 Skin Inflammation: Symptoms, Causes, and Support Strategies
Skin Inflammation: Symptoms, Causes, and Support Strategies
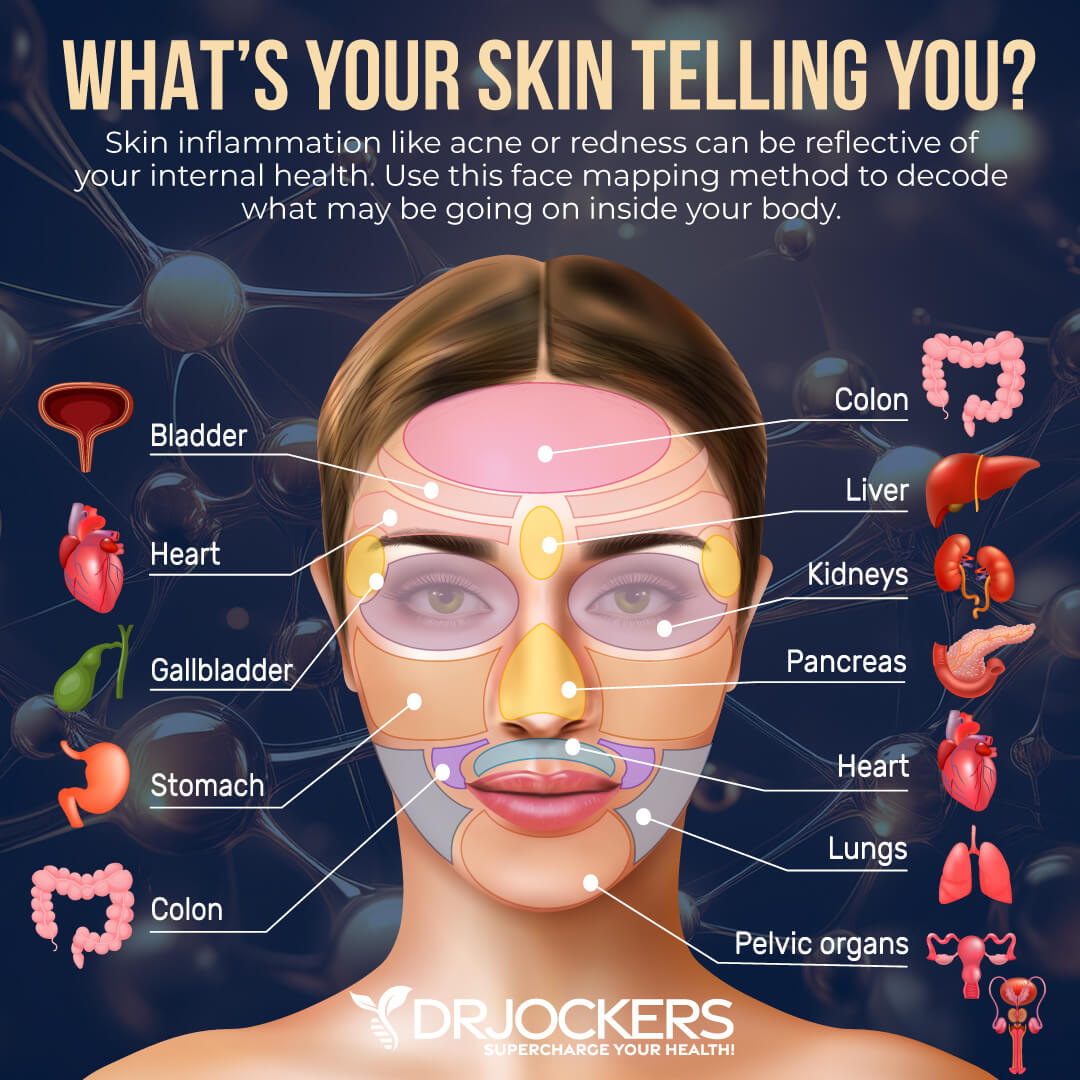
Acne, redness, itching, flaky skin, swelling, and pain. You are dealing with skin inflammation. You are not alone. Skin inflammation and its related chronic symptoms are incredibly common. Most people just try to treat them with creams and other topical options and accept them as a frustrating part of life. However, if you understand the underlying root causes of your skin inflammation, you can improve your skin with the help of some simple natural support strategies.
In this article, you will learn what skin inflammation is. You will understand the symptoms of skin inflammation. You will learn about skin anatomy and physiology. You will understand the root causes of skin inflammation. I will recommend some key functional labs to identify skin inflammation and its underlying root causes. You will learn about the top 7 foods that can damage your skin. I will recommend my top natural support strategies to improve your skin health.
What Is Skin Inflammation
Inflammation is not always a bad thing. Inflammation is part of your body’s defense mechanism and self-healing process. When you have an injury or your body encounters some foreign invaders, such as germs, infections, and allergens, your immune system runs to your defense. It creates acute inflammation to fight off these invaders and heal your wounds on a cellular level.
Acute inflammation is often visible. You may notice swelling, redness, hives, or pimples as your blood vessels dilate to increase blood flow and encourage healing. You may also experience some itching or pain.
Acute inflammation usually lasts for a few days or weeks, depending on the cause. Acute skin inflammation usually lasts only for a few days or a week or two. Your inflammation levels will reduce as your body heals.
However, when inflammation becomes chronic, it can turn into a serious problem. Following an unhealthy diet, chronic stress, unhealthy lifestyle choices, and various environmental factors can trigger your body to treat everything from processed food to emotional stress as foreign pathogens.
Everything will start triggering an immune response. Your body will start believing that you are under attack 24/7, resulting in constant inflammation.
Chronic inflammation can result in a list of health issues, including gut health issues, diabetes, autoimmunity, heart disease, neurodegenerative conditions, and cancer. Chronic inflammation can also affect your skin. It can lead to chronic skin inflammation and chronic skin health issues, including acne, puffiness, redness, hives, itching, enlarged pores, wrinkles, and signs of premature aging.
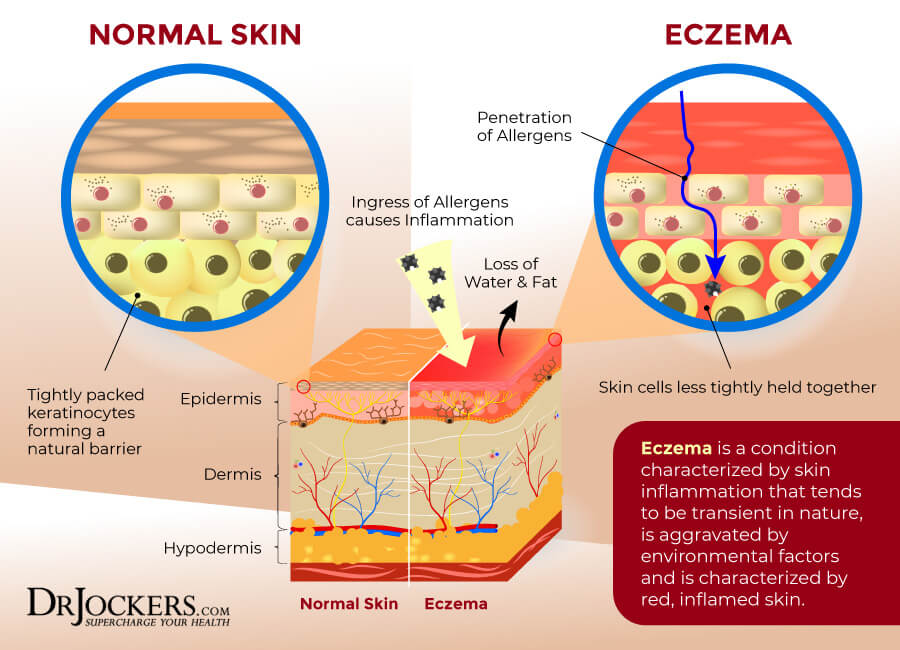
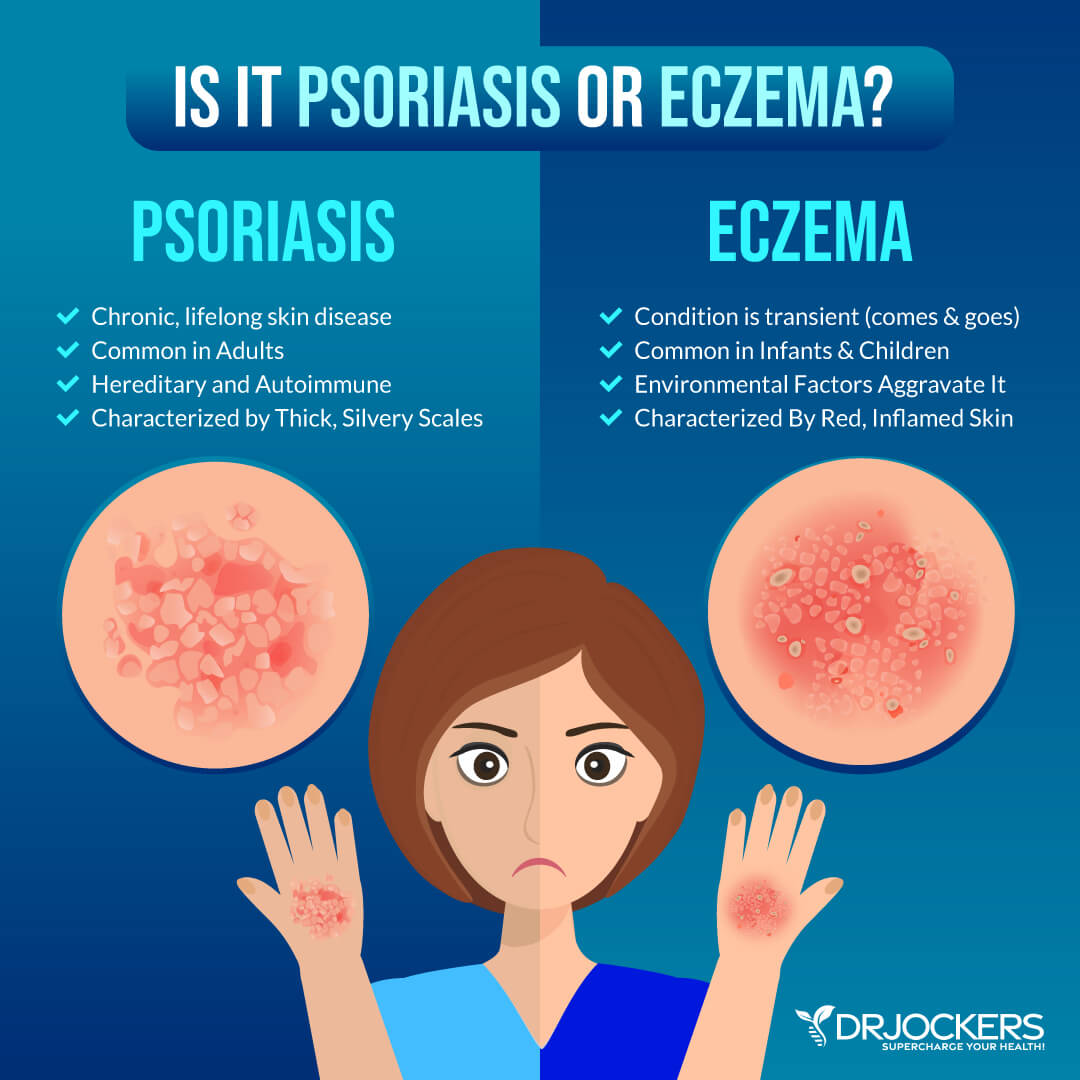
A 2014 study published in Inflammation and Allergy Drug Targets found a connection between chronic inflammation, psychological stress, and skin health issues (1). Chronic inflammation and chronic skin inflammation are also often the root cause of eczema, dermatitis, psoriasis, and other chronic skin conditions.
Symptoms of Skin Inflammation
You may experience skin inflammation for a variety of reasons, including bacteria, viruses, and fungi infections, allergic reactions, immune system dysfunction, gut health issues, hormonal issues, diet, heat, photosensitivity, and genetics.
Depending on the cause and the type of skin problem you are experiencing, your symptoms of skin inflammation may vary. Symptoms may be mild or severe. They may affect only one small area of your skin, or they may be more widespread. Symptoms may be ongoing, or they may come in flares with periods of remission in between.
There may be a variety of symptoms of skin inflammation, including:
- Acne or pimples
- Blisters
- Eczema
- Wrinkles
- Age spots
- Rashes
- Cracked or raw skin that may bleed
- Itching, burning, or stinging
- Oozing
- Redness
- Scaliness
- Warmth in the affected area
- Thickening of the skin

Skin Anatomy & Physiology
Do you ever think about your skin as an organ? You may be surprised to hear that your skin is your largest organ. It serves as a protective barrier on the outside of your body. It’s not surprising that the surface, appearance, and health of your skin are determined by dietary, lifestyle, and environmental factors.
To understand how to keep your skin healthy and glowing, free from skin inflammation, you have to first understand its anatomy and physiology.
Your skin has three major parts, including the hypodermis, dermis, and epidermis. Other parts of your skin include the sebaceous glands, elastin, collagen, dermal-epidermal junction, sebum, and blood vessels.
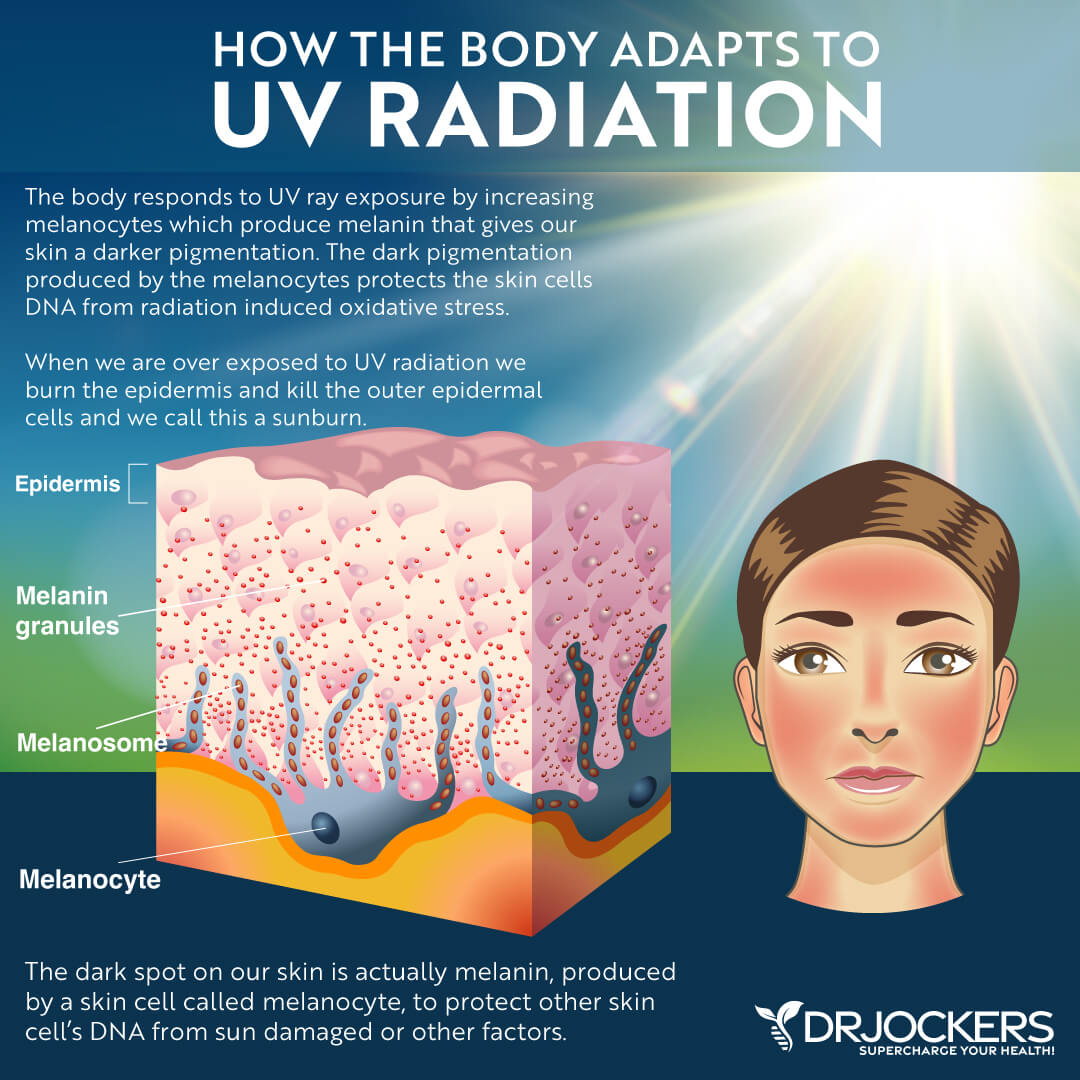
Epidermis
The epidermis is the outer layer of your skin. This layer serves as a protective barrier between your body and the environment. The stratum corneum is the outermost layer of your epidermis. It’s made up of flat, dead skin cells called corneocytes. It provides an effective buffer. The basal layer is the bottom layer of the epidermis, where your pigments are being produced.
Dermis
The dermis is the middle layer of your skin. It acts as your skin’s operation center. It is home to a number of important nerves, glands, enzymes, essential proteins, and blood cells. This layer also contains collagen and elastin, which are both vital for support and structure.
Hypodermis
The hypodermis is located just below your epidermis and dermis. This layer is made up of fat, nerves, and blood vessels. It provides cushion and insulation.
Sebaceous glands
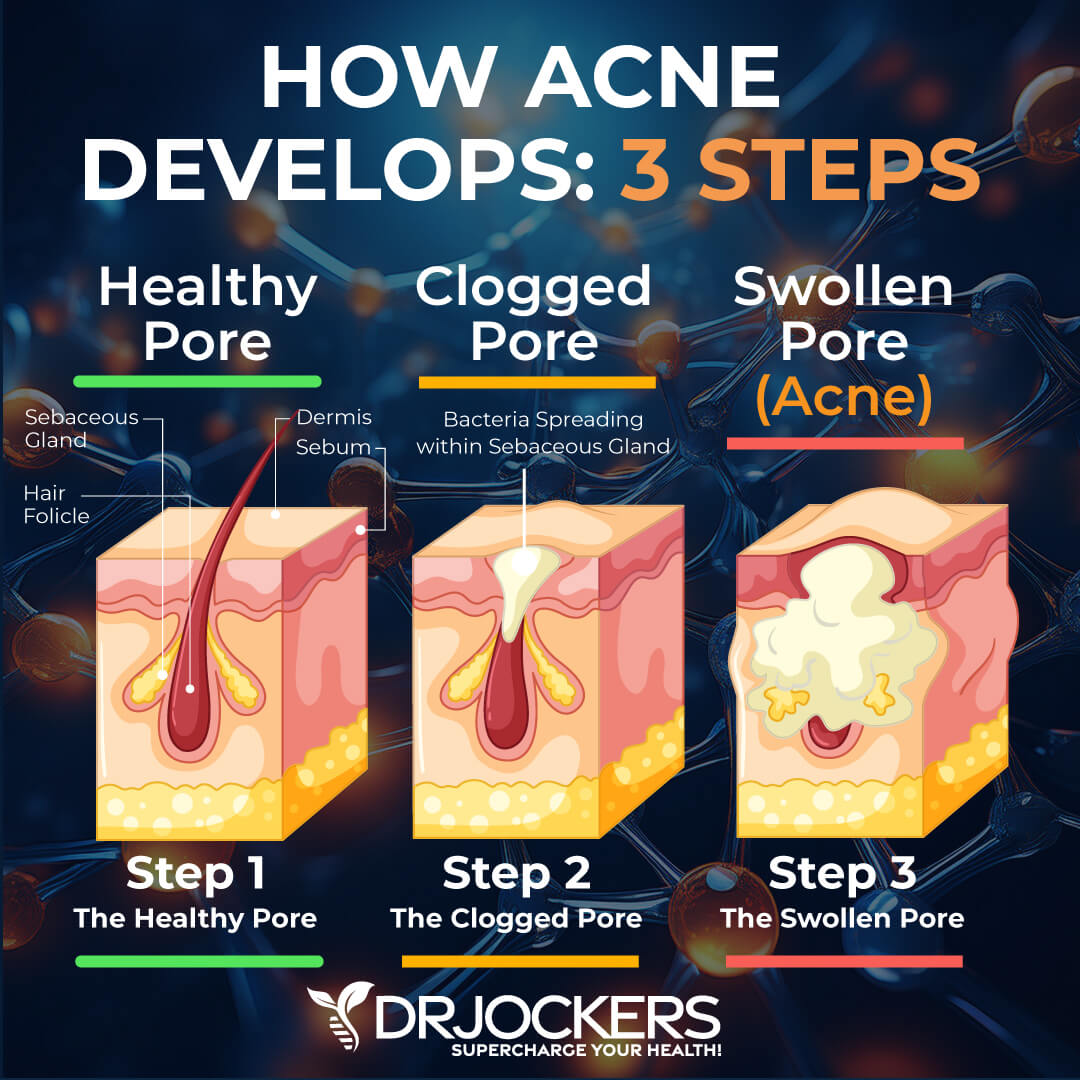
The sebaceous glands are located at the root of your hair follicles. They produce oil, or sebum, to lubricate your skin and hair. They offer protection against friction and breakdown and make your skin impervious to moisture.
Elastin
Elastin is an essential protein that allows your skin to stretch and bounce back after stretching. Sun exposure and repeated facial expressions can both cause damage to elastin, which can result in sagging skin.
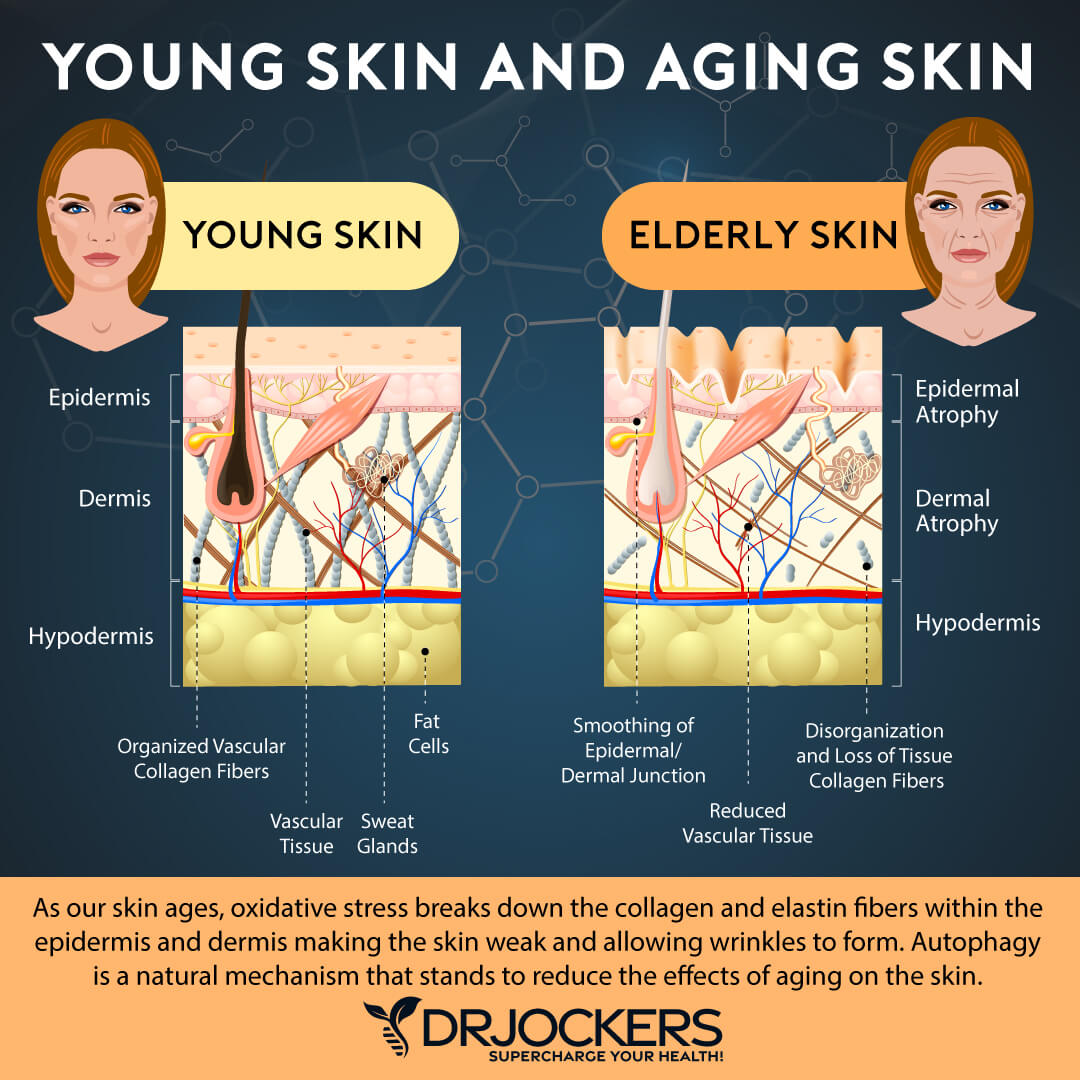
Collagen
Collagen is an essential protein that serves as the building block of your skin’s foundation. It allows your skin to have a smooth structure. Sun exposure and aging over time will result in the breakdown of collagen that causes fine lines and wrinkles.
Dermal-Epidermal Junction
The dermal-epidermal junction (DEJ) connects your epidermis and dermis. This area hosts a network of blood vessels to support the transfer of nutrients from your dermis to your epidermis.
Sebum
The sebum is an oily secretion produced by your sebaceous glands. It helps to waterproof your skin and keep it firm.
Blood Vessels
There is a network of blood vessels located in your dermis and subcutaneous layer. Their role is to supply oxygen and nutrients to your skin. These blood vessels also help to regulate your body temperature.
Root Causes of Skin Inflammation
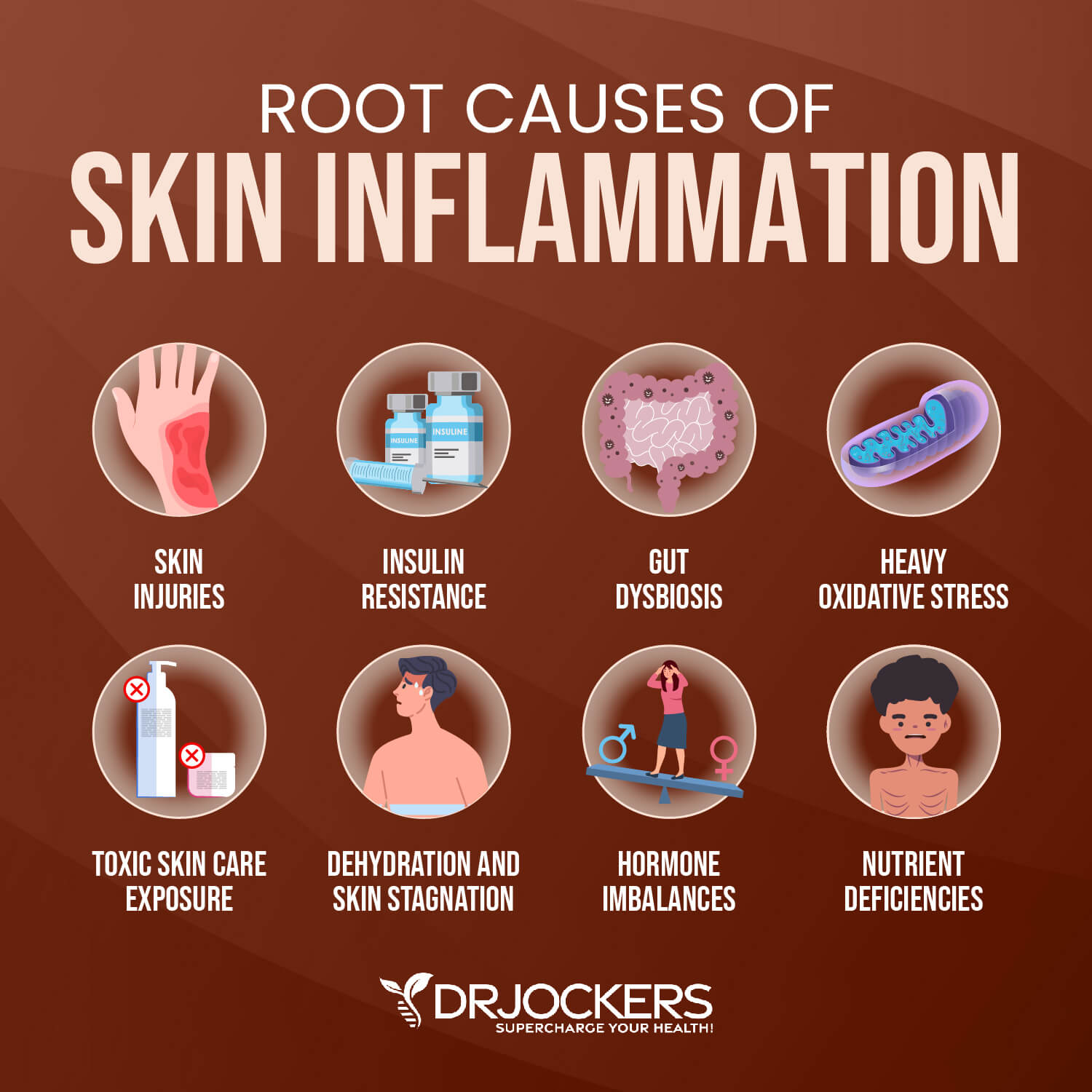
To recover from skin inflammation and chronic skin issues, first, you have to understand the root causes of skin inflammation.
The root cause of skin inflammation includes insulin resistance, gut dysbiosis, heavy oxidative stress, toxic skincare exposure, dehydration, skin stagnation, and nutritional deficiencies. Let’s talk about these root causes of skin inflammation.
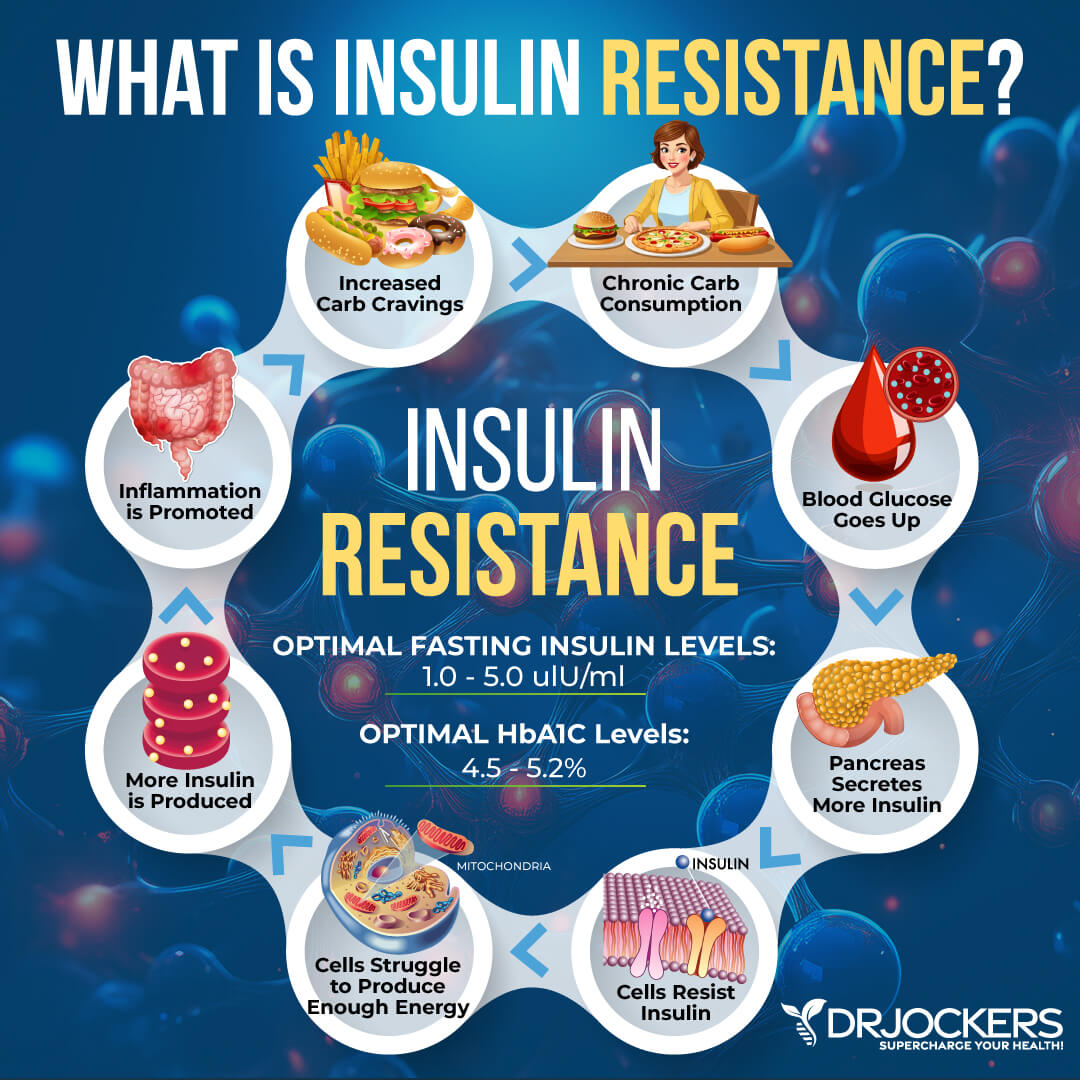
Insulin Resistance
Insulin resistance means that your body doesn’t respond to insulin well and is unable to use the glucose from your body for energy. Trying to keep up, your pancreas will start making more insulin. This can lead to ongoing high blood sugar levels, blood sugar fluctuations, prediabetes, type 2 diabetes, and chronic health issues. It can also increase your risk for skin inflammation and related skin issues.
A 2015 study published in Hindawi found that insulin resistance can increase chronic inflammation and contribute to various inflammation-related skin conditions, including psoriasis, acne, androgenetic alopecia, acanthosis nigricans, hirsutism, and more (2). A 2017 review published in Dermatology and Therapy also found that insulin resistance, diabetes, and obesity can manifest in the skin in the form of acne, hirsutism, acrochordons, and other skin conditions (3).
Moreover, insulin resistance causes dysregulated sphingolipid metabolism. Sphingolipids are complex lipids in your body. There are three major types of sphingolipids, including ceramides, phosphosphingolipids (sphingomyelins), and glycosphingolipids. They offer both structural integrity and play functional roles. They regulate major cellular processes and are an important part of the water barrier of your skin.
According to a 2013 review published in the Handbook of Experimental Pharmacology, sphingolipids play a role in the biological modulation of keratinocytes and immune cells of the skin (4). According to the article, the reduction of ceramides can lead to transepidermal water loss and skin inflammation, and sphingolipid metabolism dysregulation can result in inflammatory skin conditions, such as psoriasis or dermatitis.

Gut Dysbiosis
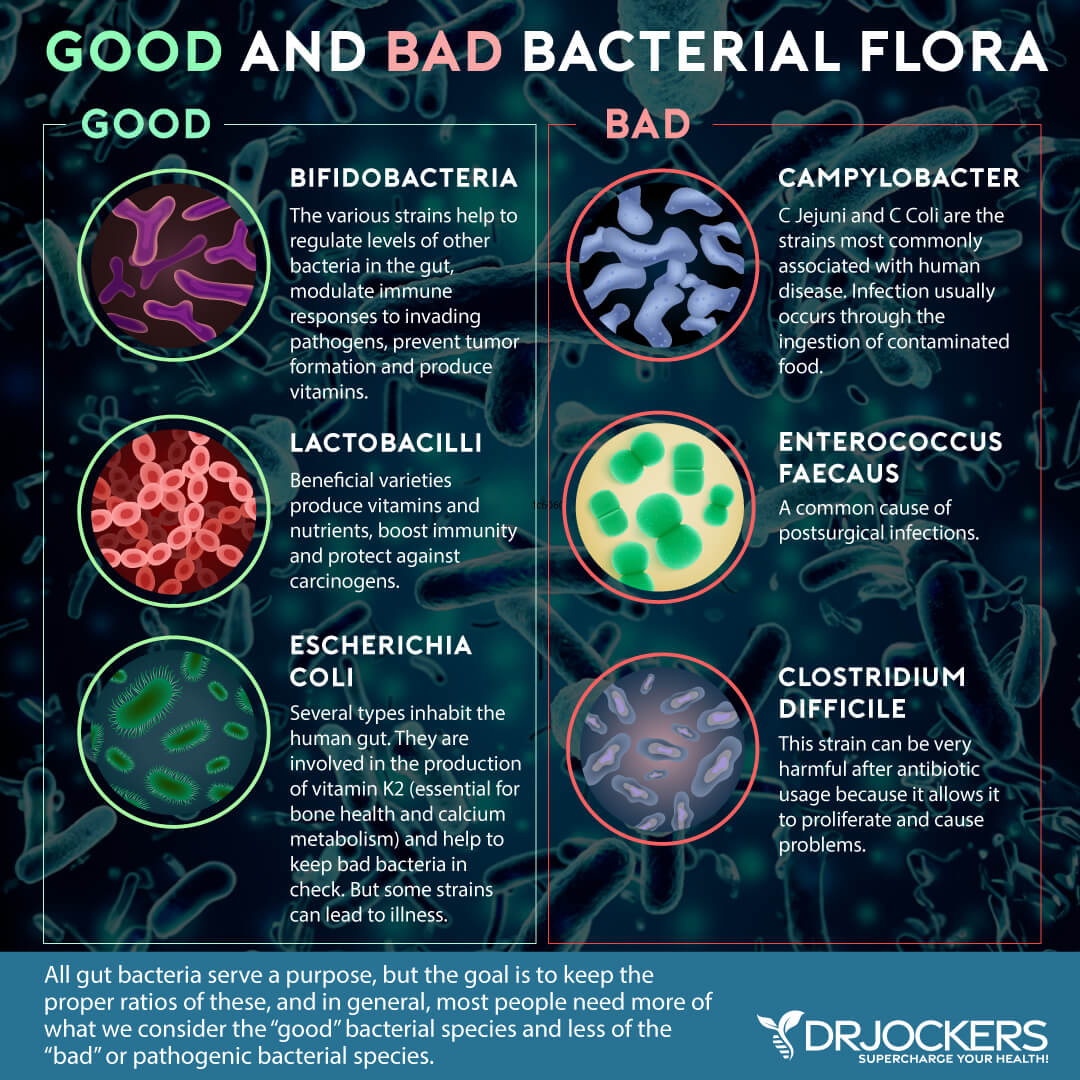
Gut dysbiosis means that your gut microbiome is out of balance. Even though gut dysbiosis occurs in your gut, it doesn’t just affect your gut. Gut dysbiosis can affect your skin greatly. H. Pylori infections can be particularly damaging to your skin.
A 2014 review published in the Hong Kong Medical Journal found that H. pylori infections can trigger a chronic systemic immune response and inflammatory response in your body (5). This can lead to a variety of chronic inflammatory skin conditions, such as rosacea and idiopathic urticaria. A 2018 study published in BMC Infectious Diseases also found that H. pylori infections can play a role in skin issues like rosacea (6).
Gut dysbiosis also impacts histamine metabolism, which can result in histamine intolerance-mediated skin inflammation. Histamines are important neurotransmitters and immune messengers. It plays a role in your immune system by getting rid of allergens and toxins.
It also plays a role in your gut health by triggering the release of hydrochloric acid to help break down your food and bacteria in your gut. It also serves as a messenger between your brain and body, playing a critical role in your brain and mental health.
Your body needs histamine. But histamine becomes a problem when there is too much of it. When you have histamine build-up in your body, it will cause histamine intolerance. Histamine intolerance can affect your entire body, and one of its main symptoms is skin inflammation and related skin problems, such as rashes, hives, and itching. A 2011 study published in the Annals of Dermatology found that histamine intolerance may play a role in dermatitis, and a low-histamine diet may help the condition (7).
Heavy Oxidative Stress
Oxidative stress means that there is an imbalance between the production and accumulation of oxygen reactive species (ROS) in your body’s tissues and cells, and your body is unable to detoxify these products properly and rapidly enough. Oxidative stress increases the risk of chronic inflammation and chronic and inflammatory health issues.
The main causes of heavy oxidative stress include smoking, too much sun exposure, pollution, certain medications, a poor diet high in inflammatory processed foods, heavy alcohol consumption, radiation, and exposure to chemicals, pesticides, and toxins.
Heavy oxidative stress can also increase the risk of skin inflammation and worsen symptoms. According to a 2005 review published in Current Drug Targets, Inflammation and Allergy, oxidative stress can result in inflammatory and allergic skin conditions, including psoriasis, atopic dermatitis, and urticaria (8). A 2014 study published in the Asian Pacific Journal of Cancer Prevention also found that oxidative stress can result in chronic inflammation, collagen fragmentation, collagen fiber disorganization, and various skin diseases, including skin cancer (9).
Toxic Skin Care Exposure
Conventional skin care brands, including creams, lotions, acne products, body wash, and make-up, are full of toxic chemicals. Unfortunately, these products can damage your skin and cause skin inflammation. According to a 2019 study published in the Journal of Preventive Medicine and Hygiene, many chemicals found in cosmetic products can cause allergic reactions, dermatitis, and other acute side effects (10).
Beyond causing allergic reactions and inflammation, many skin care products also strip away your skin’s natural moisture and oils. Instead of truly moisturizing it, they cause dependence on the product, and you will have to reapply them regularly to feel moisturized. You may learn more about toxic skin care and beauty products in this article.

Dehydration and Skin Stagnation
Dehydration can also result in skin stagnation or skin inflammation. Dehydrated skin is lacking water and moisture. This can result in itching, dullness, scaling, flaking, fine lines, and wrinkles. Dehydration may result in early visible signs of aging.
When we talk about skin hydration, many people automatically think about moisturizers and hydrating products. However, your skin’s hydration depends a lot on your body’s overall hydration levels. A 2015 study published in Clinical, Cosmetic, and Investigational Dermatology found that dietary water and hydration also affect skin hydration and skin health (11). Dehydration can result in epidermal and transepidermal water loss that may lead to skin inflammation and skin health issues.

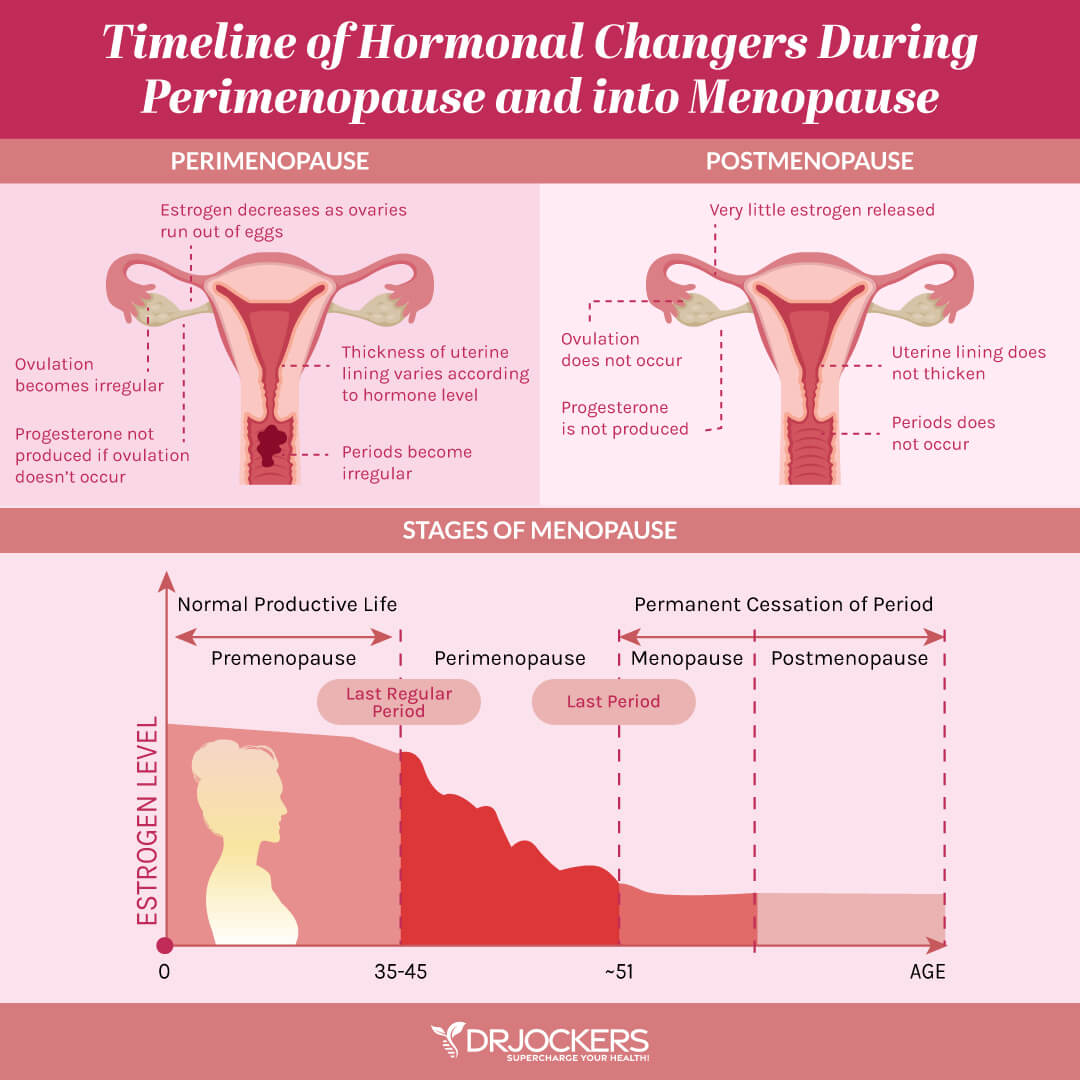
Hormone Imbalances
Hormonal imbalances can also result in skin inflammation. Estrogen and progesterone fluctuations throughout the month and an estrogen-progesterone imbalance can both impact your skin.
If you are a woman, I probably don’t have to introduce you to hormonal acne. According to a 2014 study published in the Journal of Clinical and Aesthetic Dermatology, 63 percent of adult women experience acne during the late luteal phase of their menstrual cycle, and nearly 25 percent experience an increase in the total number of acne lesions, including comedonal and inflammatory lesions (12).
However, you may also experience skin issues after menopause. According to a 2014 study published in the Journal of Midwife Health, estrogen deficiency after menopause can cause a variety of skin conditions, including alopecia, menopausal flushing, hirsutism, keratoderma climacteric, atrophic vulvovaginitis, vulvar lichen sclerosis, vulvovaginal candidiasis, and aesthetic vulvodynia (13).
Nutrient Deficiencies
Your diet and nutrition also play a critical role in your skin health. There are various nutrient deficiencies that can increase the risk of skin inflammation, including omega-3, vitamin A, vitamin D, and zinc deficiencies.
Omega-3 Fatty Acids
Omega-3 fatty acids are anti-inflammatory fatty acids found in algae, fish, flaxseed, chia seeds, hemp seeds, and walnuts. Deficiencies in omega-3 fatty acids and an omega-3: omega-6 imbalance can result in skin inflammation.
A 2020 study published in the International Journal of Molecular Sciences found that omega-3 fatty acids may help to reduce inflammatory processes and reduce psoriasis, dermatitis, acne, and other inflammatory skin problems (14). Another 2020 study published in the Journal of Cutaneous Medicine and Surgery also found that omega-3 fatty acids may benefit various dermatological conditions (15).

Vitamin A
Vitamin A is a group of fat-soluble retinoids that are essential for your skin, eyes, immune system, and bone health. They are mainly found in orange and yellow vegetables and fruits, cod liver oil, eggs, and dark leafy greens. Deficiencies in vitamin A can lead to skin inflammation.
A 1996 study published in the Scandinavian Journal of Immunology found that vitamin A deficiency can increase inflammatory processes, inflammatory reactions, and related health issues (16). A more recent, 2020 study published in the Clinical and Experimental Allergy found that vitamin A deficiency can activate the mast cells and cause a T cell-type inflammation, which may contribute to atopic dermatitis (17).

Vitamin D
Vitamin D is an important vitamin that your body gets from sunshine and certain foods, including fatty fish, egg yolks, and beef liver. It’s vital for muscle and bone health, immune health, brain, and mental health. It’s also important for your skin.
A 2015 review published in the Indian Journal of Dermatology, Venereology, and Replorogy found that vitamin D deficiency may play a role in various skin diseases (18). A 2018 study published in Skin Pharmacology and Physiology found that vitamin D deficiency may contribute to psoriasis and atopic dermatitis (19).

Zinc
Zinc is found in red meat, poultry, certain seafood, nuts, beans, and whole grains. It is essential for your immune health and metabolism, but it also plays an important role in your skin health.
According to a 2016 study published in Nihon Rinsho, zinc deficiency may play a role in the development of various skin diseases (20). A 2018 study published in Nutrients has also found that zinc deficiency may contribute to various skin issues, including alopecia, poor wound healing, and skin issues related to Ehlers-Danlos Syndrome (21).
Beyond zinc, your copper levels are also important. Zinc and copper compete against each other as antagonists to regulate physiological pathways. A proper balance between the two is essential for maintaining good skin health. A 2008 review published in the Revista Medico-Chirurgicala e Societatii de Medici Si Naturalisti Din Lasi found that the poor zinc: copper ratio can cause immunological reactions and inflammation and lead to various skin diseases (22).

Key Functional Labs
There are a number of key functional labs I like to look at when testing for skin inflammation and underlying root causes. Here is what I recommend:
Inflammation: Hs-CRP, ESR, LDH & Serum Ferritin
For inflammation, I recommend a C-Reactive Protein or CRP test, erythrocyte sedimentation rate (ESR) test, Lactate Dehydrogenase (LDH) test, and serum ferritin levels.
The Hs-CRP test measures a protein (CRP) produced in your liver that indicates inflammation levels in your body. The clinical range is between 0 and 3 mg/L, while the optimal range is 0 to 1 mg/L. When I see levels over 1 mg/L, I know the individual is having an inflammatory response that could be due to acute trauma or chronic conditions.
ESR refers to the rate at which your red blood cells in anticoagulated whole blood go down in a standardized tube over a period of one hour. Optimal ESR rates are between 0 and 10 mm/hr.
LDH is an enzyme found in all living cells. Elevated levels may indicate inflammation. Optimal levels are between 140-180. Levels over 180 indicate inflammation, and levels under 140 indicate reactive hypoglycemia.
Serum ferritin measures the level of ferritin in your body to detect iron deficiency anemia and other health issues. Elevated serum ferritin levels may indicate inflammation, liver disease, autoimmune disease, or even cancer. The clinical range is 30 to 400, and the optimal range is 50 to 150 for females and 75 to 150 for males. You can learn more about the best lab markers for inflammation in this article here.

Insulin Resistance: Fasting Insulin, HbA1C, Lipid Profile
For insulin resistance, I recommend looking at your fasting insulin, hemoglobin A1C (HbA1C) levels, and lipid profile.
Testing your fasting insulin can recognize elevated blood sugar levels and can detect inflammation, insulin resistance, blood sugar issues, and diabetes. The clinical range for fasting insulin is 2.6 – 24.9 uIU/ml, and the optimal range is 1.0 – 6.0 uIU/ml. Anything above 6 indicates insulin resistance and especially if it is above 10.
Your HbA1C levels measure your average blood sugar over the past 2 to 3 months. Hemoglobin A1C (HbA1c) gives the average amount of glucose in your blood or blood sugar over the past 3 months, making it one of the top tests for inflammation and diabetes. The clinical range is between 4.8 and 5.6, while the optimal range is 4.5 – 5.2.
Your lipid paneer may be another indication of inflammation and related issues, such as clogged arteries and cardiovascular issues, as well as insulin resistance. We are looking for low HDL or high triglycerides as a sign of insulin resistance. Having a balanced ratio of LDL to HDL and triglycerides to HDL is essential for your health.
Ideally, we are looking for an LDL: HDL ratio: 3:1 or less, 2:1 being optimal. We are also looking at a triglyceride: HDL ratio of 2:1 or less, 1:1 being optimal. Higher rates may indicate insulin resistance and inflammation. Optimal levels:
- HDL cholesterol: The ideal range is 55 to 80. Levels above 100 can indicate chronic inflammation or active infection in the body.
- Triglycerides: The ideal range is 40 to 80.
Vitamin A, Vitamin D, Plasma Zinc: Serum Copper Ratio
Vitamin A is essential for your immune system, eye health, bone health, and skin health. Normal serum vitamin A levels are between 35–60 ug/dL.
Vitamin D3 is an important vitamin that most of our population is deficient in. Poor levels may indicate inflammation. Normal levels of vitamin D are between 50-100 ng/mL
Checking your plasma zinc levels is the best way to determine zinc levels in your body. Ideal plasma zinc levels are between 90–135 ug/dL, and for serum copper, it should be 70–110 ug/dL. Zinc and copper compete against each other as antagonists to regulate physiological pathways.
A proper balance between the two is essential for maintaining good health. I recommend checking your plasma zinc and serum copper levels and their balance. The proper zinc:copper ratio should be between 1–1.2.

To test all these, I recommend the Comprehensive Blood Analysis (CBA). This is the most detailed blood test that looks at all of these markers of inflammation. This test is more sophisticated than most conventional doctors are able to order.
It examines all parameters for inflammation, blood sugar levels, thyroid function, zinc and copper ratio, vitamin A and D levels, a complete metabolic panel, complete blood count, liver function, nutrient deficiencies, and more. I recommend getting the Comprehensive Blood Analysis done regularly, both as a preventative measure and to monitor your inflammation levels and progress.

DUTCH Test
I also recommend the DUTCH Test™ — Dried Urine Test Comprehensive Hormones to check for estrogen and progesterone levels. This test offers a complete hormonal panel. Beyond your estrogen and progesterone levels, this test looks at testosterone, cortisol, DHEA, and melatonin levels.
The DUTCH Test™ is well-recognized for its ease-of-collection, coupled with comprehensive reporting that is not available from other laboratories. The DUTCH Adrenal provides free cortisol patterns that parallel saliva, with the addition of metabolite measurements for an improved marker for total cortisol production.
GI MAP
I also recommend a GI Map Stool Test to look for gut dysbiosis, parasites, H. Pylori infection, and gut inflammation markers. This is the best and most comprehensive gut test I have found to get an understanding of your gut health and help with appropriate lifestyle changes. It helps to determine whether you have underlying gut dysbiosis.
It helps to identify bacterial pathogens, parasitic pathogens, viral pathogens, normal flora, and dysbiotic flora. This test also looks at potential autoimmune triggers and all intestinal health markers. Using this test along with the other functional tests I recommend takes the guesswork out of your treatment and allows us to identify the major root causes of your health issues and create an appropriate treatment plan.
7 Foods That Damage the Skin
You are what you eat. I know this sounds like a cliche, but it’s true — your diet matters. If you are following an anti-inflammatory and nutrient-dense diet, you are reducing your risk of chronic inflammation and related health issues.
Eating a healthy diet reduces your risk of skin inflammation and supports healthy and glowing skin. Eating an unhealthy, inflammatory diet low in nutrients, on the other hand, can increase chronic inflammation and skin inflammation. It damages your skin and increases your risk of unhealthy skin and chronic skin problems.
There are 7 main foods that can damage your skin, yet most people consume them regularly. Let’s talk about these foods that can damage your skin.
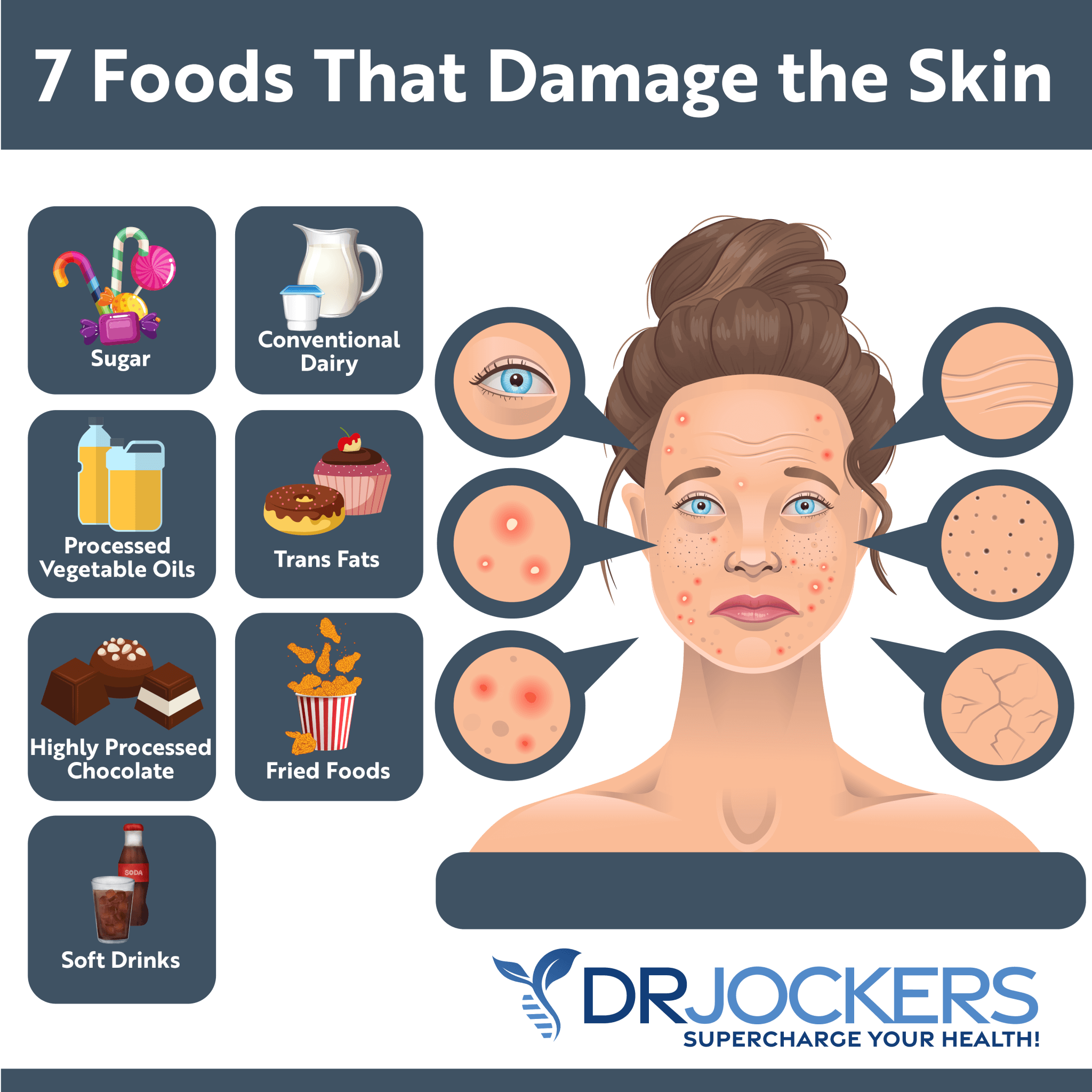
Sugar
Refined sugar is one of the, if not the, unhealthiest foods out there. It can cause chronic inflammation and lead to insulin resistance, diabetes, obesity, neurodegeneration, heart disease, mental health issues, and more. It is not surprising that sugar can also cause skin inflammation and skin damage.
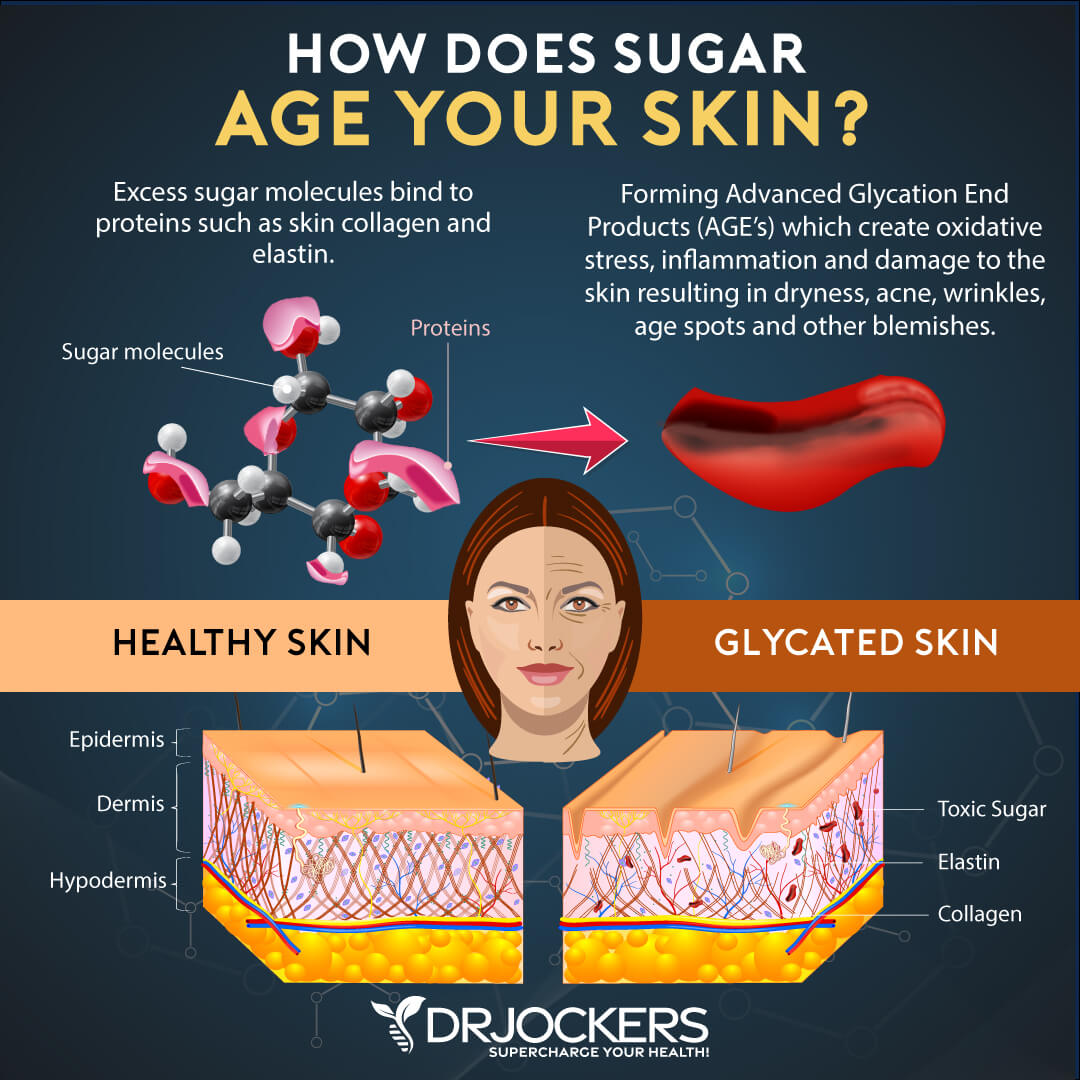
Sugar leads to chronic inflammation that can break down both elastin and collagen. The loss of elastin and collagen will result in signs of early aging, such as sagging and wrinkles. A 2007 article published in the American Journal of Clinical Nutrition found that a poor diet can result in skin sagging in middle-aged women (23).
A 2012 study published in the Journal of the European Academy of Dermatology and Venereology found that dietary habits, such as eating sugar, may increase the risk of acne (24). A 2012 study published in Dermato Enterology has found that eating too much sugar can also lead to glycation, which is the process, which digested sugar permanently attaches to the collagen in your skin (25). Glycation may increase the risk of various skin conditions, including acne and rosacea.
Conventional Dairy
Conventional dairy is one of the most advertised foods out there. Yet it is one of the top inflammatory foods. It can increase chronic inflammation. It can worsen skin inflammation and inflammatory skin problems, such as acne, eczema, psoriasis, and rashes.
Conventional dairy is high in antibiotics and growth hormones, both of which can interfere with your hormonal balance. Hormonal issues can result in skin problems, including hormonal acne.
Furthermore, most of the world and much of the US population is lactose intolerant or sensitive to dairy itself. Lactose intolerance and dairy sensitivity can both increase the risk of skin inflammation and a flare-up of chronic skin conditions. For example, according to a 2014 study published in the Journal of Clinical Aesthetics and Dermatology, dairy can increase the chances of acne (26).

Processed Vegetable Oils
Processed or refined vegetable oils, such as canola, corn, soybean, sunflower, sesame, rice bran, and cottonseed oils, became popular in the 20th century. These processed vegetable oils are made by extracting oil from plants using an oil mill or chemical solvent. Often, they are purified, refined, and even chemically altered.
Processed vegetable oils are also very high in inflammatory omega-6 fatty acids. According to a 2006 study published in the American Journal of Clinical Nutrition, you need a healthy balance of anti-inflammatory omega-3 and inflammatory omega-6 fatty acids (27).
This means that you need lots of omega-3s and fewer omega-6s than the Standard American Diet (SAD) offers. Eating a diet high in processed vegetable oils and getting too much inflammatory omega-6 fatty acids in your diet increases your risk of skin inflammation and related skin problems.

Trans-Fats
Artificial trans fats are made in an industrial process. To make them by adding hydrogen to transform liquid vegetable oils into a more solid form. Trans fats are everywhere. The main dietary source of trans fats is partially hydrogenated oils hiding in countless processed foods, including frozen pizzas, cakes, crackers, margarine, and pie crusts.
Trans fats present a serious problem when it comes to your health. According to the American Heart Association, they can increase your risk of heart disease (28). They also increase chronic inflammation, including chronic skin inflammation. They also increase the risk of skin damage and inflammatory skin conditions.

Highly Processed Chocolate
Some advertisements claim that chocolate is healthy. What they forget to tell you is that highly processed chocolate is not. Raw cacao is incredibly high in antioxidants, which means that raw chocolate can offer plenty of health benefits. Even a high-quality extra-dark chocolate can offer antioxidants. However, high-processed chocolate cannot.
Highly processed chocolate usually uses alkali-treated processed cocoa, not antioxidant-rich raw cacao. According to a 2008 study published by the Journal of Agricultural and Food Chemistry, commercial cocoa powder and cocoa products lose their antioxidant benefits and flavonol content through the alkalization process (29).
Highly processed chocolates also have very little cacao in them. Instead, they are loaded with inflammatory ingredients, including refined sugar, artificial flavors, soy lecithin, and cacao liquor. Highly processed chocolate offers no nutritional value; instead, it can lead to chronic inflammation, skin damage, and a list of health problems.
Fried Foods
Fried foods are a regular part of the SAD diet. People consume it at fast food restaurants on the go, at cookouts, at county fairs, at restaurants, and at home. The problem is that these fried foods are usually deep-fried in processed vegetable oils.
You already know that processed vegetable oils are loaded with trans fat and inflammatory omega-6 fatty acids. According to a 2012 study published in the Journal of Nutrition Metabolism, high dietary omega-6 fatty acids can increase chronic inflammation and inflammatory conditions (30). When vegetable oils are heated at high heat, they oxidize. Putting oxidized fat into your body can lead to unhealthy circulation, lack of oxygen in your skin, and damaged collagen and elastin, all of which may result in signs of early aging and skin damage.

Soft Drinks
Soft drinks are loaded with refined sugar. You already know that refined sugar can increase skin inflammation and cause skin damage (23, 24, 25). Soft drinks are also loaded with artificial sugars and other artificial ingredients that can cause skin inflammation and skin problems.
Many soft drinks, including sodas and energy drinks, are also caffeinated. Caffeine can dehydrate your body and make your skin lose moisture, causing dry and flaky skin, fine lines, and wrinkles. Too much caffeine results in increased cortisol levels, and excess cortisol can accelerate aging and result in fine lines, wrinkles, brown spots, dehydration, and skin damage.

Natural Support Strategies
Reducing skin inflammation is critical for your skin health. The good news is that there are various natural support strategies that can improve your skin. Here is what I recommend:
Anti-Inflammatory Nutrition Plan
Poor nutrition is one of the number one factors that can lead to skin inflammation and skin problems. According to a 2012 study published in Dermato Endocrinology, a poor diet can lead to early aging of your skin (31). Improving your nutrition with an anti-inflammatory nutrition plan can help to reduce chronic inflammation and skin inflammation, reduce signs of aging and poor skin, and better your skin health.
Remove inflammatory and skin-damaging foods, such as refined sugar, refined oils, deep-fried foods, additives, artificial ingredients, conventional dairy, gluten, junk food, and highly processed food. Choose organic to reduce exposure to pesticides, herbicides, hormones, and other toxins.
Follow a diet rich in anti-inflammatory foods, including greens, vegetables, herbs, spices, low-glycemic index fruits, mushrooms, grass-fed beef, pasture-raised poultry and butter, wild-caught fish and seafood, and wild game.
Focus on healthy fats, such as good fats, such as avocados, coconut oil, grass-fed ghee or butter, olives, and extra virgin olive oil, and foods rich in omega-3 fatty acids, including wild-caught fish, flaxseeds, chia seeds, and hemp seeds. Eat plenty of anti-inflammatory herbs and medicinal foods, such as ginger, turmeric, cinnamon, chili, cayenne, black pepper, rosemary, cloves, and raw honey.
Add foods that are rich in silica to reduce wrinkles and create shinier skin, including alfalfa, beets, dandelion, tomatoes, peppers, celery, carrots, and cucumber. Consume plenty of foods that are rich in antioxidants, including blueberries, strawberries, raspberries, blackberries, kale, artichokes, raw cacao, cilantro, pecans, and walnuts. You can learn more about an anti-inflammatory diet to rejuvenate your skin here.

Optimize Hydration Levels
Optimal hydration levels are essential for your overall health, including your skin health. Dehydration is one of the main reasons for fine lines, wrinkles, dry skin, and early signs of aging (11). Optimizing your hydration levels is critical for reducing skin inflammation and creating healthier and younger-looking skin. Hydration also helps your body’s detoxification processes.
While 8 to 10 glasses of water each day is the general recommendation, your personal needs may be higher, especially if you are exercising, doing physical labor, out in the sun a lot, using a sauna, sweating a lot for any reason, or sick. I recommend that you start your day with 32 oz. of clean, purified water, then drink a glass every hour throughout the day.
Drinking green juices, green smoothies, and herbal tea, and eating hydrating vegetables and fruits can also boost your hydration. You may add some lemon or lime to your water to support your metabolism, detoxification, and digestion, and create an alkaline environment in your body. You may make some vitamin water by adding cucumber, berries, mint, basil, or citrus to your water to add more nutrients and flavor.

Avoid Food Sensitivities and Intolerances
Food sensitivities and food intolerances can cause chronic inflammation, skin inflammation, and other skin issues. Dairy and sugar are some of the most common culprits; however, there are many other common and uncommon food sensitivities that may lead to an issue, including corn, eggs, shellfish, gluten, peanuts, tree nuts, and soy (24, 25, 26).
Testing for food sensitivities and food intolerances and removing them from your diet is critical for reducing skin inflammation. You can identify your food sensitivities with the combination of some blood tests, pulse testing, and an elimination diet. You can learn more about how to identify your food sensitivities in this article and how to reduce your food sensitivities in this article.
Consider a Low-FODMAP Diet Trial
Beyond food sensitivities, gut dysbiosis can affect your gut health as well, which can affect your skin health. Since gut dysbiosis can lead to skin inflammation, following a low-FODMAP diet can be beneficial as well (5, 6).
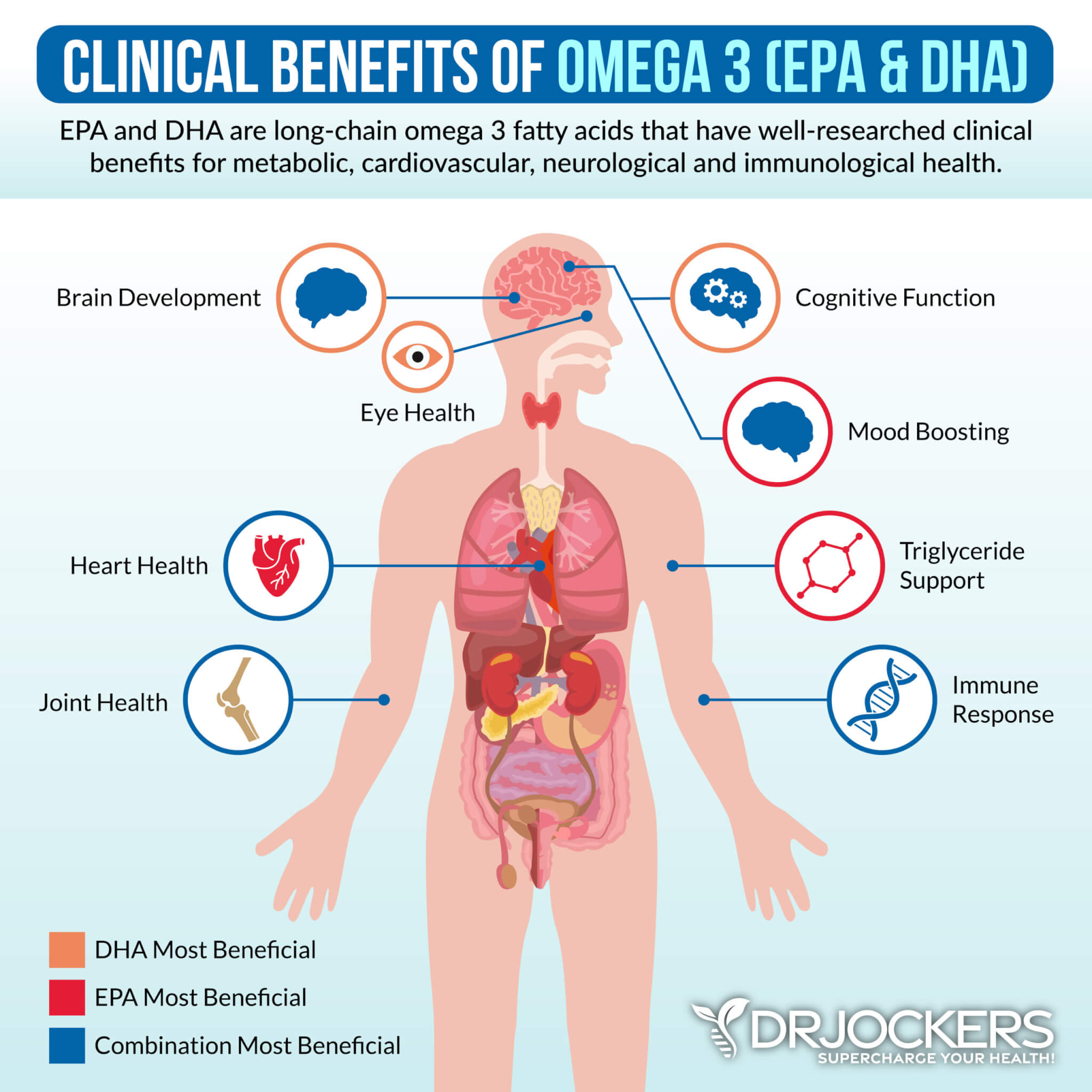
FODMAP stands for Fermentable, Oligo, Di-, and Monosaccharides, and Polyols. The low-FODMAP diet is mainly used for small intestinal bacterial overgrowth (SIBO) and similar gut health symptoms because higher FODMAP foods, such as beans, grains, cruciferous veggies, and many fruits, tend to increase SIBO symptoms.
Low-FODMAP vegetables include carrots, green beans, arugula, mint, basil, pepper, olive, pumpkin, tomato, potatoes, sweet potatoes, cucumber, zucchini, Swiss chard, lettuce, radishes, parsnip, sprouts, kale, and collard greens.
Low-FODMAP fruits include lemon, lime, kiwi, grapes, papayas, strawberries, raspberries, blueberries, melon, pineapples, and tangerines. Other low-FODMAP foods include egg, meats, fish, brazil nuts, chestnuts, butter, bone broth, seafood, quinoa, millet, rice, walnuts, and pinenuts. To learn more about the low-FODMAP diet, I recommend this article.
Consider a Low Histamine Trial
Another food intolerance that can also result in skin inflammation is poor histamine metabolism (7). Histamine intolerance is not sensitivity to histamine but an unhealthy build-up of histamine in your body, leading to an array of symptoms, including skin-related problems. A low-histamine diet plan can help.
High-histamine foods include avocados, tomatoes, bananas, strawberries, dried fruits, most citrus, eggplant, spinach, vinegar, vinegar-containing foods, cashews, walnuts, peanuts, fermented foods, cheeses, smoked fish, cured meat, many spices, processed foods, and leftovers. If you have histamine intolerance, I recommend that you remove all high-histamine foods and focus on lower-histamine foods for a month or until you feel better. Eventually, you can start re-introducing higher histamine foods at limited amounts, depending on how you tolerate them.
Beyond foods, other factors, such as chronic stress, toxins, environmental issues, gut health issues, and certain medications, can also increase histamine intolerance. It is important that you address these health and lifestyle factors, as well as those beyond your diet. You may learn more about histamine intolerance and what to do about it by reading this article.

Intermittent Fasting
Intermittent fasting is a form of fasting. It cycles between a period of eating and not eating within one day. You are basically fasting for a part of a day only but do that every day or several days a week on a regular basis. Intermittent fasting is a great way to improve your health.
A 2014 study published in the International Journal of Health Sciences (Qassim) found that intermittent fasting can decrease inflammation, reduce insulin resistance, lower the risk of disease, and improve overall health (32). According to a 2018 study published in Clinics (Sao Paulo), intermittent fasting can improve autophagy or cellular renewal (33). These benefits may impact your skin health as well.
A 2019 review published in Nutrients has found that caloric restriction through fasting and intermittent fasting can improve skin anatomy and physiology and reduce skin pathology (34). According to a 2021 study by the University of Ghent, 5:2 fasting (eating normally for 5 days and caloric restriction, fasting for 2 days can improve psoriasis (35).
One of the best ways to start with intermittent fasting is a Simple Fast. The Simple Fast only involves a 12-hour fast, including your overnight sleep. Simply stop eating after dinner and don’t eat until 12 hours later at breakfast. Extend your fasting window gradually. Most people find that they feel best using the 16:8 approach, with 16 hours of fasting and 8 hours reserved for eating. Listen to your body; however, you may feel better with a slightly shorter or longer window.
Intermittent fasting is not about caloric restriction or nutrient deprivation. Make sure to eat anti-inflammatory, nutrient-dense foods and meet your caloric needs during your eating window. Drink plenty of clean, purified water during your fasting period. Herbal tea is also allowed. You may learn more about intermittent fasting by reading this article.

Consider a 3-5-Day Partial Fast or Water Fast
Besides intermittent fasting, other fasting strategies, such as partial and water fasting, can improve your skin health as well (34). Even just a couple of days of fasting can make a difference (35). If you are doing well with intermittent fasting, you may want to try a 3 to 5-day partial fast or water fast.
A partial fast is a way to practice extended fasting without completely depriving yourself of nutrition. One of the most popular partial fasting strategies is liquid fasting, including Juice Fasting and Bone Broth Fasting. During these fasts, you will be drinking green juices or bone broth, respectively, but won’t be consuming food during your fast.

Another common partial fasting strategy is The Fasting Mimicking Diet®, or FMD®. The FMD® is a partial fasting plan that is high in nutrients, low in protein, and low in carbohydrates. It’s a 5-day protocol that you can do every 8 to 12 weeks or every month, depending on your health goals.
While on the FMD® protocol, follow this plan:
- Day 1: Restrict your calories to 1,100 calories a day. 500 of these calories should come from complex carbohydrates and 500 from healthy fats. About 100 calories or 25 grams of plant-based proteins are also allowed, mainly from nuts.
- Day 2 – 5: During the last four days, your calories are restricted to 800 calories only, with 400 calories from complex carbs and 400 calories from healthy fats.
- Day 6: Though your FMD® is officially over, day 6 is a transition day. Follow a diet rich in nutrient dense fruits, vegetables, and bone broth. Limit your consumption of cheese, milk, sugar, processed foods, and pastries. It is important to note that pastries and other foods with gluten, refined sugar, and highly processed ingredients are never healthy, even if you are not fasting. If you eat dairy, it is important that you choose organic dairy products.

Two other popular partial fasting methods include the Fast or Keto Fast and the Daniel Fast. Fat or Keto Fasting works by raising the ketone levels in your blood and pushing your body into ketosis, reducing inflammation, improving autophagy, and enhancing your health. During the Fat Fast, you need to focus on a high-fat and low-calorie diet of no more than 1,000 to 1,200 calories per day with 80 percent of your calories coming from healthy fats, such as avocados, coconut oil, pasture-raised butter and ghee, olives, and olive oil.
The Daniel Fast is a vegetarian fast based on Biblical principles. While I don’t recommend eating a vegetarian diet long-term, you may benefit from a short vegetarian fast with nutrient-dense plant-based foods. It is also a perfect fast for spiritual contemplation and connection. You may learn more about partial fasting from this article.
If you are doing well on more advanced intermittent fasting and practicing partial fasting, you may be ready for a water fast. A water fast means that you are staying away from food completely for the period of your fast. You are only drinking plenty of purified, clean water throughout the day and in some cases, also some calorie-free herbal tea. You may try this for a day, and if you do well, for several days. I personally enjoy practicing water fasting once a week.
Water fasting is a very advanced fasting strategy that I only recommend if you are an experienced faster. I also recommend that you consult your healthcare provider before going on a water fast, especially if it’s for more than a day. You may learn more about water fasting here.

Regular Exercise
Regular exercise is one of the best ways to reduce chronic inflammation. Sweating helps detoxification and cleansing of the skin. It helps to improve lymphatic health, circulation, and insulin sensitivity. It may also directly benefit your skin health.
A 2016 study published in the Journal of Physiology found that exercise can reduce lymphatic dysfunction (36). A 2018 study published in Frontiers in Cardiovascular Medicine found that exercise, especially cardiovascular exercise, can improve your circulation, blood pressure, and cardiovascular function (37).
A 2013 study published in the Journal of Clinical & Diagnostic Research found that exercise can decrease insulin resistance, inflammation, and oxidative stress (38). A 2015 study published in Aging Cell found that exercise can improve skin metabolism, support skin structure, and reduce signs of skin aging (39).
I recommend that you lead an active lifestyle and exercise regularly at least five times a week. Try a mix of cardiovascular exercise, resistance and strength training, and low-impact workouts. Resistance training is particularly important for strength, insulin sensitivity, circulation, and lymphatic health.

Reduce Stress & Improve Sleep Quality
Reducing stress and improving your sleep quality are critical for reducing chronic inflammation and improving skin rejuvenation. A 2003 study published in the Archives of Dermatology found that stress can slow wound healing, trigger dermatitis and psoriasis, and cause acne (40). A 2015 study published in Clinical Experiments in Dermatology found that poor sleep can also contribute to accelerated skin aging (41).
Reduce stress in your life by reducing stressful activities and spending time with people who bring you down, and seeking calming, joyful, uplifting, and inspiring activities and people instead. Learn to respond to stress better and bring your body’s stress levels down with the help of breathwork, meditation, guided relaxation, gratitude, visualization, journaling, positive affirmations, positive mindset shifts, prayer, and spiritual practices.
Grounding, spending time in nature, dancing, taking healing baths, and regular ‘me-time’ may also help. To learn more about how to reduce stress, I recommend reading this article.
Avoid stress, sugar, caffeine, and heavy foods before bedtime. Avoid electronics at least two hours before going to sleep. Try relaxing activities, such as taking a healing bath, coloring, arts and crafts, reading poetry or fiction, board games, and journaling instead.
Support your sleep with the help of calming essential oils, such as lavender or chamomile, a supportive and comfortable mattress, bedding, and pillows, light-blocking curtains, and an eye pillow. You may learn more about deep sleep and how to improve it in this article.

Optimize Stomach Acid and Digestive Health
Since gut dysbiosis and digestive problems can influence your skin health, optimizing your stomach acid and supporting your digestive health is critical (5, 6, 7). The most important step is, of course, eating a healthy, anti-inflammatory, and gut-supporting diet I outlined earlier.
Other strategies to improve your stomach acid levels include using apple cider vinegar water, adding ginger to your meals or tea, holding off on drinking water until after your meal, eating slowly, hydrating well outside of mealtimes, and liquid nutrition can also improve your stomach acid levels. I also recommend that you supplement with betaine hydrochloric acid, such as Acid Pro-Zyme to support stomach acid production. To learn more about how to improve your stomach acid levels, I recommend this article.
To further support your digestive health, I recommend Super Digest HCL with betaine hydrochloride (HCI) for proper stomach acidity and optimal breakdown of food. To support your digestion, I recommend taking digestive enzymes, such as Proteo Enzymes, before meals. I also recommend that you try Gut Repair for digestive support and gut health.
To support detoxification, you may want to try Activated Charcoal and BioActive Carbons to remove toxins from your gut. If you are struggling with constipation or irregular bowel movements, I recommend Bowel Mover as a herbal support for elimination.
To further support your digestion and microbiome health, I recommend taking probiotics and consuming probiotic-rich, fermented foods, such as sauerkraut, fermented vegetables, coconut kimchi, kefir, and kombucha. The exception is if you have histamine intolerance. Fermented foods are high in histamine and can trigger symptoms if you have histamine intolerance.
You may also benefit from feeding the good bacteria (probiotics) in your gut with prebiotic-rich foods, such as Jerusalem artichokes, apples, jicama, garlic, onion, and leeks. However, prebiotics-rich foods can be triggering for certain people and are not appropriate if you are on a low-FODMAP or carnivore diet. If you are on these diets or experiencing gut health symptoms, discomfort, or other symptoms, reduce or remove prebiotic foods.

Use Natural Skin Products
Using conventional skin care products with toxins and chemicals can cause skin inflammation, irritation, allergic reactions, dry skin, breakouts, and other skin problems (10). I recommend that you choose natural, organic, and homemade skin care products instead.
You can learn more about natural skin, beauty, and hygiene products in this article. You can learn more about my wife, Angel’s, natural skin care regimen from this video.
Optimize Omega-3 Fatty Acid Levels
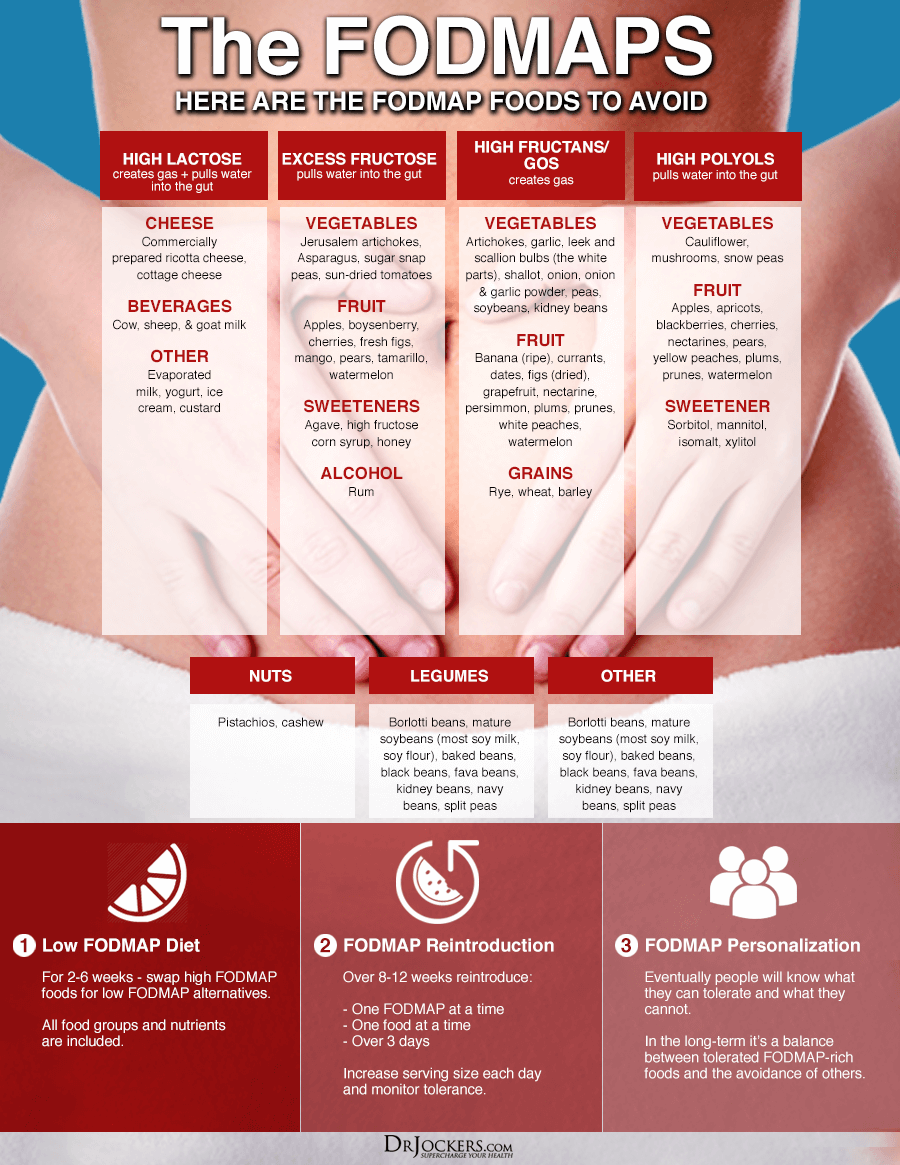
Omega-3 deficiencies can increase skin inflammation and skin issues (14, 15). To optimize your omega-3 levels, I recommend consuming wild-caught fish, flaxseed, chia seeds, hemp seeds, and walnuts.
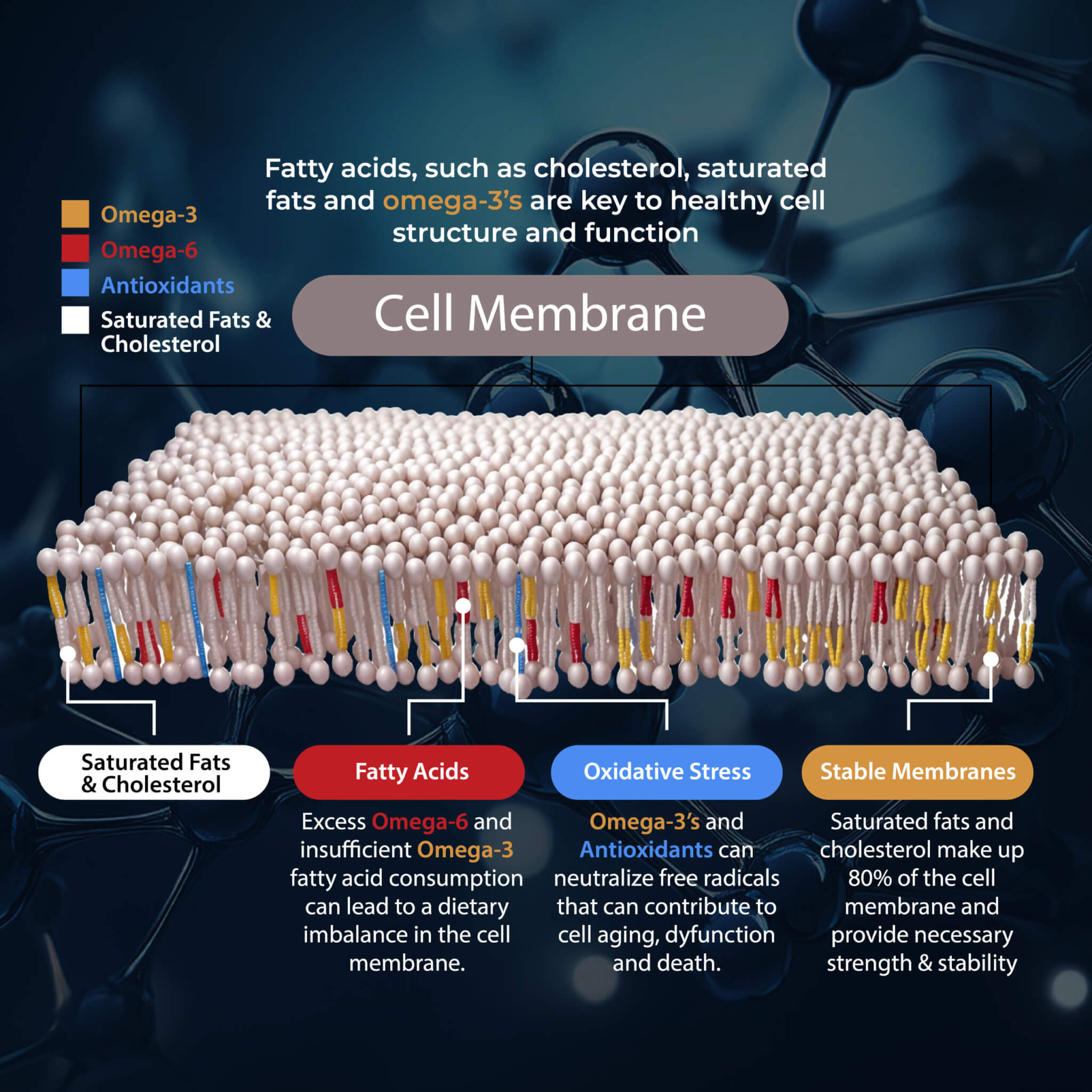
I also recommend taking a high-quality omega-3 fish oil supplement with EPA and DHA, such as Pro Omega Curcumin. This supplement offers anti-inflammatory benefits, reduces oxidative stress, promotes cellular recovery, supports skin health, improves the gut lining, supports vascular elasticity, optimizes cell signaling, and improves gene expression.
Optimize Vitamin A & D Levels
Vitamin A and vitamin D deficiencies can also increase skin inflammation (16, 17, 18, 19). To improve your vitamin A levels, I recommend eating orange and yellow vegetables and fruits, cod liver oil, eggs, grass-fed butter, and dark leafy greens high in vitamin A. If you find that you are deficient in vitamin A, I recommend using ImmunoCharge daily.
To improve your vitamin D levels, I recommend spending time out in the sun and eating vitamin D-rich fatty fish, egg yolks, and beef liver. Most people are not getting enough sunshine or consuming enough vitamin D from food. Therefore, most people need supplements to optimize their vitamin D levels.
Pairing vitamin D3 with vitamin K2 helps improve calcium absorption and inflammation control. I recommend taking a vitamin D3 supplement with at least 3,000-5,000 IU’s of vitamin D3 and at least 90 mcg of vitamin K2. I highly recommend this Vitamin D3/K2 Power.
Typically, taking 1,000 IU per 25 lbs. of body weight will help you get your levels into a healthy range. You want to test your vitamin D levels at least 1-2 times each year and get your levels between 50-100 ng/ml. It has been hypothesized that a therapeutic level for major health conditions is going to be between 70-100 ng/ml.

Optimize Zinc Levels
Zinc deficiency and a poor zinc: copper ratio can also lead to skin inflammation and skin problems (20, 21, 22). I recommend consuming zinc-rich foods such as grass-fed red meat, pasture-raised poultry, seafood, and nuts. Optimizing stomach acid is also very important for the absorption of zinc from dietary sources.
I also recommend supplementing with a high-quality zinc supplement, such as Zinc Charge, daily for optimal zinc levels. This supplement supports antioxidant activity, protects skin health, promotes immune and reproductive health, supports enzymatic reactions and protein metabolism, and improves overall sensory perception.

Consider Using Probiotics
Gut dysbiosis can cause skin inflammations and skin problems (5, 6, 7). For a healthy microbiome and skin health, I recommend supporting your gut flora with a daily probiotic supplement, such as SBO Probiotics.
Additionally, you may benefit from consuming probiotic-rich, fermented foods, unless you have histamine intolerance and are following a low histamine diet. Fermented foods are high in histamine and can be problematic if you have histamine intolerance.

Consider Using Vitamin C and Bioflavonoids
Heavy oxidative stress is one of the potential main causes of skin inflammation (8, 9). Antioxidants can help to combat oxidative stress. Bioflavonoids are protective compounds found in citrus and berries, mainly. Bioflavonoids are phytochemicals that are often found together with vitamin C in nature and are generally considered to be among the most important and interesting classes of biologically active compounds in contemporary research. They offer anti-aging and other health benefits.
Vitamin C is a powerful antioxidant offering benefits for your skin, immune health, wound healing, bones, cartilage, and other areas of your health. A 2018 study published in Frontiers in Physiology has found that vitamin C deficiency may play a role in various skin diseases, including porphyria cutanea tarda, atopic dermatitis, malignant melanoma, herpes zoster, and postherpetic neuralgia, and supplementation with vitamin C may help (42). A 2017 study published in Nutrients has also found that vitamin C can support your skin health, including collagen synthesis and antioxidant support (43).
To support your skin health, I recommend using Super C with vitamin C and bioflavonoid protection. This supplement combines high-potency vitamin C with a standardized, full-spectrum, citrus bioflavonoid complex to offer antioxidant support, immune protection, and better skin.

Consider Using Resveratrol
Resveratrol is a powerful polyphenol found in the skin of red grapes, red wine, berries, cacao, and pistachios. Resveratrol offers antioxidant and anti-inflammatory benefits. It helps to reduce UV radiation, stress, insulin resistance, and other health issues.
According to a 2012 study published in the Archives of Biochemistry and Physiology, antioxidants from grape resveratrol can benefit the outcome of various skin disorders (43). It may reduce oxidative stress, UV damage, accelerated aging, and the risk of skin cancer. According to a 2020 study published in the International Journal of Molecular Sciences, resveratrol may help to reduce inflammation related to atopic dermatitis, eczema, and skin aging (44).
To reduce skin inflammation, signs of early aging, oxidative stress, and skin problems, I recommend consuming resveratrol-rich foods, such as berries, red grapes, and pistachios, and taking a resveratrol supplement daily. I recommend Resveratrol Power with the combined power of resveratrol and an anti-inflammatory flavonol, quercetin. Resveratrol Power supports the aging process, improves skin health, provides protection against cardiovascular damage, and reduces free radical damage to neurons and mitochondria.
Consider Using Quercetin
Quercetin is a plant flavonol with complementary benefits to resveratrol. It can be found in grapes, apples, blueberries, black plums, cherries, cranberries, chokeberries, black currants, cruciferous vegetables, red leaf lettuce, romaine lettuce, kale, cabbage, kale, chicory greens, sprouts, red onions, snap peas, asparagus, peppers, herbs, and olive oil.
Quercetin offers anti-inflammatory benefits that may benefit your skin. A 2016 study published in Clinical, Cosmetic, and Investigative Dermatology found that quercetin may offer anti-itch and soothing benefits (45). A 2016 review published in Drug Discoveries Today found that quercetin may also offer anti-inflammatory benefits in atopic dermatitis (46).
Quercetin also works to improve the histamine response. This is important because histamine intolerance is often a major cause behind skin symptoms, including itching, redness, hives, and swelling (7). Quercetin helps to lower your allergic response while supporting your immune system at the same time. According to a 2016 study published in Molecules, quercetin inhibits the release of histamine and causes an anti-allergic immune response (47).
To reduce skin inflammation and histamine reactions and improve your skin health, I recommend eating quercetin-rich foods and taking a quercetin supplement. I recommend Resveratrol Power with both quercetin and resveratrol.

Use a Great Moisturizer with Antioxidants
To improve your skin health, I recommend Dream Cream, a great moisturizer with antioxidants. It is certified organic, natural, and plant-based. It’s completely free from toxins and chemicals. It moisturizes your skin naturally.
Dream Cream helps to reduce fine lines, wrinkles, age spots, dark spots, uneven skin tone, dull-looking skin, dry skin, sun damage, and saggy skin. It supports your skin with collagen-boosting vitamin C and botanicals, including organic German chamomile extracts, organic astaxanthin extract, organic helianthus annuus (sunflower) seed oil, organic aloe vera leaf juice, organic theobroma cacao seed butter, organic mango seed butter, organic camu camu fruit extract, and organic Indian gooseberry extract.
Purity Woods Age-Defying Dream Cream
Healthy, radiant looking skin is certainly a confidence booster. It is a goal that everyone tries to achieve (and keep) throughout their lives. As we begin to get older, there are millions of tricks, tips, and procedures out there to maintain the same healthy-looking skin we had when we were younger.
That’s why I would like to share my top choice for keeping skin looking young and healthy – the USDA Certified Organic Age-Defying Dream Cream from Purity Woods.
This anti-aging cream is truly a game changer when it comes to achieving and KEEPING your skin looking and feeling spectacular. Now you can save up to 38% on this amazing product, simply click here to learn more!
Red Light Therapy
Red light therapy (RLT) is a powerful therapeutic technique and an alternative healing method. It uses red low-level wavelengths of light for a variety of therapeutic purposes, including wound healing, scars, and other skin issues, inflammation, pain, hair growth, and sleep quality (48).
One of the main reasons people use red light therapy is for its skin health benefits. A study on the benefits of the stimulating, repairing, and skin benefits of RLT found that it may increase collagen production, fibroblast production, mRNA, and circulation between skin cells. As a result, RLT may help skin elasticity and facial texture, reduce fine lines and wrinkles, and lower free radical damage (49).
Red light therapy may also help to treat acne. Just like sunlight, it may reduce the effect of sebum production. However, too much sun exposure can be problematic because of the ultraviolet (UV) and UVB rays, making RLT a great option. Another study has found that it may improve complexion and the overall feeling of the skin, and help to rejuvenate skin cells (49, 50).
If you are looking for a high-quality red light therapy device, I personally use and highly recommend Mito Red Light Therapy Device. It is a third-party tested device with the highest power on the market. Use the coupon code DRJOCKERS at checkout to save 5% on the MitoRed product line.

Red Light Therapy Face Mask
If you are looking for red light therapy benefits specifically for your face, I highly recommend this HigherDOSE Red Light Face Mask. It offers a functional cordless design, which is very convenient. You can use it anywhere in the house and take it with you on trips. It helps to rejuvenate your skin and may be great for acne scarring, fine lines, wrinkles, and your overall skin tone.
Even just one session can make you feel more rejuvenated and fresh in your skin. However, if you use it regularly, you may notice a visible difference in your skin. Less scaring, fewer fine lines, fewer wrinkles, and more importantly, a visible glow are among the potential benefits.
I highly recommend that you add using a HigherDOSE Red Light Face Mask to your daily routine. This is a great time for relaxation, meditation, and some well-deserved ‘me time’. Use the coupon code DRJOCKERS15 to save 15% off on HigherDOSE products including the Red Light Face Mask.

Final Thoughts
Skin inflammation and its related chronic symptoms are incredibly common. It can cause itching, redness, swelling, pain, flakiness, acne, and other symptoms. Most people just try to deal with these symptoms of skin inflammation with various topicals or by just trying to tolerate them.
However, if you understand the underlying root causes of your skin inflammation, you can better your skin naturally. I recommend that you follow my top natural support strategies to improve your skin health.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website offers long-distance functional health coaching programs with our world-class team of health coaches. For further support with your health and other goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and Thrive in Life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!
Sources in This Article Include:








