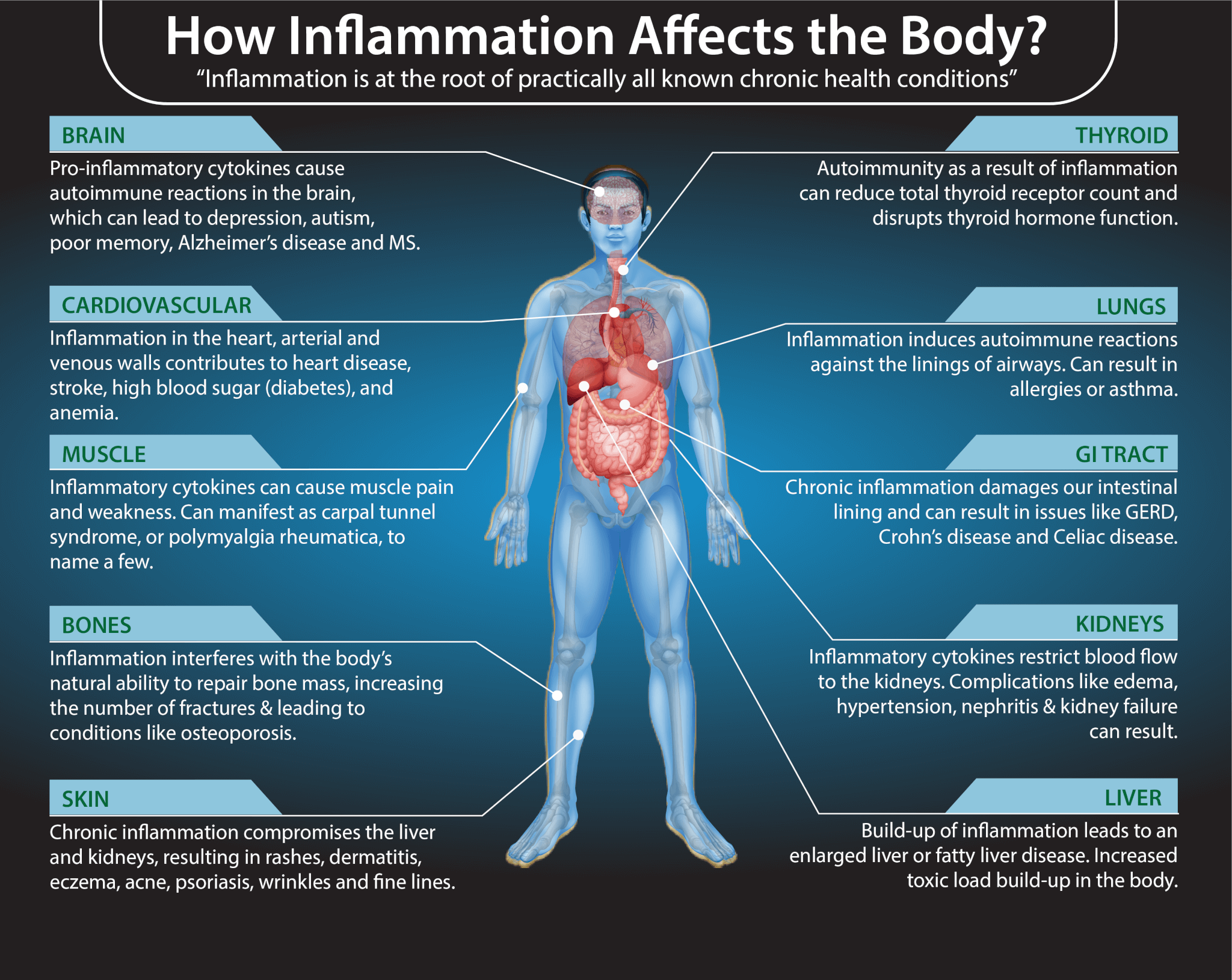
Inflammation affecting your tissues may lead to swelling and edema. According to a 2020 review published in Wound Repair and Regeneration, deep tissue inflammation may play a role in edema (4).
Acute inflammation from allergies, sprained ankles, broken bones, other physical trauma or injuries, infections, wounds, gout, or arthritis can cause swelling. However, chronic or long-term inflammation may also lead to edema. When edema is a reoccurring or ongoing problem, chronic inflammation is likely an underlying issue.
Insulin Resistance
Insulin resistance means that your body is unable to respond to and use insulin as it should. As a result, your pancreas is forced to pump out more and more insulin to deal with dietary glucose (sugar). Insulin resistance may increase the risk of prediabetes and type 2 diabetes. It is also an underlying risk factor behind many chronic health issues. It may also contribute to edema.
Too much sugar that your body cannot deal with may lead to damage to the lining of your capillaries. This may affect blood circulation, causing the swelling of the foot. According to a 2017 study published by Diabetes Research and Clinical Practice, mild compression socks may be helpful for people with edema in the lower extremities related to diabetes (5).
People with diabetes may also develop diabetes-related macular edema characterized by retinal thickening generated by the accumulation of intraretinal fluid, mainly in the inner and outer plexiform layers (6). According to a 2021 study published in the Journal of Diabetes Investigation, people with insulin resistance and type 2 diabetes may develop edema in the insulin injection site (7).

Kidney Problems
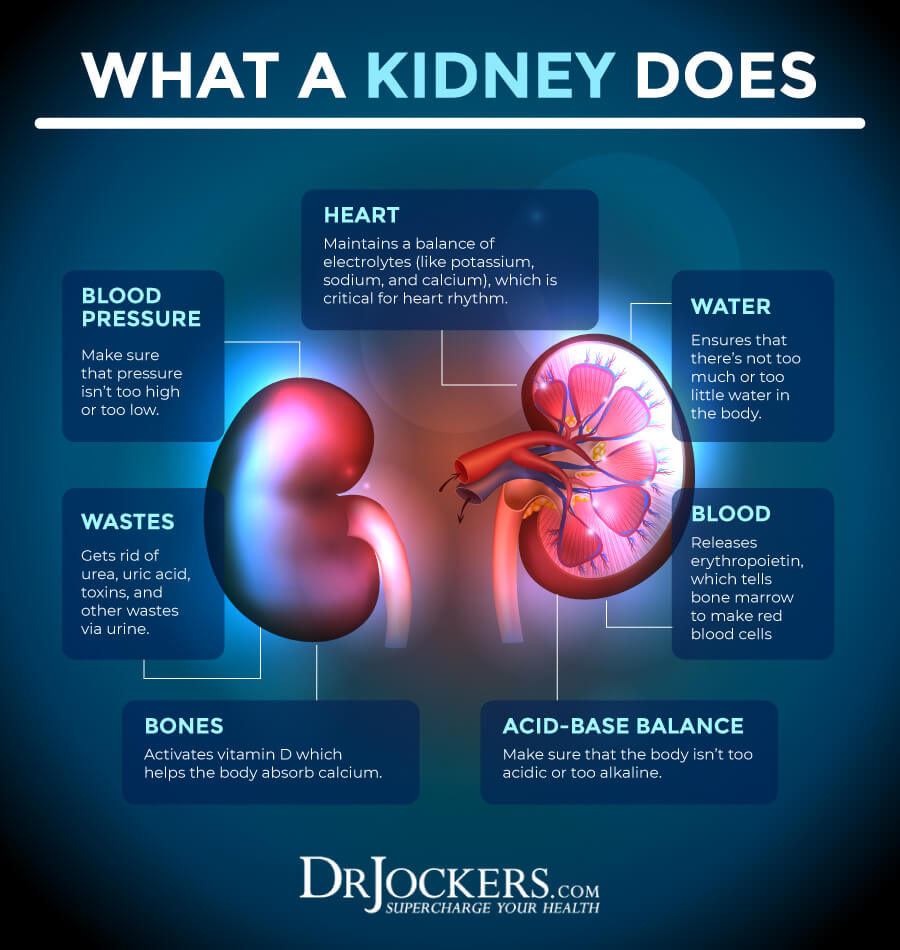
Your kidneys are a pair of organs. They are one of the most important organs of detoxification. They help to remove waste and extra water from your blood in the form of urine. They also allow your body to keep your electrolyte, including sodium, potassium, and calcium, balanced. Kidney problems can lead to a lot of health issues, including possible edema.
Kidney disease can lead to fluid and salt buildup in the blood, which may lead to edema in the legs and around your eyes. Swelling in your feet and hands can occur at stage 4 kidney disease before kidney failure occurs.
A 2016 study published in PLoS One has found that using diuretics to deal with fluid overload in chronic kidney disease may improve edema but should be used cautiously as diuretics may also result in adverse renal outcomes (8).
Lymphedema
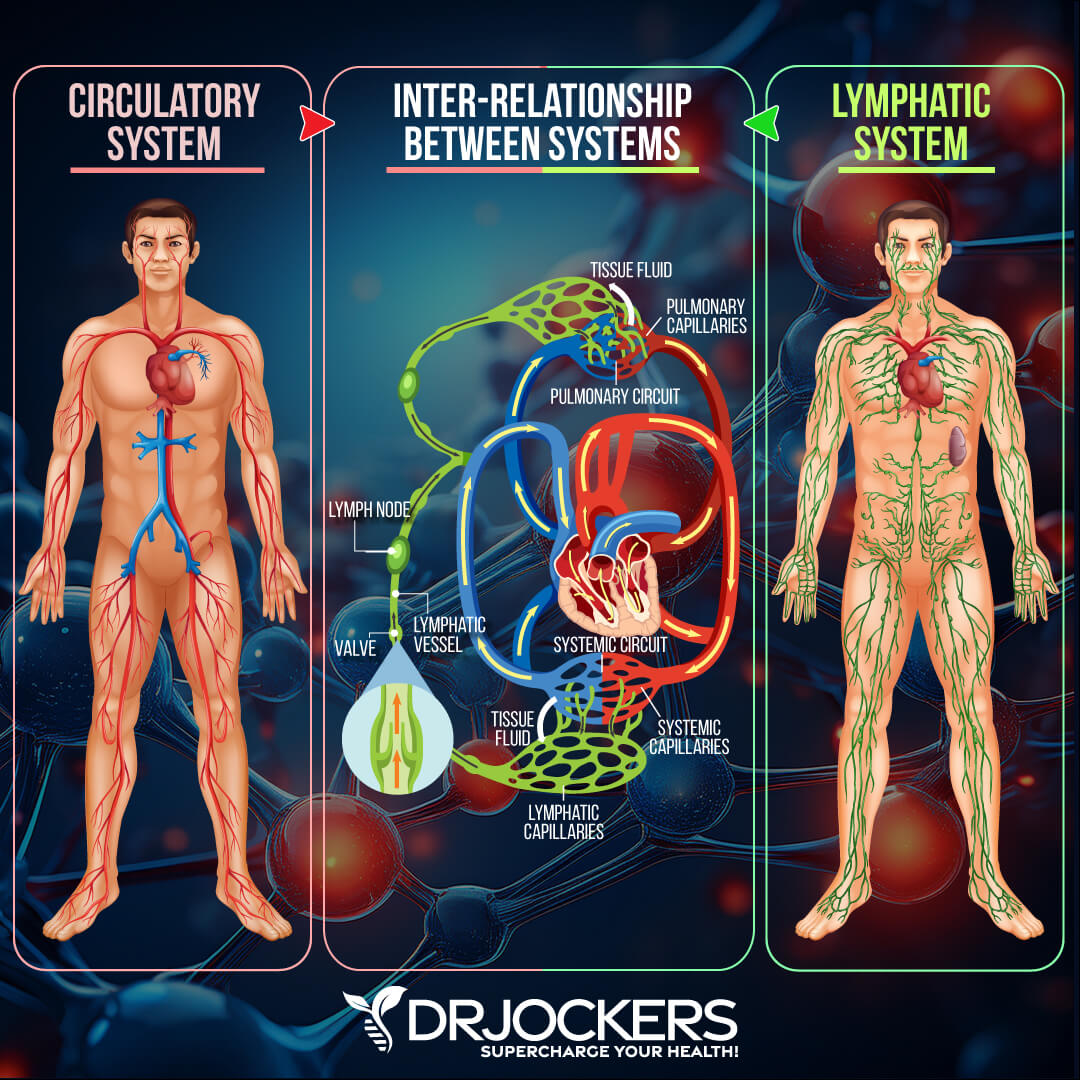
Lymphedema is a condition characterized by damage to your lymphatic system. If you have lymphedema, it means your body cannot drain fluids as it should (9). This can lead to non-pitting edema in your legs and arms.
You may develop lymphedema due to lymph node surgery, mastectomy, or radiation therapy, but also from venous insufficiency and obesity. According to a 2014 review published in Plastic and Reconstructive Surgery, obesity and postoperative weight gain may increase the risk of markedly impaired lymphatic function and primary lymphedema (10).
Varicose Veins
Problems with your veins, including varicose veins, may also increase the risk of edema. Your veins transport blood across your body, but if they aren’t able to move enough blood to your feet and then return it to your heart, it results in venous insufficiency, which can cause swollen feet and ankles.
Blood gathering in your legs pushing fluid out of your blood vessels into tissues in the areas is one of the main causes of edema in the legs. According to a 2013 review published in Duodecim, this is particularly common among those over 50, mainly in women (11).
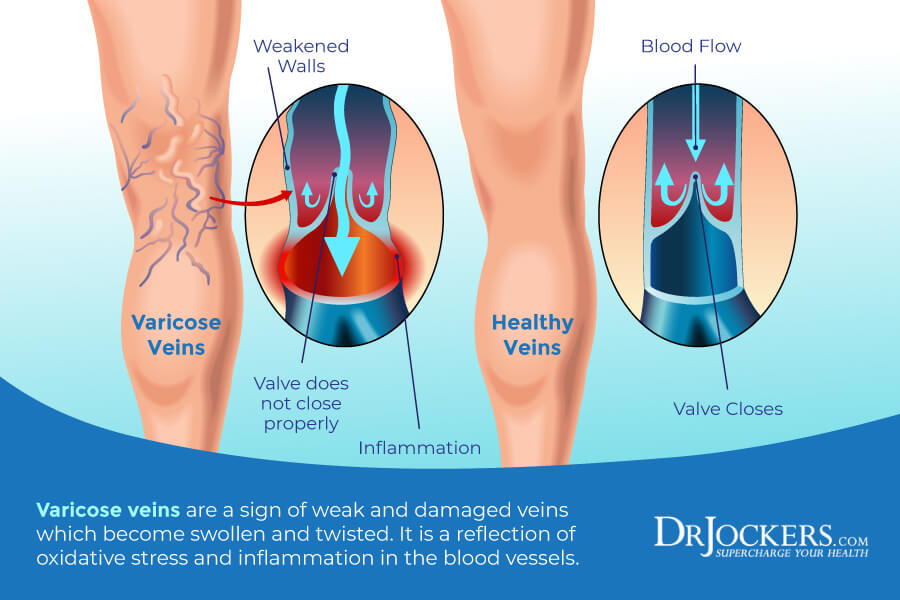
Varicose veins are twisted, large, swollen, and raised veins that are dilated and overfilled with blood. Varicose veins are bluish-purple or red in color and can be quite painful in some people.
Varicose veins can come with slight swelling to severe edema in the ankles to knees. According to a 2022 research article published in Medicines (Basel), edema may be present in 61.1 percent of individuals with varicose veins (12).
Moreover, according to a 2001 research published in the Western Journal of Medicine, edema in the lower limbs may be a sign of deep vein thrombosis (13). Slow-flowing blood may not only cause swelling but also lead to blood clots. Since varicose veins can cause blood flow to slow down, it may increase the risk of blood clots and thrombosis too.
Certain Medications
Certain medications may also increase the risk of edema. This is called drug-induced edema. Some medications may cause an imbalance in your body’s sodium and water balance, which may lead to renal dysfunction and edema.
According to a 2005 review published in Nhon Rinsho, medications that may increase the risk of edema include nonsteroidal anti-inflammatory drugs or NSAIDs (such as ibuprofen or naproxen), antihypertensive drugs, and anticancer drugs. insulin, steroid therapy, and medication for high blood pressure (14).

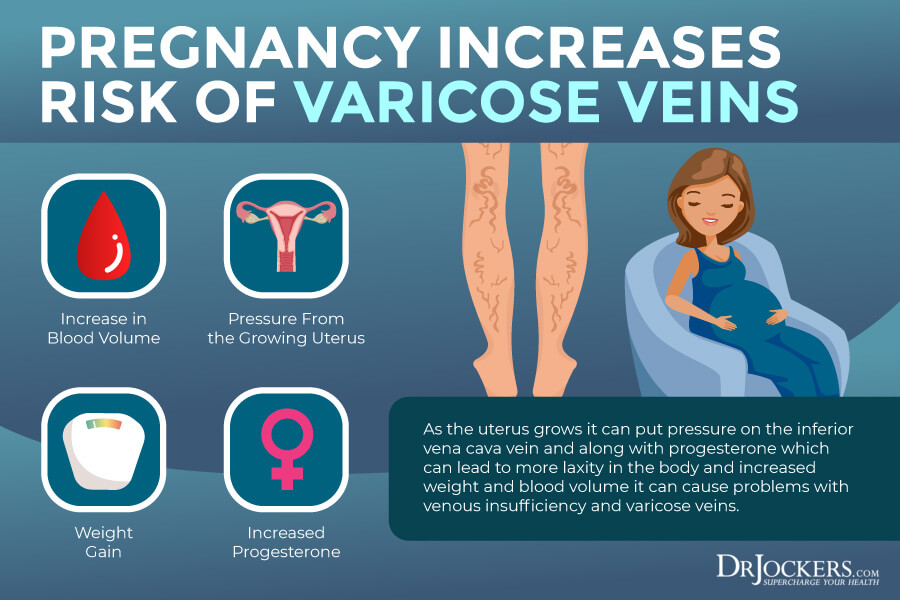
Pregnancy
Pregnancy is also a risk factor for edema. According to a 2021 report in Case Reports in Obstetrics and Gynecology, about 70 percent of pregnant women will experience swelling in the lower extremities at one point during their pregnancy (15). This generally happens in the third trimester.
If you have to rest too much in a reclined position during pregnancy, the enlarged uterus may press on the inferior vena cava, potentially causing the obstruction of the femoral veins, causing edema.
Blood clots may also develop more easily during pregnancy, increasing the risk of deep vein thrombosis and edema. Pregnancy-induced hypertension may also increase the risk of edema during pregnancy.
Sitting Too Long
Prolonged sitting and even prolonged standing may increase the risk of edema. The effects of gravity and lack of movement can cause an abnormal buildup of fluid and swelling, mainly in the ankles and feet.
According to a 2022 research article published in Biology (Basel), breaking up prolonged sitting or standing time with an intermittent mix of sitting, standing, and moving, may reduce the risk of edema (16).

Conventional Treatment Options
Treatment for edema depends on the cause of the edema. This is true for conventional treatment options for edema as well. Diuretics are commonly prescribed for edema to get rid of any excess fluid. It helps to increase urine production by your kidneys to decrease excess fluid.
Compression garments, such as stockings, socks, and sleeves, and specific exercises are also commonly recommended for edema. To reduce edema, you may also be recommended to avoid sitting for long periods, going on short walks to move your body, using a pillow under your legs when lying down to keep it elevated, and reducing your salt intake may be among the recommendations.
For macular edema, pulmonary edema, or other forms of edema, you may be recommended other kinds of medications or treatment options. Patients with lung disease or lung disease-related edema are recommended to stop smoking.
In chronic heart failure-related edema, reducing salt intake, improving fluid intake, cutting back on alcohol, and monitoring weight may be recommended. If edema is caused by medication as a side effect, stopping and switching medication may be recommended. However, it’s important not to stop taking any medication without your doctor’s approval and guidance.

Natural Support Strategies
So how can you reduce your risks and improve edema naturally? Here are my best natural support strategies for edema:
Anti-Inflammatory Nutrition Plan
Various dietary factors, including a low intake of vitamins B1, B6, and B5, malnutrition, and too much salt in the diet may increase the risk of edema (17). Chronic inflammation, insulin resistance, diabetes, and electrolyte imbalance may all also contribute to the increased risk of edema, all of which issues may be reduced through diet, lifestyle, and other natural strategies (4, 5, 6, 7).
I recommend following an anti-inflammatory nutrition plan. Remove any inflammatory foods, including refined sugar, refined oil, deep-fried foods, artificial ingredients, additives, overly processed foods, and junk food.
Focus on anti-inflammatory, nutrient-rich whole foods, including lots of greens, vegetables, herbs, spices, fermented foods, low glycemic index fruits, grass-fed beef, pasture-raised poultry and eggs, wild-caught fish and seafood, and wild-game. Keep your carb intake low from fruit and vegetable sources.
Focus on lots of healthy fats, including coconut oil, coconut meat, avocados, extra-virgin olive oil, grass-fed butter and ghee, and other animal fats. Eat a moderate amount of clean animal protein from grass-fed beef, pasture-raised poultry and eggs, wild-caught fish and seafood, and wild game.

Use Bitter Herbs for Natural Diuretics
Bitter herbs can serve as natural diuretics and may support the liver, kidneys, and lymphatic systems. According to a 2019 case report published in Medicine (Baltimore), using traditional herbal medicine may be an alternative treatment option for refractory edema (18).
Herbs I recommend for edema, include dandelion, ginger, parsley, licorice root, horsetail, juniper, hibiscus, green tea, and hawthorn.

Intermittent Fasting
Intermittent fasting is an eating approach where you are fasting (not eating) for a part of the day, keeping a specific eating window for your meals. If you are new to intermittent fasting, start with a 12-hour fast. Stop eating after dinner at 6 or 7 pm and don’t eat until the next morning, 12 hours later, and 6 or 7 am.
Intermittent fasting has many health benefits, including reducing chronic inflammation, improving insulin sensitivity, and supporting autophagy. According to a 2018 study published in Cell, intermittent fasting may reduce inflammation, including circulatory inflammation, which may increase the risk of varicose veins, insulin resistance, and diabetes (19).
Since these conditions may cause edema, intermittent fasting may decrease the risk of edema connected to chronic inflammation, circulatory inflammation, varicose veins, and insulin resistance.
Gradually increase your fasting window until you find what works for you. Most people tend to find the 16:8 approach with a 16-hour fast and 8 hours reserved for eating the best, but you may find that a shorter or longer window works best for you. Y
ou may learn more about the best intermittent fasting strategies here. You may learn more about its benefits in this article.

Regular Movement and Exercise
Sitting or standing for too long without moving or switching positions may increase the risk of edema, especially in your feet and ankles. A 2022 study published in Biology (Basel) has found that breaking up prolonged sitting or standing time with an intermittent mix of sitting, standing, and moving, may reduce the risk of edema (16).
I recommend moving your body throughout the day and exercising regularly. Start your day with a stretch, a short walk, some rebounding, or a short stretching session to wake your body up. Break up your workday by getting up regularly. Switch between a standing and sitting desk.
Get up, move around, shake out your body in place if you don’t have the option to leave your desk, or break out in a short impromptu dance session if you can. You may try a walking pad under your desk or an under-the-desk bike.
Take a walk during lunchtime, take the stairs, and bike or walks instead of driving when possible. Exercise regularly, at least 5 days a week for 20 to 30 minutes, using a mix of strength and resistance training, cardiovascular, and low-impact exercise.

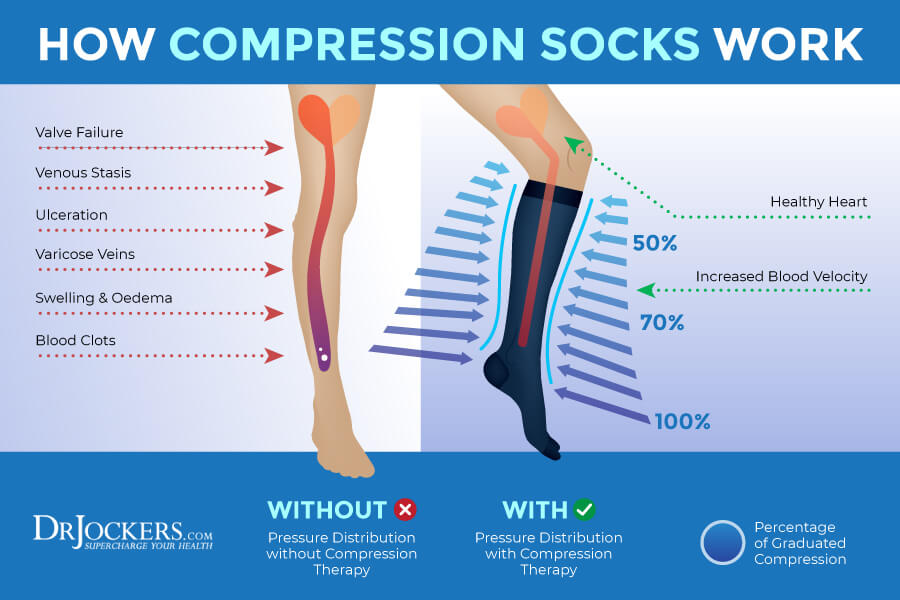
Compression Socks
Compression socks and other compression garments, such as compression stockings and sleeves, may help with edema. A 2017 study published in the Diabetes Research and Clinical Practice has found that mild compression socks may be helpful for edema in the lower extremities in those with diabetes (5).
Compression socks may also reduce the risk of edema and blood clots related to long flights and travels. You may find compression socks online. You may also get recommendations from your doctor or physical therapists to see which option works best for you.
Dry Brushing
Lymphedema and lymphatic health dysfunction may increase the risk of edema (9). Dry brushing is a strategy that supports lymphatic health and detoxification. Use a soft organic dry brush from natural materials, such as bamboo dry brushes.
Practice dry brushing daily before your shower or infrared sauna session followed by the shower. Infrared sauna further supports detoxification, and showering helps to remove toxins, dead skin cells, and sweat.
Use a circular motion starting from your feet all over your body in a logical order. Always move in the direction of your heart. In your belly area, use a clockwise motion to support digestion. Be careful, especially in sensitive areas. You may learn more about dry brushing from this article.

Massage Therapy
Massage therapy may also support lymphatic function, reduce inflammation, improve circulation, and decrease swelling. Lymphatic drainage massage may be particularly great for lymphatic-related edema. Foot and leg massages may reduce swelling in the foot, ankles, and legs.
According to a 2017 systematic review published in the Journal of Hand Therapy, massage, elevation, compression, and exercise are the top strategies to improve edema in the hands (20). According to a 2010 study published in the International Journal of Nursing Practice, foot massage may help to reduce edema during late pregnancy (21).
You may benefit from self-massage at home, but also from visiting an experienced massage therapist for professional and strategic support.
Epsom Salt Baths
Epsom salt baths have many benefits, including reducing chronic inflammation, decreasing pain, supporting detoxification, supporting liver and digestive health, improving skin health, and so on. Since Epsom salt may help to draw out toxins from your body, decrease inflammation, and support relaxation, it may help to reduce edema. According to a 2021 study published in the
Journal of Clinical and Diagnostic Research for Doctors, Epson salt water may be more beneficial than foot exercises for pregnant women with edema (22). To make an Epsom salt bath add 2 cups of Epsom salt per gallon of warm water. Take a bath for 20 to 30 minutes. You may also use Epsom salt foot soaks for edema in the feet or ankles.

Essential Oils and Castor Oil
You may also try some essential oils and castor oil for edema. I particularly recommend grapefruit and fennel essential oils. According to a 2016 study published in PLoS One, citrus essential oils may help to reduce inflammation (23). According to a 2014 review published in Biomedical Research International, fennel essential oil may have antithrombotic, circulation-supporting, and anti-inflammatory properties (24).
Both oils may help to stimulate blood circulation, reduce inflammation, decrease fluid retention, and decrease related swelling. I recommend using 3 to 4 drops of grapefruit essential mixed with 1 teaspoon of coconut oil, applied 2 to 3 times a day on the affected area until the swelling has gone down.
Use fennel essential oil in a similar way by mixing 3 to 4 drops of fennel essential oil with 1 teaspoon of any carrier oil massaging into the affected area, 1 to 3 times a day. You may also add 1 to 2 drops of fennel essential oil to a cup of warm water or warm herbal tea, soak your feet or apply a soaked towel on it.
According to the book The Oil That Heals by Dr. William A. McGarey, ricinoleic acid in castor oil may offer anti-inflammatory benefits that may help to reduce swelling and edema (25). According to a 2000 research published in Mediators of Inflammation, ricinoleic acid in castor oil may offer anti-inflammatory and analgesic properties and may reduce neuropeptide-mediated neurogenic inflammation (26).
I recommend massaging castor oil gently in the affected area and wrapping it up with a compression band. Cover it, or even place a warm water bottle or heating pad on top, for warmth, to reduce pain and swelling.
Helpful Supplements
Here are some supplements I recommend:
Lymph Active
I recommend Lymph Active for lymphatic support. This lymphatic detox formulation includes slippery elm bark, which functions as a mild diuretic, Astragalus root, which supports the liver and lymphatic system, Graviola, and Chuchuhuasi, which provides adrenal support.
Additionally, we’ve added turkey rhubarb, sheep sorrel, and burdock root, whose anthraquinones, tannins, and plant sterols have antioxidant properties, and other immune system-supporting properties. Burdock root, specifically, has been shown to be particularly effective in supporting the body’s efforts to remove biofilm.
This blend of natural ingredients and our BioActive Carbon allow for effective detoxification coupled with binding and die-off symptom mitigation. This means your detox efforts are optimized while your progression toward overall wellness is maximized.
Take 1 capsule twice daily. LymphActiv can be taken with or without food. For maximum potency, we recommend taking it between meals.
KL Support
I recommend KL Support for drainage and immune support. KL Support utilizes a blend of natural ingredients to support and promote healthy kidney and liver function. As an integral part of the body’s cleansing and filtering system, proper kidney function is essential to any detox protocol.
KL Support combines herbs and nutrients traditionally used to support kidney and liver health, including beetroot, collinsonia (stoneroot), gynostemma, marshmallow root, milk thistle seed, NAC, and parsley leaf. Together, these support fat metabolism, hepatic blood flow, and healthy urinary tract and bladder function, while helping the body carry out its natural detoxification processes.
This supplement also used Carbon Technology. Carbon Technology is a proprietary blend of fulvic acids and polysaccharides that support cellular repair and the body’s natural ability to detoxify. With a low pH, Carbon Technology also helps protect ingredients from being digested by stomach acid, so that they remain intact as they enter the desired location in the body.
Our Carbon Technology helps to bind to toxins that are removed, allowing your body to flush them out. Take 2 capsules twice daily.
Plant-Based Kidney Health
I recommend Plant-Based Kidney Health for kidney and urinary support and detoxification. Kidney Health is an enhanced blend of potent, natural herbs, containing antioxidants and nutrients that cleanse the kidneys and encourage normal kidney function. Plant-Based Kidney Health is an enhanced Raw Herbal Extract blend of all-natural, organic herbs that are rich in antioxidants and specialized nutrients.
It’s formulated to gently flush the kidneys of deposits and accumulated toxins. It supports normal kidney function and defends these critical organs against the effects of an unhealthy diet, occasional stress, and harmful organisms. Shake the bottle well. Take 1 ml in the morning and again in the evening, or as directed by your healthcare provider.
Inflam Defense
Finally, I recommend Inflam Defense to reduce inflammation and support immune health. This is a combination of herbs, including turmeric, quercetin, ginger, boswellia, and rutin, nutrients and proteolytic enzymes for modulating the inflammatory response, supporting the natural clearance of proteins like kinin and fibrin, and supporting healthy lymphatic drainage.
The ingredients in Inflam Defense™ provide natural anti-inflammatory effects and protect against oxidative stress. I recommend 1 capsule twice a day away from meals or for advanced doses, 2 capsules twice a day.
Final Thoughts
But due to various issues, water can build up in your tissues in certain areas of your body, causing swelling. This swelling is called edema, which is mainly common in the skin, especially around your ankles, feet, hands, arms, and legs, but also in various organs.
I recommend that you follow natural support strategies for edema and try my favorite supplements, to reduce your risk for edema, as outlined in this article, improve edema, and regain your health and well-being.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website offers long-distance functional health coaching programs with our world-class team of health coaches. For further support with your health and other goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!







