 Top 12 Inflammatory Lab Markers and Optimal Ranges
Top 12 Inflammatory Lab Markers and Optimal Ranges
Are you experiencing fatigue, aches and pains, skin issues, digestive complaints, headaches, or other nagging, chronic symptoms? Chronic inflammation may be the cause. Chronic inflammation is the root cause of most chronic symptoms and diseases. Testing for inflammation markers can help to find underlying health issues, uncovering the root causes of your problems, creating an appropriate treatment plan, measuring your progress, and regaining your health and vitality.
In this article, you will learn about what inflammation is. You will understand the problems with chronic inflammation. I will share the top 12 inflammatory lab markers and optimal rangers that can support your progress and health.
What Is Inflammation
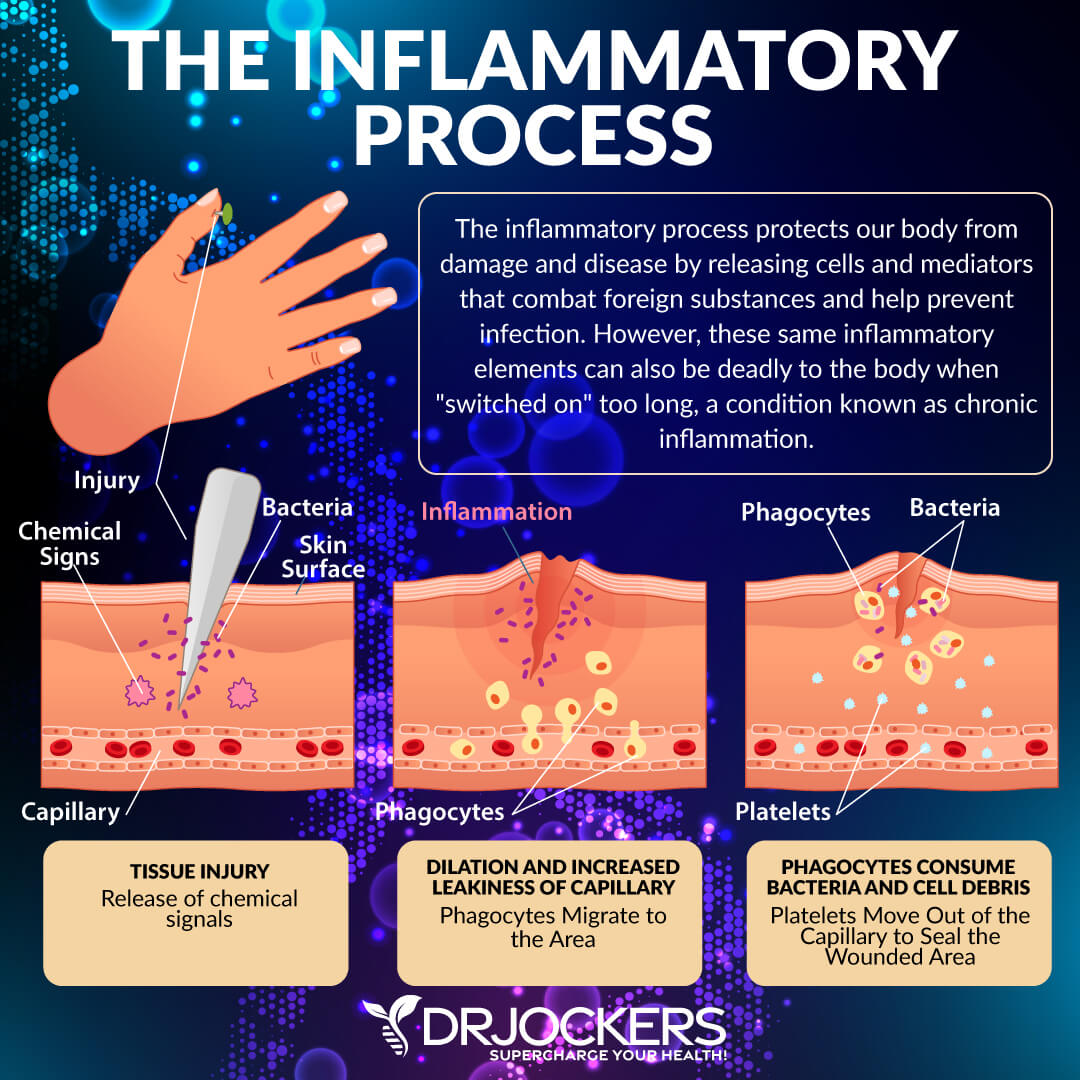
Inflammation is your body’s natural defense mechanism against foreign pathogens, toxins, allergens, injuries, and other harm. Your immune system’s response to any harm or cellular injury by increasing blood flow, capillary dilation, leukocyte infiltration, and the production of various chemical mediators. This complex process helps your body to produce antibodies and cytokines. This process helps to protect your body and fight hostile pathogens from eliminating toxic agents and repairing tissue damage.
In case of an injury, inflammation also helps to protect the affected area and support recovery. Inflammation is clearly necessary and a friend to your body when it comes to acute infections or injuries. However, as a 2015 article published in the British Journal of Nutrition explains, chronic, low-grade, systemic inflammation can be problematic and harmful (1).
The Problems with Chronic Inflammation
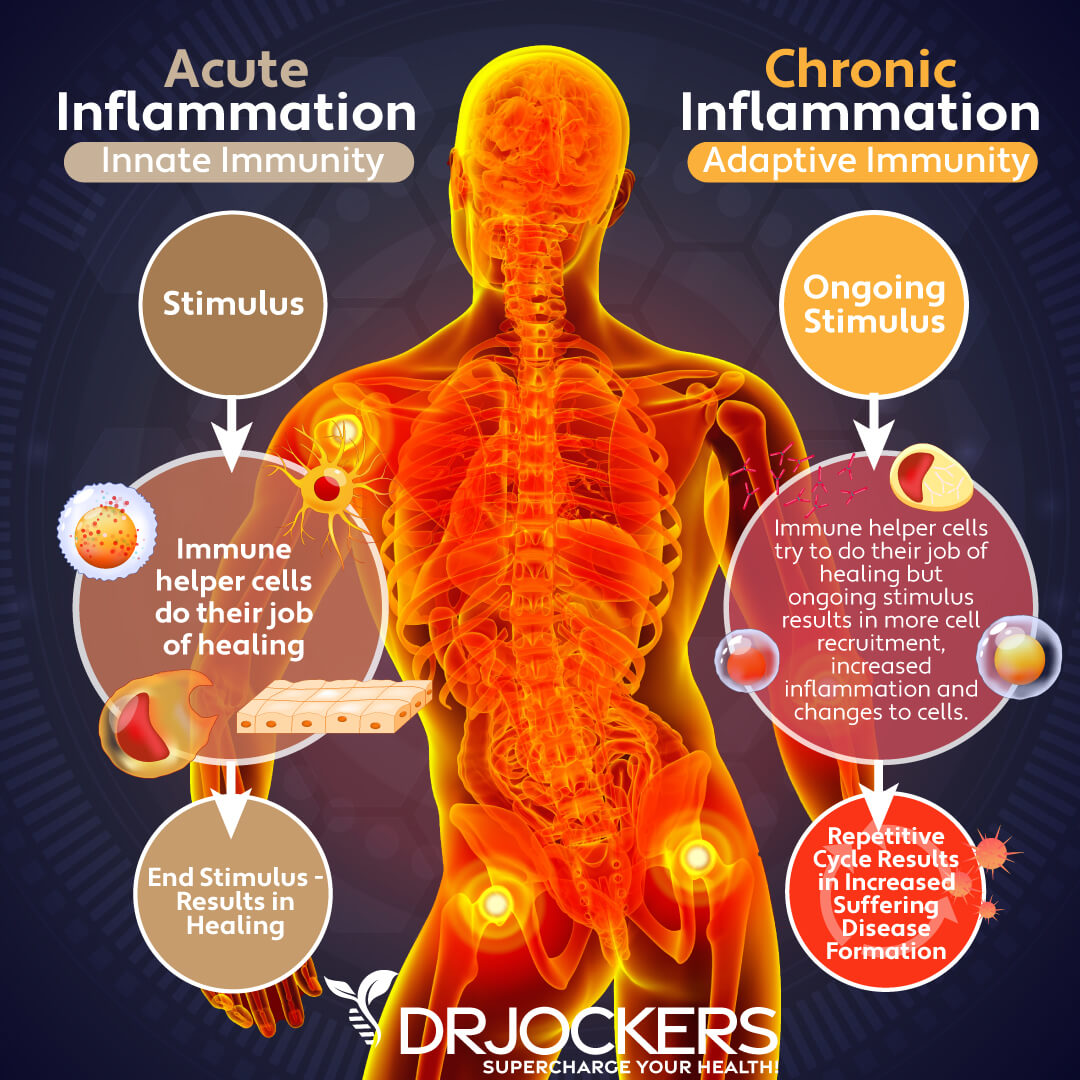
Acute inflammation is essential for your health. It’s a critical part of your body’s survival response to injury, infection, or illness. It protects you from pathogens and supports the recovery and repair of damaged cells. Acute inflammation starts quickly, usually within minutes, upon infection. It may last for a few days or in some cases a few weeks, but decreases gradually and disappears upon recovery. Signs of acute inflammation may include pain, swelling, redness, heat, itching, or in case of respiratory issues or allergies, sneezing, coughing, congestion, and watery eyes.
Chronic inflammation is different. Low-grade, chronic inflammation is systemic. It can last for months, years, or for life if not addressed. While acute inflammation tends to have a specific cause, such as an injury, infection, allergen, or toxic exposure, chronic inflammation doesn’t have one specific cause.
Chronic inflammation tends to develop over time due to a combination of issues, including a poor diet, poor lifestyle choice, chronic stress, environmental toxin exposure, and other factors. These factors place an excessive stress load on the body. As a response, your body produces inflammatory modulators throughout your body, which can overwhelm your immune system and body overall.
Chronic and ongoing inflammatory stimulus can lead to white blood cell recruitment, cellular changes, and increased inflammation. Excess white blood cells may end up attacking your cells, tissues, or internal organs, which will lead to a continuous inflammatory response and on-going health issues.
Chronic Inflammation and Chronic Disease
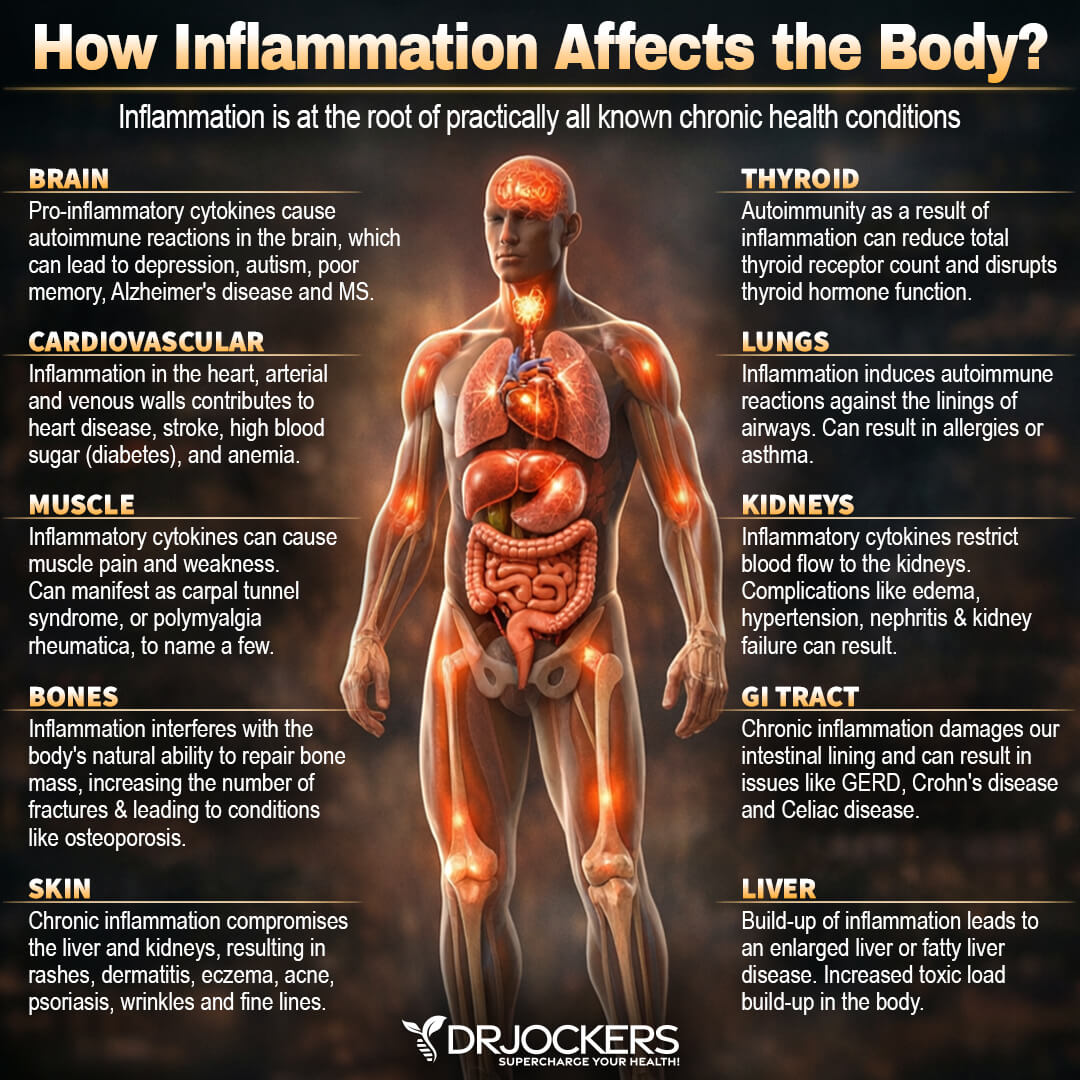
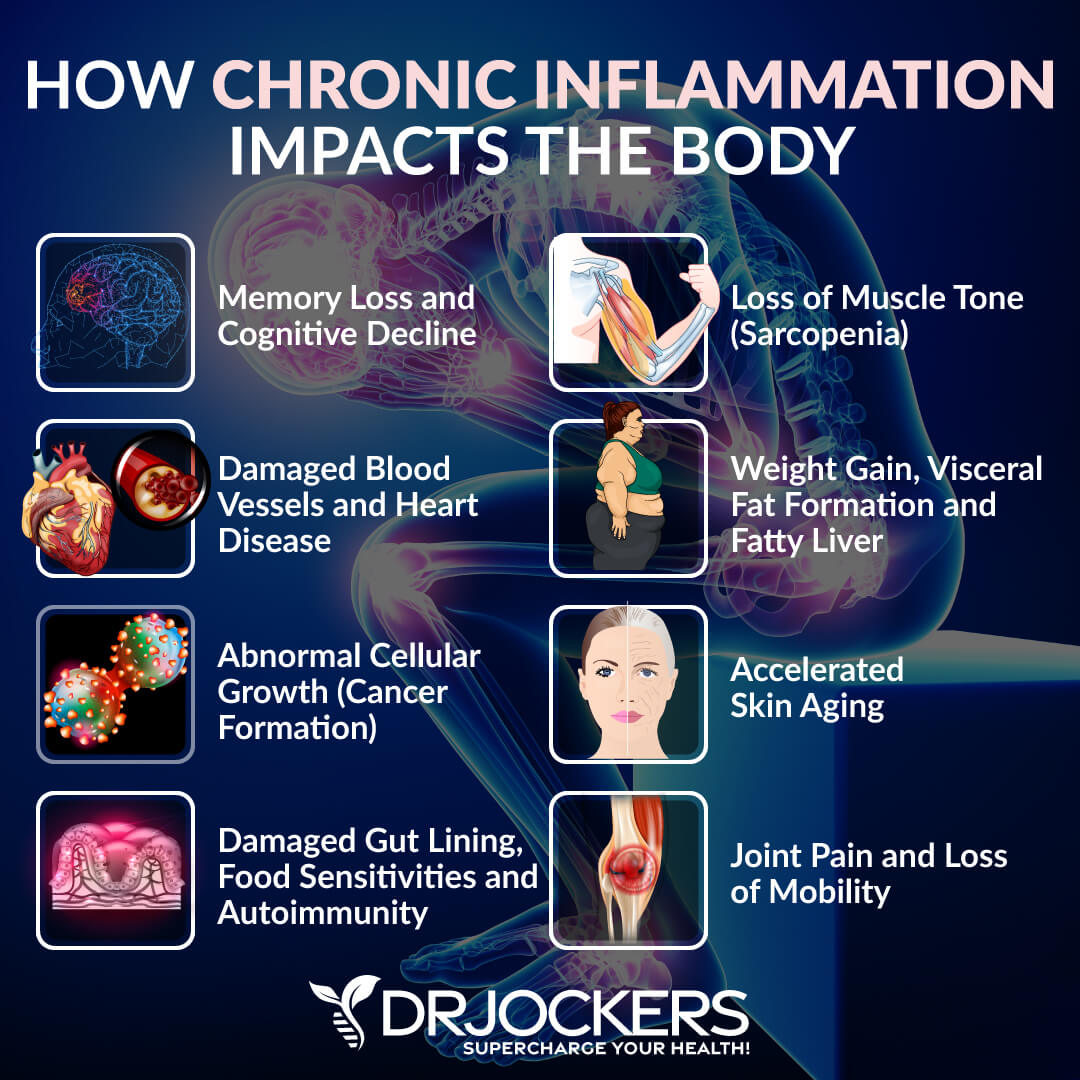
Chronic inflammation can be incredibly harmful to your body. Symptoms of chronic inflammation can vary from person to person and may include fatigue, chronic pain, headaches, migraines, muscles aches, joint pain, skin issues, brain fog, memory issues, insomnia, gastrointestinal issues, anxiety, depression, mood swings, weight gain, weight loss, obesity, hormonal issues, frequent infections, early signs of aging, and more.
Chronic inflammation can affect all areas of your body, including your digestive system, kidneys, liver, lungs, brain, endocrine system, hormonal health, heart, skin, muscles, and bones. According to a 2015 article published in the British Journal of Nutrition explains, chronic, low-grade, systemic inflammation is likely involved in the early stages of disease development. (1).
Scientific research, including a 2012 article published in EMBO Rep, has linked chronic inflammation to major degenerative diseases, including cancer, heart disease, diabetes, and amyotrophic lateral sclerosis (ALS) (2).
Chronic Inflammation and Mitochondrial Dysfunction
According to a 2010 review published in Autoimmune Reviews, chronic inflammation is also linked to autoimmune diseases (3). A 2015 study published in JAMA Psychiatry has linked chronic inflammation to brain inflammation, mental health issues, and brain health problems (4). Chronic inflammation may be connected to depression, anxiety, addictions, other mental health issues, memory issues, and neurodegenerative diseases.
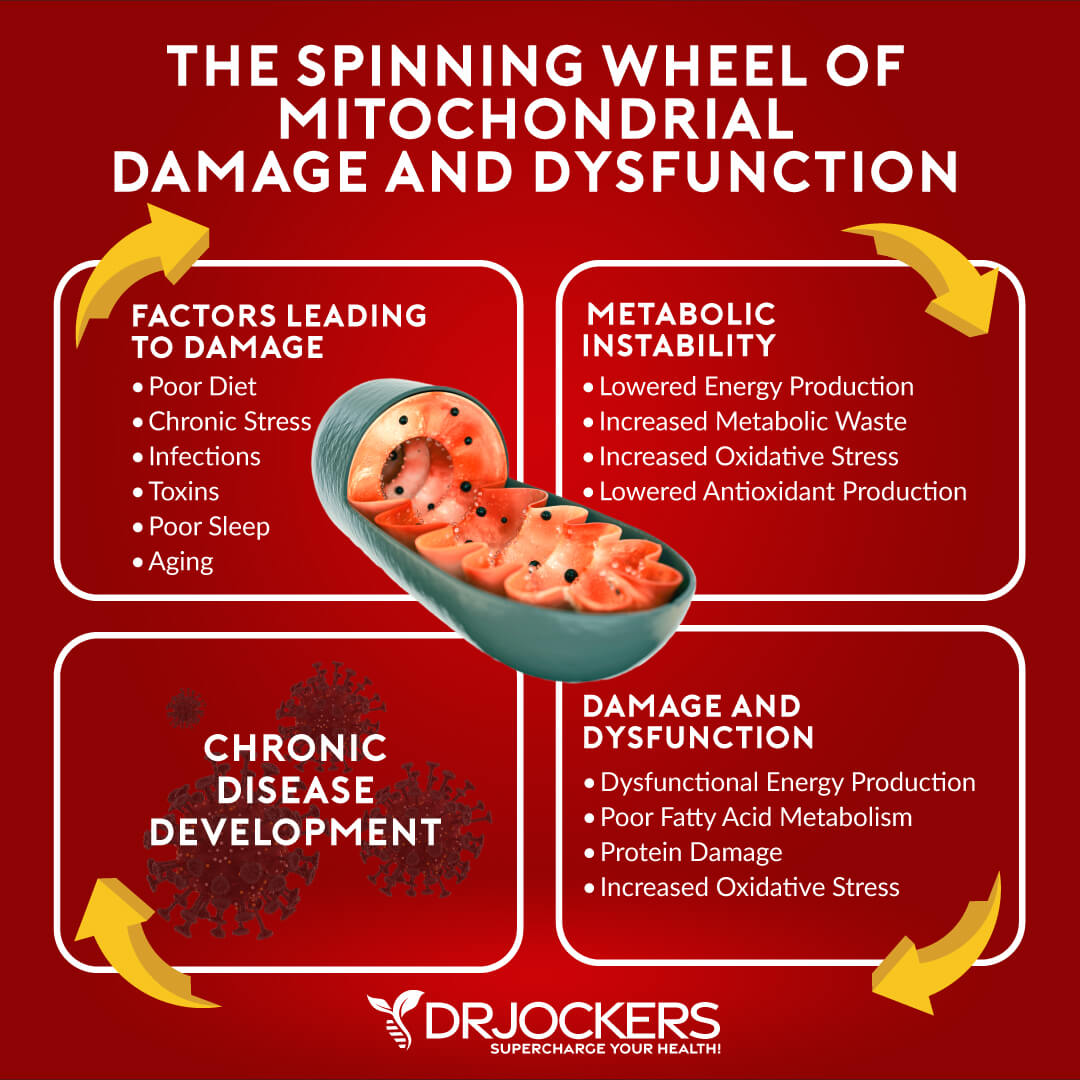
Mitochondria are tiny structures within just about every cell of your body. They are responsible for producing the energy your cells need to carry out their functions. What many people don’t realize is that these tiny structures are also very vulnerable to chronic inflammation.
What this means is that chronic inflammation damages mitochondria, lowers your body’s overall ability to function and heal, and steals energy from just about every process in your body.
Top 12 Inflammatory Lab Markers
Considering all the issues chronic inflammation can cause and all the symptoms, health issues, and diseases it’s associated with, it’s important that you get tested for inflammatory markers. Understanding inflammatory lab markers are critical for identifying underlying health issues and making appropriate changes to repair your body and regain your health and vitality.
It can help your functional health professional to create a personalized treatment plan, including dietary changes, lifestyle recommendations, and appropriate supplementation to improve your health. Here are the top 12 inflammatory lab markers you need to understand.

Hs-CRP
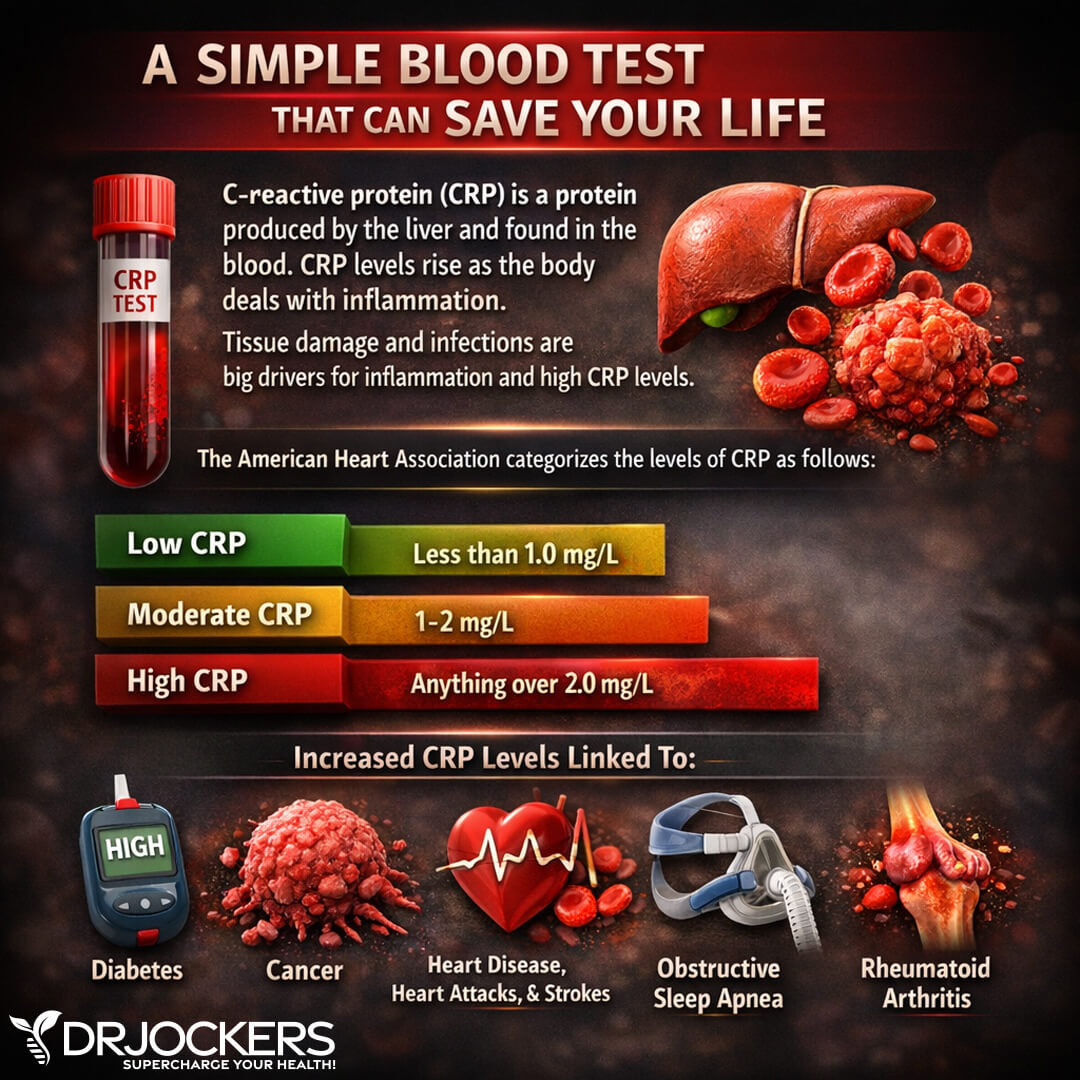
The C-Reactive Protein or CRP test is a key test I recommend. It measures a protein (CRP) produced in your liver that indicates inflammation levels in your body. A 2013 study published in Rheumatology has found that increased levels of CRP may be associated with muscle strength weakness in knee arthritis (5).
The clinical range is between 0 and 3 mg/L while the optimal range is 0 to 1 mg/L. When I see levels over 1 mg/L, I know the individual is having an inflammatory response that could be due to acute trauma or chronic conditions. Ideally, we want to see the CRP levels as low as possible, certainly under 1 mg/L and more like .50 mg/L or less.
Caution on Exercise: Be sure not to do any intense exercise within 24-48 hours of getting this lab done. If you have delayed onset muscle soreness from recent exercise, it will show up with higher CRP levels.
HbA1C
Blood sugar imbalances are one of the main causes of inflammation, so I recommend checking your hemoglobin A1C (HbA1C) levels. A 2005 study published in the Journal of Clinical Investigation, inflammation, stress, and diabetes are interlinked (6).
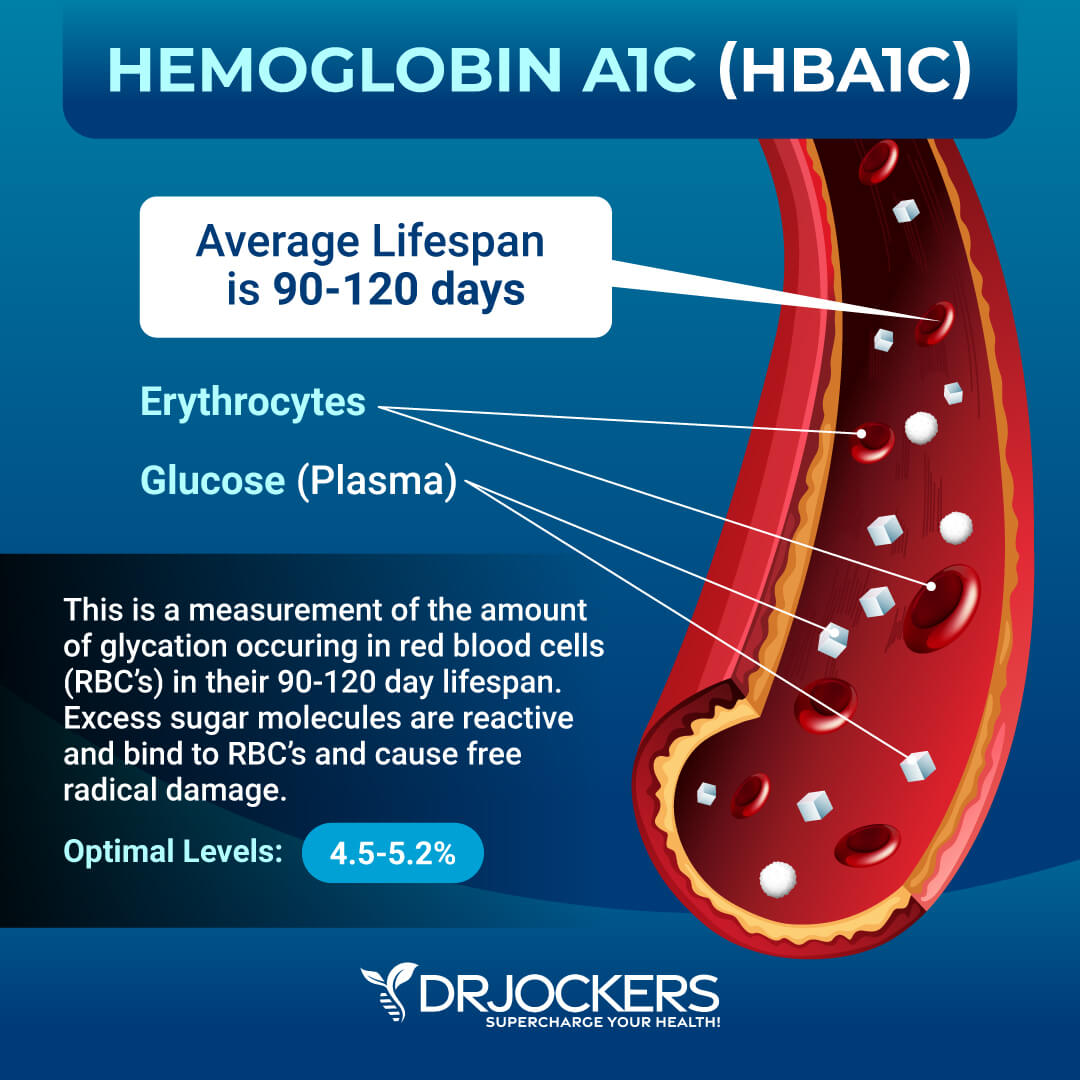
According to a study published in the Journal of Clinical Endocrine Metabolism, eating a Standard American Diet (SAD) increases the risk of obesity and metabolic diseases, which are both linked to blood sugar imbalance, increased risk of inflammation, and age-related chronic diseases (7). Your HbA1C levels measure your average blood sugar over the past 2 to 3 months.
Hemoglobin A1C (HbA1c) gives the average amount of glucose in your blood or blood sugar over the past 3 months making it one of the top tests for inflammation and diabetes. The clinical range is between 4.8 and 5.6 while the optimal range is 4.5 – 5.2.
Above 5.7% is considered prediabetic and diabetes is diagnosed with a HbA1C at 6.5% or higher.
Fasting Insulin
Blood sugar imbalances may increase your risk of inflammation. A 2016 study published in the Journal of Biomedical Sciences has found that the development of insulin resistance and increased inflammatory responses in your body may be interlinked (8).
In addition to testing your HbA1C levels, I recommend checking your fasting insulin levels. Testing your fasting insulin can recognize elevated blood sugar levels and can detect inflammation, insulin resistance, blood sugar issues, and diabetes.
The clinical range for fasting insulin is 2.6 – 24.9 uIU/ml and the optimal range is 2.0 – 5.0 uIU/ml.
You can see this is a very large difference between the lab clinical range. So, you may have a fasting insulin of 23 and it wouldn’t be flagged, and most doctors would think it is fine.
Why is Fasting Important? It is key to fast for roughly 12-14 hours before taking this lab so you don’t get a false positive or inaccurate results. If you finish dinner at 7pm, get your blood work done between 7am-9am the next day for the most accurate results.
Serum Ferritin
Serum ferritin measures the level of ferritin in your body to detect iron deficiency anemia and other health issues. A 2012 study published in the European Geriatric Medicine has found that increased ferritin levels may be associated with underlying iron deficiency and age-related inflammation in older people (9).
Ferritin is an intracellular protein that stores iron and releases it in a controlled fashion. It is the major protein responsible for storing iron within cells in a non-toxic form.
Iron is critical for producing hemoglobin within red blood cells to carry oxygen to cells. However, elevated iron in the blood acts as a free radical and increases oxidative stress. Ferritin helps store iron in a non-reactive form.
Ferritin in the blood serum is called an “acute-phase” reactant because it will elevate as an acute response to inflammation when pro-inflammatory cytokines such as IL-6 stimulate the liver to produce more ferritin.
Many bacterial, fungal and parasitic pathogens need iron and will steal it from our red blood cells. Ferritin helps protect against this so we can continue to make hemoglobin as we battle an infection.
While serum ferritin will elevate during infections but can also be elevated from non-infection related inflammatory conditions.
High ferritin levels are seen in various inflammatory conditions, including autoimmune diseases, liver damage and certain cancers. Low ferritin can also be a problem and indicate an iron deficiency anemia or subclinical anemia that isn’t quite diagnosable yet.
The normal range for serum ferritin for males and post menopausal women is 20 – 300 ng/mL and for menstruating women is 10-150 ng/mL.
The optimal range for serum ferritin is 50-150 ng/mL for females and 75 – 150 ng/mL for males.

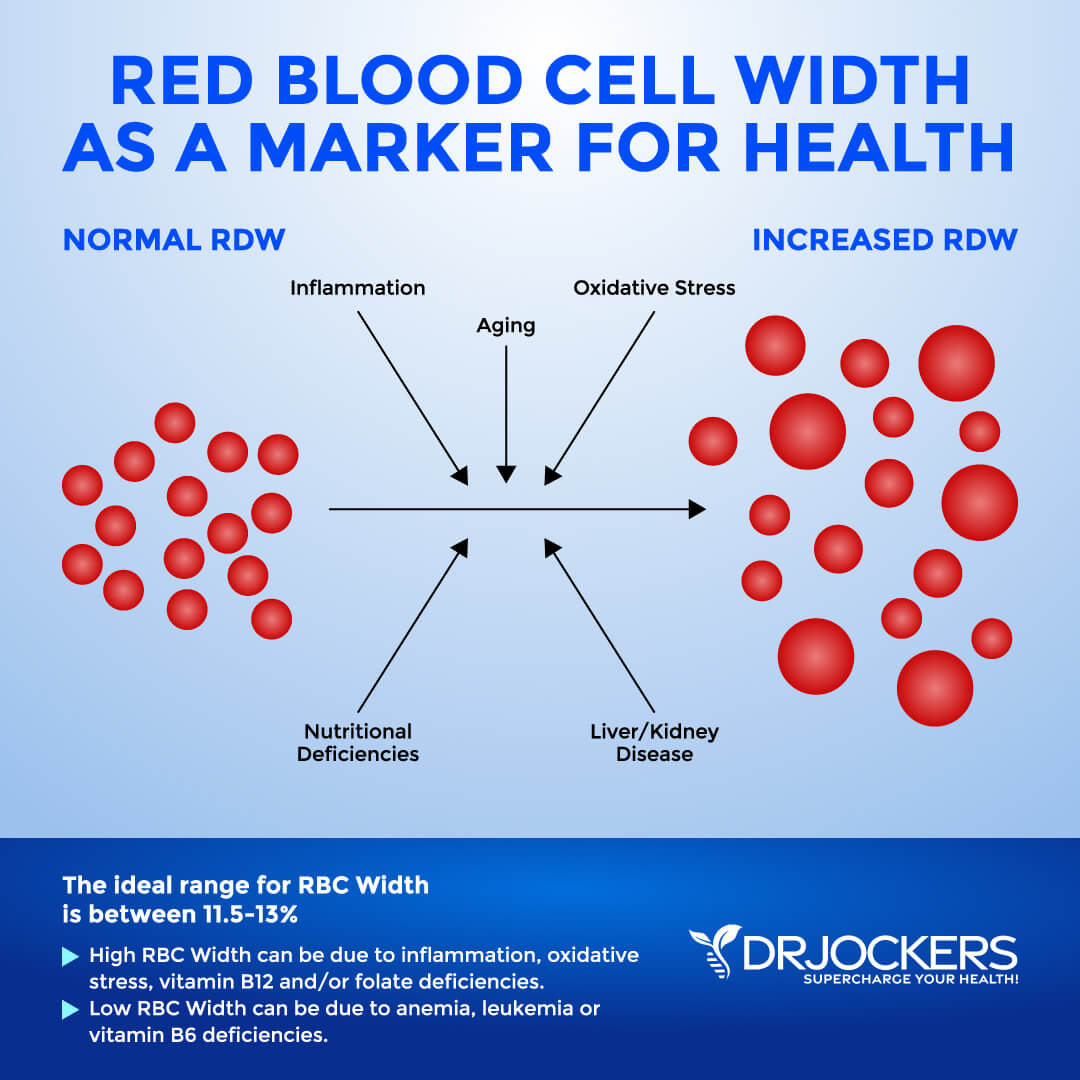
Red Blood Cell Width
The size of your blood cells has to do with maturation and also depend on methylating agents, such as folate and vitamin B12. Red Blood Cell Distribution (RDW) markers are a great way to detect underlying inflammation in your body. A 2018 study published in Science Reports has found that RDW levels may be linked to sarcopenia, an inflammation-related condition affecting older people (10).
The clinical range is between 12.3 and 15.4 percent while the optimal range is 11.5 and 13 percent. When this level is above 13% it may be a sign that inflammation has impacted the development of the red blood cell.
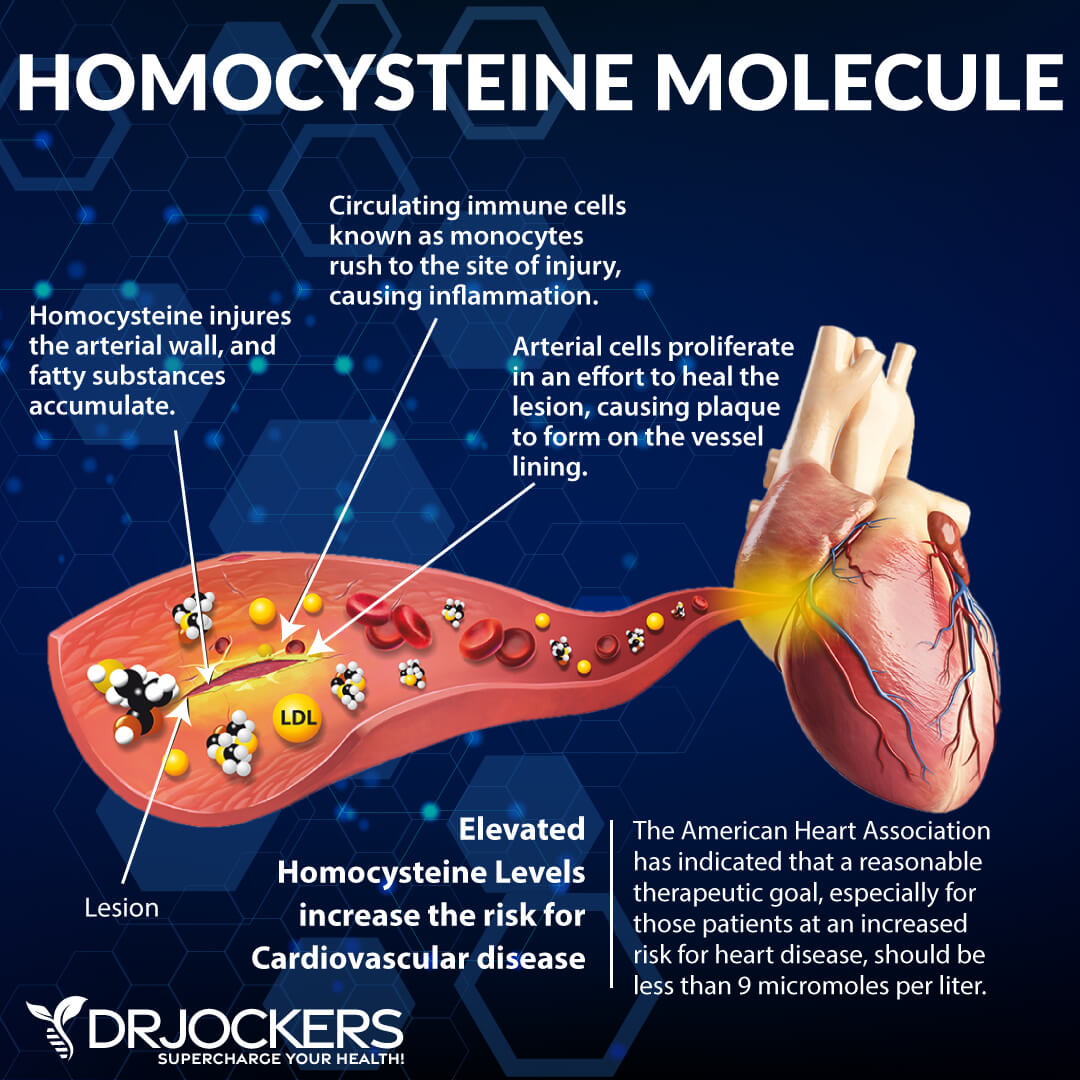
Homocysteine
Homocysteine is a common amino acid in your blood that you mostly get from eating meat. Homocysteine is particularly a good marker for cardiovascular issues.
Homocysteine is an inflammatory amino acid formed through the metabolism of another amino acid named methionine. Methionine metabolism is necessary to form key neurotransmitters such as dopamine and serotonin as well as the master antioxidant glutathione.
Homocysteine is constantly being produced in our body, but it should be kept under control. When it is elevated, it increases inflammation in the blood vessel wall and increases the risk of cardiovascular disease, high blood pressure, blood clots as well as dementia and Alzheimer’s disease.
High homocysteine occurs when people are deficient in B vitamins, especially vitamin B2, folate, vitamin B6 and vitamin B12 as well as zinc and choline.
According to a 2010 study published in Experimental & Clinical Cardiology, elevated homocysteine levels may indicate inflammation and acute coronary syndrome (11).
The normal range for homocysteine is 5 -15 umol/L while the optimal range is 4-8 umol/L. Some practitioners like to see it under 7 umol/L.
ESR
The erythrocyte sedimentation rate (ESR) is a common hematology test to look for inflammation It refers to the rate at which your red blood cells in anticoagulated whole blood go down in a standardized tube over a period of one hour.
Red blood cells (RBCs) normally have a negative surface charge due to the presence of sialic acid residues on their membranes. This negative charge causes them to repel each other, preventing them from clumping together and settling rapidly.
Inflammation causes the blood plasma to increase positively charged proteins such as fibrinogen and CRP. These positively charged proteins bind to the negatively charged RBCs and reduce their negative charge.
This results in the RBC’s sticking together or aggregating and forming stacks called rouleaux. The rouleaux has a larger mass and causes the stacks to settle in the tube faster which is measured on the ESR (12). Anything over 20 mm/hr is a sign of significant inflammation and optimal results should be under 10 mm/hr.
You can also look at platelets as a measurement tool of inflammation and the stickiness of blood. Platelets elevated above 250 is a sign of inflammation. The sweet spot for platelets is between 175 and 250. Below 175, immune function and blood clotting are compromised; the same is true for levels above 250.

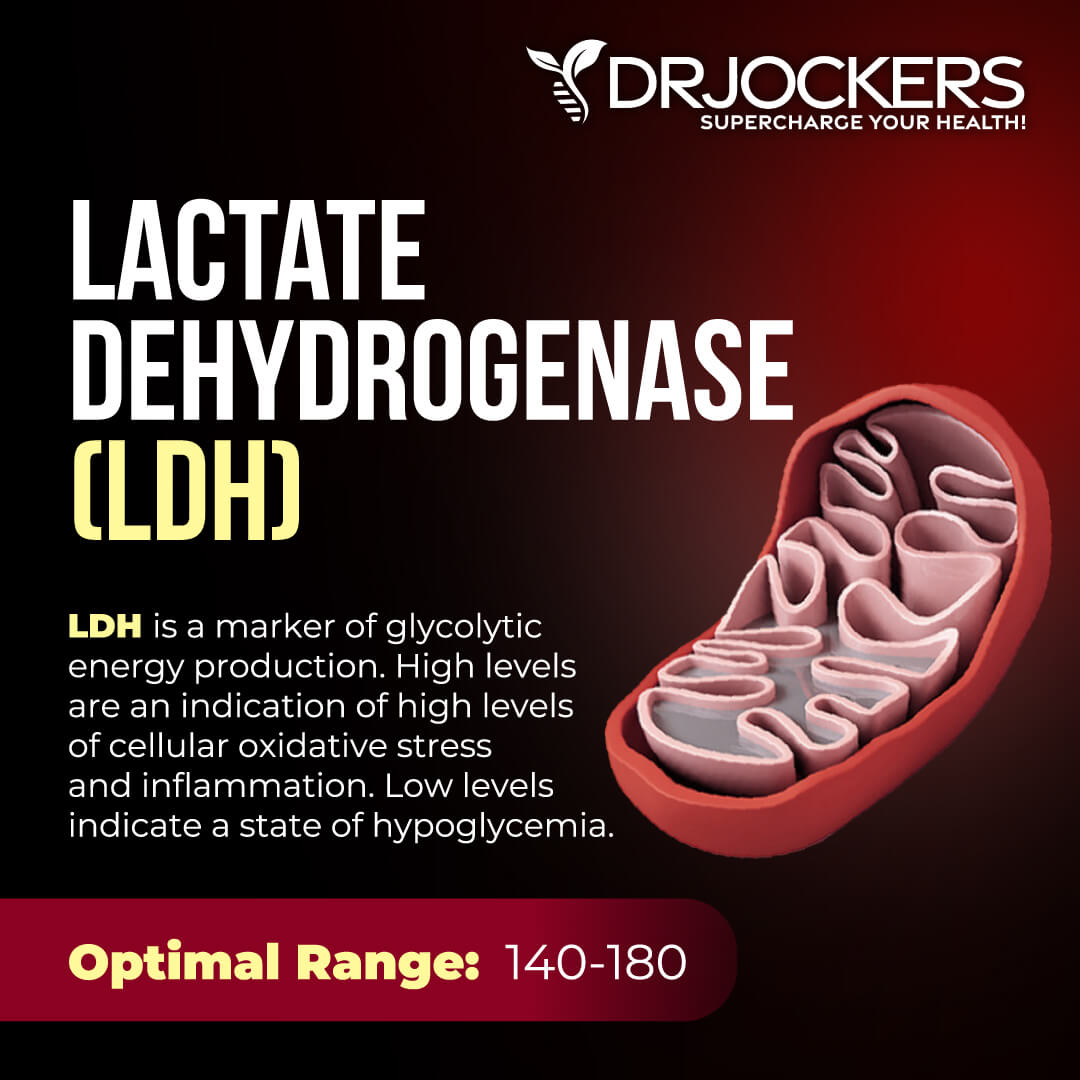
LDH
LDH is an enzyme found in almost all body tissues, including the heart, liver, kidneys, muscles, brain, and red blood cells. Its primary function is to help convert pyruvate to lactate, which is part of the process of creating cellular energy through glycolysis (the breakdown of glucose).
Under normal circumstances, there’s a low level of LDH in the blood because cells maintain their integrity. However, when cells are damaged or destroyed due to injury, disease, or infection, they release their contents, including LDH, into the bloodstream, causing levels to rise.
Additionally, high LDH is a sign the cells are stuck in “sugar burning mode” even when oxygen is present. This is called the “Warburg effect” named after the famous German doctor who studied cancer cells and found they had this phenomenon of aerobic glycolysis. We will discuss this more in chapter 3.
A high LDH is a sign of poor metabolic flexibility due to poor mitochondrial function and cellular inflammation. According to a 2020 retrospective and observational study published in Aging (Albany, NY), elevated LDH markers may be a risk factor for severe respiratory illness (13).
Normal levels of LDH are between 140 – 280 U/L. Optimal levels are between 140-180 U/L. As you can see, the optimal levels are a much lower range than what will be flagged on the lab test.
Side Note: A low LDH, under 140, is a sign of poor glycolysis, where the cells struggle to produce energy from glycolysis. This can be a sign the individual is dealing with hypoglycemia or low blood sugar levels due to a poor ability to metabolize stored glycogen.
Neutrophil-Lymphocyte Ratio
The NLR is part of the complete blood count, and it can indicate inflammatory processes. It is important to note, that you typically won’t be given the NLR, but instead you will be given the number of neutrophils and lymphocytes.
- Neutrophils are a white blood cell that are part of the innate immune system and first responders to inflammation.
- Lymphocytes are a white blood cell that are part of the adaptive immune system that are involved in long-term immune responses.
When inflammation occurs, the body will release more neutrophils and this may suppress the number of lymphocytes. This would result in a higher NLR.
Studies have shown that the NLR can be used as a prognostic marker for metabolic disease, heart disease, cancer and infections (study here, here and here). According to a 2012 study published in the International Archives of Medicine, NLR is a good measure of inflammation associated with prevalent chronic diseases (14).
NLR is usually measured with the absolute count of neutrophils and lymphocytes and not the % of these white blood cells. The optimal range is 1.2-2.0.
If you see that the number of neutrophils is more than twice the number of lymphocytes it is a sign of chronic inflammation.
Side Note: In some viral infections such as Epstein Barr and cytomegalovirus as well as certain cancers like leukemia, you will see a low NLR under 1.2.
NLR is usually measured with the absolute count, and we want to see it at roughly 1.2-2.0. If you see that the number of neutrophils is more than twice the amount of lymphocytes it is a sign of chronic inflammation.
Liver Enzymes
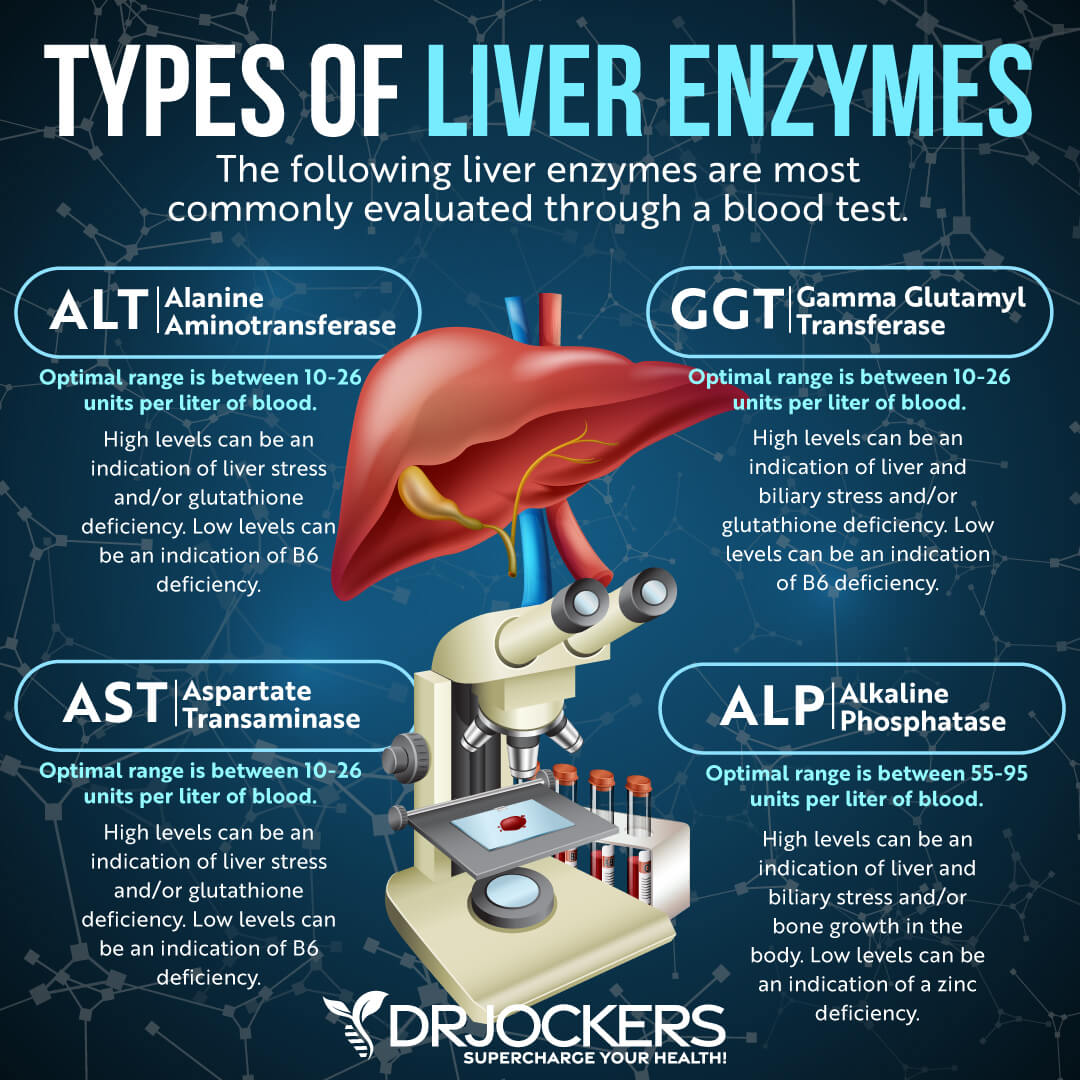
Liver enzyme levels may also indicate inflammation, as well as liver, gallbladder, bile, or kidney issues. According to a 2019 study published in the Indian Journal of Clinical Biochemistry, there is an association between elevated liver enzyme levels, inflammation, and cardiometabolic problems (15).
Alkaline phosphatase is a liver enzyme that is made by the mucosal cells that line the bile system of the liver and helps normal bile flow. Elevated levels (over 95) may indicate inflammation and liver and gallbladder problems.
Alanine aminotransferase (ALT) is a liver enzyme. Elevated levels may indicate inflammation. Normal levels are between 10 and 26 IU/L.
Aspartate transaminase (AST) is an enzyme present in the liver that spills out during times of increased liver stress. Elevated levels may indicate inflammation Normal levels are between 10 and 26 IU/L.
Gamma-Glutamyl Transpeptidase (GGT) is an enzyme in the liver, pancreas, and kidneys. Elevated levels may indicate inflammation and liver disease, usually due to alcoholism and/or sluggish gallbladder or gallstone obstruction. Normal levels are between 10 and 26 IU/L. Levels lower than 10 IU/L can be an indication of a vitamin B6 deficiency.
Lipid Panel
Your lipid paneer may be another indication of inflammation and related issues, such as clogged arteries and cardiovascular issues. According to a 2019 article in The Effect of Inflammation and Infection on Lipids and Lipoproteins published by Endotext, elevated lipid levels may indicate inflammation or infection (16).
Having a balanced ratio of LDL to HDL and triglycerides to HDL is essential for your health. Ideally, we are looking for an LDL: HDL ratio: 3:1 or less, 2:1 being optimal. As we analyze triglycerides, we want them to be under 100 and we are looking for the Tri:HDL ratio to be 2:1 or less, 1:1 being optimal. Higher rates may indicate insulin resistance and inflammation. For more info on the lipid panel, read this article. Optimal levels:
- VLDL cholesterol: The ideal range is 5 to 30 mg/dl.
- HDL cholesterol: The idea range is 55 to 80. Levels above 100 can indicate chronic inflammation or active infection in the body.
- Triglycerides: The ideal range is 40 to 80.

Vitamin D3
Vitamin D3 is an important vitamin that most of our population is deficient in. Poor levels may indicate inflammation. A 2014 study published in the Journal of Inflammation Research has connected low levels of vitamin D to inflammatory diseases, including atherosclerosis-related cardiovascular disease, inflammatory bowel disease, chronic kidney disease, nonalcoholic fatty liver disease, and asthma (17).
Optimal healthy levels of vitamin D are between 50 ng/mL and 70 ng/mL, while therapeutic levels are over 70 ng/mL up to 100 ng/mL

Comprehensive Blood Analysis
To check for these health markers, I recommend a Comprehensive Blood Analysis (CBA). This is the most detailed blood test that looks at all of these markers of inflammation. This test is more sophisticated than most conventional doctors are able to order.
It examines all parameters for inflammation, blood sugar levels, thyroid function, zinc and copper ratio, vitamin A and D levels, a complete metabolic panel, complete blood count, liver function, nutrient deficiencies, and more. I recommend getting the Comprehensive Blood Analysis done regularly both as a preventative measure and to monitor your inflammation levels and progress.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!
Final Thoughts
Chronic inflammation is the root cause of most chronic symptoms and diseases. Testing for inflammation markers can help to find underlying health issues, uncovering the root causes of your problems, creating an appropriate treatment plan, measuring your progress, and regaining your health and vitality. I recommend the Comprehensive Blood Analysis to test for the top 12 inflammatory lab markers to help your recovery.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website offers long-distance functional health coaching programs with our world-class team of health coaches. For further support with your health and other goals, just reach out—our fantastic coaches are here to support your journey.





great article. your page is execelent
Thank you!
How much does it cost to get the comprehensive blood analysis from Doctor jockers? Thank you
You can find that info here Sarah: https://drjockers.com/comprehensive-blood-analysis/
Well, here’s a question for many on Medicare – does Medicare cover the lab tests you recommend?
They may cover a few if you speak to your physician but will probably not cover all of these.
That’s very sad as we need to have these tests done and many pay high premiums for supplemental coverage.
Yes but if you request them, often your physicians will run these.
Dr. Jockers, having this list with all the why’s and what’s about each test is a great value!
Thank you for continuing to educate us on the things we really need and desire to know in a way that lays out the whole picture. Your approach resonates with me & I’ve gained so much from your articles. 🙂
So glad to hear this has been helpful Lorrie! Blessings to you!
Wondering about how to treat Afib. Both my parents had it and I now have mild afib. I can’t seem to find any articles on afib and how to treat it holistically. It’s never mentioned in heart health articles yet apparently it’s fairly common.
Hello Diane, sorry to hear this! Here is a helpful article on Afib: https://drjockers.com/atrial-fibrillation/
I’m having trouble finding any holistic cure/treatment for chronic pancreatitis EPI. Many on chronic pancreatitis but not the EPI aspect. Do you have any suggestions?
Hey Julie – yes here is an indepth article on this topic: https://drjockers.com/pancreatitis/
Excellent information Doc Jockers; thank you for your hardwork and dedication to educate the public
Thank you and blessings to you!
Thank you for the excellent article on Afib. I was recently diagnosed and have high blood pressure and Hashimoto thyroiditis. It seems they are all linked. I have a better understanding of my condition.
Yes this is true, they are all connected. Here is a helpful article on Hashimoto’s: https://drjockers.com/hashimotos-thyroiditis/
Thank you so much for this article. I was able to compare most of these to my last blood tests and interpret whether or not I was in a healthy state. This was incredibly useful.
Great to hear that Diane! Blessings to you!
Dr. Jockers,
I had a 10 day round of Cipro for a UTI about 18 months ago. I have felt ill and have never fully recovered since that time. I ache, have trouble sleeping, and seeking the help of a Psychiatrist for depression. Many of my sicknesses seem like Chronic inflammation type symptoms. I seem to have been affected by many of Cipro’s serious side effects but my Physician doesn’t believe I was affected. Would the 12 Inflammatory Lab Markers tests confirm or at least identify if Cipro has some how affected my health?
Thank you
Hello Steve,
Sorry to hear this. It will be hard to pin any lab findings to the Cipro as many factors can lead to higher levels of inflammation, but it will give you an idea of your inflammatory levels overall.
I don’t think Cipro is your problem. You were on it too short of time.
Great article!
Where can I get these tests?
Do I need a doctor prescription to get the labs?
Dr. J
I have high blood pressure and on two medication but it is not helping me. Can you help me. Please. Thank you.
Hey Veronica, sorry to hear this! Here is a helpful article: https://drjockers.com/hypertension/
Dear Dr Jockers,
Firstly, thank you for this article, I found it very informative. So please take this comment in the spirit that it is intended.
You state that Chronic Inflammation is the ‘cause’ of diseases (something oft quoted in the medical community with little evidence to prove itself), but then go on through the article mentioning that it is a symptom of various things like lifestyle, diet, disease, etc…
It cannot – I believe – the the symptom AND the cause at the same time.
If we disgusts all of the chatter and simply THINK we usually come back to ‘My inflammation is my body’s response to a problem.’ Thus, instead of looking at inflammation as the culprit, we should be looking at it as a valuable warning that something is wrong (as you actually discuss in your article).
That inflammation is present in the body when we discover illness or pain DOES NOT mean that such illness or pain is CAUSED by the inflammation (although it is possible, more actual scientific study rather than speculation is needed).
In short, correlation does not equal causation.
The problem with the conclusion that inflammation is the ‘cause’ of illness is that it sets in motion the quest to end inflammation instead of the quest to end the underlying disease – be that a virus, an injury (the body can be injured by poor diet, lifestyle choices, etc..), bacteria, heavy metals or other toxins, etc…
Instead of placing the focus on the actual ‘cause’ today’s medical profession is focusing on the symptom and body’s natural response as an enemy to fight, and so the rise in ‘anti-inflammatory’ drugs and foods.
The pharmaceutical company’s love the distraction because it sells products, but we as a species should be focused on actual healing, and ending, or at least reducing disease, and taking our attention away from the causes and placing it on the symptom is a distraction from that goal.
In closing; inflammation is our body’s way of fighting against injury in its many forms. High inflammation markets should be a warning sign that we need to cure an underlying problem NOT fight inflammation.
Again, I want to thank you for this article, and I hope that my above opinion is not taken as an insult against your great work.
Sincerely,
Joe
Colorado
Thank you for sharing Joe. Yes chronic inflammation is at the root of all chronic disease, but inflammation is caused by poor lifestyle factors, infections, toxins, etc.
I live in Canada, are these the exact names of the tests I should bring to my physician? so I can get a prescription for the Lab. Or if I got. Prescription from one of your coaches, would work here in Canada?
Thank you for such an in-depth, informative article. I do have a question—Regarding lipid panel ratios, I’m wondering if my LDL:HDL ratio (.90:1) is considered acceptable because it’s less than 1:1. Also, my triglycerides:HDL ratio ( .40:1) is less than 1:1. Should I be concerned? (My cholesterol numbers seem high—LDL: 116, HDL:128, Triglycerides:46). Thanks
Yes the HDL is very high which is often an indication of an active infection. I would recommend working with a functional health practitioner to find the root cause. https://drjockers.leadpages.co/long-distance-coaching-dr-jockers/
Excellent summary, as a Med Lab Scientist I will use it.
I have a reaction to Wifi. I experienced swelling at the lymph nodes by armpits to the back, zapping, and burning. After this latest occurrence I decided to go full Ethernet. Immediately, within 1 day, the swelling went down and I feel so much better.
Do you have any info? or have you encountered this condition?
Sorry to hear about that. We do have a helpful article on EMF here: https://drjockers.com/emf-exposure-dangers-symptoms-and-protection/
As always Dr. Jockers, excellent material, nicely done visuals and so easy to read and understand. God bless you richly
Good site! I truly love how it is nice on my eyes it is. I am wondering how I might be notified when a new post has been made. I have subscribed to your RSS feed which may do the trick? Have a great day!
Yes you can!
Why did you not include a D-dimer test? (I hope you know where I’m going with this.)
Yes that is a good test as well!
The trouble is now I have to convert all the USA measurements to metric like lots of other people around the world that do not get blood results using imperial measurements, metric units is so much more logical.
Excellent & very important article – THANK YOU! I’m sending this to my big family.
Thanks so much for your support!
Thank you Dr. Jockers for this information.
I just had the worst week of (pins, needles, zapping feeling) under my skin… Then it turned to inflamed big toe, now the inflammation went from the toes to the shoulders….. It feels like it’s just bouncing around in there, along with a headache.
I took (1.chorella, sprinula, alfalfa seed powder, charcoal,)
(2separate lemon juice)
(3baking soda with molasses)….. desperate to make it all stop…. Then castor oil on my shoulders today 4/24/25… I’m not sure how it started; high vibration through a massage gun, or a gf brownie that was homemade ingredients, no clue … But it was a horrid week. I wish there was a solution… My Dr aren’t digging to help me figure out the pins and needles… I’ll compare your blood panel suggestions to my blood panel and see if I can be a detective under cover…. God bless the work of your hands!
Very sorry to hear this! I would recommend working with a great functional health practitioner to figure this out. Our team can help: https://drjockers.lpages.co/long-distance-coaching-dr-jockers/
The only thing I could not understand is how the Triglycerides to HDL ratio ideally would be 1:1. Your optimal triglycerides were 40 – 80 mg/dl which = .45 – .90 mmol/L. Mine was .47 so still in that optimal range but barely. For HDL cholesterol you said optimal was 55 – 80 mg/dl which = 1.42 – 2.07 mmol/L. Mine was 1.69 which is in that range. But these can never be a 1:1 ratio using your optimal ranges.
I greatly appreciated this very detailed information. I appreciate being able to comment. I have blood tests showing Sjogrens & Lupus specaled pattern. My Neutrophils haved been on jumping around over number of years, and have dropped lower over the last 2-4 years. I have a healthy diet habbit. I am supplementing with Vit. D3, K2, Bmethylated complex, Zinc and Magnesium. I suffer with nerve damage. I am list to Haematologist. PLEASE What can I do to build up neutophils?