 Testing Liver Function: Key Lab Markers and Functional Analysis
Testing Liver Function: Key Lab Markers and Functional Analysis
Your liver is one of the largest and heaviest organs in your body, and is an incredible workhorse that does hundreds of critical functions. One of the main jobs of your liver is to support detoxification.
It is also critical for blood sugar stability, bile production, breakdown of fats, production of cholesterol, formation of ketones, assisting the regulation of proper hormone levels, and other health functions. However, if your liver becomes sluggish, it can hinder your body’s natural detoxification process and lead to a list of symptoms and health issues.
In this article, you will learn about the importance of good liver function. You will understand the symptoms of poor liver function. I will discuss the three phases of liver detoxification.
You will learn about key nutrients and supplement support for liver detoxification. I will recommend some key tests to check markers of liver health, including liver function lab markers, organic acid testing for liver function, and GI Map testing for liver function.
Importance of Good Liver Function
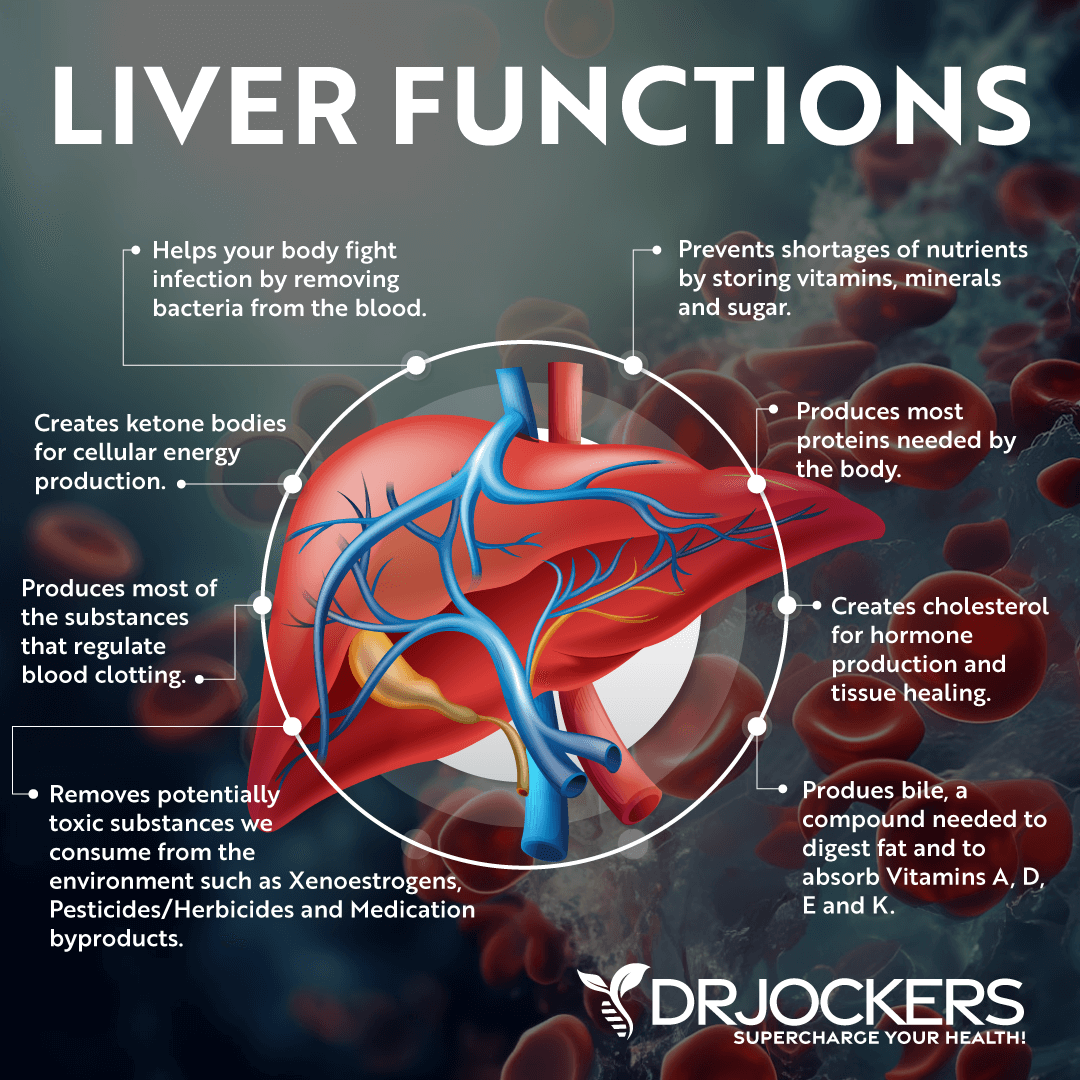
Your liver is one of the largest and heaviest organs in your body, located in the upper right portion of your abdomen under your ribs. It is a critical organ that is responsible for many functions vital to health and life (1).
Your liver is essential for detoxification, blood sugar stability, bile production, breakdown of fats, production of cholesterol, formation of ketones, assisting the regulation of proper hormone levels, and more. Since inactive T4 is converted to the active thyroid hormone T3 in the liver, a sluggish liver is also one of the main causes of thyroid dysfunction.
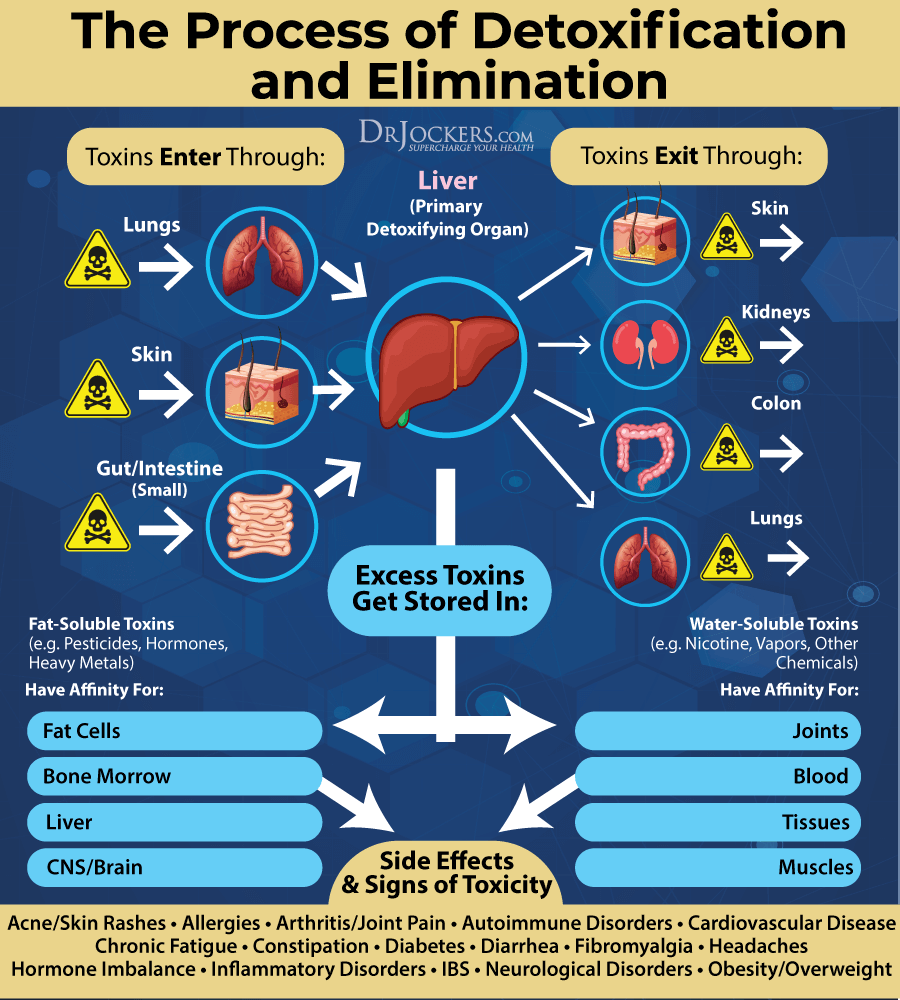
It’s a common misconception that we store toxins in the liver. This is not technically true. Our liver actually deactivates and converts toxins into a form that our body can get rid of through urine, sweat, breath, and bowel movements. The only time the liver would store toxins around the liver is when one has fatty liver. Fatty liver means that you accumulate fat around your liver, and the fat stores toxins.
However, having a sluggish liver can compromise your body’s ability to get rid of toxins at the required speed. Poor liver function can also increase the risk of a variety of chronic symptoms and chronic health issues, including fatty liver disease.
Symptoms of Poor Liver Function
Signs and symptoms of poor liver function may include (2):
- Yellowish skin and/or eyes (jaundice)
- Abdominal pain
- Abdominal swelling
- Loss of appetite
- Nausea or vomiting
- Dark urine color
- Pale stool
- Swelling in the legs or ankles
- Itchy skin
- Tendency to bruise easily.
- Weight loss without trying.
- Chronic fatigue or weakness

3 Phases of Liver Detoxification
Protecting your liver through diet and lifestyle is critical. You can learn about the best foods that can support your liver health here. However, regular detoxification can support a sluggish liver and ensure optimal liver function. Here are the 3 phases of liver detoxification I recommend:
Phase I
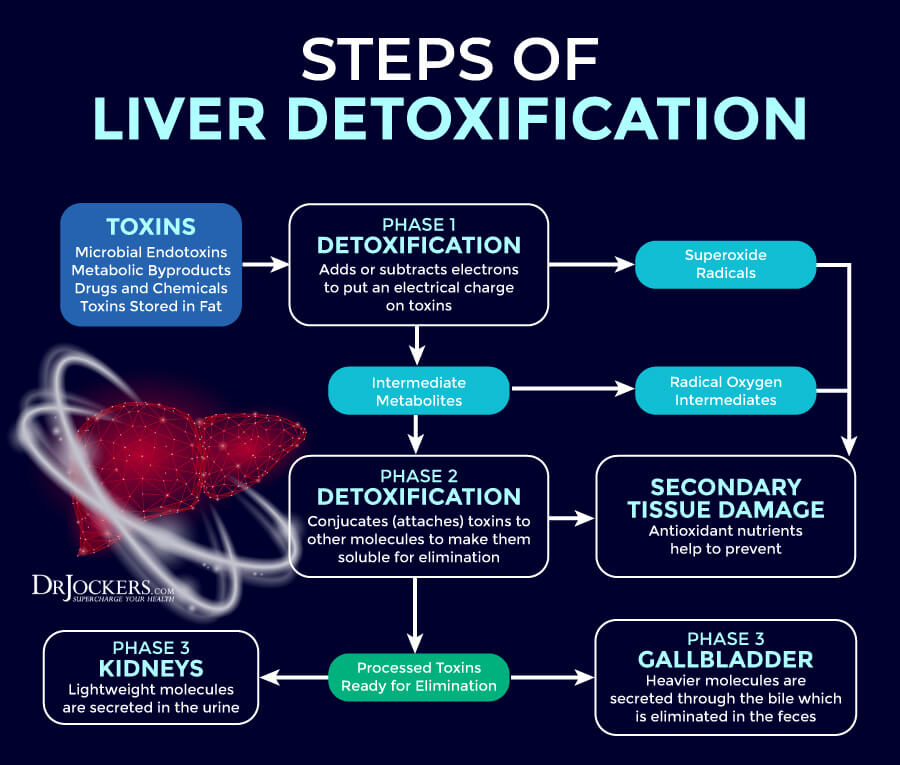
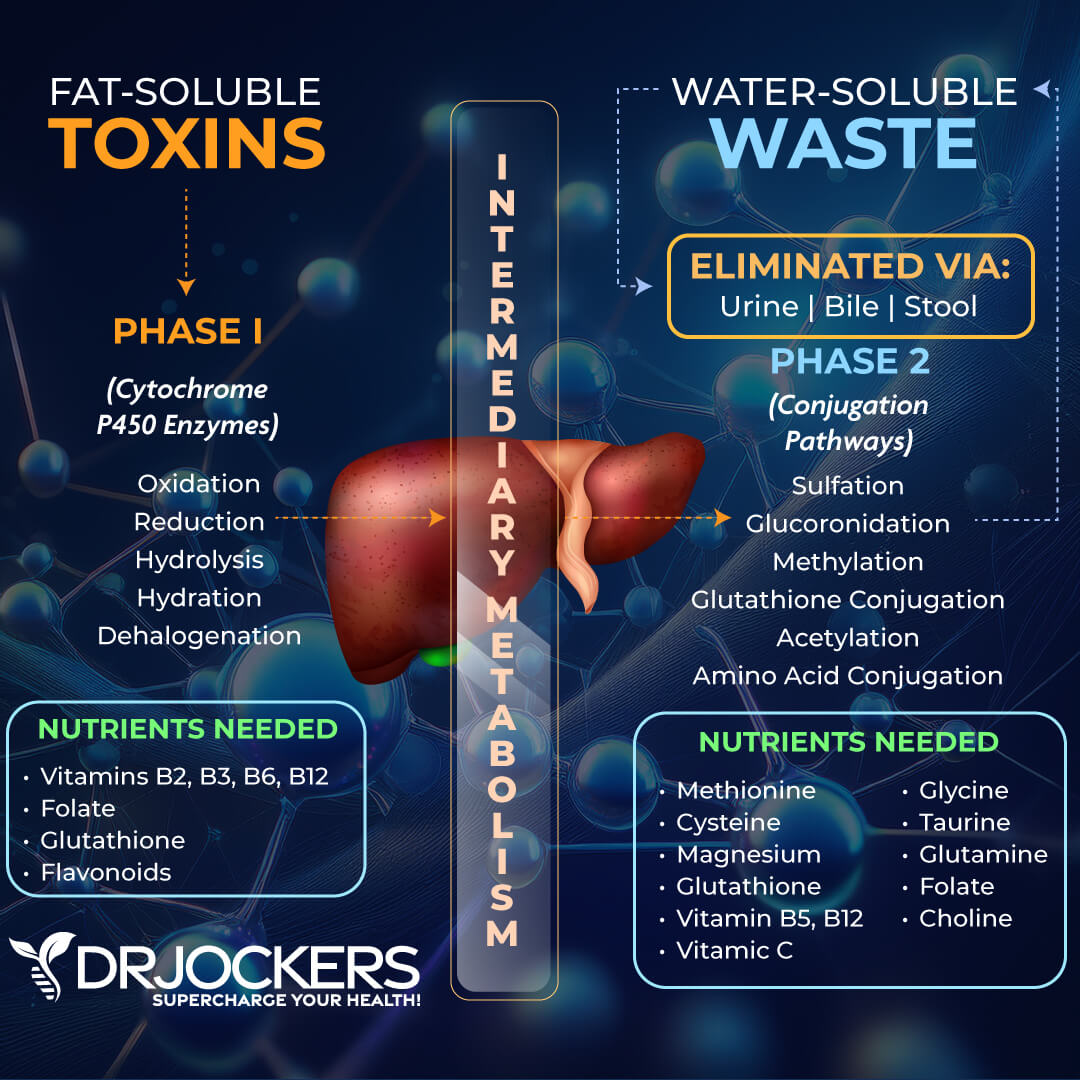
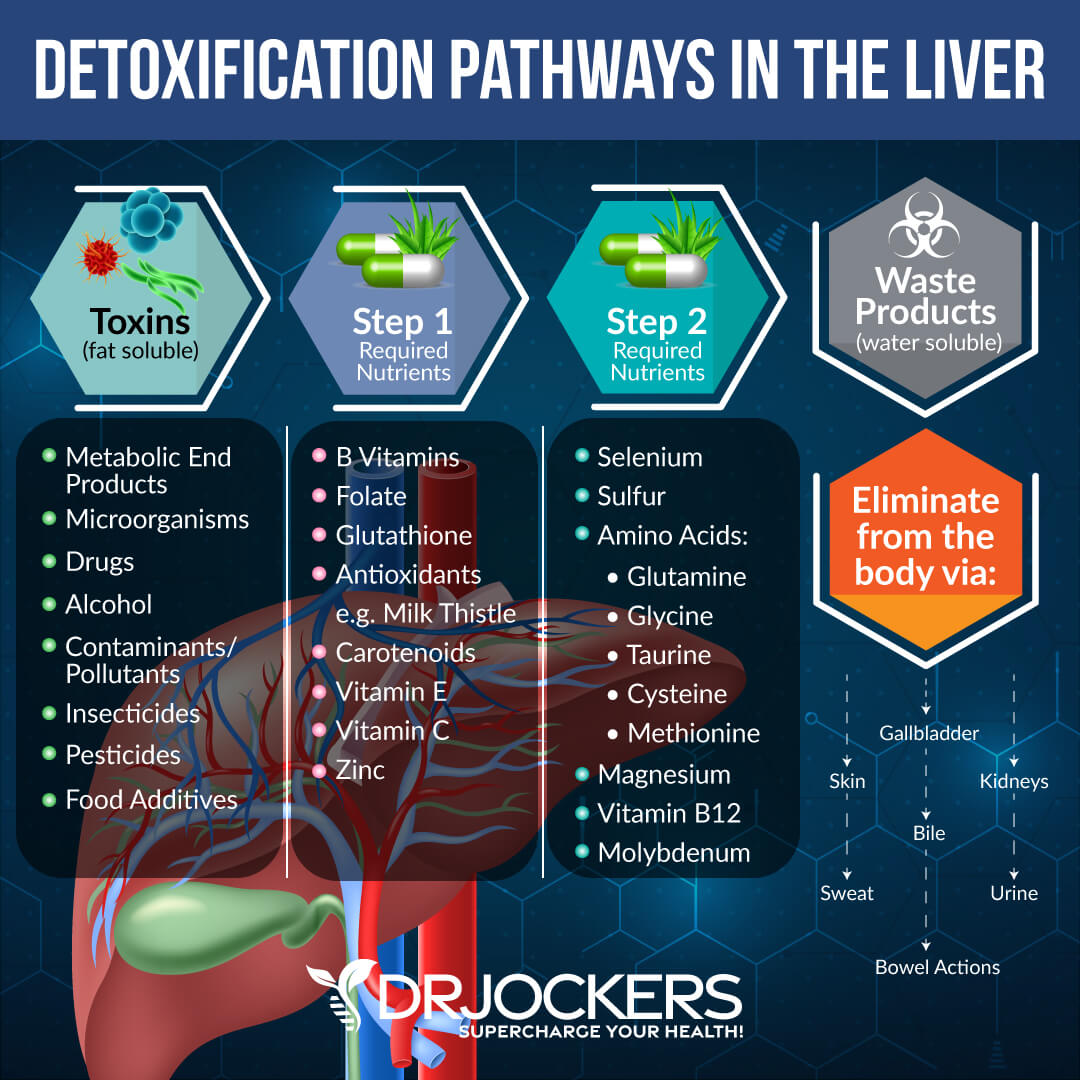
Phase I of liver detoxification is the first step against toxins. Phase I uses cytochrome p450, which is a group of enzymes that help to convert toxins into smaller particles and change toxins into a water-soluble form to get ready for the further steps of detoxification.
The goal of Phase I is the oxidation of harmful toxins and breaking them down into less harmful substances that your body can remove through detoxification pathways. This process involves adding and subtracting electrons for the purposes of oxidation, reduction, hydrolysis, hydration, and dehalogenation to change around these compounds and prepare them for phase II liver detoxification.
Phase I of liver detoxification can be activated by external toxins that your body needs to get rid of, such as alcohol, caffeine, steroids, pesticides, contraceptive pills, paint fumes, and cortisone. It may also be activated by certain herbs and foods in a favorable way. In the next section, I will discuss nutrients and supplements that can assist in Phase I of liver detoxification.
Phase II
The goal of Phase 2 of liver detoxification is conjugation. This is when your body removes metabolites from Phase I through bile, urine, and stool. Phase I creates intermediate metabolites that can create a tremendous amount of oxidative stress in the body unless they are effectively conjugated in Phase II.
The conjugation process involves 6 major metabolic pathways, including methylation, sulfation, glucuronidation, glutathione conjugation, acetylation, and glycination. Each of these pathways depends upon certain nutrients and cofactors.
Many individuals struggle with chronic health issues because they have a fast Phase I but slow Phase II liver detoxification process. In the next section, I will discuss nutrients and supplements that can support Phase II of liver detoxification.
Phase III
The goal of Phase III of liver detoxification is transportation. Everything that leaves your liver in Phase II moves to your kidneys for filtration or into your small intestine through the bile.
Then it can either leave through the bladder and urine from the kidneys or move out via stool through your gastrointestinal (GI) tract. In the next section, I will discuss nutrients and supplements that can assist Phase III of liver detoxification.
Sulfation
Sulfation is dependent on inorganic sulfate availability and is important in the detoxification of steroid hormones such as estrogen, progesterone, testosterone, and DHEA. It is key for the activation of thyroid hormone (T3) from inactive thyroid hormone (T4). The sulfation process metabolizes the catecholamine neurotransmitters norepinephrine, epinephrine, and dopamine.
Sulfation is also key for metabolizing xenobiotics, which are environmental toxins that can cause serious damage in the body. These include the following:
-
BPA (found in plastics, liners of food and drink cans, liners of water pipes, plastic cling wraps, lacquers, varnishes, inks, adhesives, flame retardants, dental sealants & composite materials, sunglasses, water coolers, sports equipment, etc.
-
Triclosan (antibacterial found in cleaning and personal care products; also used in kitchenware, computer equipment, clothes, and children’s toys).
-
Benoxophenone-3 (found in sunscreens, nail polish, makeup, hair & skin care)
-
Butylated Hydroxytoluene (BHT) (food additive/preservative in butter, meats, cereals, chewing gum, baked goods, snack foods, and dehydrated potatoes) is also used in animal feed, cosmetics, pharmaceuticals, rubber, petroleum, and electrical transformers.
-
Xylenol (found in resins, laminates, construction material, and in electric motors (cars, home appliances, power tools, etc.)

Impaired Sulfation
There are several reasons why someone may not have sufficient sulfate levels or have an impaired ability to conjugate sulfate. These include a low protein diet, low intake of sulfate rich foods, high toxin exposure (which depletes sulfate), low magnesium levels, low molybdenum levels, and issues with the sulfotransferase (SULTs) family of enzymes.
Common conditions that are associated with poor sulfation include autism, asthma, chemical sensitivities, chronic fatigue syndrome, degenerative joint disorders, intestinal disorders, lupus, neurodegenerative conditions, and migraines (3, 4, 5, 6). A lab test marker for impaired sulfation is low uric acid levels, under 3.5 mg/dL, especially if this is under 3.0 mg/dL.
Top Ways to Support Sulfation:
There are many things you can do to support the sulfation process. This includes consuming more sulfur-rich foods such as eggs, grass-fed meats, and cruciferous veggies like broccoli, kale, collard greens, cauliflower, cabbage, brussels sprouts, etc. Additionally, the allium family of veggies is rich in sulfur compounds, so eat more onions, garlic, leeks, shallots, and chives.
Epsom salt baths are rich in sulfur and help to supply sulfur compounds and magnesium, which are key for sulfation. Sun exposure is also important here as it stimulates the production of cholesterol sulfate. Finally, you can take supplemental sulfur containing amino acids, which are cysteine, methionine, and taurine. Also, supplementing with the mineral molybdenum is key for proper sulfation pathways.

Phase II: Glucuronidation:
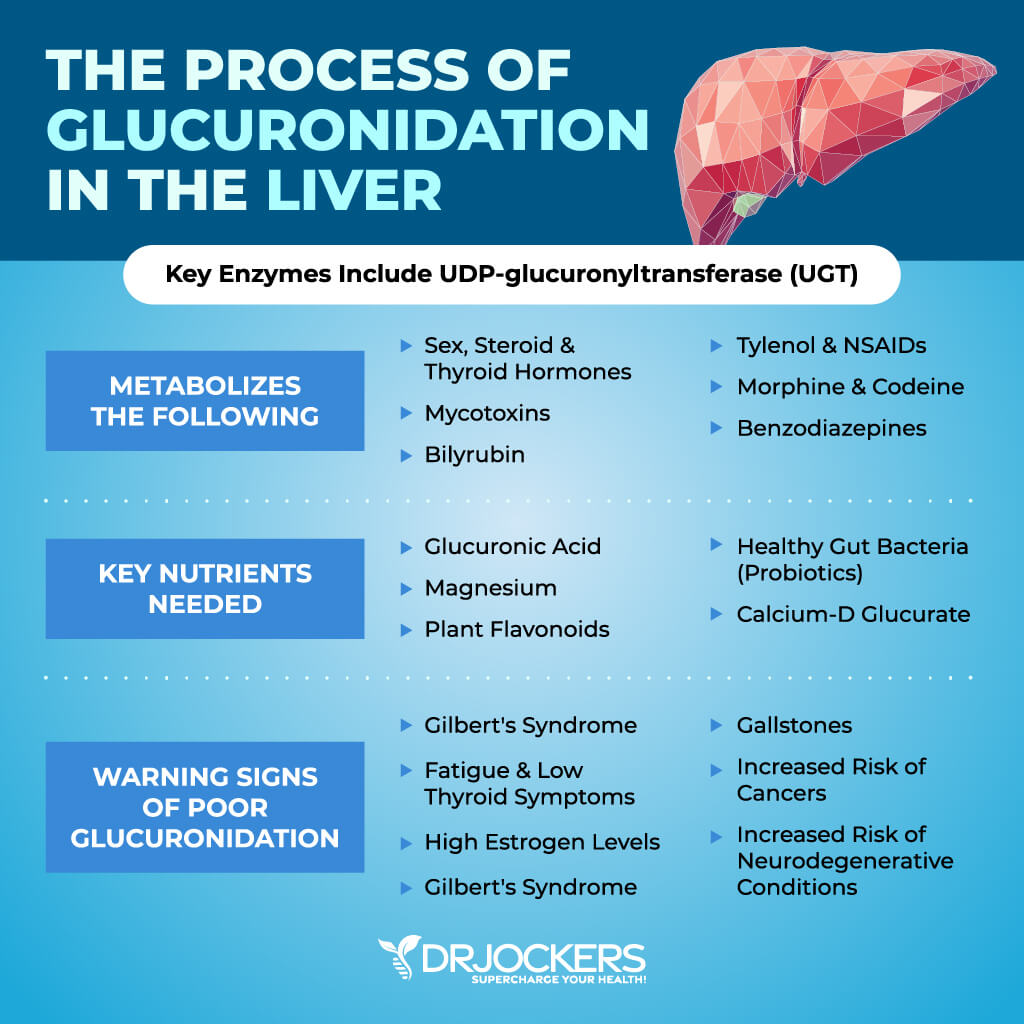
Glucuronidation is one of the most important pathways for phase 2 detoxification, and there is much overlap between sulfation and glucuronidation. Glucuronidation requires adequate levels of glucuronic acids and uses UDP-glucuronyltransferase (UGT). This pathway is especially important for the metabolism of sex hormones, thyroid hormones, mycotoxins, bilirubin, and medications.
Some of the key medications that are metabolized here include Tylenol, NSAIDs, Codeine, Morphine, and Benzodiazepines such as Lorazepam. It is estimated that around 50% of all medications are metabolized by glucuronidation.
Impaired Glucoronidation:
The activity of the UGT enzymes that operate the process of glucuronidation can have genetic weaknesses that impair their function. There is a well-known condition called Gilbert’s syndrome, which is an autosomal dominant disorder caused by a mutation in the UGT-1 gene, and this causes mild to high levels of bilirubin in the blood. This condition is thought to be present in about 10% of the population and can be aggravated during times of stress (7).
The glucorinidation process also depends upon a healthy gut microbiome. An enzyme in the gut called beta-glucuronidase can cleave the metabolites (such as estrogen) from glucuronidation and cause these metabolites to be reabsorbed. This allows these toxins to get back into the bloodstream, where they can cause problems such as estrogen dominance disorders (8).

Key Nutrients to Support Glucuronidation:
Some of the best foods here include cruciferous vegetables, berries, dandelion, milk thistle, asparagus, artichoke, and citrus fruits, which are believed to induce UGT activity. Probiotics are also especially important as they help to cultivate a healthy microbiome to reduce beta glucuronidase activity.
Additionally, supplementing with calcium d-glucurate will help to reduce beta glucuronidase activity. Other very helpful supplements to induce UGT activity include resveratrol, curcumin, astaxanthin, and quercetin (9).
Methylation:
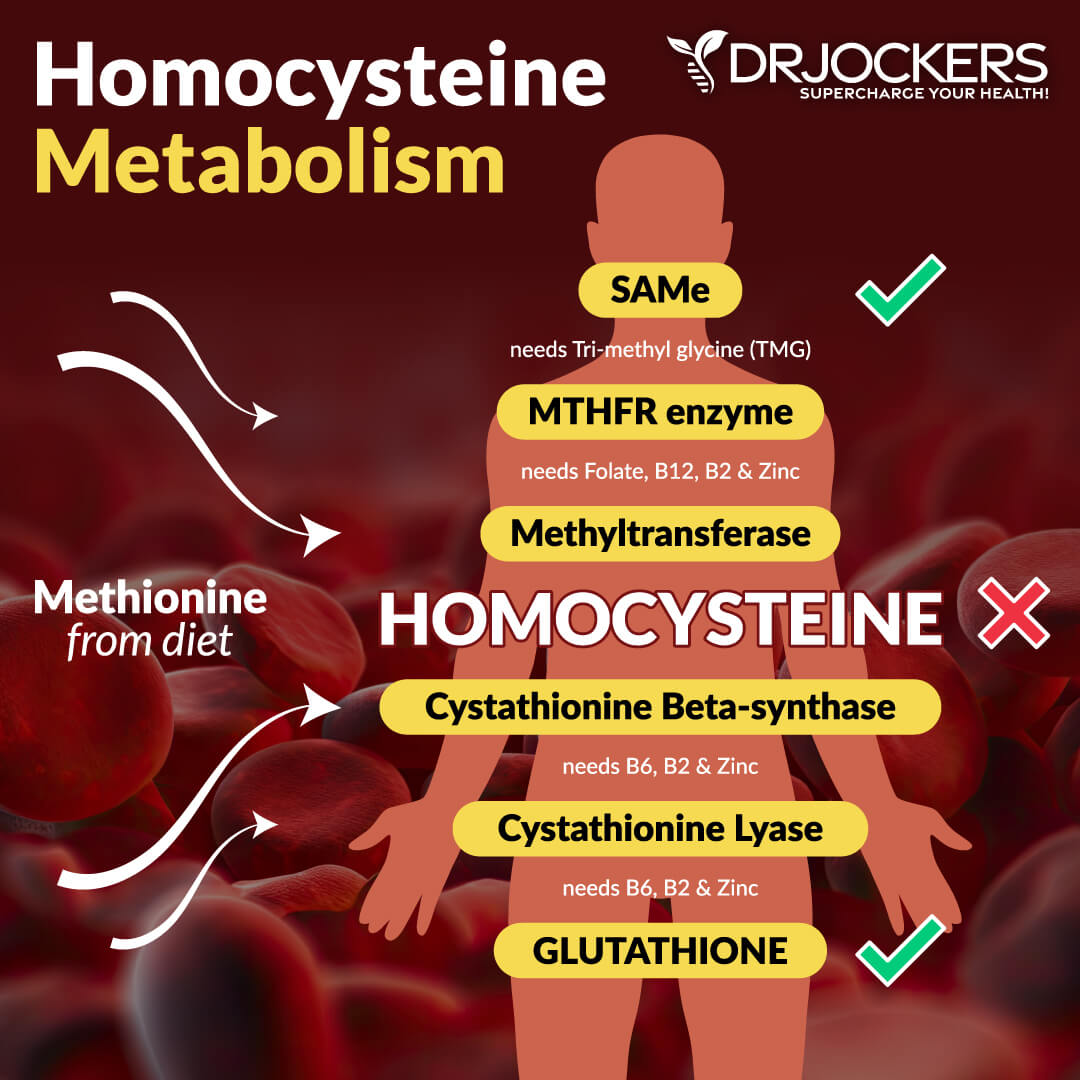
Methylation is a critical process in the liver, but also throughout all the cells of the body. Methyl conjugation occurs through a family of enzymes called methyl transferases.
One of the most famous of these enzymes is cathecol-O-methyltransferase (COMT), which is known for its role in metabolizing estrogens and catecholamines. Most of the methyl groups used for conjugation of toxins come from s-adenosylmethionine (SAMe). To synthesize SAMe, we need the amino acid methionine, choline, B12, and active folate.
Methylation is a key process for metabolizing estrogen, catecholamines, histamine, heavy metals such as arsenic, pesticides, polycystic aromatic hydrocarbons from smoke and grilled foods, and phenols found in plastics, petroleum, etc.

Impaired Methylation
Methylation is often impaired by dysfunctional genes that are producing either too much or too little methylation enzymes, such as COMT or MTHFR. Methylation genes tell us genetic predisposition but do not tell us phenotypic expression, which can be modulated by nutrient levels, gut health, toxic load, and use of methylation inhibitors (such as various drugs like PPIs, birth control pills, antibiotics, nitrous oxide, valproic acid, and cholestyramine). A high sucrose diet may also impair methylation (9).
Additionally, poor stomach acid levels or poor nutritional habits that lead to deficiencies in key amino acids, as well as folate, vitamin B6, B12, magnesium, zinc, and choline, can all cause impaired methylation. Some lab signs of poor methylation include high homocysteine levels (over 9), elevated RBC mean corpuscular volume, low RBC folate, and low serum B12.
Supporting Methylation Conjugation:
Eating a nutrient rich diet that has grass-fed animal products (amino acids, B6, zinc, B12), pasture-raised eggs (amino acids and choline), and green leafy veggies (magnesium and folate) should provide the key nutrients you need. You want to make sure you are producing adequate stomach acid levels to support the absorption of these nutrients.
Additionally, you can supplement with methyl-B12, methylfolate, trimethylglycine, P-5-P (the active form of B6), magnesium, zinc, choline, methionine, and SAMe.
Glutathione Conjugation
This pathway is by far the most important pathway for many of the environmental toxins and carcinogens we are exposed to daily. This process utilizes the enzyme glutathione transferase (GST) and is dependent on glutathione, which is a tripeptide comprised of glycine, cysteine, and glutamine. The rate limiting amino acid is cysteine, and this is why the supplement N-Acetyl Cysteine (NAC) helps boost glutathione levels (9).
Glutathione is the body’s chief antioxidant, and its actions within the detoxification pathways are multifaceted. This is why glutathione is one of the most important supplements recommended for detoxification. Glutathione conjugation occurs in phase 2 detoxification to metabolize pesticides, herbicides, mycotoxins, heavy metals, alcohol, and many medications.

Impaired Glutathione Conjugation:
The main factor that impairs glutathione conjugation is glutathione depletion. This can be due to an overabundance of toxic exposure in either a short period of time or over a chronic period of time.
Many people have amalgam fillings, which leak mercury into the bloodstream over a period of many years, and this can deplete glutathione. Other people may be exposed to a high number of pesticides one day while working in their yard, and deplete glutathione levels.
Many chronic illnesses are associated with low glutathione levels from years of glutathione depletion, which leads to heavy oxidative stress, accelerated aging, and sluggish detoxification.
Supporting Glutathione Levels:
There are a lot of commonalities in the foods and nutrients needed for sulfation and glutathione, such as cruciferous veggies, grass-fed animal products, eggs, garlic, and onions. Additionally, certain supplements help to improve glutathione levels, such as NAC, alpha lipoic acid, selenium, and vitamin C (9, 10).
Taking pure glutathione gets metabolized in the gut into amino acids, so it isn’t an effective way to boost your glutathione levels. However, I do recommend using acetylated glutathione or liposomal glutathione, which are both able to get through the gut and deliver glutathione directly into the cells of the body which bypassing the process of conversion and is the most direct way to support glutathione levels.
Acetylation:
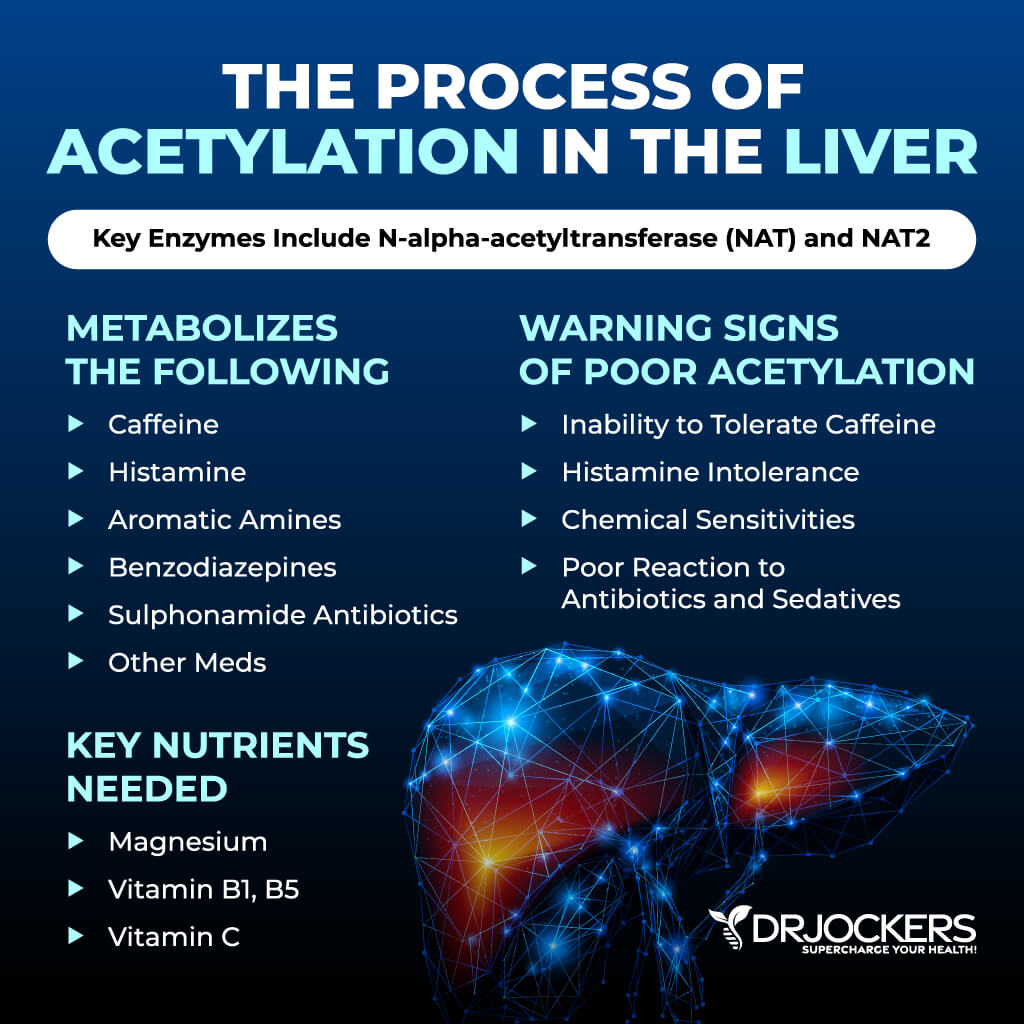
The process of acetylation attaches an acetyl Co-A molecule to the toxin to render it less harmful. The enzyme that mediates this reaction is N-alpha-acetyltransferase (NAT). NAT 2 is the enzyme that is most responsible for liver detoxification (11).
Acetylation is responsible for the metabolism of caffeine, histamine, aromatic amines from industry, and many medications including benzodiazepines (sedative), isoniazid (antibiotic), hydralazine (vasodilator for hypertension) and sulphonamides (antibiotics).
Impaired Acetylation:
While acetylation levels can be impacted by your environment, they are also greatly determined by your genetics. Reduced NAT2 activity would indicate a slower acetylation process, and this gene polymorphism is more common in Caucasians than other races.
If you have histamine intolerance or find that you don’t tolerate caffeine well, it may be a sign of sluggish acetylation (11).
Supporting Acetylation:
Acetylation is supported by a nutrient dense diet that is rich in antioxidants, minerals, and B vitamins. This includes magnesium, vitamin B1, vitamin B5, and vitamin C. Overall, less is known about the acetylation process and the key nutrients that drive it than other phase II pathways (9).
Amino Acid Conjugation or Glycination:
Glycination is the most common type of amino acid conjugation and is predominantly utilized in salicylate and benzoate conjugation. Benzoate is widely used in food preservatives, while salicylates can be found naturally in our food supply and in synthetic forms within medications and personal care products. This pathway is dependent on sufficient amounts of the amino acid glycine.
Some of the key salicylate compounds that need glycinate conjugation include aspirin, Alka Seltzer, and NSAID’s. Salicylates are also found in many common foods, including berries, almonds, peanuts, celery, cinnamon, etc. They are also found in many food dyes, toothpaste, perfumes, cosmetics, and skincare products. You can find more info on salicylates in this article.
Benzoates such as sodium benzoate are widely used preservatives in food, medications, and personal care products. There is some concern that sodium benzoate can convert into the carcinogenic molecule benzene. This has been shown to happen in soda and other products that also contain vitamin C. Additional concerns also exist around an increased risk for hyperactive behavior.

Impaired Glycination:
Glycination is dependent on glyceine-N-acetyltransferase (GLYAT) enzymes and a sufficient amount of glycine, thus, polymorphisms in this gene or insufficient protein intake could impair glycine conjugation. Impaired glycine conjugation has been implicated in increased risk for noninfectious hepatitis and liver cancer (12, 13).
Other warning signs include lethargy, accelerated aging, hepatitis, skin rashes, eczema, rosacea, hives, itchy skin, respiratory issues, headaches, cognitive difficulties, and inability to metabolize aspirin and other salicylates.

Supporting Glycination Conjugation:
There are 2 main ways to support glycination conjugation. One way is to decrease intake and exposure to salicylates and benzoates. The second way is to increase glycine consumption through foods and/or supplements. Other key nutrients needed for this process include magnesium and vitamin B6.
Some of the best foods for glycine include bone broth, collagen protein, turkey, chicken, eggs, beef, duck, lamb, fish, bison, peas, pumpkin seeds, sunflower seeds, lentils, and seaweed.
Bone broth, bone broth protein, collagen protein, or eating the tendons and joint structures of an animal (eating the synovial joint of a chicken wing as an example) is the best way to increase glycine levels from food. You can also use glycine supplements to support glycination conjugation (9).
Tendons and collagenous regions of meat are much higher in glycine than in methionine. Meanwhile, muscle meats are higher in methionine and tryptophan than glycine. Our ancestors ate equal parts of collagenous proteins and muscle meats. In our society today, we mostly consume muscle meats and are often deficient in glycine. You can read about these amino acid ratios in this article here.

Phase I-III Nutrient & Supplement Support
To support the three phases of liver detoxification, I recommend that you add certain nutrients from food and supplements to your daily regimen. Here is what I recommend:
Nutrients and supplements that can support Phase I:
- Herbs: Certain herbs, such as milk thistle, dill, and caraway, can be highly beneficial for your liver and detoxification. A 2002 systematic review published in the American Journal of Medicine has found that milk thistle has therapeutic benefits for liver disease (14). A 2018 study published in ARYA Artherosclerosis has found dill may help to reduce lipid accumulation that can cause fatty liver disease (15). A 2019 review published in Natural Products and Biophosphering has found that caraway may benefit certain diseases, including liver problems (16).
- Cruciferous vegetables: A 2020 study published in Hepatology has found that cruciferous vegetables, such as broccoli, cabbage, cauliflower, Brussel sprouts, kale, and collard greens, may help to reduce inflammation and fatty liver disease (17).
- Citrus: Citrus fruits, including lemon, lime, oranges, and tangerines, may benefit your liver. A 2020 review published in BioMed Research International has found that lemon juice may help alcohol-induced liver injury (18).
- Foods high in vitamin C: A 2003 study published in Nutrition Journal has found that vitamin C may help to reduce the risk of non-alcoholic fatty liver disease (19). Foods that are rich in vitamin C, such as strawberries, oranges, and bell peppers, may help to improve your liver health.
- Vitamins: Certain vitamins, including vitamins A, B, C, and E, may benefit your liver. A 2003 study published in Nutrition Journal has found that vitamins C and E may help to reduce the risk of non-alcoholic fatty liver disease (19). A 2016 review published in Academic Press has found that vitamin B regulation plays a role in alcoholic liver disease, and vitamin B6 and B12 deficiencies can increase the risk of the condition (20). I recommend supplementing with Super C, B Strong, and B12 Power daily.
- Minerals: Certain minerals, including magnesium, selenium, and copper, may benefit your liver health. A 2019 review published in the Annals of Translational Medicine has found that magnesium deficiency is common in liver disease (21). A 2012 clinical trial published in the National Library of Medicine has found that selenium supplementation may help cirrhosis patients with deficiencies (22). A 2019 case series published in Hepatology Communications has found that copper deficiency is a common issue in liver disease patients (23). You may benefit from supplementing with these minerals to support liver detoxification and liver health.
- Lipotropics: According to a 2020 discussion in the book, Textbook of Natural Medicine, lipotropics, such as cysteine, taurine, choline, methionine, and inositol, may help to decrease fatty deposits of the liver, support liver metabolism, and reduce liver problems (24).
- Glutathione: A 2017 study published in BMC Gastroenterology has found that glutathione may benefit the treatment of non-alcoholic fatty liver disease (25). You may benefit from asparagus, avocados, okra, amino acid-containing food, and Super Glutathione supplementation for liver health.
- Resveratrol: A 2015 review published in the Journal of Research of Medical Sciences has found that resveratrol may be beneficial for those with liver disease (26). To support liver detoxification and liver health, you may benefit from resveratrol-rich foods, such as red grapes and berries, and daily Resveratrol Power supplementation.
- Coenzyme Q10: A 2015 randomized control trial published in the Journal of the American College of Nutrition has found that coenzyme Q10 may help liver enzymes, reduce inflammation, and improve liver health (27). You may benefit from coenzyme Q10 supplementation for liver health to support this phase. I highly recommend MitoActive.
Nutrients and supplements that support Phase II:
- Sulfur-rich foods: A 2014 study published in Molecules has found that sulfur-rich foods may reduce the risk of fatty liver disease (28). Consuming sulfur-rich foods, such as cruciferous vegetables, onions, garlic, egg yolks, and meat during Phase II of liver detoxification may benefit your liver health.
- Amino acids: A 2019 review published in the Journal of Cancer Prevention has found that amino acids, including glycine, cysteine, taurine, and methionine, have therapeutic benefits for liver diseases (29). I recommend eating plenty of pasture-raised meat to meet your amino acid needs for liver health.
- Vitamin B12: A 2016 review published in Academic Press has found that vitamin B regulation plays a role in alcoholic liver disease, and vitamin B12 deficiencies can increase the risk of the condition (20). I recommend supplementing with B12 Power daily.
- Molybdenum: A 2018 animal study published in the Biological and Pharmaceutical Bulletin has found that molybdenum may reduce fat accumulation around the liver (30). You may meet your molybdenum needs from leafy green vegetables and liver. I also recommend CT-Minerals with molybdenum and other bioactive carbons.
- Glutathione: A 2017 study published in BMC Gastroenterology has found that glutathione may benefit the treatment of non-alcoholic fatty liver disease (25). You may benefit from asparagus, avocados, okra, amino acid-containing food, and glutathione supplements. I highly recommend Super Glutathione supplementation for liver health.
- Flavonoids: A 2015 review published in Current Medicinal Chemistry has found that flavonoids may benefit the treatment of non-alcoholic fatty liver disease (31). I recommend eating plenty of herbs, vegetables, and fruits to meet your flavonoid needs and support your liver. I also recommend using Gut-Liver Cleanse Protein as a good source of flavonoids and other gut-supporting nutrients.
- Ellagic acid: A 2018 animal study published in Biomedicine and Pharmacotherapy has found that ellagic acid may reduce liver damage (32). You can get ellagic acid from consuming garlic, rosemary, cabbage, and red grape skin. I recommend using Gut-Liver Cleanse Protein as a good source of ellagic acid.
Nutrients and supplements that support Phase III:
- Water: Plenty of water for proper hydration to support kidney function and elimination through urine. A 2019 randomized controlled trial published in Clinical Research in Hepatology and Gastroenterology has found that hydrogen-rich water may improve liver enzymes and reduce fat accumulation around the liver (33). I recommend that you drink plenty of water throughout the day and try hydrogenized water for extra liver support. You may learn about hydrogen water in this article.
- Gut Support: A 2018 study published in Medical Sciences studied the gut-liver axis and found that bad gut bacteria and gut dysbiosis can affect liver health (34). It’s important that you support healthy gut function to liver health and support elimination through stool. Gut-Liver Cleanse Protein is a great protein powder created to support your digestion, detoxification, and antioxidant balance while supplying you with clean protein.
Key Liver Function Lab Markers
To understand your liver health and spot underlying health issues, I recommend the following key liver function lab markers:
AST
Alanine aminotransferase (AST) is a liver enzyme. When the liver is stressed, these enzymes go up. If you have a sluggish liver or gallbladder, you may present with elevated AST levels. Normal levels are between 10 and 26 IU/L.
AST is an enzyme found in all the major muscles of the body, the kidneys, lungs, and the heart. If AST is elevated over the normal levels and far above ALT and GGT, then it typically indicates the major area of damage is outside of the liver, most commonly in the heart or kidney. This can be an indicator, along with other biomarkers such as high blood urea nitrogen (BUN) and low GFR, for kidney damage. It can also be an indicator if you see high LDH and high hs-CRP for heart inflammation.
ALT
Aspartate transaminase (ALT) is an enzyme present in the liver that spills out during times of increased liver stress. Elevated ALT levels may indicate poor liver or gallbladder health. Normal levels are between 10-26 IU/L.
If ALT is elevated above normal levels and far above AST and GGT, then it typically indicates a problem with the liver specifically. B6 is necessary to produce AST & ALT so if you see these levels low, it may indicate a B6 deficiency.
Alkaline Phosphatase
Alkaline phosphatase is a liver enzyme that is made by the mucosal cells that line the biliary system of the liver and helps normal bile flow. High alkaline phosphatase is one of the most sensitive markers for sluggish gallbladder or gallstones. If you see this elevated (over 95) and high bilirubin and liver enzymes, then think of liver and gallbladder problems.
Alkaline phosphatase is also part of the bone-building process, so it is normally high in growing children and teenagers, and in individuals who are recovering from a broken bone, and in some cases, those with bone diseases such as osteoporosis. Alkaline phosphatase is a zinc dependent enzyme, so low levels under 50 are often a sign of a zinc deficiency.
GGT
Gamma-Glutamyl Transpeptidase (GGT) is an enzyme in the liver, pancreas, and kidneys. It is elevated in all forms of liver disease and functionally increased due to alcoholism and/or sluggish gallbladder or gallstone obstruction. Normal levels are between 10 and 26 IU/L.
High levels indicate a glutathione deficiency, and levels lower than 10 IU/L can be an indication of a vitamin B6 or magnesium deficiency. High levels of GGT above the normal range and far above the AST and ALT often indicate a problem outside the liver but inside the biliary tree (gallbladder, pancreas, or common bile duct).
LDH
Lactate dehydrogenase (LD or LDH) is a critical enzyme for energy production in your cells. LDH is found in the highest levels in your liver, kidneys, heart, lungs, muscles, and blood cells. Some bacteria may also produce LDH. LDH testing may be used to detect liver problems, liver disease, tissue damage, inflammation, and anemia. It may also help to determine the prognosis of certain cancers, including lymphoma, leukemia, ovarian cancer, and testicular cancer.
LDH levels can be measured in the blood (blood LDH) and as fluid LDH around an infection or area of inflammation. Normal LDH levels are between 140 U/L to 280 U/L or 2.34 mkat/L to 4.68 mkat/L. Over 180 is a sign of inflammation often impacting the liver. Under 140 is a sign of hypoglycemia and issues with glycolytic energy production.
Bilirubin
High bilirubin is the byproduct of hemolysis (RBC destruction) and the result of the breakdown of hemoglobin. Bilirubin is excreted in bile and urine, and elevated levels may indicate certain diseases.
It causes the yellow color of bruises, the yellow discoloration in jaundice, and the brown color of feces. Increased levels are typically the signs of liver, gallbladder, or spleen dysfunction. High levels can be broken down into conjugated and unconjugated with additional testing to determine the cause.
High conjugated bilirubin and elevated liver enzymes may indicate gallbladder problems. High unconjugated bilirubin may be caused by a spleen disorder or hemolytic anemia.
Elevated bilirubin with normal liver enzymes may indicate a genetic disorder called Gilbert’s syndrome, which is a harmless condition where the liver has poor bilirubin processing and a mild state of jaundice. In certain cases, this may be an indication of poor bile flow and bile flow support nutrients should be considered. Normal levels are between 0 and 1.2 mg/dL.
Albumin
Serum albumin is one of the most important blood proteins in human plasma. It helps to transport nutrients and electrolytes, including potassium, calcium, and sodium, antioxidants, including glutathione, and hormones, such as thyroid T4. Low albumin levels may increase the risk of mortality. Most of the albumin in your body is produced by your liver.
Albumin production also heavily relies on glutathione in your liver and protein consumption. Low-protein and vegetarian diets can also increase the risk of deficiencies in albumin.
Normal albumin levels are between 4 and 5 g/dL. Low levels of albumin may indicate poor liver function, low glutathione levels, low levels of antioxidants, oxidative stress, or protein deficiency. When albumin is over 5, it is often an indicator of dehydration, acute infections, burns, recent surgery, or a heart attack.
Additional signs of oxidative stress other than low albumin include low lymphocytes (under 20%), high uric acid (above 5.9), decreased platelet levels (under 150), high LDL: HDL cholesterol ratios (over 3:1), and high globulin levels (above 2.8).

Comprehensive Blood Analysis
To check for these liver function markers, I recommend a Comprehensive Blood Analysis (CBA), which is a very detailed blood test that looks at all of these markers of inflammation. This test is more sophisticated than most conventional doctors run.
It examines all parameters for inflammation, blood sugar levels, thyroid function, zinc and copper ratio, vitamin A and D levels, a complete metabolic panel, complete blood count, liver function, nutrient deficiencies, and more. I recommend getting the Comprehensive Blood Analysis done regularly both as a preventative measure and to monitor your inflammation levels and progress if you are on a treatment plan.

Organic Acid Testing for Liver Function
In addition to these key function liver lab markers, I also recommend organic acid testing for liver function.
Hippuric Acid
Hippuric acid is found in urine as a metabolite of aromatic compounds from food components or a metabolite of therapeutic components, such as acetylsalicylic acid. The normal range of hippuric acid is 0.44 ± 0.20 g/L. High levels of hippuric acid are an indication of high phase I and low phase II liver activity.
Pyroglutamic Acid
Pyroglutamic acid is an intermediate substrate that plays a role in the synthesis of glutathione. Normal levels of pyroglutamic acid are between 28 and 58 ug/mg.
High levels of pyroglutamic acid indicate that your body is using too much glutathione and losing amino acids, which may affect your liver. Low levels of pyroglutamic acid may also mean glutathione deficiency.
2-Hydroxybutyric Acid
2-hydroxybutyric acid is a form of hydroxybutyric acid that can indicate oxidative stress. It is often found in the urine of people with lactic acidosis and ketoacidosis.
Elevated levels of 2-hydroxybutyric acid may indicate glucose intolerance and insulin resistance. Normal levels are between 0.03 and 1.8 mmol/mol creatinine.
2-Hydroxyhippuric Acid
This is a conjugate of the amino acids, glycine and hydroxybenzoic acid (salicylic acid). Intake of aspirin (salicylates) or the growth of salicylate-producing gastrointestinal bacteria may elevate levels. Also increased after the ingestion of the artificial sweetener, aspartame (Nutrasweet).
If this is high, it is a sign of poor phase II liver detoxification, and you want to boost glycine or reduce salicylates and benzoates.
Orotic Acid
Orotic acid levels are used for testing for hyperammonemia and hereditary orotic aciduria. Normal levels of orotic acid are between 0.2 and 1.5 mmol/mol creatinine. High levels of orotic acid may indicate liver problems or fatty liver disease.

GI MAP Test for Liver Function
Along with a Comprehensive Blood Analysis, I also recommend a GI Map Stool Test to further understand your liver function and digestive health, and help with appropriate lifestyle changes for improved digestive health. Besides liver function, the GI Map Stool Test also checks gut dysbiosis, parasites, gut inflammation, and other markers of digestive health.
Beta-Glucuronidase
Beta-glucuronidase is an enzyme. It is produced by unfriendly gut bacteria. It helps to break down the bond between glucuronic acid and toxins in your gut. Normal levels of beta-glucuronidase are under 2486 U/mL.
Elevated levels can disrupt your body’s natural ability to detoxify. High levels may indicate a microbiome imbalance, gut inflammation, sluggish bile flow, liver inflammation, or cirrhosis of the liver.
Steatocrit
Steatocrit levels are used for measuring the amount of fat in the stool. It only requires one single stool sample, making it a simpler and more convenient option instead of a 72-hour fecal fat test. Normal levels of steatocrit are between 0 and 14.9 percent. High levels may indicate fat malabsorption, primary biliary cirrhosis, and other liver diseases.

Final Thoughts
Your liver is one of the largest, heaviest, and most important organs. One of the main jobs of your liver is to support detoxification. It is also critical for blood sugar stability, bile production, breakdown of fats, production of cholesterol, formation of ketones, assisting the regulation of proper hormone levels, and other health functions.
If your liver function becomes sluggish and compromised, it can seriously impact your body’s natural detoxification process and lead to a list of symptoms and health issues. If you are experiencing symptoms of poor liver health, I recommend that you get tested for certain markers of liver health with the help of the tests I recommend in this article, including liver function lab markers, organic acid testing for liver function, and GI Map testing for liver function.
If you want to work with a functional health coach, I recommend this article with tips on how to find a great coach. Our website offers long-distance functional health coaching programs with our world-class team of health coaches. For further support with your health and other goals, just reach out—our fantastic coaches are here to support your journey.
Inflammation Crushing Ebundle
The Inflammation Crushing Ebundle is designed to help you improve your brain, liver, immune system and discover the healing strategies, foods and recipes to burn fat, reduce inflammation and thrive in life!
As a doctor of natural medicine, I have spent the past 20 years studying the best healing strategies and worked with hundreds of coaching clients, helping them overcome chronic health conditions and optimize their overall health.
In our Inflammation Crushing Ebundle, I have put together my very best strategies to reduce inflammation and optimize your healing potential. Take a look at what you will get inside these valuable guides below!








Thank you for the informative article. How can someone raise albumin levels?
Thank you.
Eat more protein and keep your blood sugar stable and reduce inflammation.
Very useful article
Wow, I’m going to have to reread this whole article several times. It’s been suggested that I might have Gilbert’s Syndrome and this is by far the best source of info on it that I’ve found on the web, including supplements and diet to help process the bile out of my body. I learned so much and hope that the whites of my eyes might return! Thank you.
Where do coffee enemas come in on the detoxification process? I don’t see them listed in any of the suggestions in the article and would like to know if they are a benefit. Thanks!
Yes they can be very helpful. Here is a helpful article: https://drjockers.com/detoxify-body-coffee-enemas/
My alkaline phosphatase has always been low except for the immediate postpartum/breastfeeding period. As of last measure it was 28. Yet my zinc RBC and serum are fine. Is there another way to evaluate for zinc deficiency?
Yes – you can get your plasma zinc levels tested and they should be between 90-135 https://drjockers.com/15-zinc-deficiency-symptoms/