Is Your Brain Making Enough GABA?
GABA (Gamma-Amino Butyric Acid) is an inhibitory neurotransmitter that has a calming and relaxing effect in the brain. It acts like the brakes in a car, to where it slows down and/or stops brain activity on an as-needed basis to help us function better.
When we are low in this neurotransmitter, our brain continues to hit the gas, overstimulating us with activity. Our gut microbiome plays an important role with GABA production and helps to convert glutamine and glutamic acid into GABA. A disordered microbiome is a major cause of low GABA production (1, 2).

GABA’s Activity in the Brain
GABA receptors are spread out throughout the brain and they are ligand-activated chloride channels that when activated, allow the negatively charged chloride ions across the cell membrane and into the cell where they reduce cellular activity. In addition, they help to shunt the positive charged potassium ions across the cell membrane and out of the cell in order to inhibit activity and take the nervous system away from threshold.
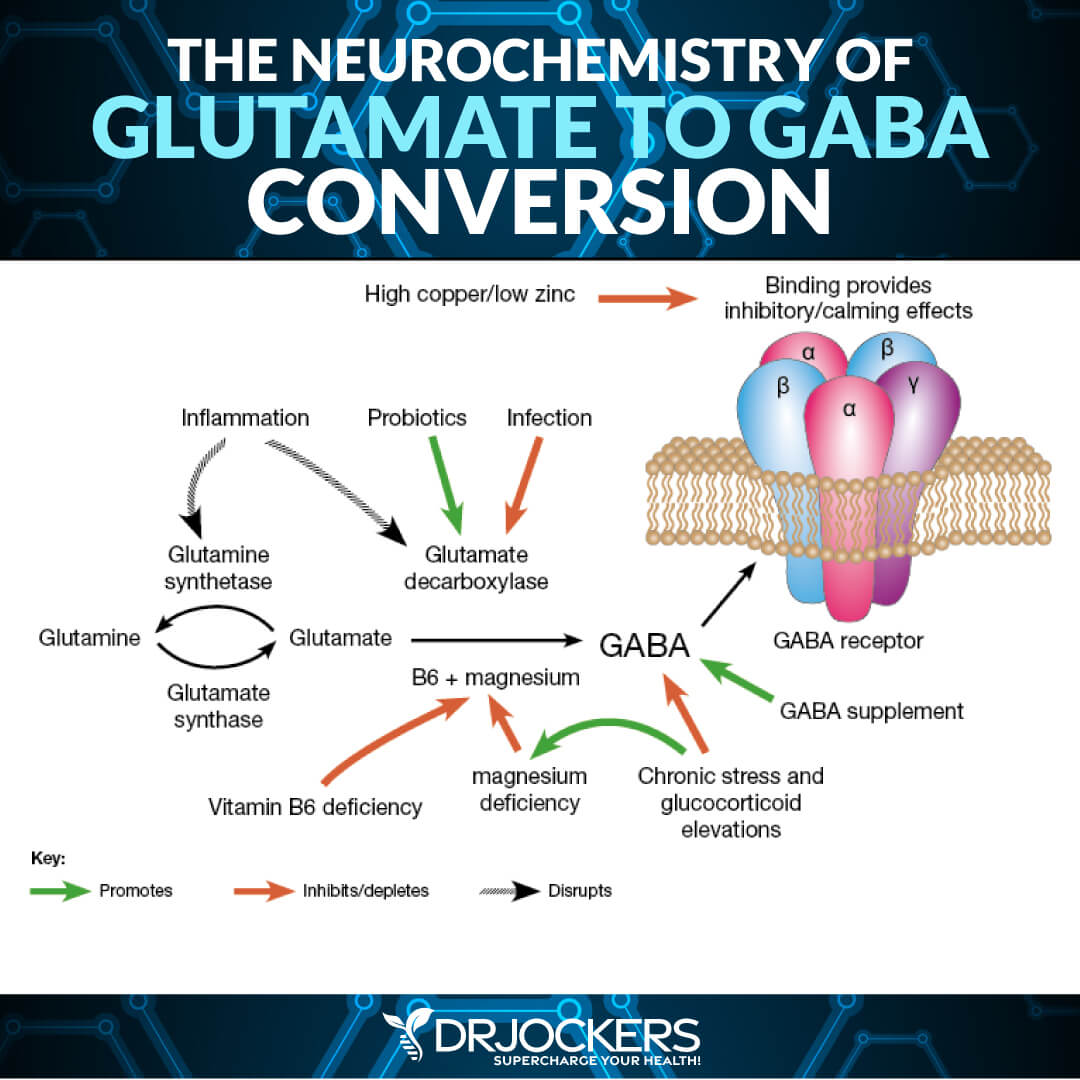
GABA is synthesized from the amino acid glutamate with the enzyme glutamate decarboxylase (GAD) and pyridoxal phosphate (which is the activated form of vitamin B6) as the key cofactor. This process converts glutamate, which is the principal excitatory neurotransmitter in the brain, to the principal inhibitory neurotransmitter GABA (3, 4).
In most regions of the brain, GABA is too large a molecule to cross the blood brain barrier (BBB) (5). However, there are certain areas that have a permeable barrier, such as the periventricular nucleus of the hypothalamus, which sits in the 3rd ventricle of the brain. GABA has been shown to influence brain activity through this region and help to modulate the amount of human growth hormone release (6).
GABA is also an important part of the synthesis of the sleep hormone melatonin. It has a key role in the conversion of serotonin into N-Acetylserotonin, which then converts to melatonin for inducing sleep (7). Melatonin also plays a huge role in the body’s immune function.

Factors Involved in Reducing GABA Levels
People with low levels will often see a worsening of these symptoms when they skip a meal or attempt to do intermittent or extended fasting. If you are noticing this, it may be a sign of low GABA levels.
There are some common factors involved in reducing GABA levels. Here are the ones to consider.

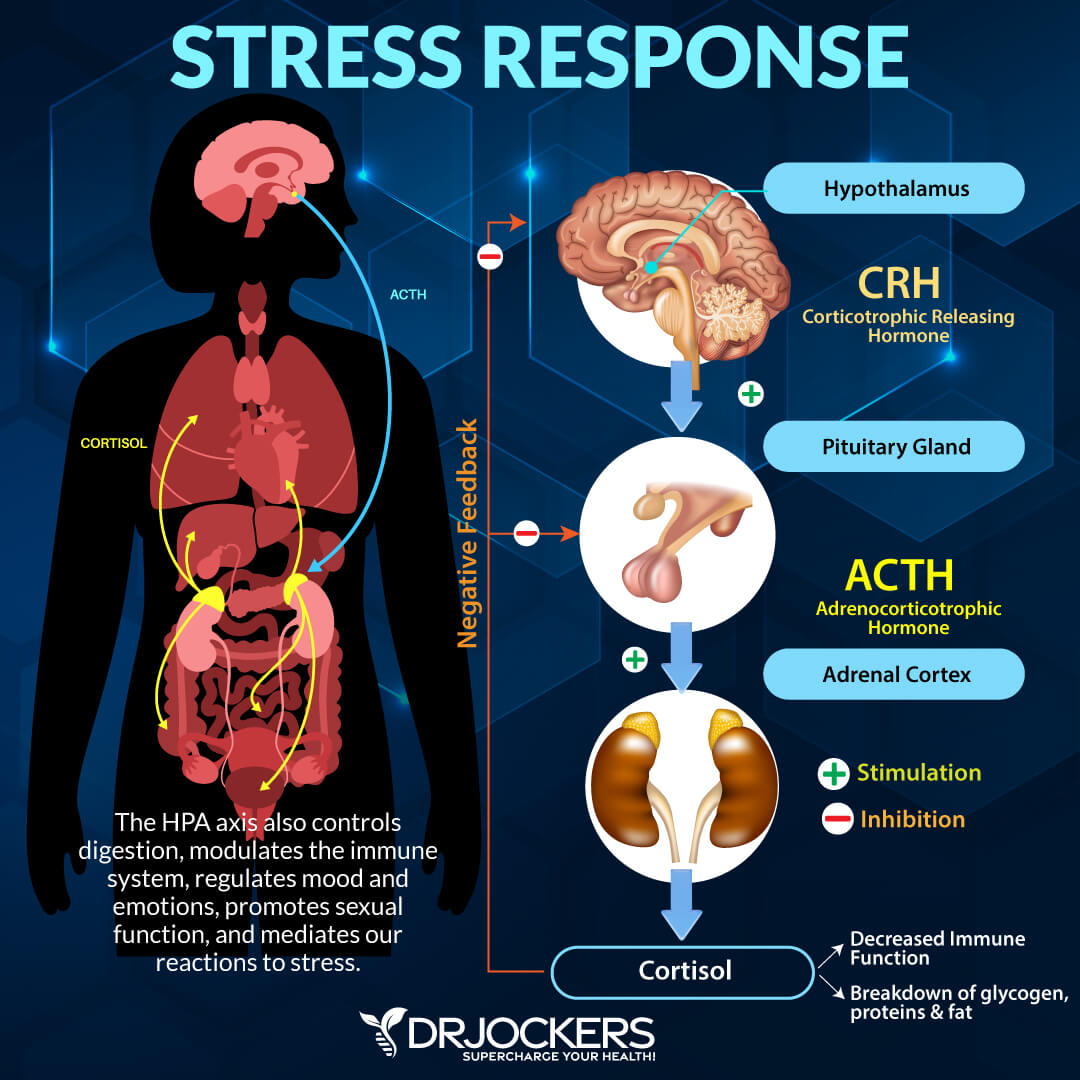
Chronic Stress and Adrenal Fatigue
Chronic stress will increase the levels of cortisol, norepinephrine and epinephrine in the brain and body. This also shunts the body into producing more excitatory glutamate and reduces GABA production (8).
Too much glutamate in the brain causes over-excitation of the brain cells. In addition, the increase in stress hormones ramps up cellular activity and causes excessive production of free radicals which damage brain cells and further reduce normal GABA production (9).
Overtime, when an individual is in a long-term, highly stressful condition, they rewire their brain cells and have a functional deficit in GABA production (10). This is where lifestyle intervention and GABA supplementation strategies done over a period of time, are so helpful in rewiring the brain to produce and use GABA effectively again.
Inadequate or Ineffective Sleep
Lack of quality sleep is a chronic stressor on the body and increases stress hormone production. This causes the same mechanisms as what was described right above. The question is, what came first, was it stress and low GABA and melatonin that caused the poor sleep or was it the poor sleep that caused chronic stress and low GABA and melatonin.
In either case, it is a true vicious cycle where several poor nights of sleep in a row can lead to a rewiring in the brain and a functional deficit in GABA production (11). This is another case where using lifestyle intervention and supplementation strategies over a period of time is so extremely helpful for rewiring the brain to produce and use GABA effectively again.

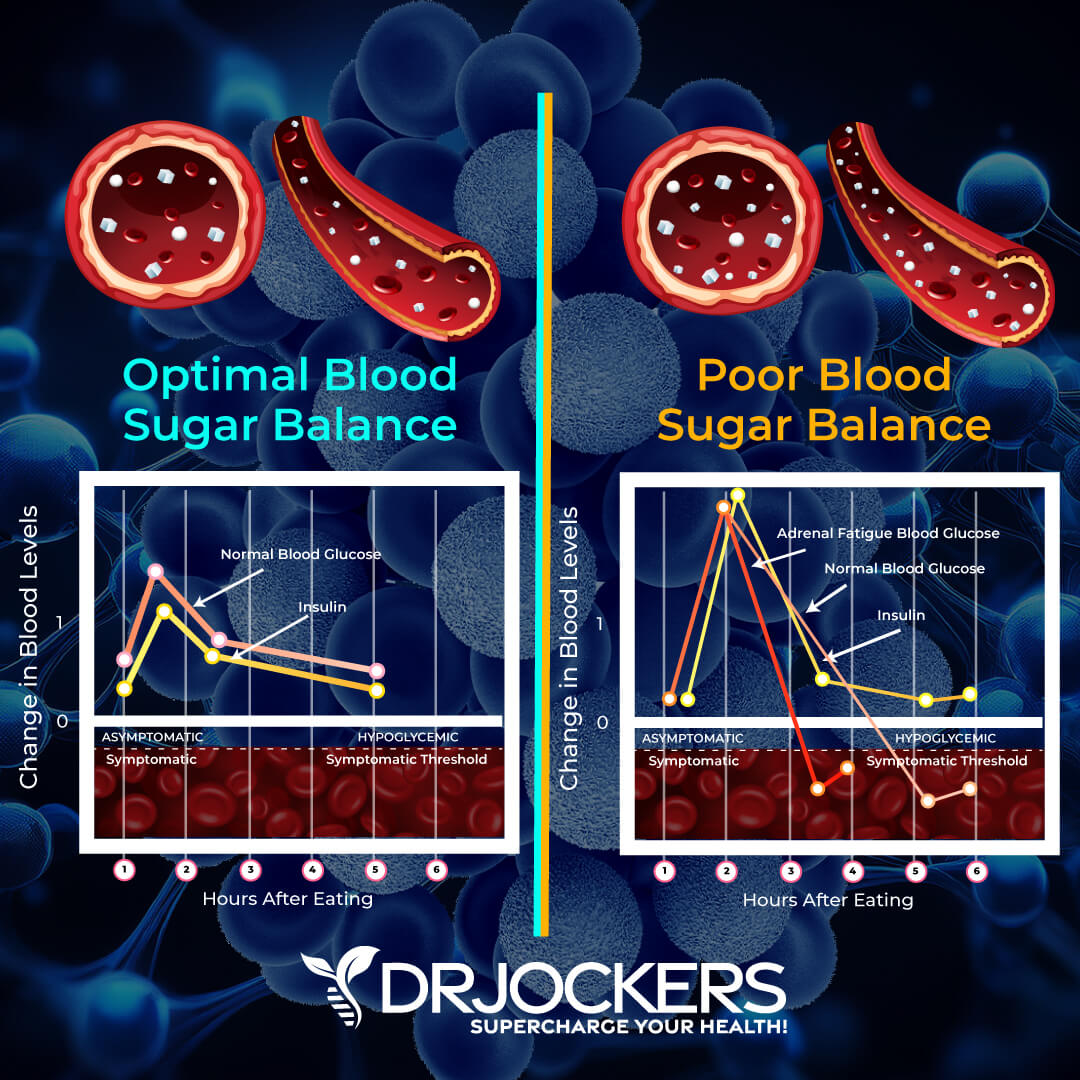
Poor Blood Sugar Stability
Blood sugar dysregulation is a significant stressor in the brain and disrupts the blood brain barrier, which is designed to protect the brain from oxidative stress, infectious microbes, toxic debris and chronic inflammation.
Hypoglycemia or low blood sugar causes a partial starvation of the brain tissue, which increases stress hormones and opens up the BBB for more nutrients to cross over. This also allows more toxins and free radicals to effect brain tissue causing elevated stress hormones and glutamate release.
Additionally, high blood sugar causes insulin resistance in the brain and a functional starvation where there is enough glucose but we cannot get it into the brain to be used. In this case, it leads to opening the BBB and excessive oxidative damage to the brain with elevated stress hormones and glutamate release.
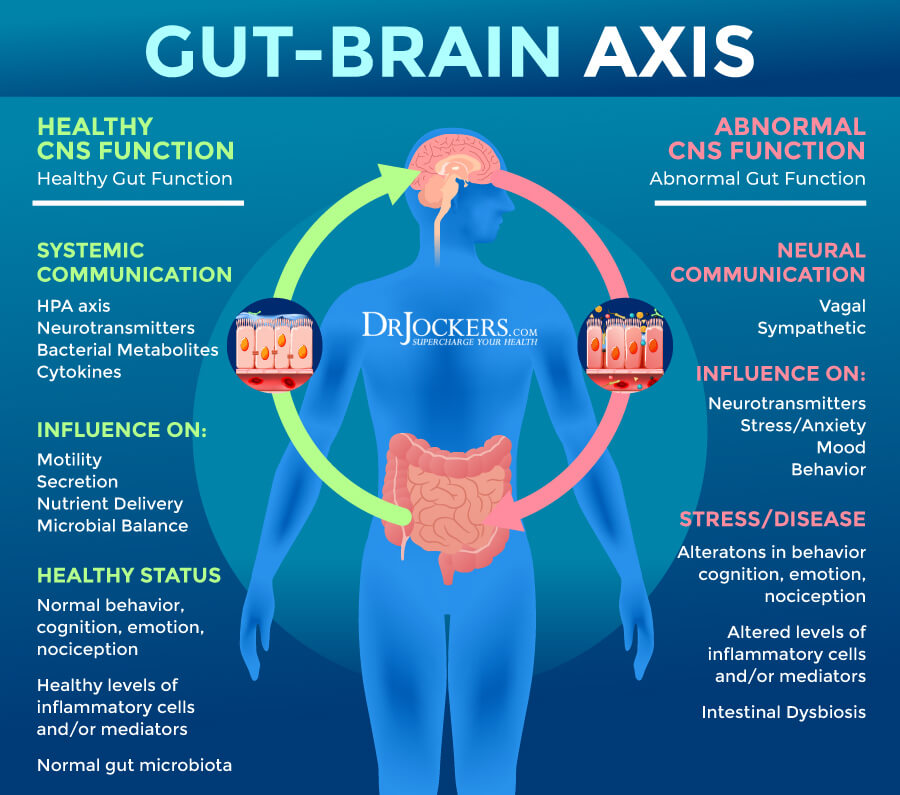
Gut Microbiome Dysbiosis
There is a growing body of research linking the gut microbiome to neurological health. Research has shown that breakdown of the intestinal lining along with low levels of good microbial inhabitants such as lactobacillus and Bifidobacterium are linked with lower GABA levels, increased brain excitability and neurological inflammation (12).
These microbes are essential for B6 absorption and activation, which is the critical cofactor in the conversion from the excitatory neurotransmitter glutamate into GABA. Without adequate activated B6, we end up with glutamate excitotoxicity and increased risk of anxiety, seizures, depression, dementia and Alzheimer’s (13, 14).
GAD Antibodies
In an earlier section we discussed how the body converts glutamine to GABA using the glutamic acid decarboxylase enzyme and the activated form of vitamin B6. Some individuals have elevated antibodies (autoimmunity) to the GAD enzyme. This is especially common in individuals with epilepsy and other seizure disorders (15).
Other research has found this condition in individuals with cerebellar ataxia, stiff man syndrome, type I diabetes, drug-resistant epilepsy, balance problems and more (16). In these cases, following protocols to reduce inflammation and autoimmunity are especially helpful. In addition, these individuals may need large doses of supplemental GABA.

Low Zinc, Vitamin B6, Magnesium, Taurine & Glutamine
The amino acid L-glutamine is the most abundant amino acid in the body, and it is the precursor to GABA production. Glutamine is first converted to glutamic acid or glutamate, which is key for a good attention span, brain energy, learning ability and memory.
This is important but we need an even percentage of the glutamic acid to then be converted into GABA or we risk over exciting our neuronal cells. The next step in converting glutamate to GABA is dependent upon the activated form of vitamin B6 (pyridoxal-5-phosphate P5P).
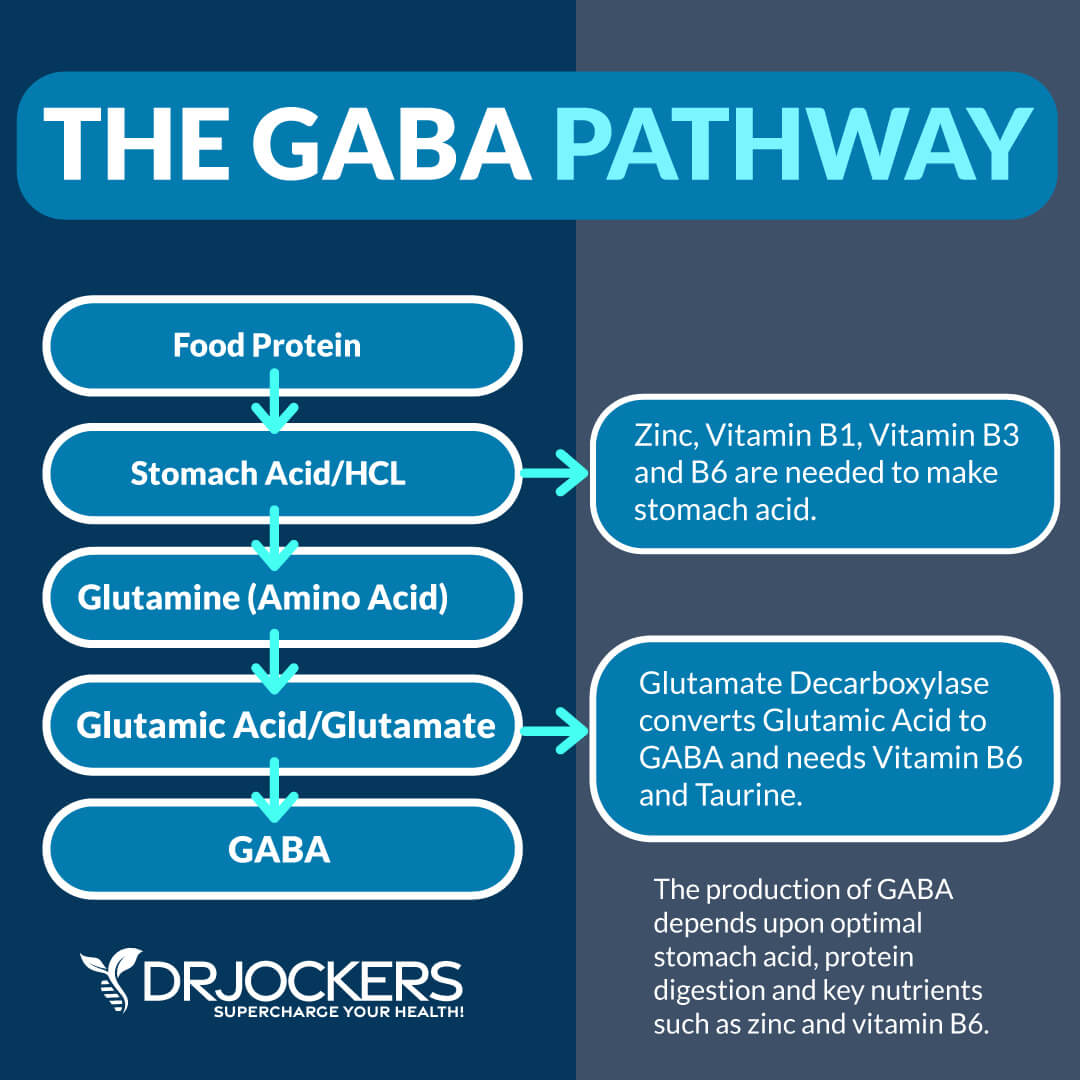
Additionally, the amino acid taurine increases the communication and productivity of P5P and promotes the production of GABA. There are studies that have shown that a deficiency of taurine can result in anxiety (17).
Zinc enhances the release of GABA by working to help activate P5P and stimulate the activity of GAD (18). Both B6 and zinc are also essential to the production and utilization of other neurotransmitters such as serotonin, dopamine, norepinephrine, epinephrine and histamine.
Magnesium is important for binding and activating GABA receptors. Without adequate magnesium, we are unable to effectively activate GABA receptors and utilize it effectively (19). Magnesium deficiency is extremely common with over 80% of women and 70% of men suffering with this and thus supplementation for most will dramatically impact GABA activity.
Testing For GABA Deficiency
The way that I and many functional health practitioners look at GABA levels is through symptom questionnaires and an organic acid test. If a client is demonstrating many of the symptoms listed above that are associated with low GABA than the organic acid test would be warranted.
The organic acid test is a urine test that will look at a biomarker of B6 called pyrodixic. Low levels can indicate that there isn’t enough B6 to successfully convert glutamate to GABA. We may also see very high or very low levels of homovanillic (HVA), which is a dopamine biomarker and vanillymandelic (VMA), a biomarker of adrenaline.
When these are very high it is a sign of heightened stress hormone production which would favor the production of glutamate over GABA. When these levels are very low, it may indicate an overwhelmed hypothalamic-pituitary – adrenal axis. You can find the organic acid test here

Strategies to Raise GABA:
In order for the body to manufacture GABA, there needs to be an abundant amount of the amino acid L-glutamine present. Glutamine is then converted into another amino acid called glutamic acid and then into GABA.
This whole process depends upon the activity of zinc, vitamin B6 and taurine. If we are deficient in these nutrients, we will not be able to produce adequate amounts of GABA.
- Adapt to Stress Better: Chronic stress will deplete your GABA levels. Find things to be grateful for, practice deep breathing, listen to enjoyable music, get regular sun exposure, find ways to laugh and find other stress management strategies to help reduce stress and become more resilient.
- Anti-Inflammatory Diet: Be sure to follow the an anti-inflammatory nutrition plan using real and organic foods in order to provide the right nutrients to support healthy neurotransmitter function. Getting enough quality protein from pasture-raised meats and eggs and wild caught fish as well as healthy fats from extra virgin olive oil, avocados and grass-fed butter is very important. You also want to get enough fiber and polyphenols from colorful fruits and vegetables.
- Sleep Better: It is key for you to prioritize sleep if you are going to improve your GABA levels. It is key for you to prioritize sleep if you are going to improve your dopa levels. Sleep improves neurotransmitter production and receptor activity. When we sleep, our brain flushes out the neurotransmitters, repairs receptor sites and regenerates neurotransmitters to be used the next day. Follow the strategies in this article to help you sleep better.
- Improve the Microbiome: Consume fermented foods, anti-microbial and carminative herbs such as garlic, onions, oregano, basil, thyme, peppermint, ginger, etc. to help improve the overall constitution of the gut microbes.
- Take Epsom Salt Baths with Essential Oils: Epsom salt baths can provide magnesium into the blood stream that acts to relax the body. Adding in essential oils such as valerian, kava, chamomile, lavender, lemon balm and passionflower can be extremely supportive for healthy GABA levels.
- Deep Breathing: Taking time to focus on breathing can be very supportive for GABA levels. Try taking 3 minutes every hour and focus on doing deep breathing with a 5-10 second inhalation and a 5-10 second exhalation. Read this article for more info on breathing properly.
- Regular Exercise: Regular movement is good for all neurotransmitters. Individuals with low GABA should be doing low-intensity movement such as walking and doing lots of deep breathing. Practicing yoga can be extremely supportive of GABA levels.

Best Foods to Boost GABA Levels:
Healthy microbes such as lactobacillus strains produce GABA naturally as a byproduct of metabolizing the amino acids L-glutamine and glutamic acid. Fermented foods that are rich in these lactobacillus microbes are rich in GABA. They are truly the only dietary source of GABA. You may see other lists online, but those are foods that are richer in
- Sauerkraut
- Kimchii
- Grass-fed cow or goat kefir or yogurt
- Coconut Water Kefir
- Beet Kvass
- Coconut milk yogurt
- Kombucha
- Pickles
- Pickled Ginger
- Miso, Natto or Tempeh

Supplements to Raise GABA Levels:
Magnesium: Supplemental magnesium helps to raise GABA levels. By far, the most effective form for this is called Magnesium L-threonate. I recommend doing 1-2 grams – 1-2 times daily.
B Complex: B6 deficiencies can cause low levels of GABA. I will typically recommend a full B complex supplement with activated forms of B vitamins to maintain.
Probiotics: In particular, supplementing with probiotics that contain a variety of lactobacillus and Bifidobacterium strains help to raise up GABA levels. I recommend taking 30-100 billion CFU’s daily.
GABA: Taking supplemental GABA can be very effective. It is thought to be too large to cross the blood brain barrier, however, most people with low levels have a disrupted BBB and respond very well to supplemental GABA. I recommend doing 100-200 mg 1-2x daily.

L-Glutamine: Supplementing with L-glutamine can be very effective for supporting GABA levels. I recommend starting with 4-5 grams to see how your body is tolerating it and gradually going up to 10-12 grams.
If you notice an increase in irritability, headaches or anxiety, you may be deficient in B6 and/or zinc. Try adding those in while reducing L-glutamine levels for a while and then try L-glutamine again.
Taurine: This is an amino acid precursor to GABA and has a similar structure but is smaller. In the brain, it helps to activate GABA receptors. I use 300-600mg, 1-2 times daily.
L-Theanine: is a naturally occurring, biologically active, free-form amino acid that provides relaxation support. L-theanine improves GABA production and induces a state of relaxation of the mind without inducing drowsiness. I recommend 50-100 mg, 1-2 times daily.
Valerian, Kava, Chamomile, Lavender, Lemon Balm & PassionFlower: These herbs help to improve GABA production and utilization in the brain. You can drink herbal teas with these or use the essential oils on your body, in an Epsom Salt bath and in a diffuser so you can breathe in these supportive compounds.

Dr Jockers Strategy:
I follow a number of the strategies, including healing the gut, balancing blood sugar and reducing stress. My main supplements I use to improve GABA levels are Brain Calm magnesium and Mood protect. Yes, you can take these both together without any problems.
Brain Calm Magnesium: This is a specific form of magnesium is the only form of magnesium proven in animal studies to cross the blood-brain barrier. Boosting the brain’s magnesium level is vital to healthy cognition, which includes long- and short-term memory, learning, stress management and sleep.
Normal Dosage: 1 scoop – 1x daily Advanced Dosage: 2 scoop – 2-3x daily
Mood Protect: Combination of herbs, nutrients and compounds that promote serotonin and GABA production to ease anxiety and improve overall mood and sleep. This product has clinical dosages of GABA, taurine, L-theanine and 5-HTP. This also contains small amounts of zinc, B6 and magnesium to improve natural GABA production.
Normal Dosage: Take 1 cap – 2 times daily (away from meals)
Advanced Dosage: Take 2 caps – 2 times daily (away from meals)
GABA Calm:
The GABA Calm is an easy to use chewable form of GABA to help calm the brain and the body. This product is very good for helping to reduce tension, irritability and anxious thoughts and to improve sleep quality. It acts quickly and effectively to calm the nervous system.
The quick release of GABA helps to create an optimal balance between the “excitatory” neurotransmitter glutamine and the calming effects of GABA. While GABA is naturally synthesized from glutamate, some people may benefit from supplemental amounts to oppose “fight or flight” feelings.
Many of our clients and followers prefer this fast acting GABA for moments when they feel more anxiety, tension or trouble focusing. Others notice that it improves their sleep. This is also a great form for young children dealing with anxiety and sleep problems because it is a chewable form and doesn’t require swallowing a pill. You can try this out here
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!
Sources For This Article Include:








I’m recovering from a shingles that went to my arm that has lymphodema . I have had cancer, chemo, mastectomy , that took 12 lymph modes. Also had 26!rpunfs of radiation and then had to have total knee replacement . All of this in 1 1/2 years and now this. The pain in my arm and the lose of being able to use it has been unreal for me. I have been taking GABA , the supplement for 2 years my doctor just prescribed the prescription. I take magnisium. B complex , a probiotic. I have been off work 6 weeks and going to therapy, but get really down because it’s hard to do things , I pray that the burning pain will stop!
We are praying for you too Sally!!
Excellent article – thanks! Recovering from Restless Leg Syndrome (iron supplementation has reduced severe symptoms to zero), but insomnia remains. Magnesium – in EVERY form is excitable to me – even taking it in the AM. Mostly when I awake at 3AM – taking an ibuprofen (a glutamate blocker) let’s me fall asleep ’till 6AM or so. I take a lot of anti-inflammation supplements and B-vitamin daily, probiotics, fiber and fermented veggies also daily. Can’t figure it out!
So sorry to hear about this Richard! Could be a glutamate conversion issue, a ketogenic diet may be helpful. You may also benefit from getting some functional lab work done to see what is really going on. You can email michael@drjockers.com if you are wanting to work with someone on this!
Some people have the GAD gene problem which keeps them from converting Glutamate to GABA. You can do genetic testing. Its very common in people of Russian ancestry. One of the reasons they drink alot of alcohol, I read. Magnesium Glycinate is excitable for me because I am one of the people that glycine is excitable for while in most it is calming. I take liquid magnesium called REMAG and it works well for me. I take a supplement called GAD Enhancer on Amazon and its for people that have the GAD gene problem. I have also had high cortisol at night issues that woke me up everynight. I take Seriphos which trains your HPA axis to stop making cortisol at night when it should be low.
Thanks so much for sharing this!
Hi, my Formiminoglutamate levels tested high (OAT test) and they recommended Folate so that it can convert to glutamate. If I’m taking glutamine and don’t have enough Folate, is that why my Formiminoglutamate levels are high? Am I not going to make much Gaba until I take Folate? I don’t have MTHFR. I was previously taking 5g of Glutamine fo a couple of months before taking the OAT test. I stopped taking it several weeks ago for another reason. Glutamine does seem to have a bit of a calming feeling when I take it but maybe it’s just helping my gut that has issues. Oh and I might have one GAD SNP. Thank you for any insight.
Hey Michael, it is more likely that you are just not converting histidine to glutamic acid effectively, which is a sign of folate deficiency.
I have a question about overstimulation. Can it be that glutamine protects the brain from the cause of a burn-out? My doctor says that glutamine has not an direct effect to stabilize overstimulation. The glutamine has only the relaxing side-effect. Thank you in advance!
Hey Michael, it is actually GABA that has this protective effect as too much glutamate can become harmful to the brain. A very stressed person can still convert excess glutamine into glutamate, the key is to support the conversion of glutamate into GABA using magnesium and B vitamins.
Hi
I have Stiff Person Syndrome and this is the best article I have read regarding GABA and GAD. I have even used a very similar way to describe it to others as this article does using a car as an example. I find stress counterproductive to what I do take for this condition. I also have ivig every 8 weeks.
Are there any supplements that I could take to increase GABA, decrease anti GAD antibodies and help me sleep?
I forgot to mention that I get serotonin syndrome so I cannot take SSRI. Would 5-HTP increase serotonin to harmful levels?
I believe genetics also factor in. I have 3 mutations on GAD1 which all reduce my production of the enzyme. I have a very active mind and when under prolonged stress a tendency towards anxiety and panic attacks.
I noticed the foods you recommend are also generally high histamine and are the same foods I am drawn to. I wonder if there is some connection between histamine and GABA. My craving for high histamine foods perhaps means compensating for low GABA with Histamine?
It is interesting to note that GABA is also produced in the Pancreas and has some relationship to blood glucose levels, insulin, and glucagon altho this is not yet well understood. I have had occasional low blood sugar.
I’ve just started trying GABA and I get a bit of a rush feeling from it for a few minutes. I tried 1500 mg and have just started doing that daily. I went from feeling like I was dragging around, unmotivated, low energy and focus to feeling wonderful, high energy, and motivated practically overnight (including a great night’s sleep). I have been doing a low carb diet as well but recently started have some cravings for carbs – and the GABA just entirely stopped that too. I notice the higher mood lasts maybe a hour or so but the general well being lasts longer.
I have tried the precursors in the past without much luck probably as I don’t make enough of the enzyme to utilize them and I do find that glutamine supplementation is helpful.
I was thinking to try spreading out over the course of a day in smaller doses and also start to reduce slowly from 1500mg until I find a good balance point. While the 1500mg did pull me out of the funk it also changed my sleep cycle. I tend to stay up late, too late, and not feel like going to bed. Now, day 2 of GABA and it is early evening and I’m yawning!
Interesting thoughts, thanks for sharing Terry!
Dear Dr.
I am a man 49 years old. 63kgs.
Suffering from GERD for two years everyday. Not severe but several times a day.
Anxiety, to worry about things too much, etc. increases it. Relaxing, walking and similar syntoms reliefs. Many times difficulties to work concentrated as I am always reevaluating my status regarding GERD.
I have been taken benzos (not now) and it reliefs. Acid inhibitors do not help.
Gaba resulted for some weeks but the problem appeared again.
All kind of herbs also tried. Valerian root has good effect strenghing esopagous esfinter and it makes good for me.
Mg and B vitamins no effect. Theanine no effect. Zn carnosine no effect. Probiotics no effect. Diet no effect. Endoscopy was ok. Blood tests for gluten intolerance were ok. White tongue in the morning and during the day.
My question: is glutamine a good option to try? What about taurine? Sorry for my bad English (from Spain)
Here’s some recommendations that you can try Pedro! https://drjockershdg.wpengine.com/beat-acid-reflux-naturally/
Dear Dr Jockers, thank you for the great article. What do you know about gene mutations affecting levels of GABA? From my 23 and Me results I came to find out that 7 of the 10 SNP’s tested are homozygous. I have always suffered from anxiety and never knew why, now I have an idea why. I know epigenetics play an important role in health but are these polymorphisms too much for my body to handle?
Thanks for your work
Hey Paul, that is a good question. I would not consider myself an expert on genetic SNP’s but following the strategies in this article should be beneficial!
Hello Dr. Jockers,
I do gaba receptors and producing gaba go hand and hand?
I am worried i fried my gaba receptors using Benzo’s, and i need a way to repair my brain to its old functionality which was completely fine. Now i have regular anxiety and a sense of worry hanging over me at most times during the day. I understand the brain is capable of repairing it self, however i am worried as this has gone on for around 3 months following the benzo use. some weeks where my stress and anxiety are very high and other weeks where they are practically non existant.
Please get back to me soon as i am very stressed about the current situation.
Hey RA, following the strategies in this article should help restore both production and receptor sensitivity with time. Sorry to hear about these long lasting effects of your medication!
GABA is extremely overrated and I think researchers have it completely backwards in a couple of phenomena. Excitation and inhibition in the brain are rarely global, unless it involves consciousness itself, and the numbing effect of GABA is one that “traps” one, more than just a “relaxing” one, and can increase motor activity in other parts of the brain I have found.
I have Akathisia and GABA is known to me by my layman’s research of possible ways of treatment, and I have also tried it again and again (and felt it clearly), and contrary to an inhibition of involuntary movement it has exactly an opposite effect to motor activity and beyond that a kind of psychological “compulsiveness”, where one can’t easily change one’s current activity, resulting from that “trapping” numbness. The “numbing” is also known from, and might be related to, other treatments by SSRIs.
The funny thing is, equating “inhibiting” with relaxing here is where “researchers” fall into a naive trap of false similarity, and perhaps arrogant condescension towards patients’ symptoms (in the case of neurologists mostly self-cause..). Akathisia is a prime example of showing that not all effects on the brain, perhaps most famously “relaxing”, are global or affect all areas or layers. Sure you can make one sleepy, but you won’t treat the “root” cause, won’t even touch it. (Also known in such simple things as breathing etc.)
And there is a mechanism behind it too: apparently GABA increases acetylcholine in the striatum, which is known to cause motor-over-excitation (!) and exactly what causes akathisia (and diverse Parkinson-likes) in the first place.
Damage to the opposing “excitatory” Glutamatate receptors on the other hand is believed to be a reason for many side-effects from taking SSRIs. And also from drinking alcohol by the way (!), because it is a GABA-analog. I haven’t tried anything to assist or “repair” the Glutamate receptors yet, if it would even work, but I bet GABA is if anything the false path to follow, and I bet researchers in many cases have it completely backwards because of a naive similarity which doesn’t apply to how the brain works at all.
And again, I have tried GABA repeatedly, and it doesn’t affect the relevant areas at all, but only seems to make them worse, and generally causes a kind of “entrapment” in the head and brain fog.
Sorry to hear about your struggles!! Very interesting comment…thank you!!
It is because GABA supplement worsen glutamate.
GABA itself can be converted back into glutamine, which is then converted back into glutamate through a metabolic pathway called the GABA shunt. So GABA supplementation can end up increasing glutamate in some people as well.
read the whole thing here.
https://www.holistichelp.net/blog/how-to-increase-gaba-and-balance-glutamate/
ketogenic diet could help you. I suffere from internal akathisia and keto diet keeps it at bay. Also google BCP 157 peptide. It regenerates intestines, nerves, joint, brain and more./
I suspect those that convert GABA strongly to Glutamate may have the GAD polymorphism. Thoughts?
Yes that can be the case with some individuals.
Thank you. We run the Alternative to Meds Center, a holistic residential psychiatric medication withdrawal center licensed by the state of AZ. I am a DC and have a post-doctoral certificate in environmental medicine. Plus I have 50 staff including therapists, psychiatrists, naturopaths, and a cacophony of holistic modalities.
Thank you for all of your work and information. http://www.alternativetomeds.com
Great to hear this Lyle! Thank you for all you do!
Akathisia is an extrapyramidal symptom associated with certain types of psych meds. Artane or trihexyphenidyl hydrochloride is a medication for akathisia. When you reach a certain age (60 or 65?), some doctors might not want to prescribe it or you might need special authorization. I am just a lay person but I wanted to share this option if your interested. If I recall correctly, akathisia has to do, in part, with the inverse relationship between dopamine and acetylcholine. Medication that reduces overactive? dopamine(DRBA or dopamine receptor blocking agent) results in an increase in acetylcholine which contributes to akathisia along with GABA, Norepinephrine, etc.
Thank you for your very informative article.
I am one of a very rare group of people… those who have suffered from metronidazole (Flaygl) toxicity. On very rare occasions Flagyl or it’s metabolites cross the blood brain barrier resulting in neuro-toxicity, leading to such symptoms as peripheral neuropathy, headaches, extreme fatigue, gastro intestinal issues, depression, anxiety, heart palpitations, muscle wasting, etc. I have read that Flagyl and/or it’s metabolites mimic thiamine, and disrupt the GABA system. Many who have suffered from metronidazole toxicity have seen dramatics improvements with the use of thiamine and magnesium suppliments. However, those with muscle wasting have not seen improvements. Do you have any experience treating toxicity caused by medications? And would you recommend that a person suffering from muscle wasting take an L glutamine suppliment?
I would recommend working with a functional nutrition practitioner to see where your hormones, gut health, etc are at then your body can be supported to heal itself!
A very thorough and well researched article thanks so much Dr. Jocker.
Quick question if you don’t mind. I have lyme disease which somehow is the root cause of my nerves to flare up all over my body. It’s quite unbearable and flares throughout the day. Gabapentin calms it down but doesn’t eliminate it telling me that maybe lyme is messing somehow with Gaba production.
When I take antibiotics (been on them for years) my nerves get worse and really bad a few days after. My theory is could it be that the antibiotics are killing off the good gut flora which produce GABA and lowering my levels causing more severe nerve pain?
Second what would you suggest is the top few things to take to improve GABA levels?
Thanks!
There are probably a number of contributing factors here Richard. The top strategies you could use are all listed above!
roughly how long does it take to rewire the brain to produce and use gaba efficiently again
I would say 6 weeks to 90 days or so!
I am an adult with ADD. I have struggled with sleep deprivation for many years. Melatonin does not work. I do everything that is suggested by physicians to sleep, that doesnt do much. If i dont take anything , i just lay awake thinking about things, i cannot shut my mind off. Lunesta and Benedryl help me but i dont want to take anything that is not natural anymore. I started taking Mood Protect 7 months ago before bed. It does help me sleep but never a deep sleep , therefore i never feel rested and my memory and emotions suffer for it. Any suggestions ?
Sorry to hear that Jennie! I would consider turning off the WiFi in your home and following the recommendations in this article here: https://drjockershdg.wpengine.com/7-lifestyle-strategies-better-sleep/
I haven’t read the article in sleep, but I thought I’d interject here just Incase the doctor didn’t cover it, you might also consider having your sex hormone levels checked. Low estrogen, progesterone, and testosterone (even in women) can have a huge effect on sleep. The book The Period Repair Manual has a lot of good info for women on improving sleep. Good luck!
Thanks for the input Melissa!
Good article.
I was curious about how you mentioned low blood sugar (or high – insulin resistant) impacts on the blood brain barrier – as below. This is confusing when it comes to intermittent fasting to 1 meal per day in the early evening and inducing ketones which are healthy for the brain? Reading below, it would be easy to assume that intermittent fasting would do the below and not be healthy?
Thanks.
“Hypoglycemia or low blood sugar causes a partial starvation of the brain tissue, which increases stress hormones and opens up the BBB for more nutrients to cross over. This also allows more toxins and free radicals to effect brain tissue causing elevated stress hormones and glutamate release”
Yes you have to gently force the keto adaptation process with IF. Here is a helpful article: https://drjockershdg.wpengine.com/best-intermittent-fasting-strategies/
Thanks, got it.
Fabulous article.
Does GABA supplementation, over time, assist the brain produce and utilise GABA more efficiently to the point that supplementation may be discontinued? Or will deficient people likely have to supplement with GABA on an ongoing basis?
I say this as I’ve recently started GABA supplementation and am noticing a world of difference, but I do hope to be able to discontinue supplementation eventually.
I’m taking 3x 750mg per day and am having fantastic results thus far.
Yes by taking stress off of the body and helping you function it will help you optimize your neurotransmitters. Some people, as long as they follow healthy lifestyle principles can keep things under control without the supplement, but I have found that most people who have struggled with low GABA in their life, enjoy being able to use the supplement ongoing but in lower dosages.
Thanks so much for your insight Dr. Jockers, it is truly appreciated!
In your experience, how long does it take to correct a deficiency? I’m sure the answer depends on multitudes of variables, but is there a general ‘rule of thumb’ that’s applicable here?
3-6 months and up to 2 years
Hi,
What dosage do You recommend during this timeframe?
Thank You,
Regards,
Johan
Yes experiment and find what will work best for you. Blessings!
Dear Dr Jockers.
Great article, thanks!
I recover from benzodiazepine use and off this “poison” for 3 months.
Mg-Threonate had disappointing effect. Can I conclude that the GABA receptors in brain is thus repaired and the problem is more in gut where GABA is produced? Also some days I feel 100% and others times heavy brain fog (probably some sort of panic attack symptom). Surely the receptors cannot be ok one day and damaged the next day.
Would you recommend Mg Peroxide to speed up gut recovery (increased oxygen in gut)? I understand that some gut bacteria does not like high oxygen levels. Will Mg Peroxide damage these flora?
Any other advice to speed up recovery will be highly appreciated!
Kind regards
So sorry to hear that! I would recommend following the recommendations in the article Levett!
Do you find a tolerance to gaba over time making it difficult to wean off?
Does body become resistant to gaba supplement over time resulting in increased dose for similar effect?
No, that isn’t what happens. It is a non-addictive supplement. As long as you address the root cause issues of why you need more GABA, you won’t need to increase the dosage over time.
What would case a depletion?
Whoops, my bad. I didn’t see the first part of the article when I scrolled up at first.
Good article.. I have been dealing with IBS for the past 30 years,that initially started off as ibs-d, followed by gerd, and then primarily ibs-c, with food triggers causing gas/bloating/burping. I was also a smoker during this time and it was helping my IBS (motility). Two years ago, I quit smoking, which worsened my IBS and caused sleep anxiety, for which I had low dose mirtazapine (7.5 for 6 months and 3.75 for 1year) which helped me fall asleep and ease my ibs symptoms at night. Going off gluten, sugar and black beans not only helped my IBS, but also my anxiety. It’s been a month since I stopped mirtazapine, and diaphragmatic breathing has been truly transformative in reducing my ibs symptoms. However, my sleep patterns have been disrupted, and anxiety is intermittent, and gets worse if I haven’t slept well. I am still getting about 5 hours of sleep, and waking up consistently at 5:30am with an urge for a bowel movement.
I have never been diagnosed with general anxiety until I quit smoking 2 years back, although I have had sleep anxiety when suffering from jet lag since a panic attack 10 years ago. I do have a tendency to ruminate and procastinate.
From my research, it appears that we could look at my illness from a neurological/emotional or a GI perspective. I have been working on improving my vagal tone (which is definitely helping my IBS), along with a nutrient rich diet and exercise, but the sleep onset anxiety is my top issue, and I was wondering if there could be sibo / bacteria that depletes gaba causing my nighttime anxiety or if retraining my brain for better sleep would be a logical next step, and what other tests would help narrow down the issue. At this time, I am only taking Vit D and B supplements along with dietary probiotics.
Yes gut issues are very commonly the underlying cause in neurotransmitter issues!
Thank you Dr. Jockers for this information ! Sadly, I wish I could understand it all. I received an update on one of my genetic testing sites that determined I have a lower glutamate system, dopamine system, and serotonin system as well.
First I heard of this. And now I am desiring to look into this – I don’t take chances.
Is there a definitive test that can be done that shows a problem for me – or none – which would be better! I worry for I am apoe3/apoe4 and I want to keep healthy.
Thank you again. 🙂
Very interesting, keep us updated. Be Blessed!
Thanks for this wonderful article. I’ve also watched your videos. I have been off Ativan of which i used daily for 5 years then again for 2 years, small dosage. I’ve been off for 11 months. I have every symptom of low gaba including an intense sensory hypersensitivity. Is it true that gaba can be permanently doenregulated? Meaning I will be in this state of extreme anxiety and sensory overload forever? I was diagnosed with generalized anxiety disorder years ago, hence why I was taking Ativan. With your supplements and diet recommend is there a chance for the gaba to upregulate? Please help! Can it honestly take this long for them to upregualate?
Hi Holly, Supplement and lifestyle changes can certainly increase GABA production. I always recommend that you should seek advice from a functional health practitioner to customize a specific plan for you. Here is a helpful article: https://drjockershdg.wpengine.com/functional-nutrition-tips-to-find-a-great-health-coach/. I also suggest reading this article for more information: https://drjockershdg.wpengine.com/magnesium-stress-anxiety/
hi there!
I was in heavy alcohol abuse and with weed too, for like 7-8 years. In 2012, I stopped drinking cold turkey and weed too. just like that and have been sober for 6 years now, I still have same serious problem with my brain, took me long time to find answers about my long suffering condition that i am in, the voices in my mind going on nonstop for 6 years. I want it gone, I was addicted to caffeine after that and right now i stopped, and used very little bit of it now. So, GABA doesnt accross the BBB, I tried theanine and it doesnt work, I found out that it just a severe anxiety that make brain become so loud, alcohol is like a brake, i was off alcohol and have been on gas since, im trying to calm down the brain, i just started working out, I need your support statement that make more confirmation about my condition to rule out and what to do about it? your product? does it work? how the science rule out that of whats real nutrition in microscopic level? how they can identify it and help us? there are many deceivers out there.
Hey Nathan, It sounds like you have taken the first steps to break your addictions. I would never rule out nutrition as a major importance in your life! I would recommend working with a functional health practitioner that will get to the root cause of your addictions and help customize a plan for you. Both of these articles to follow offer more information in navigating your health journey. I will be praying for you. https://drjockershdg.wpengine.com/addiction-causes-natural-treatments/ & https://drjockershdg.wpengine.com/functional-nutrition-tips-to-find-a-great-health-coach/
well it seems you have tried everything except hydrogen water and asking God for help 😉
thank you, lets get to the point, lets focus on trying to calm my brain down, not about my addictions, example, going to psych isnt going to help, the natural remedy is, exercise will increase gaba to slow down my brain and ease my anxiety, and its something about my eating habits too of carbs, sugar, and i found this keto is much help, anything else? I suffered so much for long time, trying to find solutions to make the voices to go away.
thank you 🙂
Nathan,
I am seeing this post many years later. But in case you ever come back to this, or if any one else is reading this that could be helped, I thought I would reply. My heart goes out to you. Congrats on breaking some very difficult addictions. That is a huge win !
I have several friends and family with schizophrenia, and I have done quite a bit of reading on the subject to try to help them. The voices that bother you could be related to schizophrenia which can be triggered by heavy marijuana use. It also can strike out of the blue, men in their late teens and early twenties and women in their thirties due to a combination of genetics and lifestyle factors and trauma.
I have a friend with marijuana induced schizophrenia. Abilify (Rx) along with diet and lifestyle changes has helped him tremendously. He has tried numerous times to wean off the Abilify but it just leads to manic episodes every single time. William Walsh Phd has written a book called Nutrient Power which looks at nutrition and meds, combining whatever works best. He has found that both meds and certain supplements are needed in most cases. Rarely has he found that someone can go completely off meds, but they can usually taper them down to just one from three or more and lower the dosages.
Abraham Hoffer has written many books advocating for high dose niacin and vit c therapy with amazing results. Schizophrenia symptoms mimic those of pellagra, which is a severe vit b3, ie niacin, deficiency. Dr Hoffer was able to get many people off their meds completely with his protocol, but they had to take the niacin and vit c permanently or else they would relapse. I have unfortunately seen this relapse in another friend of mine.
My other readings have suggested that vit d, b vitamins, vit c, vit e, magnesium, zinc, selenium, and iodine can all be very helpful. I would also think that liver support like milk thistle, dandelion root, and bitters would also be helpful. And I would not rule out past and current exposure to mold or candida while looking at contributing factors and activated charcoal can help with flushing mycotoxins out of the gut.
Dr Jockers has a plethora of great information that I think would be helpful to try. Brain health and health in general is all about reducing inflammation from the root source, and giving your body the adequate nutrients it needs to heal itself. Inflammation can be caused by parasites, toxins, illness, nutrient deficiencies, allergies, diet, lifestyle, genetic polymorphisms. etc. We all have to be patient detectives to piece together the puzzle of what needs attention and seek wisdom from those who have dealt with similar issues successfully. I hope you find a great source of information, hope and comfort. Ask, Knock, Seek and go to God about it first and foremost.
There is healing power in prayer and reading God’s scriptures. and in speaking God’s promises of healing over one another and reminding ourselves and one another of the health and healing that God wants for us. We are all Mind, Body and Spirit. They are all interconnected. We need to address health from all angles and not neglect one at expense of another. Also, no matter what your situation, look at forgiveness as a huge puzzle piece; choose forgiveness for others and for yourself. You might be surprised at the miracles that can happen when you make a conscious intention to give that gift of forgiveness to yourself and others.
I hope this was helpful and I wish you success and blessings in your journey.
Hello; my livewellO report had all red flags on my GAD snps, about 5 of them. I have been stiff and sore for 30 years, migraines, chronic pain,no sleep to speak of for my entire life-64 years- and have had a number of the signs of low gaba. I’m thinking perhaps my body doesn’t even make it at all, does this make sense? I can’t make antibodies to gad if my gads are mutations, can I? Great article!
Hi Dr. Jockers! Thank you for the informative and insightful article on GABA! I’ve been taking 500mgs of GABA and it’s helped me tremendously but I noticed because of my poor sleep, (I sleep at around 4am-5am every day), I am probably not very receptive. I am using this as motivation to sleep better.
Can I ask a question? I hope this doesn’t sound stupid but does GABA supplements affect bowel movement? Does it make your stool hard or difficult to pass through? I am experiencing this lately and thinking if the GABA supplements I’m taking have to do with it.
Also, I see that you mentioned that Magnesium L-threonate is best. However, the magnesium I have is Triple Magnesium Complex containing Magnesium Oxide, Aspartate and Citrate. What do you think of this combination?
Hey Therese, I recommend reading this article! It goes into detail about the best forms of magnesium. Blessings!
Hey Therese, that form of magnesium is going to be more well suited for reducing muscle cramps and stimulating bowel movements. However, that is not a good form to reduce stress on the brain and support GABA. For that, you will want the Brain Calm Magnesium https://store.drjockershdg.wpengine.com/products/brain-calm-magnesium
Hi Dr. Jockers! Thank you for the information!
I bought L-tryptophan because I read that it aids in the production of serotonin. But I read in web md that it can cause death and now I feel queasy. When is it safe to take l-tryptophan? I’m thinking about just limiting my usage to when I’m extremely anxious and not daily. And how does it also aid in the production of GABA? Thank you very much.
Hey Therese, Every individual is different in how they respond to supplements. It is always best to work with a qualified health practitioner.
Isn’t it better to specifically see a gab in an amino acid test? And why give glutamine, which is the most abundant amino acid and can rarely be deficient but over-stimulating?
GABA
The amino acid tests are not reliable as it is looking at urinary neurotransmitters and not brain based neurotransmitters. Looking at a collection of symptoms is more reliable and doing a trial with GABA to see if it improves is good. The research on health improvements with L-glutamine supplementation is robust and most people respond very well to it!
What is the recommended dosage for the Mood Protect and Brain Calm Magnesium supplements for a 30 lb 5yo girl with epilepsy (absence seizures), who is currently taking Ethosuximide? And can these capsules be opened and added to juice or food? My daughter can’t swallow pills. Do you have any other recommendations?
Hello Stephanie, although we are unable to give medical advice, I would recommend just doing the basic dosage. Take 1/2 scoop of the Brain Calm in water 1-2x daily. You can do 1/2 cap of Mood Protect in water or juice – 2x daily.
Thanks Doc!
I would like to add fermented foods to my diet. However, based on past experience, fermented foods tend to make me more migraine sensitive. What do you recommend to reduce the sensitivity to fermented foods?
Yes it sounds like you have histamine issues. Here is a helpful article on what to do: https://drjockershdg.wpengine.com/suffering-histamine-intolerance/
Hi,
If you take a gaba/taurine supplement is their a chance it could increase glutumate through the gaba shunt pathway? I read this somewhere and even though I have low gaba I expect I also have high levels as glutumate as well.
I haven’t seen this happen before but it is important to have zinc, magnesium and B6 on board to help with overall glutamine-GABA conversion.
Can you build a tolerance to gaba/taurine supplements resulting in higher dosage overtime? Can you teach your brain to create more gaba if you supplement long enough resulting in you not needing to supplement anymore?
Thanks
That is a good question Chris and we haven’t seen evidence to indicate a habituation to GABA and the need for higher dosages.
Hello!
Will taking a taurine or gaba supplement immediately have effects on your brain to produce more gaba and raise levels of gaba in your brain within an hour of taking the supplement? I am also curious about the question above me as well!
Hey Jenifer, yes taurine can help in the process of making GABA. Taking straight GABA doesn’t help you make it but it does provide the near immediate calming effect and by creating more balance and calmness in your brain, you get out of the vicious cycle of neuroexcitation and that helps you have more balance in the brain.
Will taking any supplement to increase gaba in the brain such as taurine increase gaba but decrease gaba receptor sites in the brain for the long term because the brain no longer needs the gaba receptor sites because it has so much gaba? so when you stop supplementing you will even have lower gaba levels because of lack of gaba receptor sites.
While we don’t have evidence for this, it is possible from a mechanistic stand point if you are hitting it with very high dosages such as 800+mg daily. Lower dosages such as 100-200 mg – 2x daily should have a calming and balancing impact and improve your sensitivity levels.
I saw online someone was taking 2 grams of taurine a day. Do you think that will lead to down regulation of the gaba receptors over the long term? They said it significantly helped them though, any possibility that could teach the brain to create more gaba even after you stop supplementing?
It is possible. That seems high but we don’t have research or clinical examples to demonstrate it would cause long-term problems.
If I take 1 g of taurine a day for months then after I stop supplementing will my brain have learned to create more gaba on its own? Does taurine significantly raise gaba as well? Will I feel relaxed within an hour after taking taurine? I know there are a few gaba receptors but will it affect all gaba receptors or only certain ones? I should also supplement magnesium zinc and B6 to help the overall conversion of gaba any suggested dosage?
Yes that is correct. As you calm your brain, you allow your brain to work more effectively. Of course, you have to address the root cause factors such as mold exposure, poor diet, chronic stress, EMF exposure, infections, etc. You may always feel better with taurine and GABA. I would recommend at least 200-300 mg of magnesium – 2-3x daily. Take 20-30 mg of zinc – 2x daily with meals and take 50mg of P-5-P form of B6 daily.
Do you think it would be okay if I got magnesium, zinc and b6 from foods such as avocadoes and salmon instead of supplements before supplementing taurine?
You can try it and see how you feel!
I have genetic polymorphisms that lead to high glutamate, low GABA. I take 600mg NAC once a day, 15mg zinc once a day, and topical magnesium once a day. I also eat a nutrient dense diet that occasionally includes oysters, beef liver, eggs, avocados, sunflower seeds, pepitas and other foods with zinc and B6. How can I gauge if that’s adequate to raise GABA levels?
It is going to be based on how you feel. If you have adequate GABA, you will feel calm, relaxed, focused during the day and be able to sleep well at night.
I suffer from acute anxiety attacks every 3 months (only and always) in my luteal phase.
They almost exclusively occur at night and I have 5-7x per night for 7-10 days.
It’s excruciating. No one can figure it out other than telling me my cortisol is high.
Have you ever heard of anything like this or know what might be triggering this to happen so weirdly cyclically?
Thank you.
Sorry to hear that! I would recommend trying out some GABA to see if it improves.
I have, after 35 years of struggling with gut issues, been diagnosed with dysbiosis. I have/had zero lactobacillus and have more bad bacteria than good. I’ve been strict no sugar, low carb and gluten free diet for 8-9 years as I became chronically hypoglycemic and preventing insulin from being triggered was the only way to manage it. The immunologist the diagnosed me added a couple of other dietary changes as well as taking pro-biotics in the morning and olive leaf extract in the evening working through past traumas to try ensure healing is more permanent and reduce the frequency of flare ups. I’m also working on managing my stress triggers and This article is the first I’ve heard of GABA and it seems to be another piece of the puzzle for me. How can I get hold of your products in South Africa?
Sorry to hear about these struggles. I would be sure to work with a functional health practitioner to get you on the right plan: https://drjockershdg.wpengine.com/functional-nutrition-tips-to-find-a-great-health-coach/
I have multiple health challenges as a result of having Covid in Sept 2021. is there anyone that can help me? High BP requiring 2 meds, SOB requiring steroids and bronchodilators, poor sleep, and feelings of weakness and intolerance to any exercise.thank you
Very sorry to hear this Audrey! Here is a helpful article for you: https://drjockershdg.wpengine.com/post-viral-syndrome/
These protocol go against every thing that Dr Ashton says in her manual as well as many other experts” regarding benzo withdrawals. It is difficult to know who & what to believe. I would like to know how often you update your research before I start following your protocol. I am going to start benzo taper & am terrified. Thank you
My glutamate and gaba are low. Supplements to boost causes irritability, but at same time need these for better sleep and wake. Dopamine and serotonin levels are normal. Taurine b-complex, prebiotic, probioticts, mg, zn to promote cause no issues. Add any thing like gaba or glutamate supplements and irritability starts. Suffer from CFS.
Good article.
However there is help for using GABA. We agree that GABA by supplement is very poorly passed through the brain’s blood-brain barrier. In medical practice we see a lot of anxiety and mild depression and many of what we are treating are children.
There is a GABA supplement that will readily pass through the blood-brain barrier with a wonderful calming effect within 30 to 45 minute, lasting 4 to 6 hours. The product has no side effects but it does competes with any benzo drug you may be taking.
The product is called GABAtrol and is made by Pure Life. (
GABAtrol has become our go-to supplement for anxiety and mild depression with children and adults.
It easily crosses the blood-brain barrier and provides a very comfortable calmness with no side effects. The supplement does compete with any benzo so they are not taken together.
We have no financial gain from recommending this product. We are only an end user and want to pass on the success we have had with this wonderful product.
.
Thank you for sharing!
My husband has dementia and I have been under stress for several years.
I am 92 and take 700 mg of GABA once or twice daily.
Can I increase this?
Yes, you can find a good dose that makes you feel calm and relaxed. Also, important to consider increasing your magnesium and b vitamins.
I am trying to understand the effects of a gene mutation where glutamine is replaced by aspartic acid and how that mutation could impact GABA supplementation for autism. Any insights would be much appreciated!
Doctor Jockers,
Thank you for the very enlightening material and articles in your website. I
have been following your website for a long time
and the more articles I read the more confident I feel about your wisdom about health, Nutrition, and healing knowledge. Having seen your recommendations about the Organic Nutrients Test, I feel that will be very useful for me to have it. I live in Hawaii, and if you administer it long distance, what protocols do I need to follow in order to get one? Would you also make the results meaningful for me and provide the guidelines to follow your advice?
Thank you
Ruth C. Viafara
tesr
Yes absolutely, we can definitely help you with this. Here is our long distance coaching info: https://drjockers.lpages.co/long-distance-coaching-dr-jockers/
Doc, would you be happy to share your thoughts (or write a short article if you have time) on Benzodiazepine Withdrawal Syndrome? So many of the issues and symptoms you have highlighted here appear with the withdrawal but I reckon the way you would respond to them would be slightly different? Many Thanks.
This article led me to wonder if my son’s adolescent onset seizures could be the result of a glutamate toxicity. When I looked up symptoms, he has all of them. Unfortunately, the only test I’ve been told that exists would require a lumbar puncture. Would the organic acid test be something to try? He had injected antibiotics for the first week of his life. With the gut/brain link being so important, I wonder if that was the beginning. Conventional medicine has no answers except medication. I’m afraid of the long-term side effects.
That is a very interesting article, I’ve never heard before about nasal breathing and anti-inflammatory diet as a way to increase gaba level! I usually take supplements, like nutraharmony gaba l-theanine, I love that it is also magnesium in it. And I will be really interested in checking some of your advice, so thank you for sharing!