 Sjogren’s Syndrome: Symptoms, Causes, and Support Strategies
Sjogren’s Syndrome: Symptoms, Causes, and Support Strategies
Sjogren’s Syndrome is an autoimmune disease that can affect the entire body. It is one of the most prevalent autoimmune conditions, affecting around 4,000,000 people in the U.S.
The most common symptom of Sjogren’s is extensive dryness, especially dry eyes and dry mouth. Other symptoms may include profound fatigue, chronic pain, organ dysfunction, neuropathy, and more.
One of the best natural strategies for Sjogren’s syndrome is to follow an autoimmune elimination diet. With this nutrition plan, you eliminate the most common immune provoking and pro-inflammatory for 6 weeks. By eliminating foods that may be triggering an immune response and giving your body time to heal, Sjogren’s symptoms may improve.
This article will discuss how to implement an autoimmune elimination diet along with other natural support strategies to improve your immune system and overall health.
What is Sjogren’s Syndrome?
Sjogren’s (pronounced SHOW-grins) syndrome is a multi-organ autoimmune disease (1). It is named after the Swedish ophthalmologist Henrik Sjogren (2). Dr. Sjogren identified the disease in the early 1930s when he saw patients who complained of dry eyes, oral dryness, and joint pain.
Sjogren’s is a type of autoimmune condition. An autoimmune condition occurs when the body’s immune system malfunctions. It mistakenly identifies healthy cells and tissues as foreign invaders and starts attacking and destroying them.
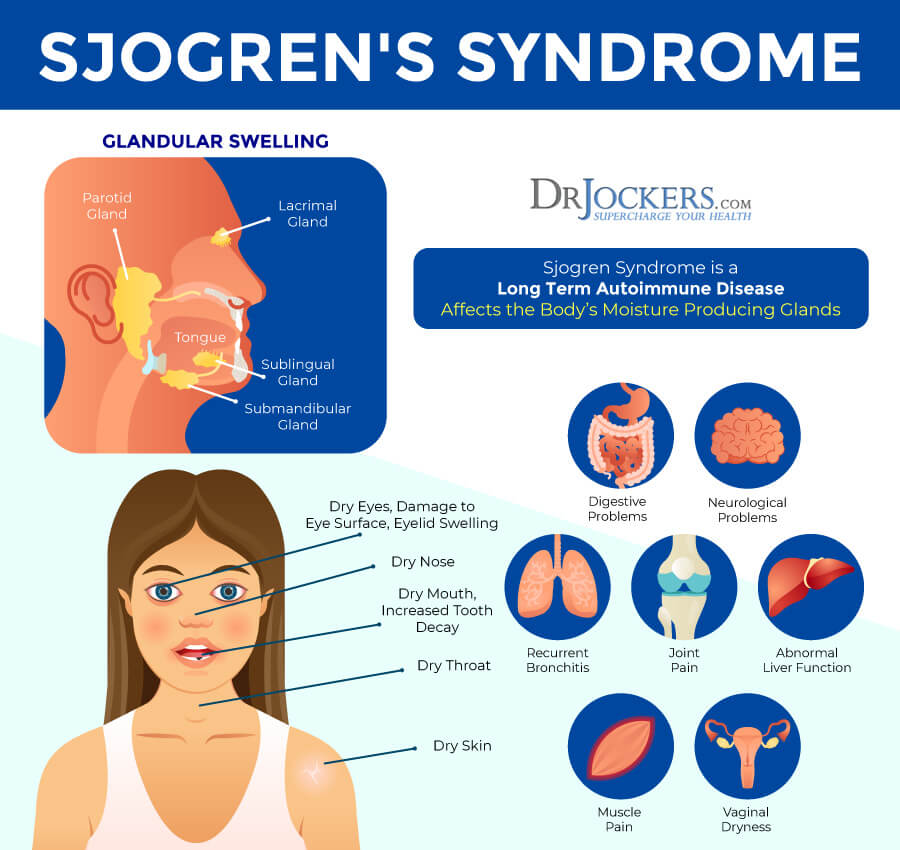
Sjogren’s syndrome begins as an organ-specific disease (exocrine glands) but extends to a systemic process. It begins with the mucous membranes and moisture secreting glands in the eyes and mouth. This leads to dryness of the eyes (keratoconjunctivitis sicca), dryness of the mouth (xerostomia), and often dryness of other areas connected to the exocrine glands (2). As it becomes systemic, Sjogren’s can damage other parts of the body including joints, thyroid, kidneys, liver, lungs, skin, and nerves.
It is estimated that at least 4 million Americans have Sjogren’s. You can develop Sjogren’s at any age, but most people are 40 or older at the time of diagnosis. Sjogren’s is also much more common in women, affecting 10 times as many women as men.
Sjogren’s often accompanies other immune system disorders. It is common for people who have Sjogren’s to also have a rheumatic disease such as lupus or rheumatoid arthritis. “Primary” Sjogren’s syndrome refers to Sjogren’s with no other rheumatic disease. “Secondary” Sjogren’s syndrome occurs in people who have another rheumatologic disease.

Symptoms of Sjogren’s
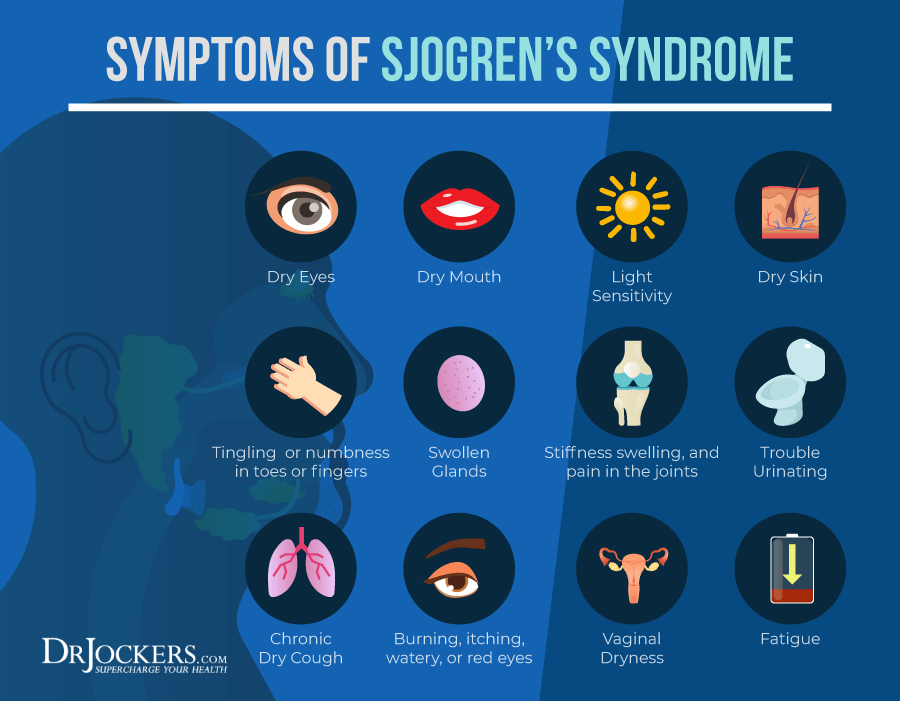
Symptoms of Sjogren’s syndrome vary in type and intensity. The two main symptoms are dry eyes and dry mouth (3). The eyes of people with Sjogren’s might burn, itch, or feel gritty. The mouth is very dry or chalky with little saliva. This makes it difficult to swallow or speak.
Additional symptoms of Sjogren’s syndrome include:
- Chronic fatigue
- Joint pain, swelling, and stiffness
- Swollen salivary glands (particularly those behind jaw and in front of ears)
- Dry skin
- Vaginal dryness
- Persistent dry cough or hoarseness
- Loss of taste
- Dry lips
- Heartburn or GERD
Complications of Sjogren’s Syndrome
Many people with Sjogren’s syndrome remain healthy and are able to lead normal lives. Most of the complications of Sjogren’s are due to the decrease in saliva and tears. People with dry eyes are at increased risk for eye infections and cornea damage. Dry mouth may increase the risk of dental decay, gingivitis (gum inflammation), and oral yeast infections (thrush).
Complications in other parts of the body are rare. These complications may include:
- Lung problems that mimic pneumonia
- Abnormal liver and kidney function tests
- Skin rashes related to inflammation of small blood vessels
- Neurological problems causing weakness and numbing
Sjogren’s is also associated with an increased risk of lymphoma (cancer of the lymph glands).
Causes of Sjogren’s Syndrome
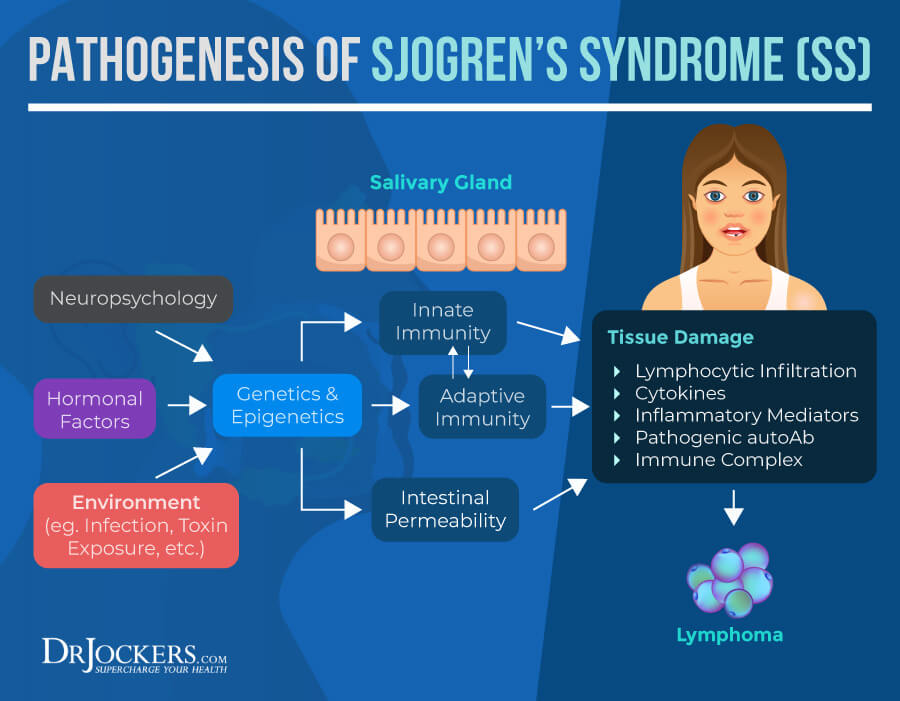
The exact cause of Sjogren’s syndrome, as with other autoimmune conditions, is not clear. Research suggests there may be a genetic susceptibility to autoimmunity and different environmental triggers that bring on the condition (4).
Around 75% of autoimmune conditions are caused by environmental factors. The 7 major environmental factors are:
- Gluten sensitivity
- Genetically modified organisms (GMOs)
- Gut dysfunction
- Neurological stress
- Toxins
- Stress and hormones
- Viral and bacterial infections

Diagnosing Sjogren’s Syndrome
Sjogren’s syndrome can be difficult to diagnose because symptoms frequently overlap with or “mimic” those of other diseases including lupus, rheumatoid arthritis, fibromyalgia, chronic fatigue syndrome, and multiple sclerosis (5). Symptoms of dryness can occur for reasons other than Sjogren’s, such as a side effect of medications.
Rheumatologists have primary responsibility for diagnosing and managing Sjogren’s syndrome. There is no single test that will confirm a diagnosis, but a positive lip biopsy is considered the “gold standard” for diagnosing Sjogren’s. A salivary gland biopsy (usually in the lower lip) may be done to confirm inflammatory cell (lymphocytic) infiltration of the minor salivary glands.
About 30% of patients are negative for autoantibody SSA, the clearest blood marker for Sjogren’s. However, being negative does not mean the patient does not have Sjogren’s. A doctor will have to determine the diagnosis through symptoms and other tests.
Blood tests your doctor may perform include:
- ANA (Antinuclear Antibody): ANAs are a group of antibodies that react against normal components of a cell nucleus. About 70% of Sjogren’s patients have a positive ANA test result.
- RF (Rheumatoid Factor): This antibody test is indicative of a rheumatic disease, including rheumatoid arthritis (RA), lupus and Sjogren’s. It doesn’t, however, specify which rheumatic disease a person has. In Sjogren’s patients, 60-70% have a positive RF.
- SS-A (or Ro) and SS-B (or La): These are the marker antibodies for Sjogren’s. Seventy percent of Sjogren’s patients are positive for SS-A and 40% are positive for SS-B (these may also be found in lupus patients).
- ESR (Erythrocyte Sedimentation Rate): This test measures inflammation. An elevated ESR indicates the presence of an inflammatory disorder, including Sjogren’s.
- IGs (Immunoglobulins): These are normal blood proteins that participate in immune reactions and are usually elevated in Sjogren’s patients.
The ophthalmologic (eye) tests include:
- Schirmer Test to measure tear production.
- Rose Bengal and Lissamine Green eye drops containing dyes to examine the surface of the eye for dry spots
The dental tests include:
- Salivary flow to measure the amount of saliva produced over a certain period of time
- Salivary scintigraphy nuclear medicine test that measures salivary gland function

Food Sensitivities and Autoimmunity
A food sensitivity is an immune-mediated response to certain foods. When you have food sensitivities, your immune system reacts to certain foods as a threat amplifying the immune response.
It is estimated that 45-75% of individuals have food sensitivities. Repeated exposure to the foods causes inflammation and other health problems. The consequences of food-induced immune system activation can be subtle initially but may become serious over time.
A recent observational study found a clear difference in food sensitivity profiles for people with autoimmune diseases (6). IgG levels for specific food antibodies were significantly higher in patients with autoimmune conditions which means they had a greater immune reaction to these foods.
Food sensitivities can be hard to identify. This is because symptoms of food sensitivities are usually delayed up to 72 hours after consuming the offending food. These symptoms are not exclusively related to the gut, and can include migraines, fatigue, joint pain, skin issues, and many others. For information about different methods of testing for food sensitivities, check out this article.

How to Implement an Autoimmune Elimination Diet
An autoimmune elimination diet can be a powerful natural strategy for Sjogren’s (7). This diet eliminates the most common allergenic/sensitivity foods which may be contributing to or causing a negative reaction and inflammation. The goal in eliminating these foods is to identify foods that may be contributing to your autoimmune condition. These foods should be eliminated for around 6 weeks.
After the elimination period, you slowly reintroduce foods, one at a time, noting any reactions and symptoms you may experience. It is important to keep a journal during the entire process to document how you are feeling as you eliminate and reintroduce the foods.

Foods Included
Foods included in the autoimmune diet include healthy fats, clean-sourced protein and low to moderate carbohydrate vegetables, fruits, and herbs. These foods help to reduce inflammation and support the immune system.
Healthy Fats
Consuming plenty of healthy fats is very important on the autoimmune diet. Healthy fats are found in coconut, olives, avocados, and their oils and in grass-fed butter and ghee. Pumpkin, flax, hemp and chia seeds, and borage, hemp or flax oils are additional sources of good fats.
Omega-3 fatty acids and conjugated linoleic acid (CLA) found in wild-caught salmon and grass-fed beef and dairy have many health benefits. These healthy fats are an efficient source of fuel for the body to combat inflammation.

Clean Protein
Great protein sources are grass-fed, pasture-raised, and organic meats. Beef, bison, lamb, buffalo, venison, chicken, pheasant, duck and turkey are all included.
Wild-caught fish such as Alaskan Sockeye salmon is an excellent choice. Hypoallergenic brown rice or pea proteins can be used as well as bone broth from clean-sourced animals.
Low Carbohydrate Vegetables, Low-Glycemic Fruits and Herbs
A variety of low to moderate carbohydrate vegetables and fruits should be included for their abundant antioxidants and phytonutrients. Examples are cruciferous vegetables, cucumbers, asparagus, and leafy greens. Fruits to include on the autoimmune diet are berries, lemons and limes, grapefruits, gogi berries, avocados, coconuts, and granny smith apples.
Herbs like rosemary, oregano, basil, cilantro, sage, and thyme have healing properties and should be included in the keto autoimmune diet. Spices and sweeteners like cinnamon, garlic, ginger, turmeric, pink salt, stevia, and monk fruit are included. However, cayenne and paprika should not be used on the autoimmune diet.

Other Foods to Include
Fermented foods and teas are excellent to include on the autoimmune diet. Organic green tea and organic herbal teas like ginger, Pau D Arco, and Nighty Night are great choices.
Fermented foods should be made without nightshade vegetables. These include coconut milk kefir or yogurt, fermented vegetables, kombucha, coconut water kefir, kimchi, and sauerkraut. Coconut milk, yogurt and kefir are fantastic dairy substitutes.
Other coconut products like coconut butter, coconut flour, and unsweetened coconut flakes are included on this diet, as well as flax crackers and organic raw apple cider vinegar.

Foods Excluded
The autoimmune diet eliminates foods that most commonly cause an immune response and additional highly pro-inflammatory foods. One of the most important foods to remove for anyone with Sjogren’s syndrome is gluten. Studies show that the prevalence of celiac disease (immune reaction to gluten) is significantly higher in people with Sjogren’s (8).
In addition to gluten, you should eliminate dairy, eggs, peanuts, tree nuts, soy, wheat, fish and shellfish. Many people are also sensitive to nightshade vegetables (tomatoes, potatoes, eggplant, bell peppers), corn, legumes, and all grains.
In addition to these foods, it is important to eliminate foods that cause inflammation. These include:
- Sugar
- Refined carbohydrates (white flour, white rice, white potatoes)
- Conventionally raised meat and dairy
- Farm-raised fish
- Processed foods, including meats
- Trans fats (partially hydrogenated oils)
- Mono-sodium Glutamate (MSG) and other food additives and preservatives
- Highly processed vegetable and seed oils, such as canola, corn, sunflower, peanut, grapeseed, cottonseed, and safflower
- Artificial Sweeteners.
It is critical to avoid foods with pesticides and added chemicals which have been linked to autoimmune conditions (9). Bisphenol A (BPA), a classic endocrine disrupting chemical that affects the immune system, may accelerate the progression and future deterioration of Sjogren’s syndrome (10).

Other Foods that May be Problematic
You may have sensitivities to the foods that are allowed on the elimination diet such as citrus fruits, seeds, berries, onions, and certain meats. Higher FODMAP foods can also cause digestive symptoms in some people. It is important to recognize any unwanted symptoms such as noticeable gas, bloating, altered bowel habits, fatigue, increased pain and inflammation, eczema, acne, insomnia, anxiety, brain fog, and mood changes that are associated with any foods.
It is also important to note that when you have a leaky gut, food sensitivities can develop to the foods you consume the most. To heal the gut, it is important to avoid any foods that may be inflaming the gut. Once your gut heals, you may be able to eat these foods again without a sensitivity or immune response. I go over how to follow and add back foods in this article. You can also try using the pulse test that I review in the video below.
Reintroducing Foods
When you are ready to reintroduce foods, it is good to follow a schedule. The recommended reintroduction schedule is:
- Bell peppers
- Tomatoes
- Almonds and almond butter
- Walnuts
- Pecans
- Pasture-raised eggs
- Grass-fed cheese
- Brazil nuts
- Pistachios
- Quinoa
Slowly reintroduce foods, one at a time, noting any reactions and symptoms you may experience. I recommend having a food journal and isolating each food as you add it back and rank it on a scale of 1-10 based on how you feel after you eat it. If you experience any negative symptom, then continue to avoid that food for a longer period.

Consider Following Ketogenic Guidelines
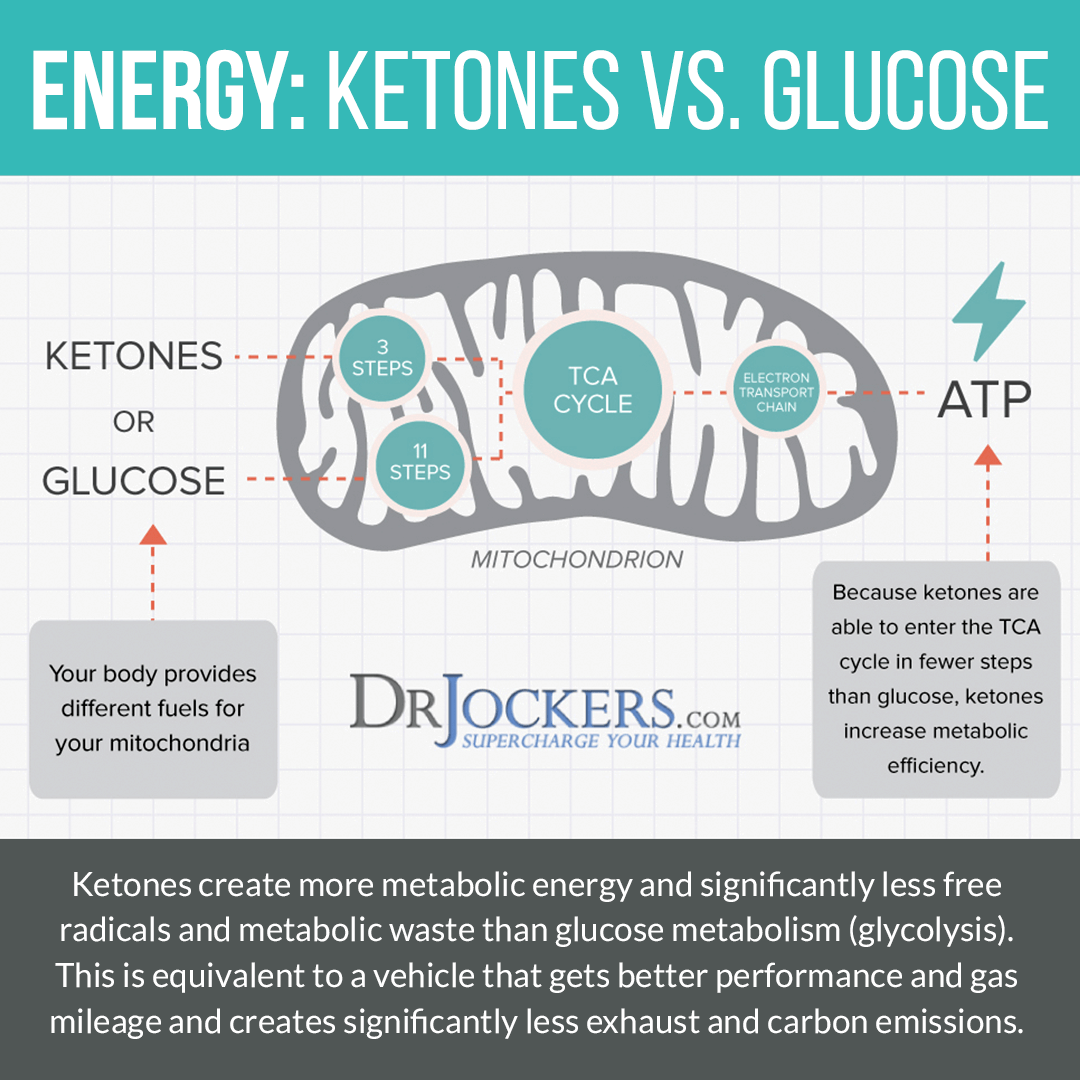
Some people with Sjogren’s may benefit from following ketogenic guidelines while doing the autoimmune elimination diet. The ketogenic diet is a nutrition and lifestyle plan that helps your body use fat (stored fat and dietary fat) rather than sugar for fuel. When the body is in ketosis, it utilizes ketones as an energy source instead of glucose.
For a keto autoimmune, you would eliminate the foods discussed above. For the foods included in the diet, you follow ketogenic diet guidelines: 70-80% of calories from fat, 15-20% from protein, and 5-10% from carbohydrates.
Transitioning from a sugar burner to a fat burner with a keto autoimmune diet may be beneficial for anyone with Sjogren’s. A major contributor to autoimmune conditions is inflammation. The ketogenic diet lowers inflammation by reducing the amount of free radical production, stabilizing blood sugar levels, and reducing insulin levels.
Support Your Mitochondria
Mitochondria are the energy powerhouses of your cells. They have essential roles in the body including producing the energy carrying molecule Adenosine Triphosphate (ATP), maintaining glutathione levels, protecting DNA, signaling cell reproduction, activating cell apoptosis, and maintaining cell electrochemical integrity.
Many autoimmune diseases, including Sjogren’s syndrome, appear to have a mitochondrial basis (11). Mitochondrial impairment is also a factor in inflammation.
It is important for individuals with Sjogren’s to support their mitochondria. Calorie restriction (such as intermittent fasting), exercise, sunlight exposure, restorative sleep, managing stress, and alternating heat and cold exposure are ways to boost your mitochondria.
Mitochondrial nutrients can be very helpful for supporting the mitochondria. You can find products that contain a blend of nutrients, nutraceuticals, botanicals, and Krebs cycle intermediates to improve healthy cellular function and efficient mitochondrial metabolism. These would include things like alpha lipoic acid, coQ10, acetyl L-carnitine, B vitamins and more.

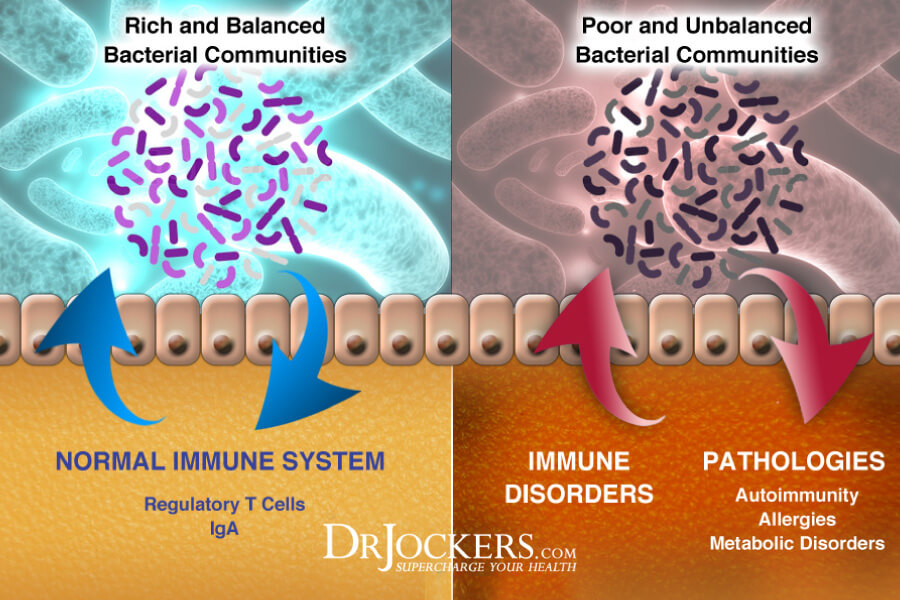
Balance the Gut Microbiome
The large and complex community of microorganisms in the gastrointestinal tract is called the gut microbiome. The gut microbiome has trillions of beneficial and pathogenic microbes. The ideal ratio of beneficial to pathogenic microbes is around 85:15.
Unfortunately, most people have dysbiosis, an inverse ratio with bad bacteria outnumbering good bacteria. Significant gut dysbiosis is associated with Sjogren’s syndrome and is related to the severity of dry eye (12).
One way to help rebalance your gut microbiome is by supplementing with probiotics. Probiotics are beneficial microorganisms (bacteria and yeasts) that keep your gut and body healthy. They are similar to the microorganisms that naturally live in our bodies and support digestive health in many ways.
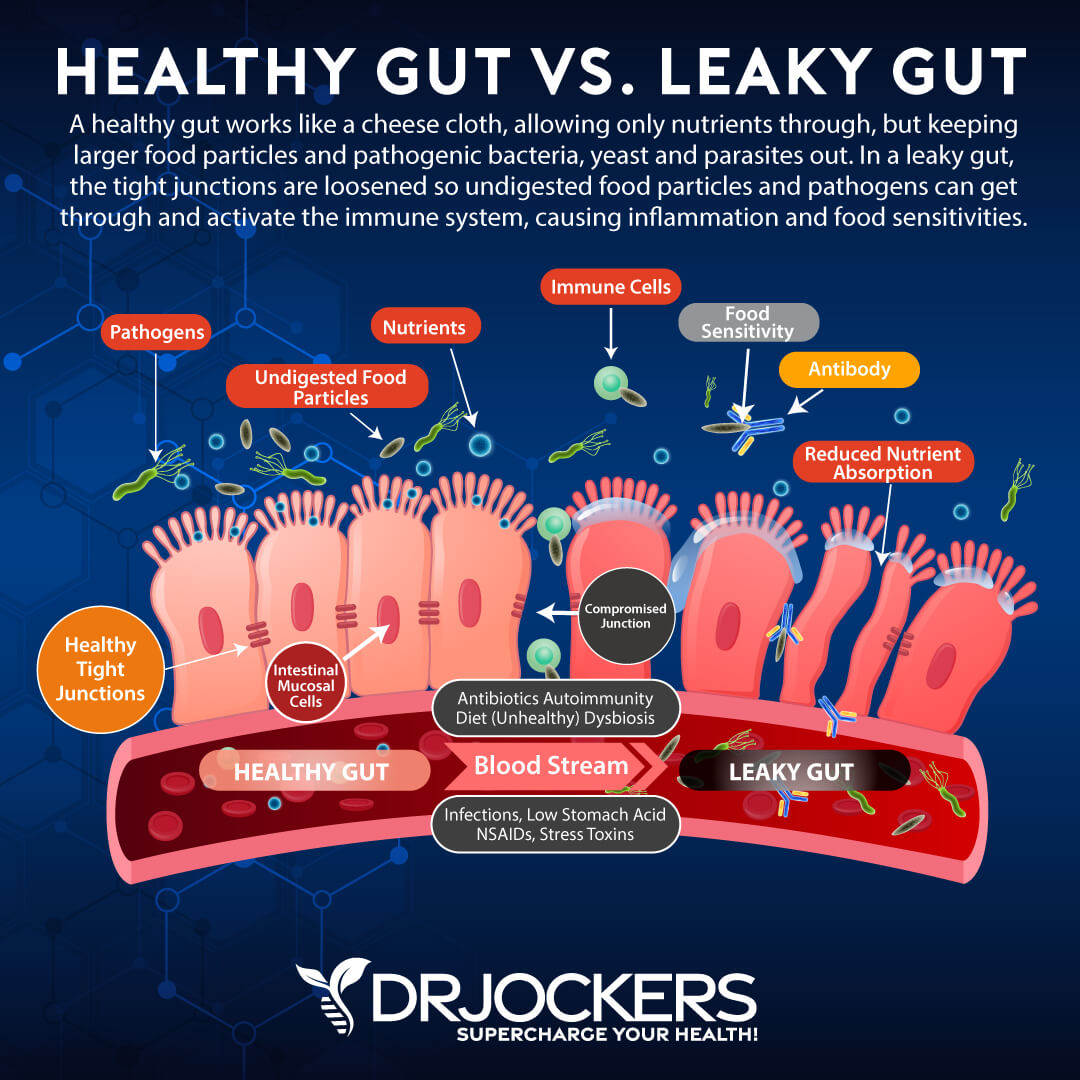
Repair Leaky Gut
To improve Sjogren’s syndrome, it is very important to heal and repair your gut. Leaky gut syndrome, or intestinal permeability, is a condition in which the tight junctions in the gut lining become too large and abnormally permeable. Undigested food particles and toxins can pass through these holes in the intestinal wall and into the bloodstream. This causes the immune system to overreact and results in chronic inflammation and food sensitivities.
Reducing stress on the gut with liquid nutrition and fasting can be very effective for repairing leaky gut. Digesting solid foods creates significant stress on the digestive system, irritates the gut lining, and leads to inflammatory processes. With fasting and liquid nutrition, our bodies can conserve the energy used in digesting, processing and assimilating solid foods. The body can use this energy instead on healing and detoxifying.
Using liquid nutrition also stimulates the digestive process and increases nutrient absorption. For Sjogren’s, a great option is to use liquid nutrition with high-quality hypoallergenic amino acids and powerful antioxidants to support gut function and improve detoxification.
Another fantastic supplement to soothe an irritated gut lining and reduce inflammation in the gut would contain key nutrients such as the amino acid l-glutamine, along with aloe vera, arabinogalactan, and licorice. The amino acid glutamine plays an important role in gut and immune function. Aloe has many health benefits including reducing inflammation in the gut. Licorice is a powerful herb that helps with indigestion and ulcers.
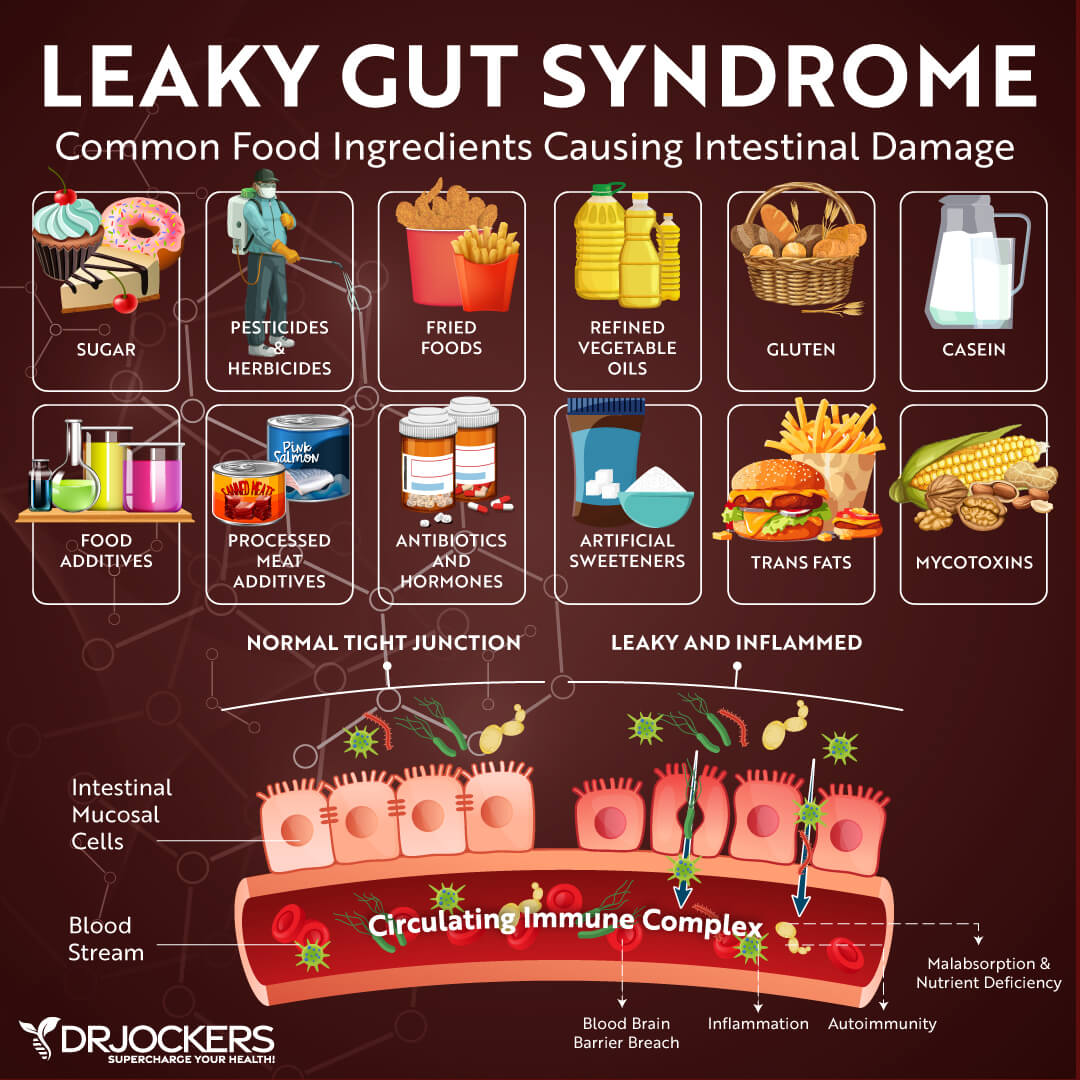
Test for and Address Gut Infections
Our GI tracts are constantly exposed to pathogens including bacteria, viruses, parasites, and fungi. When our gut immune system is compromised, gut infections often result from these pathogens. These infections damage the gut, cause inflammation, and can trigger or exacerbate autoimmune conditions.
It is important to test for and address any gut infections from bacteria, viruses, or parasites which may be contributing to Sjorgren’s syndrome. Two of the top tests for gut infections are the Comprehensive Organic Acids Test (OAT) and the GI-MAP™ Stool Analysis Test.
The OAT shows an extensive metabolic snapshot of a person’s overall health. This test measures yeast, fungal, and bacterial overgrowths and much more. It is a simple at home urine test that is very thorough. For more information on the OAT, look here.
The GI Map identifies your levels of normal (good) bacteria as well as harmful bacteria in the gut. In addition to bacteria, the GI-MAP can detect Candida and other fungi, and parasites, including both protozoa and worms.
This comprehensive stool test can reveal if you have H. pylori, viral pathogens, potential autoimmune triggers, and viruses, including the cytomegalovirus and Epstein Barr virus. It also reveals the health of your intestines with digestion, gastrointestinal, Secretory and Anti-gliadin IgA (immune response), and calprotectin (inflammation) markers. For more information on the GI-MAP and a sample report, you can look here.
Strengthen Gut Mucosa
The gut mucosa is a protective barrier that lines the digestive tract. It houses the gut microbiome, aids in the absorption of nutrients, and protects us from pathogens, toxins, and dietary antigens. It is a vital part of the immune system and contains intestinal immunomodulatory cells that control immune responses and reduce inflammation. Strengthening the gut mucosa is an important strategy for improving Sjogren’s syndrome.
For mucosal support, look for a high quality colostrum or a dairy-free, bovine serum-derived immunoglobulin concentrate (BSI). These free form immunoglobulins support gut barrier function, improve immunity, and decrease inflammation in the gut. The immunoglobulins also bind to environmental toxins, neutralize pathogens, and aid digestion.
Bovine colostrum is rich in antimicrobial substances and growth factors. Due to these properties, it may help to improve the overall health for people with Sjogren’s (13).
Support Immune Health
Sjogren’s syndrome occurs due to a dysfunctional immune system. Supporting the immune system with antioxidants and nutrients may help to normalize immune system function.
A great combination for immune health includes things like olive leaf extract, beta glucan, and vitamin C. Olive leaf is a powerful herb with antibacterial, antifungal, and antiviral effects.
It inhibits viral reproduction and supports the immune system in fighting viruses. Beta glucan is a balancing immune modulator that helps to bind to white blood cells and improve their immune coordination. Vitamin C is an antioxidant that supports immune system function.
Your lymphatic system is a vital part of your immune system. It is a network of lymph nodes connected by lymphatic vessels that transports lymph throughout the body. Sjogren’s syndrome is considered a lymphoproliferative disease (2). Supporting your lymphatic system may be helpful for improving Sjogren’s.
Lymph contains oxygen, proteins, and other nutrients that nourish the tissues. It transports foreign substances, cancer cells, and dead or damaged cells that may be present in tissues into the lymphatic vessels and to lymph organs for disposal. Harmful microorganisms are filtered out and destroyed in the lymph nodes. When the lymphatic system is functioning poorly, this can weaken the immune system.
There are ways to improve your lymphatic system including exercise, sweating, deep breathing and dry brushing. In addition, certain herbs such as sheep sorrel, burdock root, slippery elm bark, astragalus root, graviola and bioactive carbons all work to help flush lymphatic congestion and improve immune health.

Targeted Supplementation
It is important to remember that there are no supplements that are FDA approved to prevent, mitigate, treat or cure Sjogren’s Disease. However, there are supplements that can benefit the immune system, cell membrane health, mitochondrial function and a healthy inflammatory process.
Many clinicians have seen people with Sjogren’s improve their overall health and wellness with these specific supplements and they may be worth a shot to see if you feel improvements as well.
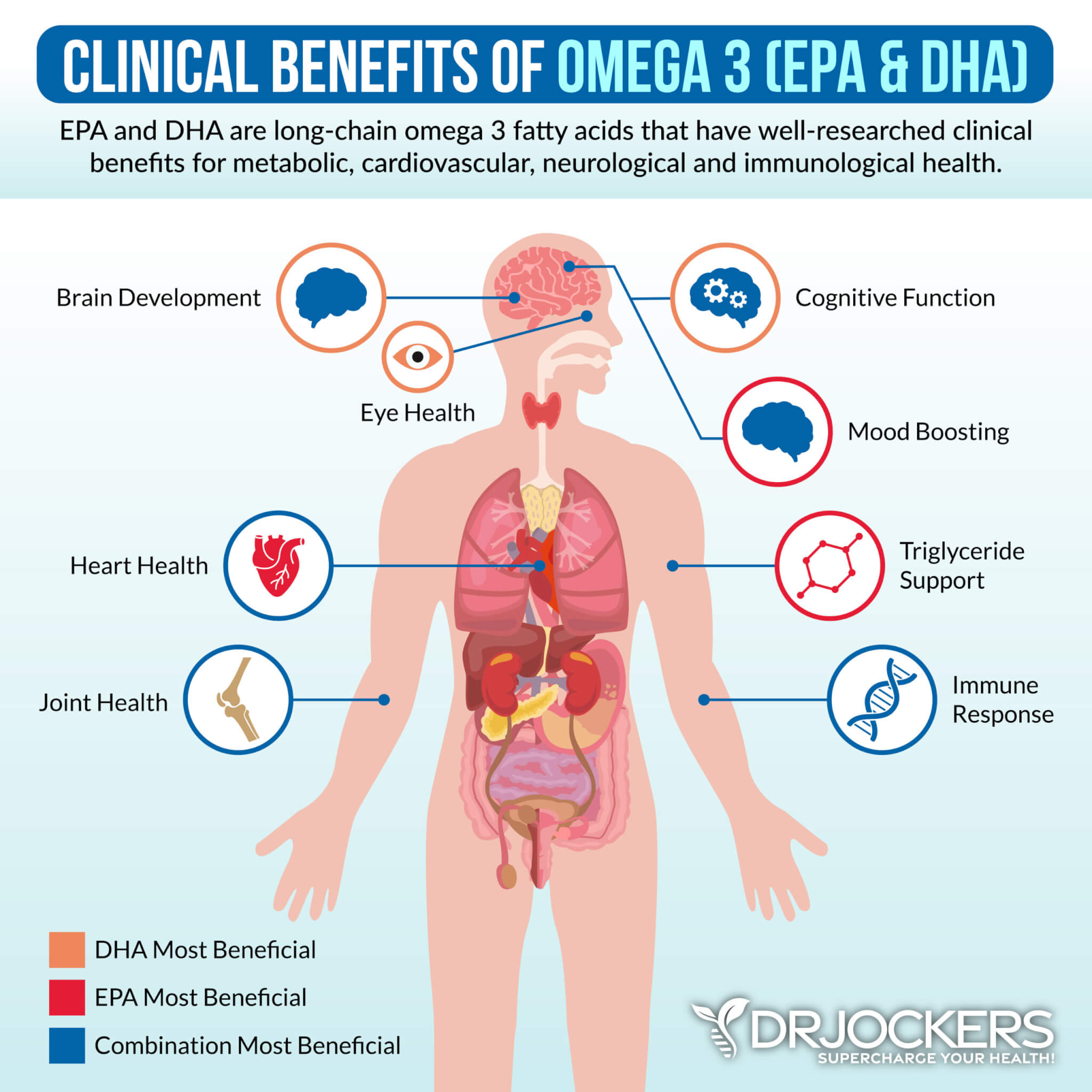
Omega-3 Fatty Acids
To help with the dryness associated with Sjogren’s syndrome, you should increase your intake of essential fatty acids. Essential fatty acids are essential fats that your body cannot produce. They include Omega 3 fatty acids which maintain cellular membrane health and have antioxidant, anti-inflammatory, and antifibrotic properties.
Cod Liver oil is one of the world’s best sources of the omega 3 fatty acids rich in both EPA and DHA. DHA is the most important essential fat for good eye health and EPA also plays a helpful role.
In addition, Cod Liver oil is a fantastic source of retinol which is the vital fat-soluble form of vitamin A that supports immune health. Vitamin A helps create “killer cells” lymphocytes which attach foreign invaders and produce antibodies.
On top of that, it also supplies us with vitamin D. Many brands have it in either a capsule form or a lemon-flavored oil so it doesn’t taste bad at all and is easy to swallow.
Curcumin
Turmeric is a powerful herb with abundant health benefits. It has been used for centuries to treat a variety of conditions. Turmeric has anti-inflammatory, antioxidant, anti-thrombotic, and antimicrobial properties. The curcuminoids in turmeric have antioxidant properties. It helps to boost the body’s natural antioxidant capacity which fights damaging free radicals.
Curcumin is the active component of turmeric. Due to its antioxidant, anti-inflammatory effects, curcumin has an important role in the prevention and treatment of autoimmune conditions (14).
Animal studies have shown that curcumin and turmeric may be a useful therapeutic intervention in Sjogren’s syndrome (15). We don’t have enough human trials to say this for sure, however, many people have seen improvements in their health with the use of turmeric and curcumin.

EGCG
Epigallocathechin-3-gallate (EGCG) is a bioactive botanical in green tea polyphenols. ECGC was shown to be protective against autoimmune-induced tissue damage in Sjogren’s syndrome in a mouse model (16). We don’t have enough human trials to confirm this in humans at this point.
EGCG is the most abundant catechin in green tea and accounts for more than half of the total polyphenol and effective content in green tea. Green tea also helps to promote the production of the antioxidants glutathione and superoxide dismutase (SOD). These antioxidants drastically lower inflammation in the body.
You can also find combination products that contain clinical dosages of EGCG, curcumin, sulforaphane, and resveratrol. While these products are not FDA approved to treat Sjogren’s or any other health condition, it does contain a powerful blend of antioxidant compounds support a healthy inflammatory response and protect the body against oxidative stress.

Conclusion
Sjogren’s is an autoimmune condition that affects the mucous membranes and moisture secreting glands of your eyes and mouth. In addition to dry eyes and dry mouth, Sjogren’s can also cause joint pain and swelling, prolonged fatigue, and other symptoms.
Sjogren’s often accompanies other immune system disorders, including rheumatoid arthritis and lupus. It can affect anyone at any age but occurs mostly in women over the age of 40.
The autoimmune diet is a 6-week elimination diet that removes pro-inflammatory foods as well as the most common immune provoking foods. This helps to decrease inflammation and gives your body a chance to heal itself. Other support strategies for Sjogren’s syndrome are supporting your mitochondria, balancing the gut microbiome, repairing leaky gut syndrome, addressing gut infections, strengthening the gut mucosa, supporting immune health, and using targeted supplementation.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website offers world class long-distance functional health coaching programs. For further support with your health goals, just reach out and our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!
Sources for this Article
1. Selifanova E, Beketova T, Spagnuolo F, Leuci S, Turkina A, A Novel Proposal of Salivary Lymphocyte Detection and Phenotyping in Patients Affected by Sjogren’s Syndrome, 2020 Feb; 9(2): 521. PMID: 32075146
2. Jonsson R, Brokstad K, Jonsson M, Delaleu N, Skarstein K, Current concepts on Sjogren’s syndrome – classification criteria and biomarkers, 2018 Oct: 126(Suppl 1): 37-48. PMID: 30178554
3. Sjogren’s Syndrome, Mayo Clinic. Link here
4. Schmidt C, Questions Persist: Environmental Factors in Autoimmune Disease, 2011 Jun; 119(6): A248-A253. PMID: 21628113
5. About Sjogren’s, Sjogren’s Syndrome Foundation. Link here
6. Coucke F, Food intolerance in patients with manifest autoimmunity. Observational study. 2018 Nov; 17(11): 1078-1080. PMID: 30213697
7. Feuerstein J, Reversal of premature ovarian failure in a patient with Sjogren syndrome using an elimination diet protocol. 2010 Jul; 16(7): 807-9. PMID: 20618099
8. Bartolini E, Bistoni O, et al, Celiac Disease Prevalence is Increased in Primary Sjogren’s Syndrome and Diffuse Systemic Sclerosis: Lessons from a Large Multi-Center Study. 2019 Apr 19; 8:4. PMID: 31010199
9. Gold LS, Ward MH, Dosemeci M, De Roos AJ, Systemic autoimmune disease mortality and occupational exposures. 2007 Oct.; 56(10): 3180-201. PMID: 17907164
10. Wang J, She C, et al, In vitro impact of bisphenol A on maturation and function of monocyte-derived dendritic cells in patients with primary Sjogren’s syndrome. 2020 Feb; 42(1): 28-36. PMID: 31876196
11. Links to Other Diseases, United Mitochondrial Disease Foundation. Link here
12. Moon J, Choi SH, Yoon CH, Kim MK, Gut dysbiosis is prevailing in Sjogren’s syndrome and is related to dry eye severity. 2020 Feb 14; 15(2): e0229020. PMID: 32059038
13. Pedersen AM, Andersen TL, et al, Oral findings in patients with primary Sjogren’s syndrome and oral lichen planus-a preliminary study on the effects of bovine colostrum-containing oral hygiene products. 2002 Mar; 6(1): 11-20. PMID: 11996158.
14. Kocaadam B, Sanlier N, Curcumin, an active component of turmeric (Curcuma longa), and its effects on health. 2017 Sep 2; 57(13): 2889-2895. PMID: 26528921
15. Kurien BT, Harris VM, et al, Significantly reduced lymphadenopathy, salivary gland infiltrates and proteinuria in MRL-lpr/lpr mice treated with ultra soluble curcumin/turmeric: increased survival with curcumin treatment. 2015 Sep
16. Hsu SD, Dickinson DP, et al, Green tea polyphenols reduce autoimmune symptoms in a murine model for human Sjogren’s syndrome and protect human salivary acinar cells from TNF-alpha-induced cytotoxicity. 2007 Mar; 40(2): 138-47. PMID: 17364504






I admire your vast knowledge
Thank you!
Finally helpful information to control Sjogrens, thank you for all your helpful research!!
Great to hear this! Thank you!
I love this! Very informative and helpful. I wish there was maybe a full list of what I should eat and maybe a small menu. I know it said a keto diet would be beneficial but I would definitely prefer your list and menu. Anyway, thank you very much for all this information. 🥰
Thank you Dr. This is very informative and helpful. The trick is in the diet. I have learnt that with proper anti inflammatory diet like alkaline foods you feel much better. Can we complement the conventional medicines with herbal teas like dandelion, sage, holy basil etc?