 Blood Clotting: Symptoms, Causes, and Support Strategies
Blood Clotting: Symptoms, Causes, and Support Strategies
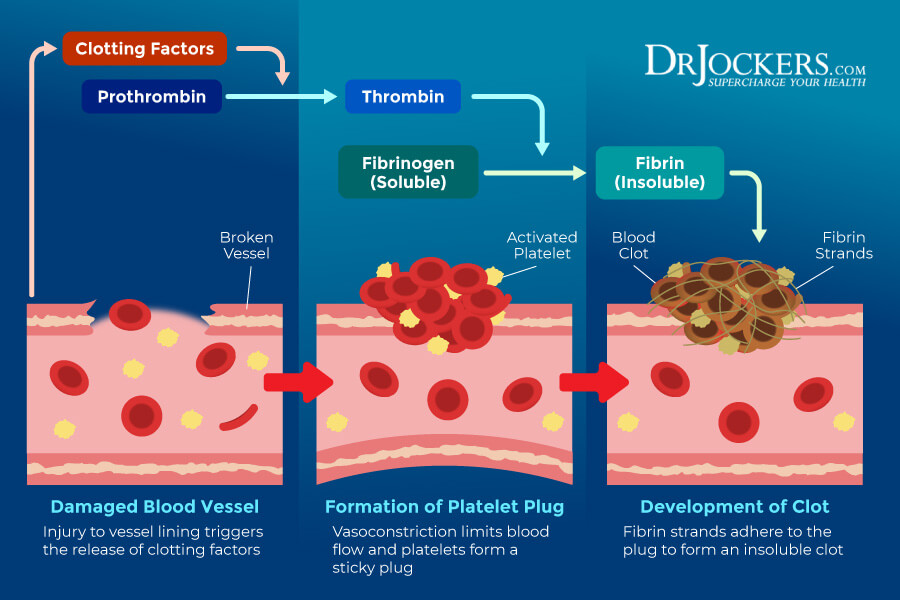
A blood clot is basically a clump of blood. Instead of the normal, not too thin, not too thick, gel-like liquid state of the blood, it turns into a semi-solid state. Blood clotting is an essential mechanism to stop bleeding and heal cuts or injuries. However, blood clots can develop inside your veins without an injury.
In some cases, blood clots resolve on their own. In other cases, blood clotting can become a serious or life-threatening issue. Fortunately, there are natural support strategies for blood clotting to improve your health.
In this article, I will go over what blood viscosity and blood clotting are. I will explain the major symptoms of poor blood viscosity. I will go over the risk factors for blood clotting. You will learn about diagnosis and conventional treatment options for blood clotting. You will understand the major functional root causes of blood clotting. I will share my top natural support strategies for blood clotting.
What is Blood Viscosity
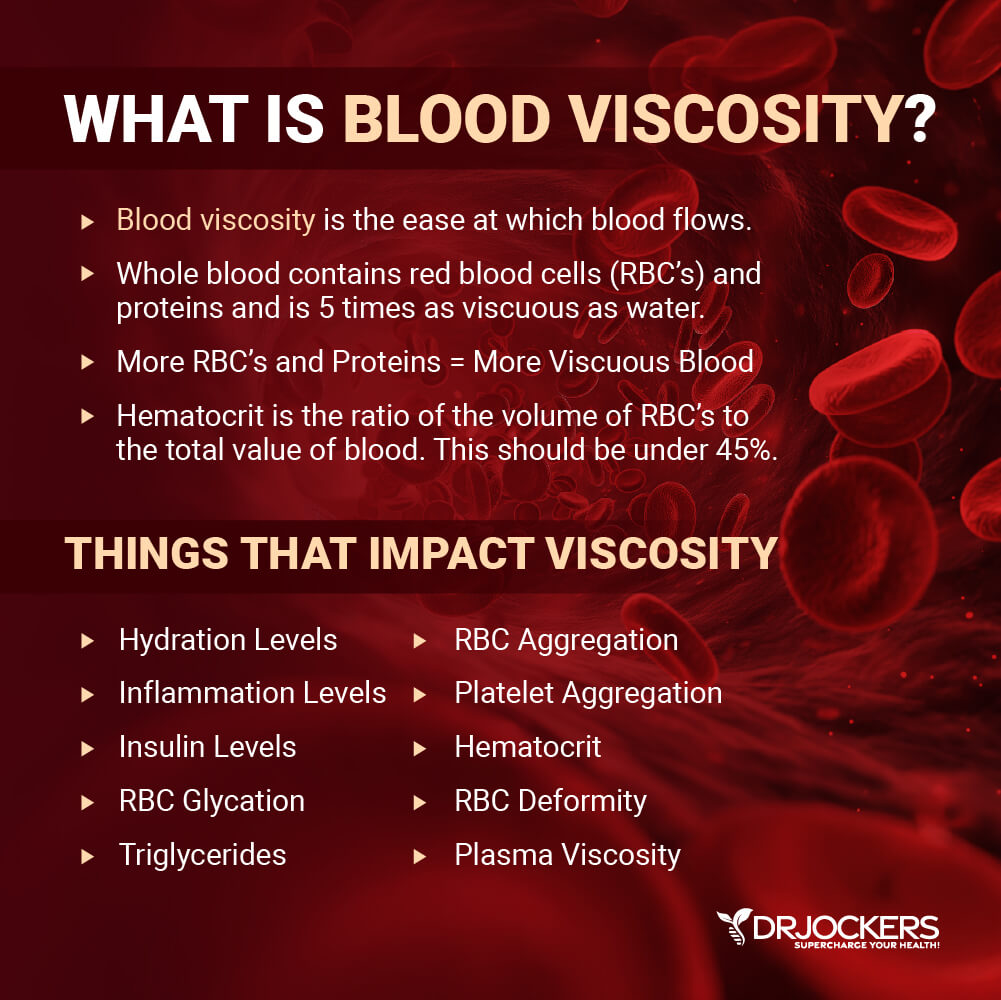
Your blood is not thin like water and not thick like ketchup but falls somewhere in-between. Viscosity is an essential characteristic of a fluid connection to the internal friction of other fluid layers close by as they pass on another. This interaction depends on the type of fluid, its chemical nature, and whether it’s homogeneous or heterogeneous.
Water, for example, is homogeneous and blood is heterogeneous in composition. Water is also a Newtonian fluid, which means that its viscosity does not depend on the flow velocity under non-turbulent conditions. The relationship between water flow and viscosity is inverse; at higher viscosities, the pressure flow will decrease.
Blood, however, works differently. Blood has a higher viscosity compared to water. It’s a non-Newtonian fluid, which means that its viscosity will increase when the velocities are at a lower flow. If your blood flow is slower, it allows more molecular interactions between your red blood cells and plasma proteins. This can cause your red cells to start sticking together bumping up your blood viscosity.
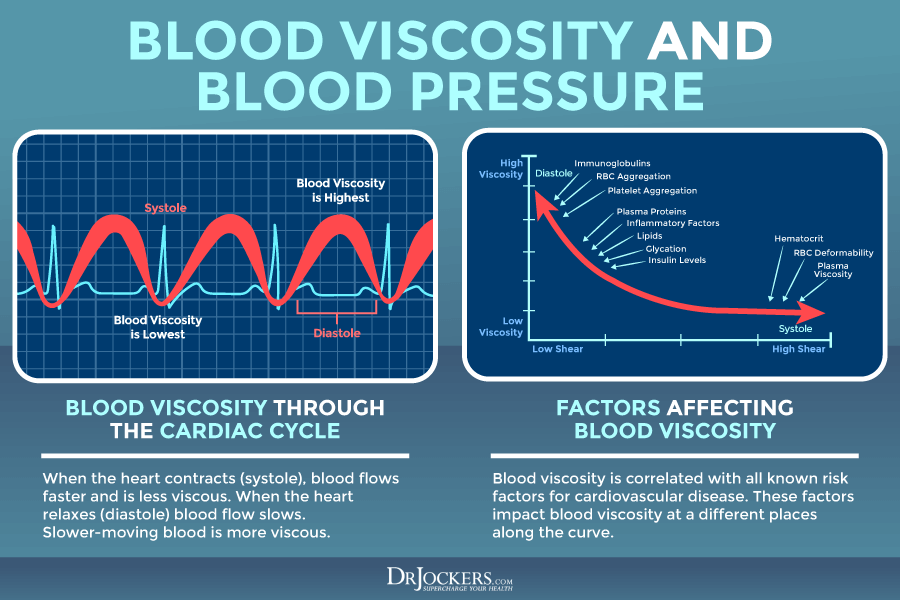
According to a 2019 study published in Frontiers in Physiology, blood viscosity can determine blood thinning or clotting behavior (1). When your blood doesn’t flow properly, it can cause blood clotting, which increases blood viscosity. A blood clot is basically a clump of blood. Instead of the normal liquid state of the blood, it turns into a semi-solid state.
Clotting is a very important mechanism if you have a cut or another injury. It will prevent major blood loss and help to heal. However, clots can also form in your veins. In some cases, these blood clots resolve on their own. In other cases, they can turn into a serious or even life-threatening problem. Blood clots that travel to your lungs or heart can interfere with blood flow and become a medical emergency.
Major Symptoms of Poor Blood Viscosity
Major symptoms of poor blood viscosity may depend on the problem and the location of the potential blood clot.
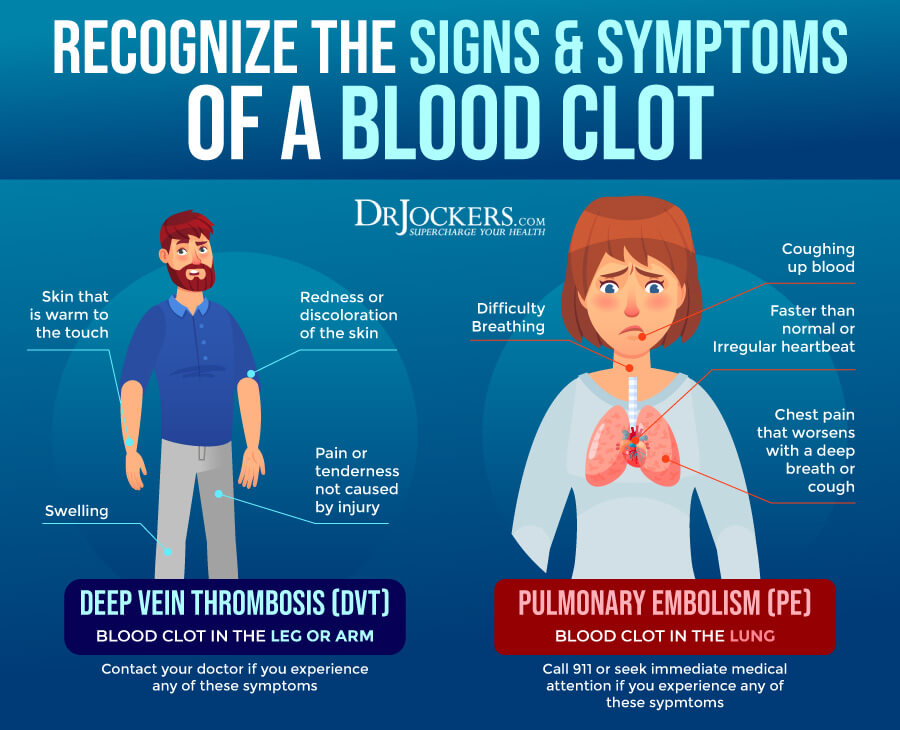
Symptoms of blood clots in the legs or arms may include:
- Pain
- Swelling
- Tenderness
- Reddish skin color
- Warmth to touch
Symptoms of a blood clot in the abdomen may include:
- Stomach swelling
- Pain
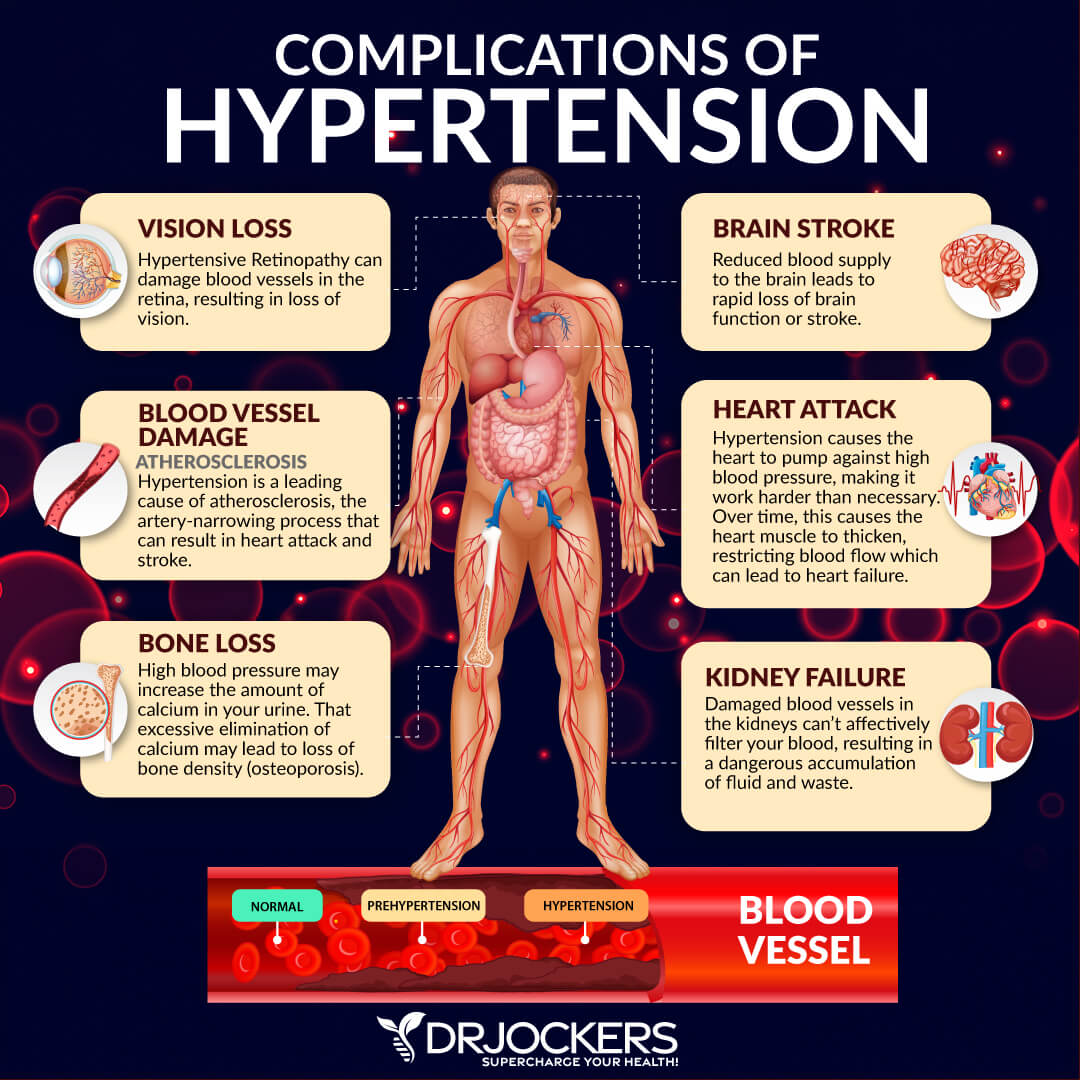
Symptoms of a blood clot in the heart (heart attack) may include:
- Shortness of breath
- Chest pain
- Fatigue
- Lightheadedness
- Nausea
- Pain or discomfort in the arms, jaw, neck, or back
Symptoms of a blood clot in the brain (stroke) may include:
- Severe headache
- Difficulty seeing
- Difficulty speaking
- Confusion
- Numbness or weakness in the face, arm, or leg
- Loss of balance
- Lack of coordination
Symptoms of a blood clot in the lung (pulmonary embolism) may include:
- Chest pain
- Shortness of breath and other breathing issues
- Cough up blood
- Rapid heart rate
Hyperviscosity syndrome is a problem that interferes with healthy blood flow. Symptoms may include:
- Headaches
- Seizures
- Reddish skin
- Abnormal bleeding.
- Vertigo
- Visual disturbances
- Shortness of breath
- Chest pain
- Difficulty walking
- Seizures
- Coma
Risk Factors for Blood Clotting
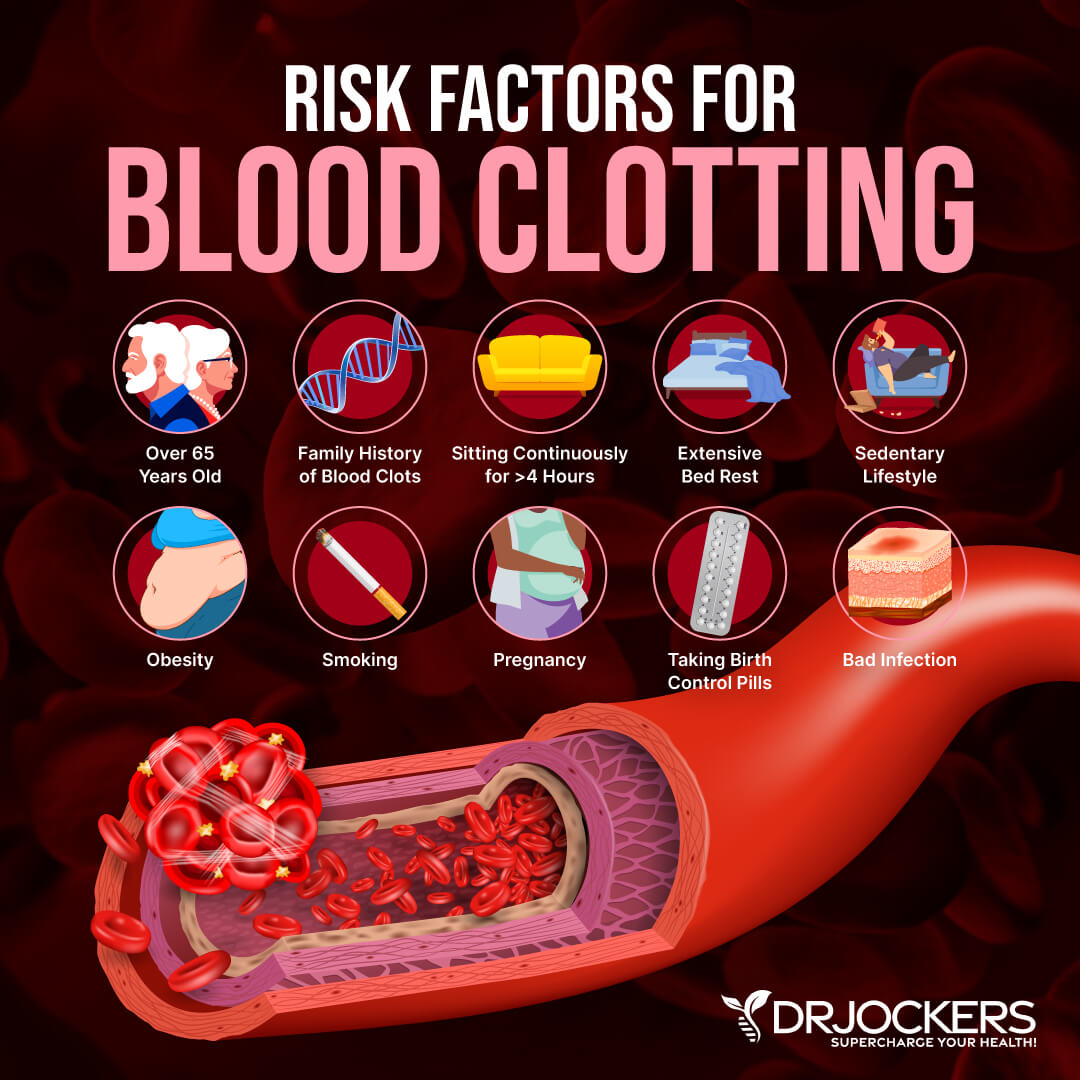
Risk factors for blood clotting may include:
- Being over the age of 65
- Family history of blood clots
- Long travel that forces you to sit for over 4 hours
- Extensive bed rest or being sedentary
- Obesity
- Smoking
- Pregnancy
- Taking birth control pills
Diagnosis of Blood Clotting
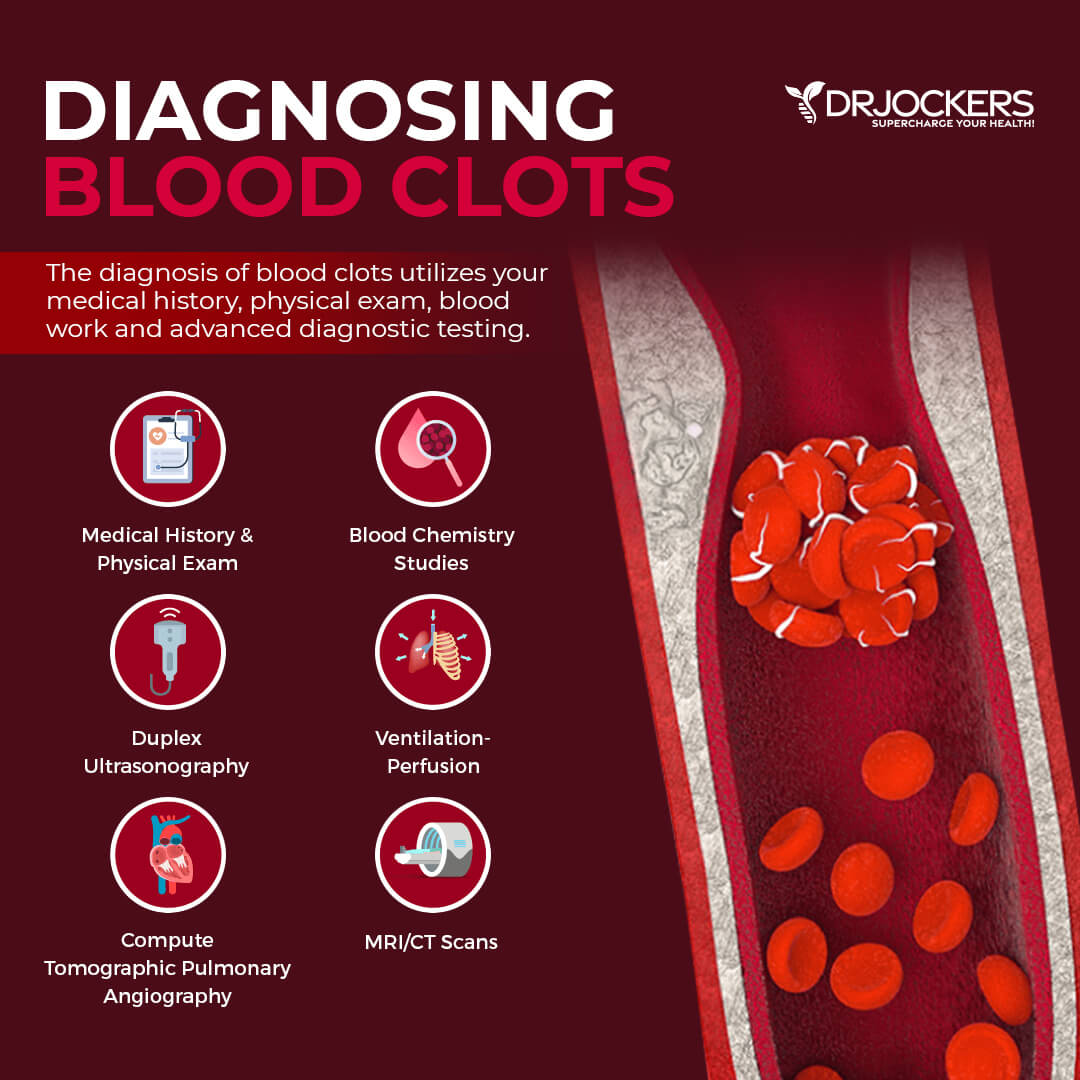
Your doctor will go over your health history and symptoms and perform a physical. According to the Centers for Disease Control and Prevention (CDC), understanding your symptoms can help to differentiate between various issues, such as deep vein thrombosis (DVT) and pulmonary embolism (PE) (2).
For further diagnosis, imaging tests, such as duplex ultrasonography look at the blood flow in your veins to detect clots, computed tomographic pulmonary angiography (CTPA) looking at the blood vessels of your lungs, ventilation-perfusion (V/Q) looking at the oxygen in your lungs, a pulmonary angiography looking inside your veins, or magnetic resonance imaging (MRI) looking at your lungs. Your doctor may also order a d-dimer blood test looking for a substance released when a clot breaks up.
Conventional Treatments for Blood Clotting
Conventional treatment methods often involve anticoagulants, or blood thinners, that help to reduce your blood’s ability to clot and reduce the risk of further cloths. Depending on your case, you may be prescribed injectable or oral anticoagulants or both. For blood clots in the leg, compression stockings are commonly recommended.
Thrombolytics or clot busters are often used to help dissolve the clot. An inferior vena cava filter may be inserted if the anticoagulants don’t work. They are inserted into the inferior vena cava to capture the clot before getting into the lung. In serious and rare cases, a thrombectomy or embolectomy is necessary to remove the clot in those with DVT. Sometimes stents are used to keep the blood vessel open.

Functional Root Causes of Blood Clotting
Understanding the risk factors of blood clotting is not enough. You have to understand the functional root causes of blood clotting as well. These functional root causes can increase your risk of health issues that may contribute to or increase your risk of blood clotting.
Insulin Resistance
Insulin resistance means that your body is unable to respond to insulin well and unable to use blood glucose for insulin. This will force your pancreas to make more insulin and make your blood sugar levels go up over time. Insulin resistance can increase your risk of blood sugar fluctuation, prediabetes, and type 2 diabetes. It may also contribute to various health issues, including blood clotting.
A 2006 study published in Diabetes has found that patients with insulin resistance and hyperglycemia are at a higher risk of thrombotic events (3). This may happen because too much insulin interferes with fibrinolysis, and too much glucose triggers coagulation. A 2000 comparative study published in the Journal of Medicine has also found that people with type 2 diabetes often have problems with blood coagulation, and a glucose clamp (GC) may help (4).

Iron Overload
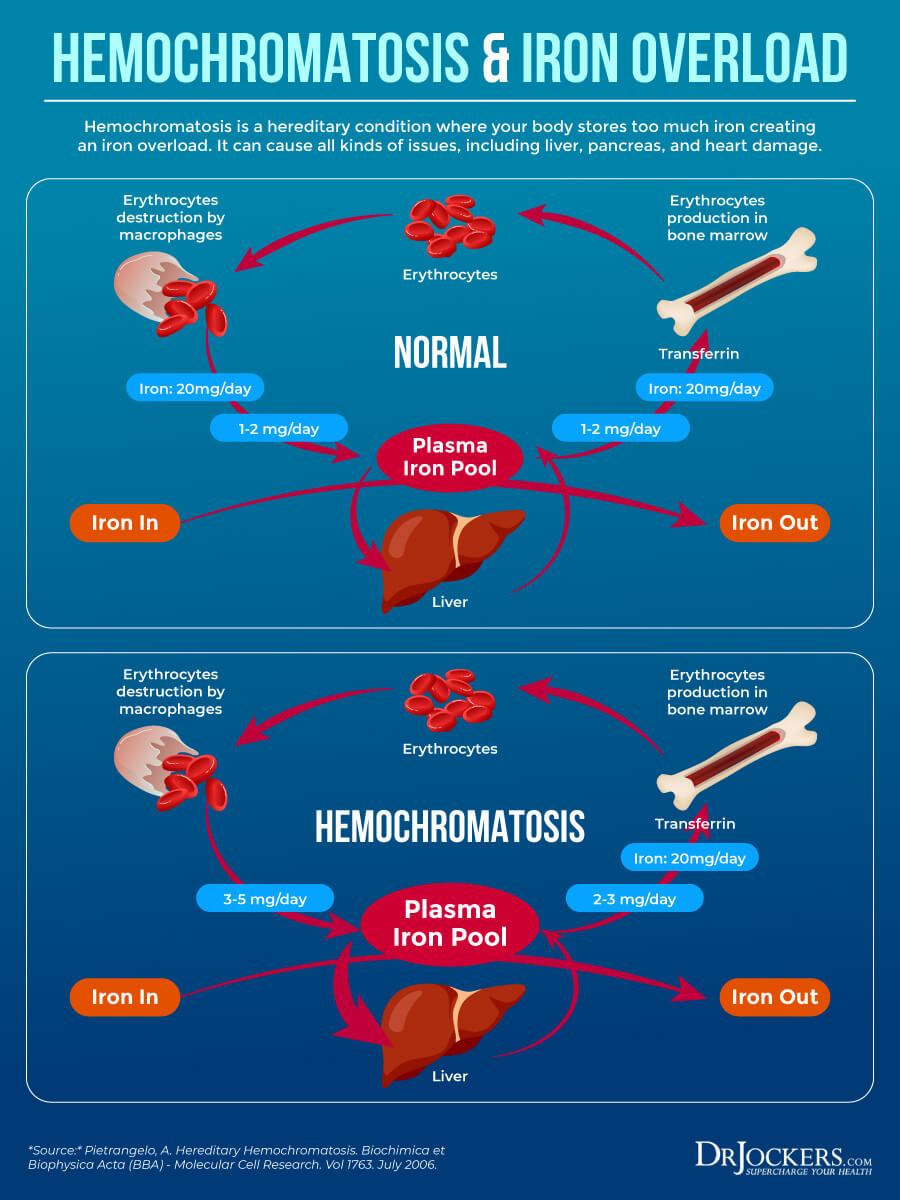
Iron is essential for your energy, focus, immune health, digestion, and other areas of your health. However, too much iron can become a problem. Hemochromatosis means that your body is absorbing too much iron from your food. This excess iron ends up being stored in your organs, including your pancreas, liver, and heart. It can lead to serious health issues, including diabetes, liver disease, and heart disease. Hereditary hemochromatosis is caused by a gene mutation.
Hemoglobin is a protein in your red blood cells. Hematocrit is the measurement of the percentage by volume of red blood cells in your blood. Both of these measurements can help diagnose too much iron or too little (anemia).
Normal hemoglobin levels are 13 to 17.7 g/dL for adult men, and 11.1 to 15.9 g/dL for adult women. Normal hematocrit (Hct) levels are between 37.5% and 51% percent for adult men and 34% to 46% for adult women. Higher levels are more common in men and post-menopausal women. With this said, we look at functional ranges which are much tighter because we are looking for functional imbalances as opposed to a clinical disease. I discuss those ranges in the lab testing section below.
Higher levels and iron overload may increase your risk of blood clotting, deep vein thrombosis, and stroke. According to a 2007 review published in the Annals of Hematology, both iron overload and iron-deficiency anemia can increase the risk of thrombosis and related cardiac events (5). A 2019 study published in the Journal of the American Heart Association has also found that higher iron levels may increase the risk of blood clotting and thrombosis (6).
Chronic Infections
Chronic infections, including viral, bacterial, and fungal infections, can impact your entire body and increase your risk of various health issues, including blood clotting. A 2012 study published in Zhejiang Da Xue Xue Bao Yi Xue Ban (Chinese) has found that H. Pylori bacteria can increase coagulation and cause blood clotting (7). A 2015 study published in Terapevticheskii Arkhiv (Russian) has found that Borrelia infection related to Lyme disease can cause blood clotting (8).
A 2020 study published in Medical Hypothesis has found that blood clots are common in COVID-19 patients (9). More than 33 percent of patients have elevated D-dimer results or high levels of blood clotting. A 2021 research published in Medical Hypothesis has also found that thrombosis is a serious concern in COVID-19 (10). This may be happening because of a high ACE2 expression in the endothelium of blood vessels binging with the spike protein of the virus causing an injury to the blood vessels.
Even your oral and dental health matters. Poor oral and dental health and oral infections can contribute to blood clots. A 2012 study published in the Society for General Microbiology has found that oral bacteria can escape from your oral cavity right into your bloodstream (11). This can lead to blood clots and heart disease.

Vitamin D Deficiency
Vitamin D is an essential vitamin that plays a critical role in many areas of your health, including bone, immune, and brain health. It can also bind to vitamin D-binding proteins and take them to various target organs as necessary. Vitamin D deficiency can cause various issues, including blood clotting.
A 2017 study published in Hematology has found that vitamin D deficiency and increased platelets can affect your blood health (12). A 2020 study published in Nutrients has also found that vitamin D deficiency can affect platelet levels and can lead to cardiovascular risks (13).
A 2019 review published in Biomolecules has found that vitamin D deficiency can increase the risk of thrombotic episodes (14). Researchers found that sunshine or vitamin D may have anti-thrombotic effects.

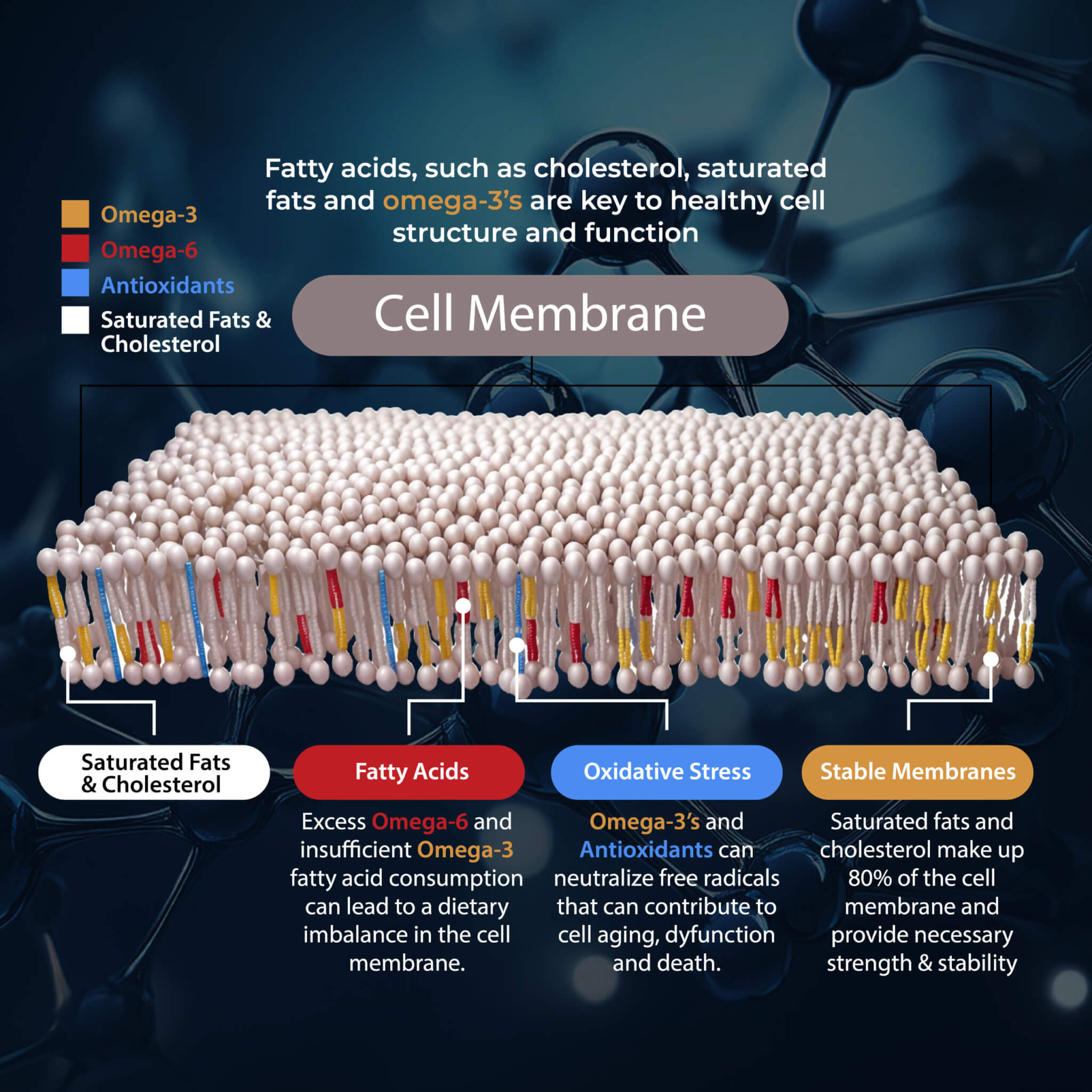
High Omega 6:3 Ratio
Omega-3 and omega-6 are two important fatty acids. Omega 3 offers anti-inflammatory benefits. While omega-6, at a certain level, is also important for your health, it has inflammatory properties, and too much is not good. Keeping a low omega 6:3 ratio is important for your health. A high omega 6:3 ratio can increase the risk of various health issues, including blood clotting.
A 2018 study published in Prostaglandins and Other Lipid Mediators has found that omega-6 and 3 fatty acids and a healthy ratio is important for healthy platelet function and reducing the risk of thrombosis (15). A 2019 study published in Open Heart has found that a low omega-6:omega-3 ratio is essential for reducing the risk of blood clotting, thrombosis, and platelet aggregation (16).
B Vitamin Deficiency
B vitamins are critical for your nerves, brain, and mental health. They are also essential for the growth of your blood cells and cellular growth. Deficiencies in B vitamins may increase the risk of blood clotting and other health issues.
A 2002 retrospective case and control study published in the Annals of Hematology has found that vitamin B12 and folate deficiency can increase the risk of thrombosis (17). A 2011 case and control study published in the International Journal of Hematology has also found that vitamin B12 deficiency and malabsorption may be linked to the increased risk of thrombosis and hyperhomocysteinemia (18). A 2012 systematic review and meta-analysis published in the Journal of Thrombosis and Thrombolysis has found that B vitamin deficiencies may increase the risk of blood clotting and thrombosis (19).

Heavy Metal Exposure
Heavy metal exposure can also increase your risk of blood clotting. Mercury is a heavy metal that people are commonly exposed to through mercury amalgam dental fillings, root canals, and mercury-containing fish. A 2010 study published in Environmental Health Perspectives has found that even low levels of mercury exposure can increase mercury-related thrombotic events (20).
Lead is another heavy metal that you may get exposed to through lead-based paint, tap water coming from old water pipes, or lead dust in furniture, clothes, or toys. A 2018 study published in the Environmental Science and Pollution Research Institute has found that lead exposure in preschool-age children can negatively affect coagulation (21).
A 2007 study published in Chemical Research in Toxicology has found that increased exposure to lead may increase the risk of thrombotic events (22). A 2014 research on people working at a lead-acid battery manufacturing plant published in the Journal of Exposure Science and Environmental Epidemiology has found that lead exposure can affect platelet count and blood coagulation (23).
Cadmium is another heavy metal with toxic effects. People commonly get exposed to cadmium through cigarette smoke and food grown in contaminated soil. A 2006 study published in Pathophysiology of Haemostatis and Thrombosis has found that chronic cadmium exposure can affect coagulation and increase the risk of thrombosis (24).

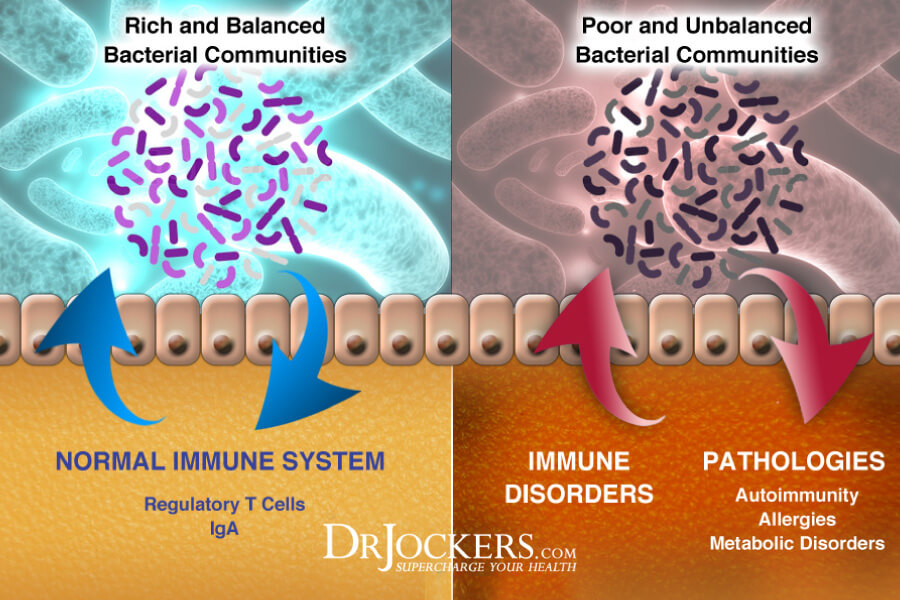
Gut Dysbiosis
Your gut is the home of trillions of bacteria. Some are beneficial, some are not. They need to live in healthy homeostasis with more beneficial bacteria than harmful ones. If the homeostasis gets interrupted and your microbiome becomes out of balance, you develop gut dysbiosis with more harmful bacteria than beneficial ones. Gut dysbiosis can increase the risk of various health issues, including blood clotting and thrombotic events.
A 2020 review published in Thrombosis Research has found that your gut microbiome health plays a role in the prevention or development of thromboembolism (26). Researchers found that certain bacteria can promote trimethylamine-N-oxide (TMAO), which may cause platelet hyperreactivity and thrombus formation.
Improving the gut microbiome and TMAO levels is critical for lowering the risk of thrombosis. A 2019 study published in HemaSphere has found that your microbiome plays a role in the development of thrombosis and reducing gut dysbiosis may help to reduce the risk of thrombosis (25).
High Stress, Poor Sleep & Sedentary Lifestyle
High stress, poor sleep, and leading a sedentary lifestyle are all poor lifestyle factors that may increase the risk of blood clotting, among many other health issues. A 2008 study by the University of Bonn found that anxiety may increase the risk of blood clots (27). A 2015 study published in Thrombosis Research has found that acute mental stress can increase the risk of thrombotic events (28).
A 2009 study published in Haematologica has found that sleep deprivation may affect blood coagulation (29). A 2011 study published in the Canadian Respiratory Journal found that sleep apnea may affect blood clotting (30).
A 2011 study published in BMJ has found that long periods of sitting can increase the risk of pulmonary embolism (31). A 2016 study published in Medicine & Science in Sports & Exercise has found that physical inactivity and poor physical fitness may increase the risk of thrombosis while regular exercise may help (32).

Major Lab Tests to Look At
To determine your risk factors for clogged arteries, I recommend a few major lab tests to look at. Getting a Comprehensive Blood Analysis is a great blood test that allows us to look at all these factors of your health.

 Blood Cell and Iron Metabolism Markers
Blood Cell and Iron Metabolism Markers
Hematocrit: This is the whole blood volume that consists of red blood cells. This can be low in iron deficient anemia or if excessive bleeding has occurred. This value may be high in times of blood clotting or in cases of dehydration or polycythemia, which is the overproduction of hemoglobin.
The clinical lab ranges are between 34-46.6%. The functional ranges for men are 39-45% while for women they are between 37-44%. Anything over 45% is a concern for reduced blood viscosity.
Hemoglobin: The functional or optimal range for hemoglobin is 13.5 to 14.5 g/dL for women and 14 to 15 g/dL for men. High levels can be linked to poor blood viscosity or high iron (possible hemochromatosis) and low levels can be a sign of functional anemia.
Serum Iron: Serum iron may be elevated with poor blood viscosity and it is always elevated with hemochromatosis. The lab range for serum iron is 27-159 ug/dL while the functional range is 85-130 ug/dL. Low levels would be related to anemia.
Ferritin: This is a blood cell protein that contains iron. This is the most reliable indicator of total iron status in the body. When it is low it indicates iron deficiency. This is the first marker for early iron depletion. However, ferritin is an acute phase reactant and is elevated with inflammatory conditions. High ferritin over 150 is a sign of oxidative stress and is often associated with poor blood viscosity.

Blood Clotting Markers
There are a few labs that look at blood clotting markers.
Fibrinogen is a protein produced by the liver. This protein helps stop bleeding by helping blood clots to form. High levels of fibrinogen can indicate chronic inflammatory conditions and increased blood clotting formation. The optimal level should be between 150-285 mg/dL.
As a signaling molecule for tissue repair, fibrinogen is a good marker for how well your body is able to repair itself. If your fibrinogen is optimal, your repair and recovery are probably meeting or outpacing wear and tear, allowing you to properly heal and recover.
Above 285, you are probably deteriorating more rapidly than you’re repairing. Fibrinogen is also a clotting factor marker, so in viral or bacterial infections, for example, high fibrinogen is indicative of a cytokine storm. Pre-cytokine storm levels are also indicative of several chronic diseases, including heart attack and cancer.
Platelets: High platelets are associated with increased inflammation or if they are very high (over 400) it can be a sign of a coagulation disorder called thrombocytosis and is typically due to chronic inflammation. Anything over 250 can be an issue if you see other inflammatory and blood clotting markers elevated.
ESR: The erythrocyte sedimentation rate (ESR) is a common hematology test to look for inflammation It refers to the rate at which your red blood cells in anticoagulated whole blood go down in a standardized tube over a period of one hour. This should be less than 10 mm/hr for good blood viscosity levels. The clinical range is 0-40 mm/hr, so it is rare to see this flagged but common to see a functional high level.

Blood Sugar
I recommend looking at your blood sugar levels:
- HbA1C: The ideal number is between 4 and 5.2%. 5.3-5.6% is moderately high. Between 5.7 and 6.4 means that you have prediabetes and a high risk of developing diabetes, and over 6.4 means that you have diabetes.
- Fasting Glucose: Optimal levels are under 90 mg/dL. Less than 100 mg/dL (5.6 mmol/L) is considered normal. 100 to 125 mg/dL (5.6 to 6.9 mmol/L) is considered prediabetes. 126 mg/dL (7 mmol/L) or higher on two separate tests means you have diabetes.
- Fasting Insulin: Optimal fasting insulin levels are between 2-5 uIu/mL. Between 6-9 uIu/mL is early insulin resistance and anything over 10uIu/mL is insulin resistance. This won’t be flagged on the lab until it is over 24.9 uIu/mL which is a state of severe insulin resistance.
Inflammatory Markers
I recommend looking at your inflammatory markers:
- HsCRP: The ideal number is under 1.
- LDH (lactose dehydrogenase): The optimal range is 140 to 180. High levels indicate chronic inflammation
- Serum ferritin: The ideal range is between 50-150. High levels indicate inflammation.
- Homocysteine: The optimal range is 6 to 9.

Comprehensive Blood Analysis
To check for these health markers, I recommend a Comprehensive Blood Analysis (CBA). This is the most detailed blood test that looks at all of these markers of inflammation. This test is more sophisticated than most conventional doctors are able to order.
It examines all parameters for inflammation, blood sugar levels, thyroid function, zinc and copper ratio, vitamin A and D levels, a complete metabolic panel, complete blood count, liver function, nutrient deficiencies, and more. I recommend getting the Comprehensive Blood Analysis done regularly both as a preventative measure and to monitor your inflammation levels and progress.

Natural Support Strategies for Blood Clotting
The good news is that there are some natural support strategies for blood clotting that may improve your health and well-being. He is what I recommend:
Anti-Inflammatory Nutrition Plan
A 2020 study published in Circulation Research has found that diet plays a role in blood clotting and an anti-inflammatory diet may help (33). I recommend removing all inflammatory foods, including refined sugar, refined oil, gluten, conventional dairy, processed and canned meat, additives, artificial ingredients, non-organic produce with pesticides or hormones, junk food, and highly processed foods.
Since cancer feeds on sugar, eating a low-carbohydrate diet is critical. If you are looking for sweetness, choose low-glycemic index, high-antioxidant berries instead of high-glycemic index foods.
Follow an anti-inflammatory nutrition plan with plenty of greens, vegetables, herbs, spices, fermented foods, grass-fed meat and butter, pasture-raised poultry and eggs, organ meats, wild-caught fish, and wild game. Eat plenty of healthy fats, including omega-3-rich fish and seafood, nuts and seeds, avocados, grass-fed butter and ghee, olives, and coconut oil.
Use anti-inflammatory and antioxidant-rich herbs and spices in your cooking, including turmeric, ginger, cinnamon, basil, rosemary, dill, cloves, cayenne pepper, black pepper, onion, and garlic. If you are taking any blood-thinner medication, avoid consuming turmeric and other blood-thinning foods. Consult your doctor about what you can or cannot eat.

Intermittent Fasting
Research has shown that insulin resistance may increase the risk of blood clotting (3, 4). Intermittent fasting may help to reduce these factors. Intermittent fasting is a form of fasting that cycles between periods of fasting (not eating) and feasting (eating) within one day. It offers a number of benefits, including better insulin sensitivity, improved gut health, and cellular regeneration.
A 2019 systematic review and meta-analysis published in the Journal of Clinical Medicine has found that intermittent fasting may reduce insulin resistance, improve glucose metabolism, and reduce body mass index (34). A 2005 study published in the Annals of Nutrition & Metabolism has found that intermittent fasting may improve coagulation status, plasma homocysteine levels, and serum lipids (35).
If you are new to intermittent fasting, start with 12 hours of fasting, including your overnight sleep. Then, gradually increase your fasting period over time. Most people feel the best with 16 hours of fasting a day. However, you may feel your best with a slightly longer or shorter fasting window. You can learn more about intermittent fasting and the best intermittent fasting strategies by searching my website.

Get Regular Blood Work or Donate Blood
Research has shown that high iron overload may increase the risk of blood clotting (5, 6). If you have high iron, high HGB, and/or high HCT levels, I recommend getting regular blood work or donating blood regularly to check your levels. Therapeutic phlebotomy is the practice of regularly removing blood from someone to reduce iron overload.
According to the National Institute of Health (NIH) Blood Bank, one unit or one pint of blood contains about 250 mg of iron (36). Removing 1 pint of blood every 1 to 16 weeks depending on your specific situation can reduce iron overload.
While hemochromatosis is a metabolic, not a blood disorder, not all blood donation centers accept blood from those with hemochromatosis. Getting regular blood work is another way to remove the blood and reduce iron load regularly. It is also a great way to check the status of various health markers.

Optimize Vitamin D Levels
Research has shown that vitamin D deficiency may contribute to a higher risk of blood clotting (12, 13, 14). Optimizing your vitamin D levels may help. A 2021 study published in Molecular and Cellular Biochemistry has found that vitamin D may help to reduce COVID-19-related blood clotting (37). A 2021 review published in the Journal of Inflammatory Research has also found that vitamin D may improve coagulation issues related to sepsis (38).
To improve your vitamin D levels, I recommend time outside in the sun every day. Unfortunately, it may not be possible on gloomy days or if you live in Northern states or colder countries to meet your daily sunshine requirements. Our indoor lifestyle may also compromise our ability to get as much sun as our ancestors did.
Most people are not getting enough sunshine or consuming enough vitamin D from food. Therefore, most people need supplements to optimize their vitamin D levels. Pairing vitamin D3 with vitamin K2 helps improve calcium absorption and inflammation control. I recommend taking a vitamin D3 supplement with at least 3,000-5,000 IU of vitamin D3 and at least 90 mcg of vitamin K2.
Typically, taking 1,000 IU per 25 lbs. of body weight will help you get your levels into a healthy range. You want to test your vitamin D levels at least 1-2 times each year and get your levels between 50-100 ng/ml. It has been hypothesized that a therapeutic level for major health conditions is going to be between 70-100 ng/ml.

Regular Movement and Exercise
Research has shown that a sedentary lifestyle, sitting too much, and poor physical fitness can increase the risk of blood clotting (31, 32). Regular movement and exercise are critical.
Begin your day by stretching, a yoga session, or a short walk. Stay active throughout the day by getting up to shake your legs and stretch, taking a walk during lunch or the evening, biking or walking instead of driving when possible, playing with your kids or pets, taking an impromptu dance break, and choosing the stairs over the elevator.
Avoid sitting for an extended period of time. Choose a standing desk if possible. Get up during work to stretch and move around a bit at least once every hour. Take some breaks during road trips. If you are on a long plane, bus, or train ride, try to get up regularly and move your legs or stretch as much as possible.
Exercise regularly, at least 20 to 30 minutes 5 times a week. Use a mix of cardiovascular workouts, strength and resistance training, and low-impact workouts. If you are on bed rest due to a surgery or health issue, talk to your doctor and physical therapist to see what movements or strategies you can use to avoid blood clotting. After a bed rest period, work with a physical therapist to get back into activity safely.

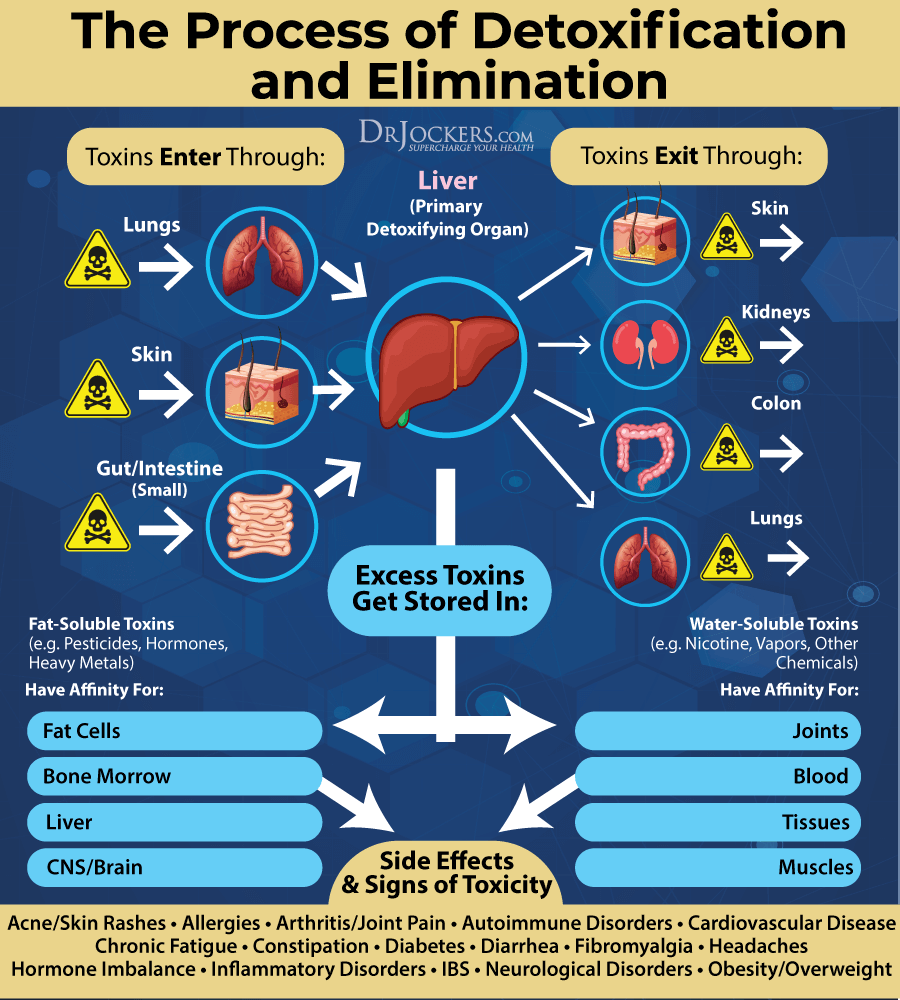
Good Hydration & Detoxification
Research has shown that heavy metal toxicity may increase your risk of blood clotting (20, 21, 22, 23, 24). Practicing good hydration, improving detoxification, and reducing toxins are critical for reducing your health risks. Drink lots of water to support hydration and detoxification through sweating and urine.
Choose filtered, purified water or tap water. Avoid drinking from plastic bottles. Choose glass or aluminum bottles, glass mason jars, other glassware, or ceramic mugs instead. Add some lemon juice, cucumbers, or berries to your water for flavor and vitamins. Eat plenty of hydrating vegetables and fruits and drink green juices, green smoothies, and protein shakes for extra hydration.
Choose organic food and organic, natural products, and reduce any other exposure to chemicals or toxins. If you have any mercury amalgam fillings, visit a biological dentist to safely remove them. Use a high-quality indoor air filtration and water filtration system to improve the air you breathe in and the water you drink. Avoid smoking and second-hand smoke. Spend time in nature to breathe in the fresh air.
Use activated coconut charcoal to remove toxins from your intestinal tract. Follow an antioxidant-rich, anti-inflammatory nutrition plan and take high-quality probiotics to improve your body’s ability to fight toxins and to support elimination. Try infrared saunas to promote detoxification through sweating. Practice rebounding and dry-skin brushing to support your lymphatic pathways. Support your two major detoxifying organs, your kidneys and liver, with kidney and liver support supplements.
Reduce Stress & Optimize Sleep
Research has shown that high stress and poor sleep can increase your risk of blood clotting (27, 28, 29, 30). Reducing stress and optimizing your sleep can help to reduce your risk and improve your health.
To reduce stress, I recommend practicing meditation, breathwork, gratitude, journaling, muscle relaxation strategies, guided visualizations, positive affirmations, yoga, Tai Chi, and prayer. Spend time in nature. Seek out a supporting community. Take part in uplifting activities with friends and family.
Have some dedicated personal time as well, no matter how short it is, you need some me-time for yourself to recharge your batteries. If you are experiencing depression or anxiety, you may benefit from support from a therapist, counselor, life coach, or spiritual counselor.
Sleeping 7 to 9 hours a night is critical. To improve your sleep, I recommend that you develop a relaxing bedtime routine that works for you. Turn down electronics and avoid sugar, heavy foods, and alcohol several hours before going to sleep. Reading, crossword puzzles, coloring, arts and crafts, journaling, listening to calming music, and meditation are beneficial and relaxing ideas to wind you down. Follow a regular sleep schedule that supports your body’s circadian rhythms. Invest in a supportive bed and comfortable bedding and pillows.

Take Omega-3 Fatty Acids
Research has shown that a poor omega 3:6 ratio can increase your risk of blood clotting (15, 16). A 2015 study published in Seminars in Thrombosis and Hemostasis has found that taking omega-3 fatty acids may decrease thrombotic potential in patients with cardiovascular disease (39).
A 2021 study published in the International Journal of Molecular Sciences has found that omega-3 fatty acids may have antithrombotic and other benefits for cardiovascular disease and may be supportive for COVID-19 (40). I recommend consuming foods rich in omega-3 fatty acids, such as fatty fish and seafood. I also recommend taking a high-quality omega-3 fish oil supplement daily.

Optimize B Vitamin Levels
Research has shown that B vitamin deficiencies may increase your risk of blood clotting (17, 18, 19). Optimizing your vitamin B levels may help. I recommend consuming foods rich in B vitamins, including liver, meat, seafood, poultry, leafy greens, and seeds.
Additionally, I recommend taking a daily high-quality B-12 and or a good multi-vitamin or B complex supplement to ensure optimal B vitamin levels. This is especially important if you have a high homocysteine level over 9 or have been tested to have low B12 or folate levels.

Use Probiotics
Research has shown that gut dysbiosis may increase your risk of blood clotting (26, 25). Research has also shown that chronic infections, including bacterial infections, that may interrupt the gut microbiome, can also increase the risk of blood clotting (7, 8, 9, 10, 11). Using probiotics can help to improve your microbiome and reduce your risk.
A 2009 study published in the Journal of Inflammation (London) has found that Lactobacillus Casei probiotics may help to regulate coagulation and reduce blood clotting (41). A 2013 study published in International Immunopharmacology has found that probiotics may help to reduce virus-induced inflammation-related coagulation issues and pulmonary damage (42).
I recommend consuming probiotic-rich foods and drinks, such as pickles, kimchi, sauerkraut, fermented foods, coconut kefir, and kombucha. I also recommend taking a daily dose of high-quality probiotic supplements.

Consider Sauna Therapy
Infrared sauna therapy is a form of sauna that uses infrared heaters that release infrared lights you experience as heat as it gets absorbed through the surface of the skin. Infrared sauna therapy uses Far Infrared Technology (FIR), which is a non-invasive light therapy that can penetrate your body as much as three inches. It used FIR wavelengths between 5.6 and 20 microns.
Through this process, infrared sauna therapy heats your muscle tissues and internal organs without heating the surrounding air. This heat helps your organs and tissues to detoxify and pushes tissues to your bloodstream to eliminate through perspiration or sweating.
The infrared wavelengths of infrared sauna therapy are able to decrease stress, stimulate multiple pathways throughout the body and support metabolic pathways, improve immune function, kill pathogenic organisms, support kidney filtration and liver detoxification, aid weight loss, and reduce health issues.
A 2011 review published in Alternative Medicine Review and a 2012 review published in Photonics Laser Medicine have both found that infrared sauna therapy can improve various health issues (43, 44). A 2015 study published in JAMA Internal Medicine has found that sauna therapy can reduce the risk of cardiovascular events and related mortality (45). A 2019 study published in the European Journal of Epidemiology has found that sauna therapy may reduce the risk of venous thromboembolism (46).

The FIR technology of infrared sauna therapy can penetrate the body 1.5 to 3 inches below the surface level. It helps to reduce the size of water clusters inside your body allowing them greater mobility and easier access to body tissues.
This helps to enhance cell membrane tone and functionality, nutrient absorption, circulatory patterns, and detoxification. It can also improve lymphatic and blood circulation, reduce inflammation, improve microcirculation throughout your body, lower lactic acid, and increase oxygen delivery to your cells.
If you are new to infrared sauna therapy, you can start with a short 5-minute session and build up over time to a 20-minute session or longer. Using it in the evening can help you sleep while using it in the morning can help you to start your day relaxed and rested. If you have time, you may fit two sauna sessions into your day.
There are also a few strategies you can try to enhance your benefits:
- Exercise before using your infrared sauna to start heating up your body, sweating, and detoxing. Rebounding is a great option for lymphatic and cardiovascular benefits.
- Take a shower before to heat up your body a bit and remove any external toxins.
- Try dry brushing before your sauna therapy session to stimulate your lymphatic system and remove dead skin cells.
- Use niacin (vitamin B3), which enhances toxin release, then exercise to kick-start your sweating process before your sauna therapy session.
- Take activated charcoal after your session to help internal detoxification.
- Eat a nutrient-dense organic diet, lower toxic exposure, exercise, reduce stress, and make healthy lifestyle choices to support detoxification, cellular repair, and rejuvenation.

Consider Proteolytic Enzymes
Proteolytic enzymes are important enzymes that help to break down food, reduce digestive issues, decrease inflammation, and support your health through various health issues, including blood clotting. A 2017 review published in the International Journal of Molecular Sciences has found that nattokinase may be a beneficial antithrombotic agent to reduce the risk of cardiovascular disease (47).
A 2021 study published in Frontiers in Pharmacology has found that serratiopeptidase may offer anti-inflammatory, mucolytic, and fibrinolytic properties, may reduce and degrade blood clots, and may be helpful in the management of COVID-19 (48). A 2017 study published in the Asian Journal of Pharmaceutical Sciences has found serratiopeptidase offers anti-inflammatory properties, which may be beneficial for blood clotting (49).

Consider Turmeric or Curcumin
Turmeric is one of the most researched spices for its anti-inflammatory and health-protective properties. The benefits of turmeric come from its active ingredient, curcumin. Turmeric can be beneficial for a variety of issues from inflammatory conditions to pain, from digestive issues to headaches, and so on. It may also be beneficial for blood clotting.
A 2018 review published in the Journal of Cellular Biochemistry has found that curcumin can improve platelet functions and may be beneficial for the treatment of thromboembolism and atherothrombosis (50).
Another 2018 review published in the Journal of Cellular Physiology has found that curcumin may offer therapeutic antithrombotic, anti-inflammatory, antioxidant, and cardiovascular-protective benefits (51). According to a 2020 article published in the Indian Journal of Clinical Biochemistry, turmeric may reduce thrombosis and blood clotting in COVID-19 (52).
I recommend using turmeric in your cooking, in curries, soups, stir-fries, and baked dishes. You can add it to your smoothies, juices, and shakes, or make golden milk or turmeric-ginger tea. I also recommend using a high-quality curcumin supplement daily.
If you are taking any blood-thinner medication, avoid consuming or taking turmeric or curcumin as they may interact negatively and cause problems. Talk to your doctor to see if turmeric or curcumin is safe for you if you are taking medications.

Consider Resveratrol and Quercetin
Resveratrol is a polyphenol found in the skin of red grapes, various berries, cacao, and pistachio. It offers anti-inflammatory and antioxidant properties. Quercetin is a plant flavanol with anti-inflammatory, antioxidant, and antihistamine benefits that may work well together with the benefits of resveratrol.
Resveratrol and quercetin offer many health benefits, including reducing the risk of blood clotting. A 2003 study published in the Journal of Thrombosis and Haemostatis has found that resveratrol and quercetin may help to reduce thrombosis and cardiovascular problems (53).
A 2019 study published in TH Open has found that quercetin may offer antithrombotic properties (54). Another 2019 review published in the International Journal of Molecular Sciences has found that resveratrol may reduce inflammation and blood clotting and may be beneficial for people with cardiovascular disease and heart failure (55).
I recommend eating foods rich in resveratrol, such as berries, grapes, and pistachios, and foods rich in quercetin, such as kale, red leaf lettuce romaine lettuce, chicory greens, cruciferous vegetables, pepper, red onion, asparagus, cabbage, sprouts, snap peas, herbs, olive oil, cranberries, black currants, blueberries, cherries, chokeberries, apples, and grapes. You can also find great supplements with resveratrol and quercetin.

Final Thoughts
A blood clot is basically a clump of blood. Instead of the normal liquid state of the blood, it turns into a semi-solid state. Blood clotting is an essential mechanism to stop bleeding and heal cuts or injuries. However, blood clots can develop inside your veins without an injury.
In some cases, blood clots resolve on their own. In other cases, blood clotting can become a serious or life-threatening issue. I recommend following my top natural support strategies for blood clotting.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website offers long-distance functional health coaching programs with our world-class team of health coaches. For further support with your health and other goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!
Sources in This Article Include:
1. Nader. Blood rheology. Frotiers in Physiology 2019. Link Here
2. Diagnosis and treatment of venous thromboembolism. CDC. Link Here
3. Stegenga. Pathphysiology Diabetes. 2006. Link Here
4. Takanashi K, Inukai T. Insulin resistance and changes in the blood coagulation-fibrinolysis system after a glucose clamp technique in patients with type 2 diabetes mellitus. J Med. 2000;31(1-2):45-62. PMID: 10998755
5. Franchini M, Targher G, Montagnana M, Lippi G. Iron and thrombosis. Ann Hematol. 2008 Mar;87(3):167-73. doi: 10.1007/s00277-007-0416-1. Epub 2007 Dec 8. PMID: 18066546
6. Journal of American Heart Association. 2019. Link Here
7. Wu HQ, Tang Y, Zhang X, Wei XH, Wang HQ, Zhang WT, Zhang GL. [Effect of Helicobacter pylori infection on platelet activation and coagulation function in patients with acute cerebral infarction]. Zhejiang Da Xue Xue Bao Yi Xue Ban. 2012 Sep;41(5):547-52. Chinese. PMID: 23086648
8. Platonov AE, Sarksyan DS, Karan LS, Shipulin GA, Gordygina EV, Malinin OV, Maleev VV. [The blood coagulation system and microcirculatory disorders in ixodid tick-borne borreliosis caused by Borrelia miyamotoi]. Ter Arkh. 2015;87(11):26-32. Russian. doi: 10.17116/terarkh2015871126-32. PMID: 26821412
9. Biswas S, Thakur V, Kaur P, Khan A, Kulshrestha S, Kumar P. Blood clots in COVID-19 patients: Simplifying the curious mystery. Med Hypotheses. 2021 Jan;146:110371. doi: 10.1016/j.mehy.2020.110371. Epub 2020 Nov 6. PMID: 33223324
10. Biswas S, Thakur V, Kaur P, Khan A, Kulshrestha S, Kumar P. Blood clots in COVID-19 patients: Simplifying the curious mystery. Med Hypotheses. 2021 Jan;146:110371. doi: 10.1016/j.mehy.2020.110371. Epub 2020 Nov 6. PMID: 33223324
11. Society for General Microbiology. “Dental plaque bacteria may trigger blood clots.” ScienceDaily. ScienceDaily, 26 March 2012. Link Here
12. Park YC, Kim J, Seo MS, Hong SW, Cho ES, Kim JK. Inverse relationship between vitamin D levels and platelet indices in Korean adults. Hematology. 2017 Dec;22(10):623-629. doi: 10.1080/10245332.2017.1318334. Epub 2017 May 10. PMID: 28486836
13. Zupo R, Castellana F, Sardone R, Lampignano L, Di Noia C, Savastano S, Giannelli G, De Pergola G. Hydroxyvitamin D Serum Levels are Negatively Associated with Platelet Number in a Cohort of Subjects Affected by Overweight and Obesity. Nutrients. 2020 Feb 13;12(2):474. doi: 10.3390/nu12020474. PMID: 32069873
14.Mohammad S, Mishra A, Ashraf MZ. Emerging Role of Vitamin D and its Associated Molecules in Pathways Related to Pathogenesis of Thrombosis. Biomolecules. 2019 Oct 24;9(11):649. doi: 10.3390/biom9110649. PMID: 31653092
15. Adili R, Hawley M, Holinstat M. Regulation of platelet function and thrombosis by omega-3 and omega-6 polyunsaturated fatty acids. Prostaglandins Other Lipid Mediat. 2018 Nov;139:10-18. doi: 10.1016/j.prostaglandins.2018.09.005. Epub 2018 Sep 25. PMID: 30266534
16. DiNicolantonio JJ, OKeefe J. Importance of maintaining a low omega-6/omega-3 ratio for reducing platelet aggregation, coagulation and thrombosis. Open Heart. 2019 May 2;6(1):e001011. doi: 10.1136/openhrt-2019-001011. PMID: 31218005
17. Remacha AF, Souto JC, Rámila E, Perea G, Sarda MP, Fontcuberta J. Enhanced risk of thrombotic disease in patients with acquired vitamin B12 and/or folate deficiency: role of hyperhomocysteinemia. Ann Hematol. 2002 Nov;81(11):616-21. doi: 10.1007/s00277-002-0560-6. Epub 2002 Nov 9. PMID: 12454698
18. Remacha AF, Souto JC, Piñana JL, Sardà MP, Queraltó JM, Martí-Fabregas J, García-Moll X, Férnandez C, Rodriguez A, Cuesta J. Vitamin B12 deficiency, hyperhomocysteinemia and thrombosis: a case and control study. Int J Hematol. 2011 Apr;93(4):458-464. doi: 10.1007/s12185-011-0825-8. Epub 2011 Apr 8. PMID: 21475950
19. Zhou K, Zhao R, Geng Z, Jiang L, Cao Y, Xu D, Liu Y, Huang L, Zhou J. Association between B-group vitamins and venous thrombosis: systematic review and meta-analysis of epidemiological studies. J Thromb Thrombolysis. 2012 Nov;34(4):459-67. doi: 10.1007/s11239-012-0759-x. PMID: 22743781
20. Lim KM, Kim S, Noh JY, Kim K, Jang WH, Bae ON, Chung SM, Chung JH. Low-level mercury can enhance procoagulant activity of erythrocytes: a new contributing factor for mercury-related thrombotic disease. Environ Health Perspect. 2010 Jul;118(7):928-35. doi: 10.1289/ehp.0901473. Epub 2010 Mar 12. PMID: 20308036
21. Zeng Z, Huo X, Zhang Y, Xiao Z, Zhang Y, Xu X. Lead exposure is associated with risk of impaired coagulation in preschool children from an e-waste recycling area. Environ Sci Pollut Res Int. 2018 Jul;25(21):20670-20679. doi: 10.1007/s11356-018-2206-9. Epub 2018 May 12. PMID: 29752673
22. Shin JH, Lim KM, Noh JY, Bae ON, Chung SM, Lee MY, Chung JH. Lead-induced procoagulant activation of erythrocytes through phosphatidylserine exposure may lead to thrombotic diseases. Chem Res Toxicol. 2007 Jan;20(1):38-43. doi: 10.1021/tx060114+. PMID: 17226925
23. Barman T, Kalahasthi R, Rajmohan HR. Effects of lead exposure on the status of platelet indices in workers involved in a lead-acid battery manufacturing plant. J Expo Sci Environ Epidemiol. 2014 Nov;24(6):629-33. doi: 10.1038/jes.2014.4. Epub 2014 May 21. PMID: 24849799
24. Koçak M, Akçil E. The effects of chronic cadmium toxicity on the hemostatic system. Pathophysiol Haemost Thromb. 2006;35(6):411-6. doi: 10.1159/000102047. PMID: 17565233
25. Vinchi F. Thrombosis Prevention: Let’s Drug the Microbiome! Hemasphere. 2019 Feb 1;3(1):e165. doi: 10.1097/HS9.0000000000000165. PMID: 31723804
26. Hasan RA, Koh AY, Zia A. The gut microbiome and thromboembolism. Thromb Res. 2020 May;189:77-87. doi: 10.1016/j.thromres.2020.03.003. Epub 2020 Mar 6. PMID: 32192995
27. University of Bonn. “Anxiety Linked To Blood Clots: Fear That Freezes The Blood In Your Veins.” ScienceDaily. ScienceDaily, 26 March 2008. Link Here
28. von Känel R. ACUTE MENTAL STRESS AND HEMOSTASIS: WHEN PHYSIOLOGY BECOMES VASCULAR HARM. Thromb Res. 2015 Feb;135(Suppl 1):S52-S55. doi: 10.1016/S0049-3848(15)50444-1. PMID: 25861135
29. Pinotti M, Bertolucci C, Frigato E, Branchini A, Cavallari N, Baba K, Contreras-Alcantara S, Ehlen JC, Bernardi F, Paul KN, Tosini G. Chronic sleep deprivation markedly reduces coagulation factor VII expression. Haematologica. 2010 Aug;95(8):1429-32. doi: 10.3324/haematol.2010.022475. Epub 2010 Apr 23. PMID: 20418241
30. Liak C, Fitzpatrick M. Coagulability in obstructive sleep apnea. Can Respir J. 2011 Nov-Dec;18(6):338-48. doi: 10.1155/2011/924629. PMID: 22187690
31. C. Kabrhel, R. Varraso, S. Z. Goldhaber, E. Rimm, C. A. Camargo. Physical inactivity and idiopathic pulmonary embolism in women: prospective study. BMJ, 2011; 343 (jul04 1): d3867 DOI. Link Here
32. Heber S, Assinger A, Pokan R, Volf I. Correlation between Cardiorespiratory Fitness and Platelet Function in Healthy Women. Medicine & Science in Sports & Exercise, May 2016. Link Here
33. Circulation Research. 2020. Link Here
34. Cho Y, Hong N, Kim KW, Cho SJ, Lee M, Lee YH, Lee YH, Kang ES, Cha BS, Lee BW. The Effectiveness of Intermittent Fasting to Reduce Body Mass Index and Glucose Metabolism: A Systematic Review and Meta-Analysis. J Clin Med. 2019 Oct 9;8(10):1645. doi: 10.3390/jcm8101645. PMID: 31601019
35. Aksungar FB, Eren A, Ure S, Teskin O, Ates G. Effects of intermittent fasting on serum lipid levels, coagulation status and plasma homocysteine levels. Ann Nutr Metab. 2005 Mar-Apr;49(2):77-82. doi: 10.1159/000084739. Epub 2005 Mar 29. PMID: 15802901
36. NIH Blood Bank. Link Here
37. Sengupta, T., Majumder, R. & Majumder, S. Role of vitamin D in treating COVID-19-associated coagulopathy: problems and perspectives. Mol Cell Biochem 476, 2421–2427 (2021). Link Here
38. Alharbi A. A Potential Role of Vitamin D on Platelet Leukocyte Aggregation and Pathological Events in Sepsis: An Updated Review. J Inflamm Res. 2021 Jul 30;14:3651-3664. doi: 10.2147/JIR.S321362. PMID: 34354363
39. McEwen BJ, Morel-Kopp MC, Tofler GH, Ward CM. The effect of omega-3 polyunsaturated fatty acids on fibrin and thrombin generation in healthy subjects and subjects with cardiovascular disease. Semin Thromb Hemost. 2015 Apr;41(3):315-22. doi: 10.1055/s-0034-1395352. Epub 2015 Feb 19. PMID: 25703517
40. Golanski J, Szymanska P, Rozalski M. Effects of Omega-3 Polyunsaturated Fatty Acids and Their Metabolites on Haemostasis-Current Perspectives in Cardiovascular Disease. Int J Mol Sci. 2021 Feb 27;22(5):2394. doi: 10.3390/ijms22052394. PMID: 33673634
41. Haro C, Villena J, Zelaya H, Alvarez S, Agüero G. Lactobacillus casei modulates the inflammation-coagulation interaction in a pneumococcal pneumonia experimental model. J Inflamm (Lond). 2009 Oct 16;6:28. doi: 10.1186/1476-9255-6-28. PMID: 19835595
42. Zelaya H, Tsukida K, Chiba E, Marranzino G, Alvarez S, Kitazawa H, Agüero G, Villena J. Immunobiotic lactobacilli reduce viral-associated pulmonary damage through the modulation of inflammation-coagulation interactions. Int Immunopharmacol. 2014 Mar;19(1):161-73. doi: 10.1016/j.intimp.2013.12.020. Epub 2014 Jan 4. PMID: 24394565
43. Vatansever F, Hamblin MR. Far infrared radiation (FIR): its biological effects and medical applications. Photonics & lasers in medicine. 2012;4:255-266. Link Here
44. Crinnion WJ. Sauna as a valuable clinical tool for cardiovascular, autoimmune, toxicant- induced and other chronic health problems. Altern Med Rev. 2011 Sep;16(3):215-25. PMID: 21951023
45. Laukkanen T, Khan H, Zaccardi F, Laukkanen JA. Association Between Sauna Bathing and Fatal Cardiovascular and All-Cause Mortality Events. JAMA Intern Med. 2015. Link Here
46. Kunutsor SK, Mäkikallio TH, Khan H, Laukkanen T, Kauhanen J, Laukkanen JA. Sauna bathing reduces the risk of venous thromboembolism: a prospective cohort study. Eur J Epidemiol. 2019 Oct;34(10):983-986. doi: 10.1007/s10654-019-00544-z. Epub 2019 Aug 1. PMID: 31372865
47. Weng Y, Yao J, Sparks S, Wang KY. Nattokinase: An Oral Antithrombotic Agent for the Prevention of Cardiovascular Disease. Int J Mol Sci. 2017 Feb 28;18(3):523. doi: 10.3390/ijms18030523. PMID: 28264497
48. Sharma C, Jha NK, Meeran MFN, Patil CR, Goyal SN, Ojha S. Serratiopeptidase, A Serine Protease Anti-Inflammatory, Fibrinolytic, and Mucolytic Drug, Can Be a Useful Adjuvant for Management in COVID-19. Front Pharmacol. 2021 Jun 24;12:603997. doi: 10.3389/fphar.2021.603997. PMID: 34248612
49. Tiwari M. The role of serratiopeptidase in the resolution of inflammation. Asian J Pharm Sci. 2017 May;12(3):209-215. doi: 10.1016/j.ajps.2017.01.003. Epub 2017 Feb 1. PMID: 32104332
50. Tabeshpour J, Hashemzaei M, Sahebkar A. The regulatory role of curcumin on platelet functions. J Cell Biochem. 2018 Nov;119(11):8713-8722. doi: 10.1002/jcb.27192. Epub 2018 Aug 11. PMID: 30098070
51. Keihanian F, Saeidinia A, Bagheri RK, Johnston TP, Sahebkar A. Curcumin, hemostasis, thrombosis, and coagulation. J Cell Physiol. 2018 Jun;233(6):4497-4511. doi: 10.1002/jcp.26249. Epub 2017 Dec 26. PMID: 29052850
52. Suresh PS. Curcumin and Coagulopathy in the COVID19 Era. Indian J Clin Biochem. 2020 Jul 15;35(4):1-2. doi: 10.1007/s12291-020-00914-5. Epub ahead of print. PMID: 32837032
53. Di Santo A, Mezzetti A, Napoleone E, Di Tommaso R, Donati MB, De Gaetano G, Lorenzet R. Resveratrol and quercetin down-regulate tissue factor expression by human stimulated vascular cells. J Thromb Haemost. 2003 May;1(5):1089-95. doi: 10.1046/j.1538-7836.2003.00217.x. PMID: 12871381
54. Stainer AR, Sasikumar P, Bye AP, Unsworth AJ, Holbrook LM, Tindall M, Lovegrove JA, Gibbins JM. The Metabolites of the Dietary Flavonoid Quercetin Possess Potent Antithrombotic Activity, and Interact with Aspirin to Enhance Antiplatelet Effects. TH Open. 2019 Jul 30;3(3):e244-e258. doi: 10.1055/s-0039-1694028. PMID: 31367693
55. Dyck GJB, Raj P, Zieroth S, Dyck JRB, Ezekowitz JA. The Effects of Resveratrol in Patients with Cardiovascular Disease and Heart Failure: A Narrative Review. Int J Mol Sci. 2019 Feb 19;20(4):904. doi: 10.3390/ijms20040904. PMID: 30791450



